Distal Femoral Extension Osteotomy and Patellar Advancement for Crouch Gait
Key Takeaway
Join us in the OR for a masterclass on correcting crouch gait through distal femoral extension osteotomy and patellar advancement. We'll meticulously cover patient selection, precise surgical anatomy, detailed intraoperative steps, critical pearls for success, and comprehensive postoperative management to restore optimal knee function and improve ambulation in complex neuromuscular conditions like cerebral palsy.
Introduction and Epidemiology
Crouch gait is a debilitating kinematic abnormality defined as walking with excessive knee flexion during the stance phase of the gait cycle. This pathological gait pattern is predominantly observed in patients with neuromuscular conditions, most notably cerebral palsy (CP), particularly in those with spastic diplegia. As the child matures, crouch gait frequently precipitates a cascade of biomechanical failures, leading to progressive loss of function, severe anterior knee pain, and, ultimately, the cessation of independent ambulation.
The management of persistent crouch gait represents one of the most complex challenges in orthopedic neuro-rehabilitation. When conservative measures and soft tissue procedures fail, or when fixed bony deformities have established themselves, Distal Femoral Extension Osteotomy (DFEO) combined with Patellar Tendon Advancement (PTA) becomes the definitive surgical intervention to restore the biomechanical integrity of the extensor mechanism and achieve full knee extension.

Pathogenesis of Crouch Gait
The etiology of crouch gait in cerebral palsy originates from preterm, perinatal, or infantile brain injury, resulting in a static encephalopathy. This upper motor neuron lesion manifests as hypertonia (primarily spasticity), impaired selective motor control, and profound muscle weakness. In a typically developing child, muscle growth is stimulated by the tension produced during normal bone growth and age-appropriate gross motor activities. However, in the presence of spasticity, musculotendinous growth is severely delayed. Spastic muscles fail to elongate normally in response to skeletal growth and physiological stretch.
Consequently, bone growth and joint development are adversely affected by this lack of normal functional activity. The persistent imbalance between spastic flexors and weak extensors alters the mechanical forces acting across the developing physis, leading to secondary torsional deformities, such as excessive femoral anteversion and external tibial torsion, which further exacerbate the mechanical inefficiency of the lower extremity.
Natural History and Progression
Crouch gait is frequently observed between 5 to 7 years of age. In this early stage, the primary drivers are dynamic: spasticity of the hamstrings, weakness of the triceps surae, and impaired balance mechanisms. If dynamic crouch persists into later childhood, structural adaptations occur. Musculotendinous contractures develop predominantly in the two-joint muscles, including the psoas, hamstrings, rectus femoris, and gastrocnemius.
Persistent alignment in a flexed knee posture places chronic, excessive tension on the extensor mechanism. This leads to the pathological elongation of the one-joint muscles and their tendinous attachments, specifically the gluteus maximus, soleus, and the quadriceps. The chronic eccentric loading of the quadriceps invariably leads to elongation of the patellar tendon, resulting in severe patella alta.
By adolescence, the combination of fixed knee flexion deformity (posterior capsular contracture) and patella alta severely compromises the lever arm of the extensor mechanism. Patients often experience a precipitous functional decline due to patellofemoral pain, stress fractures of the patella, and profound fatigue, culminating in a transition from community ambulation to wheelchair reliance.
Surgical Anatomy and Biomechanics
A thorough understanding of lower extremity kinematics and the specific anatomical alterations in the neuromuscular knee is prerequisite for successful surgical reconstruction.

Distal Femoral Osteology and Capsular Anatomy
The typical physiological knee extension range is 0 degrees (full extension). In chronic crouch gait, the posterior capsule undergoes dense fibrotic contracture due to the constant flexed posture and the continuous resting tension of the spastic hamstrings. While the intrinsic osseous anatomy of the distal femur may appear grossly normal, the spatial orientation is frequently abnormal. Torsional deformities, specifically excessive femoral anteversion, are highly prevalent in the CP population. This internal rotation of the femur lateralizes the mechanical axis and alters the tracking of the patella, contributing to extensor mechanism dysfunction.
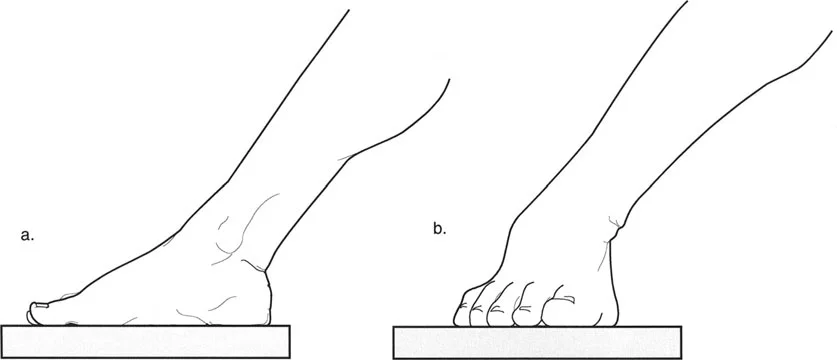
The Plantarflexion Knee Extension Couple
Normal upright posture and efficient gait depend heavily on the plantarflexion-knee extension couple. The soleus muscle is primarily responsible for restraining the forward translation of the tibia over the plantigrade foot during the second rocker of stance phase. When the soleus functions normally, the ground reaction force (GRF) vector falls anterior to the knee joint center in midstance, creating an extension moment that minimizes the muscular demand on the quadriceps.
In patients with CP, if the ankle plantarflexors are weak (often iatrogenically induced by previous isolated Achilles tendon lengthenings) or elongated, they fail to restrain this forward tibial progression. The loss of the normal plantarflexion-knee extension couple causes the GRF vector to shift posterior to the knee joint center. This generates a massive, sustained flexion moment at the knee, requiring continuous, high-intensity quadriceps firing to prevent structural collapse.

Patellofemoral Mechanics and Patella Alta
The continuous demand on the quadriceps in the setting of a flexed knee acts as a chronic stretching force on the patellar tendon. The patella migrates proximally, exiting the trochlear groove. Patella alta drastically reduces the mechanical advantage of the quadriceps by shortening its moment arm. Furthermore, the patella loses its bony stability from the trochlea, leading to subluxation, altered contact pressures, cartilage degradation, and intractable anterior knee pain. Surgical intervention must simultaneously address the bony flexion deformity and the proximal migration of the patella to restore the biomechanical efficiency of the knee.
Indications and Contraindications
Distal femoral extension osteotomy is indicated when structural deformities preclude the restoration of upright posture through soft tissue lengthening alone. Patient selection is critical, as this is a highly invasive procedure requiring significant postoperative rehabilitation.

Operative Thresholds
| Indication Category | Specific Criteria for DFEO + PTA |
|---|---|
| Clinical Deformity | Fixed knee flexion contracture ≥ 10 to 15 degrees under anesthesia. |
| Radiographic Findings | Insall-Salvati ratio > 1.2 (indicating significant patella alta). |
| Gait Kinematics | Persistent stance phase knee flexion > 20-30 degrees not correctable by AFOs. |
| Symptomatology | Intractable anterior knee pain, declining walking velocity, increased energy expenditure. |
| Previous Surgery | Failed prior soft-tissue hamstring lengthenings resulting in recurrent crouch. |
| Contraindication Category | Specific Criteria |
|---|---|
| Absolute | Active joint infection, severe medical comorbidities precluding prolonged anesthesia. |
| Relative (Biomechanical) | Severe, unaddressed hip flexion contractures (>20 degrees) or fixed equinus. These must be addressed concurrently in a Single-Event Multilevel Surgery (SEMLS) approach. |
| Relative (Bone Quality) | Profound osteopenia precluding rigid internal fixation (requires modified fixation strategies). |
| Relative (Functional) | Non-ambulatory patients (GMFCS Level V) where the goal is purely positioning; a simpler procedure may suffice unless pain is the primary indication. |
Pre Operative Planning and Patient Positioning
Meticulous preoperative planning is required to quantify the exact degree of deformity in the sagittal, coronal, and axial planes.
Clinical Examination and Gait Analysis
The physical examination must differentiate between dynamic spasticity and fixed contracture. The popliteal angle is measured to assess hamstring tightness, while the Thomas test evaluates concurrent hip flexion contractures. The Duncan-Ely test assesses rectus femoris spasticity.
Three-dimensional Instrumented Gait Analysis (IGA) is the gold standard for preoperative planning. IGA provides objective kinematic and kinetic data, confirming the presence of a persistent knee flexion moment during stance and quantifying the degree of internal hip rotation (femoral anteversion) and external tibial torsion. This data dictates whether the DFEO must incorporate a derotational component.

Radiographic Evaluation
Standard weight-bearing anteroposterior (AP) and lateral radiographs of the lower extremities are obtained. A true lateral of the knee at 30 degrees of flexion is critical for measuring the Insall-Salvati ratio or the Caton-Deschamps index to quantify patella alta. Long-leg alignment films are utilized to assess coronal plane mechanical axis deviation, which can be corrected concurrently during the osteotomy. The exact angle of the anterior closing wedge is templated based on the degree of fixed flexion deformity measured clinically and radiographically.
Operating Room Setup and Positioning
The patient is positioned supine on a radiolucent operating table to allow for unencumbered fluoroscopic imaging in both the AP and lateral planes. A sterile tourniquet is applied to the proximal thigh. A bump may be placed under the ipsilateral hip to control external rotation if necessary. The entire lower extremity is prepped and draped free to allow intraoperative assessment of range of motion and alignment.
Detailed Surgical Approach and Technique
The procedure is typically performed as part of a Single-Event Multilevel Surgery (SEMLS). The DFEO and PTA are executed sequentially to address the bony and soft-tissue components of the deformity.

Surgical Exposure
An anterior longitudinal incision is generally preferred as it provides excellent access for both the distal femoral osteotomy and the patellar tendon advancement. The incision extends from the distal third of the femur, over the midline of the patella, down to the tibial tubercle.
Deep dissection utilizes a subvastus or transvastus approach to expose the distal femoral metaphysis. The vastus medialis is elevated off the intermuscular septum and retracted anteriorly and laterally. Perforating vessels are meticulously identified and ligated. The suprapatellar pouch is elevated, and the anterior, medial, and lateral aspects of the distal femur are exposed subperiosteally. The posterior periosteum is carefully elevated to protect the neurovascular bundle in the popliteal fossa.
Distal Femoral Extension Osteotomy
- Guidewire Placement: Under fluoroscopic guidance, a reference guidewire is placed parallel to the distal femoral articular surface in the coronal plane, and perpendicular to the mechanical axis in the sagittal plane.
- Osteotomy Cuts: An anterior closing wedge osteotomy is designed in the supracondylar region. The size of the wedge corresponds to the degree of fixed knee flexion deformity. Using an oscillating saw, the proximal and distal cuts are made.
- Preserving the Posterior Hinge: It is paramount to leave the posterior cortex intact initially to act as a hinge. This prevents posterior translation of the distal fragment, which can compromise the neurovascular structures and complicate fixation.
- Deformity Correction: The wedge of bone is removed. If femoral anteversion requires correction, the posterior hinge is carefully completed, and the distal fragment is externally rotated to the desired degree (typically restoring normal anteversion of 10-15 degrees). The knee is then fully extended, closing the anterior osteotomy gap.

Patellar Tendon Advancement
To address patella alta, the extensor mechanism must be distalized.
1. Mobilization: The patellar tendon is isolated. In skeletally immature patients with open apophyses, a tibial tubercle osteotomy is contraindicated due to the risk of genu recurvatum from premature physeal closure.
2. Soft Tissue Advancement: Instead, the tendon is advanced via a soft tissue technique. The tendon is split coronally or detached with a thin sliver of periosteum.
3. Imbrication and Fixation: The patella is drawn distally into the trochlear groove (restoring an Insall-Salvati ratio of approximately 1.0). The tendon is then aggressively imbricated and sutured using heavy, non-absorbable sutures (e.g., #2 or #5 Krackow stitch) anchored through drill holes in the proximal tibia or secured with suture anchors.
Hardware Fixation and Closure
Rigid internal fixation of the osteotomy is mandatory to allow for early mobilization.
1. Implant Selection: Depending on surgeon preference and patient size, a 90-degree pediatric blade plate or a pre-contoured distal femoral locking compression plate (LCP) is utilized.
2. Application: The plate is applied to the lateral or medial aspect of the femur. If a blade plate is used, the seating chisel is driven into the distal condyles parallel to the joint line prior to completing the osteotomy. Once the wedge is closed and rotation is corrected, the plate is secured to the proximal shaft with cortical screws.
3. Validation: Fluoroscopy confirms anatomic alignment, complete closure of the osteotomy site, and appropriate hardware placement without intra-articular penetration.
4. Closure: The surgical site is copiously irrigated. A closed suction drain is often placed due to the extensive bony and soft tissue dissection. The fascial layers, subcutaneous tissue, and skin are closed meticulously.

Complications and Management
While highly effective, the complexity of DFEO and PTA in a neuromuscular population carries a distinct complication profile. Meticulous surgical technique and rigorous postoperative care are required to mitigate these risks.
Intraoperative and Postoperative Challenges
| Complication | Incidence/Risk Factors | Prevention and Salvage Management |
|---|---|---|
| Peroneal Nerve Palsy | High risk with severe, chronic flexion contractures (>20-30 degrees) due to acute stretch upon extension. | Prevention: Limit acute correction; consider prophylactic peroneal nerve decompression or gradual correction with external fixation in severe cases. Management: Ankle-foot orthosis (AFO) to prevent drop foot; most neurapraxias resolve within 3-6 months. |
| Loss of Fixation / Nonunion | Associated with poor bone stock (osteopenia), inadequate plate sizing, or non-compliance with weight-bearing restrictions. | Prevention: Use locking plates in osteopenic bone; ensure stable cortical contact at the osteotomy site. Management: Revision open reduction internal fixation (ORIF) with bone grafting. |
| Patellar Tendon Rupture | Rare but catastrophic; related to aggressive early flexion or inadequate suture technique during PTA. | Prevention: Use heavy non-absorbable sutures; rigid postoperative immobilization in extension for 4-6 weeks. Management: Immediate surgical repair and prolonged immobilization. |
| Overcorrection (Genu Recurvatum) | Excessive anterior wedge resection or iatrogenic damage to the proximal tibial physis during PTA. | Prevention: Precise preoperative templating; avoid tibial tubercle osteotomies in skeletally immature patients. Management: Orthotic management (KAFO); severe cases may require a corrective flexion osteotomy. |
| Knee Stiffness | Common due to extensive scarring, prolonged immobilization, and inherent spasticity. | Prevention: Initiate controlled range of motion (ROM) as soon as radiographic healing permits. Management: Aggressive physical therapy; manipulation under anesthesia (MUA) or arthroscopic lysis of adhesions if refractory. |

Post Operative Rehabilitation Protocols
The success of a DFEO and PTA relies heavily on a structured, multiphase rehabilitation program. The primary goals are to protect the osteotomy and tendon advancement, restore range of motion, and rebuild extensor mechanism strength.
Phased Recovery and Orthotic Management
Phase I: Protection and Healing (Weeks 0-4)
Immediately postoperatively, the knee is immobilized in full extension using a rigid cylinder cast or a locked knee immobilizer. Weight-bearing status is typically restricted to toe-touch weight-bearing (TTWB) or non-weight-bearing (NWB) to protect the patellar tendon advancement and the osteotomy site. Spasticity management is critical during this phase; pharmacological agents (e.g., diazepam, baclofen) are optimized to prevent violent muscle spasms that could compromise fixation.
Phase II: Early Mobilization (Weeks 4-8)
Upon radiographic evidence of early callus formation and clinical stability of the extensor mechanism, the rigid cast is transitioned to a hinged knee brace. Range of motion exercises are initiated, typically limiting initial flexion to 30-45 degrees and advancing gradually. Weight-bearing is progressively increased. Crucially, Ground Reaction Ankle-Foot Orthoses (GRAFOs) or solid AFOs are utilized to support the plantarflexion-knee extension couple, preventing the recurrence of tibial collapse and secondary crouch.
Phase III: Strengthening and Gait Training (Weeks 8-12+)
Once radiographic union is confirmed, immobilization is discontinued. Therapy focuses on aggressive quadriceps strengthening, hamstring stretching, and neuromuscular re-education. Aquatic therapy is highly beneficial in this phase. Intensive gait training aims to integrate the new biomechanical alignment into a functional, energy-efficient walking pattern. Patients often require 6 to 12 months of dedicated physical therapy to achieve their new baseline functional status.
Summary of Key Literature and Guidelines
The paradigm of treating crouch gait has shifted significantly over the past three decades, moving away from isolated soft-tissue lengthenings toward comprehensive bony and soft-tissue reconstructions.
Evidence Based Outcomes
Historically, isolated hamstring lengthenings were the standard of care for crouch gait. However, literature has unequivocally demonstrated that while this may temporarily reduce knee flexion, it severely weakens the hip extensors, leading to increased anterior pelvic tilt and an eventual, often more severe, recurrence of crouch.
Current clinical guidelines strongly advocate for Single-Event Multilevel Surgery (SEMLS). Seminal studies by Novacheck, Gage, and colleagues at Gillette Children's Specialty Healthcare have validated the efficacy of DFEO combined with PTA. Long-term kinematic data from these cohorts demonstrate that when the bony deformity is corrected and the extensor mechanism is restored, patients maintain significant improvements in stance phase knee extension, walking velocity, and overall energy efficiency.
Furthermore, Stout et al. highlighted that addressing patella alta concurrently with the fixed flexion deformity is non-negotiable; failure to distalize the patella results in persistent extensor lag and high rates of recurrent crouch. The integration of 3D gait analysis into preoperative planning has been shown to significantly reduce the rates of over-lengthening and under-correction, solidifying DFEO and PTA as the cornerstone interventions for the operative management of severe crouch gait in the neuromuscular population.
Clinical & Radiographic Imaging









You Might Also Like