Comprehensive Surgical Management of Idiopathic Scoliosis: Infantile, Juvenile, and Adolescent
Key Takeaway
Idiopathic scoliosis encompasses a complex spectrum of three-dimensional spinal deformities affecting infants, juveniles, and adolescents. Management requires a profound understanding of spinal biomechanics, pulmonary development, and curve progression risk factors. This comprehensive guide details evidence-based surgical strategies, including growth-sparing techniques for early-onset deformity and definitive posterior spinal fusion for adolescents, emphasizing preoperative MRI screening, meticulous surgical execution, and avoidance of the crankshaft phenomenon.
Introduction and Classification
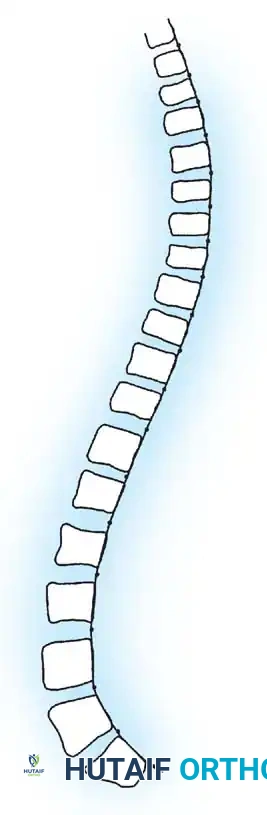
Idiopathic scoliosis is a complex, three-dimensional structural deformity of the spine characterized by lateral curvature, axial rotation, and sagittal plane alterations (typically lordosis). Historically classified by James into infantile (birth to 3 years), juvenile (4 to 10 years), and adolescent (11 years to skeletal maturity), modern nomenclature increasingly divides these into Early-Onset Scoliosis (EOS, occurring before age 10) and Late-Onset or Adolescent Idiopathic Scoliosis (AIS).
The distinction is not merely semantic; it is fundamentally rooted in pulmonary development. Alveolar multiplication occurs rapidly until age 8. Severe spinal deformity during this critical window leads to thoracic insufficiency syndrome, restrictive lung disease, and potentially fatal cor pulmonale. Consequently, the orthopedic surgeon must balance the dual imperatives of controlling spinal deformity and permitting maximal thoracic volume expansion.
Pathogenesis and Natural History
Biomechanics and Biplanar Asymmetry
The pathogenesis of idiopathic scoliosis remains multifactorial, involving genetic predisposition, connective tissue anomalies (e.g., elastic fiber pathology), and neurohormonal factors such as melatonin dysfunction. However, the biomechanical manifestation is universally characterized by biplanar asymmetry. As described by Dickson and colleagues, the primary lesion in thoracic idiopathic scoliosis is an anterior overgrowth relative to the posterior elements, creating a localized lordosis. As the spine buckles under axial load, this lordosis rotates laterally, presenting radiographically as a coronal curve.
The Crankshaft Phenomenon
First described by Dubousset, the "crankshaft phenomenon" is a critical biomechanical concept in the surgical management of immature spines (Risser 0, open triradiate cartilages). If a solid posterior spinal fusion is performed in a young child, the anterior vertebral bodies continue to grow. Tethered posteriorly, this anterior growth forces the spine to twist around the fusion mass like a crankshaft, leading to progressive rotational deformity, rib hump exacerbation, and coronal decompensation despite a solid posterior arthrodesis.
Surgical Warning: Posterior-only definitive fusion in patients with open triradiate cartilages carries a high risk of the crankshaft phenomenon. These patients require either growth-sparing instrumentation or combined anterior-posterior fusion to arrest anterior physeal growth.
Clinical Evaluation and Imaging
Radiographic Prognosticators
In infantile idiopathic scoliosis, differentiating between resolving and progressive curves is paramount. Mehta’s Rib-Vertebra Angle Difference (RVAD) is the gold standard. An RVAD greater than 20 degrees at the apical vertebra strongly predicts curve progression. Furthermore, Phase II rib-vertebra relationships (where the rib head overlaps the vertebral body) indicate an inexorable progression requiring intervention.
Indications for MRI Screening
While AIS is typically a diagnosis of exclusion, the incidence of neural axis abnormalities (e.g., syringomyelia, Arnold-Chiari malformation, tethered cord) in infantile and juvenile populations is significantly higher (up to 20%).
Routine MRI of the entire neuroaxis is mandatory in the following scenarios:
* Age of onset less than 10 years (Infantile and Juvenile).
* Atypical curve patterns (e.g., left thoracic curves).
* Rapid curve progression (>1 degree per month).
* Presence of neurologic deficits, asymmetric abdominal reflexes, or cavus foot deformity.
* Severe pain (uncommon in classic idiopathic scoliosis).
Non-Operative Management
Before considering surgical intervention, non-operative modalities must be exhausted or deemed inappropriate.
* Serial Casting: For progressive infantile curves, serial elongation-derotation-flexion (EDF) casting (Mehta casting) applied under general anesthesia can be curative or significantly delay the need for surgery.
* Bracing: Thoracolumbosacral orthoses (TLSO) or Milwaukee braces are indicated for curves between 25 and 45 degrees in growing children (Risser 0-2). Bracing alters the natural history of AIS but is less effective in juvenile curves and ineffective in curves >50 degrees.
Surgical Management of Early-Onset Scoliosis (EOS)
When conservative measures fail and curves progress beyond 50 degrees in a child under 10 years of age, surgical intervention is indicated. The goal is to control the deformity while allowing spinal and thoracic growth.
Growth-Sparing Techniques: Dual Growing Rods
The dual growing rod technique, popularized by Akbarnia, has become a workhorse for progressive EOS.
Indications:
* Progressive EOS >50 degrees.
* Age < 10 years (significant remaining spinal and thoracic growth).
* Failure of bracing or casting.
Positioning and Setup:
1. The patient is positioned prone on a pediatric Jackson frame or Relton-Hall frame.
2. All pressure points are meticulously padded.
3. Multimodality intraoperative neuromonitoring (SSEP and MEP) is mandatory.
Surgical Approach (Step-by-Step):
1. Foundation Exposure: Two limited midline incisions are made—one over the proximal foundation (upper thoracic) and one over the distal foundation (lower lumbar/pelvis). The intervening spine is left completely undisturbed to prevent spontaneous autofusion.
2. Anchor Placement:
* Proximal Foundation: Typically utilizes pedicle screws or a claw hook construct spanning 2-3 levels to distribute pull-out forces.
* Distal Foundation: Pedicle screws are placed in the lower lumbar spine or iliac/S2-alar-iliac (S2AI) screws if pelvic fixation is required.
3. Submuscular Tunneling: A specialized rod passer is used to create a submuscular, extraperiosteal tunnel connecting the proximal and distal incisions. Preserving the periosteum is critical to prevent unintended fusion.
4. Rod Insertion and Contouring: Two rods are contoured to maintain physiologic sagittal alignment (thoracic kyphosis and lumbar lordosis). They are passed through the submuscular tunnels.
5. Connection and Distraction: The rods are connected using tandem connectors (dominoes) located in the thoracolumbar region. Gentle distraction is applied to correct the coronal deformity and lengthen the spine.
6. Closure: Meticulous layered closure is performed to prevent wound dehiscence over the prominent hardware.
Clinical Pearl: Avoid over-distraction during the index procedure. The primary goal is to establish the foundation and control the curve. Over-distraction dramatically increases the risk of proximal junctional kyphosis (PJK) and anchor pull-out.
Postoperative Protocol:
Patients are typically mobilized on postoperative day 1. A custom TLSO may be used for 3-6 months to protect the construct. The patient returns every 6 months for minor outpatient surgical lengthenings until skeletal maturity is reached, at which point a definitive posterior spinal fusion is performed.
Surgical Management of Adolescent Idiopathic Scoliosis (AIS)
For adolescents with curves exceeding 45-50 degrees, definitive arthrodesis is indicated to halt progression, achieve three-dimensional correction, and restore coronal and sagittal balance.
Posterior Spinal Fusion (PSF) with Segmental Instrumentation
Modern AIS surgery relies on all-pedicle screw constructs or hybrid constructs (screws, hooks, and sublaminar wires) to provide rigid segmental fixation, allowing for powerful derotation maneuvers and eliminating the need for postoperative bracing.
Positioning:
The patient is positioned prone on an open Jackson frame. The abdomen must hang completely free to decrease intra-abdominal pressure, thereby reducing epidural venous engorgement and intraoperative blood loss.
Surgical Approach (Step-by-Step):
1. Exposure: A straight midline incision is made over the planned fusion levels. Subperiosteal dissection is carried out bilaterally to the tips of the transverse processes in the thoracic spine and the facet joints in the lumbar spine. Meticulous hemostasis is maintained using bipolar electrocautery and bone wax.
2. Facetectomies and Osteotomies:
* Inferior articulating processes are resected (Smith-Petersen or Ponte osteotomies) at the apical levels. This releases the posterior tether, increases spinal flexibility, and provides a vascularized bed for the bone graft.
3. Pedicle Screw Insertion (Freehand Technique):
* Thoracic Spine: The entry point is typically at the junction of the bisected transverse process and the superior articular facet. A gearshift probe is advanced down the pedicle, maintaining a trajectory parallel to the superior endplate and angled medially based on preoperative CT or MRI morphometry (Parent et al.).
* Lumbar Spine: The entry point is at the intersection of the pars interarticularis, the midpoint of the transverse process, and the superior articular facet.
* All tracts are palpated with a ball-tipped probe to ensure five distinct bony walls (medial, lateral, superior, inferior, and anterior).
4. Rod Contouring: Two rods (typically 5.5mm or 6.0mm titanium or cobalt-chrome) are contoured. The concave rod is contoured to the desired sagittal profile, not the existing deformity.
5. Correction Maneuvers:
* Rod Derotation: The concave rod is engaged into the screw heads and rotated 90 degrees, converting the coronal curve into thoracic kyphosis.
* Direct Vertebral Rotation (DVR): Derotation tubes are attached to the apical pedicle screws, and direct force is applied to derotate the vertebral bodies, correcting the rib hump.
* Compression/Distraction: Applied segmentally to level the end vertebrae and fine-tune the coronal and sagittal balance.
6. Decortication and Bone Grafting: The posterior elements (laminae, transverse processes) are aggressively decorticated using a high-speed burr. Autograft (from local bone spinous processes and facetectomies) and allograft are packed tightly over the decorticated surfaces to ensure a robust arthrodesis.
7. Closure: A deep subfascial drain may be placed. The fascia is closed in a watertight fashion, followed by layered closure of the subcutaneous tissue and skin.
Anterior Spinal Fusion (ASF)
While largely supplanted by all-posterior pedicle screw constructs, anterior spinal fusion remains indicated for specific curve patterns, particularly isolated thoracolumbar or lumbar curves (Lenke Type 5).
Advantages of ASF:
* Saves distal fusion levels (often stopping at L3 instead of L4).
* Provides powerful derotation of the lumbar spine.
* Directly addresses the anterior overgrowth.
Technique Overview:
Performed via a retroperitoneal approach or thoracophrenolumbotomy. Segmental vessels are ligated. Complete anterior discectomies are performed back to the posterior longitudinal ligament. Structural grafts (rib autograft or cages) are placed in the disc spaces, and a single or dual rod construct is applied to the lateral aspect of the vertebral bodies, applying compression to correct the coronal curve and induce lordosis.
Complications and Avoidance
- Neurologic Injury: The most devastating complication. Risk is mitigated by mandatory multimodality neuromonitoring (SSEP/MEP). If signals drop during correction, the surgeon must immediately release the correction, increase mean arterial pressure (MAP > 85 mmHg), and rule out technical errors (e.g., medial pedicle screw breach).
- Proximal Junctional Kyphosis (PJK): Occurs when the spine kyphoses acutely above the uppermost instrumented vertebra (UIV). Prevented by avoiding over-dissection of the proximal facet capsules, utilizing transition rods, and ensuring appropriate sagittal balance.
- Pseudoarthrosis and Implant Failure: Rare with modern rigid fixation but can occur in non-compliant patients or those with metabolic bone disease. Meticulous decortication and copious bone grafting are the best prevention.
- Infection: Deep surgical site infections require prompt aggressive irrigation and debridement. Implants are generally retained if the fusion mass is not yet solid, provided the infection can be suppressed with targeted intravenous antibiotics.
Postoperative Protocol and Rehabilitation
- Immediate Postoperative Phase: Patients are extubated in the operating room. Pain is managed via multimodal analgesia (PCA, epidural, or intrathecal morphine, combined with NSAIDs and muscle relaxants).
- Mobilization: Early mobilization is critical. Patients are typically out of bed with physical therapy on postoperative day 1.
- Bracing: With modern segmental pedicle screw fixation, postoperative bracing is generally unnecessary for AIS.
- Return to Activity:
- 2-4 weeks: Return to school.
- 3 months: Light non-contact activities (swimming, stationary biking).
- 6 months: Return to non-contact sports.
- 12 months: Radiographic evaluation of fusion mass. If solid, clearance for all activities, including contact sports, is typically granted, though high-impact collision sports may be restricted depending on the distal extent of the fusion.
Conclusion
The surgical management of idiopathic scoliosis demands a rigorous understanding of spinal biomechanics, meticulous preoperative planning, and precise surgical execution. Whether employing growth-sparing techniques to preserve pulmonary function in the infantile patient or executing a complex three-dimensional derotation via posterior spinal fusion in the adolescent, the orthopedic surgeon's goal remains constant: to achieve a balanced, stable, and painless spine while minimizing neurologic risk and maximizing the patient's long-term quality of life.
📚 Medical References
- idiopathic scoliosis surgery: a multivariate statistical analysis, J Pediatr Orthop 11:465, 1991.
- Farey ID, McAfee PC, Davis RF, et al: Pseudarthrosis of the cervical spine after anterior arthrodesis: treatment by posterior nerve-root decompression, stabilization, and arthrodesis, J Bone Joint Surg 72A:1171, 1990.
- Feiertag MA, Boden SD, Schimandle JH, et al: A rabbit model for nonunion of lumbar intertransverse process spine arthrodesis, Spine 21:27, 1996.
- Fielding JW, Lusskin R, Batista A: Multiple segment anterior cervical spinal fusion, Clin Orthop Relat Res 54:29, 1967.
- Flynn JC, Hoque A: Anterior fusion of the lumbar spine: endresult study with long-term follow-up, J Bone Joint Surg 61A:1143, 1979.
- Freebody D, Bendall R, Taylor RD: Anterior transperitoneal lumbar fusion, J Bone Joint Surg 53B:617, 1971.
- Frempong-Boadu A, Houten JK, Osborn B, et al: Swallowing and speech dysfunction in patients undergoing anterior cervical discectomy and fusion, J Spinal Disord 15:362, 2002.
- Friedlaender GE: Current concepts review: bone grafts, J Bone Joint Surg 69A:786, 1987.
- Fujimake A, Crock HV, Bedbrook GM: The results of 150 anterior lumbar interbody fusion operations performed by two surgeons in Australia, Clin Orthop Relat Res 165:164, 1982.
- Gill K, O’Brien JP: Observations of resorption of the posterior lateral bone graft in combined anterior and posterior lumbar fusion, Spine 18:1885, 1993.
- Glassman SD, Anagnost SC, Parker A, et al: The effect of cigarette smoking and smoking cessation on spinal fusion, Spine 25:2608, 2000.
- Goldner JL, Urbaniak JR, McCollum DE: Anterior disc excision and interbody spinal fusion for chronic low back pain, Orthop Clin North Am 2:543, 1971.
- Grob D, Scheier HJG, Dvorak J, et al: Circumferential fusion of the lumbar and lumbosacral spine, Arch Orthop Trauma Surg 111:20, 1991.
- Hibbs RA: An operation for progressive spinal deformities, N Y Med J 93:1013, 1911.
- Hibbs RA, Risser JC: Treatment of vertebral tuberculosis by the spine fusion operation: a report of 286 cases, J Bone Joint Surg 10:805, 1928.
- Hilibrand AS, Fye MA, Emery SE, et al: Impact of smoking on the outcome of
You Might Also Like