Posterolateral Approach to the Thoracic Spine: A Comprehensive Surgical & Anatomical Guide
Key Takeaway
The posterolateral approach to the thoracic spine (costotransversectomy) provides critical access to the anterolateral vertebral column, minimizing open chest morbidity. It's ideal for treating spinal infections, tumors, trauma (burst fractures), and limited anterior fusions, particularly in patients with high risks for major intrathoracic surgery, balancing anterior access with reduced physiological insult.
Posterolateral Approach to the Thoracic Spine: When It's Best
Introduction & Epidemiology
The posterolateral approach to the thoracic spine, often synonymous with costotransversectomy, represents a critical surgical corridor facilitating access to the anterolateral aspect of the vertebral column without requiring a formal transthoracic thoracotomy. Historically, this approach gained prominence in the early 20th century, primarily developed for the drainage of tuberculous abscesses (Pott's disease) involving the thoracic vertebrae, a prevalent and debilitating condition at the time. Its primary advantage lay in its ability to address anterior column pathology while minimizing the significant morbidity associated with open chest cavity procedures of that era.
In contemporary spine surgery, the posterolateral approach maintains a vital role, although its indications have evolved considerably. While less extensive than a full thoracotomy and offering a comparatively more limited exposure, it strikes a balance between direct anterior access and the reduced physiological insult associated with purely posterior approaches. This makes it particularly suitable for select pathologies, especially in patients who may be at elevated risk for major intrathoracic surgery due to significant pulmonary compromise, severe pre-existing pleural adhesions, or other systemic comorbidities.
Epidemiologically, conditions necessitating a posterolateral approach include a diverse spectrum of thoracic spinal pathologies. Spinal infections, whether pyogenic or granulomatous, continue to be a significant indication, particularly for abscess drainage and debridement. Primary and metastatic spinal tumors affecting the vertebral body, requiring debulking or partial resection for neural decompression and stabilization, frequently benefit from this corridor. Trauma, especially burst fractures with retropulsed bone fragments causing anterior spinal cord compression, can be effectively managed. Furthermore, limited anterior spinal fusion, correction of post-traumatic kyphosis, or situations requiring vertebral body biopsy where a posterior approach is insufficient and a full thoracotomy is deemed excessive or contraindicated, fall within its utility. The ability to combine a posterolateral approach with a standard posterior spinal fixation procedure allows for comprehensive, circumferential decompression and stabilization in a single setting, addressing both anterior and posterior column pathology.
Surgical Anatomy & Biomechanics
A thorough understanding of the regional anatomy is paramount for safe and effective execution of the posterolateral approach.
Skeletal Anatomy
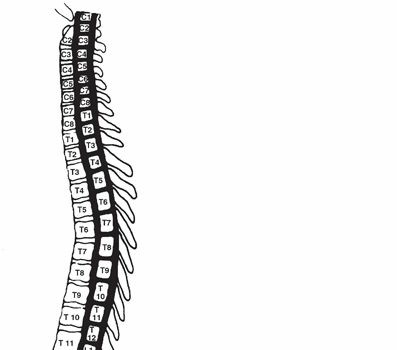
The thoracic spine comprises twelve vertebrae (T1-T12), characterized by their articulation with the ribs. Each typical thoracic vertebra features a vertebral body, pedicles, laminae, spinous process, and transverse processes. Crucially, the transverse processes possess facets for articulation with the tubercles of the ribs (costotransverse joints), while the vertebral bodies bear facets for the heads of the ribs (costovertebral joints). The posterolateral approach exploits the anatomical window created by the resection of a rib segment and its associated costotransverse joint, providing direct access to the posterolateral aspect of the vertebral body and the ipsilateral pedicle.
Muscular Anatomy
The surgical dissection traverses several muscle layers:
*
Superficial Layer
: Trapezius and Latissimus Dorsi. These are typically reflected or split along their fibers.
*
Intermediate Layer
: Rhomboid Major and Minor. These muscles are encountered deep to the trapezius and are typically elevated subperiosteally.
*
Deep Layer (Erector Spinae Group)
: This substantial muscle mass, composed of the Iliocostalis, Longissimus, and Spinalis muscles, lies deep to the rhomboids. For a posterolateral approach, these muscles are meticulously subperiosteally elevated off the spinous processes, laminae, and transverse processes to expose the underlying osseous structures.
*
Deepest Layer
: Intercostal muscles (external, internal, innermost) lie between the ribs. The serratus posterior superior and inferior muscles may also be encountered depending on the level and extent of the approach.
Neurovascular Structures
- Spinal Cord and Nerves : The spinal cord resides within the vertebral canal. Segmental spinal nerves exit through the intervertebral foramina. The intercostal nerves, which are the ventral rami of the thoracic spinal nerves, run inferior to each rib along with the intercostal artery and vein (VAN: Vein-Artery-Nerve, superior to inferior within the costal groove). Careful identification and protection of these neurovascular bundles are essential during rib resection and pleural manipulation.
- Segmental Arteries : Each thoracic level has a pair of segmental arteries arising directly from the aorta. These vessels pass around the vertebral body, deep to the pleura, and give off branches to the spinal canal. The Great Radicular Artery (Artery of Adamkiewicz), typically arising from a left-sided segmental artery between T9 and T12 (though its origin can vary from T5 to L5), is the major blood supply to the lower two-thirds of the spinal cord. Damage to this artery can result in devastating spinal cord ischemia and paraplegia. Meticulous identification, preservation, or judicious ligation distal to its origin is crucial.
- Sympathetic Chain : The thoracic sympathetic trunk lies on the heads of the ribs and the sides of the vertebral bodies, medial to the intercostal vessels. It must be carefully retracted or dissected to avoid injury.
- Pleura : The parietal pleura lines the thoracic cavity. It is immediately anterior to the vertebral bodies and medial to the ribs and intercostal spaces. While the posterolateral approach aims to avoid entering the thoracic cavity, the pleura is intimately encountered and must be carefully dissected and retracted anteriorly. Inadvertent breach is a recognized complication requiring prompt repair.
Biomechanics
The thoracic spine derives significant stability from its inherent kyphosis, the rib cage attachments, and its strong ligamentous structures. The posterolateral approach, by resecting a transverse process, rib head, and potentially parts of the pedicle and vertebral body, can compromise the anterior and middle columns of the spine (Denis classification). Therefore, when used for decompression or tumor resection, it frequently necessitates anterior column reconstruction (e.g., with a cage or structural graft) and often requires supplementary posterior instrumentation (pedicle screws) to restore global spinal stability and promote fusion. Failure to restore adequate stability can lead to progressive deformity, hardware failure, or pseudarthrosis.
Indications & Contraindications
The selection of the posterolateral approach is contingent upon a precise understanding of the spinal pathology, patient comorbidities, and the specific surgical goals.
Indications
-
Spinal Infections
:
- Drainage and debridement of epidural or prevertebral abscesses (e.g., tuberculous spondylodiscitis, pyogenic infections).
- Vertebral osteomyelitis with anterior column destruction and associated instability.
-
Spinal Tumors
:
- Biopsy of vertebral body lesions (primary or metastatic).
- Debulking or partial vertebral body resection for spinal cord decompression in cases of metastatic disease or primary tumors not amenable to complete en bloc resection via this approach.
- Restoration of anterior column support following tumor resection.
-
Spinal Trauma
:
- Decompression of the spinal cord in burst fractures with retropulsed bone fragments into the canal, especially when the anterior column is significantly compromised.
- Limited anterior column reconstruction for specific fracture patterns.
-
Anterolateral Decompression
:
- Relief of neural compression from conditions such as severe disc herniations or ossification of the posterior longitudinal ligament (OPLL) that require access beyond a pure posterior corridor.
-
Limited Anterior Spinal Fusion
:
- For specific cases of instability, deformity, or pseudarthrosis where limited anterior column support or fusion is required.
-
High-Risk Patients
:
- Patients with significant pulmonary dysfunction, severe pleural adhesions from previous thoracotomy or infection, or other medical comorbidities precluding a formal transthoracic approach.
-
Adjunctive to Posterior Fixation
:
- Often combined with a posterior pedicle screw instrumentation procedure in a single setting to achieve circumferential decompression and stabilization.
Contraindications
-
Extensive Anterior Column Pathology
:
- Lesions requiring wide, bilateral exposure of the anterior vertebral bodies or major vascular structures (aorta, vena cava) that cannot be safely managed through a limited posterolateral window.
-
Severe Spinal Deformity
:
- Complex kyphoscoliosis requiring comprehensive vertebral column resection or extensive osteotomies, which are typically better addressed via direct anterior (thoracotomy/laparotomy) or combined posterior approaches.
-
Major Vascular Involvement
:
- Tumors or infections directly invading or extensively encasing the aorta or vena cava where direct visualization and proximal/distal control are critical.
-
Significant Uncontrolled Coagulopathy
:
- Increased risk of bleeding in a relatively confined space.
-
Prior Extensive Posterior Surgery
:
- Severe scarring and anatomical distortion from previous posterior approaches may complicate dissection and increase the risk of iatrogenic injury.
-
Pathology Beyond Reach
:
- Lesions located too far anteriorly or contralaterally to be safely or adequately accessed through the limited posterolateral corridor.
Operative vs. Non-Operative Indications
| Condition | Indication for Posterolateral Approach | Indication for Other Approaches / Non-operative Management |
|---|---|---|
| Spinal Infection (e.g., Abscess) | Epidural or prevertebral abscess with neurological deficit, severe pain, instability, or failure of medical management; vertebral destruction. | Small, contained abscesses without neurological compromise, stable spine, responsive to antibiotics; diffuse spondylodiscitis without significant collapse or neurological involvement (consider medical management, percutaneous drainage). |
| Metastatic Spinal Tumor | Anterior cord compression with neurological deficit, intractable pain, impending fracture, or instability (especially in high-risk patients). | Asymptomatic lesions, stable spine, diffuse bone metastases without neurological compromise (consider radiation, chemotherapy, watchful waiting); lesions requiring wide en bloc resection (consider anterior or combined approaches); purely posterior compression (posterior laminectomy/decompression). |
| Thoracic Burst Fracture | Significant anterior cord compression from retropulsed fragments, progressive kyphosis, neurological deficit, or severe instability (Denis B/C). | Stable fractures (Denis A), minimal or no neurological deficit, no significant canal compromise, no progressive deformity (consider bracing, activity modification); fractures requiring extensive anterior column reconstruction (consider thoracotomy or mini-open anterior). |
| Vertebral Body Biopsy | Need for tissue diagnosis of a vertebral body lesion when posterior approach is insufficient and percutaneous biopsy is inconclusive or unsafe. | Easily accessible posterior element lesions (posterior biopsy); successful percutaneous CT-guided biopsy; lesions requiring open biopsy but better accessed anteriorly or with less invasive techniques. |
| Limited Anterior Spinal Fusion | Focal anterior column defect or pseudarthrosis requiring direct graft placement and stabilization in conjunction with posterior fixation. | Extensive multi-level anterior column reconstruction (thoracotomy); purely posterior pathology (posterior fusion); non-operative management for stable pseudarthrosis without symptoms. |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning and precise patient positioning are fundamental to the success and safety of the posterolateral approach.
Pre-Operative Planning
-
Imaging Review
:
- Computed Tomography (CT) : Essential for delineating bony anatomy, assessing vertebral body destruction, cortical breaches, and the extent of canal compromise. CT angiography may be helpful to identify segmental vessel anatomy, especially the Artery of Adamkiewicz.
- Magnetic Resonance Imaging (MRI) : Crucial for visualizing soft tissue pathology (e.g., epidural abscess, tumor extension, disc herniation), spinal cord compression, and intrinsic cord signal changes.
- Plain Radiographs : Evaluate overall spinal alignment, kyphosis, and potential instability.
-
Medical Optimization
:
- Cardiopulmonary Assessment : Detailed evaluation of pulmonary function (PFTs) is critical, particularly in patients for whom this approach is chosen due to pulmonary compromise. Optimize respiratory status pre-operatively.
- Nutritional Status : Important for wound healing, especially in patients with chronic infections or malignancy.
- Coagulation Profile : Address any coagulopathies.
-
Surgical Strategy
:
- Level Identification : Accurately identify the target vertebral level(s) using pre-operative imaging. Intraoperative fluoroscopy will be used for confirmation.
- Extent of Resection : Determine the precise amount of rib, transverse process, pedicle, and vertebral body to be resected.
- Decompression Goals : Define the extent of neural decompression required (e.g., anterior epidural, circumferential).
- Reconstruction Plan : Select appropriate anterior column reconstruction (e.g., titanium cage, allograft, autograft) and plan for posterior instrumentation if combined.
- Blood Management : Anticipate potential blood loss and arrange for cell saver, pre-donated blood, or cross-matched units.
- Neuromonitoring : Strongly consider intraoperative somatosensory evoked potentials (SSEPs) and motor evoked potentials (MEPs) for spinal cord protection, especially during decompression near the cord.
Patient Positioning
The patient is typically positioned prone on the operating table.
1.
Supports
: Use chest rolls or gel bolsters placed longitudinally on each side of the rib cage, extending from the clavicle to the iliac crest. This allows the abdomen to hang freely, reducing intra-abdominal pressure, minimizing epidural venous bleeding, and facilitating chest expansion for respiration.

2.
Head Position
: Securely position the head in a neutral position with adequate padding, often in a Mayfield head holder if cervical spine pathology is also addressed or if neuromonitoring electrodes are applied to the scalp.
3.
Extremities
: Arms can be positioned either abducted on arm boards (less than 90 degrees to avoid brachial plexus stretch) or adducted along the torso, depending on the surgeon's preference and the need for C-arm access. Ensure proper padding of elbows, knees, and ankles to prevent nerve compression or pressure sores.

4.
C-arm Access
: Verify unobstructed C-arm access for intraoperative fluoroscopy in both anteroposterior and lateral planes to confirm the surgical level and guide instrumentation.
5.
Draping
: Drape widely over the entire rib cage area, extending from the midline posteriorly to well into the lateral thorax, and sufficiently superior and inferior to encompass potential incision extensions. This allows for potential lateral extension of the incision if broader access is unexpectedly required.

Landmarks and Incision
- Palpation : Palpate the spinous processes in the target area. The inferior angle of the scapula typically overlies the T7 spinous process.
- Pre-operative Localization : Use fluoroscopy or X-ray to confirm the target vertebral level and mark the skin. Inject methylene blue or use a needle to localize the level precisely, correlating with anatomical landmarks.
- Incision : A standard midline or paramedian incision is made, centered over the spinous process corresponding to the vertebral body requiring access. The length of the incision depends on the number of levels to be addressed and whether concomitant posterior instrumentation is planned. For a single-level costotransversectomy, a paramedian incision typically starts one level above and extends one level below the target pathology. Alternatively, a hockey-stick incision can be employed, extending laterally from the midline at the target level.
Detailed Surgical Approach / Technique
The posterolateral approach involves a systematic, layered dissection to reach the anterolateral aspect of the thoracic vertebral body.
1. Incision and Initial Exposure
- Skin Incision : Make a paramedian incision approximately 3-4 cm lateral to the midline on the side of the pathology. This allows direct access to the transverse process and rib head with less muscle retraction. Alternatively, a midline incision can be made, followed by subperiosteal elevation of the paraspinal musculature to the desired lateral extent.
- Subcutaneous Tissue and Fascia : Incise the subcutaneous tissue down to the thoracolumbar fascia. Identify and incise the fascia.
-
Muscle Dissection
: Subperiosteally dissect the paraspinal muscles (erector spinae group) from the spinous processes, laminae, and transverse processes. This dissection should extend laterally to expose the transverse process and the rib corresponding to the target vertebral level. The dissection proceeds just lateral to the facet joints. Ensure complete elevation of muscle attachments to allow for proper visualization.

2. Costotransversectomy
- Identify Target Rib and Transverse Process : Confirm the correct level using intraoperative fluoroscopy. The rib articulating with the target vertebral body is typically resected. For example, to access the T8 vertebral body, the T8 rib (which articulates with T7 and T8 vertebral bodies) and the T8 transverse process are typically targeted.
- Resection of Transverse Process : Use an osteotome or Leksell rongeur to resect the transverse process at its base.
- Disarticulation of Costotransverse Joint : Carefully disarticulate the rib from the inferior border of the transverse process and the adjacent vertebral body. This exposes the costo-transverse ligament and costo-vertebral ligament.
-
Rib Resection
: Resect approximately 3-5 cm of the rib segment just lateral to the costotransverse joint and extending anteriorly. This creates the primary working window. Use a rib cutter, being mindful of the underlying intercostal neurovascular bundle and pleura. The rib head will be the final portion removed.

3. Access to Vertebral Body and Decompression
- Pleural Management : After rib resection, the pleura becomes visible. It is usually adherent to the vertebral body. Carefully dissect the pleura anteriorly and medially from the lateral aspect of the vertebral body and pedicle using blunt dissection (e.g., peanut sponges or blunt elevators). The goal is to retract the pleura without violating it. If the pleura is inadvertently torn, it should be immediately repaired with fine non-absorbable sutures and tested for air leak at the end of the procedure.
- Identify Segmental Vessels : The segmental artery and vein typically pass over the waist of the vertebral body, deep to the pleura, supplying the spinal canal. These may need to be ligated or cauterized if they obstruct the surgical field, but extreme caution is required due to the potential presence of the Artery of Adamkiewicz. If identified, the artery of Adamkiewicz must be meticulously protected. Ligation should only occur distal to its origin, if absolutely necessary, and only after confirming no alternative major supply exists.
-
Pediculectomy
: For broader anterior access to the vertebral body and spinal canal, the pedicle ipsilateral to the approach is resected using osteotomes or high-speed burrs. This directly exposes the posterolateral aspect of the vertebral body and the dura mater.
 - Vertebral Body Resection/Decompression : With the pedicle removed, the spinal cord and anterior dura are visible. Using a high-speed burr, Kerrison rongeurs, and curettes, remove the pathological tissue (e.g., tumor, infection, retropulsed bone fragments) from the vertebral body. The goal is to decompress the spinal cord effectively. Ensure precise removal, often using neuromonitoring feedback, to avoid cord injury. The posterior longitudinal ligament can be carefully resected if necessary.
- Anterior Column Reconstruction : Once decompression is complete, if significant vertebral body loss has occurred, anterior column support is essential. A structural graft (e.g., titanium cage packed with autograft or allograft, fibula strut graft) is typically impacted into the created defect to restore height and stability. The anterior cortical endplates of the adjacent vertebrae must be prepared to receive the graft.
4. Posterior Stabilization (if combined)
- If combined with posterior fixation, pedicle screws are placed at the levels above and below the pathology, and rods are contoured and secured to provide immediate stability. This is often performed concurrently with the posterolateral approach.
5. Closure
- Hemostasis : Achieve meticulous hemostasis throughout the surgical field.
- Dural Repair : If a dural tear occurred, it should be primarily repaired using fine sutures (e.g., 6-0 Prolene) with or without an onlay graft (e.g., fascia, allograft dura) and sealed with fibrin glue.
- Pleural Repair : If the pleura was entered, repair it with running absorbable sutures and perform a Valsalva maneuver to check for air leaks. A chest tube may be inserted prophylactically, especially if the breach was large or difficult to seal.
- Drainage : A deep suction drain (e.g., Jackson-Pratt) is often placed to manage potential post-operative bleeding or fluid collections.
- Layered Closure : Reapproximate the paraspinal muscles, fascia, subcutaneous tissues, and skin in layers.
Complications & Management
Despite its advantages, the posterolateral approach to the thoracic spine is associated with a specific set of potential complications that require diligent intraoperative prevention and prompt postoperative management.
| Complication | Incidence (Approximate) | Salvage Strategies / Management ## The Posterolateral Approach to the Thoracic Spine: A Comprehensive Review
Introduction & Epidemiology
The posterolateral approach to the thoracic spine, often referred to as a costotransversectomy or an extracavitary approach, represents a versatile and widely utilized surgical corridor in spine surgery. Its origins can be traced back to the early 20th century, notably pioneered by Capener in 1934 and later refined by Hodgson, particularly for the drainage and debridement of tuberculous abscesses (Pott's disease) in the thoracic region. This historical context underscored its distinct advantage: enabling direct access to the anterior and anterolateral aspects of the vertebral body while circumventing the morbidity associated with a formal transthoracic thoracotomy.
In contemporary orthopedic and neurosurgical practice, the posterolateral approach has transcended its initial infectious disease indications. It occupies a critical niche, offering a balanced compromise between the extensive exposure of a formal thoracotomy and the limitations of purely posterior approaches. While it provides less comprehensive visualization of the anterior column than a direct transthoracic route, it grants sufficient access for targeted pathologies, particularly in patients deemed high-risk for intrathoracic interventions due to pre-existing pulmonary dysfunction, severe pleural adhesions, or significant cardiac comorbidities. Furthermore, the ability to integrate this anterior column access with a posterior spinal fixation procedure in a single operative setting allows for truly circumferential decompression and robust stabilization.
Epidemiologically, the conditions managed via this approach are diverse. Spinal infections, both pyogenic and granulomatous (e.g., Staphylococcus aureus , tuberculosis), remain a significant indication, especially when involving epidural or prevertebral abscesses and bony destruction leading to instability or neurological compromise. The rising incidence of spinal metastatic disease, often presenting with vertebral body destruction and concomitant spinal cord compression, frequently dictates the use of a posterolateral approach for tumor debulking, decompression, and anterior column reconstruction. Thoracic burst fractures with retropulsed fragments causing anterior canal compromise, and select cases of post-traumatic kyphosis requiring limited anterior column grafting, also fall within its purview. Rarer indications include vertebral body biopsy for undiagnosed lesions, removal of severe disc herniations or ossified posterior longitudinal ligament (OPLL) causing anterolateral cord compression, and limited anterior fusions for degenerative or post-laminectomy instability.
Surgical Anatomy & Biomechanics
A profound understanding of the complex regional anatomy is indispensable for the safe and effective execution of the posterolateral approach.
Skeletal Anatomy
The typical thoracic vertebra comprises a body, pedicles, laminae, transverse processes, and a spinous process. Key anatomical features for this approach include:
*
Costovertebral Joints
: Articulations between the heads of the ribs and the vertebral bodies/intervertebral discs.
*
Costotransverse Joints
: Articulations between the tubercles of the ribs and the transverse processes.
The posterolateral approach primarily targets the resection of a segment of the rib and its associated costotransverse joint, often extending to the pedicle and posterolateral vertebral body. This creates a direct corridor to the anterior column pathology. The vertebral body itself serves as the primary target for decompression, resection, or fusion.
Muscular Anatomy
The surgical dissection through the posterior musculature is layered:
1.
Skin and Subcutaneous Tissue
: Initial incision.
2.
Thoracolumbar Fascia
: Incised to expose the superficial muscle layers.
3.
Superficial Muscles
: Trapezius and Latissimus Dorsi. These are typically retracted or partially incised.
4.
Intermediate Muscles
: Rhomboid Major and Minor. These muscles are encountered deep to the trapezius and are subperiosteally elevated from the spinous processes and laminae.
5.
Deep Muscles (Erector Spinae Group)
: Comprising the Iliocostalis, Longissimus, and Spinalis muscles, this substantial muscle mass is meticulously elevated subperiosteally from the spinous processes, laminae, and transverse processes. The extent of lateral dissection is critical for adequate exposure of the target rib and transverse process.
6.
Deepest Muscles
: Intercostal muscles (external, internal, innermost) lie between adjacent ribs. During rib resection, these muscles are incised with care to avoid pleural injury. The serratus posterior superior and inferior muscles may also be encountered and require elevation or incision depending on the level and trajectory.
Neurovascular Structures
The high-risk nature of the thoracic spine necessitates meticulous attention to crucial neurovascular structures:
*
Spinal Cord and Nerves
: The spinal cord occupies the vertebral canal. Segmental spinal nerves emerge through the intervertebral foramina. The intercostal nerves, ventral rami of the thoracic spinal nerves, course inferior to each rib within the costal groove, accompanied by the intercostal artery and vein (VAN: Vein-Artery-Nerve, from superior to inferior). Protection of these bundles is paramount during rib resection and pleura retraction.
*
Segmental Arteries and Veins
: Each thoracic level receives paired segmental arteries directly from the aorta and veins draining into the azygos/hemiazygos systems. These vessels course around the vertebral bodies, deep to the pleura, supplying both the vertebral body and the spinal canal. The
Great Radicular Artery of Adamkiewicz
is the dominant blood supply to the lower two-thirds of the spinal cord. It typically originates from a left-sided segmental artery between T9 and T12, though anatomical variations are common (T5-L5). Identification and preservation of this artery are critical. Ligation of segmental vessels should be performed judiciously and only after confirming the absence of a major radicular artery at that level. Pre-operative CT angiography can be invaluable.
*
Sympathetic Chain
: The thoracic sympathetic trunk lies on the heads of the ribs and the sides of the vertebral bodies, medial to the intercostal vessels. It must be carefully identified and retracted to prevent injury, which could lead to Horner's syndrome (if superior thoracic levels) or other autonomic dysregulation.
*
Pleura
: The parietal pleura forms the innermost lining of the thoracic cavity and is intimately related to the anterolateral aspect of the vertebral bodies and ribs. While the posterolateral approach aims to avoid pleural entry, it is consistently encountered and meticulously dissected and retracted anteriorly. Inadvertent breach is a well-recognized complication.
Biomechanics
The thoracic spine's inherent kyphosis, combined with the rigidity provided by the rib cage and strong ligamentous structures, contributes significantly to its stability. The posterolateral approach, by definition, involves resection of posterolateral bony elements (transverse process, rib head) and potentially portions of the pedicle and vertebral body. This compromises the integrity of the anterior and middle columns (Denis' three-column model). Therefore, for most indications involving decompression or tumor removal, the procedure mandates anterior column reconstruction (e.g., with structural grafts or cages) and almost invariably requires supplementary posterior instrumentation (pedicle screws) to restore immediate global spinal stability, prevent progressive deformity, and facilitate successful arthrodesis. Failure to address spinal stability adequately can result in progressive kyphosis, implant failure, pseudarthrosis, and persistent pain or neurological deficits.
Indications & Contraindications
The judicious selection of the posterolateral approach hinges on a precise definition of the spinal pathology, meticulous assessment of patient comorbidities, and clear surgical objectives.
Indications
-
Spinal Infections
:
- Abscess Drainage and Debridement : Most commonly for epidural or prevertebral abscesses (e.g., tuberculous spondylodiscitis, pyogenic vertebral osteomyelitis) causing spinal cord compression or intractable pain, especially when medical management fails or neurological deficits are present.
- Vertebral Debridement : Resection of infected or necrotic bone, often accompanied by anterior column reconstruction and fusion.
-
Spinal Tumors
:
- Biopsy : Open biopsy of vertebral body lesions (primary or metastatic) when percutaneous techniques are inconclusive or unsafe.
- Debulking and Decompression : Partial vertebral body resection for spinal cord decompression in cases of primary or metastatic tumors, particularly to alleviate neurological deficits or intractable pain.
- Anterior Column Reconstruction : Post-resection for stabilization.
-
Spinal Trauma
:
- Spinal Cord Decompression : Resection of retropulsed bone fragments in thoracic burst fractures (e.g., Type B3/C fractures) causing significant anterior spinal cord compression and neurological compromise.
- Limited Anterior Column Reconstruction : To restore height and stability after fracture reduction and decompression.
-
Anterolateral Decompression
:
- Relief of neural compression from severe, calcified thoracic disc herniations or ossification of the posterior longitudinal ligament (OPLL) that extend beyond the reach of a purely posterior approach.
-
Limited Anterior Spinal Fusion
:
- For specific cases of post-traumatic kyphosis, pseudarthrosis, or instability requiring focal anterior column support or fusion in conjunction with posterior instrumentation.
-
High-Risk Patients
:
- Individuals with severe pulmonary compromise, extensive previous intrathoracic surgery leading to prohibitive pleural adhesions, or significant cardiac comorbidities that contraindicate a formal transthoracic thoracotomy.
-
Combined Approach for Circumferential Pathology
:
- When both anterior column pathology (requiring decompression/reconstruction) and posterior column pathology (requiring extensive laminectomy or instrumentation) are present, enabling a single-position, single-stage procedure.
Contraindications
- Extensive Anterior Column Pathology : Lesions requiring wide, bilateral anterior vertebral body exposure (e.g., aggressive tumors crossing the midline, pan-vertebral body destruction) or extensive major vascular dissection (aorta, vena cava) that cannot be safely achieved through a limited posterolateral window.
- Severe Global Spinal Deformity : Complex kyphoscoliosis requiring multi-level vertebral column resection or extensive corrective osteotomies, which are often better addressed via direct anterior (thoracotomy/laparotomy) or combined posterior approaches.
- Major Vascular Involvement : Tumors or infections directly invading or extensively encasing major vessels (aorta, superior vena cava) where direct visualization and proximal/distal control are paramount.
- Significant Uncontrolled Coagulopathy : The confined nature of the posterior-lateral corridor increases the risk of uncontrolled bleeding.
- Prior Extensive Posterior Surgery : Severe scarring, anatomical distortion, or instrumentation from previous posterior procedures may significantly complicate dissection, increase operative time, and heighten the risk of iatrogenic injury.
- Pathology Beyond Reach : Lesions that are situated too far anteriorly, contralaterally, or involve multiple contiguous vertebral segments beyond the effective working range of a single-level posterolateral window.
- Poor Bone Quality : Severe osteoporosis may complicate instrumentation and graft placement, though this is often a relative contraindication if meticulously planned.
Operative vs. Non-Operative Indications Table
| Condition | Indication for Posterolateral Approach (Operative) | Indication for Other Approaches / Non-operative Management |
|
Spinal Cord Compression
| Manifesting neurological deficits (weakness, numbness, bowel/bladder dysfunction) secondary to acute trauma, tumor, or infection; rapidly progressive symptoms. | Asymptomatic compression, stable neurological status, slow progression without significant functional impact (consider observation, medical management, radiation therapy for tumors, bracing for stable fractures). |
|
Spinal Instability
| Traumatic instability (e.g., severe burst fractures), tumor-related instability with impending collapse or pain, progressive deformity (e.g., kyphosis), or symptomatic pseudarthrosis not amenable to conservative care. | Stable fractures, asymptomatic degenerative changes, stable post-operative constructs (consider conservative care, bracing, activity modification); instability that can be sufficiently addressed via purely posterior instrumentation for select pathologies. |
|
Intractable Pain
| Severe, unremitting pain secondary to mechanical instability, pathological fracture, or tumor invasion that is refractory to maximal conservative measures (analgesics, nerve blocks, physical therapy). | Mild to moderate pain responsive to analgesics, physical therapy, spinal injections; pain related to diffuse metastatic disease without focal structural compromise (consider systemic therapy, radiation). |
|
Abscess Drainage (Vertebral)
| Deep-seated vertebral or epidural abscess requiring surgical debridement and drainage, especially with bone destruction, sepsis, or neurological compromise. | Small, contained abscesses responsive to intravenous antibiotics, percutaneous drainage (if accessible and safe), no significant bone destruction, no neurological deficit, patient able to tolerate prolonged antibiotic therapy. |
|
Vertebral Body Mass for Biopsy
| Suspicious vertebral body lesion requiring tissue diagnosis when percutaneous biopsy is inconclusive, contraindicated, or unsafe due to location or proximity to vital structures. | Lesions amenable to safe and effective percutaneous CT-guided or fluoroscopy-guided biopsy; purely posterior element lesions accessible by open posterior biopsy; lesions that are unequivocally benign on imaging. |
Pre-Operative Planning & Patient Positioning
Successful outcomes with the posterolateral approach are heavily reliant on meticulous pre-operative planning and precise patient positioning.
Pre-Operative Planning
-
Comprehensive Imaging Assessment
:
- Computed Tomography (CT) : Indispensable for detailed bony anatomy, assessment of vertebral body destruction, cortical breaches, spinal canal compromise, and facet joint integrity. Thin-slice axial and sagittal reconstructions are essential. CT Angiography (CTA) can be highly beneficial, especially for mid-thoracic to thoracolumbar levels, to map the segmental arterial supply, identify the origin of the Artery of Adamkiewicz, and assess its relationship to the planned surgical corridor.
- Magnetic Resonance Imaging (MRI) : Crucial for visualizing soft tissue pathology such as epidural or prevertebral abscesses, tumor extension into the spinal canal or paravertebral spaces, degree of spinal cord compression, and intrinsic spinal cord signal changes (e.g., edema, myelomalacia). T2-weighted and T1-weighted post-contrast sequences are vital.
- Plain Radiographs : Anteroposterior, lateral, and flexion-extension views (if stability is a concern) provide an overview of spinal alignment, kyphosis, and potential gross instability.
-
Medical Optimization and Risk Stratification
:
- Cardiopulmonary Evaluation : Thorough assessment of pulmonary function (spirometry, arterial blood gas, cardiology consult if indicated) is paramount, particularly as this approach is often selected for patients with compromised respiratory status who cannot tolerate a full thoracotomy. Optimize respiratory function pre-operatively.
- Nutritional Status : Essential for wound healing and overall recovery, especially in patients with malignancy, chronic infection, or malnutrition. Pre-operative nutritional support may be warranted.
- Coagulation Profile : Strict management of antiplatelet agents and anticoagulants. Address any underlying coagulopathies.
- Anesthetic Assessment : Detailed discussion with the anesthesia team regarding positioning challenges, potential for significant blood loss, and need for one-lung ventilation capability (even if pleura is not intentionally entered, inadvertent breach is possible).
-
Surgical Strategy Development
:
- Accurate Level Identification : Confirm the target vertebral level(s) with high certainty from imaging. Intraoperative fluoroscopy or navigation will be used for final confirmation.
- Extent of Resection : Clearly define the planned extent of rib, transverse process, pedicle, and vertebral body resection to achieve the surgical goals (e.g., complete tumor debulking, circumferential decompression).
- Decompression Goals : Precisely determine the amount and direction of neural decompression required (e.g., anterior epidural, complete circumferential).
- Reconstruction Plan : Select the appropriate anterior column reconstruction material (e.g., expandable titanium cage packed with autograft/allograft, structural allograft, fibula strut graft) and ensure availability of appropriate sizes. Plan for posterior instrumentation (pedicle screws, rods) often as a concomitant procedure for multi-column stabilization.
- Blood Management : Anticipate potential significant blood loss. Arrange for cell saver, pre-donated autologous blood, or cross-matched allogeneic blood units. Discuss hemostatic agents.
- Neuromonitoring : Intraoperative neuromonitoring (Somatosensory Evoked Potentials – SSEPs, Motor Evoked Potentials – MEPs, and sometimes EMG) is strongly recommended for spinal cord protection during decompression, especially in cases of pre-existing neurological deficit or significant cord compression.
Patient Positioning
The patient is positioned prone on a specialized spinal frame (e.g., Jackson table, OSI table) or standard operating table with appropriate supports.
1.
Frame/Bolsters
: Use chest rolls or gel bolsters placed longitudinally on each side of the rib cage, extending from the clavicle to the iliac crest. This allows the abdomen to hang freely, minimizing intra-abdominal pressure, reducing epidural venous bleeding, and facilitating unrestricted chest excursion for respiration. Ensure there is no pressure on the anterior iliac spines or breasts.

2.
Head Position
: Securely position the head in a neutral, flexed, or slightly extended position, ensuring adequate padding and maintaining cervical spine alignment. A Mayfield head holder may be used if neuromonitoring electrodes are placed on the scalp or if cervical spine pathology requires immobilization.
3.
Upper Extremities
: Arms can be positioned either abducted on arm boards (less than 90 degrees to avoid brachial plexus stretch) or adducted along the torso, depending on surgeon preference and the need for C-arm access. Ensure proper padding of elbows, wrists, and hands to prevent nerve compression or pressure sores.

4.
Lower Extremities
: Knees should be slightly flexed with pillows or bolsters underneath, and ankles padded to prevent pressure injuries to the peroneal nerve or skin.
5.
C-arm Access
: Crucially, verify unobstructed C-arm access for intraoperative fluoroscopy in both anteroposterior and lateral planes. This is vital for confirming the surgical level, guiding rib/pedicle resection, and assisting with anterior column reconstruction and posterior instrumentation.
6.
Draping
: A wide sterile field draping is performed, encompassing the entire rib cage area. The drape should extend from the midline posteriorly to well into the lateral thorax, and sufficiently superior and inferior to allow for potential extension of the incision if broader access is unexpectedly required.

Landmarks and Incision
- Palpation : Palpate the spinous processes in the target area. The inferior angle of the scapula typically overlies the T7 spinous process in most individuals.
- Pre-operative Localization : Use fluoroscopy or a pre-operative plain X-ray with a radiopaque marker to confirm the target vertebral level. Mark the skin incision with indelible ink. A spinal needle can be inserted to the spinous process and confirmed with fluoroscopy for precise localization.
-
Incision
: A paramedian skin incision, approximately 3-4 cm lateral to the midline on the side of the pathology, is commonly used. This offers a more direct trajectory to the transverse process and rib head with less extensive muscle dissection. The length of the incision is dictated by the number of levels involved and whether concomitant posterior instrumentation is planned (typically one level above to one level below the pathology). Alternatively, a hockey-stick incision can be used, starting midline and curving laterally at the target level. For multi-level pathology or extensive posterior instrumentation, a midline incision with bilateral subperiosteal muscle dissection may be preferred.

Detailed Surgical Approach / Technique
The posterolateral approach is a meticulously choreographed sequence of dissections and resections designed to safely access the anterolateral thoracic spine.
1. Incision and Paraspinal Muscle Dissection
- Skin Incision : Make the paramedian skin incision as marked, typically extending one vertebral level above and one level below the pathology to allow for adequate exposure. For pathologies at T1-T3, the trapezius may need to be incised or retracted.
- Subcutaneous Tissue and Fascia : Deepen the incision through the subcutaneous fat to the level of the thoracolumbar fascia. Incise the fascia longitudinally.
- Paraspinal Muscle Elevation : Subperiosteally elevate the paraspinal muscles (erector spinae group, including the deep multifidus and semispinalis thoracis) from the spinous processes and laminae. The dissection proceeds laterally, exposing the facet joints, mamillary processes, transverse processes, and the ribs. Ensure complete and wide elevation of these muscles on the ipsilateral side to visualize the target rib and transverse process fully. The plane between the longissimus and iliocostalis can be exploited.
2. Identifying the Target Level and Rib Resection
- Radiographic Confirmation : Once the bony elements are exposed, use intraoperative fluoroscopy (AP and lateral views) to confirm the precise vertebral level. This often involves placing a metallic marker (e.g., K-wire) on a spinous process and comparing it to pre-operative imaging.
- Target Rib and Transverse Process Selection : To access a specific vertebral body, the rib that articulates with the pedicle of that vertebral body is typically resected. For example, to access the T8 vertebral body, the T8 rib (which articulates with T7 and T8 vertebral bodies) and the T8 transverse process are removed.
- Resection of Transverse Process : Using an osteotome or Leksell rongeur, resect the transverse process at its base, close to the vertebral body. This exposes the underlying costotransverse joint and the neck of the rib.
-
Rib Resection
:
- Carefully detach the costotransverse ligaments and the intercostal muscles from the superior aspect of the rib at the level of the transverse process.
- Disarticulate the rib head from the costovertebral joint. This requires careful manipulation and often a blunt instrument to protect the pleura anteriorly.
-
Resect a segment of the rib, typically 3-5 cm in length, just lateral to the costotransverse joint and extending anteriorly. Use a rib cutter, ensuring controlled transection. Protect the intercostal neurovascular bundle which runs along the inferior border of the rib. Meticulous hemostasis is vital.
 - The remaining rib stump is carefully managed to avoid sharp edges.
3. Exposure of the Vertebral Body and Spinal Canal
-
Pleural Dissection and Retraction
: After rib resection, the parietal pleura becomes visible, lying anterior to the vertebral body. Using blunt dissection (e.g., peanut sponges, fine-tipped Cobb elevators), carefully dissect the pleura anteriorly and medially away from the lateral aspect of the vertebral body and pedicle. The goal is to create a working space without violating the pleural cavity. A small self-retaining retractor with a pleural blade can be carefully inserted to maintain this retraction.
- Management of Pleural Breach : If the pleura is inadvertently torn, it should be immediately identified. Small tears can sometimes be managed with primary repair using fine non-absorbable sutures (e.g., 5-0 Prolene) and a fibrin sealant. Larger tears or those with significant air leakage often necessitate the placement of a chest tube post-operatively.
-
Segmental Neurovascular Bundle Management
: The intercostal neurovascular bundle (segmental artery, vein, and nerve) courses across the lateral aspect of the vertebral body. These vessels are typically ligated and divided if they obstruct access to the vertebral body, but extreme caution must be exercised. It is critical to confirm the absence of the Artery of Adamkiewicz at this level, especially in the thoracolumbar region. If identified, the Artery of Adamkiewicz must be meticulously preserved.
 - Pediculectomy : For optimal access to the vertebral body and spinal canal, the pedicle ipsilateral to the approach is usually resected. This can be performed with an osteotome, Kerrison rongeur, or a high-speed burr, proceeding carefully from lateral to medial. This exposes the lateral aspect of the dura mater and the posterolateral vertebral body.
4. Decompression, Resection, and Reconstruction
- Spinal Cord Decompression : With the pedicle removed, the dura mater and spinal cord are visible. Using a high-speed burr, Kerrison rongeurs, and fine curettes, carefully remove pathological tissue (e.g., tumor, abscess, retropulsed fracture fragments) from the vertebral body. The decompression should proceed from posterior to anterior, working away from the spinal cord. Maintain irrigation and use continuous neuromonitoring feedback. The posterior longitudinal ligament can be carefully excised if contributing to neural compression.
- Vertebral Body Resection : For tumor debulking or debridement of infected bone, a partial or complete corpectomy of the target vertebral body can be performed. Ensure clear margins (for tumors) or thorough debridement (for infections). The superior and inferior endplates of the adjacent healthy vertebrae must be prepared to receive the anterior column graft.
-
Anterior Column Reconstruction
: After adequate decompression and resection, the anterior column defect is reconstructed.
- Graft Selection : Common choices include expandable titanium cages packed with autologous bone graft (from the resected rib or iliac crest) or allograft, or structural allograft (e.g., femoral ring allograft).
- Graft Placement : The chosen graft is carefully impacted into the defect to restore vertebral body height and proper sagittal alignment. Ensure secure seating within the prepared endplates.
- Supplemental Anterior Plating : In some cases, a small anterior plate may be applied to the lateral aspect of the cage and adjacent vertebral bodies for additional stability, though this is less common with expandable cages combined with posterior fixation.
5. Posterior Instrumentation (if combined)
- If the primary goal also includes global spinal stabilization or correction of deformity, posterior pedicle screw instrumentation is performed. Pedicle screws are inserted into the vertebral bodies above and below the pathology (and potentially at the level of the corpectomy if a structural cage allows for screw placement). Contoured rods are then attached and secured to the screws, providing multi-column stability and allowing for compression or distraction as needed to achieve optimal alignment.
6. Closure
- Hemostasis : Achieve meticulous hemostasis throughout the entire surgical field. Use bipolar cautery, bone wax, and absorbable hemostatic agents.
- Dural Repair : If a dural tear occurred, perform a primary repair with fine non-absorbable sutures (e.g., 6-0 Prolene) in a watertight fashion. Augment with fascial or allograft patches and fibrin glue.
- Pleural Integrity : Re-inspect the pleura. If it was breached, confirm successful repair and perform a Valsalva maneuver to check for air leaks. If a significant leak persists, a chest tube connected to suction (e.g., Pleur-evac) should be inserted and secured.
- Wound Drainage : Place a deep suction drain (e.g., Jackson-Pratt) in the retrofascial space to manage potential post-operative bleeding or fluid collections.
- Layered Closure : Reapproximate the paraspinal muscles, thoracolumbar fascia, subcutaneous tissues, and skin in anatomical layers. Ensure tension-free closure.
Complications & Management
The posterolateral approach, while offering excellent access, is associated with a range of potential complications given the intricate anatomy of the thoracic spine. Awareness and meticulous technique are key to prevention and management.
| Complication | Incidence (Approximate) | Salvage Strategies / Management |
|
* |
*Key Features:
Addresses the anterolateral aspect of the thoracic spine from a posterior approach, avoiding intentional entry into the chest cavity. Allows for simultaneous posterior instrumentation. Relatively less physiological burden than full thoracotomy. |
Key Features:
Formal Thoracotomy (Direct Anterior):
Wider, more direct anterior visualization of the vertebral body and great vessels. Better for large, extensive anterior column lesions, complex deformities, or when vascular control is paramount.
Lateral Extracavitary Approach (Modified Posterolateral):
More extensive rib resection and muscle dissection, often involving resection of the costal pleura, allowing for broader anterior visualization than traditional posterolateral but still avoiding true intra-thoracic entry.
Purely Posterior Approach (Laminectomy/Posterior Fixation):
Minimal muscle dissection, focuses on posterior neural decompression (laminectomy/facetectomy) and posterior instrumentation. Limited to no anterior column access.
Minimally Invasive Approaches:
Smaller incisions, muscle sparing, faster recovery; however, limited exposure and may not be suitable for complex anterior column pathology.
Non-Operative Management:
Conservative care (pain medication, physical therapy, bracing) for stable, asymptomatic, or mildly symptomatic conditions. Radiation/chemotherapy for systemic tumors. Observation for mild compression without progressive neurological deficit. |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning and precise patient positioning are fundamental to the success and safety of the posterolateral approach.
Pre-Operative Planning
-
Comprehensive Imaging Assessment
:
- Computed Tomography (CT) : Indispensable for detailed bony anatomy, assessment of vertebral body destruction, cortical breaches, spinal canal compromise, and facet joint integrity. Thin-slice axial and sagittal reconstructions are essential for understanding the 3D pathology. CT Angiography (CTA) can be highly beneficial, especially for mid-thoracic to thoracolumbar levels (T7-L2), to map the segmental arterial supply, identify the probable origin of the Great Radicular Artery of Adamkiewicz, and assess its relationship to the planned surgical corridor. This helps in pre-emptively identifying vessels that need careful management.
- Magnetic Resonance Imaging (MRI) : Crucial for visualizing soft tissue pathology such as epidural or prevertebral abscesses, tumor extension into the spinal canal or paravertebral spaces, degree of spinal cord compression, and intrinsic spinal cord signal changes (e.g., edema, myelomalacia). T2-weighted and T1-weighted post-contrast sequences are vital. Diffusion-weighted imaging (DWI) can aid in differentiating active infection from old changes.
- Plain Radiographs : Anteroposterior, lateral, and flexion-extension views (if stability is a concern) provide an overview of spinal alignment, kyphosis, and potential gross instability. Assessment of pre-existing scoliosis or kyphosis is important for planning instrumentation.
-
Medical Optimization and Risk Stratification
:
- Cardiopulmonary Evaluation : Thorough assessment of pulmonary function (spirometry, arterial blood gas, cardiology consult if indicated) is paramount. This approach is often selected for patients with compromised respiratory status who cannot tolerate a full thoracotomy; therefore, optimizing respiratory function pre-operatively is crucial.
- Nutritional Status : Essential for wound healing and overall recovery, especially in patients with malignancy, chronic infection, or malnutrition. Pre-operative nutritional support and vitamin supplementation may be warranted.
- Coagulation Profile : Strict management of antiplatelet agents and anticoagulants is mandatory. Address any underlying coagulopathies pre-operatively. Discontinue antiplatelet agents (e.g., aspirin, clopidogrel) per established guidelines.
- Anesthetic Assessment : Detailed discussion with the anesthesia team regarding positioning challenges, potential for significant blood loss (and the need for large-bore IV access, arterial line, central venous access), and the capability for intraoperative blood salvage (cell saver) and rapid transfusion protocols. Even without planned pleural entry, preparedness for one-lung ventilation may be prudent in case of inadvertent pleural injury.
-
Surgical Strategy Development
:
- Accurate Level Identification : Confirm the target vertebral level(s) with high certainty from imaging. Intraoperative fluoroscopy or navigation will be used for final confirmation. Marking the skin with indelible ink pre-operatively, referencing anatomical landmarks and confirmed by X-ray, is standard.
- Extent of Resection : Clearly define the planned extent of rib, transverse process, pedicle, and vertebral body resection to achieve the surgical goals (e.g., complete tumor debulking, circumferential decompression of the spinal cord). Consider the necessary width of the bone window.
- Decompression Goals : Precisely determine the amount and direction of neural decompression required (e.g., anterior epidural decompression, complete circumferential decompression for burst fractures).
- Reconstruction Plan : Select the appropriate anterior column reconstruction material. Options include expandable titanium cages (often packed with autologous bone graft), structural allografts (e.g., femoral ring allograft), or autograft from the resected rib or iliac crest. Ensure availability of various sizes and shapes. Plan for posterior instrumentation (pedicle screws, rods) as a concomitant procedure for multi-column stabilization, usually spanning at least one level above and one level below the corpectomy.
- Blood Management : Anticipate potential significant blood loss. Arrange for cell saver, pre-donated autologous blood, or cross-matched allogeneic blood units. Discuss the use of intravenous hemostatic agents (e.g., tranexamic acid).
- Neuromonitoring : Intraoperative neuromonitoring (Somatosensory Evoked Potentials – SSEPs, Motor Evoked Potentials – MEPs, and sometimes EMG) is strongly recommended for spinal cord protection, especially during decompression near the cord, in cases of pre-existing neurological deficit, or significant cord compression.
Patient Positioning
The patient is positioned prone on a specialized spinal frame (e.g., Jackson table, OSI table) or standard operating table with appropriate supports to minimize abdominal compression and facilitate venous drainage.
1.
Frame/Bolsters
: Use chest rolls or gel bolsters placed longitudinally on each side of the rib cage, extending from the clavicle to the iliac crest. This allows the abdomen to hang freely, minimizing intra-abdominal pressure, thereby reducing epidural venous bleeding and facilitating unrestricted chest excursion for respiration. Ensure there is no pressure on the anterior iliac spines, breasts, or genitalia.

2.
Head Position
: Securely position the head in a neutral, flexed, or slightly extended position, ensuring adequate padding and maintaining cervical spine alignment. A Mayfield head holder may be used if neuromonitoring electrodes are placed on the scalp or if cervical spine pathology requires immobilization. Protect the eyes and ears.
3.
Upper Extremities
: Arms can be positioned either abducted on arm boards (less than 90 degrees at the shoulder to avoid brachial plexus stretch) or adducted along the torso, depending on surgeon preference and the need for C-arm access. Ensure proper padding of elbows, wrists, and hands to prevent nerve compression or pressure sores.

4.
Lower Extremities
: Knees should be slightly flexed with pillows or bolsters underneath, and ankles padded to prevent pressure injuries to the peroneal nerve or skin.
5.
C-arm Access
: Crucially, verify unobstructed C-arm access for intraoperative fluoroscopy in both anteroposterior (AP) and lateral planes. This is vital for confirming the surgical level, guiding rib/pedicle resection, assisting with anterior column reconstruction, and verifying posterior instrumentation placement.
6.
Draping
: A wide sterile field draping is performed, encompassing the entire rib cage area. The drape should extend from the midline posteriorly to well into the lateral thorax, and sufficiently superior and inferior to allow for potential extension of the incision if broader access is unexpectedly required. This wide field also allows for potential chest tube placement if a pleural injury occurs.

Landmarks and Incision
- Palpation : Palpate the spinous processes in the target area. The inferior angle of the scapula typically overlies the T7 spinous process in most individuals. The C7 spinous process is the most prominent.
- Pre-operative Localization : Use fluoroscopy or a pre-operative plain X-ray with a radiopaque marker to confirm the target vertebral level. Mark the skin incision with indelible ink. A spinal needle can be inserted to the spinous process and confirmed with fluoroscopy for precise localization just prior to incision. This step is critical to avoid wrong-level surgery.
-
Incision
: A paramedian skin incision, approximately 3-4 cm lateral to the midline on the side of the pathology, is commonly used. This offers a more direct trajectory to the transverse process and rib head with less extensive muscle dissection. The length of the incision is dictated by the number of levels involved and whether concomitant posterior instrumentation is planned (typically one vertebral level above to one vertebral level below the pathology). Alternatively, a hockey-stick incision can be used, starting midline and curving laterally at the target level. For multi-level pathology or extensive posterior instrumentation, a midline incision with bilateral subperiosteal muscle dissection may be preferred.

Detailed Surgical Approach / Technique
The posterolateral approach is a meticulously choreographed sequence of dissections and resections designed to safely access the anterolateral thoracic spine. The goal is to create an adequate working corridor to the anterior column pathology while preserving critical neurovascular structures and minimizing morbidity.
1. Incision and Paraspinal Muscle Dissection
- Skin Incision : Make the paramedian skin incision as marked, typically extending one vertebral level above and one level below the pathology to allow for adequate exposure. For pathologies at T1-T3, the trapezius may need to be incised or retracted laterally.
- Subcutaneous Tissue and Fascia : Deepen the incision through the subcutaneous fat to the level of the thoracolumbar fascia. Incise the fascia longitudinally. Electrocautery is used for precise and controlled dissection, ensuring adequate hemostasis.
- Paraspinal Muscle Elevation : Subperiosteally elevate the paraspinal muscles (erector spinae group, including the deep multifidus and semispinalis thoracis) from the spinous processes and laminae. The dissection proceeds laterally along the facet joints, exposing the mamillary processes, transverse processes, and the ribs. Ensure complete and wide elevation of these muscles on the ipsilateral side to fully visualize the target rib and transverse process. The plane between the longissimus and iliocostalis can be exploited to facilitate this lateral exposure. Self-retaining retractors are carefully placed to maintain the muscle exposure.
2. Identifying the Target Level and Rib Resection
- Radiographic Confirmation : Once the bony elements are exposed, use intraoperative fluoroscopy (AP and lateral views) to confirm the precise vertebral level. This often involves placing a metallic marker (e.g., K-wire) on a spinous process and comparing it to pre-operative imaging. Absolute certainty of the level is crucial.
- Target Rib and Transverse Process Selection : To access a specific vertebral body (e.g., T8), the rib that articulates with the pedicle of that vertebral body (T8 rib) is typically resected. This means the rib that has its costotransverse joint with the transverse process of the target vertebra is usually chosen.
- Resection of Transverse Process : Using an osteotome or Leksell rongeur, resect the transverse process at its base, close to the vertebral body. This exposes the underlying costotransverse joint and the neck of the rib.
-
Rib Resection
:
- Carefully detach the costotransverse ligaments and the intercostal muscles from the superior aspect of the rib at the level of the transverse process.
- Disarticulate the rib head from the costovertebral joint. This requires careful manipulation and often a blunt instrument (e.g., a curved pituitary rongeur or small osteotome) to protect the pleura anteriorly. Avoid excessive force to prevent pleural tear.
-
Resect a segment of the rib, typically 3-5 cm in length, just lateral to the costotransverse joint and extending anteriorly. Use a rib cutter, ensuring controlled transection. Protect the intercostal neurovascular bundle which runs along the inferior border of the rib. Meticulous hemostasis is vital at this stage.
 - The remaining rib stump is carefully managed to avoid sharp edges that could irritate surrounding tissues or puncture the pleura.
3. Exposure of the Vertebral Body and Spinal Canal
-
Pleural Dissection and Retraction
: After rib resection, the parietal pleura becomes visible, lying immediately anterior to the vertebral body. Using blunt dissection (e.g., peanut sponges, fine-tipped Cobb elevators), carefully dissect the pleura anteriorly and medially away from the lateral aspect of the vertebral body and pedicle. The goal is to create a working space without violating the pleural cavity. A small self-retaining retractor with a pleural blade (e.g., Capener retractor) can be carefully inserted to maintain this retraction.
- Management of Pleural Breach : If the pleura is inadvertently torn, it should be immediately identified. Small tears can sometimes be managed with primary repair using fine non-absorbable sutures (e.g., 5-0 Prolene) and a fibrin sealant. Larger tears or those with significant air leakage often necessitate the placement of a chest tube post-operatively, typically through a separate incision.
-
Segmental Neurovascular Bundle Management
: The intercostal neurovascular bundle (segmental artery, vein, and nerve) courses across the lateral aspect of the vertebral body. These vessels are typically ligated and divided if they obstruct access to the vertebral body, but extreme caution must be exercised. It is critical to confirm the absence of the Artery of Adamkiewicz at this level, especially in the thoracolumbar region. If identified, the Artery of Adamkiewicz must be meticulously preserved. Ligation of segmental vessels should be performed distal to the neural foramen to avoid compromising spinal cord blood supply.
 - Pediculectomy : For optimal access to the vertebral body and spinal canal, the pedicle ipsilateral to the approach is usually resected. This can be performed with an osteotome, Kerrison rongeur, or a high-speed burr, proceeding carefully from lateral to medial. This exposes the lateral aspect of the dura mater and the posterolateral vertebral body. The nerve root exiting at that level should be identified and protected.
4. Decompression, Resection, and Reconstruction
- Spinal Cord Decompression : With the pedicle removed, the dura mater and spinal cord are visible. Using a high-speed burr (with diamond burr if near dura), Kerrison rongeurs, and fine curettes, carefully remove pathological tissue (e.g., tumor, abscess, retropulsed fracture fragments) from the vertebral body. The decompression should proceed from posterior to anterior, working away from the spinal cord. Maintain generous irrigation and use continuous neuromonitoring feedback. The posterior longitudinal ligament can be carefully excised if contributing to neural compression, revealing the anterior dura.
- Vertebral Body Resection : For tumor debulking or debridement of infected bone, a partial or complete corpectomy of the target vertebral body can be performed. Ensure clear margins (for tumors) or thorough debridement (for infections). The superior and inferior endplates of the adjacent healthy vertebrae must be meticulously prepared (decorticated) to receive the anterior column graft, ensuring bleeding bone surfaces for fusion.
-
Anterior Column Reconstruction
: After adequate decompression and resection, the anterior column defect is reconstructed to restore height and stability.
- Graft Selection : Common choices include expandable titanium cages packed with autologous bone graft (from the resected rib or iliac crest) or allograft, or structural allograft (e.g., femoral ring allograft). The choice depends on surgeon preference, defect size, and bone quality.
- Graft Placement : The chosen graft is carefully impacted into the defect to restore vertebral body height and proper sagittal alignment. Ensure secure seating within the prepared endplates. Fluoroscopy is used to confirm optimal graft position and correction of kyphosis.
- Supplemental Anterior Plating : In some cases, a small anterior plate may be applied to the lateral aspect of the cage and adjacent vertebral bodies for additional stability, though this is less common with expandable cages combined with robust posterior fixation.
5. Posterior Instrumentation (if combined)
- If the primary goal also includes global spinal stabilization or correction of deformity, posterior pedicle screw instrumentation is performed concurrently. Pedicle screws are inserted into the vertebral bodies above and below the pathology (and potentially at the level of the corpectomy if a structural cage allows for screw placement in the adjacent body). Contoured rods are then attached and secured to the screws, providing multi-column stability and allowing for compression or distraction as needed to achieve optimal alignment. Final contouring and tightening of the constructs are performed.
6. Closure
- Hemostasis : Achieve meticulous hemostasis throughout the entire surgical field using bipolar cautery, bone wax, and absorbable hemostatic agents. Persistent bleeding can lead to hematoma and neurological compromise.
- Dural Repair : If a dural tear occurred, perform a primary repair with fine non-absorbable sutures (e.g., 6-0 Prolene) in a watertight fashion. Augment with fascial or allograft patches and fibrin glue. Test for CSF leak with Valsalva maneuver.
- Pleural Integrity : Re-inspect the pleura. If it was breached, confirm successful repair and perform a Valsalva maneuver to check for air leaks. If a significant leak persists, a chest tube connected to suction (e.g., Pleur-evac) should be inserted through a separate stab incision and secured, ensuring it is positioned to drain effectively.
- Wound Drainage : Place a deep suction drain (e.g., Jackson-Pratt) in the retrofascial space to manage potential post-operative bleeding or fluid collections.
- Layered Closure : Reapproximate the paraspinal muscles, thoracolumbar fascia, subcutaneous tissues, and skin in anatomical layers. Ensure tension-free closure to minimize wound complications. Apply sterile dressings.
Complications & Management
The posterolateral approach, while offering excellent access, is associated with a range of potential complications given the intricate anatomy of the thoracic spine and the extensive dissection involved. Awareness, meticulous surgical technique, and prompt postoperative recognition are key to prevention and effective management.
| Complication | Incidence (Approximate) | Salvage Strategies / Management |
|
* |
*Key Features:
|
|
*
*Infection (e.g., Abscess)
| * Debridement of infected bone and soft tissue. |
|
*
*Trauma (e.g., Burst Fracture)
| * Anterior column reconstruction (e.g., cage insertion) following decompression. |
|
* | * Targeted vertebral body biopsy. |
|
*Spine Trauma
| * Pedicle screw fixation for multi-segment stabilization. |
|
*
*Tumors (Primary/Metastatic)
| * Neurological assessment (motor strength, sensation, reflexes, gait). |
|
*
*Limited Anterior Fusion
| * Neurological assessment to document any existing deficits or radiculopathies. |
|
*
*Tumors (Primary/Metastatic)
| * Pain assessment (VAS scale, pain medication requirements). |
|
*
*Vertebral Body Mass for Biopsy
| * Careful post-operative monitoring for neurological changes, pain, and bleeding. |
|
*
*Anterolateral Decompression
| * Strict adherence to neurological baseline during post-op assessment. |
|
*
*Degenerative Conditions
| * Early mobilization and physical therapy. |
|
*
*Post-Traumatic Kyphosis
| * Bracing or external support as indicated. |
|
*
*Dural Tear / CSF Leak
| * Primary repair with fine suture (e.g., 6-0 Prolene). |
|
*
*Vascular Injury (e.g., Aorta, Adamkiewicz)
| * Careful dissection and meticulous hemostasis. |
|
*
*Respiratory Complications
| * Aggressive physiotherapy and pulmonary toilet. |
|
*
*Pneumothorax / Hemothorax
| * Chest tube placement for drainage.
Clinical & Radiographic Imaging
You Might Also Like