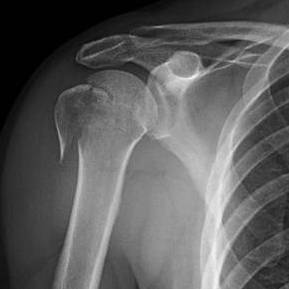
Proximal Humerus Fractures Epidemiology: Trends, Causes & Management
Key Takeaway
Looking for accurate information on Proximal Humerus Fractures Epidemiology: Trends, Causes & Management? Humerus fractures epidemiology indicates they are common, accounting for 4-6% of all fractures. They are the third most frequent non-vertebral fracture in elderly patients (>65 years old), occurring more often in females (2:1 ratio). Increasing age is associated with more complex types, typically resulting from low-energy falls in osteoporotic bones.
Introduction & Epidemiology
Proximal humerus fractures (PHFs) represent a significant orthopaedic challenge, standing as the third most common fracture in individuals over 65 years of age, following hip and distal radius fractures. They account for 4-6% of all fractures and affect women twice as often as men, correlating strongly with the prevalence of osteoporosis. The global incidence is on a trajectory of continuous increase, driven primarily by demographic shifts toward an aging population, with projections indicating a substantial rise in fracture burden and associated healthcare costs. While low-energy falls in osteoporotic elderly individuals are the predominant mechanism of injury, high-energy trauma can result in complex PHFs in younger, active patients.
The classification of PHFs is critical for prognosis and treatment planning. The Neer classification system, based on the number of displaced anatomical segments (greater tuberosity, lesser tuberosity, articular segment, and humeral shaft), remains widely utilized, categorizing fractures into two-, three-, and four-part patterns. Displacement is defined by greater than 1 cm of translation or 45 degrees of angulation. Two-part surgical neck fractures are the most common pattern, particularly in the elderly. Increasing age is often correlated with greater fracture complexity and poorer bone quality, significantly influencing management decisions and outcomes. The economic burden associated with PHFs is substantial, encompassing surgical costs, hospitalizations, rehabilitation, and long-term disability, underscoring the importance of evidence-based management strategies.
Surgical Anatomy & Biomechanics
A thorough understanding of the regional anatomy and biomechanics is paramount for successful surgical management of proximal humerus fractures.
Surgical Anatomy
- Bony Anatomy: The proximal humerus comprises the humeral head (articular surface), anatomical neck, surgical neck, greater tuberosity (GT), and lesser tuberosity (LT). The bicipital groove lies between the GT and LT, housing the long head of the biceps tendon. The surgical neck, distal to the tuberosities, is the most common fracture site.
- Vascularity: The vascular supply to the humeral head is crucial for its viability. The primary blood supply derives from the anterior and posterior circumflex humeral arteries, branches of the axillary artery. The anterior circumflex humeral artery gives rise to the arcuate artery (ascending branch), which typically enters the humeral head through the bicipital groove. The posterior circumflex humeral artery also contributes significantly, especially posteromedially. Disruption of these vessels, particularly the medial circumflex humeral artery (a branch of the posterior circumflex humeral artery which contributes to the ascending branch supplying the articular segment) and the ascending branch of the anterior circumflex humeral artery, is a major determinant of avascular necrosis (AVN) risk. Factors such as a disrupted medial hinge, increased fracture complexity (especially three- and four-part patterns), and displacement greater than 10 mm or angulation greater than 45° are associated with increased vascular insult. Preservation of ≥ 8mm of calcar attached to the articular segment is a strong predictor of humeral head vascularity.
- Neurological Structures: The axillary nerve is the most vulnerable nerve during proximal humerus surgery. It typically courses approximately 5-7 cm distal to the lateral acromion, inferior to the glenohumeral joint capsule, innervating the deltoid and teres minor. Care must be taken during lateral plate application or deltoid-splitting approaches to avoid iatrogenic injury. The musculocutaneous nerve lies within the coracobrachialis, and the radial nerve, while more distal, can be at risk with extensive dissection or humeral shaft extension fractures.
-
Soft Tissue & Rotator Cuff:
The rotator cuff tendons (supraspinatus, infraspinatus, teres minor, subscapularis) insert onto the greater and lesser tuberosities. These tendons are critical for shoulder function and their integrity and accurate reattachment are essential for restoring biomechanics.
- Supraspinatus: Inserts on the superior facet of the GT.
- Infraspinatus: Inserts on the middle facet of the GT.
- Teres Minor: Inserts on the inferior facet of the GT.
-
Subscapularis: Inserts on the LT.
Displacement of tuberosity fragments is often driven by the unopposed pull of these muscles.
Biomechanics
-
Fracture Displacement Patterns:
The specific fracture pattern and fragment displacement are largely dictated by the pull of the surrounding musculature and the initial trauma vector.
- Greater Tuberosity: Often displaced superiorly and posteriorly by the supraspinatus, infraspinatus, and teres minor.
- Lesser Tuberosity: Pulled medially by the subscapularis.
- Humeral Head: In surgical neck fractures, the humeral head can be abducted and externally rotated by the rotator cuff, while the shaft is adducted and internally rotated by the pectoralis major, latissimus dorsi, and teres major.
- Bone Quality: In osteoporotic bone, implant purchase is compromised, leading to increased risk of screw cutout, loss of reduction, and implant failure. This necessitates careful surgical planning, use of locking plates, suture augmentation, and medial calcar support.
- Medial Calcar Support: Restoration of medial calcar support is a critical biomechanical principle for stable fixation. Compression or reduction of the medial comminution, or impaction bone grafting, significantly increases the stability of locking plate constructs, reducing the risk of varus collapse and screw cutout. Without adequate medial support, locking screws in the humeral head can act as a fulcrum, leading to eventual failure.
- Load Sharing vs. Load Bearing: Locking plates primarily act as load-bearing devices, especially in osteoporotic bone. However, achieving anatomical reduction and cortical contact (load sharing) between the fracture fragments helps distribute stress and offload the plate, improving overall construct stability and healing potential.
Indications & Contraindications
The decision-making process for managing proximal humerus fractures involves a careful assessment of fracture morphology, patient demographics, functional demands, bone quality, and concomitant injuries.
Non-Operative Indications
- Minimally Displaced Fractures: Two-part surgical neck or tuberosity fractures with less than 1 cm displacement and less than 45° angulation.
- Stable Valgus-Impacted Fractures: These inherently stable fractures often have an intact medial hinge and are less prone to collapse or AVN.
- Low-Demand Patients: Elderly, frail patients with significant medical comorbidities who have limited functional expectations.
- Significant Medical Comorbidities: Patients for whom the risks of general anesthesia and surgery outweigh the potential benefits.
- Patient Preference: After thorough discussion of risks, benefits, and alternatives.
Operative Indications
-
Displaced Two-Part Fractures:
- Surgical neck fractures with >45° angulation or >1 cm translation.
- Greater tuberosity fractures with >5 mm retraction (can cause impingement and rotator cuff dysfunction).
- Lesser tuberosity fractures (rare, often associated with posterior dislocation, and can block reduction).
- Three-Part and Four-Part Fractures: Generally, these are unstable and often require surgical intervention to restore anatomy and function. The choice between ORIF and arthroplasty depends on age, bone quality, fracture pattern, and humeral head viability.
- Fracture-Dislocations: Require urgent reduction and often internal fixation or arthroplasty depending on the associated fracture.
- Open Fractures: Require urgent debridement and stabilization to prevent infection.
- Polytrauma Patients: Early stabilization may be necessary for overall patient management and mobilization.
- Young, Active Patients: With significant displacement, to optimize functional recovery and prevent long-term sequelae.
- Vascular Compromise: If associated with arterial injury requiring repair.
Contraindications
-
Absolute Contraindications:
- Active infection (relative for arthroplasty, often requiring two-stage procedure).
- Severe medical comorbidities precluding safe anesthesia and surgery.
- Non-reconstructible anatomy (especially for ORIF, might shift to arthroplasty).
-
Relative Contraindications:
- Extremely poor bone quality (for ORIF, may favor arthroplasty).
- Extensive soft tissue damage or devitalized skin, precluding safe closure.
- Patient's functional demands do not justify surgical risks.
Operative vs. Non-Operative Indications
| Fracture Type/Pattern | Non-Operative | Operative |
|---|---|---|
| Minimally Displaced 2-part | Yes (angulation <45°, translation <1 cm) | Rarely, in very active patients with slight displacement where optimal function is critical. |
| Displaced 2-part Surgical Neck | Yes (in frail, low-demand patients, or high risk for surgery) | Yes (angulation >45°, translation >1 cm), especially in young, active patients. |
| Displaced 2-part Greater Tuberosity | No (if retraction >5mm causing impingement) | Yes (retraction >5mm, particularly in young patients, to prevent impingement and restore rotator cuff function). |
| Displaced 2-part Lesser Tuberosity | No (if causing block to reduction or instability) | Yes (often associated with posterior dislocation, requires fixation if blocking reduction or causing instability). |
| 3-part Fractures | Rarely (very specific stable configurations, low demand) | Yes (significant displacement, angulation; choice between ORIF or arthroplasty based on age, bone quality, vascularity). |
| 4-part Fractures | No | Yes (often arthroplasty due to high AVN risk and reconstructive difficulty; ORIF in select younger patients with excellent bone and vascularity potential). |
| Fracture-Dislocation | No | Yes (urgent closed reduction; if unstable or irreducible, open reduction +/- fixation/arthroplasty depending on associated fracture). |
| Open Fractures | No | Yes (urgent surgical debridement and stabilization, potentially with external fixation followed by internal fixation). |
| Valgus-Impacted Fractures | Yes (stable, intact medial hinge) | Rarely (if loss of reduction or significant articular incongruity after initial non-op trial). |
| Segmental Bone Loss | No | Yes (ORIF with bone graft or arthroplasty if non-reconstructible). |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is the cornerstone of successful surgical outcomes in proximal humerus fractures, particularly given the complexity and variability of these injuries.
Pre-Operative Planning
-
Imaging Assessment:
- Plain Radiographs: Standard trauma series (AP, scapular Y, axillary lateral views) are the initial imaging modalities. These provide basic information on fracture pattern, displacement, and articular involvement.
-
Computed Tomography (CT) Scan:
Essential for almost all displaced or complex PHFs. A fine-cut CT scan with 3D reconstructions provides invaluable information regarding:
- True fracture morphology (number of parts, comminution, articular impaction).
- Displacement and angulation of fragments.
- Assessment of humeral head involvement and potential bone loss.
- Identification of impacted fragments or osteochondral lesions.
- Evaluation of glenoid involvement in fracture-dislocations.
- Planning screw trajectories and plate positioning.
- Magnetic Resonance Imaging (MRI): Rarely indicated acutely, but can be useful for assessing concomitant soft tissue injuries, such as rotator cuff tears, or for evaluating vascularity of the humeral head in uncertain cases (though less reliable than direct observation intraoperatively).
-
Fracture Classification & Surgical Strategy:
- Classification Systems: Re-evaluate the fracture using Neer and AO/OTA classification systems based on CT findings. The AO/OTA system provides a more detailed description of fracture complexity, which aids in selecting the most appropriate surgical technique.
-
Implant Selection:
Determine whether Open Reduction Internal Fixation (ORIF) with a locking plate, intramedullary nailing, hemiarthroplasty (HA), or reverse shoulder arthroplasty (RSA) is most appropriate.
- ORIF: Indicated for reconstructible fractures in younger, active patients with good bone quality and potentially salvageable humeral head vascularity. Requires careful consideration of plate length, screw type (locking vs. non-locking), and suture augmentation.
- Intramedullary Nailing: Less common for complex PHFs, but can be an option for select two-part surgical neck fractures, particularly in younger patients, to avoid extensive soft tissue stripping.
- Hemiarthroplasty: Historically used for irreparable four-part fractures, head-splitting fractures, or high-risk AVN in elderly patients with intact rotator cuffs. Outcomes are often variable due to tuberosity healing issues.
- Reverse Shoulder Arthroplasty (RSA): Increasingly the favored option for elderly patients with complex, irreparable fractures, poor bone quality, or pre-existing rotator cuff deficiency. It offers more predictable functional outcomes, especially for active elevation, by bypassing the need for tuberosity healing.
- Pre-Contouring: If ORIF is planned, consider pre-contouring the plate using a plastic model or 3D print to match the specific humeral anatomy.
- Contingency Planning: Always have a backup plan. Be prepared for potential conversion to arthroplasty if ORIF is deemed unfeasible or unstable intraoperatively.
-
Medical Optimization:
- Collaborate with anesthesia and internal medicine teams to optimize patient comorbidities (cardiac, pulmonary, diabetes, anticoagulation management).
- Ensure adequate nutritional status, especially in elderly patients.
-
Informed Consent:
- A thorough discussion with the patient and family regarding the nature of the injury, proposed treatment plan, alternative options (including non-operative), potential risks (AVN, nonunion, malunion, infection, nerve injury, stiffness, implant failure, need for revision surgery), expected outcomes, and rehabilitation protocol.
Patient Positioning
The choice of patient positioning significantly impacts surgical exposure and ease of reduction.
-
Beach Chair Position (Semi-Fowler's):
- Description: The patient is positioned with the torso elevated 30-70 degrees from horizontal, head supported, and both arms free. The torso is angled, and the legs are slightly bent.
- Advantages: Excellent visualization of the anterior and superior shoulder, allowing for easy access via the deltopectoral approach. Gravity assists in reducing bleeding, and both arms are accessible for manipulation and comparison. Allows for easy conversion to an open glenohumeral approach if needed.
- Disadvantages: Risk of "beach chair hypotension" (cerebral hypoperfusion) requiring meticulous blood pressure monitoring. Potential for brachial plexus stretch injury if the arm is not properly supported or extreme abduction is applied.
- Setup: Head secured in a headrest (e.g., Mayfield), torso supported, safety straps across the chest and hips. Axillary roll placed to protect the brachial plexus. Arm draped free or with a sterile stockinette.
-
Lateral Decubitus Position:
- Description: The patient is positioned on their side, with the affected shoulder superior.
- Advantages: Generally more stable for the patient, less risk of hypotension. Can be advantageous for certain posterior approaches or for traction.
- Disadvantages: More challenging to position the affected arm for free manipulation. Requires careful padding of bony prominences. Can make intraoperative fluoroscopy challenging.
-
Traction Table:
- Description: Used primarily for intramedullary nailing or complex fracture-dislocations where sustained traction is needed for reduction.
- Advantages: Provides consistent traction, freeing surgeon's hands for manipulation.
- Disadvantages: Limits direct manipulation of fragments, increases risk of brachial plexus traction injury, can restrict fluoroscopic views.
Regardless of the position, proper padding of all pressure points, securing the patient to the operating table, and meticulous sterile preparation and draping are essential to prevent iatrogenic injuries and surgical site infection. Ensure a wide sterile field to accommodate fluoroscopy and potential instrument trays.
Detailed Surgical Approach / Technique
This section will focus on the open reduction and internal fixation (ORIF) of proximal humerus fractures using a locking plate via the deltopectoral approach, which is the most common operative strategy for reconstructible fractures. Brief considerations for arthroplasty will also be included.
Deltopectoral Approach for ORIF with Locking Plate
-
Incision:
- A curvilinear incision is made in the deltopectoral groove, typically starting just inferior to the clavicle, extending distally towards the deltoid insertion. The length is dictated by fracture complexity and need for exposure.
- Deepen the incision through the skin and subcutaneous tissue.
-
Internervous Plane & Dissection:
- Identify the cephalic vein, which lies within the deltopectoral groove. It is typically retracted laterally with the deltoid. Protect it meticulously to prevent thrombosis or injury.
- The internervous plane is between the deltoid (innervated by the axillary nerve, posterior cord C5-C6) laterally and the pectoralis major (innervated by medial and lateral pectoral nerves, medial and lateral cords C5-T1) medially. This plane is relatively avascular and devoid of major motor nerves.
- Incise the clavipectoral fascia medial to the cephalic vein to further expose the interval.
- Retract the deltoid laterally and the pectoralis major medially using self-retaining retractors (e.g., Weitlaner) or army-navy retractors.
-
Exposure of the Fracture:
- The underlying structures – the coracoid process with its attached conjoined tendon (coracobrachialis and short head of biceps) – will become visible medially.
- The fracture hematoma is evacuated carefully.
- The fracture fragments are identified: humeral head, shaft, greater tuberosity, and lesser tuberosity.
- The subscapularis tendon, which inserts on the lesser tuberosity, is identified. If the lesser tuberosity is fractured and displaced, the subscapularis may be retracted medially. For better exposure of the glenohumeral joint or more complex reductions, the subscapularis may need to be released from the lesser tuberosity or tenotomized (repair required later).
- Protect the axillary nerve carefully. It courses posteriorly and laterally to the anterior circumflex humeral artery and veins, approximately 5-7 cm distal to the acromion.
- Minimize soft tissue stripping to preserve remaining vascularity to the humeral head fragments, especially posteromedially. Use stay sutures in the rotator cuff or tuberosity fragments for manipulation.
-
Fracture Reduction:
- Indirect Reduction: Start with gentle traction on the arm to disimpact fragments. External rotation of the forearm can help reduce the humeral head into varus angulation, while internal rotation can help reduce valgus.
-
Direct Reduction:
- Humeral Head: Use K-wires as joy-sticks, bone hooks, or an assistant's hand to maneuver the humeral head into anatomical position relative to the glenoid and tuberosities.
- Shaft: The shaft is typically medialized. Gentle lateralization and aligning with the head fragment is crucial.
- Tuberosities: These are often the most challenging fragments to reduce. Use non-absorbable sutures (e.g., FiberWire) passed through the rotator cuff tendons (supraspinatus, infraspinatus, subscapularis) to manipulate and reduce the greater and lesser tuberosities.
- Temporary Fixation: Once reduced, temporary K-wires are placed through the fragments (head-to-shaft, tuberosity-to-head) to maintain reduction while preparing for plate application.
- Medial Calcar Support: This is paramount. Assess the medial comminution. If present, consider bone grafting (autograft or allograft) or impaction of the medial metaphyseal bone into the defect to provide a stable buttress. The goal is to prevent varus collapse.
-
Plate Application & Fixation:
- Plate Selection: Choose a pre-contoured locking plate specifically designed for the proximal humerus (e.g., PHILOS, Synthes; Peri-Loc, Smith & Nephew). The plate should accommodate divergent and convergent locking screws for maximum head purchase.
- Plate Positioning: Position the plate on the lateral aspect of the humerus. The superior edge of the plate should be placed approximately 5-8 mm distal to the superior articular margin of the humeral head to avoid subacromial impingement with the acromion. Malpositioning too high is a common pitfall.
-
Proximal Fixation (Humeral Head):
- Insert multiple locking screws into the humeral head, aiming for divergent and convergent trajectories to maximize bone purchase and engage as many fragments as possible. These screws should be of appropriate length to engage the subchondral bone without penetrating the articular surface. Use fluoroscopy in multiple planes (AP, Y, axillary) to confirm screw length and avoid intra-articular penetration.
- Ensure good engagement of the calcar region with at least one or two screws.
-
Distal Fixation (Humeral Shaft):
- Secure the plate to the humeral shaft using cortical screws initially to compress the shaft to the plate, then locking screws to create a stable construct. Usually, 3-4 bicortical screws are sufficient for distal fixation.
-
Tuberosity Fixation:
- Utilize sutures, often passed through the plate eyelets or specific suture holes, to reattach the greater and lesser tuberosities to the plate and the humeral head. This provides additional rotational stability and allows for biological healing of the rotator cuff insertions. Typically, 2-3 strong non-absorbable sutures for each tuberosity are used.
- Tie these sutures carefully, ensuring the tuberosities are anatomically reduced and held securely against the humeral head and plate.
-
Intraoperative Fluoroscopy:
- Confirm final reduction, plate position, and screw lengths in AP, Y, and axillary views. Confirm no intra-articular screw penetration. Perform dynamic imaging through a range of motion to ensure no impingement or instability.
-
Wound Closure:
- Copious irrigation.
- Consider a subfascial drain if there's significant oozing, especially if concerns about hematoma formation are present.
- Close the deltopectoral fascia.
- Close subcutaneous tissues and skin in layers.
Arthroplasty Considerations (Briefly)
- Hemiarthroplasty (HA): For highly comminuted 4-part fractures or head-splitting fractures where ORIF is not feasible, especially in younger, high-demand patients with good bone stock and intact rotator cuff. The humeral head is replaced with a prosthetic stem and head. Tuberosity healing to the implant is critical for good function, but often unpredictable.
- Reverse Shoulder Arthroplasty (RSA): Increasing indication for elderly patients with irreparable fractures, poor bone quality, or pre-existing rotator cuff dysfunction. The ball-and-socket configuration is reversed, with a glenosphere on the glenoid and a socket on the humeral side. This medializes the center of rotation and increases the deltoid moment arm, allowing for deltoid-driven elevation independent of rotator cuff function. Tuberosity healing is less critical for functional outcome compared to HA.
Complications & Management
Proximal humerus fracture surgery, despite advancements, is associated with a range of potential complications, which can significantly impact functional outcomes. Proactive identification and appropriate management are crucial.
Complications and Salvage Strategies
| Complication | Incidence (Approx. Range) | Salvage Strategy |
|---|---|---|
| Avascular Necrosis (AVN) of Humeral Head | 10-30% (ORIF of 3/4-part) | Early (pre-collapse): Observation, activity modification. Late (post-collapse, symptomatic): Conversion to Hemiarthroplasty (HA) for younger patients with intact rotator cuff, or Reverse Shoulder Arthroplasty (RSA) for elderly, low-demand patients, or those with rotator cuff deficiency. |
| Nonunion / Delayed Union | 10-20% (ORIF) | Contributing Factors: Poor biology, inadequate reduction/fixation, AVN, infection, smoking, NSAID use. Management: Revision ORIF with plate augmentation (e.g., longer plate, locking blade plate), aggressive bone grafting (autograft or allograft, often with biologics like PRP/BMPs), conversion to HA or RSA, especially in the elderly or those with poor bone quality. |
| Malunion | 20-40% (ORIF) | Causes: Inadequate initial reduction, loss of reduction post-op, tuberosity displacement (especially greater tuberosity causing impingement). Management: Mild, asymptomatic: Observation. Symptomatic (pain, limited ROM, impingement): Corrective osteotomy (rare, complex), arthroscopic or open debridement for impingement, conversion to HA or RSA if severe articular incongruity or significant functional impairment. Tuberosity osteotomy for impingement. |
| Screw Penetration into Joint | 5-15% (ORIF) | Causes: Incorrect screw length measurement, inadequate fluoroscopy, technical error. Management: Early post-op (asymptomatic): Revision surgery to replace penetrating screws with shorter ones or remove them, if appropriate. Late (symptomatic): Arthroscopic removal of prominent screws, or open revision with potential debridement of articular cartilage, microfracture, or conversion to arthroplasty if significant articular damage. |
| Implant Failure / Pullout | 5-10% (ORIF) | Causes: Poor bone quality (osteoporosis), inadequate medial support, excessive load-bearing, early aggressive rehabilitation. Management: Revision ORIF with improved fixation (e.g., longer plate, more screws, bone grafting, medial calcar augmentation, suture augmentation), conversion to HA or RSA, especially if significant bone loss or irreparable. |
| Infection | 1-3% | Acute (early post-op): Urgent surgical irrigation and debridement, tissue cultures, appropriate IV antibiotics, potentially implant retention if stable. Chronic (late): Two-stage revision (implant removal, debridement, antibiotic spacer, then delayed reimplantation or arthroplasty), long-term antibiotics. |
| Nerve Injury (Axillary Nerve) | 5-10% (transient neuropraxia) | Causes: Traction, direct injury during dissection, nerve entrapment, prolonged retraction. Management: Transient Neuropraxia: Observation, electrodiagnostic studies (EMG/NCS) at 3-6 months. Persistent Deficit: Surgical exploration and neurolysis or repair if indicated, usually after 3-6 months of observation. |
| Stiffness / Adhesive Capsulitis | 20-50% | Causes: Prolonged immobilization, pain, subacromial scarring, inadequate rehabilitation. Management: Aggressive physiotherapy (PROM, AAROM, AROM), analgesia, subacromial steroid injections. If persistent and debilitating after 6-12 months: Manipulation Under Anesthesia (MUA) followed by intensive physiotherapy, or arthroscopic capsular release. |
| Rotator Cuff Pathology | Variable (often related to tuberosity issues) | Causes: Nonunion/malunion of tuberosities, iatrogenic injury, pre-existing tear. Management: Repair of tuberosity nonunion (with bone graft), rotator cuff repair, conversion to RSA if severe rotator cuff deficiency and loss of function. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is a critical component of successful management following proximal humerus fracture surgery. The protocol must be individualized based on the fracture pattern, stability of fixation, bone quality, age, patient compliance, and surgical technique employed. The overarching goal is to balance the need for fracture healing with the prevention of stiffness and restoration of optimal function.
General Principles
- Phased Approach: Rehabilitation typically progresses through distinct phases, gradually increasing load and range of motion.
- Protection of Fixation: The primary objective in the early phases is to protect the surgical repair, especially tuberosity fixation in ORIF and the prosthetic components in arthroplasty.
- Pain Management: Adequate pain control is essential to facilitate patient participation in therapy.
- Patient Education: Thorough education on activity restrictions, home exercise programs, and warning signs is vital for compliance.
Phase I: Immobilization & Early Passive Motion (Weeks 0-6)
-
Goals:
- Protect the healing fracture/repair.
- Control pain and swelling.
- Prevent stiffness of the elbow, wrist, and hand.
- Initiate gentle passive range of motion (PROM) for the shoulder.
-
Immobilization:
- Arm placed in a sling (e.g., sling with abduction pillow) for comfort and protection. Sling can be removed for hygiene and exercises.
-
Exercises (Daily):
- Elbow, Wrist, Hand AROM: Active flexion, extension, pronation, supination of the elbow, and active wrist/hand exercises to prevent stiffness and maintain circulation.
- Pendulum Exercises: Gentle, gravity-assisted circular motions (Codman's exercises) of the affected arm, with the trunk bent forward. Performed without active muscle contraction of the shoulder.
-
Passive Shoulder ROM:
- Forward Flexion: Supine position, therapist or unaffected hand assists in gentle elevation of the affected arm to pain-free limits (typically 0-90° initially).
- External Rotation: Supine position, arm at side, elbow flexed to 90°, gentle external rotation to pain-free limits (typically 0-30° initially).
- Internal Rotation: Hand to abdomen/lumbar spine.
- Scapular Mobility: Gentle active scapular retraction and protraction.
-
Restrictions:
- No active shoulder motion (lifting, pushing, pulling).
- No weight-bearing on the affected arm.
- Avoid sudden movements or jerking of the arm.
- No reaching behind the back or overhead for ORIF patients.
Phase II: Active-Assisted & Active Range of Motion (Weeks 6-12)
-
Goals:
- Gradually restore full non-painful shoulder range of motion.
- Begin light isometric strengthening.
- Improve neuromuscular control.
-
Progression:
- Radiographic assessment for signs of fracture healing (callus formation, bridging).
- Pain levels should be decreasing significantly.
-
Exercises (Progressive):
- Active-Assisted Range of Motion (AAROM): Progress from PROM to AAROM using pulleys, sticks, or the unaffected arm to assist in achieving full flexion, abduction, and rotation.
- Active Range of Motion (AROM): Once fracture stability is confirmed and pain allows, begin active shoulder motion against gravity.
- Light Isometric Strengthening: Begin gentle isometric exercises for the rotator cuff (subscapularis, infraspinatus, supraspinatus) and deltoid, performed in multiple directions (internal rotation, external rotation, abduction, flexion) at various angles, without movement of the joint.
- Scapular Stabilization: Continue with active scapular strengthening exercises.
-
Restrictions:
- Continue to avoid heavy lifting or sudden, forceful movements.
- Avoid resisted abduction and external rotation until tuberosity healing is well advanced (typically >10-12 weeks for ORIF).
Phase III: Progressive Strengthening & Return to Activity (Weeks 12+)
-
Goals:
- Maximize strength, endurance, and power.
- Restore full functional use of the arm.
- Return to desired activities and sports.
-
Progression:
- Continued radiographic evidence of healing.
- Full pain-free AROM achieved.
-
Exercises (Intensive):
- Progressive Resistance Exercises (PREs): Using resistance bands, light weights, and bodyweight exercises for all major shoulder muscle groups (rotator cuff, deltoid, scapular stabilizers).
- Eccentric Strengthening: Incorporate eccentric exercises to improve muscle control and shock absorption.
- Proprioceptive Training: Balance and coordination exercises to improve joint position sense.
- Functional Training: Simulate specific activities relevant to the patient's daily life, work, or sport.
- Sport-Specific Drills: Gradual reintroduction to sport-specific movements for athletes.
-
Return to Activity:
- Gradual return to light daily activities and work.
- Return to full, unrestricted activity and sport is typically 4-6 months, often longer for contact sports or overhead athletes, and contingent on full strength, ROM, and stability.
Special Considerations for Arthroplasty
- Hemiarthroplasty (HA): Rehabilitation is similar to ORIF, with a strong emphasis on protecting tuberosity repair. Tuberosity nonunion or malunion is a common cause of poor outcomes, so meticulous protection in early phases is paramount.
- Reverse Shoulder Arthroplasty (RSA): Rehabilitation protocols can often be more aggressive in terms of early passive and active range of motion, particularly for active elevation. This is due to the inherent stability of the implant and its reliance on the deltoid muscle for function, rather than rotator cuff healing. Specific protocols vary, but early deltoid activation exercises are common. However, internal and external rotation may still be restricted initially to protect surgical soft tissue repair.
Regular communication between the surgeon and the physical therapist is crucial to adjust the protocol based on individual patient progress and potential complications.
Summary of Key Literature / Guidelines
The landscape of proximal humerus fracture management has evolved significantly over recent decades, driven by clinical trials, systematic reviews, and meta-analyses. Key literature has helped to refine indications for surgery, compare treatment modalities, and inform rehabilitation strategies.
Non-Operative vs. Operative Management
- The PROFHIT Trial (2015, BMJ ): This landmark multicenter randomized controlled trial (RCT) compared surgical fixation (ORIF) with non-surgical management for displaced proximal humerus fractures in the elderly. The study found no significant difference in patient-reported outcomes (Oxford Shoulder Score) at 12 and 24 months between the two groups. Critically, the surgical group had a significantly higher rate of complications requiring reoperation. This trial has fundamentally shifted the paradigm, strengthening the argument for non-operative management in many elderly patients with displaced fractures, particularly stable two-part surgical neck fractures, if their functional demands are not high.
- Cochrane Review (2020): Meta-analyses and systematic reviews consistently demonstrate that for minimally displaced fractures, non-operative management is as effective as surgical intervention, with fewer associated risks. For displaced fractures in the elderly, current evidence often shows no clear superiority of surgery over non-operative care in terms of functional outcomes, while surgical treatment carries higher risks of complications.
- Younger Patients: For displaced fractures in younger, active patients, surgical fixation is generally favored to restore anatomy and function, despite limited high-level comparative evidence with non-operative treatment in this specific demographic.
ORIF vs. Arthroplasty
-
Increasing Role of Reverse Shoulder Arthroplasty (RSA):
For complex (3- and 4-part) fractures in elderly patients, particularly those with osteoporotic bone or pre-existing rotator cuff dysfunction, RSA is increasingly favored over hemiarthroplasty (HA) and even ORIF. Studies have shown RSA to provide more predictable functional outcomes (especially active elevation), lower reoperation rates (compared to ORIF in some series), and superior patient satisfaction compared to HA, largely due to bypassing the challenges of tuberosity healing.
- Brudvig et al. (2006, JSES ): Early work highlighting the advantages of RSA for complex fractures in the elderly.
- Hemiarthroplasty (HA): While historically the gold standard for irreparable 4-part fractures, HA outcomes have been variable due to unpredictable tuberosity healing, which is critical for good function. Its role is now largely limited to younger patients with irreparable articular damage but intact rotator cuffs, or as a salvage procedure.
-
ORIF for Complex Fractures:
In younger, active patients with reconstructible 3- or 4-part fractures and good bone quality, ORIF remains the preferred choice to preserve the native humeral head. However, the risk of avascular necrosis (AVN) remains a significant concern, especially in 4-part fractures.
- Court-Brown et al. (2004, JBJS-Br ): High complication rates with ORIF in complex PHFs, pushing the envelope towards arthroplasty in selected patients.
Technical Considerations for ORIF
-
Medial Calcar Support:
Numerous studies and biomechanical analyses emphasize the critical importance of restoring medial calcar support during ORIF with locking plates. This can involve anatomical reduction, impaction bone grafting, or placement of calcar screws. Absence of medial support significantly increases the risk of varus collapse and screw cutout.
- Gardner et al. (2007, JSES ): Landmark cadaveric study demonstrating the biomechanical benefit of medial column support in locking plate fixation.
- Suture Augmentation: Supplementing plate fixation with rotator cuff sutures tied through plate eyelets or around the shaft, to pull the tuberosities into place and maintain reduction, is a widely accepted technique to enhance construct stability and promote tuberosity healing.
- Screw Length & Placement: Careful intraoperative fluoroscopy is mandatory to ensure appropriate screw length, avoiding intra-articular penetration. High plate placement or excessive screw length can lead to subacromial impingement or articular damage.
Guidelines & Future Directions
- AAOS Guidelines: While specific, comprehensive guidelines for all PHF types are challenging due to fracture heterogeneity, various society guidelines (e.g., European Shoulder Associates) generally support non-operative management for minimally displaced fractures and increasingly favor RSA for complex fractures in the elderly.
- Patient-Reported Outcomes (PROs): The emphasis in modern orthopaedics is on PROs, guiding treatment decisions based on what matters most to the patient.
- Biologics: The use of adjuncts like bone morphogenetic proteins (BMPs) or platelet-rich plasma (PRP) to enhance healing in nonunions or poor bone quality is an area of ongoing research, though their routine use in acute PHF management is not yet evidence-based.
- Customized Implants & 3D Planning: Advancements in 3D printing and patient-specific instrumentation hold promise for improving anatomical reduction and fixation, particularly in complex cases.
In summary, the management of proximal humerus fractures continues to evolve, with a growing appreciation for individualized treatment based on robust evidence, meticulous surgical technique, and comprehensive post-operative rehabilitation. The trend towards non-operative management for many stable fractures and the increasing role of RSA for complex fractures in the elderly reflect a patient-centric approach aiming to optimize functional outcomes while minimizing complications.
You Might Also Like