Orthopaedic Problems in Children with CP: Prevention & Treatment
Key Takeaway
Discover the latest medical recommendations for Orthopaedic Problems in Children with CP: Prevention & Treatment. Orthopaedic problems in children with cerebral palsy commonly include contractures, hip dislocation, scoliosis, and foot deformities. Early diagnosis and treatment, physical therapy, orthotics, and sometimes surgery or medication are crucial to manage these conditions. Addressing these common problems in children helps prevent progression, improve mobility, reduce pain, and enhance their overall quality of life.
Introduction & Epidemiology
Cerebral palsy (CP) is a static encephalopathy resulting from a non-progressive lesion to the developing brain, leading to permanent impairments in movement and posture. Its clinical manifestations, however, are dynamic and progressive, particularly concerning secondary musculoskeletal deformities. The global prevalence of CP ranges from 1.5 to 3.0 per 1,000 live births, making it the most common cause of childhood physical disability.
The etiology is multifactorial, encompassing prenatal (e.g., intrauterine infection, genetic factors), perinatal (e.g., asphyxia, prematurity, low birth weight), and postnatal insults (e.g., head trauma, meningitis). Classification systems are crucial for prognosis and guiding intervention. The Gross Motor Function Classification System (GMFCS) stratifies functional mobility from Level I (ambulates without limitations) to Level V (severe limitations, requiring maximal assistance). The Manual Ability Classification System (MACS) categorizes upper extremity function, while the Communication Function Classification System (CFCS) assesses communication abilities. Topographical classifications (e.g., hemiplegia, diplegia, quadriplegia) describe the affected body regions.
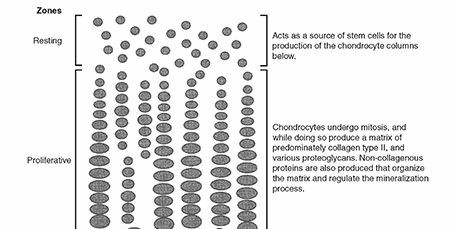
Orthopaedic problems in children with CP are secondary consequences of the primary neurological lesion and include muscle spasticity, weakness, altered muscle tone, impaired selective motor control, and abnormal reflexes. These factors lead to progressive deformities due to unbalanced muscle forces acting on growing bones and joints. Common orthopaedic sequelae include:
*
Hip Dysplasia and Dislocation:
Prevalent in up to 30-35% of children with CP, particularly GMFCS Levels III-V.
*
Equinus, Planovalgus, and Varus Foot Deformities:
Affecting gait mechanics and brace wear.
*
Knee Flexion Contractures and Patellar Instability:
Contributing to crouch gait.
*
Spinal Deformities:
Primarily neuromuscular scoliosis and kyphosis, often associated with pelvic obliquity, especially in GMFCS Levels IV-V.
*
Upper Extremity Deformities:
Wrist and finger flexion contractures, forearm pronation.
Early diagnosis and intervention are paramount to mitigate the progression of these deformities, preserve joint integrity, reduce pain, improve functional independence, facilitate caregiving, and ultimately enhance quality of life. The management of orthopaedic problems in CP requires a comprehensive, multidisciplinary approach tailored to the child's age, GMFCS level, specific deformities, and functional goals.
Surgical Anatomy & Biomechanics
Understanding the complex interplay of altered anatomy and dysfunctional biomechanics is fundamental to surgical planning in CP. The primary neurological insult results in muscle imbalance, spasticity, and weakness, which exert abnormal forces on the musculoskeletal system, leading to progressive bony and soft tissue deformities.
Hip Joint
The hip is a ball-and-socket joint, inherently stable due to its bony configuration (acetabulum and femoral head) and surrounding musculature. In CP, this stability is compromised:
*
Muscle Imbalance:
Spasticity and contracture of hip adductors (adductor longus, brevis, magnus, gracilis, pectineus) and flexors (iliopsoas, rectus femoris) create a medially and superiorly directed force on the femoral head. Concurrently, weakness of hip abductors (gluteus medius, minimus) and extensors (gluteus maximus, hamstrings) further destabilizes the joint.
*
Bony Morphology:
*
Femoral Anteversion:
Increased femoral neck anteversion is common, leading to external rotation gait or compensatory internal rotation of the entire limb.
*
Coxa Valga:
Increased femoral neck-shaft angle reduces the mechanical advantage of the abductors and contributes to subluxation.
*
Acetabular Dysplasia:
Chronic subluxation leads to a shallow, poorly developed acetabulum, with inadequate anterior and superior coverage of the femoral head.
*
Pelvic Obliquity:
Often seen in association with scoliosis or unilateral hip subluxation, where one hemipelvis is elevated or depressed, affecting sitting balance and spinal alignment.
*
Biomechanics of Subluxation:
The unopposed pull of spastic adductors and psoas muscles, combined with limited weight-bearing in GMFCS Levels III-V, results in lateral migration of the femoral head. The Reimers Migration Percentage (MP) quantifies the degree of femoral head subluxation relative to the lateral margin of the acetabulum on an anteroposterior pelvic radiograph. An MP >33% often indicates significant subluxation requiring intervention, while >60% suggests frank dislocation.
Knee Joint
Knee deformities in CP are primarily characterized by flexion contractures and patellar abnormalities.
*
Muscle Imbalance:
Spasticity and contracture of hamstrings (semimembranosus, semitendinosus, biceps femoris) lead to knee flexion contracture. Spasticity of the rectus femoris can also contribute to dynamic knee flexion in swing phase or produce a stiff-knee gait pattern.
*
Bony Morphology:
Chronic knee flexion can lead to posterior femoral condyle changes and patella alta (high-riding patella), increasing extensor mechanism demands and predisposing to patellar subluxation.
*
Biomechanics of Crouch Gait:
Persistent knee flexion throughout the gait cycle (crouch gait) is a hallmark of diplegic CP. This increases quadriceps demand, energy expenditure, and can lead to progressive patellofemoral pain and premature osteoarthritis.
Foot and Ankle Complex
Foot and ankle deformities are diverse and significantly impair gait and orthosis use.
*
Muscle Imbalance:
*
Equinus:
Spasticity and contracture of the triceps surae (gastrocnemius and soleus) are the primary drivers of equinus deformity, where the ankle is fixed in plantarflexion.
*
Planovalgus:
Spasticity of the peroneus longus/brevis and/or weakness of the tibialis posterior, combined with triceps surae tightness, can lead to hindfoot valgus and midfoot collapse.
*
Varus:
Spasticity of the tibialis posterior, often coupled with weakness of the peroneals, can result in hindfoot varus and forefoot adduction.
*
Bony Morphology:
Chronic abnormal forces can lead to forefoot adduction, midfoot collapse (rocker-bottom foot), or compensatory changes in the talus and calcaneus.
*
Biomechanics:
Equinus prevents heel strike and adequate dorsiflexion for foot clearance, leading to toe walking or a calcaneal gait if overcorrected. Planovalgus results in an unstable foot lever, poor push-off, and difficulty with shoe wear. Varus leads to concentrated pressure on the lateral border of the foot.
Spine
Neuromuscular scoliosis is a common and often severe deformity in CP.
*
Muscle Imbalance:
Truncal muscle weakness and asymmetry, coupled with spasticity, result in unbalanced forces acting on the vertebral column. Involvement of paraspinal muscles, obliques, and quadratus lumborum can contribute.
*
Bony Morphology:
Progressive vertebral wedging and rotation lead to a C-shaped or S-shaped curve. Pelvic obliquity, where one side of the pelvis is higher than the other, is frequently observed and is often coupled to the primary spinal curve.
*
Biomechanics:
Progressive scoliosis compromises sitting balance, pulmonary function, and causes pain. The loss of stable trunk support further limits upper extremity function and activities of daily living. Severe curves can lead to thoracic cage distortion and restrictive lung disease.
Upper Extremity
While less frequently requiring complex surgical intervention than lower extremities, upper limb deformities impact fine motor skills.
*
Muscle Imbalance:
Spasticity of the wrist and finger flexors (flexor carpi ulnaris/radialis, flexor digitorum superficialis/profundus) and forearm pronators (pronator teres/quadratus) often coexists with weakness of extensors and supinators.
*
Biomechanics:
This leads to a characteristic posture of wrist flexion, ulnar deviation, and thumb-in-palm deformity, significantly impairing grasp and release functions.
Indications & Contraindications
Management of orthopaedic problems in CP involves a spectrum of non-operative and operative strategies, dictated by the patient's age, GMFCS level, specific deformity, functional goals, and the presence of pain or functional limitation.
Indications for Non-Operative Management
Non-operative interventions are typically first-line treatments, aiming to prevent progression, improve function, and reduce pain. They are particularly indicated for dynamic deformities or those not yet fixed.
-
Physical Therapy (PT) / Occupational Therapy (OT):
- Indications: All GMFCS levels, to improve strength, range of motion (ROM), flexibility, motor control, balance, and functional skills. Essential for post-operative rehabilitation.
-
Serial Casting:
- Indications: Mild to moderate fixed contractures (e.g., equinus, knee flexion contracture, wrist flexion contracture) in younger children or as a preparatory measure for surgery.
-
Orthotics (AFOs, DAFOs, KAFOs, TLSOs):
- Indications: To support joints, control dynamic deformities, improve alignment, enhance stability during standing/gait, and prevent progression of mild to moderate fixed deformities (e.g., AFO for equinus, TLSO for mild scoliosis).
-
Botulinum Toxin Type A (BoNT-A) Injections:
- Indications: Localized dynamic spasticity causing functional limitations, pain, or contributing to deformity (e.g., spastic gastrocnemius, adductors, hamstrings, flexor carpi ulnaris). Temporary effect, typically lasting 3-6 months. Often used in conjunction with PT/casting.
-
Oral Medications (e.g., Baclofen, Diazepam, Tizanidine):
- Indications: Generalized spasticity impacting multiple muscle groups, causing pain or interfering with function/care. Systemic side effects can be limiting.
-
Intrathecal Baclofen (ITB) Pump:
- Indications: Severe, generalized spasticity, particularly in GMFCS Levels IV-V, refractory to oral medications and BoNT-A, causing significant functional impairment, pain, or difficulty with care. Requires surgical implantation and ongoing management.
-
Selective Dorsal Rhizotomy (SDR):
- Indications: Severe spasticity primarily affecting lower extremities, significantly impacting gait and motor function, in carefully selected ambulant children (GMFCS I-III) with good underlying strength and motor control. Irreversible procedure.
Indications & Contraindications for Operative Management
Surgical intervention is considered when non-operative measures fail, when deformities are fixed and progressive, or when they cause significant pain, functional limitation, or interfere with care. A comprehensive evaluation, including gait analysis for ambulators, is often warranted.
| Category | Operative Indications | Non-Operative Indications |
|---|---|---|
| Hip |
- Progressive hip subluxation (Reimers MP >33%) despite non-operative management.
- Frank hip dislocation (MP >90%). - Pain (e.g., from subluxation/dislocation, labral tear). - Significant pelvic obliquity due to hip asymmetry. - Interference with seating, hygiene, or caregiver burden. - Acetabular dysplasia or excessive femoral anteversion/coxa valga contributing to instability. |
- Reimers MP <33% with no progression.
- Dynamic adductor/flexor spasticity without fixed contracture or bony changes (target for BoNT-A). - Mild adduction/flexion contractures manageable with PT, stretching, and bracing. - Surveillance imaging for early detection of subluxation. |
| Foot & Ankle |
- Fixed equinus deformity limiting dorsiflexion to neutral or beyond, affecting brace wear or gait (e.g., toe walking, impaired foot clearance).
- Fixed planovalgus or varus deformity causing pain, poor weight-bearing, skin breakdown, or inability to wear standard shoes/orthoses. - Lever arm dysfunction leading to inefficient gait. - Bony deformities refractory to soft tissue releases. |
- Dynamic equinus responsive to BoNT-A and serial casting.
- Mild planovalgus/varus without fixed bony deformity, manageable with orthotics and PT. - Flexible deformities with good passive correction. - Post-operative maintenance of correction. |
| Knee |
- Fixed knee flexion contracture (>10-15 degrees) causing significant crouch gait, increased energy expenditure, or quadriceps strain.
- Patella alta or recurrent patellar subluxation associated with crouch gait or extensor mechanism dysfunction. - Persistent hamstring spasticity contributing to crouch gait despite non-operative measures. |
- Dynamic knee flexion responsive to BoNT-A.
- Mild knee flexion contractures manageable with PT and serial casting. - Mild crouch gait managed with orthotics. - Selective dorsal rhizotomy (SDR) as an alternative for severe spasticity contributing to crouch gait in suitable candidates. |
| Spine (Scoliosis) |
- Progressive neuromuscular scoliosis with Cobb angle >40-50 degrees, especially with associated pelvic obliquity.
- Loss of sitting balance or trunk control. - Significant pain. - Pulmonary compromise due to thoracic deformity. - Intractable skin breakdown over bony prominences exacerbated by deformity. - Failure of bracing to control progression. |
- Mild curves (<20 degrees) managed with observation and PT.
- Moderate curves (20-40 degrees) in younger children that are flexible, managed with bracing (TLSO) to prevent progression (though efficacy in neuromuscular scoliosis is limited compared to idiopathic). - Prioritization of medical stability for non-ambulators before surgery. |
| Upper Extremity |
- Fixed wrist/finger flexion contractures or forearm pronation significantly impairing functional use (grasp, release, hygiene) and refractory to conservative measures.
- Tendon transfers for improved function (e.g., pronator teres rerouting). - Tenodesis procedures for wrist stability. - Bony procedures for severe, fixed deformities (e.g., distal radius osteotomy). |
- Dynamic spasticity responsive to BoNT-A with PT and splinting.
- Mild contractures manageable with serial casting, stretching, and splinting. - Functional training in OT for compensatory strategies. - Consider SDR for generalized upper extremity spasticity in select cases. |
| General |
- Persistent pain not controlled by non-operative means.
- Progressive deformity leading to significant functional decline or interference with activities of daily living/care. - Bony deformities beyond correction by soft tissue releases. - Failure of appropriate non-operative management attempts. - Patient/family desire for improved function or appearance within realistic expectations. |
Contraindications for all Operative Management:
- Acute medical instability or severe systemic comorbidities precluding safe anesthesia and recovery. - Unrealistic patient/family expectations. - Poor underlying general health or nutrition status. - Lack of adequate post-operative rehabilitation support. - Non-fixed, dynamic deformities that could respond to less invasive treatment. |
General Contraindications for Operative Management:
- Acute Medical Instability: Uncontrolled seizures, severe respiratory compromise, critical nutritional status, active infections.
- Poor General Health: Significant cardiopulmonary disease, severe osteopenia/osteoporosis, poor wound healing potential.
- Lack of Rehabilitation Potential: Inability to participate in post-operative therapy due to cognitive limitations or lack of support system, which may negate surgical benefits.
- Unrealistic Expectations: Failure of the patient or caregivers to comprehend the limitations of surgery or the demands of rehabilitation.
- Non-Fixed Deformities: Dynamic deformities that may respond to less invasive interventions like BoNT-A injections or serial casting.
Pre-Operative Planning & Patient Positioning
Thorough pre-operative planning is critical for optimizing outcomes and minimizing complications in children with CP. This requires a comprehensive assessment and a multidisciplinary team approach.
Pre-Operative Planning
-
Comprehensive Patient Assessment:
- History: Detailed medical history, neurological status, seizure control, feeding method, bowel/bladder function, previous surgeries, medications. Family and caregiver concerns and functional goals.
-
Physical Examination:
- GMFCS Level: To guide functional expectations and rehabilitation.
- Range of Motion (ROM): Passive and active ROM for all affected joints, noting fixed contractures.
- Spasticity: Ashworth or Modified Ashworth Scale.
- Selective Motor Control: Ability to isolate muscle activation.
- Strength: Manual muscle testing.
- Gait Analysis: For ambulators (GMFCS I-III), clinical observation and 3D instrumented gait analysis (kinematics, kinetics, EMG) are invaluable for identifying specific muscle contributions to deformities and guiding surgical targets.
- Skin Integrity: Especially important for potential cast application sites or pressure points.
-
Imaging:
- Radiographs: Anteroposterior pelvis (Reimers MP for hip subluxation), weight-bearing lower extremity alignment views, foot series, standing full-length spine series (Cobb angle, pelvic obliquity).
- MRI/CT: May be indicated for complex bony deformities, spinal cord evaluation in scoliosis, or assessment of hip anatomy (e.g., acetabular version).
- Bone Density: Dual-energy X-ray absorptiometry (DXA) for children with limited mobility, as osteopenia is common and impacts hardware selection and fixation.
- Nutritional Assessment: Many children with severe CP are malnourished. Pre-operative nutritional optimization (e.g., G-tube feeding, dietitian consultation) is essential for wound healing and overall recovery.
- Anesthesia Consultation: Evaluation of airway, respiratory function (spirometry for scoliosis), cardiac status, and potential for difficult intubation. Blood availability, especially for major reconstructive cases.
-
Multidisciplinary Team Meeting:
- Involvement of orthopaedic surgeon, neurosurgeon (if ITB/SDR involved), physiatrist, neurologist, anesthesiologist, physical therapist, occupational therapist, social worker, and sometimes pulmonologist/gastroenterologist.
- Review of all findings, discussion of surgical goals, potential risks, and expected outcomes.
- Development of a comprehensive surgical plan (e.g., single-event multi-level surgery - SEMLS).
-
Informed Consent: Detailed discussion with family regarding the procedure(s), potential benefits, risks (including general and specific complications), expected recovery, and long-term implications.
Patient Positioning
Correct patient positioning is paramount for surgical access, prevention of iatrogenic injury, and accurate execution of the procedure. Specific considerations apply to children with CP due to their spasticity, contractures, and potential for osteopenia.
-
General Principles:
- Padding: Meticulous padding of all bony prominences (heels, malleoli, knees, elbows, shoulders, occiput) to prevent pressure sores and nerve palsies.
- Support: Use of gel pads, foam, and blankets to maintain position and distribute pressure.
- Circulation: Avoidance of tourniquet application over areas of spasticity or bony deformities without careful consideration. For lower extremity procedures, a pneumatic tourniquet is often used; ensure correct size and inflation pressure.
- Monitoring: Continuous physiological monitoring (ECG, pulse oximetry, capnography, core temperature, blood pressure). Neuromonitoring (SSEP, MEP, EMG) is essential for spinal and certain complex lower extremity surgeries.
- Anesthesia Access: Ensure unimpeded access to IV lines, arterial lines, and the airway.
-
Specific Positions:
-
Supine:
Common for lower extremity soft tissue releases, most foot surgeries (with foot of bed down), and some hip procedures (e.g., adductor/psoas releases).
- Considerations: Ensure hips are not excessively abducted or adducted, knees not hyperflexed.
-
Lateral Decubitus:
Used for hip reconstructive procedures (e.g., femoral osteotomy, pelvic osteotomy).
- Considerations: Stabilize torso and pelvis with beanbag or vacuum mattress. Lower leg flexed, upper leg straight. Axillary roll under the dependent axilla. Ensure adequate padding of dependent ear, shoulder, iliac crest, knee, and ankle. Careful positioning of the arm to prevent brachial plexus injury.
-
Prone:
Standard for posterior spinal fusion.
- Considerations: Chest rolls or spinal frame (e.g., Jackson table) to allow for free abdominal movement, reducing intra-abdominal pressure and epidural venous bleeding. Head in a neutral position, well-padded. Arms abducted less than 90 degrees, forearms pronated. Knees slightly flexed with pillows underneath to prevent peroneal nerve compression. Ensure secure endotracheal tube.
- Beach Chair: Seldom used for CP orthopaedics, but occasionally for complex upper extremity procedures.
-
Supine:
Common for lower extremity soft tissue releases, most foot surgeries (with foot of bed down), and some hip procedures (e.g., adductor/psoas releases).
-
Tourniquet Use:
- Typically used for lower extremity surgeries (foot, ankle, knee) to provide a bloodless field.
- Inflation pressures usually 50-100 mmHg above systolic BP.
- Duration should be minimized, typically <90-120 minutes.
- Consider sequential tourniquet release in complex multi-level surgeries.
Detailed Surgical Approach / Technique
Given the extensive range of orthopaedic problems in CP, this section will detail three common and impactful surgical interventions:
1.
Hip Reconstruction:
Addressing subluxation/dislocation (e.g., Varus Derotation Osteotomy (VDRO) + Dega Osteotomy).
2.
Equinus Deformity Correction:
(e.g., Z-Lengthening of Achilles Tendon).
3.
Spinal Fusion for Neuromuscular Scoliosis:
1. Hip Reconstruction: Varus Derotation Osteotomy (VDRO) & Dega Osteotomy
This combined procedure addresses femoral head deformity (coxa valga, increased anteversion) and acetabular dysplasia, commonly indicated for GMFCS Levels III-V with Reimers MP >33%.
A. Varus Derotation Osteotomy (VDRO) of the Proximal Femur
- Pre-operative Considerations: Templating for appropriate hardware (plate and screws). Consider a contralateral adductor/psoas release if indicated.
- Patient Positioning: Lateral decubitus with the affected hip superior. Beanbag for stability.
-
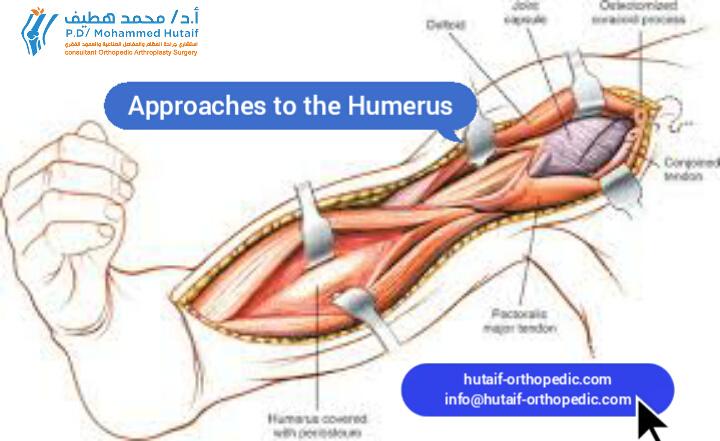
Surgical Approach:
Lateral approach to the proximal femur.
- Incision: Straight lateral incision centered over the proximal femoral shaft, extending from the greater trochanter distally approximately 8-10 cm.
- Dissection: Incise skin, subcutaneous tissue. Deep fascia (fascia lata) is incised longitudinally. The vastus lateralis muscle is identified and incised longitudinally along its anterior border, approximately 1 cm posterior to the intermuscular septum. This internervous plane is between the vastus lateralis (supplied by the femoral nerve, anterior division) and the vastus intermedius (supplied by the femoral nerve, posterior division).
- Exposure: Retract the vastus lateralis anteriorly and vastus intermedius posteriorly to expose the lateral cortex of the femur at the level of the lesser trochanter. The gluteus medius and minimus insertions on the greater trochanter are generally left undisturbed if not performing a trochanteric advancement.
- Osteotomy Planning: Determine the level of the osteotomy, typically just distal to the lesser trochanter. Mark the femur for rotational and varus correction using osteotomy guides or k-wires. The amount of varus (typically 15-20 degrees) and derotation (to achieve 10-15 degrees of residual anteversion) is determined pre-operatively based on clinical and radiographic assessment.
- Osteotomy: Perform a transverse or oblique osteotomy using an oscillating saw. Protect soft tissues posteriorly with a malleable retractor.
- Correction: Perform the planned varus and derotation correction. The distal fragment is internally rotated and adducted relative to the proximal fragment. The degree of derotation is often guided by aiming the patella straight anteriorly with the hip in neutral rotation on the table.
- Fixation: Secure the osteotomy with a pre-contoured paediatric hip plate (e.g., a dynamic hip screw (DHS) plate, pediatric locking plate, or blade plate). Ensure proper screw placement in both proximal and distal fragments, avoiding penetration of the joint.
- Wound Closure: Hemostasis, layered closure of the vastus lateralis, fascia lata, subcutaneous tissue, and skin.
B. Dega Osteotomy (Pelvic Osteotomy)
- Pre-operative Considerations: Essential for acetabular dysplasia, providing lateral and anterior coverage.
- Patient Positioning: Often performed sequentially with VDRO, so patient may be re-draped or positioned similarly.
-
Surgical Approach:
Modified anterior (Smith-Peterson) approach to the ilium.
- Incision: Oblique incision along the anterior iliac crest, extending from just posterior to the ASIS towards the PSIS, approximately 8-10 cm.
- Dissection: Incise skin, subcutaneous tissue. The superficial fascia is incised. The muscle attachments to the iliac crest (internal and external obliques, transversus abdominis) are sharply incised and stripped subperiosteally off the lateral aspect of the ilium. The sartorius and tensor fascia lata are reflected from the ASIS. The internervous plane is between the muscles arising from the iliac crest and the gluteal muscles.
- Exposure: The outer table of the ilium is exposed from the ASIS posteriorly to the sacroiliac joint. Subperiosteal dissection exposes the inner table of the ilium as well. The sciatic notch should be carefully identified and protected.
- Osteotomy: An osteotomy is performed in the supra-acetabular region, beginning at the outer table just superior to the acetabulum, extending posteriorly and inferiorly towards the triradiate cartilage (but not violating it). The cut should be directed towards the sciatic notch. The inferior cut is left incomplete, creating a greenstick fracture anteriorly or a complete posterior cut, hinging on the intact posterior column.
- Acetabular Correction: The distal fragment (containing the acetabulum) is rotated laterally and anteriorly to provide increased coverage for the femoral head. A bone graft (from the iliac crest) is typically wedged into the osteotomy gap to maintain correction.
- Fixation: The osteotomy is stabilized with K-wires or cancellous screws crossing the osteotomy and anchoring the repositioned acetabular fragment to the stable posterior ilium.
- Wound Closure: Hemostasis, reattachment of muscle origins to the iliac crest, layered closure.
2. Equinus Deformity Correction: Achilles Tendon Z-Lengthening
This procedure corrects fixed equinus deformity, common in ambulators and non-ambulators. The goal is to achieve plantigrade foot position and facilitate dorsiflexion to neutral or slight dorsiflexion.
- Pre-operative Considerations: Clinical assessment of gastroc-soleus contracture vs. isolated gastroc. Consider a concomitant posterior capsulotomy if very severe bony equinus.
- Patient Positioning: Supine with a bolster under the ipsilateral hip for slight external rotation, or prone. A pneumatic tourniquet is applied to the proximal thigh.
-
Surgical Approach:
Medial or lateral longitudinal approach to the Achilles tendon.
- Incision: A longitudinal incision (typically 3-5 cm) is made along the medial or lateral border of the Achilles tendon, approximately 3-5 cm proximal to its insertion on the calcaneus. The internervous plane is in the subcutaneous tissue, avoiding major nerves/vessels. Protect the sural nerve (lateral incision) and posterior tibial neurovascular bundle (medial incision).
- Dissection: Incise skin and subcutaneous tissue. Identify the Achilles tendon. Retract the paratenon if possible.
-
Tenotomy (Z-Lengthening):
- Proximal Cut: A transverse cut is made through approximately 50% of the tendon width on one side (e.g., medial).
- Distal Cut: A transverse cut is made through approximately 50% of the tendon width on the opposite side (e.g., lateral), approximately 2-3 cm distal to the first cut.
- Longitudinal Split: The remaining central portion of the tendon is split longitudinally between the two transverse cuts, creating a Z-configuration.
- Lengthening: Gently dorsiflex the ankle to the desired position (neutral or 5-10 degrees of dorsiflexion). This allows the Z-lengthened tendon to slide and lengthen. The amount of lengthening should be carefully controlled to avoid over-lengthening, which can lead to a calcaneal gait.
- Repair: Suture the lengthened Z-plasty with non-absorbable sutures (e.g., Ethibond, Fiberwire) to maintain the corrected length. Ensure a smooth repair without knot impingement.
- Wound Closure: Hemostasis, layered closure of subcutaneous tissue and skin.
- Immobilization: Apply a short-leg cast with the ankle in neutral or slight dorsiflexion.
3. Posterior Spinal Fusion for Neuromuscular Scoliosis
Indicated for progressive curves >40-50 degrees or those causing functional decline in GMFCS Levels IV-V.
- Pre-operative Considerations: Neuromonitoring (SSEP, MEP) is mandatory. Blood loss management (tranexamic acid, cell saver). Pre-operative halo traction sometimes used for severe, rigid curves.
- Patient Positioning: Prone on a spinal frame (e.g., Jackson table) to allow for free abdominal movement, reducing venous congestion. Ensure adequate padding and secure endotracheal tube.
-
Surgical Approach:
Posterior midline approach to the spine.
- Incision: Midline skin incision extending from the upper instrumented vertebra (UIV) to the lower instrumented vertebra (LIV), often extending to the posterior superior iliac spine (PSIS) or even the greater trochanter for sacropelvic fixation.
- Dissection: Incise skin and subcutaneous tissue. The lumbodorsal fascia is incised longitudinally in the midline. Subperiosteal dissection proceeds laterally to expose the spinous processes, laminae, and facet joints bilaterally. Use Cobb elevators to strip muscle attachments (erector spinae, multifidus, rotatores) off the posterior elements. Hemostasis is critical.
- Exposure: Expose the posterior elements from the UIV to the LIV. For sacropelvic fixation, extend exposure to the sacrum and PSIS.
-
Instrumentation (Pedicle Screws):
- Pilot Holes: Carefully create pilot holes using an awl or drill, adhering to anatomical landmarks and trajectory rules. Pedicle morphology can be abnormal in CP, requiring careful palpation and sometimes fluoroscopic guidance.
- Screw Insertion: Insert appropriately sized pedicle screws into each instrumented vertebra. The choice of UIV and LIV is crucial. For neuromuscular scoliosis, fusion typically extends to the pelvis (S1/S2 alar-iliac screws) to address pelvic obliquity and prevent distal junctional kyphosis.
- Neuromonitoring: Constant vigilance and interpretation of neuromonitoring signals (EMG, SSEP, MEP) during screw placement to detect potential nerve root or spinal cord irritation.
- Decompression (if needed): For any associated spinal cord compression or neural impingement, laminectomy or facetectomy may be performed.
- Facetectomy/Decortication: Perform facetectomies (superior and inferior articular processes) to mobilize the spine and create raw bone surfaces for fusion. Decorticate the laminae and transverse processes to prepare a bed for bone graft.
- Rod Contouring and Placement: Contour two rigid rods (typically cobalt-chrome or titanium alloy) to the corrected spinal alignment, accommodating physiological kyphosis and lordosis. Insert the rods into the screw heads.
- Correction and Derotation: Apply compression, distraction, and segmental derotation maneuvers through the rod and screw constructs to achieve maximal correction of the deformity while maintaining spinal balance.
- Bone Grafting: Apply autogenous bone graft (from iliac crest or local decorticated bone) and/or allograft (demineralized bone matrix, cancellous chips) liberally over the decorticated posterior elements to promote solid fusion.
- Final Tightening: Ensure all set screws are securely tightened.
- Wound Closure: Thorough hemostasis, placement of a subfascial drain, layered closure of fascia, subcutaneous tissue, and skin.
Complications & Management
Complications following orthopaedic surgery in children with CP can be diverse, reflecting the complexity of their underlying condition and the extensive nature of the procedures. Proactive management and a high index of suspicion are essential.
| Complication | Incidence | Management Strategy |
|---|---|---|
| General Surgical Complications | ||
| Infection (SSI) | 2-10% (higher in CP patients due to malnutrition, altered immunity) |
- Superficial: Oral antibiotics, wound care.
- Deep: Surgical debridement, IV antibiotics, hardware removal (if persistent/chronic or involves infected pseudarthrosis). Culture-specific antibiotics. |
| Bleeding/Hematoma | Variable, often higher in spinal surgery (up to 20-30% requiring transfusion in scoliosis) |
- Intra-op: Meticulous hemostasis, tranexamic acid, cell saver.
- Post-op: Close monitoring, drain management. Re-exploration for uncontrolled bleeding. |
| DVT/PE | Low in children, but increased risk with prolonged immobilization, major surgery. |
- Prophylaxis: Early mobilization (where appropriate), pneumatic compression devices. Pharmacological prophylaxis (LMWH) for high-risk cases.
- Treatment: Anticoagulation (LMWH, Coumadin). |
| Anesthetic Complications | Higher in CP patients (respiratory compromise, aspiration risk, seizure, difficult airway) |
- Pre-op: Thorough anesthesia evaluation, optimize respiratory/cardiac status.
- Intra-op: Close monitoring, careful airway management, seizure precautions. |
| Pressure Sores/Skin Breakdown | Common with prolonged casting, immobility, poor nutrition. |
- Prevention: Meticulous padding, frequent repositioning, nutritional optimization.
- Treatment: Wound care, debridement, pressure relief, specialized mattresses. |
| Specific Complications | ||
| Hip Reconstruction (VDRO/Pelvic) | ||
| Avascular Necrosis (AVN) | 5-15% of femoral head, especially with extensive dissection or previous failed surgery. |
- Prevention: Meticulous surgical technique, preserve blood supply. Minimize capsular stripping.
- Treatment: Observation, protected weight-bearing. Surgical options (e.g., core decompression, osteotomy, arthroplasty) for severe cases and collapse. |
| Re-subluxation/Dislocation | 5-10%, higher in GMFCS IV-V, poor initial correction, non-compliance with post-op protocols. |
- Prevention: Achieving adequate initial reduction and coverage, meticulous surgical technique, appropriate post-op immobilization/bracing.
- Treatment: Revision surgery (re-osteotomy, revision pelvic osteotomy, salvage procedures like Girdlestone). |
| Hardware Complications | 5-10% (prominence, migration, breakage, loosening). |
- Symptomatic hardware removal after bone healing.
- Revision fixation for migration/breakage with loss of correction. |
| Limb Length Discrepancy (LLD) | Variable, especially after VDRO if non-union or over-shortening occurs. |
- Prevention: Careful surgical planning.
- Treatment: Shoe lift for small discrepancies. Epiphysiodesis or lengthening procedures for significant LLD if functional impact. |
| Achilles Tendon Lengthening | ||
| Over-lengthening (Calcaneal Gait) | 5-10% (more common with open Z-lengthening than percutaneous or isolated gastroc recession). |
- Prevention: Meticulous intra-operative assessment of length, aiming for neutral or slight dorsiflexion, never hyper-dorsiflexion.
- Treatment: AFOs for support. Tendon advancement or transfer of posterior tibial tendon or peroneus brevis to calcaneus for severe, persistent calcaneal deformity. |
| Recurrence of Equinus | 10-20%, higher in severe spasticity, non-compliance, growth spurts. |
- Prevention: Adequate initial lengthening, regular PT, AFO use, BoNT-A.
- Treatment: Repeat Achilles lengthening, serial casting, or BoNT-A. |
| Painful Scar/Adhesions | Uncommon but possible, especially with open approaches. |
- Prevention: Careful wound closure, gentle tissue handling.
- Treatment: Scar massage, silicone sheets. Surgical scar revision if severe and functional impact. |
| Spinal Fusion for Scoliosis | ||
| Neurological Deficit | 0.5-2%, higher with severe curves, revision surgery, or specific syndromes (e.g., tethered cord). |
- Prevention: Intraoperative neuromonitoring (SSEP, MEP), wake-up test (if feasible), careful correction maneuvers.
- Treatment: Immediate reversal of corrective maneuvers, steroid administration, emergent decompression. |
| Pseudarthrosis | 5-15%, higher in GMFCS V, osteopenia, poor nutrition, extensive fusion to pelvis. |
- Prevention: Meticulous decortication, adequate bone graft, stable instrumentation, post-op immobilization (if indicated).
- Treatment: Revision surgery with re-debridement, fresh bone graft (autograft), and often revision of instrumentation to achieve solid fusion. |
| Hardware Failure | 5-10%, often associated with pseudarthrosis, especially at the lumbosacral junction. |
- Prevention: Strong instrumentation constructs, fusion to pelvis, optimized bone quality.
- Treatment: Revision surgery, often involving removal of broken hardware, re-fusion, and stronger sacropelvic fixation (e.g., S2 alar-iliac screws). |
| Crankshaft Phenomenon | <5%, typically in young children with significant growth remaining through unfused anterior column. |
- Prevention: Posterior-anterior-posterior (PAP) fusion for young, rapidly growing patients; or combined anterior/posterior fusion.
- Treatment: Revision posterior fusion, possibly with anterior column release or fusion. |
| Proximal Junctional Kyphosis (PJK) | 5-15%, more common in CP due to fragile bone and muscle weakness above construct. |
- Prevention: Careful UIV selection, sagittal balance consideration, prophylactic laminar hooks/screws.
- Treatment: Observation for mild cases. Revision surgery (extension of fusion) for progressive PJK causing pain or functional decline. |
| Distal Junctional Kyphosis/Failure | Less common with sacropelvic fusion, but possible with inadequate distal fixation. |
- Prevention: Robust sacropelvic fixation (e.g., S2 alar-iliac screws).
- Treatment: Revision surgery with extension of fusion to include stable pelvic fixation. |
| Instrumentation Prominence | Common with large constructs and thin patients. |
- Prevention: Deep seating of hardware, appropriate implant size.
- Treatment: Elective hardware removal after solid fusion if symptomatic. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is an integral component of the surgical management of children with CP, aiming to optimize functional outcomes, prevent recurrence, and integrate the surgical correction into daily activities. Protocols are highly individualized based on the specific procedure(s) performed, the child's age, GMFCS level, and pre-existing functional status. A multidisciplinary team, including orthopaedic surgeons, physiatrists, physical therapists, and occupational therapists, guides this process.
General Principles of Post-Operative Care:
- Pain Management: Aggressive, multimodal pain management (opioids, NSAIDs, regional blocks, epidurals) is crucial to facilitate early mobilization and therapy participation.
- Wound Care: Daily inspection of surgical incisions and cast edges. Maintain cleanliness and monitor for signs of infection.
- Respiratory Care: Especially important for children with severe CP or following spinal surgery. Incentive spirometry, chest physiotherapy, and early mobilization to prevent atelectasis and pneumonia.
- Nutritional Support: Continue nutritional optimization to support healing.
- Psychosocial Support: Address patient and family psychological needs, as recovery can be prolonged and challenging.
Specific Protocols by Procedure Type:
1. Hip Reconstruction (VDRO & Pelvic Osteotomy)
-
Immobilization:
- Duration: Typically 6-8 weeks in a hip spica cast (double hip spica if bilateral) or an abduction brace. The cast maintains the hip in a position of stability (flexion, abduction, slight internal rotation).
- Cast Care: Regular checks for pressure points, skin irritation, and fit.
- Weight-Bearing: Non-weight-bearing (NWB) or touch-down weight-bearing (TDWB) on the operative leg for the duration of immobilization.
-
Physical Therapy (Post-Cast Removal):
- Weeks 6-12: Gentle passive and active-assisted range of motion (ROM) exercises. Focus on regaining hip flexion, abduction, and rotation without stressing the osteotomy sites. Initiate isometric strengthening of hip abductors and extensors. Gentle transfers and bed mobility.
- Months 3-6: Progressive weight-bearing with assistive devices (walker, crutches). Gait training with emphasis on correct limb alignment. Continue strengthening exercises for hip musculature and core stability. Gradual return to activities within limits.
- Long-Term: Maintenance of ROM and strength. Close monitoring for recurrence or complications. Bracing (abduction brace) may be continued at night for several months or years, particularly in GMFCS Levels IV-V.
2. Achilles Tendon Z-Lengthening
-
Immobilization:
- Duration: 4-6 weeks in a short-leg cast or controlled ankle motion (CAM) boot with the ankle in neutral or slight dorsiflexion.
- Cast Care: Similar to hip spica.
-
Weight-Bearing:
- In Cast: Typically weight-bearing as tolerated in the cast if the procedure was isolated. NWB if multi-level surgery.
-
Physical Therapy (Post-Cast Removal):
- Weeks 4-8: Gentle ankle ROM exercises, emphasizing controlled dorsiflexion to prevent re-contracture without overstretching. Progressive strengthening of ankle dorsiflexors.
- Weeks 8-12: Gait training with an emphasis on heel-strike pattern. Fitting for ankle-foot orthosis (AFO) or dynamic AFO (DAFO) to maintain correction, provide support, and prevent recurrence.
- Long-Term: Continued use of AFOs as prescribed. Regular stretching, strengthening, and functional activities. Surveillance for recurrence of equinus, especially during growth spurts.
3. Posterior Spinal Fusion for Neuromuscular Scoliosis
-
Immobilization:
- Bracing: Post-operative bracing (TLSO) is controversial and surgeon-dependent. Some surgeons use it for 3-6 months, especially in GMFCS V patients with osteopenia, while others advocate early mobilization without a brace.
-
Weight-Bearing/Mobilization:
- Day 1-3 (ICU/Acute Care): Log-rolling for repositioning. Respiratory therapy. Begin sitting at the edge of the bed with assistance.
- Week 1-2: Progressive increase in sitting tolerance. Begin standing with maximal assistance or in a standing frame. Transfers. Gentle upper extremity ROM. Avoid excessive twisting or bending of the trunk.
- Weeks 2-6: Progress to ambulation with assistive devices (if applicable) or independent transfers/standing. Core strengthening (without spinal loading).
- Months 3-6: Gradual increase in activity level. Strengthening of trunk musculature. Resumption of light recreational activities. Avoid contact sports or heavy lifting for 6-12 months.
-
Physical Therapy:
- Focus on trunk stability, balance, transfers, and functional mobility based on the child's GMFCS level.
- Education on proper body mechanics and lifting techniques for caregivers.
- Long-term follow-up for fusion assessment and potential complications (e.g., PJK, hardware prominence).
Single-Event Multi-Level Surgery (SEMLS)
- Considerations: Rehabilitation after SEMLS is complex due to multiple sites of surgical intervention. Protocols are often a combination of the above, tailored to the specific procedures.
- Goal: Achieve maximal functional improvement with minimal surgical episodes.
- Intensity: Requires highly intensive and coordinated therapy input, often necessitating inpatient rehabilitation.
- Timing: Therapy typically begins as soon as medically stable, adapting to casting/bracing and pain levels.
Regular follow-up with the orthopaedic surgeon, physiatrist, and therapists is crucial to monitor progress, adjust protocols, and identify/manage any developing complications or recurrences. The ultimate goal is to integrate surgical corrections into the child's overall developmental and functional trajectory.
Summary of Key Literature / Guidelines
The management of orthopaedic problems in children with CP is continuously evolving, guided by evidence-based research and expert consensus. Key literature and guidelines inform best practices.
1. Hip Surveillance and Management:
- Early Detection is Key: The natural history of hip displacement in CP, particularly in GMFCS Levels III-V, is progressive and leads to pain, functional loss, and caregiver burden. Hip surveillance programs, often based on the Swedish CPUP program , have demonstrated efficacy in reducing the incidence of hip dislocation.
- Guidelines: The American Academy for Cerebral Palsy and Developmental Medicine (AACPDM) provides clinical practice guidelines endorsing routine hip surveillance for all children with CP, commencing from early childhood. This involves regular physical examinations and radiographic assessment (AP pelvis radiograph with Reimers Migration Percentage (MP)) every 6-12 months, depending on GMFCS level and age.
- Intervention Thresholds: MP >33% generally indicates the need for intervention, starting with non-operative measures (BoNT-A, PT, abduction orthoses) for dynamic subluxation. MP >40-50% or progressive subluxation despite non-operative management often necessitates surgical intervention (e.g., adductor/psoas releases, VDRO, pelvic osteotomies). MP >90% (frank dislocation) in older children may require more complex reconstruction or salvage procedures.
- Literature: Landmark studies by Hagglund et al. (Sweden) and others have provided long-term data on the effectiveness of surveillance and early intervention.
2. Management of Lower Extremity Deformities (Gait Disorders):
- Single-Event Multi-Level Surgery (SEMLS): A cornerstone of surgical management for ambulant children with CP (GMFCS I-III). SEMLS involves addressing multiple deformities (e.g., hip flexion, knee flexion, equinus) concurrently during one surgical episode.
- Evidence for SEMLS: Numerous studies, often utilizing 3D instrumented gait analysis, have shown that SEMLS leads to superior and more sustainable functional improvements (e.g., improved gait kinematics, reduced energy expenditure, better walking speed) compared to staged procedures.
- Gait Analysis: Gait laboratories play a critical role in pre-operative planning and post-operative assessment for ambulant children, providing objective data to guide surgical decision-making and evaluate outcomes.
- Literature: Research by authors such as Delp, Gorton, and Shore has extensively explored the biomechanics of CP gait and the role of SEMLS. The European Society for Movement Analysis in Adults and Children (ESMAC) and Gait and Clinical Movement Analysis Society (GCMAS) provide guidelines for gait analysis methodology.
3. Management of Neuromuscular Scoliosis:
- Indications for Surgery: Progressive curves >40-50 degrees, loss of sitting balance, pain, pulmonary compromise, or difficulties with personal care are primary indications for surgical correction and fusion.
- Fusion to the Pelvis: For most GMFCS Levels IV-V patients with significant pelvic obliquity, fusion to the pelvis (typically S2 alar-iliac fixation) is recommended to achieve stable sitting balance and correct pelvic obliquity. This is critical for preventing distal junctional problems and allowing proper seating.
- Complications: Neuromuscular scoliosis surgery carries higher complication rates (infection, pseudarthrosis, neurological deficits) compared to idiopathic scoliosis due to patient comorbidities and often larger, more rigid curves.
- Literature: Studies by O'Brien et al., Newton et al., and the Pediatric Orthopaedic Society of North America (POSNA) have contributed significantly to understanding the complexities and outcomes of neuromuscular scoliosis surgery. The use of intraoperative neuromonitoring (SSEP, MEP) has become standard practice.
4. Upper Extremity Management:
- Goals: Focus on improving functional grasp, release, hygiene, and self-care.
- Treatment Continuum: Ranges from splinting, occupational therapy, BoNT-A injections to surgical options like tendon lengthenings, transfers (e.g., pronator teres rerouting), and occasionally osteotomies for fixed bony deformities.
- Literature: Contributions from medical societies like AACPDM and POSNA provide guidance on evidence-based approaches for upper extremity interventions.
5. General Principles and Future Directions:
- Multidisciplinary Approach: Consensus guidelines consistently emphasize the necessity of a coordinated multidisciplinary team for comprehensive patient care, from diagnosis to long-term follow-up.
- Evidence-Based Practice: Continued research focusing on long-term outcomes, cost-effectiveness of interventions, and development of patient-reported outcome measures (PROMs) is crucial.
- Technological Advances: Ongoing advancements in surgical techniques, instrumentation, imaging (e.g., low-dose biplanar radiography), and rehabilitation technologies continue to refine treatment paradigms.
- Registries: National and international registries (e.g., CPUP, various scoliosis registries) are vital for collecting large-scale, long-term data to assess treatment effectiveness and identify risk factors.
The prevailing philosophy in orthopaedic management of CP is early, individualized, and goal-directed intervention, integrating both non-operative and operative strategies to maximize functional independence and quality of life throughout the patient's lifespan.
You Might Also Like