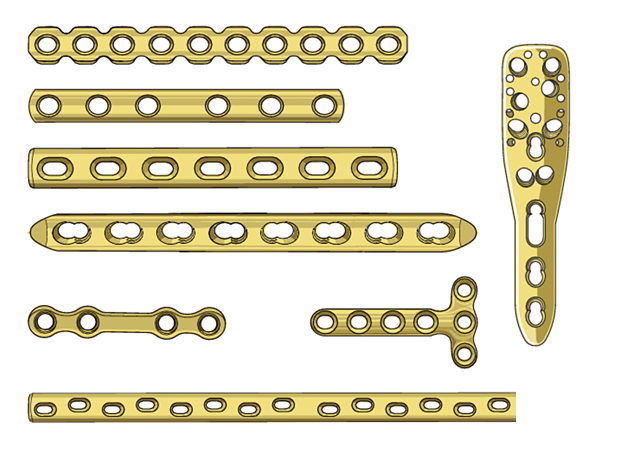
Submuscular Minimally Invasive Locking Condylar Plate Application: A Comprehensive Surgical Guide
Key Takeaway
The submuscular minimally invasive locking condylar plate application is a premier technique for managing complex distal femur fractures. By utilizing a biological osteosynthesis approach, surgeons can preserve the metaphyseal fracture hematoma while providing robust, angle-stable fixation. This guide details the critical steps of articular reduction, submuscular plate insertion, coronal and sagittal alignment, and optimal screw configuration to prevent malunion and hardware failure.
INTRODUCTION TO MINIMALLY INVASIVE PLATE OSTEOSYNTHESIS (MIPO)
The evolution of distal femur fracture management has fundamentally shifted from extensive, biologically taxing open exposures to Minimally Invasive Plate Osteosynthesis (MIPO). The submuscular minimally invasive locking condylar plate application represents the pinnacle of this biological approach. By preserving the delicate extraosseous blood supply and the metaphyseal fracture hematoma, surgeons can achieve reliable union in complex, comminuted fracture patterns (AO/OTA 33-A and 33-C).
This technique leverages the biomechanical principles of an "internal-external fixator." Unlike conventional plating, which relies on absolute friction between the plate and the bone, locking plate constructs provide angle-stable fixation. This allows the plate to sit off the bone, preserving periosteal perfusion while delivering unparalleled stability in osteoporotic bone and highly comminuted metaphyseal segments.
PREOPERATIVE PLANNING AND TEMPLATING
Thorough preoperative planning is the cornerstone of successful MIPO. Because the fracture site is not directly visualized, the surgeon must rely heavily on preoperative templating and intraoperative fluoroscopy to restore length, alignment, and rotation.
Imaging Requirements
Standard anteroposterior (AP) and lateral radiographs of the affected femur and knee are mandatory. Furthermore, a computed tomography (CT) scan with sagittal and coronal reconstructions is highly recommended for any fracture involving the articular block (AO/OTA 33-C). CT imaging is critical for identifying coronal plane fractures (Hoffa fractures) and severe intercondylar comminution that may dictate the sequence of articular reconstruction.
Contralateral Templating
Close scrutiny of contralateral knee radiographs facilitates the identification of anatomical nuances. Preoperative templating on the uninjured limb allows the surgeon to determine the appropriate plate length, anticipate the required working length, and select the optimal screw trajectory.
Clinical Pearl: Beware of anatomical variances, such as a hypoplastic lateral condyle. A hypoplastic condyle alters the normal valgus angle of the distal femur. Failure to recognize this during templating can make reconstruction and implant positioning exceedingly difficult, often resulting in iatrogenic varus or valgus malalignment.
BIOMECHANICAL PRINCIPLES OF LOCKING PLATES
Understanding the biomechanics of locking condylar plates is essential for construct optimization. The goal is to achieve relative stability at the metaphyseal fracture site to promote secondary bone healing via callus formation, while maintaining absolute stability at the articular block.
The "Internal-External Fixator" Concept
Many periarticular plates do not perfectly match every patient’s unique anatomy, resulting in a variable offset of the plate from the femoral shaft. If threaded reduction instrumentation or nonlocking cortical screws are used to forcefully seat the plate to the bone, the bone will be drawn to the plate, inadvertently inducing a varus or valgus malalignment. When an offset is identified, the plate must be applied strictly as an "internal-external fixator," utilizing locking screws to maintain the anatomically reduced coronal plane without deforming the bone.
Construct Rigidity and Working Length
Ideally, a long plate construct with well-spaced fixation is sought. The "working length" is the distance between the closest screws on either side of the fracture.
Surgical Warning: Locking screw fixation placed in excessively close proximity to metaphyseal comminution drastically decreases the working length. This results in a highly rigid construct that concentrates stress, limits interfragmentary strain, and contributes to inconsistent callus formation, ultimately leading to nonunion or implant failure.
PATIENT POSITIONING AND PREPARATION
Meticulous patient positioning is critical to facilitate unhindered fluoroscopic imaging and to assist in the indirect reduction of the fracture.
- Table and Patient Orientation: Position the patient supine on a fully radiolucent table. Ensure that the C-arm can freely arc 180 degrees to obtain perfect AP and lateral views of the entire femur.
- Limb Positioning: Place a well-padded bump under the ipsilateral hip. This elevates the hemipelvis and maintains the femur in neutral rotation, counteracting the natural tendency of the lower limb to externally rotate.
- Knee Support: Position the injured limb on a sterile bump or a triangular bolster. Flexing the knee to approximately 30 to 40 degrees relaxes the deforming force of the gastrocnemius muscle, which typically pulls the distal articular fragment into extension (recurvatum).
- Draping: Prepare and drape the limb in the standard sterile fashion, ensuring the iliac crest is accessible if autologous bone grafting is anticipated.
SURGICAL APPROACH
The surgical approach is dictated by the fracture pattern. The objective is to achieve absolute anatomical reduction of the articular surface while leaving the metaphyseal comminution undisturbed.
Lateral Parapatellar Arthrotomy
For intra-articular fractures (AO/OTA 33-C), expose the distal femur using the distal extent of a lateral parapatellar arthrotomy. This approach provides excellent visualization of the articular surface, allowing for direct reduction of the condyles.
Direct Lateral Approach
Alternatively, a direct lateral approach may be utilized for extra-articular fractures (AO/OTA 33-A) or those with very simple, non-displaced articular components. This approach minimizes disruption to the extensor mechanism while providing adequate access for plate insertion.
STEP-BY-STEP SURGICAL TECHNIQUE
1. Articular Reduction
The foundation of distal femur fracture fixation is the anatomical reconstruction of the articular block.
* Clean the fracture hematoma from the intra-articular split.
* Reduce the condylar fragments anatomically using pointed reduction forceps.
* Provisionally stabilize the condyles with multiple Kirschner wires (K-wires). Ensure these wires are placed peripherally so they do not interfere with the subsequent trajectory of the locking plate screws.
* Place the condylar plate guide on the lateral cortex. This helps determine the proper position for the placement of independent interfragmentary lag screws, ensuring they maintain the condylar reduction without obstructing the path of the plate.
2. Submuscular Plate Insertion
- Using anatomical landmarks and continuous C-arm imaging, slide the selected locking condylar plate in a submuscular, extraperiosteal fashion proximally along the lateral femoral shaft.
- Do not attempt to reduce the proximal diaphyseal fragments at this stage; the goal is simply to position the plate over the reconstructed condyles.
3. Establishing Coronal Plane Alignment
- Insert a 2.5-mm guidewire through the central hole of the wire guide, aiming parallel to the femorotibial joint line.
- Obtain an AP fluoroscopic image to confirm perfectly parallel placement.
Pitfall: For this portion of the procedure, wire placement is absolutely critical because it "sets" the distal position of the plate in the coronal plane. Nonparallel positioning of this initial reference wire will inadvertently induce a varus or valgus coronal plane malalignment once the plate is secured to the shaft.
4. Establishing Sagittal Plane Alignment
- Switch to the lateral fluoroscopic plane.
- Confirm that the distal positioning of the plate parallels the posterior cortex of the femur. This ensures appropriate sagittal plane alignment, preventing iatrogenic flexion or extension deformities.
- Once appropriate positioning is confirmed in both planes, place additional guidewires through the locking guides to provisionally secure the plate to the distal articular segment.
5. Restoring Length, Alignment, and Rotation
- Apply longitudinal traction to the limb.
- Use the targeting instrumentation to permit the placement of a provisional guidewire in the most proximal hole of the chosen plate.
- CRITICAL STEP: It is imperative that the length and rotational reduction be meticulously assessed before proceeding. Compare the rotation to the uninjured leg (if draped) or utilize the cortical step sign and lesser trochanter profile on fluoroscopy.
- In particularly comminuted fractures of the distal femoral metaphysis, a single proximal wire may not provide sufficient length maintenance. Additional provisional fixation or external distractors may be required.
- Once length and rotational alignment are "set," place a small bolster under the metaphyseal portion of the fracture to fine-tune sagittal flexion and extension.
6. Screw Insertion Sequence
Locking screws can technically be inserted in any order, but a systematic approach ensures construct stability and prevents displacement.
* Distal Fixation: It is usually best to insert the 7.3-mm central locking screw first. Follow this with the surrounding 5.0-mm cannulated locking screws into the distal articular segment. Ensure adequate spread of screws to capture both the anterior and posterior aspects of the condyles.
* Proximal Fixation: Proximal fixation is achieved with the placement of 4.5-mm cortical screws or 5.0-mm locking cortical screws through the targeting instrumentation. A minimum of eight cortices (four bicortical screws) should be obtained proximally to ensure adequate pull-out strength.
7. Mitigating Stress Risers
Take extreme care when placing proximal fixation into the diaphyseal shaft. The transition from the rigid plate to the flexible native bone creates a significant stress riser, which is a common site for periprosthetic fractures.
* Consider filling the most proximal hole in the construct with a unicortical locking screw or a bicortical nonlocking screw. This technique gradually decreases the stiffness of the construct, smoothing the biomechanical transition and minimizing stress riser formation.
8. Final Verification and Closure
- Obtain final AP and lateral fluoroscopic images to confirm fracture reduction, plate position, and screw length. Ensure no screws are penetrating the intercondylar notch or the patellofemoral joint.
- Securely tighten all screws using the appropriate torque-limiting screwdriver before wound closure.
- Perform fascial and skin closure in the standard fashion, ensuring meticulous hemostasis.
LESS INVASIVE STABILIZATION SYSTEM (LISS)
The Less Invasive Stabilization System (LISS) is a specialized variant of the locking condylar plate. While the application technique is in many respects very similar to the standard MIPO technique described above, several key biomechanical and structural differences must be highlighted.
Material and Modulus of Elasticity
The LISS system is constructed entirely of titanium alloy, whereas many standard locking condylar plates are manufactured from stainless steel. Titanium possesses a lower modulus of elasticity, making it significantly more flexible. This increased flexibility promotes greater interfragmentary strain at the fracture site, which is highly conducive to secondary bone healing and robust callus formation.
Reduction Philosophy
Whereas the design of many standard locking condylar plates allows for limited plate-to-bone reduction techniques (using non-locking screws to pull bone to the plate), the LISS system strictly relies on the reduction being achieved before implant positioning.
Unicortical Fixation
The LISS truly functions as an "internal-external fixator." Fixation with locking screws placed near and far from the fracture provides the greatest stability. Because of the increased flexibility of the titanium LISS plate, this wide-span fixation is better tolerated compared to stiffer stainless steel plates. Furthermore, the diaphyseal screw fixation in the LISS system is designed to be solely unicortical. These self-drilling, self-tapping unicortical locking screws provide excellent pull-out strength while minimizing damage to the medullary blood supply.
POSTOPERATIVE CARE AND REHABILITATION
The postoperative protocol must balance the need for early joint mobilization with the protection of the metaphyseal fracture site.
- Early Mobilization: Early passive motion, supplemented with active-assisted motion, is begun immediately postoperatively as tolerated by the patient.
- Extension Focus: Particular focus is placed on passive extension exercises. The knee is highly prone to flexion contracture formation following distal femur trauma, and achieving full terminal extension early is critical for normal gait mechanics.
- Weight-Bearing Restrictions: Because MIPO relies on relative stability and secondary bone healing, the construct must be protected from full axial loading until bridging callus is visible. Weight-bearing is strictly avoided (Non-Weight Bearing - NWB) for 10 to 12 weeks.
- Continuous Monitoring: Active and passive range of motion should be aggressively encouraged during this non-weight-bearing period. Serial radiographs are obtained at 2, 6, and 12 weeks to monitor alignment, hardware integrity, and the progression of callus formation. Progression to partial and full weight-bearing is dictated by radiographic evidence of union.
CONCLUSION
The submuscular minimally invasive locking condylar plate application is a highly sophisticated, biologically friendly technique that has revolutionized the treatment of distal femur fractures. By adhering strictly to the principles of anatomical articular reduction, meticulous coronal and sagittal alignment, and optimized construct working length, orthopedic surgeons can minimize complications such as nonunion and hardware failure. Whether utilizing a standard locking condylar plate or the titanium LISS system, mastery of this technique is an essential component of the modern orthopedic trauma surgeon's armamentarium.
📚 Medical References
- [: technique guide, Paoli, Penn, 2001, Synthes.
Lotke PA, Ecker ML: Transverse fractures of the patella, Clin Orthop Relat Res 158:180, 1981.](https://pubmed.ncbi.nlm.nih.gov/?term=%3A%20technique%20guide%2C%20Paoli%2C%20Penn%2C%202001%2C%20Synthes.%0A%0ALotke%20PA%2C%20Ecker%20ML%3A%20Transverse%20fractures%20of%20the%20patella%2C%20Clin%20Orthop%20Relat%20Res%20158%3A180%2C%201981.)
- Lottes JO, Key JA: Complications and errors in technic in medullary nailing for fractures of the femur, Clin Orthop Relat Res 2:38, 1953.
- Lund B, Sørensen OH, Lund B, et al: Vitamin D metabolism and osteomalacia in patients with fractures of the proximal femur, Acta Orthop Scand 53:251, 1982.
- MacAusland WR Jr, Eaton RG: The management of sepsis following intramedullary fi xation for fractures of the femur, J Bone Joint Surg 45A:1643, 1963.
- MacNamee PB, Bunker TD, Scott TD: The Herbert screw for osteochondral fractures: brief report, J Bone Joint Surg 70B:145, 1988.
- Maffulli N, Yip KM, Cowman JE, et al: Ender nailing for ipsilateral femoral shaft fractures after Austin-Moore hemiarthroplasty, J Trauma 42:20, 1997.
- Magerl F, Wyss A, Brunner C, et al: Plate osteosynthesis of femoral shaft fractures in adults: a follow-up study, Clin Orthop Relat Res 138:62, 1979.
- Malkani AL, Helfet DL: Blade-plate fi xation of supracondylar femur fractures, Tech Orthop 9:203, 1995.
- Mariani EM, Rand JA: Nonunion of intertrochanteric fractures of the femur following open reduction and internal fi xation: results of second attempt to gain union, Clin Orthop Relat Res 218:81, 1987.
- Markmiller M, Konrad G, Südkamp N: Femur-LISS and distal femoral nail for fi xation of distal femoral fractures: are there differences in outcome and complications, Clin Orthop Relat Res 426:252, 2004.
- Marsh JL, Smith ST, Do TT: External fi xation and limited internal fi xation for complex fractures of the tibial plateau, J Bone Joint Surg 77A:661, 1995.
- Marti A, Fankhauser C, Frenk A, et al: Biomechanical evaluation of the less invasive stabilization system for the internal fi xation of distal femur fractures, J Orthop Trauma 15:482, 2001.
- Martinet O, Cordey J, Harder Y, et al: The epidemiology of fractures of the distal femur, Injury 31:C62, 2000.
- McClelland SJ, Bauman PA, Medley CF Jr, et al: Obturator
You Might Also Like