Pediatric Orthopaedic Scored And Re Review | Dr Hutaif - ...
14 Apr 2026
50 min read
85 Views
Key Takeaway
This interactive board review contains 100 randomly selected orthopedic surgery questions with clinical images, immediate feedback, and detailed references.
Pediatric Orthopaedic Scored And Re Review | ...
00:00
Start Quiz
Question 1High Yield
A 36-year-old woman dislocated her elbow 6 months ago. The elbow was congruently reduced and rehabilitated. She continues to have a sense of painful clunking in her elbow when she pushes up from a chair with forearm supination, but not pronation. What structure did not heal properly?
Explanation
The patient is showing signs of posterolateral rotatory instability after elbow dislocation. The lateral ulnar collateral ligament is responsible for stabilizing the elbow against this type of instability. The posterior and anterior bands of the medial collateral ligament are primarily resistors of valgus load, with the anterior band being the most significant contributor. The radial collateral ligament does not control the posterolateral rotatory instability described.
Question 2High Yield
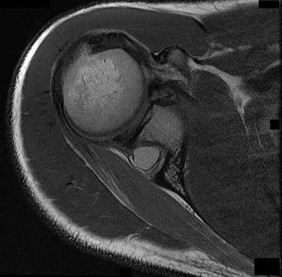
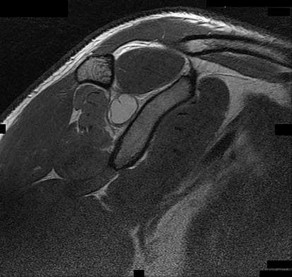
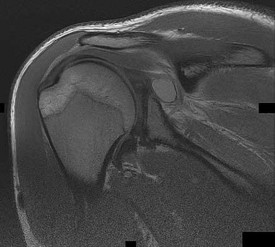
The cystic lesion shown on the MR images in Figures 46a through 46c should cause denervation changes in which muscle?
A B
A B
Explanation
The cystic lesion is shown in an area adjacent to the spinoglenoid notch. A space-occupying lesion in this area has the potential to compress the suprascapular nerve as it passes through the spinoglenoid notch to innervate the infraspinatus. Compression of the nerve can cause denervation and atrophy of the infraspinatus muscle. The supraspinatus is innervated by the suprascapular nerve proximal to the compressive lesions and will not undergo atrophy. The subscapularis and the teres major are innervated by the subscapular nerve.
RECOMMENDED READINGS
1. Getz CL, Ramsey ML, Williams GR. Paralabral cysts of the shoulder. In: Galatz LM, ed. Orthopaedic Knowledge Update: Shoulder and Elbow 3. Rosemont, IL: American Academy of Orthopaedic Surgeons; 2008:339-344.
2. [Takagishi K, Saitoh A, Tonegawa M, Ikeda T, Itoman M. Isolated paralysis of the infraspinatus muscle. J Bone Joint Surg Br. 1994 Jul;76(4):584-7. PubMed PMID: 8027145.](http://www.ncbi.nlm.nih.gov/pubmed/8027145)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/8027145)
RECOMMENDED READINGS
1. Getz CL, Ramsey ML, Williams GR. Paralabral cysts of the shoulder. In: Galatz LM, ed. Orthopaedic Knowledge Update: Shoulder and Elbow 3. Rosemont, IL: American Academy of Orthopaedic Surgeons; 2008:339-344.
2. [Takagishi K, Saitoh A, Tonegawa M, Ikeda T, Itoman M. Isolated paralysis of the infraspinatus muscle. J Bone Joint Surg Br. 1994 Jul;76(4):584-7. PubMed PMID: 8027145.](http://www.ncbi.nlm.nih.gov/pubmed/8027145)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/8027145)
Question 3High Yield
A 50-year-old man who underwent an arthroscopic rotator cuff repair 5 days ago now returns for an early postoperative follow-up because of increasing pain in his shoulder. He reports increasing malaise and has a low-grade fever. Examination reveals no redness or swelling, but he has scant serous drainage from the posterior portal. An emergent Gram stain is positive for gram-positive cocci. The next most appropriate step in management should consist of
Explanation
An infection of the shoulder is considered a surgical emergency unless there are medical reasons that a patient cannot be taken to the operating room. If cultures of wound drainage are in question, then an aspiration should be done emergently, not several days later. The hallmark of infection in any major joint is increasing pain out of proportion to what is expected. Drainage occurring 1 to 2 days after an arthroscopic procedure is not normal, and it should be aggressively treated. Delay in diagnosis can result in sepsis and on a delayed basis, postinfectious arthritis. Both the glenohumeral joint and the subacromial space require debridement and irrigation, followed by antibiotics after both areas are cultured.
REFERENCES: Mansat P, Cofield RH, Kersten TE, Rowland CM: Complications of rotator cuff repair. Orthop Clin North Am 1997;28:205-213.
Settecerri JJ, Pitner MA, Rock MG, Hanssen AD, Cofield RH: Infection after rotator cuff repair. J Shoulder Elbow Surg 1999;8:1-5.
Ward WG, Eckardt JJ: Subacromial/subdeltoid bursa abscesses: An overlooked diagnosis. Clin Orthop 1993;288:189-194.
Ward WG, Goldner RD: Shoulder pyarthrosis: A concomittant process. Orthopedics 1994;17:591-595.
REFERENCES: Mansat P, Cofield RH, Kersten TE, Rowland CM: Complications of rotator cuff repair. Orthop Clin North Am 1997;28:205-213.
Settecerri JJ, Pitner MA, Rock MG, Hanssen AD, Cofield RH: Infection after rotator cuff repair. J Shoulder Elbow Surg 1999;8:1-5.
Ward WG, Eckardt JJ: Subacromial/subdeltoid bursa abscesses: An overlooked diagnosis. Clin Orthop 1993;288:189-194.
Ward WG, Goldner RD: Shoulder pyarthrosis: A concomittant process. Orthopedics 1994;17:591-595.
Question 4High Yield
Nerve conduction velocity is slowed by
Explanation
A number of factors affect nerve conduction velocity; for example, increased body temperature increases nerve conduction velocity. Nerve conduction velocity is slowed by advancing age, compression, decreased blood flow, and fibrosis (from large imprecise sutures used for nerve repair). There is no association between hand dominance and nerve conduction velocity.
RECOMMENDED READINGS
57. Dodds SD. Peripheral Nervous System. In Boyer MI, ed. AAOS Comprehensive Orthopaedic Review. Vol 1. 2nd ed. Rosemont, IL: American Academy of Orthopaedic Surgeons; 2014:113-126.
58. Freedman M, Helber G, Pothast J, Shahwan TG, Simon J, Sher L. Electrodiagnostic evaluation of compressive nerve injuries of the upper extremities. Orthop Clin North Am. 2012 Oct;43(4):409-16. doi:10.1016/j.ocl.2012.07.010. Epub 2012 Sep 10. Review. PubMed PMID: 23026456.
59. Lundborg G. A 25-year perspective of peripheral nerve surgery: evolving neuroscientific concepts and clinical significance. J Hand Surg Am. 2000 May;25(3):391-414. Review. PubMed PMID: 10811744.
RECOMMENDED READINGS
57. Dodds SD. Peripheral Nervous System. In Boyer MI, ed. AAOS Comprehensive Orthopaedic Review. Vol 1. 2nd ed. Rosemont, IL: American Academy of Orthopaedic Surgeons; 2014:113-126.
58. Freedman M, Helber G, Pothast J, Shahwan TG, Simon J, Sher L. Electrodiagnostic evaluation of compressive nerve injuries of the upper extremities. Orthop Clin North Am. 2012 Oct;43(4):409-16. doi:10.1016/j.ocl.2012.07.010. Epub 2012 Sep 10. Review. PubMed PMID: 23026456.
59. Lundborg G. A 25-year perspective of peripheral nerve surgery: evolving neuroscientific concepts and clinical significance. J Hand Surg Am. 2000 May;25(3):391-414. Review. PubMed PMID: 10811744.
Question 5High Yield
According to the MRI scan shown in Figure 1, which pathologic finding is expected to be encountered during arthroscopy?
Explanation
images show a flap tear of the medial meniscus (Figure 2), anterior cruciate ligament tear (Figure 3), and a full thickness articular cartilage defect (Figure 5). Other less likely causes of a double PCL sign include intermeniscal ligament, meniscofemoral ligaments, loose bodies, osteophytes, and fracture fragments.
13
13
Question 6High Yield
Which of the following is a true statement regarding the results of surgery for a contracted joint in arthrogryposis:
Explanation
The beginning and end of the range may change, but the total amount of motion remains about the same.
The amount of the range cannot be significantly increased. The endpoint can change, but not the amount of the range. The joint does not usually become stiffer.
There may be an indication for surgery to put the joints in a functional position.
The amount of the range cannot be significantly increased. The endpoint can change, but not the amount of the range. The joint does not usually become stiffer.
There may be an indication for surgery to put the joints in a functional position.
Question 7High Yield
What type of injury is considered the major mechanism of cervical fracture, dislocation, and quadriplegia in contact sports and diving?
Explanation
A compression or burst injury occurs with vertical loading of the spine, such as from a blow to the vertex with the neck flexed (eg, spear tackling in football). This leads to vertebral end plate fractures before disk injury. At higher forces, the entire vertebra and disk may explode into the spinal canal. Analysis has shown this to be the major mechanism of cervical fracture, dislocation, and quadriplegia. With the normal head-up posture, the cervical spine has a gentle lordotic curve, and forces transmitted to the head are largely dissipated in the cervical muscles. When the neck is flexed, the cervical spine becomes straight, with the vertebral bodies lined up under one another. This allows for minimal dissipation of the impact forces to be absorbed by the neck muscles.
REFERENCES: Cantu RC: Head and spine injuries in youth sports. Clin Sports Med 1995;14:517-532.
Proctor MR, Cantu RC: Head and neck injuries in young athletes. Clin Sports Med 2000;19:693-715.
Torg JS: Epidemiology, pathomechanics, and prevention of athletic injuries to the cervical spine. Med Sci Sports Exerc 1985;17:295-303.
REFERENCES: Cantu RC: Head and spine injuries in youth sports. Clin Sports Med 1995;14:517-532.
Proctor MR, Cantu RC: Head and neck injuries in young athletes. Clin Sports Med 2000;19:693-715.
Torg JS: Epidemiology, pathomechanics, and prevention of athletic injuries to the cervical spine. Med Sci Sports Exerc 1985;17:295-303.
Question 8High Yield
Which of the following is a significant side effect of biphosphonates (e.g., alendronate):
Explanation
The most significant side effect of biphosphonates is esophagitis and dyspepsia. Biphosphonates must be taken on an empty stomach with no oral intake for 30 minutes. In addition, patients should remain upright
Question 9High Yield
A 25-year-old man underwent a Putti-Platt repair for recurrent anterior dislocation of his right shoulder 9 months ago. He reports no further episodes of instability but continues to have severely restricted motion, with external rotation limited to less than 0 degrees with the arm at the side. He has pain at the ends of range of motion and restricted activities of daily living despite undergoing nearly 9 months of physical therapy. Radiographs of the shoulder show no arthritic changes. Management should now consist of
Explanation
Open release allows lengthening of the shortened subscapularis and is preferred when there are extra-articular contractures. Arthroscopic release, combined with the use of an interscalene catheter postoperatively, is an excellent treatment for capsular contractures but is contraindicated after procedures that result in extracapsular shortening (ie, Magnuson-Stack, Putti-Platt). Additional physical therapy or manipulation under anesthesia is not likely to be helpful. Shoulder hemiarthroplasty is contraindicated with normal articular surfaces, but prosthetic arthroplasty is sometimes necessary for arthritis associated with instability or overly tight instability repairs.
REFERENCES: Harryman DT II, Matsen FA III, Sidles JA: Arthroscopic management of refractory shoulder stiffness. Arthroscopy 1997;13:133-147.
Warner JJ: Frozen shoulder: Diagnosis and management. J Am Acad Orthop Surg 1997;5:130-140.
Warner JJ, Allen AA, Marks PH, Wong P: Arthroscopic release of postoperative capsular contracture of the shoulder. J Bone Joint Surg Am 1997;79:1151-1158.
MacDonald PB, Hawkins RJ, Fowler PJ, Miniaci A: Release of the subscapularis for internal rotation contracture and pain after anterior repair for recurrent anterior dislocation of the shoulder. J Bone Joint Surg Am 1992;74:734-737.
REFERENCES: Harryman DT II, Matsen FA III, Sidles JA: Arthroscopic management of refractory shoulder stiffness. Arthroscopy 1997;13:133-147.
Warner JJ: Frozen shoulder: Diagnosis and management. J Am Acad Orthop Surg 1997;5:130-140.
Warner JJ, Allen AA, Marks PH, Wong P: Arthroscopic release of postoperative capsular contracture of the shoulder. J Bone Joint Surg Am 1997;79:1151-1158.
MacDonald PB, Hawkins RJ, Fowler PJ, Miniaci A: Release of the subscapularis for internal rotation contracture and pain after anterior repair for recurrent anterior dislocation of the shoulder. J Bone Joint Surg Am 1992;74:734-737.
Question 10High Yield
In comparing the clinical efficacy of intra-articular sodium hyaluronate injections vs triamcinolone injections for the treatment of hallux rigidus, which factor showed significantly better improvement in the sodium hyaluronate group:
Explanation
In a prospective randomized study comparing sodium hyaluronate vs cortisone injections for hallux rigidus, gait pain and AOFAS scores were significantly better in the sodium hyaluronate-treated group. There was no significant difference between the two treatment groups with regard to rest pain, pain with mobilization, pain with palpation, and use of analgesics.
Question 11High Yield
A 15-year-old girl has severe hip pain 3 years after a slipped capital femoral epiphysis that was complicated by avascular necrosis. Recommended treatment is a hip arthrodesis. In response to questions about late effects, after surgery the patient should be told that she is most likely to experience:
Explanation
Low back pain, followed closely by ipsilateral knee pain, is the most common late effect of hip arthrodesis in young patients. The tolerable pain usually occurs much later but may be treated by conversion to arthroplasty, if needed.
Ipsilateral hip pain should be minimal or absent if the fusion is successful.
Activity following arthrodesis is not significantly limited. Sports and heavy physical activities are feasible. The limp is usually minimal because the loss of hip motion is masked by lumbar motion.
Pain in the contralateral hip is rare and is often minimal after hip arthrodesis.
Ipsilateral hip pain should be minimal or absent if the fusion is successful.
Activity following arthrodesis is not significantly limited. Sports and heavy physical activities are feasible. The limp is usually minimal because the loss of hip motion is masked by lumbar motion.
Pain in the contralateral hip is rare and is often minimal after hip arthrodesis.
Question 12High Yield
Which is the best match in surface topography when performing an osteochondral autograft transplantation procedure from the distal femur to the talar dome for an osteochondral lesion of the talus:
Explanation
In a magnetic resonance imaging topography study looking for the best corresponding shape of the articular surface between the non-weightbearing femoral condyle and the medial talar dome, plugs from the supero-lateral femoral condyle had the best fit with osteochondral lesions of the medial talus in the anterior, central, and posterior zones.
Question 13High Yield
Which of the following statements best characterizes the natural history of metatarsus adductus in a newborn:
Explanation
Virtually all patients with metatarsus adductus will improve with time in the absence of active treatment.
C asts are not needed for the majority of cases because spontaneous improvement is by far the most common outcome. Reverse last shoes are not needed in the majority of patients with metatarsus adductus.
Most patients will not need surgery.
Equinus of the hindfoot is not part of the pathology in metatarsus adductus.
C asts are not needed for the majority of cases because spontaneous improvement is by far the most common outcome. Reverse last shoes are not needed in the majority of patients with metatarsus adductus.
Most patients will not need surgery.
Equinus of the hindfoot is not part of the pathology in metatarsus adductus.
Question 14High Yield
Evaluation of a nonambulatory 11-year-old girl with spinal muscular atrophy reveals mild scoliosis and full painless range of motion in her hips. An AP radiograph of her pelvis is shown in Figure 40. What is the most appropriate management for the hips?
Explanation
DISCUSSION: Hip instability in nonambulatory children with spinal muscular atrophy has been shown to be an infrequent cause of pain or disability; therefore, aggressive treatment generally is not indicated. Observation is the most appropriate management.
**36 • American Academy of Orthopaedic Surgeons**
REFERENCES: Sporer SM, Smith BG: Hip dislocation in patients with spinal muscular atrophy. J Pediatr Orthop 2003;123:10-14.
Thompson CE, Larsen LJ: Recurrent hip dislocation in intermediate spinal atrophy. J Pediatr Orthop 1990;10:638-641.
**36 • American Academy of Orthopaedic Surgeons**
REFERENCES: Sporer SM, Smith BG: Hip dislocation in patients with spinal muscular atrophy. J Pediatr Orthop 2003;123:10-14.
Thompson CE, Larsen LJ: Recurrent hip dislocation in intermediate spinal atrophy. J Pediatr Orthop 1990;10:638-641.
Question 15High Yield
Figures below show the clinical photograph and radiograph obtained from a 62-year-old man who has
deformity and pain 1 year after primary total hip arthroplasty. What is the reason for the observed deformity?
deformity and pain 1 year after primary total hip arthroplasty. What is the reason for the observed deformity?

Explanation
Figure 1 reveals an external rotation deformity of the right lower extremity. This deformity can have numerous causes, including extra-articular deformity. Figure 2 reveals a loose, subsided femoral component. Femoral stems typically subside into retroversion due to proximal femoral biomechanics, which cause a compensatory external rotation deformity. The combined findings from both images suggest an external rotation deformity most likely related to subsidence into retroversion.
Question 16High Yield
Exposure of tendons to ciprofloxacin in vitro causes all of the following except:
Explanation
C iprofloxacin was shown to cause a decrease in fibroblast proliferation, proteoglycan synthesis, and collagen synthesis. Matrix degrading proteolytic activity was increased.
Question 17High Yield
Figure 1 is the radiograph of a 12-year-old right-hand dominant baseball pitcher who has had right shoulder pain for the past 3 months. He recalls no specific injury. Pain initially occurred only with throwing, but now is bothersome during daily activities. He denies neck pain, or extremity numbness or tingling. Examination demonstrates a BMI of 31.5, a mild decrease in passive glenohumeral internal rotation with a symmetric increase in external rotation, and normal neurovascular findings. What factor most is likely related to the patient’s pain?
8
8
Explanation
The description and radiograph reveal a case of proximal humeral epiphysiolysis, also called Little Leaguer’s shoulder (LLS). This is an overuse condition resulting from chronic repetitive microtraumatic forces imposed on the unossified cartilage of the proximal humeral
physis. Classic radiographic findings include widening of the proximal humeral physis with increased sclerosis and/or mineralization/lucency. Many factors have been studied as possible contributors to the development of LSS, including all options presented. However, no clear relationship between body weight/height or throwing mechanics exist with LSS. It has also been claimed that the use of breaking pitches (e.g. curve balls, sliders) at an early age are a contributing factor, but this has been refuted by a number of recent studies. By far, the most important factors are the numbers of pitches thrown and the frequency of pitching. This is reflected in a number of indicators, including numbers of innings pitched, number of throwing days, numbers of pitches or pitched innings per week, month and year, and playing for multiple teams.
physis. Classic radiographic findings include widening of the proximal humeral physis with increased sclerosis and/or mineralization/lucency. Many factors have been studied as possible contributors to the development of LSS, including all options presented. However, no clear relationship between body weight/height or throwing mechanics exist with LSS. It has also been claimed that the use of breaking pitches (e.g. curve balls, sliders) at an early age are a contributing factor, but this has been refuted by a number of recent studies. By far, the most important factors are the numbers of pitches thrown and the frequency of pitching. This is reflected in a number of indicators, including numbers of innings pitched, number of throwing days, numbers of pitches or pitched innings per week, month and year, and playing for multiple teams.
Question 18High Yield
Which of the following zones of the physis is involved in Salter Harris Type I and II fractures:
Explanation
Salter Harris Type I and II fractures occur through the zone of provisional calcification or through the hypertrophiCzone. The reserve and proliferative zone remain intact and growth can proceed normal after healing of the fracture
Question 19High Yield
Slide 1 Slide 2 Slide 3
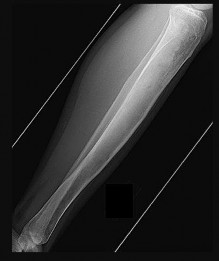
A 12-year-old boy is brought to the clinic by his concerned parents. The boyâs forearm is bowed, and his parents are confused as to the possible diagnosis and treatment options. You notice that the right forearm of the child is bowed ulnarwards and is shorter compared to the left forearm. The pronosupination is markedly decreased on the right side but is also limited on the left side. The patient has a good grip, pinch, and grasp. He is neurologically intact as well.
The parents say that they first noticed the deformity around 6 or 7 years ago, and the mother informs you that she had noticed a hard bump on the forearm. She has recently noticed another bump on his right leg. The child does not complain of pain and is using both of his hands quite well. The parents were informed by a previous physician that the child has Madelungâs deformity and are concerned that the disease is now involving other areas of his body.
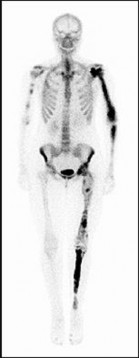
You order a radiograph of the forearm. The anteroposterior radiograph is shown (Slide 1). The childâs skeletal radiograph survey is also presented (Slide 2 and Slide 3).
Which of the following is not true regarding the possibility of malignant degeneration in this child:
A 12-year-old boy is brought to the clinic by his concerned parents. The boyâs forearm is bowed, and his parents are confused as to the possible diagnosis and treatment options. You notice that the right forearm of the child is bowed ulnarwards and is shorter compared to the left forearm. The pronosupination is markedly decreased on the right side but is also limited on the left side. The patient has a good grip, pinch, and grasp. He is neurologically intact as well.
The parents say that they first noticed the deformity around 6 or 7 years ago, and the mother informs you that she had noticed a hard bump on the forearm. She has recently noticed another bump on his right leg. The child does not complain of pain and is using both of his hands quite well. The parents were informed by a previous physician that the child has Madelungâs deformity and are concerned that the disease is now involving other areas of his body.
You order a radiograph of the forearm. The anteroposterior radiograph is shown (Slide 1). The childâs skeletal radiograph survey is also presented (Slide 2 and Slide 3).
Which of the following is not true regarding the possibility of malignant degeneration in this child:
Explanation
Bone scan cannot differentiate between an active lesion and a malignant transformation.
Question 20High Yield
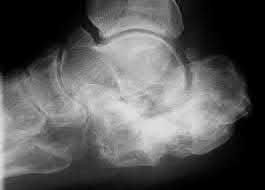
Which of the following is not commonly seen following malunion of a conservatively-managed calcaneus fracture?
Explanation
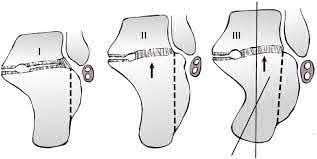
The most common deformities associated with calcaneal fracture malunion are decreased calcaneal height, increased calcaneal width, hindfoot varus, lateral exostosis secondary to lateral wall blow-out, and dorsiflexion of the talus resulting in ankle impingement. While not always symptomatic, subtalar arthritis also develops in the majority of cases. Although subfibular impingement does occur, this is due to the increased calcaneal width and lateral exostosis and not due to hindfoot valgus, which is otherwise uncommon.
Controversy continues to surround the benefit of operative management of displaced intra-articular calcaneal fractures. However, adverse sequelae of calcaneal malunions are well-described. Treatment of calcaneal malunions depends on the clinical symptomatology and may include addressing one or many of the aforementioned pathologies. A CT-based classification of calcaneal malunion (Illustration A) has been proposed and serves to direct management based on the most common individual and combined deformities. The goals of corrective surgery are to alleviate pain, improve fit of footwear, and improve walking ability.
Hsu et al. review the controversies and more recent advances in management of displaced intra-articular calcaneal fractures. The authors discuss the transition to more limited and minimally-invasive approaches to reduction and fixation of these injuries with the goal of mitigating the traditionally frequent and significant surgical complications.
Jackson et al. discuss the utility of distraction subtalar arthrodesis for the management of symptomatic calcaneal malunion in the setting of subtalar arthritis. The authors review the surgical technique and successful outcomes following the procedure. Thy advocate for careful patient selection given the preponderance of radiographic but often minimally symptomatic subtalar arthritis following calcaneal fracture malunion.
Griffin et al. performed a randomized controlled trial directly comparing operative versus nonoperative management of closed displaced intra-articular calcaneal fractures. The findings of the investigation supported no significant benefit to operative management at two-year follow-up in regard to standardized functional outcomes scores evaluating health, function, and quality of life. They advocated for nonoperative management given the substantially higher risk of complications following surgery.
Illustration A depicts the CT-based classification of calcaneal malunions. Type I involves lateral exostosis, necessitating lateral wall excision. Type II includes additional subtalar arthritis, requiring the addition of a subtalar arthrodesis.
Lastly, type III includes significant hindfoot varus in addition to the aforementioned sequelae, which may be addressed through a concomitant valgus osteotomy. Illustration B is a lateral radiograph of the foot in a patient with a calcaneal malunion, demonstrating significant loss of calcaneal height and resultant talar dorsiflexion with tibiotalar impingement.
Incorrect Answers:
Answer 1: Decreased hindfoot height and increased calcaneal width secondary to fracture collapse are among the most common sequelae reported following conservatively managed calcaneal fractures.
Answer 3: Lateral wall exostosis frequently results from lateral wall "blow-out", and directly results in peroneal tendon irritation, possible tears, and tendon subluxation.
Answer 4: Radiographic subtalar arthritis is common following calcaneal fracture, though generally clinical symptoms are much less frequent.
Answer 5: Tibiotalar impingement has been described to occur as a result of loss of calcaneal height and dorsiflexion of the talus.
Controversy continues to surround the benefit of operative management of displaced intra-articular calcaneal fractures. However, adverse sequelae of calcaneal malunions are well-described. Treatment of calcaneal malunions depends on the clinical symptomatology and may include addressing one or many of the aforementioned pathologies. A CT-based classification of calcaneal malunion (Illustration A) has been proposed and serves to direct management based on the most common individual and combined deformities. The goals of corrective surgery are to alleviate pain, improve fit of footwear, and improve walking ability.
Hsu et al. review the controversies and more recent advances in management of displaced intra-articular calcaneal fractures. The authors discuss the transition to more limited and minimally-invasive approaches to reduction and fixation of these injuries with the goal of mitigating the traditionally frequent and significant surgical complications.
Jackson et al. discuss the utility of distraction subtalar arthrodesis for the management of symptomatic calcaneal malunion in the setting of subtalar arthritis. The authors review the surgical technique and successful outcomes following the procedure. Thy advocate for careful patient selection given the preponderance of radiographic but often minimally symptomatic subtalar arthritis following calcaneal fracture malunion.
Griffin et al. performed a randomized controlled trial directly comparing operative versus nonoperative management of closed displaced intra-articular calcaneal fractures. The findings of the investigation supported no significant benefit to operative management at two-year follow-up in regard to standardized functional outcomes scores evaluating health, function, and quality of life. They advocated for nonoperative management given the substantially higher risk of complications following surgery.
Illustration A depicts the CT-based classification of calcaneal malunions. Type I involves lateral exostosis, necessitating lateral wall excision. Type II includes additional subtalar arthritis, requiring the addition of a subtalar arthrodesis.
Lastly, type III includes significant hindfoot varus in addition to the aforementioned sequelae, which may be addressed through a concomitant valgus osteotomy. Illustration B is a lateral radiograph of the foot in a patient with a calcaneal malunion, demonstrating significant loss of calcaneal height and resultant talar dorsiflexion with tibiotalar impingement.
Incorrect Answers:
Answer 1: Decreased hindfoot height and increased calcaneal width secondary to fracture collapse are among the most common sequelae reported following conservatively managed calcaneal fractures.
Answer 3: Lateral wall exostosis frequently results from lateral wall "blow-out", and directly results in peroneal tendon irritation, possible tears, and tendon subluxation.
Answer 4: Radiographic subtalar arthritis is common following calcaneal fracture, though generally clinical symptoms are much less frequent.
Answer 5: Tibiotalar impingement has been described to occur as a result of loss of calcaneal height and dorsiflexion of the talus.
Question 21High Yield
When fracture step-off is greater than the accepted limits, which of the following complications is the most common:
Explanation
Studies by Livesley, Kjaer-Petersen, and others have shown that patients with fractures with more than a 1-mm step-off after reduction were more likely to develop arthritis at the thumb carpometacarpal joint. Pain, decreased range of motion, and decreased pinch strength also correlated with these poor outcomes.
Question 22High Yield
When performing a total knee replacement, posterior stability can be achieved by all of the following except:
Explanation
Posterior stability can be achieved through the soft tissues or the implant. The posterior cruciate ligament can be retained and posterior instability can still be achieved. The anterior cruciate ligament plays no role in posterior stability and is always resected during a total knee replacement
Question 23High Yield
A 25-year-old female presents to the emergency room for the fourth time in the last week. She has vague complaints of extremity pain. Physical examination by a male ER resident has been limited each visit because she is terrified of the pain that the clinician may cause. On physical examination, she is withdrawn and frightened.
Regions of ecchymosis are noted throughout chest and abdomen. She has requested multiple radiographs, MRI and CT scans. Today's imaging (radiographs, MRI, CT scan) has been unrevealing. What is the most likely diagnosis?
Regions of ecchymosis are noted throughout chest and abdomen. She has requested multiple radiographs, MRI and CT scans. Today's imaging (radiographs, MRI, CT scan) has been unrevealing. What is the most likely diagnosis?
Explanation
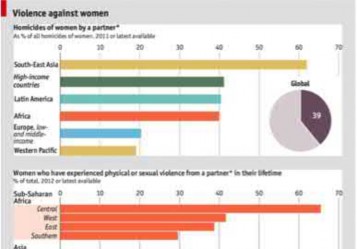
Based on the history and clinical presentation, the most likely diagnosis is intimate partner violence.
Domestic violence or intimate partner violence can be in the form of mental or physical abuse, neglect or abandonment. Close to 25% of women will experience domestic violence. Risk factors include young age (19-29 years of age), females, pregnancy and lower socioeconomic status. Affected patients will have repeated visits to the emergency room, find reasons to stay in a treatment facility for an extended period of time and constantly seek approval
of their partner.
Shields et al. reviewed factors influence outcome in treatment of patients affected by domestic violence. They found that positive outcomes were associated with interdisciplinary approaches to management. This included better history assessment, providing written documentation regarding intervention and better access to information on community resources.
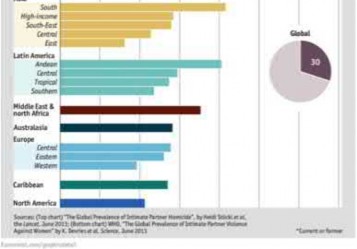
Illustration A is a chart documenting the frequency of female domestic violence throughout the world as of 2012.
Incorrect Answers
Answers 1, 2, 3, 5: These conditions are not consistent with this patient’s history.
Domestic violence or intimate partner violence can be in the form of mental or physical abuse, neglect or abandonment. Close to 25% of women will experience domestic violence. Risk factors include young age (19-29 years of age), females, pregnancy and lower socioeconomic status. Affected patients will have repeated visits to the emergency room, find reasons to stay in a treatment facility for an extended period of time and constantly seek approval
of their partner.
Shields et al. reviewed factors influence outcome in treatment of patients affected by domestic violence. They found that positive outcomes were associated with interdisciplinary approaches to management. This included better history assessment, providing written documentation regarding intervention and better access to information on community resources.
Illustration A is a chart documenting the frequency of female domestic violence throughout the world as of 2012.
Incorrect Answers
Answers 1, 2, 3, 5: These conditions are not consistent with this patient’s history.
Question 24High Yield
A 32-year-old male sustained a right grade IIIB open tibial shaft fracture 10 months ago when he fell down a ledge while hiking. Due to the location of the injury, it took EMS 15 hours to transport the patient to the ED, where IV antibiotics were promptly started. Subsequently,
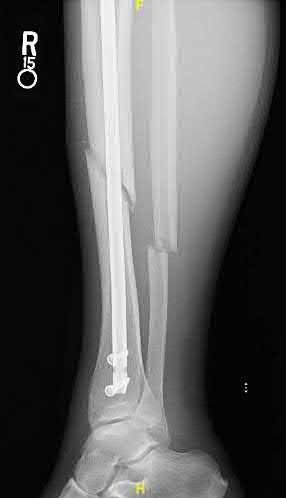
the patient underwent external fixation with serial debridements followed by definitive flap coverage and unreamed intramedullary nailing six days after the injury. The patient continues to have pain in the leg with weight-bearing but denies any fevers or chills. His surgical wounds appear well-healed with a small sinus tract over the open fracture site. Figures A and B are the current radiographs. Recent labs reveal an ESR, CRP and 25-hydroxyvitamin D2 of 32 mm/hr (reference 0-20 mm/hr), 15 mg/dL (reference 0-3 mg/dL), and 50 ng/mL (reference 20-100 ng/mL). What factor is most likely associated with this patient's current condition?
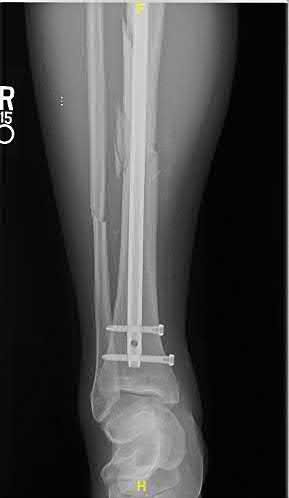
the patient underwent external fixation with serial debridements followed by definitive flap coverage and unreamed intramedullary nailing six days after the injury. The patient continues to have pain in the leg with weight-bearing but denies any fevers or chills. His surgical wounds appear well-healed with a small sinus tract over the open fracture site. Figures A and B are the current radiographs. Recent labs reveal an ESR, CRP and 25-hydroxyvitamin D2 of 32 mm/hr (reference 0-20 mm/hr), 15 mg/dL (reference 0-3 mg/dL), and 50 ng/mL (reference 20-100 ng/mL). What factor is most likely associated with this patient's current condition?
Explanation
The patient is presenting with a septic nonunion following an open tibial shaft fracture. Of the given answer choices, the timely administration of antibiotics, ideally within 3 hours of injury, is associated with decreased wound infection
rates and subsequent septic nonunion.
Tibial shaft fractures are the most common long bone fracture, with up to 24% of fractures presenting as an open injury. Appropriate initial management of these injuries is crucial to optimizing outcomes, as they are often fraught with high wound complication and infection rates. Literature has demonstrated that the prompt delivery of appropriate IV antibiotic coverage is one of the most important factors in minimizing wound infection rates and subsequent septic nonunions. The risk of infection is decreased substantially when antibiotics are started within three hours of the injury, compared to later treatment. Ideal coverage includes 1st generation cephalosporins for grades I and II, sometimes with the addition of gentamicin for grade III injuries. During the evaluation for septic nonunion, elevated CRP and ESR levels are suggestive of an infection.
Babhulkar et al. retrospectively reviewed 113 patients with long bone fracture nonunions of various etiologies, including 16 tibial shaft nonunions. The authors reported that the initial treatment of these injuries consisted of six intramedullary nails, four platings, two external fixators, and one plaster cast, which resulted in nine aseptic and four septic nonunions. Following appropriate treatment, all patients eventually attained fracture union, with 16% of tibial nonunions resulting in an acceptable malunion, 13% resulting in limb shortening, and two patients with a persistent septic nonunion that was successfully treated with Ilizarov frame. The authors concluded that successful treatment of long bone fracture nonunions requires consideration of the pathophysiology of the nonunion and appropriately addressing stability, infection control, and provision of an osteogenic environment.
Mundi et al. reviewed the management of open tibial shaft fractures. The authors supported the use of either bacitracin or castile soap irrigation, with no difference in infection outcomes, while low-pressure irrigation delivery was associated with lower reoperation rates due to infections, nonunion, and wound healing problems. They also supported that definitive closure of wounds within seven days of the initial injury was associated with a reduced rate of complications, including infection. The authors concluded that prompt administration of appropriate antibiotic prophylaxis was the single-most important determinant in minimizing wound infections.
The investigators of the SPRINT (The Study to Prospectively Evaluate Reamed Intramedullary Nails in Patients with Tibial Fractures) study performed a multicenter blinded randomized trial of 1319 patients treated with either reamed or unreamed intramedullary nailing for tibial shaft fractures. In the 406 patients with open fractures, of which 137 were grade III, there was no
treatment benefit between reamed and unreamed nails. However, the investigators reported a significantly increased union rate with reamed intramedullary nails for closed tibial shaft fractures. They concluded that reamed intramedullary nailing appears to have a treatment benefit only for closed tibial shaft fractures.
Figures A and B are the AP and lateral radiographs of the right tibia and fibula demonstrating a comminuted fracture of the tibia with minimal healing after intramedullary nail fixation.
Incorrect answers:
Answer 1: Definitive wound coverage should be performed within seven days of the injury in wounds requiring delayed closure in order to minimize the risk of infection. Wound coverage for the patient in this scenario was delayed < 7 days.
Answer 2: Union rates are comparable between unreamed and reamed intramedullary nailing for open tibial shaft fractures.
Answer 4: The patient has a normal vitamin D level, and an elevated CRP suggests an infectious rather than a nutritional etiology of the nonunion. Answer 5: Low-pressure irrigation is associated with lower reoperation rates due to infection, wound complications, and nonunion.
rates and subsequent septic nonunion.
Tibial shaft fractures are the most common long bone fracture, with up to 24% of fractures presenting as an open injury. Appropriate initial management of these injuries is crucial to optimizing outcomes, as they are often fraught with high wound complication and infection rates. Literature has demonstrated that the prompt delivery of appropriate IV antibiotic coverage is one of the most important factors in minimizing wound infection rates and subsequent septic nonunions. The risk of infection is decreased substantially when antibiotics are started within three hours of the injury, compared to later treatment. Ideal coverage includes 1st generation cephalosporins for grades I and II, sometimes with the addition of gentamicin for grade III injuries. During the evaluation for septic nonunion, elevated CRP and ESR levels are suggestive of an infection.
Babhulkar et al. retrospectively reviewed 113 patients with long bone fracture nonunions of various etiologies, including 16 tibial shaft nonunions. The authors reported that the initial treatment of these injuries consisted of six intramedullary nails, four platings, two external fixators, and one plaster cast, which resulted in nine aseptic and four septic nonunions. Following appropriate treatment, all patients eventually attained fracture union, with 16% of tibial nonunions resulting in an acceptable malunion, 13% resulting in limb shortening, and two patients with a persistent septic nonunion that was successfully treated with Ilizarov frame. The authors concluded that successful treatment of long bone fracture nonunions requires consideration of the pathophysiology of the nonunion and appropriately addressing stability, infection control, and provision of an osteogenic environment.
Mundi et al. reviewed the management of open tibial shaft fractures. The authors supported the use of either bacitracin or castile soap irrigation, with no difference in infection outcomes, while low-pressure irrigation delivery was associated with lower reoperation rates due to infections, nonunion, and wound healing problems. They also supported that definitive closure of wounds within seven days of the initial injury was associated with a reduced rate of complications, including infection. The authors concluded that prompt administration of appropriate antibiotic prophylaxis was the single-most important determinant in minimizing wound infections.
The investigators of the SPRINT (The Study to Prospectively Evaluate Reamed Intramedullary Nails in Patients with Tibial Fractures) study performed a multicenter blinded randomized trial of 1319 patients treated with either reamed or unreamed intramedullary nailing for tibial shaft fractures. In the 406 patients with open fractures, of which 137 were grade III, there was no
treatment benefit between reamed and unreamed nails. However, the investigators reported a significantly increased union rate with reamed intramedullary nails for closed tibial shaft fractures. They concluded that reamed intramedullary nailing appears to have a treatment benefit only for closed tibial shaft fractures.
Figures A and B are the AP and lateral radiographs of the right tibia and fibula demonstrating a comminuted fracture of the tibia with minimal healing after intramedullary nail fixation.
Incorrect answers:
Answer 1: Definitive wound coverage should be performed within seven days of the injury in wounds requiring delayed closure in order to minimize the risk of infection. Wound coverage for the patient in this scenario was delayed < 7 days.
Answer 2: Union rates are comparable between unreamed and reamed intramedullary nailing for open tibial shaft fractures.
Answer 4: The patient has a normal vitamin D level, and an elevated CRP suggests an infectious rather than a nutritional etiology of the nonunion. Answer 5: Low-pressure irrigation is associated with lower reoperation rates due to infection, wound complications, and nonunion.
Question 25High Yield
Figure 1 is the radiograph of a 6-year-old 40-kg boy who landed awkwardly onto his left leg on a trampoline. He has immediate pain and deformity of the thigh and is unable to ambulate. His canal diameter is 7 cm, and he is treated with two 3.0-mm titanium flexible elastic nails (TENs) and nonweightbearing. His fracture shortens 2 cm postoperatively and falls into 20 degrees of varus angulation. What characteristic is most responsible for the malunion?

Explanation
■
The image reveals a length-unstable fracture pattern (the length of the fracture line is more than double the cortical width at the level of the fracture). These fractures are associated with higher risk of malunion. TENs with at least 80% canal fill were placed, and his weight is below recommended upper limits (<49 kg).
■
The image reveals a length-unstable fracture pattern (the length of the fracture line is more than double the cortical width at the level of the fracture). These fractures are associated with higher risk of malunion. TENs with at least 80% canal fill were placed, and his weight is below recommended upper limits (<49 kg).
Question 26High Yield
Figures 1 and 2 are the radiographs of a 10-year-old girl who injured her elbow in an all-terrain vehicle accident. Figures 3 and 4 are radiographs of the elbow following closed manipulation. What is the best next step in management?

Explanation
■
The patient has sustained a displaced radial neck fracture. Generally, acceptable alignment of a pediatric radial neck fracture is considered to be <30% translation and <30° of angulation. After closed manipulation, the current alignment is unacceptable, and long arm casting without further treatment is not recommended. The next best step in management of this injury is an attempt at percutaneous reduction of the fracture with a Steinman pin. Open reduction should be performed only if the fracture cannot be reduced to an acceptable position with a closed or percutaneous method, due to the association of open reduction with greater stiffness and poor outcomes.
■
The patient has sustained a displaced radial neck fracture. Generally, acceptable alignment of a pediatric radial neck fracture is considered to be <30% translation and <30° of angulation. After closed manipulation, the current alignment is unacceptable, and long arm casting without further treatment is not recommended. The next best step in management of this injury is an attempt at percutaneous reduction of the fracture with a Steinman pin. Open reduction should be performed only if the fracture cannot be reduced to an acceptable position with a closed or percutaneous method, due to the association of open reduction with greater stiffness and poor outcomes.
Question 27High Yield
A 24-year-old white man presents to the emergency department. He was bitten on his fist while fighting with another man. You notice teeth marks on the dorsum of the metacarpophalangeal (MC P) joint of the right middle finger. The bite does not appear to be deep because the joint is not exposed, and you can see the extensor tendon, which seems intact. The patient has active extension at the MC P joint. The wound is red and swollen, but there is no tenderness or redness on the volar aspect of the MC P joint. The patient has some limitation in range of motion. He is afebrile. Radiographs reveal air in the joint but no joint
dislocation or fracture, and there is no neurovascular deficit. All of the following are appropriate steps in the management of this patient except:
dislocation or fracture, and there is no neurovascular deficit. All of the following are appropriate steps in the management of this patient except:
Explanation
Human bite wounds on the hand are typically found over the MP joint. The mechanism of injury is a clenched-fist blow to the mouth. Oral flora enters the wound, which often communicates with the joint. Eikenella corrodens is frequently cultured from human bite wounds, but the most common pathogen is staphylococcus aureus. Appropriate treatment includes the administration of tetanus toxoid, exploration if there is air in the joint or frank infection, observation, intravenous antibiotics, arm elevation, and splinting. All bites over joints should be assumed to penetrate and require formal incision and drainage.
Question 28High Yield
A 45-year-old distance runner has a hyaluronic acid injection to his knee because of degenerative arthritis. He immediately develops a severe rash and a systemic hypersensitivity reaction. This patient most likely is also allergic to which of the following?
Explanation
DISCUSSION: Preparations of hyaluronic acid can be divided into low and high molecular weight compounds. Contraindications to intra-articular hyaluronic acid include joint or skin infection, overlying skin disease, and allergies to chicken or egg products if using a preparation derived from rooster comb.
REFERENCES: Gloyscen DN, Gillespie MJ, Schenek RC: The effects of medication in sports injuries, in DeLee JC, Drez D Jr, Miller MD (eds): Orthopedic Sports Medicine: Principles and Practice, ed 2.
Philadelphia, PA, WB Saunders, 2003, vol 1, pp 121-124.
Schenck RC Jr: New approaches to the treatment of osteoarthritis: Oral glucosamine and chondroitin sulfate. Instr Course Lect 2000;49:491-494.
DISCUSSION: Preparations of hyaluronic acid can be divided into low and high molecular weight compounds. Contraindications to intra-articular hyaluronic acid include joint or skin infection, overlying skin disease, and allergies to chicken or egg products if using a preparation derived from rooster comb.
REFERENCES: Gloyscen DN, Gillespie MJ, Schenek RC: The effects of medication in sports injuries, in DeLee JC, Drez D Jr, Miller MD (eds): Orthopedic Sports Medicine: Principles and Practice, ed 2.
Philadelphia, PA, WB Saunders, 2003, vol 1, pp 121-124.
Schenck RC Jr: New approaches to the treatment of osteoarthritis: Oral glucosamine and chondroitin sulfate. Instr Course Lect 2000;49:491-494.
Question 29High Yield
If all levels of injury severity are taken into account, what is the likelihood of osteonecrosis among all patients with this injury?
Explanation
Talar neck fractures are devastating injuries that generally portend poor outcomes, even if they are fixed well. Although there has been a traditional emphasis on risk for osteonecrosis after these injuries, it is now known that posttraumatic subtalar arthrosis is a more common result and often is functionally debilitating. These injuries have been difficult to study because of their relative
infrequency. However, the largest study on these injuries revealed that time from injury to surgery had little bearing on risk for complications. The energy imparted at the time of injury (comminution and open fracture) was much more relevant. The safest approach to this injury that provides the widest exposure is a 2-incision lateral and medial approach with a medial malleolar osteotomy, if needed. Some of the blood supply to the talus proceeds through the deltoid ligament, so it is not to be violated. A 2015 meta-analysis noted that the rate of osteonecrosis, if all injury severities were taken into account, was 31%. That same meta-analysis noted a mean rate of subtalar arthritis of 49%. This rate increased to 81% in studies with more than 2 years of follow-up.
RECOMMENDED READINGS
8. [Dodd A, Lefaivre KA. Outcomes of Talar Neck Fractures: A Systematic Review and Meta-analysis. J Orthop Trauma. 2015 May;29(5):210-5. doi: 10.1097/BOT.0000000000000297. Review. PubMed PMID: 25635362.](http://www.ncbi.nlm.nih.gov/pubmed/25635362)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/25635362)
9. [Vallier HA, Nork SE, Barei DP, Benirschke SK, Sangeorzan BJ. Talar neck fractures: results and outcomes. J Bone Joint Surg Am. 2004 Aug;86-A(8):1616-24. ](http://www.ncbi.nlm.nih.gov/pubmed/15292407)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/15292407)
10. [Lindvall E, Haidukewych G, DiPasquale T, Herscovici D Jr, Sanders R. Open reduction and stable fixation of isolated, displaced talar neck and body fractures. J Bone Joint Surg Am. 2004 Oct;86-A(10):2229-34. PubMed PMID: 15466732. ](http://www.ncbi.nlm.nih.gov/pubmed/15466732)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/15466732)
11. [Ohl X, Harisboure A, Hemery X, Dehoux E. Long-term follow-up after surgical treatment of talar fractures: Twenty cases with an average follow-up of 7.5 years. Int Orthop. 2011 Jan;35(1):93-9. doi: 10.1007/s00264-009-0930-y. Epub 2009 Dec 22. ](http://www.ncbi.nlm.nih.gov/pubmed/20033158)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/20033158)
infrequency. However, the largest study on these injuries revealed that time from injury to surgery had little bearing on risk for complications. The energy imparted at the time of injury (comminution and open fracture) was much more relevant. The safest approach to this injury that provides the widest exposure is a 2-incision lateral and medial approach with a medial malleolar osteotomy, if needed. Some of the blood supply to the talus proceeds through the deltoid ligament, so it is not to be violated. A 2015 meta-analysis noted that the rate of osteonecrosis, if all injury severities were taken into account, was 31%. That same meta-analysis noted a mean rate of subtalar arthritis of 49%. This rate increased to 81% in studies with more than 2 years of follow-up.
RECOMMENDED READINGS
8. [Dodd A, Lefaivre KA. Outcomes of Talar Neck Fractures: A Systematic Review and Meta-analysis. J Orthop Trauma. 2015 May;29(5):210-5. doi: 10.1097/BOT.0000000000000297. Review. PubMed PMID: 25635362.](http://www.ncbi.nlm.nih.gov/pubmed/25635362)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/25635362)
9. [Vallier HA, Nork SE, Barei DP, Benirschke SK, Sangeorzan BJ. Talar neck fractures: results and outcomes. J Bone Joint Surg Am. 2004 Aug;86-A(8):1616-24. ](http://www.ncbi.nlm.nih.gov/pubmed/15292407)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/15292407)
10. [Lindvall E, Haidukewych G, DiPasquale T, Herscovici D Jr, Sanders R. Open reduction and stable fixation of isolated, displaced talar neck and body fractures. J Bone Joint Surg Am. 2004 Oct;86-A(10):2229-34. PubMed PMID: 15466732. ](http://www.ncbi.nlm.nih.gov/pubmed/15466732)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/15466732)
11. [Ohl X, Harisboure A, Hemery X, Dehoux E. Long-term follow-up after surgical treatment of talar fractures: Twenty cases with an average follow-up of 7.5 years. Int Orthop. 2011 Jan;35(1):93-9. doi: 10.1007/s00264-009-0930-y. Epub 2009 Dec 22. ](http://www.ncbi.nlm.nih.gov/pubmed/20033158)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/20033158)
Question 30High Yield
A surgeon recommends an interscalene regional block to a patient undergoing shoulder arthroscopy. When asked about potential complications, which of the following is most likely to occur?
Explanation
**
Sensory neuropathy is the most common complication seen with interscalene regional block.
Sensory neuropathy is the most common complication seen with interscalene regional block.
Question 31High Yield
In the anterior cruciate ligament-deficient knee, what structure provides an important secondary restraint to anterior tibial translation?
Explanation
DISCUSSION: Cadaveric studies have demonstrated the important role of the posterior horn of the medial meniscus in stabilizing the anterior cruciate ligament-deficient knee with significantly greater resultant force in the medial meniscus when subjected to anterior tibial loads. The posterior horn of the medial meniscus is thought to limit anterior tibial translation by acting as a buttress by wedging against the posterior aspect of the medial femoral condyle. The other soft tissues mentioned do not play any significant role in prevention of anterior tibial translation in the anterior cruciate ligament-deficient knee.
REFERENCES: Garrick JG (ed): Orthopaedic Knowledge Update: Sports Medicine 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2004, p 200.
Allen CR, Wong EK, Livesay GA, et al: Importance of the medial meniscus in the anterior cruciate ligament-deficient knee. J Orthop Res 2000;18:109-115.
Levy IM, Torzilli PA, Warren RF: The effect of medial meniscectomy on anterior-posterior motion of the knee. J Bone Joint Surg Am 1982;64:883-888.
Figure 31
DISCUSSION: Cadaveric studies have demonstrated the important role of the posterior horn of the medial meniscus in stabilizing the anterior cruciate ligament-deficient knee with significantly greater resultant force in the medial meniscus when subjected to anterior tibial loads. The posterior horn of the medial meniscus is thought to limit anterior tibial translation by acting as a buttress by wedging against the posterior aspect of the medial femoral condyle. The other soft tissues mentioned do not play any significant role in prevention of anterior tibial translation in the anterior cruciate ligament-deficient knee.
REFERENCES: Garrick JG (ed): Orthopaedic Knowledge Update: Sports Medicine 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2004, p 200.
Allen CR, Wong EK, Livesay GA, et al: Importance of the medial meniscus in the anterior cruciate ligament-deficient knee. J Orthop Res 2000;18:109-115.
Levy IM, Torzilli PA, Warren RF: The effect of medial meniscectomy on anterior-posterior motion of the knee. J Bone Joint Surg Am 1982;64:883-888.
Figure 31
Question 32High Yield
A 55-year-old man with a 4-part proximal humerus fracture with intra-articular comminution and a large greater tuberosity fragment
Explanation
- Hemiarthroplasty_
Question 33High Yield
The addition of which of the following food supplements may lead to a decrease in neural tube defects?

Explanation
DISCUSSION: The use of folic acid in developed countries has lead to a decrease in neural tube defects. The incidence of neural tube defects is increased in third world countries.
REFERENCES: Abel MF (ed): Orthopaedic Knowledge Update: Pediatrics 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2006, pp 111-122.
Lemke L, Dias L: Spina bifida, in Cramer KE, Scherl SA, Einhom TA (eds): Orthopaedic Surgery Essentials: Pediatrics. Philadelphia, PA, Lippincott Williams & Wilkins, 2004, pp 203-210.
Figure 42
DISCUSSION: The use of folic acid in developed countries has lead to a decrease in neural tube defects. The incidence of neural tube defects is increased in third world countries.
REFERENCES: Abel MF (ed): Orthopaedic Knowledge Update: Pediatrics 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2006, pp 111-122.
Lemke L, Dias L: Spina bifida, in Cramer KE, Scherl SA, Einhom TA (eds): Orthopaedic Surgery Essentials: Pediatrics. Philadelphia, PA, Lippincott Williams & Wilkins, 2004, pp 203-210.
Figure 42
Question 34High Yield
A 57-year-old man has a bone lesion that was identified on radiograph and MR imaging (Figures 17a and 17b) that were taken to evaluate anterior knee pain. An examination reveals a positive patellar apprehension test finding. The patient brings his imaging findings to his appointment, and you learn that an image-guided core needle biopsy was performed based upon the radiologist’s interpretation of the imaging. The core needle biopsy pathology interpretation text reads, “a low-
grade cartilage consistent with either enchondroma or low-grade chondrosarcoma. Clinical and imaging correlation is recommended.” What is the best next step?
grade cartilage consistent with either enchondroma or low-grade chondrosarcoma. Clinical and imaging correlation is recommended.” What is the best next step?
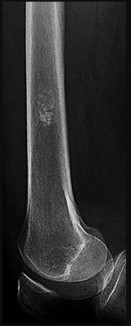
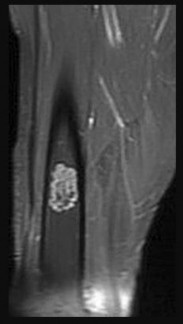
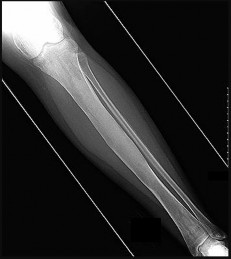
Explanation
Low-grade cartilage lesions are among the few diagnoses for which proceeding to definitive surgical treatment without a definitive histologic diagnosis is appropriate. Extended curettage with adjuvants is an acceptable treatment option for both enchondroma and low-grade chondrosarcoma of the extremities; as such, it is appropriate to proceed to definitive treatment when these are the only diagnoses in the differential. There is no consensus regarding the number and type of adjuvants used in intralesional curettage. There is also lack of consensus regarding how to reconstruct the resultant defect, with some favoring cement and others favoring bone grafting. A wide resection with intercalary resection is not indicated. Most commonly, serial radiologic studies are recommended to ensure no change occurs over time when the lesion is found incidentally, as in this patient.
The t(9;22) translocation occurs in extraskeletal myxoid chondrosarcoma, which is not a consideration for this patient based upon location, imaging, and the biopsy interpretation. Repeat core needle biopsy is not indicated because the value of core needle biopsy in general for low-grade cartilage lesions is questionable in light of sampling error concerns and the inability of expert pathologists to reliably distinguish between enchondroma and low-grade chondrosarcoma. Many orthopaedic oncologists favor proceeding directly to curettage with adjuvants without any biopsy
when the imaging is classic for a low-grade cartilage tumor without any evidence of dedifferentiation. Enchondromas are frequently positron emission tomography (PET) avid, and PET is not used to distinguish enchondroma from low-grade chondrosarcoma.
RECOMMENDED READINGS
30. [Hickey M, Farrokhyar F, Deheshi B, Turcotte R, Ghert M. A systematic review and meta-analysis of intralesional versus wide resection for intramedullary grade I chondrosarcoma of the extremities. Ann Surg Oncol. 2011 Jun;18(6):1705-9. doi: 10.1245/s10434-010-1532-z. Epub 2011 Jan 22. Review. PubMed PMID: 21258968. ](http://www.ncbi.nlm.nih.gov/pubmed/21258968)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/21258968)
31. [Meftah M, Schult P, Henshaw RM. Long-term results of intralesional curettage and cryosurgery for treatment of low-grade chondrosarcoma. J Bone Joint Surg Am. 2013 Aug 7;95(15):1358-64. doi: 10.2106/JBJS.L.00442. PubMed PMID: 23925739. ](http://www.ncbi.nlm.nih.gov/pubmed/23925739)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/23925739)
32. [Skeletal Lesions Interobserver Correlation among Expert Diagnosticians (SLICED) Study Group. Reliability of histopathologic and radiologic grading of cartilaginous neoplasms in long bones. J Bone Joint Surg Am. 2007 Oct;89(10):2113-23. PubMed PMID: 17908885. ](http://www.ncbi.nlm.nih.gov/pubmed/17908885)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/17908885)
33. Jesus-Garcia R, Osawa A, Filippi RZ, Viola DC, Korukian M, de Carvalho Campos Neto G, Wagner
[J. Is PET-CT an accurate method for the differential diagnosis between chondroma and chondrosarcoma? Springerplus. 2016 Feb 29;5:236. doi: 10.1186/s40064-016-1782-8. eCollection 2016. PubMed PMID: 27026930. ](http://www.ncbi.nlm.nih.gov/pubmed/27026930)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/27026930)
CLINICAL SITUATION FOR QUESTIONS 18 THROUGH 21
Figures 18a through 18c are the radiographs and bone scan of a 23-year-old woman.
The t(9;22) translocation occurs in extraskeletal myxoid chondrosarcoma, which is not a consideration for this patient based upon location, imaging, and the biopsy interpretation. Repeat core needle biopsy is not indicated because the value of core needle biopsy in general for low-grade cartilage lesions is questionable in light of sampling error concerns and the inability of expert pathologists to reliably distinguish between enchondroma and low-grade chondrosarcoma. Many orthopaedic oncologists favor proceeding directly to curettage with adjuvants without any biopsy
when the imaging is classic for a low-grade cartilage tumor without any evidence of dedifferentiation. Enchondromas are frequently positron emission tomography (PET) avid, and PET is not used to distinguish enchondroma from low-grade chondrosarcoma.
RECOMMENDED READINGS
30. [Hickey M, Farrokhyar F, Deheshi B, Turcotte R, Ghert M. A systematic review and meta-analysis of intralesional versus wide resection for intramedullary grade I chondrosarcoma of the extremities. Ann Surg Oncol. 2011 Jun;18(6):1705-9. doi: 10.1245/s10434-010-1532-z. Epub 2011 Jan 22. Review. PubMed PMID: 21258968. ](http://www.ncbi.nlm.nih.gov/pubmed/21258968)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/21258968)
31. [Meftah M, Schult P, Henshaw RM. Long-term results of intralesional curettage and cryosurgery for treatment of low-grade chondrosarcoma. J Bone Joint Surg Am. 2013 Aug 7;95(15):1358-64. doi: 10.2106/JBJS.L.00442. PubMed PMID: 23925739. ](http://www.ncbi.nlm.nih.gov/pubmed/23925739)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/23925739)
32. [Skeletal Lesions Interobserver Correlation among Expert Diagnosticians (SLICED) Study Group. Reliability of histopathologic and radiologic grading of cartilaginous neoplasms in long bones. J Bone Joint Surg Am. 2007 Oct;89(10):2113-23. PubMed PMID: 17908885. ](http://www.ncbi.nlm.nih.gov/pubmed/17908885)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/17908885)
33. Jesus-Garcia R, Osawa A, Filippi RZ, Viola DC, Korukian M, de Carvalho Campos Neto G, Wagner
[J. Is PET-CT an accurate method for the differential diagnosis between chondroma and chondrosarcoma? Springerplus. 2016 Feb 29;5:236. doi: 10.1186/s40064-016-1782-8. eCollection 2016. PubMed PMID: 27026930. ](http://www.ncbi.nlm.nih.gov/pubmed/27026930)[View Abstract at PubMed](http://www.ncbi.nlm.nih.gov/pubmed/27026930)
CLINICAL SITUATION FOR QUESTIONS 18 THROUGH 21
Figures 18a through 18c are the radiographs and bone scan of a 23-year-old woman.
Question 35High Yield
A 12-year-old girl soccer player has a 4-week history of pain, swelling, and tenderness of the right knee. She has not started her menstrual periods. The patient practices 4 nights per week and plays up to 4 games each weekend but is now unable to compete because of the pain. Examination reveals a tender mass at the right tibial tubercle. The cruciate ligaments are stable and the meniscal signs are negative. She demonstrates an antalgic limp. Radiographs are shown in Figures 1 and

Explanation
■
The patient has Osgood Schlatter syndrome, a traction apophysitis of the tibial tubercle as a result of overuse repetitive strain on the secondary ossification center. Radiographic changes include irregularity of the apophysis, separation from the tibial tubercle, and fragmentation. Radiographs are recommended in all unilateral cases of Osgood Schlatter to rule out infection or tumor. About 90% of patients respond to rest, ice, activity modification, and NSAIDs. In rare cases, surgical excision of the ossicle may provide good results in skeletally mature patients.
■
The patient has Osgood Schlatter syndrome, a traction apophysitis of the tibial tubercle as a result of overuse repetitive strain on the secondary ossification center. Radiographic changes include irregularity of the apophysis, separation from the tibial tubercle, and fragmentation. Radiographs are recommended in all unilateral cases of Osgood Schlatter to rule out infection or tumor. About 90% of patients respond to rest, ice, activity modification, and NSAIDs. In rare cases, surgical excision of the ossicle may provide good results in skeletally mature patients.
Question 36High Yield
What inflammatory mediator has been most closely associated with the magnitude of the systemic inflammatory response to trauma and with the development of multiple organ dysfunction syndrome (MODS)?
Explanation
Multiple cytokines (inflammatory mediators) are released following trauma, and their levels can be measured in serum. Persistent elevated levels of IL-6 (> 800 pg/mL) indicate an exaggerated systemic inflammatory response to trauma and have been associated with the development of MODS. Recent work has shown that extensive surgical procedures should be avoided when IL-6 levels remain elevated to prevent the precipitation of MODS. In the future, it is likely that this mediator and possibly others will be used to determine timing and techniques of future treatment.
REFERENCES: Patrick DA, Moore FA, Moore EE, et al: Jack A. Barney Resident Research Award winner: The inflammatory profile of interleukin-6, interleukin-8, and soluble intercellular adhesion molecule-1 in postinjury multiple organ failure. Am J Surg 1996;172:425-429.
Pape HC, van Griesven M, Rice J, et al: Major secondary surgery in blunt trauma patients and perioperative cytokine liberation: Determination of the clinical relevance of biochemical markers. J Trauma 2001;50:989-1000.
Giannoudis PV: When is the safest time to undertake secondary definitive fracture stabilization procedures in multiply injured patients who were initially managed using a strategy of primary temporary skeletal fixation. J Trauma 2002;52:811-812.
REFERENCES: Patrick DA, Moore FA, Moore EE, et al: Jack A. Barney Resident Research Award winner: The inflammatory profile of interleukin-6, interleukin-8, and soluble intercellular adhesion molecule-1 in postinjury multiple organ failure. Am J Surg 1996;172:425-429.
Pape HC, van Griesven M, Rice J, et al: Major secondary surgery in blunt trauma patients and perioperative cytokine liberation: Determination of the clinical relevance of biochemical markers. J Trauma 2001;50:989-1000.
Giannoudis PV: When is the safest time to undertake secondary definitive fracture stabilization procedures in multiply injured patients who were initially managed using a strategy of primary temporary skeletal fixation. J Trauma 2002;52:811-812.
Question 37High Yield
A 19-year-old man sustains a low-velocity gunshot wound to the forearm. What
factor most strongly correlates with the development of compartment syndrome
after this injury?
factor most strongly correlates with the development of compartment syndrome
after this injury?
Explanation
In a multivariate analysis, the strongest factor for the development of compartment syndrome is fracture of the proximal third of the forearm. However, compartment syndrome can still occur without a fracture. Therefore, these patients should be followed with a high level of suspicion for the development of compartment syndrome.
REFERENCES: Moed BR, Fakhouri AJ: Compartment syndrome after low-velocity gunshot wounds to the forearm. J Orthop Trauma 1991;5:134-137.
Hahn M, Strauss E, Yang EC: Gunshot wounds to the forearm. Orthop Clin North Am 1995;26:85-93.
REFERENCES: Moed BR, Fakhouri AJ: Compartment syndrome after low-velocity gunshot wounds to the forearm. J Orthop Trauma 1991;5:134-137.
Hahn M, Strauss E, Yang EC: Gunshot wounds to the forearm. Orthop Clin North Am 1995;26:85-93.
Question 38High Yield
Superficial frostbite injuries result in:
Explanation
Superficial frostbite typically involves minimal tissue loss. Patients have pliable skin with sensation. Deep frostbite typically results in significant soft tissue loss with firm anesthetic tissue that forms hemorrhagic blisters.
Question 39High Yield
Which of the following tissues has the highest maximum load to failure?
Explanation
All of the tissues noted above are stronger than native ACL. Although it is often thought that the bone-patellar tendon-bone graft is the strongest when selecting a graft source for ACL reconstruction, biomechanical studies show that the quadruple semitendinosus and gracilis tendons are the strongest of the tissues listed.
REFERENCES: Woo SL, Hollis JM, Adams DJ, et al: Tensile properties of the human femur-anterior cruciate ligament-tibia complex: The effects of specimen age and orientation. Am J Sports Med 1991;19:217-225.
Staubli HU, Schatzmann L, Brunner P, et al: Quadriceps tendon and patellar ligament cryosectional anatomy and structural properties in young adults. Knee Surg Sports Traumatol Arthrosc 1996;4:100-110.
Wilson TW, Zafuta MP, Zobitz M: A biomechanical analysis of matched bone-patellar tendon-bone and doubled looped semitendinosus and gracilis tendon grafts. Am J Sports Med 1999;27:202-207.
REFERENCES: Woo SL, Hollis JM, Adams DJ, et al: Tensile properties of the human femur-anterior cruciate ligament-tibia complex: The effects of specimen age and orientation. Am J Sports Med 1991;19:217-225.
Staubli HU, Schatzmann L, Brunner P, et al: Quadriceps tendon and patellar ligament cryosectional anatomy and structural properties in young adults. Knee Surg Sports Traumatol Arthrosc 1996;4:100-110.
Wilson TW, Zafuta MP, Zobitz M: A biomechanical analysis of matched bone-patellar tendon-bone and doubled looped semitendinosus and gracilis tendon grafts. Am J Sports Med 1999;27:202-207.
Question 40High Yield
Figure 26 is a radiograph of an 11-year-old boy with insidious-onset anterior knee pain.
Explanation
- MRI
Question 41High Yield
A 10-year-old boy has chronic renal failure and activity-related groin pain.
Explanation
- Widening of the proximal femoral physis with normal femoral head-neck junction offset
Question 42High Yield
Which pathology is associated with this condition?
Explanation
- Apophysitis of the tibial tubercle_
Question 43High Yield
Figures below depict the radiographs obtained from a 76-year-old woman with a painful total knee
arthroplasty. She describes an uneventful recovery with no wound-healing issues and was pain free for the first 10 years. Although reporting no trauma or inciting event, she now describes pain in the entire knee that is most severe with her first few steps. She has begun to notice night pain and, more recently, constant swelling. What is the most appropriate work-up at this time?
arthroplasty. She describes an uneventful recovery with no wound-healing issues and was pain free for the first 10 years. Although reporting no trauma or inciting event, she now describes pain in the entire knee that is most severe with her first few steps. She has begun to notice night pain and, more recently, constant swelling. What is the most appropriate work-up at this time?

Explanation
An evaluation of the painful total knee must be supported by an understanding of the potential etiologies of pain. They may include, aseptic loosening, infection, osteolysis, gap imbalance, referred pain, stiffness, and complex regional pain syndrome. In this case, the patient demonstrates start-up pain and had no prior history of infections. Her radiographs show subsidence of the tibia, indicating a loose prosthesis. Knowing that the prosthesis is already loose precludes the need for a bone scan. It is, however, important to rule out infection in this case; therefore, CRP and ESR testing is essential. Aspiration is also recommended when going into knee arthroplasty, and infection is a concern.
Question 44High Yield
A 17-year-old male baseball catcher has groin pain and intermittent hip locking. Examination demonstrates reproduction of the pain with hip flexion, internal rotation, and adduction. MR imaging reveals an anterosuperior labral tear.
Explanation
- Abnormal femoral head-neck junction offset
Question 45High Yield
The Lisfranc ligament connects the base of the
Explanation
The Lisfranc ligament arises from the lateral surface of the first (medial) cuneiform and is directed obliquely outward and slightly downward to insert on the medial surface of the second metatarsal base. It is the strongest of the tarsometatarsal interosseous ligaments.
REFERENCES: Sarrafian SK: Anatomy of the Foot and Ankle: Descriptive, Topographic, Functional, ed 2. Philadelphia, PA, JB Lippincott, 1993.
Solan MC, Moorman CT III, Miyamoto RG, et al: Ligamentous restraints of the second tarsometatarsal joint: A biomechanical evaluation. Foot Ankle Int 2001;22:637-641.
REFERENCES: Sarrafian SK: Anatomy of the Foot and Ankle: Descriptive, Topographic, Functional, ed 2. Philadelphia, PA, JB Lippincott, 1993.
Solan MC, Moorman CT III, Miyamoto RG, et al: Ligamentous restraints of the second tarsometatarsal joint: A biomechanical evaluation. Foot Ankle Int 2001;22:637-641.
Question 46High Yield
Figures 1 and 2 display the radiographs obtained from a woman who had volar plating of the distal radius 8 months earlier. Two days ago, she noticed she could not actively extend her thumb. What is the most appropriate treatment that would restore active thumb extension?
---
---
---
---








Explanation
Although the fracture is aligned in anatomic position, prominence of a least one of the distal screws is evident on the lateral radiographic view. The prominent screw is the most likely cause of the EPL tendon rupture. If the patient chooses surgical treatment, the best option would be removal of the offending hardware combined with extensor indicis proprius to EPL tendon transfer. Intercalary grafting would also be an acceptable option. If the tendon transfer were to be performed alone, the prominent screw(s) could rupture the transferred tendon as well. Also, it is rarely possible to repair the EPL tendon primarily in such cases, because this rupture is an attrition type. Casting would obviously not provide any benefit in this situation, and IP arthrodesis would not be the first surgical treatment option. This problem can be avoided by using shorter screws or not placing screws in plate holes that direct screws into the third dorsal extensor compartment. Intraoperative fluoroscopy and special views, such as the carpal shoot-through _view, are useful for avoiding this complication._
Question 47High Yield
**CLINICAL SITUATION**
Figures 1 and 2 are the radiographs of a 35-year-old man who is brought into the emergency department after a motor vehicle collision. He is complaining of isolated knee pain. Examination reveals swelling, blood filled blisters, popliteal ecchymosis, joint line pain, and limited knee joint motion. His pulses and sensation are normal.
The surgical approach for definitive reduction and stabilization of this pattern is
---
---
Figures 1 and 2 are the radiographs of a 35-year-old man who is brought into the emergency department after a motor vehicle collision. He is complaining of isolated knee pain. Examination reveals swelling, blood filled blisters, popliteal ecchymosis, joint line pain, and limited knee joint motion. His pulses and sensation are normal.
The surgical approach for definitive reduction and stabilization of this pattern is
---
---
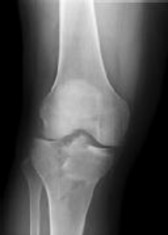
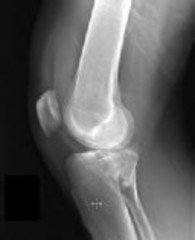
Explanation
Posterior partial articular tibial plateau fractures are rare. Failure to recognize this pattern can lead to poor patient outcomes secondary to poor surgical decision making. Pathognomonic findings on the lateral radiograph include maintenance of continuity between the anterior articular surface and tibial shaft along with subluxation of the knee joint with excessively anterior tibial station (the femoral condyles remain with the fractured posterior articular pieces while the remainder of the tibia subluxes anteriorly).
Initial management of axially unstable tibial plateau fractures with soft tissue swelling should consist of spanning external fixation and closed manipulative realignment. This allows for soft tissue recovery with the knee joint provisionally stabilized in reduced station. It also provides time for pre-operative planning, which is typically empowered via a CT scan with reconstructions. If the pattern was initially misdiagnosed as a more typically bicondylar tibial plateau fracture, the CT scan will clarify the misconception and allow for better surgical decision making.
Attempting to visualize, reduce, and stabilize a posterior partial articular pattern in the supine position from an anterior approach is fraught with difficulties. Prone positioning is preferred for definitive fixation. Surgical approaches vary, but typically incorporate a posteromedial interval deep to the popliteus and soleus to provide buttress plating to the posterior column of the tibia.
Posterior partial articular tibial plateau fractures are rare. Failure to recognize this pattern can lead to poor patient outcomes secondary to poor surgical decision making. Pathognomonic findings on the lateral radiograph include maintenance of continuity between the anterior articular surface and tibial shaft along with subluxation of the knee joint with excessively anterior tibial station (the femoral condyles remain with the fractured posterior articular pieces while the remainder of the tibia subluxes anteriorly).
Initial management of axially unstable tibial plateau fractures with soft tissue swelling should consist of spanning external fixation and closed manipulative realignment. This allows for soft tissue recovery with the knee joint provisionally
stabilized in reduced station. It also provides time for pre-operative planning, which is typically empowered via a CT scan with reconstructions. If the pattern was initially misdiagnosed as a more typically bicondylar tibial plateau fracture, the CT scan will clarify the misconception and allow for better surgical decision making.
Attempting to visualize, reduce, and stabilize a posterior partial articular pattern in the supine position from an anterior approach is fraught with difficulties. Prone positioning is preferred for definitive fixation. Surgical approaches vary, but typically incorporate a posteromedial interval deep to the popliteus and soleus to provide buttress plating to the posterior column of the tibia.
Initial management of axially unstable tibial plateau fractures with soft tissue swelling should consist of spanning external fixation and closed manipulative realignment. This allows for soft tissue recovery with the knee joint provisionally stabilized in reduced station. It also provides time for pre-operative planning, which is typically empowered via a CT scan with reconstructions. If the pattern was initially misdiagnosed as a more typically bicondylar tibial plateau fracture, the CT scan will clarify the misconception and allow for better surgical decision making.
Attempting to visualize, reduce, and stabilize a posterior partial articular pattern in the supine position from an anterior approach is fraught with difficulties. Prone positioning is preferred for definitive fixation. Surgical approaches vary, but typically incorporate a posteromedial interval deep to the popliteus and soleus to provide buttress plating to the posterior column of the tibia.
Posterior partial articular tibial plateau fractures are rare. Failure to recognize this pattern can lead to poor patient outcomes secondary to poor surgical decision making. Pathognomonic findings on the lateral radiograph include maintenance of continuity between the anterior articular surface and tibial shaft along with subluxation of the knee joint with excessively anterior tibial station (the femoral condyles remain with the fractured posterior articular pieces while the remainder of the tibia subluxes anteriorly).
Initial management of axially unstable tibial plateau fractures with soft tissue swelling should consist of spanning external fixation and closed manipulative realignment. This allows for soft tissue recovery with the knee joint provisionally
stabilized in reduced station. It also provides time for pre-operative planning, which is typically empowered via a CT scan with reconstructions. If the pattern was initially misdiagnosed as a more typically bicondylar tibial plateau fracture, the CT scan will clarify the misconception and allow for better surgical decision making.
Attempting to visualize, reduce, and stabilize a posterior partial articular pattern in the supine position from an anterior approach is fraught with difficulties. Prone positioning is preferred for definitive fixation. Surgical approaches vary, but typically incorporate a posteromedial interval deep to the popliteus and soleus to provide buttress plating to the posterior column of the tibia.
Question 48High Yield
A 37-year-old woman has had intermittent paresthesias and numbness in the plantar foot for the past 6 months. She reports that the symptoms are worse with activity, and the paresthesias are beginning to awaken her at night. MRI scans are shown in Figures 6a and 6b. What is the most likely diagnosis?
Explanation
The symptoms are consistent with tarsal tunnel syndrome. Ganglion cysts are a well-known cause of tarsal tunnel syndrome. The MRI scans show a high intensity, well-circumscribed mass in the tarsal tunnel that is consistent with a fluid-filled cyst. Patients usually respond well to excision of the ganglion and resolution of the tarsal tunnel symptoms. The surrounding fat is a different signal intensity on the MRI scans, which rules out a lipoma. Synovial cell sarcoma has a heterogeneous appearance on an MRI scan. Metastatic tumors are most commonly found in the osseous structures of the foot, not the soft tissues.
REFERENCES: Rozbruch SR, Chang V, Bohne WH, et al: Ganglion cysts of the lower extremity: An analysis of 54 cases and review of the literature. Orthopedics 1998;21:141-148.
Llauger J, Palmer J, Monill JM, et al: MR imaging of benign soft-tissue masses of the foot and ankle. Radiographics 1998;18:1481-1498.
Takakura Y, Kitada C, Sugimoto K, et al: Tarsal tunnel syndrome: Causes and results of operative treatment. J Bone Joint Surg Br 1991;73:125-128.
REFERENCES: Rozbruch SR, Chang V, Bohne WH, et al: Ganglion cysts of the lower extremity: An analysis of 54 cases and review of the literature. Orthopedics 1998;21:141-148.
Llauger J, Palmer J, Monill JM, et al: MR imaging of benign soft-tissue masses of the foot and ankle. Radiographics 1998;18:1481-1498.
Takakura Y, Kitada C, Sugimoto K, et al: Tarsal tunnel syndrome: Causes and results of operative treatment. J Bone Joint Surg Br 1991;73:125-128.
Question 49High Yield
A 26-year-old professional football player presents for evaluation of ankle pain. He was playing in a match 2 days ago and felt a pop in his ankle. On examination, the peroneal tendon is felt to subluxate anterior to the fibula. Magnetic resonance imaging confirms a tear of the superior peroneal retinaculum. Recommended treatment includes:
Explanation
An acute dislocation of the peroneal tendon must be repaired. The results of immobilization are not predictable and, in a professional athlete, the added potential for failure with nonoperative treatment must be considered. With a rupture of the
superior peroneal retinaculum likely to be the cause of the dislocation, the peroneal tendon should be repaired. When repair of an acute dislocation is performed, it should not be necessary to deepen the fibular groove.
superior peroneal retinaculum likely to be the cause of the dislocation, the peroneal tendon should be repaired. When repair of an acute dislocation is performed, it should not be necessary to deepen the fibular groove.
Question 50High Yield
A 12-year-old boy is diagnosed with osteomyelitis and subperiosteal abscess of the distal tibia demonstrated on the MRI. CRP is 13 mg/l. He is taken to the operating room (OR) for incision and drainage. Intraoperative cultures as well as blood cultures grow methicillin-resistant Staphylococcus aureus (MRSA). On postoperative day 2, he develops swelling in the leg, as well as an increased oxygen requirement. What should be the next step in evaluation?
Explanation
■
This child has a MRSA osteomyelitis. Many recent studies have shown that these infections are more difficult to treat and are associated with severe complications and longer hospitalizations. They may also require an increased number of surgical procedures to get control of the infection source. Deep venous thrombosis (DVT) and pulmonary embolism, as well as septic emboli to the lungs occur more commonly with MRSA infections. Increased swelling of the leg may be related to the onset of a DVT and venous ultrasonography is an easy and quick study to help determine if a DVT is present. Currently, the patient has an increased oxygen requirement. Helical CT scan is the next best test to evaluate for septic pulmonary emboli. Plain radiograph of the chest is helpful to look for areas of pneumonia but not diagnostic for septic emboli. Repeat MRI of the leg will be abnormal because of the recent surgical procedure and most likely will not add anything diagnostically. Given his clinical improvement and decreasing CRP, a repeat return to the OR is not indicated at this time, although it is not uncommon for children with MRSA infections to require more than one surgical procedure.
This child has a MRSA osteomyelitis. Many recent studies have shown that these infections are more difficult to treat and are associated with severe complications and longer hospitalizations. They may also require an increased number of surgical procedures to get control of the infection source. Deep venous thrombosis (DVT) and pulmonary embolism, as well as septic emboli to the lungs occur more commonly with MRSA infections. Increased swelling of the leg may be related to the onset of a DVT and venous ultrasonography is an easy and quick study to help determine if a DVT is present. Currently, the patient has an increased oxygen requirement. Helical CT scan is the next best test to evaluate for septic pulmonary emboli. Plain radiograph of the chest is helpful to look for areas of pneumonia but not diagnostic for septic emboli. Repeat MRI of the leg will be abnormal because of the recent surgical procedure and most likely will not add anything diagnostically. Given his clinical improvement and decreasing CRP, a repeat return to the OR is not indicated at this time, although it is not uncommon for children with MRSA infections to require more than one surgical procedure.
You Might Also Like

Medically Verified Content by
Prof. Dr. Mohammed Hutaif
Consultant Orthopedic & Spine Surgeon

