Pediatric Fractures and Dislocations: Operative Principles and Techniques
Key Takeaway
Pediatric fractures require specialized operative strategies due to unique bone biomechanics, thick periosteum, and the presence of physes. While many pediatric injuries remodel through compensatory growth, specific injuries—termed "fractures of necessity"—demand precise open reduction and internal fixation to prevent growth arrest and angular deformity. This guide details the surgical management, biomechanical principles, and postoperative protocols for complex pediatric fractures and dislocations.
Introduction to Pediatric Traumatology
The management of fractures and dislocations in children demands a profound understanding of the unique biomechanical, physiological, and anatomical properties of the immature skeleton. Unlike adult bone, pediatric bone is highly porous, possesses a lower modulus of elasticity, and is enveloped by a robust, osteogenic periosteum. These factors dictate not only the patterns of injury but also the philosophy of treatment.
While the vast majority of pediatric fractures are managed non-operatively due to the immense remodeling potential of the growing skeleton, the modern orthopaedic surgeon must be acutely aware of the absolute indications for surgical intervention. The physes (growth plates) represent the weakest biomechanical link in the pediatric musculoskeletal system, making them highly susceptible to shear and tension forces. Failure to achieve anatomic reduction in specific intra-articular or physeal injuries can lead to catastrophic complications, including premature physeal closure, angular deformity, and lifelong functional impairment.
Clinical Pearl: The pediatric periosteum is significantly thicker and more biologically active than in adults. It typically tears on the convex (tension) side of a fracture but remains intact on the concave (compression) side. This intact periosteal hinge is the surgeon’s greatest ally, aiding in the stabilization of closed reductions and drastically reducing the incidence of open fractures.
Biomechanics and Principles of Remodeling
According to the foundational work of Currey and Butler, the malleability of children’s bones allows for unique injury patterns, such as plastic deformation (bowing injuries), greenstick fractures, and torus (buckle) fractures. Because pediatric bone can absorb substantially more energy before catastrophic failure, the resulting fracture patterns often differ markedly from those seen in adults.
Blount’s Rules of Remodeling
Historically, Blount established the definitive rules governing the spontaneous correction of angular deformities in pediatric long bones. The potential for a fracture to remodel is dictated by three primary factors:
1. Age of the Patient: Remodeling potential is inversely proportional to the child's age. Two years of remaining growth is generally considered the minimum required for clinically significant remodeling.
2. Distance from the Physis: Fractures adjacent to the physis (metaphyseal) remodel far better than diaphyseal fractures.
3. Plane of Deformity: Angulation in the plane of motion of the adjacent hinge joint (e.g., flexion/extension at the knee or elbow) remodels robustly.
Surgical Pitfall: Never rely on remodeling for rotational malalignment. Rotational deformities are permanent and will not correct with growth. Furthermore, varus and valgus angulations remodel poorly compared to sagittal plane deformities and must be corrected acutely.
Compensatory Overgrowth
In certain fractures, particularly diaphyseal fractures of the femur in children aged 2 to 10 years, the hyperemic response of fracture healing stimulates the adjacent physes, leading to longitudinal overgrowth. Surgeons must often accept 1 to 2 centimeters of overriding at the fracture site to compensate for this anticipated overgrowth.
"Fractures of Necessity": Absolute Indications for Surgery
While closed treatment is the mainstay of pediatric orthopaedics, certain injuries are universally recognized as "fractures of necessity." These injuries carry an unacceptably high rate of nonunion, malunion, avascular necrosis (AVN), or growth arrest if treated non-operatively. As Boyd noted, nonunions in children are exceedingly rare; when they do occur, they are almost exclusively the result of open fractures, pathological bone, or iatrogenic mismanagement of these specific fractures.
The three classic pediatric fractures of necessity are:
1. Lateral Humeral Condyle Fractures
2. Femoral Neck Fractures
3. Distal Tibial Epiphyseal Fractures (Tillaux and Triplane)
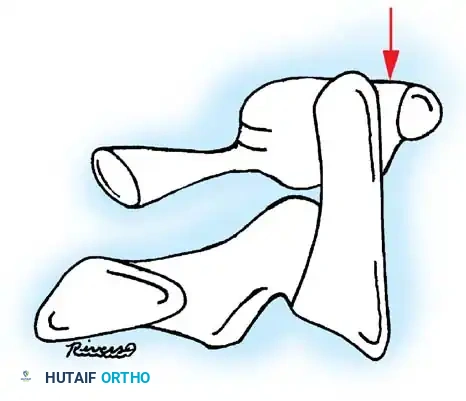
Surgical Masterclass: Lateral Humeral Condyle Fractures
Lateral condyle fractures are the second most common pediatric elbow fracture but are the most common to require open reduction and internal fixation (ORIF). They are Salter-Harris Type IV injuries, meaning the fracture line traverses the metaphysis, physis, and epiphysis, entering the articular surface.
Indications for Surgery
- Displacement > 2 mm.
- Articular incongruity.
- Late presentations with progressive displacement.
Positioning and Preparation
- Position: Supine with the operative arm extended on a radiolucent hand table.
- Tourniquet: High sterile arm tourniquet.
- Fluoroscopy: C-arm positioned parallel to the arm board, entering from the head or foot of the table to allow unhindered AP and lateral imaging.
Surgical Approach: Lateral Kocher Approach
- Incision: Make a 3 to 5 cm longitudinal incision centered over the lateral epicondyle, extending proximally over the supracondylar ridge.
- Interval: Develop the interval between the brachioradialis (anterior) and the triceps (posterior).
- Exposure: Incise the fascia and expose the fracture.
Surgical Warning: DO NOT dissect the soft tissues off the posterior aspect of the lateral condyle fragment. The blood supply to the capitellum enters posteriorly. Stripping this tissue will inevitably lead to avascular necrosis of the capitellum.
Reduction and Fixation
- Joint Visualization: Open the joint capsule anteriorly to directly visualize the articular surface (the capitellotrochlear groove).
- Reduction: Use a dental pick or a small single-prong skin hook to gently manipulate the fragment. Anatomic reduction of the articular cartilage is paramount; metaphyseal alignment is secondary.
- Fixation: Drive two smooth Kirschner wires (K-wires), typically 1.6 mm (0.062 inch), from the lateral condyle across the fracture site into the intact medial metaphysis.
- Biomechanics of Pinning: The pins must be divergent to maximize biomechanical stability and rotational control. Ensure the pins engage the opposite intact cortex.
- Closure: Bend the pins outside the skin to facilitate removal in the clinic. Close the capsule, fascia, and skin in layers.
Postoperative Protocol
- Apply a well-padded long-arm cast with the elbow at 90 degrees of flexion and the forearm in neutral rotation.
- Radiographs at 1 and 2 weeks to ensure maintenance of reduction.
- Pin removal and cast discontinuation at 3 to 4 weeks, followed by active range of motion.
Surgical Masterclass: Pediatric Femoral Neck Fractures
Pediatric hip fractures are high-energy injuries associated with a devastatingly high rate of avascular necrosis (AVN), premature physeal closure, and coxa vara. The Delbet classification dictates management:
* Type I: Transepiphyseal separation (often associated with dislocation).
* Type II: Transcervical fracture (most common).
* Type III: Cervicotrochanteric fracture.
* Type IV: Intertrochanteric fracture.
Indications for Surgery
All Delbet Type I, II, and III fractures require urgent surgical stabilization. Type IV fractures may occasionally be treated with a spica cast if undisplaced, but operative fixation is increasingly preferred to prevent varus collapse.
Positioning and Preparation
- Position: Supine on a radiolucent fracture table.
- Traction: Gentle longitudinal traction with internal rotation to achieve closed reduction. Avoid forceful or repeated reduction attempts, which exacerbate the risk of AVN.
Surgical Approach and Decompression
Clinical Pearl: The role of capsulotomy is debated, but the prevailing evidence-based consensus strongly favors an urgent anterior capsulotomy to decompress the intracapsular hematoma. This reduces tamponade effect on the delicate retinacular vessels, potentially lowering the risk of AVN.
- Approach: A standard Watson-Jones or Smith-Petersen approach can be utilized for open reduction and capsulotomy. Alternatively, a percutaneous approach is used if closed reduction is anatomic, combined with a percutaneous capsulotomy using a surgical blade under fluoroscopy.
Fixation Strategy
The choice of implant depends on the child's age and the location of the fracture relative to the capital femoral physis.
1. Children < 4 years: Use smooth, unthreaded K-wires or Steinmann pins to cross the physis. Threaded implants will cause immediate growth arrest.
2. Children 4 to 12 years: Use partially threaded cannulated screws (4.0 mm or 4.5 mm). If the fracture is transcervical (Type II), the screws must stop short of the physis to preserve growth. If the fracture is transepiphyseal (Type I), smooth pins must be used, or the surgeon must accept physeal arrest as a consequence of screw fixation.
3. Adolescents (> 12 years): Treat similarly to adults using 6.5 mm or 7.0 mm cannulated screws.
Postoperative Protocol
- A one-and-a-half hip spica cast is routinely applied for children under 10 years of age to neutralize the massive lever-arm forces of the lower extremity.
- Older, compliant adolescents may be managed with strict non-weight-bearing mobilization.
- Serial radiographs are required for up to 2 years to monitor for the insidious onset of AVN or chondrolysis.
Surgical Masterclass: Distal Tibial Epiphyseal Fractures (Tillaux and Triplane)
These fractures occur exclusively during the transitional period of adolescence (typically ages 12-15) when the distal tibial physis is undergoing asymmetric closure. The physis closes from central to anteromedial, then posteromedial, and finally lateral.
- Tillaux Fracture: A Salter-Harris III avulsion of the anterolateral epiphysis by the anterior inferior tibiofibular ligament (AITFL).
- Triplane Fracture: A complex Salter-Harris IV equivalent with fracture lines in the sagittal (epiphysis), axial (physis), and coronal (metaphysis) planes.
Indications for Surgery
- Intra-articular step-off or gap > 2 mm.
- Inability to achieve or maintain closed reduction (often blocked by interposed periosteum).
Positioning and Preparation
- Position: Supine with a bump under the ipsilateral hip to internally rotate the leg to neutral.
- Tourniquet: Thigh tourniquet.
- Fluoroscopy: C-arm positioned to provide perfect mortise and lateral views of the ankle.
Surgical Approach: Anterolateral Approach
- Incision: Make a 4 to 5 cm longitudinal incision over the anterolateral aspect of the distal tibia, just medial to the fibula.
- Dissection: Protect the superficial peroneal nerve. Retract the extensor tendons medially.
- Exposure: Incise the extensor retinaculum and expose the fracture site.
Surgical Pitfall: The anterior periosteum is frequently torn and invaginated into the fracture site, preventing closed reduction. This must be meticulously extracted using a Freer elevator before reduction is attempted.
Reduction and Fixation
- Reduction: Use a pointed reduction forceps (Weber clamp). Place one tine on the anterolateral fragment and the other on the intact medial malleolus. Gently compress to restore articular congruity.
- Verification: Direct visualization of the joint line via a small arthrotomy or arthroscopic assistance is highly recommended to confirm a step-free articular surface.
- Fixation (Tillaux): Place a single 4.0 mm partially threaded cannulated screw from lateral to medial, parallel to the joint line, entirely within the epiphysis.
- Fixation (Triplane): Requires two screws. One epiphyseal screw (lateral to medial) to compress the sagittal fracture, and one metaphyseal screw (anterior to posterior) to compress the coronal fracture.
- Physeal Considerations: Because these fractures occur in physes that are already closing, crossing the physis with a screw is generally acceptable and will not cause clinically significant leg length discrepancy, though it should be avoided if possible.
Postoperative Protocol
- Apply a short-leg, non-weight-bearing cast or rigid boot for 4 weeks.
- Transition to progressive weight-bearing in a CAM boot at 4 weeks.
- Hardware removal is generally not required unless the screws become symptomatic under the skin.
Psychosocial Impact and Complications
The management of pediatric trauma extends beyond the operating room. As noted by Stancin et al., serious pediatric fractures requiring hospitalization induce significant functional limitations and family stress for up to 6 months post-injury. Lower extremity fractures requiring prolonged immobilization (e.g., spica casting for femur fractures) exert the most profound negative impact on the family unit. Surgeons must provide clear, empathetic communication regarding expected timelines, cast care, and the psychological toll of immobilization.
Late Complications
- Growth Arrest: The most feared complication of physeal injuries. Parents must be counseled preoperatively that despite perfect surgical execution, the initial trauma to the physis may result in premature closure. Serial follow-up for 12 to 24 months is mandatory.
- Nonunion: Exceedingly rare. If encountered, the surgeon must immediately suspect infection, pathological bone (e.g., bone cyst, osteogenesis imperfecta), or soft tissue interposition.
- Chondrolysis: A rapid, painful stiffening of the joint (most common in the hip and knee) resulting from articular cartilage necrosis. It is often associated with unrecognized intra-articular hardware penetration. Meticulous fluoroscopic evaluation during surgery is the only prevention.
By adhering to strict biomechanical principles, respecting the delicate vascularity of the pediatric skeleton, and executing precise surgical techniques for "fractures of necessity," the orthopaedic surgeon can reliably restore anatomy and ensure normal growth and function for the pediatric trauma patient.
📚 Medical References
- pediatric fractures: mechanism and treatment, J Pediatr Orthop 9:310, 1989.
- McLauchlan GJ, Cowan B, Annan IH, et al: Management of completely displaced metaphyseal fractures of the distal radius in children: a prospective randomised controlled trial, J Bone Joint Surg 84B:413, 2002.
- Mikic ZD: Galeazzi fracture-dislocation, J Bone Joint Surg 57A:107, 1975.
- Milch H: Roentgenographic diagnosis of torsional deformities in tubular bones, Surgery 15:440, 1944.
- Monteggia GB: Instit Chirurg 5:130, 1814 (translated by Helen Rang). Myers GJC, Gibbons PJ, Glithero PR: Nancy nailing of diaphyseal forearm fractures, J Bone Joint Surg 86B:581, 2004.
- Nelson CA, Buchanan JR, Harrison CS: Distal ulnar growth arrest, J Hand Surg 9A:164, 1984.
- Nielson AB, Simonsen O: Displaced forearm fractures in children treated with plates, Injury 15:393, 1984.
- Nimityongskul P, Anderson LD, Sri P: Plastic deformation of the forearm: a review and case reports, J Trauma 31:1678, 1991.
- O’Brien ET: Fractures of the hand and wrist region. In Rockwood CA Jr, Wilkins KE, King RE, eds: Fractures in children, Philadelphia, 1984, Lippincott. Ogden JA: Skeletal injury in the child, Philadelphia, 1982, Lea & Febiger. Onley BW, Menelaus MB: Monteggia and equivalent lesions in childhood, J Pediatr Orthop 9:219, 1989.
- Ortega R, Loder RT, Louis DS: Open reduction and internal fi xation of forearm fractures in children, J Pediatr Orthop 16:651, 1996.
- Price CT, Scott DS, Kurzner ME, et al: Malunited forearm fractures in children, J Pediatr Orthop 10:705, 1990.
- Qidwai SA: Treatment of diaphyseal forearm fractures in children by intramedullary Kirschner wires, J Trauma 50:303, 2001.
- Ray TD, Tessler RH, Dell PC: Traumatic ulnar physeal arrest after distal forearm fractures in children, J Pediatr Orthop 16:195, 1996.
- Reckling FW: Unstable fracture-dislocations of the forearm (Monteggia and Galeazzi lesions), J Bone Joint Surg 64A:857, 1982.
- Richter D, Ostermann PA, Ekkernkamp A, et al: Elastic intramedullary nailing: a minimally invasive concept in the treatment of unstable forearm fractures in children, J Pediatr Orthop 18:457, 1998.
- Roposch A, Reis M, Molina M, et al: Supracondylar fractures of the humerus associated with ipsilateral forearm fractures in children: a report of forty-seven cases, J Pediatr Orthop 21:307, 2001.
- Salter RB, Harris WR: Injuries involving the epiphyseal plate, J Bone Joint Surg 45A:587, 1963.
- Sanders WE, Heckman JD: Traumatic plastic deformation of the radius and ulna, Clin Orthop Relat Res 188:58, 1984.
- Shoemaker SK, Comstock CDP, Mubarak SJ, et al: Intramedullary Kirschner wire fi xation of open or unstable forearm fractures in children, J Pediatr Orthop 19:329, 1999.
- Smith VA, Goodman HJ, Strongwater MD, et al: Treatment of pediatric both-bone forearm fractures: a comparison of operative techniques, J Pediatr Orthop 25:309, 2005.
- Speed JS, Boyd HB: Treatment of fractures of the ulna with dislocation of the head of the radius (Monteggia fracture), JAMA 115:1900, 1940.
- Stanitski CL, Micheli LS: Simultaneous ipsilateral fractures of the arm and forearm in children, Clin Orthop Relat Res 153:218 1980.
- Tabak AY, Çelebi L, Murath HH, et al: Closed reduction and percutaneous fi xation of supracondylar fracture of the humerus and ipsilateral fracture of the forearm in children, J Bone Joint Surg 85B:1169, 2003.
- Theodorou SD, Ierodiaconou MN, Roussis N: Fracture of the upper end of the ulna associated with dislocation of the head of the radius in children, Clin Orthop Relat Res 228:240, 1988.
- Thompson JL: Acute plastic bowing of bone, J Bone Joint Surg 64B:123, 1982.
- Vainionpää S, Böstman O, Pätiälä H, et al: Internal fi xation of forearm fractures in children, Acta Orthop Scand 58:121, 1987.
- Van der Reis WL, Otsuka NY, Moroz P, et al: Intramedullary nailing versus plate fi xation for unstable forearm fractures in children, J Pediatr Orthop 18:9, 1998.
- Verstreken L, Delronge G, Lamoureux J: Shaft forearm fractures in children: intramedullary nailing with immediate motion: a preliminary report, J Pediatr Orthop 8:450, 1988.
- Vesely DG: Isolated traumatic dislocations of the radial head in children, Clin Orthop Relat Res 50:31, 1967.
- Vince KG, Miller JE: Cross-union complicating fracture of the forearm: II. Children, J Bone Joint Surg 69A:654, 1987.
- Vittas D, Larsen E, Torp-Pedersen S: Angular remodeling of midshaft forearm fractures in children, Clin Orthop Relat Res 265:261, 1991.
- Voto SJ, Weiner DS, Leighley B: Redisplacement after closed reduction of forearm fractures in children, J Pediatr Orthop 10:79, 1990.
- Voto SJ, Weiner DS, Leighley B: Use of pins and plaster in the treatment of unstable pediatric forearm fractures, J Pediatr Orthop 10:85, 1990.
- Vrsansky P, Bourdelat D, Al Faour A: Flexible stable intramedullary pinning technique in the treatment of pediatric fractures, J Pediatr Orthop 20:23, 2000.
- Walker JL, Rang M: Forearm fractures in children: cast treatment with the elbow extended, J Bone Joint Surg 73B:299, 1991.
- Walsh HPJ, McLaren CAN, Owen R: Galeazzi fractures in children, J Bone Joint Surg 69B:730, 1987.
- Weber BG, Brunner C, Frueler F, eds: Treatment of fractures in children and adolescents, New York, 1980, Springer-Verlag. Wiley JJ, Galey JP: Monteggia injuries in children, J Bone Joint Surg 67B:728, 1985.
- Wyrsch B, Mencio GA, Green NE: Open reduction and internal fi xation of pediatric forearm fractures, J Pediatr Orthop 16:644, 1996.
- Young S, Letts M, Jarvis J: Avascular necrosis of the radial head in children, J Pediatr Orthop 20:15, 2000.
- Yuan PS, Pring ME, Gaynor TP, et al:
You Might Also Like