Minimally Invasive Submuscular Plating for Pediatric Femur Fractures
Key Takeaway
Discover the latest medical recommendations for Minimally Invasive Submuscular Plating for Pediatric Femur Fractures. Submuscular bridge plating is a minimally invasive, soft tissue-preserving approach that provides relative stability for length-unstable pediatric diaphyseal femur fractures. It serves as a surgical treatment alternative to flexible elastic nailing for more complex cases, such as comminuted fractures or in children over 10 years old, offering a robust option for pediatric femur fractures.
Introduction and Epidemiology
Femur fractures are the most common cause of hospital admission due to orthopaedic trauma for pediatric patients. The management of pediatric femoral shaft fractures has evolved significantly over the past several decades, transitioning from prolonged immobilization in spica casts and traction to operative stabilization. Operative management mitigates the psychosocial and economic burdens of prolonged hospitalization, facilitates earlier mobilization, and reduces the risk of malunion and joint stiffness.
Submuscular bridge plating has emerged as a highly effective, minimally invasive, soft-tissue-preserving approach that provides relative stability for length-unstable pediatric diaphyseal femur fractures. By bypassing the fracture site and providing fixation proximally and distally, this technique preserves the fracture hematoma and the periosteal blood supply, thereby promoting rapid secondary bone healing through robust callus formation.
Epidemiology and Mechanism of Injury
Pediatric femur fractures exhibit a bimodal age distribution. The first peak occurs in early childhood (younger than 4 years old), often secondary to low-energy falls or non-accidental trauma. The second peak occurs in adolescence, typically resulting from high-energy mechanisms such as motor vehicle collisions, sports injuries, or falls from height. Male patients are disproportionately affected compared to female patients across both age peaks.
Fractures of the femoral diaphysis are significantly more common than those involving the trochanteric region or the distal femoral metaphysis. Because many of these injuries in older children represent high-energy trauma, a comprehensive trauma evaluation is mandatory. Concomitant injuries, including traumatic brain injury, visceral trauma, and other musculoskeletal injuries, must be systematically ruled out.
Child abuse (non-accidental trauma) must be a primary consideration in any pediatric patient presenting with a femur fracture, particularly in non-ambulatory children or those younger than 2 years of age. A thorough history detailing the mechanism of injury is critical; discrepancies between the reported mechanism and the developmental capabilities of the child or the severity of the fracture should prompt a multidisciplinary child protection evaluation, including a complete skeletal survey. Additionally, pathologic fractures must be considered. A detailed medical and family history may reveal underlying conditions such as osteogenesis imperfecta, cerebral palsy, or benign bone cysts, which predispose the pediatric femur to low-energy fractures.
Surgical Anatomy and Biomechanics
A thorough understanding of the femoral anatomy and the biomechanical principles of bridge plating is essential for successful execution of the submuscular plating technique.
Femoral Osteology and Soft Tissue Envelope
The pediatric femur exhibits an anterior and lateral bow, which must be accommodated during plate selection and contouring to prevent iatrogenic malalignment. The blood supply to the femoral diaphysis is dual-sourced: the endosteal supply via the nutrient artery (derived from the profunda femoris) and the periosteal supply via muscular attachments and perforating vessels. High-energy fractures often disrupt the endosteal supply, making the preservation of the periosteal blood supply critical for fracture union.

The submuscular plating technique exploits a safe internervous and avascular plane. The distal margin of the vastus lateralis lies deep to the iliotibial band and fascia lata, generally in line with the proximal pole of the patella. The muscle fibers of the distal vastus lateralis are oriented obliquely. Crucially, the vastus lateralis muscle belly is not densely adherent to the underlying lateral femoral periosteum. This anatomic relationship provides a natural, easily developable extraperiosteal plane between the muscle and the lateral femur, allowing for the seamless distal-to-proximal insertion of a plate without devitalizing the underlying bone.
Biomechanical Principles of Bridge Plating
Submuscular plating relies on the principles of relative stability. Unlike absolute stability (achieved via anatomic reduction and interfragmentary compression), relative stability tolerates micromotion at the fracture site, which stimulates cartilaginous and subsequent bony callus formation (secondary bone healing).
To optimize this biomechanical environment, surgeons must adhere to specific construct parameters:
1. Plate Span Ratio: The ratio of the plate length to the fracture length should be greater than 2 to 3 in comminuted fractures, and greater than 8 to 10 in simple fractures. A longer plate decreases the pull-out force on the terminal screws.
2. Screw Density: The ratio of inserted screws to the total number of plate holes should ideally be less than 0.5. Leaving holes empty over the fracture site increases the working length of the plate.
3. Working Length: This is the distance between the two innermost screws adjacent to the fracture. A longer working length decreases the stiffness of the construct, allowing for optimal interfragmentary strain (between 2% and 10%) that promotes callus formation while preventing implant fatigue failure.
Indications and Contraindications
Operative stabilization is the treatment of choice for pediatric femur fractures in most children from 5 years of age through skeletal maturity. While flexible intramedullary (IM) elastic nailing is highly successful for the majority of transverse or short oblique diaphyseal femur fractures, it has distinct biomechanical limitations.
Factors such as severe comminution, long oblique length-unstable fractures, and patient age greater than 10 years (or weight exceeding 50 kg / 110 lbs) are associated with unacceptably high complication rates when treated with flexible elastic nailing. These complications include loss of reduction, leg length discrepancy, and implant prominence.
For these complex fracture patterns and larger patients, submuscular bridge plating is highly indicated. It provides rigid stabilization, avoids the risk of avascular necrosis (AVN) of the femoral head associated with rigid antegrade trochanteric or piriformis entry nails, and easily spans the diaphyseal-metaphyseal junctions. Submuscular plating is also a reliable option for proximal or distal one-third femur fractures where flexible nails may fail to achieve adequate three-point fixation. However, adequate bone stock must exist to accommodate at least two to three screws in the proximal or distal fragment without violating the physis.
| Parameter | Operative Indications | Non-Operative Indications |
|---|---|---|
| Patient Age | 5 years to skeletal maturity (routine); <5 years with polytrauma or open fractures. | Birth to 5 years (isolated fractures). |
| Fracture Pattern | Comminuted, long oblique, spiral, length-unstable, polytrauma, open fractures. | Isolated, closed, stable fractures with acceptable shortening (<2 cm). |
| Patient Weight | >50 kg (indicates plating or rigid nail over flexible nails). | <20 kg (highly amenable to spica casting). |
| Associated Injuries | Floating knee, head trauma, vascular injury, compartment syndrome. | Isolated orthopaedic injury. |
| Specific Modality | Submuscular Plate: Length-unstable, comminuted, proximal/distal third, heavy child. Flexible Nails: Transverse, short oblique, midshaft, weight <50kg. |
Pavlik Harness: Infants <6 months. Spica Cast: 6 months to 4-5 years. |
A relative contraindication for submuscular plating is a purely transverse, length-stable midshaft fracture in a child under 50 kg, for which flexible IM nailing remains the gold standard due to its load-sharing characteristics and smaller incisions.
Pre Operative Planning and Patient Positioning
Thorough preoperative planning is fundamental to minimizing operative time and avoiding intraoperative complications.
Imaging and Templating
Standard anteroposterior (AP) and lateral radiographs of the entire injured femur are mandatory. Furthermore, imaging must include orthogonal views of the ipsilateral hip and knee. Pediatric femur fractures are high-energy injuries, and ipsilateral femoral neck fractures or physeal injuries around the knee can be easily missed if not actively excluded.

Preoperative templating utilizes the contralateral intact femur (if available) to determine the appropriate plate length and contour. The selected plate must be long enough to span the fracture site and allow for a minimum of three bicortical screws (or equivalent locking screws) in both the proximal and distal fragments. Narrow 4.5 mm locking compression plates (LCP) are typically utilized for older adolescents, while 3.5 mm LCPs may be appropriate for younger or smaller children (typically 5 to 8 years old). Pre-contouring the plate to match the anterior and lateral femoral bow is critical to prevent displacement of the fracture during screw insertion, particularly when using non-locking screws to draw the bone to the plate.
Operating Room Setup and Positioning
The procedure can be performed on a radiolucent flat-top table or a fracture table, depending on surgeon preference and the size of the child.
- Radiolucent Flat-Top Table: This is the preferred setup for many pediatric orthopaedic surgeons. The patient is placed supine with a radiolucent bump under the ipsilateral hip to internally rotate the leg, bringing the patella forward and neutralizing the natural external rotation of the lower extremity. This setup allows for free draping of the limb, facilitating intraoperative assessment of clinical alignment, rotation, and limb length.
- Fracture Table: This may be utilized for older, heavier adolescents to assist with sustained traction and length restoration. However, it restricts the ability to clinically assess rotation and requires meticulous fluoroscopic evaluation.

The C-arm fluoroscopy unit is typically positioned on the contralateral side of the table, perpendicular to the patient, allowing for easy transitions between AP and lateral views of the entire femur without compromising the sterile field.
Detailed Surgical Approach and Technique
The submuscular plating technique requires meticulous attention to soft tissue handling and fluoroscopic anatomy. The objective is to slide the plate extraperiosteally, reduce the fracture indirectly, and secure the construct without opening the fracture hematoma.
Incision and Superficial Dissection
The procedure begins with the determination of the plate insertion site, which is typically distal, though a proximal insertion can be utilized for distal third fractures.
For the standard distal-to-proximal insertion, a 3 to 5 cm longitudinal incision is made on the lateral aspect of the distal thigh, centered over the expected distal end of the plate. The incision is carried through the skin and subcutaneous tissue. The iliotibial band (fascia lata) is identified and incised longitudinally in line with its fibers.

Deep to the fascia lata, the vastus lateralis is visualized. The distal fibers of the vastus lateralis are carefully elevated off the lateral intermuscular septum. Using blunt dissection with a periosteal elevator or Cobb elevator, the extraperiosteal plane between the vastus lateralis and the lateral cortex of the femur is developed. It is imperative to stay strictly extraperiosteal to preserve the critical periosteal blood supply to the fracture fragments.
Submuscular Tunneling and Plate Insertion
Once the plane is established distally, an appropriately sized and pre-contoured locking compression plate is introduced into the submuscular tunnel. A tunneling instrument or a long Cobb elevator can be passed carefully along the lateral cortex, bridging the fracture site, to ensure the pathway is clear of soft tissue interposition.

The plate is inserted with the distal end held manually and the proximal end sliding cephalad. The plate must remain in constant contact with the lateral cortex to avoid wandering into the anterior or posterior musculature, which could endanger the neurovascular bundles (e.g., the profunda femoris posteriorly). Fluoroscopy is utilized continuously during this step to confirm the trajectory of the plate across the fracture site and to ensure it rests appropriately on the proximal fragment.
Fracture Reduction Strategies
Reduction is achieved indirectly. Because the fracture site is not exposed, the surgeon must rely on traction, percutaneous instruments, and the plate itself to restore length, alignment, and rotation.
- Length: Longitudinal traction is applied manually or via a femoral distractor. If a distractor is used, Schanz pins are placed percutaneously into the proximal and distal fragments, taking care to position them outside the planned footprint of the plate.
- Alignment (Coronal and Sagittal): Bumps placed under the thigh can correct sagittal plane deformities (apex posterior angulation). Percutaneous joysticks (Schanz pins) or a percutaneous pointed reduction clamp can be used to manipulate the fragments. The pre-contoured plate acts as a template; as the bone is brought to the plate, coronal and sagittal alignment are restored.
- Rotation: Assessing rotation is the most challenging aspect of indirect reduction. The surgeon must evaluate the cortical step sign at the fracture site under fluoroscopy. Additionally, comparing the profile of the lesser trochanter on the injured side to the contralateral normal hip (obtained during pre-op templating) on a true AP view provides an excellent radiographic proxy for femoral version. Clinically, with the patella facing directly anterior, the foot should exhibit symmetric external rotation compared to the uninjured side.

Plate Fixation Sequence
Once acceptable reduction is achieved and the plate is optimally positioned, fixation commences.
- Provisional Fixation: K-wires are placed through the proximal and distal ends of the plate to hold it provisionally to the bone. A proximal stab incision is made over the proximal end of the plate, localized via fluoroscopy. The iliotibial band and vastus lateralis are split bluntly to expose the plate holes.
- Initial Screw Placement: A non-locking cortical screw is typically placed first in the distal fragment to compress the plate to the bone. Next, a non-locking screw is placed in the proximal fragment. If there is a gap between the plate and the bone proximally, tightening this screw will draw the proximal fragment to the plate, effectively correcting varus or valgus malalignment (assuming the plate was contoured correctly).
- Construct Completion: After the initial non-locking screws have approximated the bone to the plate, locking screws are added to create a fixed-angle construct. This is particularly important in length-unstable or comminuted fractures where the plate must function as a load-bearing bridge. A minimum of three bicortical screws (or equivalent locking screws) should be placed in both the proximal and distal fragments.

Care must be taken to ensure that proximal screws do not violate the capital femoral physis or the trochanteric apophysis, and that distal screws remain proximal to the distal femoral physis.

Following final fluoroscopic confirmation of alignment, hardware placement, and fracture reduction in orthogonal planes, the wounds are irrigated. The fascia lata is closed with absorbable sutures, followed by standard closure of the subcutaneous tissue and skin.
Complications and Management
While submuscular plating is highly successful, it is not without potential complications. Recognizing these risks and understanding their management is critical for the orthopaedic surgeon.

The most unique complication in pediatric femur fractures is leg length discrepancy due to femoral overgrowth. The hyperemia associated with fracture healing stimulates the physes, leading to an average overgrowth of 1 to 2 cm in children aged 2 to 10 years. Therefore, anatomic reduction (end-to-end) in a younger child may paradoxically result in a longer limb at skeletal maturity. While bridge plating does not allow for controlled shortening (as spica casting does), the overgrowth phenomenon is generally less pronounced in older children and adolescents (the primary demographic for this procedure).
| Complication | Incidence | Etiology / Risk Factors | Prevention and Salvage Strategies |
|---|---|---|---|
| Hardware Prominence / Pain | 10% - 30% | Distal plate irritation of the IT band; inadequate soft tissue coverage. | Prevent by ensuring the plate sits flush against the bone. Salvage via elective hardware removal after complete radiographic consolidation (usually >12 months). |
| Leg Length Discrepancy (Overgrowth) | 5% - 15% | Hyperemic response stimulating physes (most common in ages 2-10). | Educate parents preoperatively. Minor discrepancies (<2 cm) are treated with shoe lifts. Major discrepancies may require contralateral epiphysiodesis near skeletal maturity. |
| Malunion (Varus/Valgus/Rotational) | 2% - 8% | Inadequate intraoperative reduction; failure to pre-contour plate. | Prevent by using the contralateral lesser trochanter profile for rotation and pre-contouring the plate to the femoral bow. Salvage requires corrective osteotomy and revision fixation. |
| Delayed Union / Nonunion | 1% - 3% | Stripping of periosteum; excessive construct rigidity (inadequate working length). | Prevent by strictly maintaining the extraperiosteal plane and leaving empty holes over the fracture. Salvage via dynamization (removing locking screws) or bone grafting with revision plating. |
| Implant Failure | < 2% | Premature weight-bearing; insufficient plate span ratio. | Ensure plate span ratio >3 for comminuted fractures. Strict adherence to NWB/TTWB protocols. Salvage requires revision open reduction internal fixation (ORIF) and bone grafting. |
| Infection | 1% - 2% | Open fractures; prolonged operative time; poor soft tissue envelope. | Prophylactic antibiotics; meticulous soft tissue handling. Treat with aggressive irrigation and debridement, culture-specific antibiotics, and retention of hardware until union if stable. |
Post Operative Rehabilitation Protocols
Postoperative rehabilitation must be tailored to the stability of the fixation, the quality of the bone, and the compliance of the pediatric patient.
In the immediate postoperative period, the extremity is not typically immobilized in a cast or splint, allowing for early mobilization of the hip and knee joints. This represents a significant advantage over non-operative management.
- Weight-Bearing Status: Because submuscular plating for comminuted fractures relies on a bridging construct that is load-sharing rather than load-bearing, patients are generally restricted to non-weight-bearing (NWB) or toe-touch weight-bearing (TTWB) with the assistance of crutches or a walker for the first 4 to 6 weeks.
- Physical Therapy: Early active and active-assisted range of motion (ROM) of the hip, knee, and ankle is encouraged immediately to prevent capsular contracture and muscle atrophy.
- Progression: At the 4-to-6-week postoperative visit, clinical and radiographic evaluations are performed. If bridging callus is visible on orthogonal radiographs and the patient is pain-free at the fracture site, weight-bearing is progressively advanced to weight-bearing as tolerated (WBAT). Full return to high-impact sports or contact activities is typically restricted until complete radiographic remodeling occurs, often 4 to 6 months postoperatively.
- Hardware Removal: Routine removal of asymptomatic plates in pediatric patients remains controversial. While some surgeons advocate for removal to prevent stress shielding or complications during future surgeries (e.g., adult total hip arthroplasty), the risk of refracture after plate removal, coupled with the risks of a second anesthetic, must be weighed carefully. Hardware removal is definitively indicated for symptomatic prominence, typically deferred until at least 12 to 18 months post-injury to ensure robust cortical remodeling.
Summary of Key Literature and Guidelines
The evolution of pediatric femur fracture management is heavily supported by orthopaedic literature and clinical practice guidelines. The American Academy of Orthopaedic Surgeons (AAOS) Clinical Practice Guideline on the Treatment of Pediatric Diaphyseal Femur Fractures provides evidence-based recommendations supporting operative intervention in older children.
Key literature has clearly delineated the boundaries of flexible intramedullary nailing. Studies by Flynn et al. and Moroz et al. established that flexible nailing in children weighing more than 50 kg or older than 10 years is associated with a significantly higher rate of poor outcomes, including loss of reduction and malunion.
Consequently, submuscular plating was popularized as a superior alternative for this demographic. Sink et al. demonstrated that submuscular plating provides excellent clinical and radiographic outcomes for length-unstable pediatric femur fractures, with high rates of union and low rates of complications. The technique's ability to preserve the fracture hematoma while providing rigid, fixed-angle stability (via locking screws) aligns perfectly with the biological principles of secondary bone healing described by Perren's strain theory.
Furthermore, comparative studies between submuscular plating and rigid trochanteric-entry intramedullary nailing have shown that while both provide excellent stability, plating completely circumvents the devastating, albeit rare, risk of avascular necrosis of the femoral head associated with rigid nailing in the skeletally immature patient. Plating also avoids the potential for proximal femoral valgus deformity or trochanteric arrest.
In conclusion, submuscular bridge plating stands as a highly reliable, biologically sound, and biomechanically robust surgical option. It is an indispensable technique in the armamentarium of the orthopaedic surgeon managing complex, length-unstable diaphyseal femur fractures in the pediatric and adolescent population.
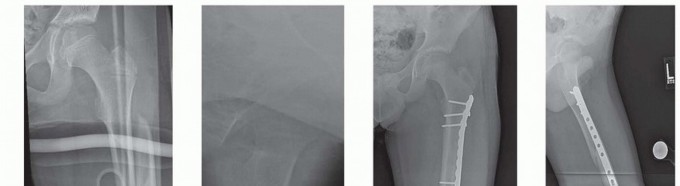
Clinical & Radiographic Imaging









You Might Also Like