Complex Pediatric Distal Tibial Physeal Fracture: Risks of Single-Sport Specialization
Key Takeaway
Complex pediatric distal tibial physeal fractures are diagnosed via clinical exam, plain X-rays, and essential CT scans. CT reveals precise fracture morphology, displacement, and articular involvement. This detailed imaging is critical for optimal treatment, especially for injuries linked to single-sport specialization in young athletes.
Patient Presentation & History
A 14-year-old male, Tanner Stage IV, presented to the emergency department following an acute injury to his right ankle during a competitive soccer match. The patient, a central midfielder, reported planting his right foot firmly while attempting a rapid directional change, followed by an immediate twisting sensation and a loud "pop" emanating from his ankle. He experienced instant, severe pain, rendering him unable to bear weight, and noted rapid swelling. There was no direct contact with another player or object at the time of injury.
Relevant history revealed the patient is a highly specialized athlete, having participated in competitive soccer year-round for the past seven years. His training regimen involved 5-6 days per week, often accumulating over 18 hours of high-intensity activity, split between his club team and school team commitments. He reported no structured off-season or regular cross-training in other sports. For the past six months, he had intermittently experienced a vague, deep-seated pain in his right distal tibia, particularly after prolonged training sessions, which he and his coaches attributed to "shin splints" and managed with rest and ice. There was no history of prior ankle sprains or significant lower extremity injuries. The patient denied any systemic comorbidities or relevant family medical history. He was otherwise fit and healthy, with no known allergies or regular medications. The mechanism described, an external rotation force on a planted foot, is characteristic of the injury sustained and is frequently observed in sports requiring rapid directional changes on varying surfaces. The insidious onset of prodromal symptoms, initially dismissed as overuse syndrome, is a critical component of the patient's history, highlighting the long-term impact of single-sport specialization and inadequate recovery.
Clinical Examination
Upon arrival, the patient was in acute distress due to pain.
Inspection:
The right ankle exhibited significant diffuse edema, particularly prominent over the distal aspect of the tibia and fibula, extending into the midfoot. Moderate ecchymosis was evident along the medial and lateral aspects of the ankle joint. There was a visible, subtle deformity with the foot appearing to be in slight external rotation relative to the tibia. Skin integrity was intact, with no open wounds or signs of impending compartment syndrome.
Palpation:
Marked tenderness was elicited circumferentially around the distal tibia and fibula, maximal over the distal tibial metaphysis, physis, and epiphysis. Specific point tenderness was noted over the anterolateral distal tibia and the medial malleolus. The syndesmosis was tender to palpation, and the distal fibula also had associated tenderness. Distal pulses (dorsalis pedis and posterior tibial) were palpable and strong bilaterally. Capillary refill was brisk in all toes.
Range of Motion (ROM):
Active and passive ankle ROM was severely restricted in all planes due due to pain and guarding. Dorsiflexion was approximately 0 degrees, plantarflexion 10 degrees, inversion 5 degrees, and eversion 0 degrees. Attempts at even gentle motion provoked significant pain.
Neurological Assessment:
Sensation was intact to light touch in the saphenous, superficial peroneal, deep peroneal, sural, and tibial nerve distributions. Motor function, assessed by toe plantarflexion and dorsiflexion, was limited by pain but no gross neurological deficits were identified.
Vascular Assessment:
Bilateral dorsalis pedis and posterior tibial pulses were 2+ and symmetrical. Capillary refill time was less than 2 seconds in all digits. No signs of compartment syndrome were present.
Stability Assessment:
Given the acute pain and likely fracture, no formal stress testing was performed. However, gross instability was appreciated with gentle manipulation. Proximal palpation of the tibia and fibula did not elicit pain, localizing the injury to the ankle joint and distal leg.
Imaging & Diagnostics
Plain Radiographs:
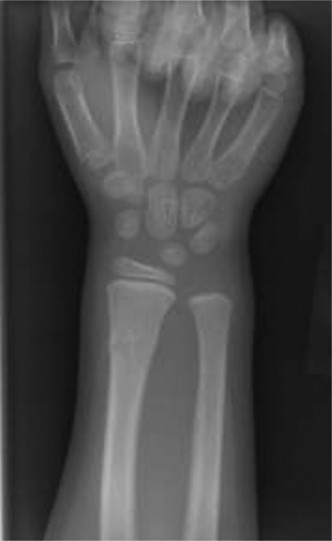
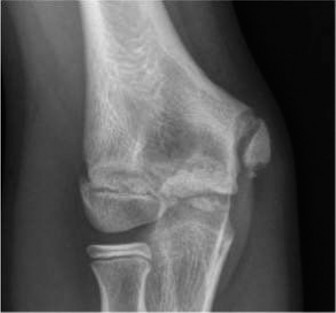
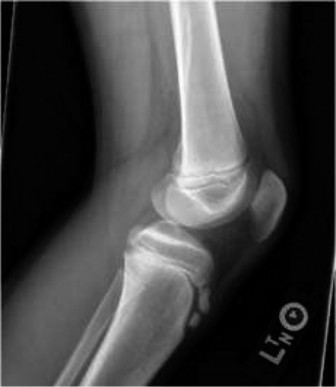
Initial radiographs of the right ankle included anteroposterior (AP), lateral, and mortise views.
* The AP view revealed a fracture line extending vertically through the lateral epiphysis of the distal tibia, indicative of a Tillaux-like component.
* The lateral view demonstrated a fracture line propagating horizontally through the distal tibial physis and then obliquely through the posterior metaphysis, consistent with a metaphyseal component. There was posterior displacement of the distal tibial fragment.
* The mortise view further highlighted the displacement of the lateral epiphyseal fragment, which remained attached to the fibula via the anterior inferior tibiofibular ligament. There was also widening of the distal tibiofibular clear space, suggesting syndesmotic involvement or rotational instability.
These findings were highly suggestive of a complex physeal injury involving the distal tibia.
Computed Tomography (CT) Scan:
Given the multiplanar nature of the injury and its involvement of the articular surface and physis, a non-contrast CT scan of the right ankle was immediately performed. The CT scan with multiplanar reconstructions (axial, sagittal, and coronal) was indispensable for delineating the precise fracture morphology, displacement, and articular involvement.
*
Axial views:
Clearly demonstrated the sagittal fracture through the lateral epiphysis (Type III component) and its extension to the lateral margin of the physis, as well as the coronal fracture component involving the posterior aspect of the metaphysis. Rotational displacement of the entire distal fragment was evident.
*
Sagittal views:
Provided detailed visualization of the posterior metaphyseal spike (Type II component) and the transverse physeal fracture. The extent of posterior displacement and angulation was precisely measured.
*
Coronal views:
Confirmed the involvement of the articular surface and the degree of lateral displacement of the epiphyseal fragment relative to the main tibial shaft.
The CT scan confirmed a
three-part (anterior, central, and posterior fragments) Triplane fracture of the distal tibia (Salter-Harris Type IV equivalent)
with significant posterior and rotational displacement of the combined epiphyseal-physeal-metaphyseal fragment. Crucially, it revealed an articular step-off of approximately 4mm and a rotational malalignment of 15 degrees, confirming the need for anatomical reduction. There was no evidence of concomitant fibular fracture. The syndesmotic widening observed on plain radiographs was further clarified as rotational malalignment rather than a true disruption requiring primary syndesmotic fixation.
Magnetic Resonance Imaging (MRI): Not typically indicated for acute Triplane fractures where CT provides sufficient bony detail for surgical planning. However, in cases with persistent pain post-reduction or concerns for occult osteochondral lesions, ligamentous instability beyond the immediate fracture, or growth plate bridge formation, MRI can be valuable. In this specific acute trauma, it was deemed unnecessary given the clear CT findings. Had the patient presented with chronic symptoms of ankle pain post-trauma or concerns for pre-existing stress response related to his specialization, MRI would have been a primary diagnostic tool.
Templating:
The CT images were used for meticulous pre-operative templating.
* 3D reconstructions were particularly useful for visualizing the fragment relationships and planning screw trajectories.
* Measurements of fragment size, displacement, and angular deformity guided the selection of appropriate fixation hardware (cannulated screws, K-wires).
* The plan was formulated to achieve anatomical reduction of the articular surface and physeal alignment, minimizing the risk of post-traumatic arthrosis and growth disturbance. The anticipated reduction maneuvers, including distraction, derotation, and direct fragment manipulation, were mentally rehearsed.
Differential Diagnosis
The presentation of acute ankle pain in an adolescent athlete requires careful differentiation to identify physeal injuries, which carry specific implications for growth and long-term joint function.
| Diagnosis | Key Clinical Features | Key Imaging Findings | Management Implications |
|---|---|---|---|
| Triplane Fracture (Distal Tibia) | Acute, severe ankle pain post-torsional injury. Inability to bear weight. Significant edema, ecchymosis, and palpable tenderness over distal tibia. Deformity (rotational, angulation). Often in 12-15 year olds. | X-ray: Apparent Salter-Harris II/III/IV depending on view. May see multiple fracture lines. CT: Definitive. Coronal metaphyseal component, transverse physeal component, sagittal epiphyseal component. Articular incongruity, displacement (posterior, rotational), widening of distal tibiofibular clear space. | Primary Diagnosis. Operative fixation (ORIF) is almost always indicated for displaced fractures to restore articular congruence and physeal alignment, preventing growth arrest and post-traumatic arthritis. Urgent evaluation for vascular compromise. |
| Tillaux Fracture (Distal Tibia) | Similar presentation to Triplane, often a supination-external rotation mechanism. More common in slightly older adolescents as physis begins to close laterally. | X-ray: Salter-Harris III involving the lateral epiphysis. Vertical fracture through epiphysis, horizontal through physis. CT: Crucial. Confirms sagittal epiphyseal fracture and absence of metaphyseal component. Assesses articular step-off. | Often requires ORIF if displaced (>2mm articular step-off) for anatomical reduction. Non-operative management with casting may be considered for truly non-displaced fractures. |
| Salter-Harris Type II Distal Tibia Fx | Acute ankle pain, swelling, tenderness over distal tibia. Less articular involvement. | X-ray: Fracture through the physis with a metaphyseal spike (Thurston-Holland sign). Epiphysis intact. CT: May be used to assess extent of metaphyseal component and rule out articular extension if suspected. | Most common physeal injury. Often amenable to closed reduction and cast immobilization. ORIF if irreducible or unstable after closed reduction. Prognosis for growth generally good if reduction is stable. |
| Isolated Lateral Malleolus Fracture | Lateral ankle pain, swelling, tenderness over lateral malleolus. May have an associated syndesmotic injury. | X-ray: Fracture line in the distal fibula. AP, lateral, mortise views to classify (e.g., Weber A, B, C or Lauge-Hansen). Rule out proximal fibula fracture (Maissoneuve). | Management depends on stability: non-operative (cast/boot) for stable fractures, ORIF for unstable fractures (e.g., displaced Weber B, Weber C, or associated syndesmotic disruption). |
| Severe Ankle Sprain | Acute ankle pain, swelling, ecchymosis. Mechanism often inversion or eversion. Tenderness over ligamentous structures, not bony prominences (though differentiating can be challenging acutely). | X-ray: No evidence of fracture. May show soft tissue swelling. MRI: Can confirm ligamentous disruption. Stress radiographs may show instability. | Non-operative management: RICE (Rest, Ice, Compression, Elevation), bracing, progressive rehabilitation focusing on proprioception and strengthening. Return to sport guided by functional recovery. |
| Tibial Stress Fracture (Progressed) | History of chronic, insidious, activity-related shin pain, exacerbated by activity, relieved by rest. Acute sudden pain after continued activity or minor trauma. | X-ray: May be normal in early stages. Later, cortical thickening, periosteal reaction, or a visible fracture line. MRI: Highly sensitive for stress response, marrow edema, and subtle fracture lines. | If complete fracture: often requires ORIF, especially if displaced or at high risk for nonunion (e.g., anterior cortex of tibia). If stress reaction/incomplete: rest, activity modification, gradual return to sport, addressing biomechanics and training load. |
Surgical Decision Making & Classification
The decision for operative intervention in this case was unequivocally indicated based on the patient's age, skeletal maturity, and the specific characteristics of the Triplane fracture:
1.
Articular Incongruity:
The CT scan demonstrated a 4mm articular step-off. Any intra-articular displacement exceeding 2mm in weight-bearing joints of active individuals, particularly adolescents with significant growth potential remaining, is a strong indication for anatomical reduction to prevent accelerated post-traumatic osteoarthritis.
2.
Physeal Displacement and Rotational Malalignment:
The significant displacement and 15 degrees of rotational malalignment of the physeal component carry a high risk of growth arrest (physeal bar formation), angular deformity, and functional impairment if not precisely reduced.
3.
Fragment Instability:
The Triplane fracture, by its very nature, is unstable due to its involvement across three planes (metaphyseal, physeal, epiphyseal, and articular components), making non-operative management prone to malunion or redisplacement.
4.
Patient's Activity Level:
As a highly competitive athlete, optimal restoration of joint mechanics and limb alignment was paramount for his long-term function and return to sport.
Classification:
The injury was classified as a
Salter-Harris Type IV equivalent Triplane fracture of the distal tibia
.
*
Salter-Harris Classification:
A system used for epiphyseal plate fractures.
*
Type I:
Fracture through the physis, often difficult to see on X-ray.
*
Type II:
Fracture through the physis and metaphysis (Thurston-Holland sign).
*
Type III:
Fracture through the physis and epiphysis, involving the articular surface (e.g., Tillaux fracture).
*
Type IV:
Fracture through the epiphysis, physis, and metaphysis, involving the articular surface. This is the classification our Triplane fracture primarily aligns with, though its complexity extends beyond a simple Type IV.
*
Type V:
Compression injury to the physis (rare, poor prognosis).
*
Triplane Fracture:
A unique variant of Salter-Harris fractures typically occurring in adolescents between 12-15 years, when the distal tibial physis is undergoing asymmetric closure (laterally-to-medially, posteriorly-to-anteriorly). The fracture pattern consists of:
* A sagittal fracture line through the epiphysis (Type III component).
* A transverse fracture line through the physis (shared by all types II, III, IV).
* A coronal fracture line through the posterior metaphysis (Type II component).
This creates three fragments (anterior/lateral epiphyseal, posterior metaphyseal, and the main tibial shaft) that are often displaced and rotated relative to each other. The specific displacement pattern often relates to the external rotation mechanism of injury.
The surgical objective was to achieve anatomical reduction of the articular surface, restore physeal alignment, and stabilize the fracture with appropriate internal fixation, considering the patient's remaining growth potential.
Surgical Technique / Intervention
Pre-Operative Preparation:
After obtaining informed consent, the patient received pre-operative intravenous antibiotics (Cefazolin 2g) within 60 minutes of incision. Standard fasting protocols were observed.
Patient Positioning:
The patient was positioned supine on a radiolucent operating table. A high thigh tourniquet was applied to the right lower extremity. A bump was placed under the ipsilateral hip to achieve neutral rotation of the limb. The image intensifier was positioned for optimal AP, lateral, and mortise views of the ankle, allowing for real-time fluoroscopic assessment during reduction and fixation.
Approach:
Given the predominant anterior and lateral epiphyseal component, and the posterior metaphyseal involvement, an
anterolateral approach
was primarily utilized to access the articular surface and the main epiphyseal fragment. An optional
posterolateral approach
could be considered if the posterior metaphyseal fragment required direct visualization for reduction, or if there was significant posterior displacement that could not be addressed adequately from anterior. In this case, reduction was achieved primarily via the anterolateral window.
1. A curvilinear incision approximately 5-7 cm in length was made, centered over the distal tibia, extending from just proximal to the joint line towards the base of the 4th metatarsal, between the tendons of the extensor digitorum longus (EDL) and peroneus tertius.
2. The superficial peroneal nerve branches were identified and carefully protected.
3. The extensor retinaculum was incised, and the interval between the EDL and peroneus tertius was developed, exposing the anterolateral aspect of the distal tibia, the fracture site, and the articular surface.
Reduction Techniques:
The goal was anatomical reduction of all three fragments to the main tibial shaft, prioritizing the articular surface.
1.
Initial Distraction:
Gentle traction was applied to the foot to aid in fragment disengagement and provide space for manipulation.
2.
Addressing Rotational Deformity:
The foot and distal fragment were gently derotated internally to counteract the external rotation mechanism of injury. This was guided by fluoroscopy and direct visualization of the fracture lines.
3.
Direct Fragment Manipulation:
*
Posterior Metaphyseal Fragment:
This fragment, often responsible for the posterior displacement, was initially addressed. A small periosteal elevator or a K-wire joystick was used to push the posterior fragment anteriorly, aligning it with the main tibial shaft.
*
Lateral Epiphyseal Fragment:
This fragment, containing the articular surface, was then reduced. Using a combination of gentle anterior translation and internal rotation of the foot, coupled with direct pressure on the fragment, anatomical reduction of the articular surface was meticulously achieved. The fracture line in the sagittal plane was directly visualized, and reduction was confirmed by palpating the articular surface for congruence.
4.
Temporary Fixation:
Once anatomical reduction was achieved, it was maintained with percutaneous 1.6mm or 2.0mm K-wires placed from the main epiphyseal fragment into the tibial shaft, ensuring they did not cross the physis or articular surface perpendicularly. Fluoroscopy (AP, lateral, mortise views) confirmed perfect alignment in all planes, with no residual articular step-off or physeal displacement.
Fixation Construct:
Stable internal fixation was performed using cannulated, partially threaded screws, selected to provide compression across the fracture planes while respecting the physis.
1.
Screw Placement for Epiphyseal Fragment:
One or two 3.5mm or 4.0mm cannulated partially threaded screws were placed from the anterolateral aspect of the reduced epiphyseal fragment. The screws were directed posteriorly and medially, parallel to the physis, crossing the intra-epiphyseal fracture line and engaging securely into the main tibial metaphysis. This trajectory avoids perpendicular physeal transgression, minimizing the risk of growth arrest. The partially threaded design allows for compression across the fracture.
2.
Screw Placement for Metaphyseal Fragment (if needed):
In some cases, if the posterior metaphyseal component remained unstable or could not be adequately controlled with the primary screws, an additional screw or K-wire from the posterior metaphyseal fragment into the main tibial shaft might be considered. However, in this instance, adequate stability was achieved with the anterolateral screw fixation after meticulous reduction.
3.
Syndesmotic Assessment:
Post-reduction, the syndesmosis was re-assessed under fluoroscopy with external rotation stress. If widening persisted (suggesting persistent instability despite anatomical reduction of the tibia), a temporary syndesmotic screw (e.g., 3.5mm cortical screw through 3 cortices) could be considered, typically removed at 6-8 weeks. In this case, the syndesmosis was stable after reduction of the Triplane fracture, indicating that the apparent widening was due to rotational malalignment of the distal tibial fragment.
4.
Final Fluoroscopic Check:
Final AP, lateral, and mortise views were obtained to confirm anatomical reduction, appropriate hardware placement, and absence of hardware prominence or intra-articular violation.
Closure:
The wound was copiously irrigated. The extensor retinaculum was loosely repaired. Subcutaneous tissues were closed with absorbable sutures, and the skin was closed with non-absorbable sutures. A sterile dressing was applied, followed by a well-padded posterior splint.
Post-Operative Protocol & Rehabilitation
Phase 1: Immediate Post-Operative (Weeks 0-6)
*
Immobilization:
A well-padded posterior splint immediately post-op, converted to a short leg cast (non-weight bearing) at the first post-operative visit (typically 7-10 days). The limb was kept elevated to minimize swelling.
*
Weight Bearing:
Strict non-weight bearing (NWB) on the operative extremity, utilizing crutches or a knee scooter.
*
Pain Management:
Multimodal analgesia.
*
Wound Care:
Daily dressing changes initially, monitoring for signs of infection. Suture removal at 2-3 weeks.
*
Goals:
Protect fixation, control pain and swelling, maintain skin integrity.
Phase 2: Early Mobilization & Protected Weight Bearing (Weeks 6-12)
*
Radiographic Assessment:
Radiographs (AP, lateral, mortise) at 6 weeks post-op to assess for early signs of fracture healing and maintain reduction.
*
Immobilization Change:
If radiographs show adequate healing, the cast is removed and replaced with a removable controlled ankle motion (CAM) boot.
*
Weight Bearing:
Gradual progression of weight bearing in the CAM boot, as tolerated, guided by pain and radiographic healing. Typically, touch-down weight bearing (TDWB) to partial weight bearing (PWB) over 2-4 weeks.
*
Physical Therapy:
Initiated with gentle active and passive range of motion exercises for the ankle and subtalar joints. Focus on scar management, edema control, and maintaining hip/knee strength. No aggressive stretching or forced movements.
*
Goals:
Restore initial ankle ROM, progress weight-bearing tolerance, begin light strengthening.
Phase 3: Strengthening & Proprioception (Weeks 12-20)
*
Weight Bearing:
Discontinue CAM boot as tolerated, transition to supportive athletic shoe. Full weight bearing (FWB) anticipated.
*
Physical Therapy:
Intensified strengthening program for ankle dorsiflexors, plantarflexors, invertors, and evertors. Incorporate balance and proprioception exercises (e.g., single-leg stance, wobble board). Initiate low-impact cardiovascular training (e.g., stationary bike, swimming).
*
Sport-Specific Drills (Non-Contact):
Begin sport-specific drills without impact or contact, such as dribbling drills, light jogging, agility ladders, and controlled passing.
*
Goals:
Achieve full pain-free ROM, symmetrical strength, improved proprioception, and re-establish basic movement patterns.
Phase 4: Return to Sport (Months 5-8+ post-op)
*
Criteria for Return:
Full, pain-free ROM; symmetrical strength (isokinetic testing >90% contralateral limb); excellent balance and proprioception; completion of sport-specific training. No residual pain or swelling.
*
Phased Return:
Gradual, progressive return to full sport activity, monitored closely by the coaching staff and medical team.
* Initially, limited participation in practice, avoiding full contact or high-intensity sprints/jumps.
* Progress to full practice participation.
* Return to competitive play with monitored game time.
*
Prevention Strategy:
Emphasize the importance of periodization, cross-training (e.g., swimming, cycling, resistance training), adequate rest and recovery periods (minimum 1-2 days/week, 2-3 months off a primary sport annually), and proper nutrition. Education for the athlete, parents, and coaches on the risks of single-sport specialization and overuse injuries.
*
Hardware Removal:
Typically not routine unless symptomatic (e.g., impingement, pain, infection). If indicated, it would be considered approximately 6-12 months post-surgery after fracture consolidation.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls
- High Index of Suspicion: Always suspect a physeal injury in adolescent athletes presenting with acute ankle trauma, especially with any history of chronic, insidious pain suggestive of overuse. The adolescent physis is weaker than surrounding ligaments and bone.
- Importance of Multiplanar Imaging: Plain radiographs are often insufficient for complex physeal fractures like Triplane injuries. CT scanning is mandatory for accurate diagnosis, precise characterization of fragment displacement (articular step-off, rotation, translation), and meticulous pre-operative planning. It is critical to obtain both two-dimensional reconstructions and three-dimensional models.
- Anatomic Reduction is Paramount: For intra-articular physeal fractures (Salter-Harris III and IV equivalents), anatomical reduction of the articular surface (ideally <1-2mm step-off) is critical to prevent post-traumatic arthritis. Furthermore, precise reduction of the physis is essential to minimize the risk of growth arrest and subsequent angular deformity.
- Surgical Timing: Displaced physeal fractures should be reduced promptly. While not an absolute emergency like an open fracture or compartment syndrome, delays can make reduction more challenging due to swelling and early callus formation.
- Physeal Sparing Fixation: The primary goal of fixation is to stabilize the reduction without violating the physis perpendicular to its axis in a way that risks growth arrest. Cannulated, partially threaded screws placed parallel to the physis (from epiphysis into metaphysis or across the epiphyseal fragment into the main epiphysis/metaphysis) are the preferred method. K-wires can be used for temporary fixation but generally do not provide adequate compression or stability for definitive fixation of a displaced Triplane fracture.
- Understanding Growth Plate Closure: Knowledge of the distal tibial physeal closure pattern (lateral to medial, posterior to anterior) is crucial. Triplane fractures typically occur in the transitional period of closure, often explaining the fracture morphology.
-
Addressing Etiology – Single Sport Specialization:
This case highlights the heightened risk of complex injuries in highly specialized adolescent athletes. Education for patients, parents, and coaches on injury prevention strategies, including:
- Periodization: Structured training with planned rest and recovery phases.
- Cross-Training: Participation in multiple sports or diverse athletic activities to develop balanced musculature and motor skills, reducing repetitive stress on specific anatomical areas.
- Adequate Rest: Minimum of 1-2 days/week away from organized sport and 2-3 months off the primary sport annually.
- Monitoring Training Load: Avoiding rapid increases in training volume or intensity.
- Nutrition and Sleep: Critical for recovery and growth.
Pitfalls
- Underestimating Displacement on Plain Radiographs: Triplane fractures can appear deceptively benign on initial X-rays, particularly in only one plane. Failure to obtain a CT scan can lead to missed articular step-off or rotational malalignment, resulting in inadequate treatment and long-term complications.
- Inadequate Reduction: Accepting residual articular incongruity or physeal displacement. Even small degrees of displacement (<2mm) can lead to significant issues over time in an active adolescent.
- Perpendicular Physeal Violation: Placing fixation hardware directly across the physis perpendicular to its orientation, especially with fully threaded screws, can lead to growth arrest or angular deformity. Careful pre-operative planning and intra-operative fluoroscopic guidance are essential.
- Overlooking Associated Injuries: Missing subtle fibular fractures, syndesmotic instability (if persistent after tibial reduction), or osteochondral lesions.
- Early Return to Sport: Allowing the athlete to return to high-intensity, specialized activity too soon, before complete fracture healing, adequate strength, and proprioceptive rehabilitation are achieved. This dramatically increases the risk of re-injury or new overuse injuries.
- Failure to Educate on Prevention: Not addressing the underlying contributing factors (e.g., single-sport specialization, excessive training volume) in the long-term management plan. Without lifestyle and training modifications, the athlete remains at high risk for future musculoskeletal pathology.

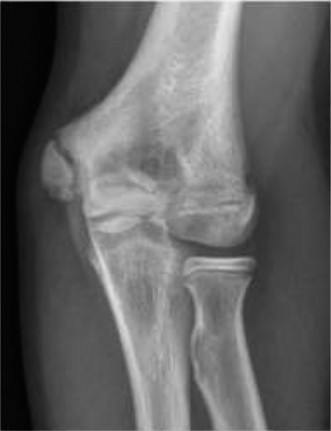
Clinical & Radiographic Imaging

You Might Also Like