Gas Gangrene and Soft Tissue Complications in Orthopaedic Trauma
Key Takeaway
Gas gangrene, primarily caused by Clostridium perfringens, is a life-threatening necrotizing soft tissue infection characterized by rapid myonecrosis and systemic toxicity. Successful orthopaedic management demands high clinical suspicion, immediate aggressive surgical debridement, and broad-spectrum intravenous antibiotics. This guide details the pathophysiology, surgical techniques for radical debridement, and evidence-based protocols for managing associated soft tissue complications, including fracture blisters and wound dehiscence, in high-energy trauma patients.
GAS GANGRENE AND CLOSTRIDIAL MYONECROSIS
The term "gas gangrene" historically implies a fulminant, life-threatening infection driven by the Clostridium species of anaerobic bacteria. However, in contemporary orthopaedic trauma, it is critical to recognize that many necrotizing soft tissue infections (NSTIs) presenting with subcutaneous gas are polymicrobial, caused by a synergistic mix of aerobic and anaerobic gram-negative and gram-positive bacteria. While Clostridium species can be cultured from approximately 30% of deep traumatic infections, only a fraction of these progress to true clostridial myonecrosis.
When true clostridial myonecrosis does occur, it is one of the most dramatic and rapidly progressive surgical emergencies in orthopaedics. The Clostridium species—most commonly C. perfringens, C. novyi, and C. septicum—cause the most devastating infections. Historically, these infections were highly lethal, with mortality rates reported at 40%. However, with the advent of aggressive early surgical intervention, modern critical care, and broad-spectrum antimicrobial therapy, recent reports have noted survival rates exceeding 90%.
Pathophysiology and Microbiology
Clostridium perfringens is responsible for approximately 90% of all gas gangrene infections. It is a gram-positive, spore-forming, obligate anaerobe ubiquitous in soil and the human gastrointestinal tract. The virulence of C. perfringens is mediated by its production of potent exotoxins. The organism produces four major lethal toxins: alpha, beta, epsilon, and theta.
Clinical Pearl: The alpha toxin (a phospholipase C/lecithinase) is the primary mediator of clostridial myonecrosis. It is profoundly hemolytic, destroying platelets and polymorphonuclear leukocytes (PMNs), and causes widespread capillary damage and microvascular thrombosis. This leads to a rapidly advancing zone of tissue hypoxia, creating an ideal anaerobic environment for further bacterial proliferation and gas production.
The theta toxin acts as a pore-forming cytolysin, further contributing to vascular leak, shock, and direct myocardial depression. The synergistic effect of these toxins results in the profound systemic toxicity, hemodynamic instability, and rapid tissue destruction characteristic of the disease.
Epidemiology and Historical Context
Gas gangrene has historically been intimately associated with war injuries, where high-energy penetrating trauma, gross soil contamination, and delayed surgical care created the perfect storm for clostridial proliferation.
* World War I: Gas gangrene occurred in 6% of open fractures and 1% of all open wounds.
* World War II: The frequency decreased to 0.7% due to earlier surgical debridement and the introduction of penicillin.
* Korean War: Incidence fell to 0.2%.
* Vietnam War: Incidence plummeted to 0.002% due to rapid helicopter evacuation and immediate surgical care.
Currently, in the United States, 1,000 to 3,000 cases of gas gangrene are reported annually. While it remains strongly associated with open fractures, agricultural injuries, and severe soft tissue crush trauma, it can also occur postoperatively (especially following lower extremity amputations for ischemia) or spontaneously (often linked to C. septicum in patients with underlying gastrointestinal malignancies or immunosuppression). Clostridial infections predominantly ravage soft tissues and skeletal muscle; they only rarely affect bone directly.
Clinical Presentation and Diagnosis
The hallmark of gas gangrene is pain out of proportion to the physical findings, often beginning within 12 to 24 hours of the initial injury or surgery.
- Early Signs: Severe, unrelenting pain, tachycardia (often out of proportion to fever), and a sense of impending doom. The skin may appear tense, pale, or bronzed.
- Late Signs: Development of hemorrhagic bullae, palpable crepitus (subcutaneous gas), a sweet or "mousy" foul odor, and profound septic shock.
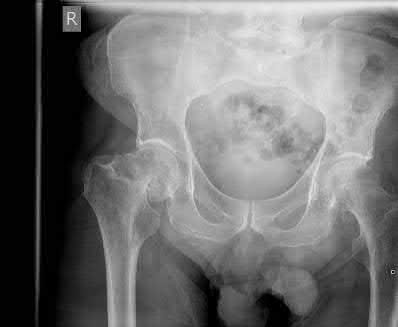
- Imaging: Radiographs may reveal feathery radiolucencies within the muscle planes, indicating gas tracking along fascial lines. However, the absence of radiographic gas does not rule out the diagnosis.
- Laboratory: Gram stain of wound exudate typically shows large, boxcar-shaped gram-positive rods with a conspicuous absence of polymorphonuclear leukocytes (due to destruction by the alpha toxin).
SURGICAL MANAGEMENT OF GAS GANGRENE
The most critical factors in the successful treatment of gas gangrene are early diagnosis and immediate, aggressive surgical intervention. Surgery must never be delayed for imaging or hyperbaric oxygen therapy.
Preoperative Preparation
- Hemodynamic Resuscitation: Aggressive intravenous fluid resuscitation and vasopressor support as needed.
- Empiric Antibiotics: Immediate administration of high-dose intravenous Penicillin G (to target Clostridium) combined with Clindamycin. Clindamycin is crucial as it binds to the 50S ribosomal subunit, halting the production of the deadly exotoxins. Broad-spectrum coverage (e.g., Vancomycin and Piperacillin-Tazobactam) should be added to cover polymicrobial necrotizing fasciitis until cultures result.
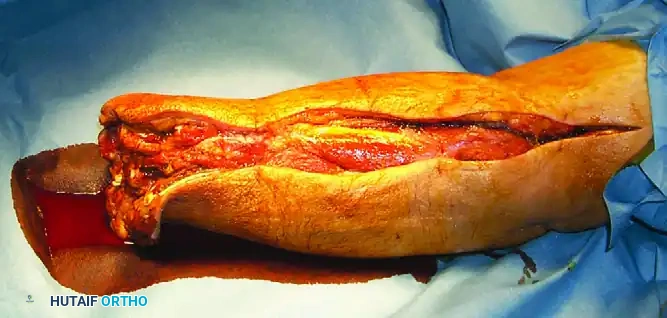
Surgical Approach and Radical Débridement
The goal of surgery is the complete extirpation of all necrotic, infected, and poorly perfused tissue.
- Positioning and Setup: Position the patient to allow circumferential access to the affected limb. Avoid the use of a tourniquet if possible, as it exacerbates tissue hypoxia and obscures the assessment of tissue viability (bleeding).
- Incision: Make generous, longitudinal incisions extending well beyond the clinically apparent margins of infection. Fasciotomies of all involved compartments are mandatory to relieve compartment syndrome secondary to profound edema.
- Tissue Assessment: Evaluate muscle viability using the classic "4 C's":
- Color: Viable muscle is beefy red; necrotic muscle is pale, gray, or "cooked" in appearance.
- Consistency: Viable muscle is firm; necrotic muscle is friable and mushy.
- Contractility: Viable muscle contracts when stimulated with electrocautery or forceps.
- Capacity to Bleed: Viable muscle bleeds briskly when cut.

Surgical Warning: In cases of fulminant clostridial myonecrosis, muscle necrosis advances at an alarming rate (up to several inches per hour). If radical debridement would render the limb functionless, or if the patient is in extremis and cannot tolerate a prolonged debridement, guillotine amputation is the life-saving procedure of choice. Do not hesitate to amputate to save the patient's life.
Postoperative Protocol and Hyperbaric Oxygen (HBO)
Following initial debridement, the wound is left open. The patient is transferred to the Intensive Care Unit (ICU) for ongoing resuscitation.
* Second-Look Surgery: A mandatory return to the operating room is scheduled within 24 hours for re-evaluation and further debridement.
* Hyperbaric Oxygen Therapy (HBO): The use of HBO remains controversial. Proponents argue that high oxygen tensions inhibit clostridial growth and halt alpha toxin production. Some studies report improved survival rates with rapid initiation of HBO. However, others dispute its value, citing the logistical difficulties of transporting critically ill patients and the risk of delaying essential surgical debridement. HBO is an adjunct, never a substitute for surgical debridement.
TETANUS PROPHYLAXIS IN ORTHOPAEDIC TRAUMA
Clostridium tetani, another spore-forming anaerobe, poses a significant risk in open orthopaedic injuries. According to a 2011 CDC report, an alarming 96% of patients who sought care for tetanus-prone wounds did not receive appropriate tetanus prophylaxis.
Orthopaedic surgeons must rigorously assess the tetanus vaccination status of all trauma patients. High-risk populations include:
* Individuals older than 65 years of age.
* Patients with poorly controlled diabetes mellitus.
* Intravenous drug users (IVDU).
Prophylaxis Guidelines:
* Clean, Minor Wounds: Administer Tdap or Td if it has been >10 years since the last dose.
* All Other Wounds (Contaminated, Puncture, Crush, Burns): Administer Tdap or Td if it has been >5 years since the last dose. If the patient has an unknown or incomplete vaccination history (<3 prior doses), both the vaccine (Tdap/Td) and Tetanus Immune Globulin (TIG) must be administered at separate anatomical sites.
MANAGEMENT OF SOFT TISSUE COMPLICATIONS
High-energy orthopaedic trauma imparts massive kinetic energy to the soft tissue envelope, leading to a cascade of complications that can jeopardize both limb salvage and fracture union.
Wound Dehiscence and Nutritional Optimization
Wound dehiscence following surgical fixation is frequently a harbinger of occult or impending deep infection.
* Surgical Management: The definitive treatment for dehiscence with underlying necrosis is prompt return to the operating room for formal surgical debridement of all non-viable tissue. Early consultation with plastic surgery is highly recommended to plan for soft tissue coverage (e.g., local rotational flaps or free tissue transfer).
* Nutritional Support: The metabolic demand of severe trauma and subsequent surgery is immense. Many trauma patients enter a catabolic state and develop rapid nutritional deficiencies during hospitalization, leading to impaired wound healing, immunosuppression, and infection.
* Protocol: Assess baseline nutritional markers (Prealbumin, Albumin, Total Lymphocyte Count). Initiate aggressive nutritional support via enteral feeding (preferred to maintain gut mucosal integrity) or parenteral nutrition if the enteral route is contraindicated.
Fracture Blisters (Blebs)
Fracture blisters are a direct consequence of high-energy trauma, severe soft tissue swelling, and local tissue hypoxia. They most commonly occur in areas with restricted skin mobility and minimal subcutaneous fat, such as the ankle, calcaneus, elbow, and tibia.
Histologically, fracture blisters resemble second-degree thermal burns, representing a cleavage at the dermal-epidermal junction due to profound interstitial edema. They are clinically categorized into two types:
- Clear Blisters: These represent an intraepidermal cleavage plane. The underlying dermis retains a thin layer of epithelial cells. They carry a lower risk of infection, and surgical incisions through these areas, while not ideal, are generally better tolerated.
- Bloody Blisters: These represent a deeper, subepidermal cleavage plane. The dermis is completely stripped of its protective epithelial cover, exposing the deep dermal vascular plexus. Bloody blisters carry a significantly higher risk of colonization and deep infection; surgical incisions through bloody blisters should be strictly avoided.
Management Protocols for Fracture Blisters:
* Conservative/Delayed Approach: If clinically feasible, the limb is elevated, and the blisters are allowed to resolve spontaneously. This process typically takes 10 to 14 days, after which surgical fixation can proceed safely.
* Aggressive "Burn Protocol" Approach: For patients requiring earlier intervention, an aggressive burn-care protocol can be utilized. This involves:
* Strict sterile technique in the operating room or at the bedside.
* Surgical excision (unroofing) of the necrotic blister canopy.
* Application of 1% Silver Sulfadiazine (Silvadene) ointment dressings daily.
* Outcome: Utilizing this protocol, stable epithelialization is often attained more rapidly (within 5 to 10 days), with a reduced incidence of superficial bacterial colonization.
Timing of Surgical Intervention: The "Wrinkle Test"
Post-traumatic swelling is a primary limiting factor in the timing of definitive open reduction and internal fixation (ORIF). Premature surgical incision through massively swollen, non-compliant skin dramatically increases the risk of wound necrosis, dehiscence, and deep infection.
Clinical Pearl: The timing of surgery should be dictated by the soft tissue envelope, not the calendar. We prefer to delay definitive surgery until the "Wrinkle Test" is positive. The skin must demonstrate fine wrinkling on clinical examination, indicating that the interstitial edema has subsided and the skin possesses adequate pliability to support surgical retraction and tension-free closure.
THROMBOEMBOLIC COMPLICATIONS
Orthopaedic trauma patients are at an exceptionally high risk for venous thromboembolism (VTE), including deep vein thrombosis (DVT) and pulmonary embolism (PE), due to the fulfillment of Virchow’s Triad: endothelial injury (trauma/surgery), venous stasis (immobilization), and hypercoagulability (systemic inflammatory response to injury).
While fatal pulmonary emboli are relatively rare in the modern trauma setting, the occurrence of non-fatal PE or extensive DVT significantly complicates the patient's hospital course, delays further surgical interventions, and increases long-term morbidity (e.g., post-thrombotic syndrome).
Prophylaxis and Management:
* Mechanical Prophylaxis: Sequential compression devices (SCDs) should be applied to the uninjured extremities immediately upon admission.
* Chemoprophylaxis: Low-molecular-weight heparin (LMWH), such as Enoxaparin, is the gold standard for VTE prophylaxis in orthopaedic trauma. It should be initiated as soon as it is deemed safe from a bleeding perspective (typically within 24-48 hours post-injury or post-operatively, barring traumatic brain injury or solid organ lacerations).
* Surveillance: Routine screening duplex ultrasonography is generally not recommended for asymptomatic patients, but a low threshold for diagnostic imaging (Venous Doppler or CT Pulmonary Angiography) must be maintained for any patient exhibiting unexplained tachycardia, hypoxia, or asymmetric limb swelling.
📚 Medical References
- Gas gangrene complicating open forearm fractures: report of fi ve cases, J Bone Joint Surg 59A:135, 1977.
- Robertson P, Karol LA, Rab GT: Open fractures of the tibia and femur in children, J Pediatr Orthop 16:621, 1996.
- Roy DR, Crawford AH: Operative management of fractures of the shaft of the radius and ulna, Orthop Clin North Am 21:245, 1990.
- [
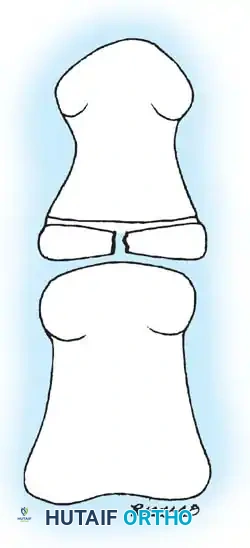
Fig. 33-213 Fissuring (not fracture) of physis of proximal phalanx of great toe. (Redrawn from Lyritis G: Developmental disorders of the proximal epiphysis of the hallux, Stereoradiology 10:250, 1983.)
Skaggs DL, Kautz SM, Kay RM, et al: Effect of delay of surgical treatment on rate of infection in open fractures in children, J Pediatr Orthop 20:19, 2000.](https://pubmed.ncbi.nlm.nih.gov/?term=%21%5BFig.%2033-213%20Fissuring%20%28not%20fracture%29%20of%20physis%20of%20proximal%20phalanx%20of%20great%20toe.%20%28Redrawn%20from%20Lyritis%20G%3A%20Developmental%20disorders%20of%20the%20proximal%20epiphysis%20of%20the%20hallux%2C%20Stereoradiology%2010%3A250%2C%201983.%29%5D%28/media/hutaifortho/hutaifortho-references-p1714-66072c.webp%29%0A%0A%2AFig.%2033-213%20Fissuring%20%28not%20fracture%29%20of%20physis%20of%20proximal%20phalanx%20of%20great%20toe.%20%28Redrawn%20from%20Lyritis%20G%3A%20Developmental%20disorders%20of%20the%20proximal%20epiphysis%20of%20the%20hallux%2C%20Stereoradiology%2010%3A250%2C%201983.%29%2A%0A%0ASkaggs%20DL%2C%20Kautz%20SM%2C%20Kay%20RM%2C%20et%20al%3A%20Effect%20of%20delay%20of%20surgical%20treatment%20on%20rate%20of%20infection%20in%20open%20fractures%20in%20children%2C%20J%20Pediatr%20Orthop%2020%3A19%2C%202000.)
- Song KM, Sangeorzan B, Benirschke S, et al: Open fractures of the tibia in children, J Pediatr Orthop 16:635, 1996.
- Walker RN, Green NE, Spindler KP: Stress fractures in skeletally immature patients, J Pediatr Orthop 16:578, 1996.
- Hand and Wrist Fractures, Dislocations, and Fracture-Dislocations Abram LJ, Thompson GH: Deformity after premature closure of the distal radial physis following a torus fracture with a physeal compression injury: report of a case, J Bone Joint Surg 69A:1450, 1987.
- Al-Qattan MM: Phalangeal neck fractures in children: classifi cation and outcome in 66 cases, J Hand Surg 26B:112, 2001.
- Beatty E, Light TR, Belsole RJ, et al: Wrist and hand skeletal injuries in children, Hand Clin 6:723, 1990.
- Blount WP: Fractures in children, Baltimore, 1955, Williams & Wilkins. Campbell RM: Operative treatment of fractures and dislocations of the hand and wrist region in children, Orthop Clin North Am 21:217, 1990.
- Coonrad RW, Pohlman MH: Impacted fractures in the proximal portion of the proximal phalanx of the fi nger, J Bone Joint Surg 51A:1291, 1969.
- Crick JC, Franco RS, Conner JJ: Fractures about the interphalangeal joints in children, J Orthop Trauma 1:318, 1988.
- Dameron TB: Traumatic dislocation of the distal radioulnar joint, Clin Orthop Relat Res 83:55, 1972.
- Davidson JS, Brown DJ, Barnes SN, et al: Simple treatment for torus fractures of the distal radius, J Bone Joint Surg 83B:1173, 2001.
- Farabeuf LHF (as quoted by Barnard HL): Dorsal dislocation of the fi rst phalanx of the little fi nger: reduction by Farabeuf’s dorsal incision, Lancet 1:88, 1901.
- Gamble JG, Simmons SC: Bilateral
You Might Also Like