Operative Management of Suprascapular Nerve Pathology and Spinal Accessory Nerve Neurotization
Key Takeaway
The suprascapular nerve is highly susceptible to entrapment and traumatic injury, leading to profound shoulder dysfunction. This comprehensive guide details the surgical anatomy, clinical evaluation, and operative management of suprascapular neuropathy. It provides a step-by-step masterclass on the Mackinnon and Colbert technique for neurotization using the spinal accessory nerve, alongside protocols for managing brachial plexus compression syndromes.
INTRODUCTION TO SUPRASCAPULAR NERVE PATHOLOGY
The suprascapular nerve (SSN) is a critical mixed motor and sensory peripheral nerve responsible for the dynamic stability and functional kinematics of the shoulder girdle. It provides the primary motor innervation to the supraspinatus and infraspinatus muscles, facilitating shoulder abduction and external rotation. Pathologic conditions affecting the SSN range from chronic entrapment neuropathies at the suprascapular or spinoglenoid notches to devastating traction injuries associated with upper trunk brachial plexus avulsions.
When the SSN is irreparably damaged—such as in severe brachial plexus injuries—nerve transfer (neurotization) becomes the gold standard for restoring shoulder function. The transfer of the distal spinal accessory nerve (SAN) to the suprascapular nerve, popularized by Mackinnon and Colbert, is a highly reliable procedure that leverages a synergistic motor donor to reanimate the rotator cuff.
SURGICAL ANATOMY OF THE SUPRASCAPULAR NERVE
A profound understanding of the SSN's anatomical course is mandatory for safe surgical exploration, decompression, and neurotization.
Origin and Proximal Course
Arising primarily from the upper trunk of the brachial plexus (C5, C6 nerve roots, with variable contribution from C4), the SSN courses through the posterior triangle of the neck. It runs parallel to the posterior belly of the omohyoid muscle, passing deep to the anterior border of the trapezius muscle as it descends toward the superior border of the scapula.
The Suprascapular Notch
The nerve traverses the suprascapular notch, a critical anatomic bottleneck. It passes deep (inferior) to the superior transverse scapular ligament.
Surgical Pearl: The "Army over Navy" Rule
At the suprascapular notch, the suprascapular Artery passes over the superior transverse scapular ligament, while the suprascapular Nerve passes under the ligament. This relationship is critical during surgical release to avoid catastrophic vascular injury.
Distal Course and Innervation
Upon entering the supraspinatus fossa, the SSN provides:
* Motor branches to the supraspinatus muscle.
* Articular branches to the glenohumeral and acromioclavicular joints (providing up to 70% of the sensory innervation to the shoulder capsule).
The nerve then courses around the lateral border of the scapular spine through the spinoglenoid notch (deep to the spinoglenoid ligament) to enter the infraspinatus fossa, where it terminates by providing motor innervation to the infraspinatus muscle.
CLINICAL EVALUATION AND DIAGNOSIS
Mechanisms of Injury
The SSN is vulnerable to injury via multiple mechanisms:
* Traction/Trauma: High-energy anterior shoulder dislocations, clavicle fractures, or fractures of the superolateral scapula involving the notch.
* Iatrogenic: Penetrating trauma or oncologic resections in the posterior triangle of the neck.
* Entrapment: Chronic microtrauma in overhead athletes (volleyball, baseball) leading to hypertrophy of the transverse scapular ligament.
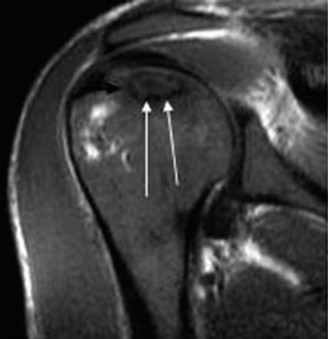
* Space-Occupying Lesions: Paralabral cysts (ganglions) associated with superior labral anterior-posterior (SLAP) tears, typically compressing the nerve at the spinoglenoid notch.
Physical Examination
Patients typically present with vague, deep, aching pain in the posterior shoulder, accompanied by weakness in abduction and external rotation.
- Proximal Lesions (Suprascapular Notch): Result in profound atrophy of both the supraspinatus and infraspinatus muscles. Weakness is noted in both initial shoulder abduction and external rotation.
- Distal Lesions (Spinoglenoid Notch): Result in isolated atrophy of the infraspinatus muscle. The supraspinatus remains intact. Patients exhibit isolated weakness in external rotation, often with a positive external rotation lag sign.
Clinical Pitfall:
Isolated infraspinatus atrophy is frequently misdiagnosed as a massive rotator cuff tear. Always maintain a high index of suspicion for a spinoglenoid notch cyst, especially in younger patients or overhead athletes.
Diagnostic Modalities
- Electromyography (EMG) and Nerve Conduction Studies (NCS): The gold standard for confirming denervation, localizing the level of compression, and assessing the severity of axonal loss.
- Magnetic Resonance Imaging (MRI): Essential for identifying space-occupying lesions (e.g., paralabral cysts) and assessing the degree of fatty infiltration and muscle atrophy in the rotator cuff.
BRACHIAL PLEXUS COMPRESSION SYNDROME (PECTORALIS MINOR SYNDROME)
While evaluating shoulder and periscapular pain, the surgeon must consider proximal compression syndromes. The neurovascular bundle exiting the thorax may be compressed by the pectoralis minor tendon at its coracoid attachment.
Pathophysiology
Originally described by Wright in 1945 as "hyperabduction syndrome," this condition occurs when the axillary artery and brachial plexus cords are tethered and compressed beneath the taut pectoralis minor tendon during prolonged shoulder hyperabduction.
Clinical Presentation
- Aching pain in the arm and shoulder, frequently referred to the anterior chest and periscapular region.
- Symptoms are reliably reproduced by sustained abduction and external rotation of the arm (Wright's test) or by direct palpation over the coracoid process.
- Paresthesias in the distribution of the lower trunk (C8-T1) may be present.
Management
- Conservative: The first line of treatment includes postural re-education, scapular stabilization exercises, and heat therapy. Avoidance of provocative hyperabduction is paramount.
- Surgical: In refractory cases with persistent pain and documented neurovascular compromise (via angiography or EMG), surgical release of the pectoralis minor tendon from the coracoid process is indicated.
OPERATIVE TECHNIQUE: NEUROTIZATION OF THE SUPRASCAPULAR NERVE WITH THE SPINAL ACCESSORY NERVE
When the SSN is irreparably injured proximally (e.g., upper trunk avulsion), neurotization using the distal spinal accessory nerve (SAN) is the procedure of choice. The Mackinnon and Colbert technique provides a reliable, tension-free coaptation via a posterior approach.
Indications
- C5-C6 brachial plexus root avulsions.
- Upper trunk ruptures not amenable to primary grafting.
- Severe, delayed proximal SSN injuries with viable distal motor endplates (ideally performed within 6 to 9 months of injury).
Preoperative Planning
Confirm the functional integrity of the spinal accessory nerve and the trapezius muscle clinically and electrodiagnostically. The distal SAN (innervating the lower trapezius) is utilized, preserving the proximal branches to the upper trapezius to maintain shoulder elevation.
Patient Positioning and Anesthesia
- Position: The patient is placed in the prone position. All pressure points are meticulously padded. The operative shoulder, arm, and hemithorax are prepped and draped free to allow intraoperative manipulation.
- Anesthesia: General anesthesia without long-acting paralytics is mandatory to allow for intraoperative nerve stimulation.
Step-by-Step Surgical Approach (Mackinnon and Colbert)
1. Incision and Superficial Dissection
- Identify the anatomic landmarks: the spine of the scapula, the acromion, and the expected location of the suprascapular notch.
- Mark a transverse incision approximately 2 cm superior and parallel to the spine of the scapula, centered over the suprascapular notch.
- Incise the skin and subcutaneous tissue, carrying the dissection down to the investing fascia of the trapezius muscle.
2. Trapezius Split and Deep Dissection
- Split the trapezius muscle bluntly along the transverse course of its muscle fibers. Retract the split edges to reveal the underlying supraspinatus muscle and the fat pad occupying the suprascapular fossa.
- Carry the dissection bluntly over the superficial fascia of the supraspinatus muscle, directing the approach anteriorly and medially toward the superior border of the scapula.
3. Identification of the Suprascapular Notch
- Palpate the superior border of the scapula to identify the distinct U- or V-shaped suprascapular notch.
- Utilize blunt dissection (e.g., a "peanut" sponge or Kittner) to clear the overlying fibrofatty tissue and expose the superior transverse scapular ligament.
Surgical Warning:
The suprascapular artery courses directly over the superior transverse scapular ligament. It must be meticulously identified, isolated, and protected with a vessel loop before any attempt is made to divide the ligament.
4. Ligament Release and Nerve Isolation
- While protecting the artery, divide the superior transverse scapular ligament under direct vision using a scalpel or Kerrison rongeur.
- Identify the suprascapular nerve lying deep within the notch.
- Use a handheld nerve stimulator to stimulate the SSN. In the setting of a complete proximal injury, there will be a confirmed lack of motor response in the supraspinatus and infraspinatus muscles.
- Dissect the SSN as far proximally (anteriorly) as possible into the posterior triangle to maximize nerve length. Transect the nerve proximally, preparing it for a tension-free repair.
5. Identification of the Spinal Accessory Nerve
- Direct the subtrapezius dissection medially toward the vertebral border of the scapula.
- Identify the distal spinal accessory nerve on the deep surface of the trapezius muscle, accompanied by the transverse cervical artery and vein.
- Stimulate the SAN to confirm robust trapezius contraction.
- Dissect the SAN distally to gain adequate length, then transect it, ensuring that proximal branches to the upper and middle trapezius are preserved.
6. Microsurgical Coaptation (Neurorrhaphy)
- Transpose the proximal stump of the distal SAN laterally toward the distal stump of the SSN.
- Ensure the nerve ends meet with absolutely zero tension. If tension is present, further mobilize the nerves or consider an interpositional nerve graft (though primary coaptation is vastly superior).
- Under the operating microscope, trim the epineurium of both nerve ends to expose healthy, pouting fascicles.
- Perform an epineurial repair using 4 to 6 interrupted 8-0 or 9-0 nylon sutures.
- Supplement the repair with fibrin glue to seal the coaptation site and prevent axonal escape.
Closure
- Irrigate the surgical bed copiously.
- Achieve meticulous hemostasis to prevent postoperative hematoma, which can compress the neurorrhaphy.
- Close the trapezius fascia with absorbable sutures.
- Close the subcutaneous tissue and skin in a standard layered fashion.
POSTOPERATIVE PROTOCOL AND REHABILITATION
The success of a nerve transfer relies heavily on strict adherence to postoperative immobilization and a phased rehabilitation program.
Phase I: Protection (Weeks 0-4)
- The patient is placed in a shoulder immobilizer or sling with an abduction pillow immediately postoperatively.
- The primary goal is to prevent any traction across the neurorrhaphy site.
- Active and passive range of motion (ROM) of the elbow, wrist, and hand are encouraged to prevent distal stiffness.
- Shoulder ROM is strictly prohibited.
Phase II: Early Mobilization (Weeks 4-8)
- The sling is gradually weaned.
- Initiate gentle, therapist-assisted passive ROM of the shoulder, focusing on forward elevation and external rotation.
- Avoid aggressive stretching or sudden, jerky movements.
Phase III: Motor Re-education (Months 2-12+)
- Nerve regeneration occurs at a rate of approximately 1 mm per day. Clinical signs of reinnervation (e.g., advancing Tinel's sign, palpable muscle flicker) may take 4 to 6 months to appear.
- Once early motor function is detected (usually via EMG first, then clinically), initiate biofeedback and motor re-education.
- Patients are taught to consciously contract the trapezius (shoulder shrug) to initiate supraspinatus and infraspinatus activation (shoulder abduction and external rotation). Over time, neuroplasticity allows this movement to become intuitive and independent.
- Progressive resistance exercises are introduced only after the muscle achieves a grade 3/5 strength on manual muscle testing.
COMPLICATIONS AND PITFALLS
While the SAN to SSN transfer is highly successful, surgeons must be vigilant regarding potential complications:
- Vascular Injury: Inadvertent laceration of the suprascapular artery during notch decompression can lead to massive hemorrhage, obscuring the surgical field and risking ischemic damage to the nerve.
- Tension at the Coaptation Site: The most common cause of neurotization failure. If the nerves do not meet passively, the surgeon must aggressively mobilize the SAN or accept the use of a short sural nerve graft.
- Inadequate Proximal Dissection: Failure to dissect the SSN far enough proximally through the notch will result in insufficient length for a primary repair.
- Donor Site Morbidity: Over-harvesting the SAN too proximally can denervate the upper trapezius, leading to profound shoulder drooping and secondary impingement. Always stimulate and preserve the proximal branches.
- Failure of Reinnervation: Can occur due to delayed surgical intervention (motor endplate degradation), poor microsurgical technique, or postoperative hematoma.
By adhering to meticulous microsurgical principles, respecting the complex anatomy of the suprascapular notch, and executing a tension-free neurorrhaphy, the orthopaedic surgeon can reliably restore critical shoulder function in patients with devastating upper trunk brachial plexus injuries.
You Might Also Like