Post-Traumatic Elbow Contracture: Diagnosis & Management of Heterotopic Ossification
Key Takeaway
Severe post-traumatic elbow stiffness often results from heterotopic ossification (HO), where bone forms in soft tissues after injury or surgery. Diagnosis involves detailed patient history, clinical examination, and advanced imaging like CT scans with 3D reconstructions to precisely map HO and plan effective surgical management, restoring essential range of motion.
Patient Presentation & History
A 48-year-old right-hand dominant male presented to our clinic with a chief complaint of progressively worsening right elbow stiffness and pain, significantly impacting his daily activities and work. His history dates back eight months prior, following a high-energy motor vehicle accident (MVA) in which he sustained a comminuted right distal humerus fracture (AO/OTA 13-C2) and an ipsilateral radial head fracture.
The initial injury was managed surgically with open reduction and internal fixation (ORIF) of the distal humerus using a dual-plate construct (medial and lateral columns) and excision of the radial head due to comminution that was deemed unreconstructable. Post-operatively, he was immobilized in a long-arm splint for three weeks, followed by a referral for physical therapy. Despite diligent adherence to the physical therapy regimen for five months, his elbow range of motion (ROM) plateaued and then progressively deteriorated.
At presentation, he reported an inability to fully extend or flex his elbow, making tasks such as reaching for objects overhead, grooming, and working at a computer extremely difficult. He described the pain as a dull ache at rest, intensifying to a sharp, restrictive pain at the end-range of attempted motion. He denied any acute trauma since the initial injury.
His past medical history is notable for well-controlled hypertension and a 20-pack-year smoking history, which he quit six months prior. He has no history of head trauma or burns. His occupation involves manual labor, making functional elbow motion critical for his livelihood.
Clinical Examination
Inspection
On visual inspection, the right elbow demonstrated significant soft tissue scarring consistent with his prior surgical incision, extending along the posterior aspect of the distal arm and elbow. There was mild efferent swelling but no overt erythema or signs of active infection. The carrying angle appeared subtly altered, favoring a slight valgus deformity, though this was difficult to ascertain definitively given the contracture. Marked atrophy of the triceps and forearm musculature was evident compared to the contralateral limb. No skin tenting or open wounds were present.
Palpation
Palpation revealed a firm, non-tender mass along the posterior-medial aspect of the elbow, extending from the distal humerus to the proximal ulna, suggestive of heterotopic ossification (HO). Tenderness was elicited over the medial and lateral epicondyles with deep palpation. The ulnar nerve groove felt thickened and somewhat immobile at the cubital tunnel. There was no palpable joint effusion. The surgical hardware appeared well-seated, with no signs of prominence or superficial irritation.
Range of Motion (ROM)
Active and passive ROM measurements were performed, demonstrating severe limitations:
*
Flexion-Extension Arc:
From 70 degrees of extension deficit (meaning 70 degrees was his maximal extension) to 105 degrees of flexion. This represents a severely restricted arc of 35 degrees (70-105 degrees).
*
End-feel:
Both extension and flexion had a hard, bony end-feel.
*
Forearm Rotation:
Pronation was limited to 45 degrees (normal 80-90 degrees), and supination was limited to 30 degrees (normal 80-90 degrees). These limitations were likely secondary to capsular and soft tissue contracture, as well as the radial head excision.
Neurological and Vascular Assessment
Neurological examination of the right upper extremity revealed mild paresthesia in the ulnar nerve distribution (small finger and ulnar half of the ring finger). Sensation to light touch and two-point discrimination was diminished in this area. Motor strength testing demonstrated mild weakness of the flexor carpi ulnaris (FCU) and the interossei (Grade 4/5), consistent with mild ulnar neuropathy. The median and radial nerves were intact with no motor or sensory deficits. Radial and ulnar pulses were 2+ bilaterally, and capillary refill was prompt.
Imaging & Diagnostics
X-ray Findings
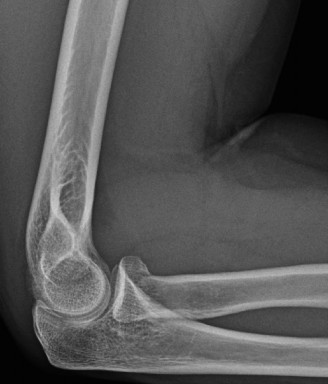
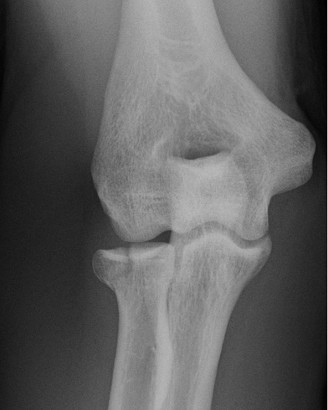
Initial radiographs obtained at the time of presentation demonstrated a healed distal humerus fracture with retained hardware (dual-plate construct). There was no evidence of hardware loosening or breakage. However, significant mature heterotopic ossification (HO) was clearly visible, particularly along the posterior-medial aspect of the elbow, bridging the olecranon fossa to the olecranon, and also within the anterior capsule. The joint space appeared maintained, and there were no obvious signs of degenerative changes or loose bodies identifiable on plain films.
Pre-operative anteroposterior radiograph demonstrating extensive heterotopic ossification.
CT Scan Indications & Findings
Given the significant bony end-feel and radiographic evidence of HO, a computed tomography (CT) scan with 3D reconstructions was crucial for detailed assessment and surgical planning.
*
Findings:
The CT scan confirmed extensive, mature heterotopic ossification bridging the olecranon fossa posteriorly and extending into the anterior joint capsule, forming bony blocks to both extension and flexion. Specific HO formations included a large posterior ossific mass obliterating the olecranon fossa and a smaller, but significant, anterior ossific spur arising from the coronoid fossa. The articular surface of the distal humerus appeared well-maintained without significant arthrosis, and the previous fracture reduction was anatomically satisfactory without malunion contributing directly to the bony block, apart from the HO. The hardware remained well-seated, though some screws were noted to be slightly prominent within the HO mass. The ulnar nerve path was encased in scar tissue and HO.
*
Templating:
3D reconstructions allowed for precise localization and volume assessment of the HO. This facilitated pre-operative templating, identifying specific osteotomy sites for HO excision, estimating the expected post-excision joint morphology, and planning the approach to protect critical neurovascular structures, particularly the ulnar nerve.
MRI Indications & Findings
Magnetic Resonance Imaging (MRI) was not indicated as the primary diagnostic tool in this case, as the predominant cause of stiffness was clearly bony (HO and previous hardware). MRI would be considered if there was suspicion of significant soft tissue pathology not evident on CT, such as severe ligamentous injury, intra-articular cartilage damage, or subtle loose bodies, especially in the absence of obvious bony blocks. In cases where the primary stiffness is thought to be capsular, MRI can delineate capsular thickening and fibrosis, but for post-traumatic contractures with evident HO, CT remains superior for bony detail.
Differential Diagnosis
A thorough differential diagnosis is crucial when evaluating post-traumatic elbow stiffness to guide appropriate management. For this patient, the primary differential considerations included heterotopic ossification, severe capsular contracture, and malunion.
| Feature / Condition | Post-Traumatic Heterotopic Ossification (HO) | Post-Traumatic Capsular Contracture | Malunion / Nonunion with Articular Incongruity |
|---|---|---|---|
| Pathoanatomy | Ectopic bone formation within soft tissues (muscle, fascia, capsule) surrounding the elbow joint. | Fibrosis, thickening, and shortening of the anterior and/or posterior joint capsule. | Deformity of bone due to healed fracture in suboptimal position, or failure of fracture to heal (nonunion). |
| Mechanism / Etiology | High-energy trauma, severe soft tissue injury, head injury, burns, prolonged immobilization, genetic predisposition. | Prolonged immobilization, inflammation, inadequate early rehabilitation, complex regional pain syndrome. | Incomplete initial reduction, fixation failure, premature weight-bearing, poor bone biology. |
| Clinical Examination | Palpable firm, bony mass. Restricted ROM with a distinct hard, bony end-feel. Pain often disproportionate to motion. | Restricted ROM, firm but often slightly compliant, leathery end-feel. No palpable bony mass. | Restricted ROM, bony end-feel, palpable deformity, crepitus, visible angulation/rotation. |
| Radiographic Findings | Mature lamellar bone formation on plain X-rays; well-defined, dense masses on CT bridging joint segments. | Normal plain X-rays; subtle capsular thickening on MRI, often a diagnosis of exclusion on imaging. | Callus deformity, step-off, gap at nonunion site, articular surface incongruity, implant impingement on X-ray/CT. |
| Impact on ROM | Mechanical block to motion (flexion and/or extension) due to ectopic bone impinging. | Restricted motion in a capsular pattern (often flexion > extension) due to shortened capsule. | Direct mechanical block to motion due to malaligned bone fragments or joint surface disruption. |
| Treatment Considerations | Surgical excision (after maturation), HO prophylaxis (NSAIDs, XRT), early aggressive motion. | Aggressive physical therapy, dynamic splinting, surgical capsular release (arthroscopic or open). | Corrective osteotomy, revision ORIF, arthroplasty (if severe articular destruction). |
In our patient's case, the strong evidence from clinical examination (palpable bony mass, hard end-feel) and imaging (extensive, mature HO on X-ray and CT) clearly pointed towards post-traumatic heterotopic ossification as the primary pathological entity causing the severe mechanical block to elbow motion. While an element of capsular contracture likely coexisted due to prolonged stiffness, the dominant issue was the HO. Malunion was largely ruled out by the excellent reduction achieved in the initial ORIF, as confirmed on CT.
Surgical Decision Making & Classification
Rationale for Operative vs. Non-operative Management
The decision to proceed with operative intervention for post-traumatic elbow stiffness is made after careful consideration of several factors:
1.
Failure of Non-operative Management:
Our patient had undergone five months of intensive physical therapy with no improvement, and indeed, progressive deterioration in ROM. This demonstrated the ineffectiveness of conservative measures in overcoming the mechanical block caused by the HO.
2.
Functional Deficit:
An arc of motion of 35 degrees (70-105 degrees) is severely dysfunctional, preventing most activities of daily living. A functional arc of motion for the elbow is generally considered to be 30-130 degrees of flexion-extension. Our patient's arc fell significantly short of this.
3.
Nature of the Stiffness:
The hard, bony end-feel and clear imaging evidence of mature heterotopic ossification indicated a mechanical bony block that could only be addressed surgically. Capsular contractures or soft tissue adhesions might respond to therapy; bony blocks rarely do.
4.
Maturation of HO:
Crucially, the HO must be mature before surgical excision to minimize the risk of recurrence. Maturity is typically assessed clinically (pain reduction, stable ROM) and radiographically (cortication of the HO mass, a distinct lucent rim on plain films or CT). Our patient was 8 months post-injury, and the CT scan confirmed mature, well-corticated HO. Operating on immature HO carries a significantly higher risk of recurrence.
5.
Patient Factors:
The patient's young age, active lifestyle, and occupational demands made surgical intervention highly desirable to restore function and improve quality of life. The mild ulnar neuropathy also added to the indication for surgical exploration.
Relevant Classifications
Several classifications aid in understanding and communicating elbow stiffness:
-
Hastings and Graham Classification of Elbow Stiffness: This classification distinguishes between the primary pathology:
- Extrinsic Contracture: Due to pathology outside the joint (e.g., skin, muscle, capsule, ligaments, heterotopic ossification).
- Intrinsic Contracture: Due to pathology within the joint (e.g., articular incongruity, loose bodies, arthrosis).
-
Mixed Contracture:
A combination of intrinsic and extrinsic factors.
Our patient presented with a mixed contracture , primarily extrinsic due to extensive heterotopic ossification and capsular fibrosis, but also potentially intrinsic given the severity and chronicity, even if direct articular damage wasn't the primary mechanical block.
-
Broberg and Morrey Classification for Heterotopic Ossification: This radiographic classification grades the severity of HO:
- Grade I: Islands of bone within the soft tissues.
- Grade II: Bone spurs from one bone, with at least 1 cm space between opposing bone surfaces.
- Grade III: Bone spurs from one or both bones, reducing the space between opposing bone surfaces to less than 1 cm.
-
Grade IV:
Apparent ankylosis of the joint.
Based on our patient's imaging, he presented with Grade III HO , with significant reduction in the joint space due to ossification, encroaching on the functional arc of motion. This severity strongly supported surgical intervention.
-
Mayo Elbow Performance Score (MEPS): While not a classification of stiffness, the MEPS is a widely used outcome measure that quantifies pain, ROM, stability, and function. Pre-operatively, our patient's MEPS score was likely very poor, and this would serve as a baseline to measure post-operative improvement.
Considering the severe functional deficit, mature HO causing a mechanical bony block, and failure of conservative management, the decision was made to proceed with open elbow arthrolysis and extensive heterotopic ossification excision.
Surgical Technique / Intervention
Pre-operative Planning
Extensive pre-operative planning was undertaken based on the CT 3D reconstructions. This involved mapping the exact location and extent of the HO, identifying its relationship to the ulnar nerve and collateral ligaments, and templating the sequential steps of excision to ensure maximal bone removal while preserving stability.
Patient Positioning and Preparation
The patient was positioned in the lateral decubitus position with the affected arm draped free over a padded arm rest. This position offers excellent access to both the medial and lateral aspects of the elbow, allowing for comprehensive release. A high-arm tourniquet was applied and inflated after exsanguination. Careful padding of all pressure points, especially the contralateral arm and leg, was ensured.
Surgical Approach
A
posterior approach with triceps-sparing modification
was utilized. The previous posterior incision was re-incised. A full-thickness skin and subcutaneous tissue flap was elevated.
1.
Ulnar Nerve Exploration:
The ulnar nerve was meticulously identified proximally, deep to the Osborne's ligament, and carefully dissected free from the surrounding scar tissue and HO. It was found to be significantly compressed and encased. Given the pre-existing ulnar neuropathy and the extensive HO, a decision was made to perform a
subcutaneous anterior transposition
of the ulnar nerve after its complete neurolysis.
-
Posterior Compartment Release and HO Excision:
- A longitudinal incision was made through the triceps fascia, splitting the triceps tendon carefully along its fibers to access the posterior capsule and olecranon fossa.
- Extensive heterotopic ossification was encountered, completely obliterating the olecranon fossa and bridging from the distal humerus to the olecranon. This bony mass was carefully excised using osteotomes, rongeurs, and a high-speed burr, taking care to preserve the underlying articular cartilage.
- The posterior capsule was then completely released from the distal humerus and proximal ulna, allowing for greater elbow flexion.
- The olecranon fossa was debrided of all remaining HO and hypertrophic synovium.
-
Anterior Compartment Release and HO Excision:
- To address the anterior contracture and HO, the common flexor and extensor origins were released from the medial and lateral epicondyles respectively, in a pie-crusting fashion to expose the anterior joint capsule.
- The anterior capsule was then released extensively from the coronoid fossa and the surrounding bony structures. A significant anterior HO spur arising from the coronoid fossa was identified and carefully excised.
- Any prominent hardware from the previous distal humerus fixation that was causing impingement or was embedded in HO was carefully removed, if it did not compromise the stability of the remaining fixation construct. In this case, two screws were identified as being prominent and were removed.
- Loose bodies or osteophytes within the joint were identified and removed.
-
Assessment of ROM and Stability:
- After meticulous release and HO excision, the elbow was taken through a full range of motion. We achieved a full extension to 0 degrees and flexion to approximately 140 degrees intraoperatively.
- Dynamic stability was assessed throughout the arc of motion, particularly in extension and valgus/varus stress. The medial and lateral collateral ligaments were found to be intact and competent, ensuring joint stability. This is a critical step, as achieving motion must not come at the cost of instability.
-
Closure:
- The wound was copiously irrigated.
- A negative pressure wound therapy (NPWT) dressing was initially applied to manage the dead space and potential for hematoma, given the extensive dissection. Alternatively, a large suction drain can be placed and removed within 24-48 hours.
- The triceps was repaired, and the ulnar nerve was positioned subcutaneously in its transposed bed.
- Subcutaneous and skin layers were closed meticulously.
- The elbow was placed in a dynamic extension splint for immediate post-operative positioning.
Intra-operative photograph illustrating the extensive heterotopic ossification being excised from the posterior compartment.

Post-operative radiograph after HO excision, demonstrating improved joint space and removal of bony blocks.

Post-Operative Protocol & Rehabilitation
The success of elbow arthrolysis relies heavily on an immediate, aggressive, and well-structured post-operative rehabilitation protocol coupled with effective heterotopic ossification prophylaxis.
Immediate Post-Operative Period (Day 0-7)
- Wound Care: The NPWT dressing was changed or removed after 3-5 days. If a drain was used, it was removed when output was minimal.
- Pain Management: Multimodal analgesia including oral opioids, NSAIDs (if not contraindicated), acetaminophen, and gabapentinoids was employed to ensure effective pain control, facilitating early motion. A regional nerve block (e.g., supraclavicular or axillary block) can be highly beneficial for the initial 24-48 hours.
-
Heterotopic Ossification (HO) Prophylaxis:
- NSAIDs: Indomethacin 25 mg orally three times daily was initiated within 12 hours post-surgery and continued for 3-6 weeks, pending gastrointestinal tolerance and renal function. This is contraindicated in patients with renal impairment, history of GI bleeding, or allergy.
- Radiation Therapy (XRT): For high-risk patients (e.g., TBI, burn patients, previous history of HO, or very extensive initial HO as in this case), a single dose of 700-800 cGy radiation therapy was considered for administration within 24-72 hours post-operatively. In this case, given the extent of HO and the prior history, a single dose of 800cGy was given on post-op day 1 to the operative field.
-
Early Mobilization:
- Continuous Passive Motion (CPM) machine: Initiated within 24-48 hours post-op, set to the maximum tolerable range of motion achieved intra-operatively (0-140 degrees), for at least 6-8 hours daily. The patient was instructed on its use and encouraged to utilize it as much as possible, including during sleep.
- Physical Therapy (PT): Formal PT began on post-operative day 1, focusing on gentle active-assisted and passive range of motion exercises. The initial goals were to maintain the surgical gains and prevent new adhesions. Sling use was minimized to only for comfort and protection, not for immobilization.
Subacute Phase (Weeks 2-6)
- Intensified PT: Therapy progressed to include active range of motion, gentle stretching, scar massage, and desensitization of the ulnar nerve transposition site.
- Strengthening: Light isometric exercises were introduced, gradually progressing to isotonic exercises as tolerated, avoiding heavy resistance in early stages to protect soft tissue healing.
- Dynamic Splinting: For patients struggling to maintain ROM gains, particularly at end-range, a dynamic or static progressive splint (e.g., Dynasplint or JAS splint) was prescribed for use during periods of rest or overnight, to provide a low-load, prolonged stretch. This was used for our patient, primarily for extension deficit, but also intermittently for flexion.
- Patient Education: Emphasized the importance of consistent home exercise programs and understanding the protracted nature of rehabilitation.
Chronic Phase (Weeks 6-12 and beyond)
- Functional Progression: PT focused on progressive strengthening, endurance, and return to functional activities, including work-specific tasks.
- Monitoring for Recurrence: Clinical monitoring for recurrent pain, stiffness, or palpable masses suggestive of HO. Radiographs were obtained at 6 weeks, 3 months, 6 months, and 1 year post-op to assess for recurrent HO.
- Return to Activity: Gradual return to light duty work around 3 months, with full return to heavy manual labor anticipated around 6 months, contingent on achieving satisfactory strength and ROM.
Expected Outcomes
With aggressive rehabilitation and HO prophylaxis, an improvement in the functional arc of motion (e.g., 30-130 degrees) is generally achievable. Our patient demonstrated significant improvement, achieving a 15-degree extension deficit and 130 degrees of flexion at 6 months post-op, representing a functional arc of 115 degrees. His ulnar nerve symptoms also resolved.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls for Success in Managing Post-Traumatic Elbow Contractures:
- Timing is Everything for HO Excision: Ensure HO is mature (usually 6-12 months post-injury) before excision. Operating on immature HO dramatically increases the risk of recurrence. Radiographically, look for distinct cortical margins and a lucent rim around the ossification on plain films or CT. Clinically, pain should be diminished, and ROM should have plateaued.
- Pre-operative Imaging is Paramount: A high-quality CT scan with 3D reconstructions is indispensable. It allows for precise mapping of HO, identification of its relationship to neurovascular structures, detection of subtle articular incongruity, and pre-operative templating.
- Ulnar Nerve Management: Always identify and protect the ulnar nerve. Prophylactic neurolysis and anterior transposition are often warranted, especially in cases of extensive posterior-medial HO, previous trauma/surgery, or pre-existing neuropathy. Better to transpose than to risk injury or entrapment.
- Comprehensive Release: Do not be timid. A full capsular release, both anterior and posterior, must be performed along with meticulous HO excision. This often requires releasing the common flexor and extensor origins. Ensure the coronoid and olecranon fossae are completely clear.
- Intra-operative ROM Check: Achieve full or near-full physiological ROM (e.g., 0-140 degrees) and confirm stability under fluoroscopy or direct visualization after release. This dictates the maximum potential for post-operative gains.
- Aggressive Post-operative Rehabilitation: This is the most critical factor for maintaining surgical gains. Initiate CPM within 24-48 hours. Continuous passive motion (CPM) devices are strongly recommended for 6-8 hours daily for several weeks. Early, active-assisted ROM, splinting, and dedicated physical therapy are non-negotiable.
- HO Prophylaxis: For high-risk patients (extensive HO, head injury, burns, prior HO), use NSAIDs (Indomethacin) for 3-6 weeks and/or post-operative radiation therapy (single dose within 24-72 hours) to minimize recurrence.
- Stability is Key: While achieving motion is the goal, never compromise elbow stability. Assess medial and lateral collateral ligament integrity intraoperatively. Repair if necessary.
Pitfalls to Avoid:
- Operating Too Early: Excising immature HO often leads to rapid and exuberant recurrence, potentially worse than the original condition.
- Incomplete Release: Residual bony impingement or capsular tightness will limit the ultimate ROM gain, leading to patient dissatisfaction and potential for revision.
- Inadequate HO Prophylaxis: Failure to implement appropriate HO prophylaxis in high-risk patients significantly increases recurrence rates.
- Poor Patient Compliance: Without dedicated patient adherence to the intensive post-operative rehabilitation protocol, surgical gains will be lost. This needs thorough pre-operative counseling.
- Iatrogenic Neurovascular Injury: The ulnar nerve is highly susceptible to injury during elbow arthrolysis due to scarring and distortion of anatomy by HO. Meticulous dissection and early identification are paramount.
- Post-operative Instability: Over-releasing ligaments, especially in an already compromised joint, can lead to iatrogenic instability, requiring further intervention. Always check dynamic stability.
- Infection: As with any complex surgical procedure, infection remains a risk, especially with extensive soft tissue dissection and long surgical times.
- Heterotopic Ossification Recurrence: Even with prophylaxis, recurrence can occur, necessitating close follow-up and management.
Clinical & Radiographic Imaging
You Might Also Like