Comprehensive Diagnosis of Developmental Dysplasia of the Hip (DDH) in a Young Adult
Key Takeaway
Diagnosing Developmental Dysplasia of the Hip (DDH) in young adults involves a comprehensive approach. This includes patient history of chronic hip pain, clinical examination (ROM, provocative tests), and advanced imaging. Key diagnostics: X-rays showing acetabular undercoverage, MRI for soft tissues, and 3D CT scans for precise anatomical confirmation.
Patient Presentation & History
A 28-year-old female presented to our clinic with a chief complaint of chronic, progressive right hip pain of approximately three years duration. The pain was initially insidious, localized to the groin and lateral hip, and described as a deep ache, occasionally sharp, particularly with activity. Over the last 12 months, the pain had significantly worsened, limiting her ability to perform daily activities, including prolonged walking, stair climbing, and recreational sports. She reported mechanical symptoms, including occasional catching and stiffness, primarily after periods of rest. She denied any acute traumatic event or specific mechanism of injury.
Her past medical history was notable for being diagnosed with developmental dysplasia of the hip (DDH) as an infant, managed non-operatively with a Pavlik harness for six months. She had been largely asymptomatic throughout childhood and adolescence, participating in competitive soccer until college. She denied any prior hip surgeries or significant hip injuries. She reported no systemic inflammatory conditions, neurological deficits, or significant comorbidities. Her BMI was 23 kg/m². Social history included being a non-smoker and consuming alcohol occasionally. She worked as an accountant, requiring prolonged sitting, which also exacerbated her symptoms. Initial non-operative management, including activity modification, NSAIDs, and a course of physical therapy focusing on core strengthening and hip muscle balance, provided only transient relief. An intra-articular hip injection performed by her referring physician offered approximately two months of relief before symptoms recurred with similar intensity.
Clinical Examination
On general inspection, the patient walked with a subtle right-sided antalgic gait. A mild Trendelenburg sign was noted on the right. She displayed no obvious leg length discrepancy (LLD) in standing, though a thorough supine measurement was later performed. There was no visible swelling, erythema, or skin changes around the hip. Muscle bulk appeared symmetrical bilaterally.
Palpation revealed tenderness over the anterior hip capsule and mild tenderness in the region of the greater trochanter. No palpable masses or crepitus were identified.
Range of motion (ROM) of the right hip was assessed bilaterally and compared.
*
Flexion
: Right 95° (left 110°)
*
Extension
: Right 10° (left 15°)
*
Abduction
: Right 25° (left 40°)
*
Adduction
: Right 15° (left 25°)
*
Internal Rotation
: Right 5° (left 30°) – significantly restricted, with associated pain at end-range.
*
External Rotation
: Right 35° (left 45°)
Specific provocative tests were performed:
*
Flexion-Adduction-Internal Rotation (FADIR) test
: Strongly positive on the right, reproducing her groin pain.
*
Flexion-Abduction-External Rotation (FABER) test
: Positive on the right, with limited external rotation and pain in the anterior hip/groin.
*
Posterior Impingement Test (Flexion-External Rotation-Adduction)
: Negative.
*
Log Roll Test
: Positive for pain on internal rotation.
*
Trendelenburg Test
: Positive, indicating gluteus medius insufficiency or compensation.
Neurological examination of the lower extremities revealed intact motor strength (5/5 in all major muscle groups), sensation to light touch and pinprick, and symmetrical deep tendon reflexes (patellar and Achilles +2 bilaterally). Peripheral pulses (femoral, popliteal, dorsalis pedis, posterior tibial) were all palpable and symmetrical. No signs of vascular compromise were present. Lumbar spine examination was unremarkable, ruling out a significant radicular component to her pain.
Imaging & Diagnostics
Initial diagnostic workup commenced with standard radiographic series of the pelvis and hip.
Plain Radiographs (Weight-bearing AP Pelvis, Frog-Leg Lateral, False Profile View of the Right Hip):
*
AP Pelvis
: Demonstrated features consistent with residual hip dysplasia.
*
Lateral Center-Edge Angle (LCEA)
: Measured at 12° on the right (normal >25°), indicating acetabular undercoverage.
*
Tönnis Angle (Acetabular Index)
: Measured at 20° on the right (normal <10°), indicating acetabular steepness and superior inclination.
*
Femoral Head Extrusion Index
: Approximately 35% on the right (normal <25%), further confirming inadequate coverage.
*
Shenton's Line
: Disrupted on the right, suggesting mild superolateral subluxation of the femoral head.
*
Cross-over sign
: Absent.
*
Ischial Spine Sign
: Negative.
* Mild sclerosis and subchondral cyst formation were noted superiorly within the acetabulum, indicative of early osteoarthritic changes.
* Joint space narrowing was minimal but identifiable superiorly.
*
Frog-Leg Lateral
: Showed a spherical femoral head but subtle anterior acetabular deficiency. No definitive cam lesion was evident, though an alpha angle measurement was difficult due to the global dysplasia.
*
False Profile View
: Confirmed anterior acetabular undercoverage, with an anterior center-edge angle (ACEA) of 15° (normal >20°).
Magnetic Resonance Imaging (MRI) of the Right Hip (with intra-articular contrast):
* Performed to assess the labrum, articular cartilage, and surrounding soft tissues.
* Revealed a detachment and degeneration of the anterior and superior acetabular labrum.
* Focal areas of Grade II-III chondral delamination and fissuring were noted on the anterior-superior aspect of the acetabulum and corresponding anterosuperior femoral head.
* No evidence of avascular necrosis, significant osteonecrosis, or other intra-articular pathology beyond the dysplastic changes and secondary degenerative changes was observed.
* Capsular laxity was suggested by mild contrast extravasation.
Computed Tomography (CT) Scan of the Pelvis with 3D Reconstruction:
* A CT scan was ordered for precise 3D evaluation of the acetabular and femoral anatomy, crucial for surgical planning.
* Confirmed the severe acetabular dysplasia, with marked anterior and lateral undercoverage.
* Provided detailed measurements of anteversion and inclination, confirming inadequate global acetabular coverage.
* Detailed evaluation of the posterior column confirmed its integrity and suitability for osteotomy.
* This study was critical for pre-operative templating of the periacetabular osteotomy (PAO), allowing for virtual simulation of the osteotomy cuts and the degree of fragment rotation required to achieve optimal coverage, joint congruence, and restoration of physiological biomechanics. It aided in determining the appropriate screw lengths and positions for fixation.
Pre-operative Imaging for Planning:
The combination of plain radiographs, MRI, and CT provided a comprehensive understanding of the patient's hip pathology. The radiographs established the overall bony deformity, the MRI characterized the soft tissue and chondral damage, and the CT scan provided the necessary 3D blueprint for the complex osteotomies involved in a PAO.

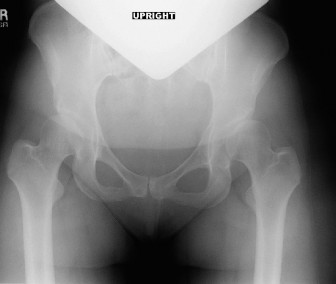
Figure 1: Representative pre-operative AP pelvis radiograph demonstrating features of residual hip dysplasia, including reduced lateral center-edge angle and increased acetabular index, indicative of inadequate acetabular coverage and superolateral subluxation.
Differential Diagnosis
Given the patient's chronic hip pain, young age, and radiographic findings, several conditions were considered in the differential diagnosis. A structured approach helped refine the primary diagnosis.
| Feature | Developmental Dysplasia of the Hip (DDH) with Secondary FAI and Chondrolabral Degeneration (Primary Diagnosis) | Primary Femoroacetabular Impingement (FAI) - Cam/Pincer | Avascular Necrosis (AVN) of the Femoral Head | Early Primary Osteoarthritis of the Hip |
|---|---|---|---|---|
| Pathophysiology | Congenital malformation of the acetabulum leading to insufficient coverage, joint instability, abnormal contact pressures, and compensatory labral hypertrophy/damage. Can lead to secondary FAI (dysplastic FAI). | Abnormality in femoral head-neck junction (cam) or acetabular rim (pincer) causing impingement between femur and acetabulum during motion, leading to labral and chondral damage. | Interruption of blood supply to the femoral head, leading to subchondral bone death, collapse, and secondary OA. | Progressive wear and tear of articular cartilage due to biological/mechanical factors, often idiopathic or post-traumatic. |
| Patient History | Childhood history of DDH (Pavlik harness). Chronic, progressive groin/lateral pain. Mechanical symptoms (catching). Pain with prolonged activity/sitting. | Chronic, progressive groin/lateral pain. Pain with squatting, deep flexion. Mechanical symptoms (clicking, locking). Often athletic individuals. | Acute or insidious onset of pain. May have risk factors (steroid use, alcohol, sickle cell, trauma). Pain initially subtle, progressing to severe. | Insidious onset, progressive pain. Stiffness, especially morning stiffness. May have history of trauma or predisposing conditions. |
| Clinical Examination | Antalgic gait, Trendelenburg sign. Restricted abduction and internal rotation (often painful). Positive FADIR/FABER. Leg length discrepancy possible. | Restricted internal rotation (especially in flexion). Positive FADIR. May have hyper-abduction or external rotation with pincer. | Pain with weight-bearing. Restricted ROM, especially internal rotation and abduction, which may be more globally restricted than FAI. | Reduced ROM in multiple planes (flexion, abduction, IR). Pain at end-range. Antalgic gait. |
| Radiographic Findings (Plain X-ray) | LCEA <20-25° , Tönnis angle >10° , femoral head extrusion >25%, Shenton's line disruption. Early joint space narrowing/sclerosis superiorly. | Cam: Pistolgrip deformity, alpha angle >55°. Pincer: Cross-over sign, profunda/protrusio acetabuli, ischial spine sign. Normal acetabular coverage. | Crescent sign (subchondral collapse), patchy sclerosis/lucency, flattening of femoral head. Often normal in early stages. | Joint space narrowing (superior > medial), osteophyte formation, subchondral sclerosis, subchondral cysts. |
| MRI Findings | Labral detachment/degeneration, chondral delamination superiorly/anteriorly. Possible signs of capsular laxity. Acetabular undercoverage. | Labral tears (often anterior-superior), chondral lesions at rim. Cam/pincer morphology visible. | Low signal intensity on T1, variable signal on T2 (double-line sign characteristic). Early stages may be normal. | Cartilage thinning/loss, osteophytes, synovial inflammation. |
| CT Scan Findings | 3D confirmation of acetabular undercoverage (anterior, lateral). Precise measurements of version/inclination. Early OA changes. | Precise 3D morphology of cam/pincer lesions. Evaluation of acetabular retroversion (pincer). | Confirms bone architecture, extent of necrosis and collapse. | Detailed bony changes, osteophytes. |
| Response to Intra-articular Injection | Often temporary relief, confirming intra-articular source of pain. | Often temporary relief, confirming intra-articular source of pain. | Variable, may relieve some pain if secondary synovitis, but not addressing primary pathology. | Temporary relief, confirming intra-articular source of pain. |
| Management | Periacetabular Osteotomy (PAO) for joint preservation if significant dysplasia and mild/moderate OA. Total Hip Arthroplasty (THA) for advanced OA. | Arthroscopy (rim trimming, labral repair) for mild/moderate FAI. Open surgery for complex FAI. | Core decompression, vascularized fibular graft, THA in advanced cases. | THA for symptomatic, advanced disease. Non-operative management for mild. |
This patient's constellation of findings, including the childhood history of DDH, classic radiographic parameters of acetabular dysplasia, symptomatic impingement, and chondrolabral damage on MRI, led to a primary diagnosis of symptomatic residual developmental dysplasia of the hip with secondary femoroacetabular impingement and early degenerative changes . AVN was ruled out by MRI findings, and primary FAI was less likely given the significant acetabular undercoverage. Early primary OA was present but secondary to the dysplasia, and the patient's age and desire for joint preservation favored reconstruction over arthroplasty.
Surgical Decision Making & Classification
The decision for surgical intervention, specifically a periacetabular osteotomy (PAO), was made based on several key factors:
- Persistent Symptoms: Despite a comprehensive course of conservative management, the patient continued to experience disabling hip pain and functional limitations impacting her quality of life and work.
- Age and Activity Level: At 28 years old, the patient is young, active, and has a high expectation for long-term joint function. Joint preservation was paramount to defer or potentially avoid total hip arthroplasty (THA).
- Radiographic Evidence of Dysplasia: The LCEA of 12°, Tönnis angle of 20°, and femoral head extrusion index of 35% unequivocally confirmed significant acetabular dysplasia.
- MRI Findings of Chondrolabral Damage: The presence of labral detachment and Grade II-III chondral lesions, while early, indicated ongoing joint damage secondary to the abnormal biomechanics, underscoring the urgency for intervention to prevent further progression to end-stage osteoarthritis.
- Absence of Advanced Osteoarthritis: While early degenerative changes were noted, the joint space narrowing was minimal, and the cartilage damage was not extensive enough to preclude joint preservation surgery. Advanced osteoarthritis (Tönnis Grade 2 or 3) would typically contraindicate PAO. Our patient was Tönnis Grade 1.
- Desire for Joint Preservation: The patient was well-informed about the surgical options and expressed a strong preference for a joint-preserving procedure.
Classification Systems Guiding Decision-Making:
-
Developmental Dysplasia of the Hip (DDH):
- Tönnis Classification of Osteoarthritis: This system helps grade the severity of osteoarthritis, which is crucial for determining suitability for PAO. Our patient was Tönnis Grade 1 (mild subchondral sclerosis and slight joint space narrowing, no significant osteophytes or cysts), making her an excellent candidate for joint preservation. Tönnis Grade 2 and 3 would indicate more advanced disease, pushing towards arthroplasty.
- Crowe Classification: While primarily for subluxation/dislocation severity, it highlights the structural deficiency. Our patient demonstrated significant subluxation on radiography, reinforcing the need for correction of coverage.
- Lateral Center-Edge Angle (LCEA) of Wiberg: An LCEA <20° indicates definite dysplasia, while 20-25° is borderline. Our patient's LCEA of 12° firmly placed her in the dysplastic category requiring surgical correction.
-
Femoroacetabular Impingement (FAI):
- Although the primary pathology was dysplasia, the presence of impingement symptoms and labral damage indicated secondary FAI, often termed "dysplastic FAI." This occurs when the malformed acetabulum causes abnormal contact with a relatively normal or mildly dysmorphic femoral head.
- The management of the secondary FAI (labral tear, chondral damage) would be addressed concurrently during the PAO.
Contraindications to PAO:
It is important to review contraindications, none of which applied to our patient:
* Advanced osteoarthritis (Tönnis Grade 2 or 3)
* Significant active infection
* Severe osteoporosis
* Neuromuscular disorders affecting gait
* Morbid obesity
* Lack of patient compliance
* Non-physiological range of motion (e.g., severe contractures)
* Acetabular retroversion as the primary cause of impingement (though some cases can be corrected with PAO, pure retroversion might be better addressed with osteoplasty alone).
Given the patient's age, symptoms, radiographic findings, and the aim of improving biomechanics, reducing pain, and delaying/preventing future arthroplasty, a Bernese periacetabular osteotomy (PAO) was deemed the most appropriate reconstructive procedure.
Surgical Technique / Intervention
The patient underwent a right Bernese Periacetabular Osteotomy (PAO).
1. Patient Positioning and Preparation:
* The patient was placed in a supine position on a radiolucent operating table.
* A lateral bump was placed under the right buttock to slightly elevate the operative side and facilitate access.
* The entire lower extremity was prepared and draped free to allow for full range of motion intraoperatively, crucial for assessing correction and impingement.
* Fluoroscopy was used throughout the procedure to confirm osteotomy cuts and fragment positioning.
2. Surgical Approach (Modified Smith-Petersen):
* A "bikini" incision was made, extending from the anterior superior iliac spine (ASIS) curvilinearly towards the greater trochanter. This cosmetically favorable incision allows for excellent access to the lateral aspect of the ilium, anterior capsule, and the osteotomy sites.
* Dissection was carried down through subcutaneous tissue. The tensor fascia lata (TFL) was incised in line with its fibers, approximately 2-3 cm posterior to the ASIS.
* The interval between the sartorius and rectus femoris anteriorly, and the TFL and gluteus medius posteriorly, was identified and developed.
* The direct head of the rectus femoris was identified and released from the ASIS and anterior inferior iliac spine (AIIS). The indirect head was also released.
* The iliopsoas muscle was identified medially and protected. A Penrose drain was placed around the femoral neurovascular bundle for retraction and protection. The lateral femoral cutaneous nerve was identified and protected, typically running superficial to the sartorius.
3. Exposure of Osteotomy Sites:
* The superior pubic ramus was exposed. The pectineus muscle was elevated from the superior pubic ramus.
* The inner and outer tables of the ilium were exposed. The gluteus medius and minimus were elevated off the outer table of the ilium superiorly and posteriorly, exposing the sciatic notch and posterior column. Care was taken to preserve the blood supply to the mobilized bone fragment.
* The anterior acetabular rim and capsule were exposed. The labrum and chondral lesions were inspected at this stage; a partial labrectomy and chondroplasty were performed on the anterior-superior aspect to remove degenerate tissue and address focal impingement.
4. Performance of Osteotomies:
The Bernese PAO involves four sequential osteotomies, performed with oscillating saws, osteotomes, and drills:
-
Ischial Osteotomy:
- A Hohmann retractor was placed around the posterior column inferior to the acetabulum, protecting the sciatic nerve.
- A curved osteotome was used to perform a partial cut inferior to the acetabulum, just above the ischial tuberosity and through the superior border of the ischial ramus. This cut was advanced carefully, aiming towards the obturator foramen.
- Completion of the ischial osteotomy was achieved with an oscillating saw, under fluoroscopic guidance, ensuring it exited anteriorly, above the obturator externus muscle and below the acetabulum.
-
Pubic Osteotomy:
- The superior pubic ramus was exposed.
- A K-wire was inserted to guide the saw cut.
- An oscillating saw was used to perform the osteotomy through the superior pubic ramus, approximately 2-3 cm medial to the acetabulum, under fluoroscopic control. This completed the inferior and anterior disarticulation of the acetabular fragment.
-
Iliac Osteotomy (Supra-Acetabular):
- This is the most critical osteotomy. A vertical osteotomy was made superior to the acetabulum, extending from the outer table to the inner table of the ilium.
- The osteotomy began approximately 1.5 cm superior to the acetabular roof and was directed posteriorly towards the sciatic notch.
- It was crucial to leave an intact posterior bone hinge (the posterior column osteotomy) initially. This hinge provides stability and controls the fragment during mobilization. This cut was performed with an oscillating saw, avoiding violation of the joint.
-
Posterior Column Osteotomy (Partial/Completing Iliac):
- Once the first three osteotomies were complete, the remaining posterior iliac hinge was carefully completed.
- This involved drilling multiple small holes (drill-hole technique) along the desired line of the posterior column, from the sciatic notch superiorly towards the iliac crest cut, and then connecting them with a small osteotome or saw.
- This partial osteotomy (allowing for controlled greenstick fracture) freed the entire acetabular fragment while maintaining periosteal and muscular attachments medially for vascularity.
5. Mobilization and Repositioning of the Acetabular Fragment:
* Once all osteotomies were completed, the acetabular fragment was carefully mobilized using specific PAO clamps (e.g., Ganz clamps) and osteotomes.
* The fragment was rotated and translated to achieve optimal femoral head coverage:
*
Lateralization:
To increase the LCEA and decrease the Tönnis angle.
*
Anteriorization:
To increase the ACEA and correct anterior undercoverage.
*
External Rotation:
To increase femoral head coverage and reduce anterior impingement.
* Fluoroscopy was used repeatedly to assess the correction of the LCEA, Tönnis angle, and Shenton's line. Intraoperative range of motion was assessed by flexing, internally rotating, and adducting the hip to ensure no residual impingement. The goal was to achieve an LCEA of 25-35° and a Tönnis angle of 0-10°.
6. Fixation:
* Once optimal positioning was achieved, the acetabular fragment was provisionally fixed with multiple K-wires.
* Definitive fixation was then performed using 3-4 cortical screws (typically 4.5 mm or 3.5 mm self-tapping cortical screws) placed across the iliac osteotomy from the repositioned acetabular fragment into the stable ilium. The choice of screw length and trajectory was guided by pre-operative templating and intra-operative fluoroscopy to ensure bicortical purchase and avoid intra-articular violation or neurovascular structures.
* The defect created in the ilium was often filled with autologous bone graft (harvested from the iliac wing during the approach) or synthetic graft material to promote healing and provide structural support.
7. Wound Closure:
* The hip joint capsule was repaired, and the rectus femoris origin was reattached.
* The fascia lata was repaired, and subcutaneous tissues were closed in layers.
* A drain was often placed to manage hematoma. Skin was closed with absorbable sutures.
Post-Operative Protocol & Rehabilitation
The post-operative protocol following a Bernese Periacetabular Osteotomy is crucial for optimal healing and functional recovery.
Immediate Post-Operative (Day 0-3):
*
Pain Management:
Multimodal analgesia including epidural/nerve blocks, oral opioids, and NSAIDs (if not contraindicated).
*
Weight-Bearing:
Strictly non-weight-bearing (NWB) or touch-down weight-bearing (TDWB) of 10-15 kg on the operative leg for the first 6-8 weeks, using crutches or a walker. This protects the osteotomies from excessive stress during initial healing.
*
DVT Prophylaxis:
Chemical (e.g., LMWH) and mechanical (e.g., pneumatic compression devices) DVT prophylaxis.
*
CPM Machine:
Continuous passive motion (CPM) machine may be initiated for gentle ROM, typically 0-90° flexion, for 4-6 hours daily to prevent adhesions and promote cartilage health.
*
Physical Therapy (PT):
*
Bed mobility and transfers:
Training for safe transitions.
*
Deep breathing and ankle pump exercises:
To prevent pulmonary complications and DVT.
*
Gentle isometric gluteal and quadriceps sets.
*
Assisted ROM:
Passive range of motion within pain-free limits (typically 0-90° flexion, limited abduction/adduction/rotation initially).
*
Precautions:
Avoid extreme flexion (>90°), internal rotation, and adduction for the first 6 weeks to protect the hip capsule and osteotomy.
Early Rehabilitation (Weeks 1-6):
*
Weight-Bearing:
Continued NWB/TDWB. Strict adherence is critical.
*
PT Focus:
*
ROM:
Gradual increase in active-assisted and active ROM within safe limits.
*
Strength:
Progress isometric exercises. Begin gentle, pain-free active hip flexion and extension.
*
Gait Training:
Focus on proper gait mechanics with crutches, emphasizing NWB/TDWB.
*
Core Stability:
Begin gentle core strengthening exercises (e.g., pelvic tilts).
*
Scar Management:
Gentle massage once the incision is healed.
*
Activities:
Avoid activities that place shear stress or torsion on the healing osteotomies.
Intermediate Rehabilitation (Weeks 6-12):
*
Radiographic Assessment:
X-rays at 6 weeks post-op to assess osteotomy healing.
*
Weight-Bearing Progression:
If osteotomies show adequate healing, gradual progression to partial weight-bearing (PWB) (25-50% body weight) with crutches, then full weight-bearing (FWB) over 2-4 weeks.
*
PT Focus:
*
Strength:
Advance strengthening exercises (e.g., light resistance bands, hip abductor/adductor strengthening, hamstring curls, leg presses). Focus on gluteal muscle strengthening.
*
ROM:
Continue to improve full ROM.
*
Balance:
Begin balance and proprioception exercises.
*
Gait Training:
Wean off crutches as tolerance and strength allow. Normalize gait pattern.
*
Activities:
Continue to avoid high-impact activities, deep squats, or pivoting motions.
Advanced Rehabilitation (Months 3-6):
*
Weight-Bearing:
Full weight-bearing, without assistive devices.
*
PT Focus:
*
Strength and Endurance:
Progressive resistance training, functional strength, and endurance building.
*
Agility and Sport-Specific Training:
Gradually introduce light jogging, swimming, cycling. Progress to sport-specific drills if applicable, focusing on controlled movements.
*
Plyometrics:
Very carefully introduce low-level plyometric exercises (e.g., step-ups, box jumps) towards the end of this phase, if indicated.
*
Activities:
Gradual return to activities of daily living and work.
*
Imaging:
X-rays at 3-6 months to confirm complete osteotomy union.
Long-Term Rehabilitation (Months 6-12+):
*
Return to Sport/Activity:
Gradual and progressive return to desired sports and high-impact activities. This is highly individualized and depends on healing, strength, and confidence. Full return to competitive sports may take 9-12 months or longer.
*
Maintenance:
Continue a home exercise program focusing on hip and core strength, flexibility, and mobility.
*
Follow-up:
Regular follow-up appointments with the surgeon to monitor progress and assess for any long-term complications or progression of osteoarthritis.
It is critical to emphasize patient education regarding activity modification, proper body mechanics, and adherence to the rehabilitation program to optimize outcomes and prolong the life of the reconstructed hip.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls:
- Patient Selection is Paramount: The ideal PAO candidate is typically young (<40-45 years), active, with symptomatic hip dysplasia, and minimal to mild osteoarthritis (Tönnis Grade 0 or 1). Advanced osteoarthritis (Tönnis Grade >1) is a strong contraindication.
- Pre-operative Planning (3D CT): A detailed 3D CT scan is indispensable for understanding the unique anatomy of each dysplastic hip. It allows for precise templating of osteotomy cuts, calculation of fragment rotation/translation, and identification of critical neurovascular structures. This improves efficiency and accuracy intraoperatively.
- Modified Smith-Petersen Approach: The bikini incision and interval between sartorius/rectus femoris and TFL/gluteus medius offer excellent exposure of all four osteotomy sites while minimizing muscle damage and improving cosmetic outcomes. Careful identification and protection of the lateral femoral cutaneous nerve (LFCN) is vital.
- Sequential, Controlled Osteotomies: Performing the ischial, pubic, and then iliac osteotomies, leaving the posterior column as a controlled hinge, facilitates safe mobilization. The posterior column is often "greensticked" or completed with drill holes to maintain some medial periosteal attachments for fragment vascularity.
- Intraoperative Fluoroscopy and Assessment: Regular use of fluoroscopy is critical to confirm accurate osteotomy placement, fragment mobilization, and post-correction radiographic parameters (LCEA, Tönnis angle, Shenton's line). Intraoperative range of motion assessment (flexion-adduction-internal rotation) is crucial to ensure impingement has been eliminated.
- Optimal Fragment Repositioning: The goal is to achieve an LCEA of 25-35° and a Tönnis angle of 0-10°. Overcorrection or undercorrection can lead to new problems (e.g., FAI with overcorrection, persistent instability with undercorrection). The repositioning should aim to restore concentricity and normalize joint mechanics.
- Addressing Concurrent Pathology: During the PAO, it is essential to address any associated labral tears, chondral lesions, or capsular laxity (e.g., labral repair/debridement, capsular plication) to maximize outcomes.
- Rehabilitation Adherence: Strict adherence to the post-operative NWB/TDWB protocol for the first 6-8 weeks is non-negotiable for osteotomy healing. A progressive, structured rehabilitation program is crucial for regaining strength, range of motion, and function.
Pitfalls:
-
Neurovascular Injury:
- Sciatic Nerve: Risk during posterior column osteotomy or deep retraction near the sciatic notch. Careful placement of Hohmann retractors and precise osteotome work are paramount.
- Femoral Nerve/Artery/Vein: Risk during anterior dissection, especially with medial retraction. Use of Penrose drains and blunt dissection to protect the neurovascular bundle.
- Lateral Femoral Cutaneous Nerve (LFCN): High risk of injury or neuropraxia due to its variable course and superficial location, leading to meralgia paraesthetica. Careful identification and protection, or intentional neurotomy if sacrificing for exposure, is important.
- Non-Union or Malunion of Osteotomies: Inadequate fixation, premature weight-bearing, or poor bone quality can lead to delayed union or non-union. Careful surgical technique and patient compliance are essential. Malunion can lead to persistent or new biomechanical issues.
- Infection: As with any major orthopedic surgery, deep infection is a severe complication. Meticulous sterile technique, appropriate prophylactic antibiotics, and careful wound management are necessary.
-
Overcorrection or Undercorrection:
- Undercorrection: Persistent dysplasia, leading to ongoing pain and accelerated osteoarthritis.
- Overcorrection: Can lead to iatrogenic pincer-type FAI, causing new impingement and pain. Precise intraoperative assessment is critical.
- Avascular Necrosis (AVN) of the Acetabular Fragment: Although rare with the Bernese technique (due to preservation of medial soft tissue attachments), excessive stripping or damage to the fragment's blood supply during mobilization can lead to AVN.
- Post-Operative Sciatic or Femoral Nerve Palsy: Transient neuropraxia can occur due to prolonged traction or direct injury during surgery. While often reversible, it can cause significant morbidity.
- Heterotopic Ossification: Can occur, particularly in the soft tissues around the hip, limiting ROM. Prophylaxis with NSAIDs (e.g., Indomethacin) or radiation therapy may be considered in high-risk patients.
- Progression of Osteoarthritis: Despite successful correction, pre-existing chondral damage can continue to progress, potentially necessitating total hip arthroplasty in the long term. This risk should be clearly communicated to the patient pre-operatively.
You Might Also Like