Operative Management of Thermal Hand Burns
Key Takeaway
Thermal burns of the hand require urgent evaluation to preserve viable tissue, prevent infection, and avoid debilitating contractures. Management dictates a systematic approach, prioritizing life-threatening injuries before assessing burn depth and distal perfusion. Treatment ranges from conservative topical therapies for superficial injuries to early tangential excision, skin grafting, and escharotomy for deep, circumferential burns. Rigorous postoperative rehabilitation is essential for optimal functional recovery.
INTRODUCTION AND INITIAL RESUSCITATION
The evaluation and management of patients with severe thermal burns to the upper extremity must be contextualized within the broader framework of advanced trauma life support (ATLS). Life-threatening injuries, airway compromise, and extensive total body surface area (TBSA) burns take absolute precedence over isolated hand burns.
A critical initial step is the assessment for inhalation injury. The presence of an inhalation injury drastically alters the patient's prognosis; mortality from burns associated with inhalation injury approaches 35%, whereas mortality from burns without inhalation injury is approximately 2%.
Once the patient is hemodynamically stabilized—encompassing appropriate intravenous fluid resuscitation (e.g., Parkland formula), securing of intravenous lines, administration of tetanus prophylaxis, empiric antibiotic therapy (if indicated), and preparation for potential blood transfusions—attention may be directed to the upper extremity.
The overarching priorities in the management of thermal hand burns are:
* Preservation of viable tissue and distal perfusion.
* Prevention of invasive wound infection.
* Control of fibrotic cascades.
* Avoidance of debilitating, irreversible contractures.
Clinical Pearl: The initial examination of a burned hand is often confounded by severe pain, profound edema, and concomitant injuries. However, an accurate estimation of burn depth and a rigorous assessment of distal perfusion are non-negotiable prerequisites for formulating a surgical plan.
CLASSIFICATION AND ASSESSMENT OF BURN DEPTH
Determining the precise depth of a thermal injury dictates the surgical algorithm. While clinical judgment remains the cornerstone of assessment, it can be subjective. Advanced modalities, such as noncontact laser Doppler imaging, have emerged as highly accurate adjuncts for predicting burn depth and healing potential by quantifying microvascular perfusion.
Burns are anatomically classified based on the extent of dermal and epidermal destruction.
Superficial Burns (First-Degree)
Superficial burns involve only the epidermis. Clinically, these present as erythematous, exquisitely tender lesions without blister formation. Capillary refill remains brisk, and the underlying dermis is unharmed. These injuries typically heal spontaneously without surgical intervention.
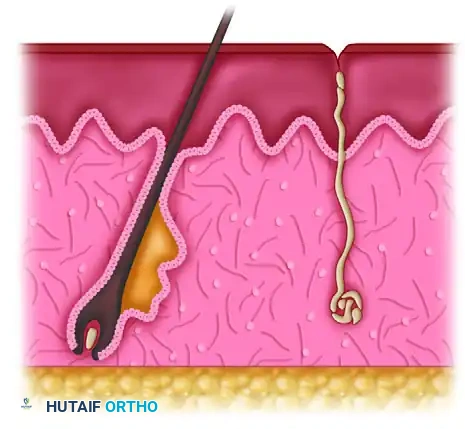
Partial-Thickness Burns (Second-Degree)
Partial-thickness burns extend into the dermis and are subdivided based on the depth of dermal penetration:
* Superficial Partial-Thickness: The injury extends into the papillary dermis. Blisters (vesicles) are a hallmark feature. The wound bed is pink, moist, and hypersensitive. Capillary refill is intact.
* Deep Partial-Thickness: The injury extends into the reticular dermis. The wound bed appears mottled, pale, or waxy. Capillary refill is sluggish or absent, and sensation is markedly diminished due to the destruction of cutaneous nerve endings. Thrombosed superficial veins may be visible.

Full-Thickness Burns (Third and Fourth-Degree)
Full-thickness burns involve the complete destruction of the epidermis and dermis, extending into the subcutaneous fat (third-degree) or deeper structures such as muscle, tendon, and bone (fourth-degree). The skin assumes a leathery, eschar-like appearance that can range from white to brown or charred black. There is a complete absence of capillary refill and sensation.
VASCULAR EVALUATION AND COMPLICATIONS
The most critical immediate determination in upper extremity thermal trauma is the adequacy of distal circulation, particularly in the presence of circumferential burns.
Assessment of Perfusion
Circulation is deemed adequate if the hand and digits exhibit rapid capillary refill, remain pink and warm, and demonstrate pulsatile flow on handheld Doppler ultrasonography of the palmar arch and digital vessels.
Conversely, signs of vascular compromise include:
* Pale, cool, and firm digits.
* Delayed or absent capillary refill.
* Loss of pulsatile Doppler signals in the distal vessels.
* Intractable pain out of proportion to the injury (a hallmark of impending compartment syndrome).
Surgical Warning: The inelastic nature of full-thickness, circumferentially burned skin creates a rigid envelope. As obligatory burn edema accumulates, interstitial pressures rise rapidly, creating a tourniquet effect. If left untreated, this progresses to tissue ischemia, myonecrosis, and irreversible nerve damage.
Escharotomy and Fasciotomy
If distal perfusion is compromised by a circumferential eschar, an immediate escharotomy is indicated. Incisions are made through the eschar to release the constricting envelope.
* Digital Escharotomies: Performed along the mid-axial lines of the digits, carefully avoiding the neurovascular bundles.
* Hand/Forearm Escharotomies: Placed along the radial and ulnar borders.
If intracompartmental pressures remain elevated (>30 mm Hg) despite adequate escharotomy, or if the burn involves deep muscle compartments (e.g., high-voltage electrical injuries), formal fasciotomies of the forearm and hand (including intrinsic compartments) are mandatory.
Arterial Thrombosis and Embolism
Thermal injuries can precipitate local arterial thrombosis. If digital plethysmography or Doppler reveals poor backflow, microvascular intervention may be required.
* Vein Grafting: If the thrombosed segment is localized, it should be resected under operating microscope magnification until normal intima is visualized. A reversed interposition vein graft (typically harvested from the volar forearm or saphenous vein) is then anastomosed.
* Contraindications to Grafting: Erythrocytosis, inadequate peripheral "runoff" on angiography, and patient refusal to cease smoking.
Furthermore, acute arterial emboli in the upper extremity (accounting for 15% to 20% of all emboli) must be differentiated from local thrombosis. Approximately 70% of these emboli are cardiogenic (e.g., atrial fibrillation, mural thrombi). Presentation includes the classic "6 Ps": pallor, pain, paresthesia, paralysis, pulselessness, and poikilothermia. Treatment involves systemic heparinization, Fogarty catheter embolectomy, and potentially intra-arterial thrombolytics (e.g., streptokinase, reteplase) if administered within 36 hours.
SURGICAL MANAGEMENT STRATEGIES
The functional and cosmetic outcome of a burned hand is dictated by burn depth, prevention of infection, and the timing of surgical intervention. The Falcone and Edstrom algorithm provides a structured approach based on TBSA and burn depth.
Management of Superficial Burns
Superficial burns require conservative management. If protected from secondary trauma and infection, they re-epithelialize within 14 to 21 days without significant functional impairment. Treatment consists of topical antimicrobials, synthetic dressings (e.g., Biobrane, Xeroform), and early mobilization.
Management of Partial-Thickness Burns
The management of partial-thickness burns remains a topic of academic debate, generally divided into two schools of thought:
- The "Wait-and-See" Conservative Approach:
Advocates argue that with meticulous wound care (hydrotherapy, topical silver sulfadiazine, mafenide acetate, or povidone-iodine) and aggressive physical therapy, deep dermal burns can heal with functional outcomes comparable to surgery, avoiding donor site morbidity. - The Early Operative Approach (3 to 5 Days):
Proponents of early surgery cite superior outcomes due to accurate early depth determination, rapid physiological closure, accelerated rehabilitation, and the prevention of hypertrophic scarring associated with prolonged healing.
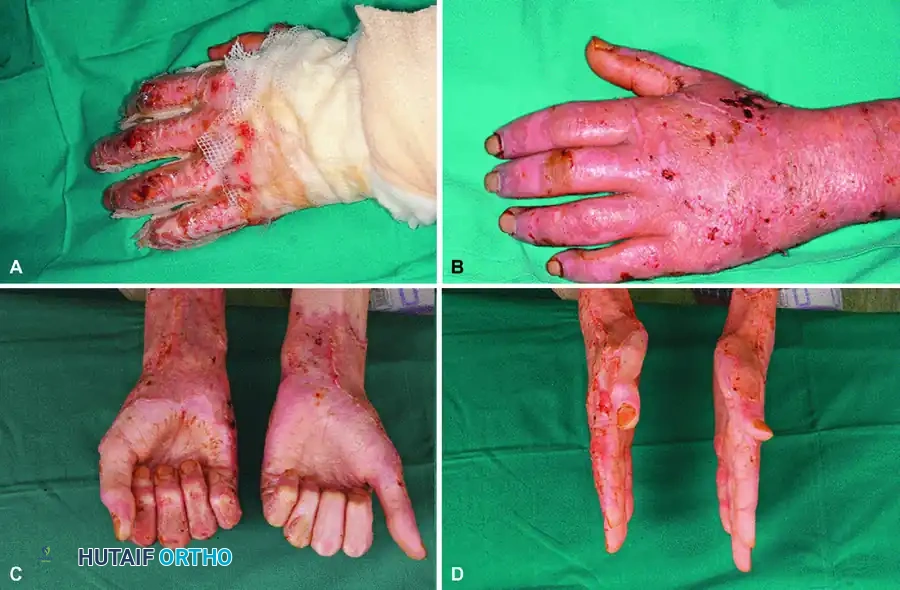
Clinical application of a Biobrane glove to a superficially burned hand, demonstrating excellent cosmetic and functional results after spontaneous healing.
The Dorsal vs. Volar Dichotomy
The unique biomechanical and anatomical properties of the hand necessitate a tailored approach:
* Dorsal Burns: The dorsal skin is exceptionally thin, and the underlying extensor mechanism and interphalangeal joints are highly vulnerable. Dorsal burns benefit from early excision (within 14 days) and grafting to provide protective coverage and permit early mobilization, preventing devastating extension contractures.
* Volar Burns: The palmar skin is thick, glabrous, and tethered by robust fascial septa. The flexor tendons are deeply situated and well-protected. Consequently, volar burns may tolerate a delayed approach (up to 3 weeks) to allow for potential spontaneous epithelialization before committing to excision.
Management of Full-Thickness Burns
Deep full-thickness burns mandate primary full-thickness excision and immediate skin grafting.
When thermal destruction extends beyond the skin to involve tendons, nerves, vessels, or joints, complex reconstructive procedures are required:
* Skeletal Stabilization: Destroyed joints or unstable fractures may require temporary stabilization with Kirschner wires (K-wires) or primary arthrodesis.
* Soft Tissue Coverage: Exposed bone, tendon without paratenon, or neurovascular structures cannot support a free skin graft. These defects necessitate local pedicled flaps (e.g., groin flaps, cross-finger flaps) or free tissue transfer (e.g., anterolateral thigh flap, lateral arm flap) utilizing microvascular techniques.
OPERATIVE TECHNIQUE: TANGENTIAL EXCISION AND GRAFTING
1. Patient Positioning and Preparation
- The patient is positioned supine with the affected extremity extended on a radiolucent hand table.
- A pneumatic tourniquet is applied to the proximal arm to minimize blood loss during excision, though it must be deflated periodically to assess tissue viability and achieve hemostasis.
- The limb is prepped and draped in a standard sterile fashion.
2. Tangential Excision
- Using a Weck blade, Goulian knife, or Watson dermatome, the burn eschar is excised in sequential, paper-thin layers (tangential excision).
- Endpoint of Excision: Excision continues until a bed of viable, punctate bleeding dermal tissue or healthy, glistening yellow subcutaneous fat is reached.
- If the burn is deep, a full-thickness excision down to the investing muscle fascia may be necessary to ensure a viable graft bed.
3. Hemostasis
- Meticulous hemostasis is paramount to prevent subgraft hematoma, the leading cause of graft failure.
- The tourniquet is deflated. Hemostasis is achieved using warm saline compresses, topical epinephrine (1:100,000) soaks, and precise bipolar electrocautery.
4. Skin Grafting
- Split-Thickness Skin Grafts (STSG): Typically harvested from the anterior thigh at a thickness of 0.012 to 0.016 inches. STSGs are preferred for large dorsal defects. They may be meshed (1.5:1) to allow for drainage of exudate, though unmeshed (sheet) grafts provide superior cosmetic results on the hand.
- Full-Thickness Skin Grafts (FTSG): Harvested from the groin or lower abdomen. FTSGs undergo less secondary contracture and are ideal for palmar defects or flexion creases to prevent joint contractures.
- The graft is secured using surgical staples, absorbable sutures, or fibrin glue.
5. Vacuum-Assisted Closure (VAC)
- The advent of negative pressure wound therapy (VAC) has revolutionized graft take. A VAC dressing applied over the grafted site at -75 to -125 mm Hg continuous pressure splints the graft, evacuates hematoma/seroma, and promotes rapid neoangiogenesis.
POSTOPERATIVE PROTOCOL AND REHABILITATION
The surgical intervention is merely the first phase of treatment; rigorous rehabilitation is the primary determinant of ultimate hand function. The rehabilitation team must include specialized hand therapists, occupational therapists, and often psychiatric support to address the profound psychological impact of disfiguring burns.
Splinting and Positioning
Immediately postoperatively, the hand must be immobilized to protect the graft. The hand is placed in the "Intrinsic Plus" (Safe) Position:
* Wrist extended 20° to 30°.
* Metacarpophalangeal (MCP) joints flexed 70° to 90° (to maintain the collateral ligaments at their maximal length, preventing extension contractures).
* Interphalangeal (IP) joints fully extended (to prevent boutonnière deformities).
* Thumb abducted and opposed (to maintain the first web space).
Mobilization and Scar Management
- Early Phase (Days 0-5): Immobilization to ensure graft adherence. Edema control via strict elevation.
- Intermediate Phase (Days 5-14): Once graft take is confirmed, active and active-assisted range of motion (ROM) exercises are initiated. Continuous passive motion (CPM) machines may be utilized.
- Late Phase (Weeks to Months): Focus shifts to scar management. Hypertrophic scarring is mitigated through the use of custom-fitted compression garments (providing >30 mm Hg pressure), silicone gel sheets, and aggressive soft tissue mobilization. Dynamic splinting is employed to combat developing contractures.
Clinical Pearl: Patient compliance is the most significant variable in the late phase of burn recovery. A technically perfect excision and grafting procedure will inevitably fail if the patient does not adhere to the rigorous, often painful, months-long rehabilitation and splinting protocols.
You Might Also Like
