Operative Management of Pes Planus and Tarsal Coalition: A Comprehensive Surgical Guide
Key Takeaway
Pes planus and tarsal coalition represent complex hindfoot deformities requiring precise biomechanical correction. Surgical management ranges from soft tissue reconstruction and lateral column lengthening to corrective osteotomies and arthrodesis. This comprehensive guide details the indications, surgical approaches, and postoperative protocols for procedures including the Evans calcaneal lengthening, medializing calcaneal osteotomy, Kidner procedure, and tarsal coalition resection, providing evidence-based strategies for orthopedic surgeons to optimize patient outcomes.
Introduction to Pes Planus and Tarsal Coalition
The surgical management of pes planus (flatfoot) and tarsal coalition represents a cornerstone of reconstructive foot and ankle surgery. Historically, the literature—ranging from the seminal works of Evans, Grice, and Kidner to the modern biomechanical analyses of Mosca, Sangeorzan, and Cowell—has dictated a progressive, stepwise approach to these complex deformities.
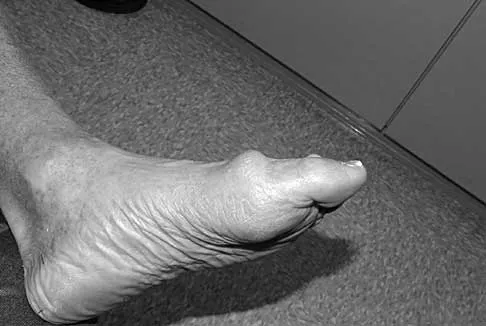
Pes planus is not a singular diagnosis but a spectrum of peritalar subluxations. It ranges from the pediatric flexible flatfoot to the rigid, degenerative adult-acquired flatfoot deformity (AAFD). Conversely, tarsal coalition presents as a "peroneal spastic flatfoot," characterized by a rigid, painful hindfoot secondary to anomalous mesenchymal segmentation. This masterclass delineates the evidence-based surgical indications, biomechanical principles, and step-by-step operative techniques required to correct these profound architectural collapses.
Biomechanics and Pathoanatomy
Understanding the kinematic chain of the hindfoot is paramount. The talocalcaneonavicular joint functions as the acetabulum pedis, a dynamic socket that dictates midfoot and forefoot positioning.
In pes planus, failure of the static stabilizers (the spring ligament complex, plantar fascia, and plantar ligaments) and dynamic stabilizers (primarily the posterior tibial tendon [PTT]) leads to a predictable sequence of collapse:
1. Hindfoot Valgus: Eversion of the calcaneus beneath the talus.
2. Midfoot Abduction: Uncovering of the talar head as the navicular subluxates laterally.
3. Forefoot Supination: A compensatory mechanism to keep the medial column plantigrade, which eventually becomes a fixed supinatus deformity.
Clinical Pearl: Always assess the flexibility of the hindfoot and the reducibility of the forefoot supinatus (the Silfverskiöld test and the Hubscher maneuver/Jack's test). A fixed forefoot varus/supinatus will doom a hindfoot correction if not addressed concurrently with a medial column procedure (e.g., plantarflexing medial cuneiform osteotomy).
Surgical Management of Flexible Pes Planus
When conservative measures (orthoses, physical therapy) fail in the symptomatic patient, surgical intervention aims to restore the medial longitudinal arch while preserving joint kinematics.
Lateral Column Lengthening (The Evans and Mosca Procedures)
Originally described by Evans and later refined by Mosca, lateral column lengthening corrects midfoot abduction and hindfoot valgus by tensioning the plantar fascia and spring ligament through the "windlass" mechanism.
Indications:
Symptomatic flexible pes planus with significant uncovering of the talonavicular joint (>30%) and midfoot abduction.
Patient Positioning:
Supine with a bump under the ipsilateral hip to internally rotate the leg, bringing the lateral border of the foot directly anterior.
Surgical Approach:
1. Make an oblique incision over the sinus tarsi, extending from the tip of the lateral malleolus toward the base of the fourth metatarsal (Ollier approach).
2. Carefully identify and retract the sural nerve and peroneal tendons inferiorly.
3. Elevate the extensor digitorum brevis (EDB) muscle belly to expose the calcaneocuboid (CC) joint and the anterior process of the calcaneus.
Step-by-Step Technique:
1. Osteotomy Placement: Identify the CC joint. The osteotomy is performed exactly 1.5 cm proximal to the CC joint line, parallel to the joint surface.
2. Bone Cut: Use an oscillating saw to cut the lateral cortex, proceeding medially. Leave the medial calcaneal cortex intact to act as a periosteal hinge.
3. Distraction: Insert a lamina spreader into the osteotomy. Gently distract to lengthen the lateral column. Clinically observe the correction of the midfoot abduction and the spontaneous restoration of the medial arch.
4. Grafting: Harvest a tricortical structural graft from the ipsilateral iliac crest (or utilize a precisely sized allograft wedge, typically 8 to 12 mm). Shape the graft into a trapezoid and impact it into the defect.
5. Fixation: While the graft is often stable under compression, fixation with a cervical spine plate or a fully threaded cortical screw is highly recommended to prevent graft extrusion.
Surgical Warning: Over-lengthening the lateral column can lead to catastrophic calcaneocuboid joint subluxation, lateral column overload, and fifth metatarsal stress fractures. Do not exceed a 12 mm graft in pediatric patients.
Medializing Calcaneal Osteotomy (Koutsogiannis Procedure)
For patients with hindfoot valgus without severe midfoot abduction, a medial displacement calcaneal osteotomy (MDCO) shifts the mechanical axis of the Achilles tendon medially, converting it from an evertor to an invertor of the hindfoot.
Indications:
Stage II Adult Acquired Flatfoot Deformity (PTTD) or pediatric flexible flatfoot driven primarily by hindfoot valgus.
Surgical Approach:
1. Make an oblique lateral incision posterior to the peroneal tendons and sural nerve, angled at 45 degrees to the plantar aspect of the foot.
2. Dissect sharply to the periosteum of the calcaneal tuberosity.
Step-by-Step Technique:
1. Osteotomy: Using a sagittal saw, perform an osteotomy at a 45-degree angle to the plantar surface, ensuring the cut is posterior to the posterior facet of the subtalar joint.
2. Displacement: Complete the medial cortex cut with a broad osteotome. Manually translate the posterior tuberosity medially by 10 to 15 mm (approximately 50% of the calcaneal width).
3. Fixation: Secure the osteotomy with one or two 6.5 mm or 7.3 mm cannulated, partially threaded screws directed from the posterior-inferior heel toward the anterior process of the calcaneus.
Surgical Management of the Symptomatic Accessory Navicular
The accessory navicular (os tibiale externum) alters the insertion of the posterior tibial tendon, weakening its mechanical advantage and leading to flatfoot and localized pain.
The Modified Kidner Procedure
Indications:
Type II or Type III accessory navicular with localized pain, PTT tendinosis, and failure of conservative management.
Surgical Approach:
1. Make a medial longitudinal incision centered over the prominent navicular tuberosity.
2. Identify the PTT and its insertion into the accessory bone.
Step-by-Step Technique:
1. Excision: Make a longitudinal incision in the PTT. Carefully shell out the accessory navicular using a scalpel and small osteotomes, preserving the continuity of the plantar fibers of the PTT.
2. Reshaping: Resect the prominent medial flare of the primary navicular until it is flush with the medial cuneiform.
3. Tendon Advancement: Advance the PTT anteriorly and inferiorly. Secure it to the plantar-medial aspect of the primary navicular using suture anchors. This restores the tendon's physiological tension and arch-supporting function.
Surgical Management of Rigid Pes Planus (Adult Acquired Flatfoot)
When the deformity becomes rigid and arthritic (Stage III AAFD), joint-sparing osteotomies are contraindicated. Arthrodesis becomes the gold standard.
Triple Arthrodesis
A triple arthrodesis fuses the subtalar, talonavicular (TN), and calcaneocuboid (CC) joints.
Indications:
Rigid, painful pes planus, severe degenerative joint disease of the hindfoot, or failed prior reconstructions.
Step-by-Step Technique:
1. Approaches: Utilize a dual-incision technique. A lateral Ollier approach for the subtalar and CC joints, and a medial utility approach for the TN joint.
2. Joint Preparation: Denude all cartilage from the TN, CC, and subtalar joints using osteotomes, curettes, and a high-speed burr. Punctate the subchondral bone to expose bleeding cancellous bone (the "fish-scale" technique).
3. Correction of Deformity: The key to a triple arthrodesis is the reduction. First, correct the hindfoot valgus at the subtalar joint. Second, reduce the talonavicular joint by plantarflexing the talus and rotating the navicular medially.
4. Fixation Sequence:
* Subtalar Joint: Fix with one or two 7.3 mm cannulated screws from the calcaneal tuberosity into the talar dome.
* Talonavicular Joint: Fix with two 4.5 mm or 5.0 mm screws, or a specialized compression plate. This is the most critical joint for stability.
* Calcaneocuboid Joint: Fix with a single 4.5 mm screw or staples.
Pitfall: Failure to adequately prepare the talonavicular joint is the leading cause of nonunion in triple arthrodesis. Ensure aggressive decortication and rigid compression.
Surgical Management of Tarsal Coalition (Spastic Flatfoot)
Tarsal coalitions restrict normal peritalar motion, leading to adaptive shortening of the peroneal tendons (spasticity) and a rigid flatfoot. The two most common types are calcaneonavicular (CN) and talocalcaneal (TC) middle facet coalitions.
Calcaneonavicular Coalition Resection
Indications:
Symptomatic CN coalition in a patient typically aged 8-12 years, without advanced secondary degenerative changes.
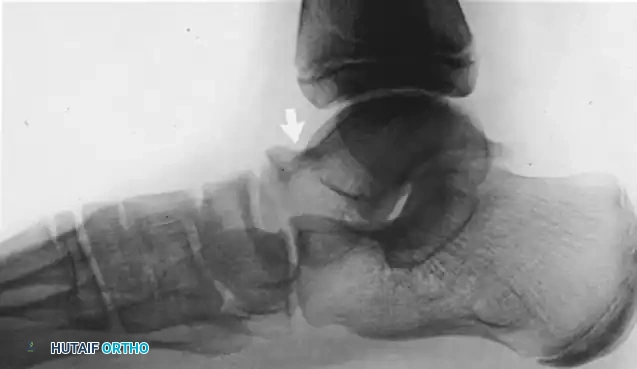
Radiographic Sign: The "Anteater Nose" sign on the lateral radiograph.
Step-by-Step Technique:
1. Approach: Lateral Ollier incision.
2. Exposure: Elevate the EDB muscle belly proximally to expose the coalition between the anterior process of the calcaneus and the lateral navicular.
3. Resection: Use a sagittal saw and rongeurs to resect a rectangular block of bone (at least 1.5 cm wide) to completely eradicate the coalition. Ensure normal cartilage is visualized on the talar head medially and the cuboid distally.
4. Interposition: To prevent recurrence, mobilize the EDB muscle belly and suture it into the defect using drill holes in the calcaneus or navicular. Alternatively, a free fat graft may be utilized.
Talocalcaneal (Middle Facet) Coalition Resection
Indications:
Symptomatic TC coalition (typically presenting at ages 12-16) involving less than 50% of the posterior facet surface area, with no hindfoot arthritis.
Radiographic Sign: The "C-Sign" on the lateral radiograph and bridging on the coronal CT scan.
Step-by-Step Technique:
1. Approach: Medial longitudinal incision centered inferior to the medial malleolus, following the course of the PTT.
2. Exposure: Retract the PTT dorsally and the flexor digitorum longus (FDL) and neurovascular bundle plantarward. The flexor hallucis longus (FHL) runs directly plantar to the sustentaculum tali and must be protected.
3. Identification: The coalition replaces the normal middle facet of the subtalar joint, appearing as a continuous bridge of bone or fibrocartilage between the talus and the sustentaculum tali.
4. Resection: Use a high-speed burr and small osteotomes to resect the coalition from medial to lateral. The resection is complete when the posterior facet cartilage is visualized laterally and normal subtalar motion is restored intraoperatively.
5. Interposition: Pack the defect with a robust autologous fat graft (harvested from the Kager's fat pad or gluteal region) or bone wax to prevent hematoma organization and re-ossification.
Surgical Warning: The neurovascular bundle and the FHL tendon are at extreme risk during middle facet resection. Maintain meticulous hemostasis and use blunt retractors (e.g., mini-Hohmanns) to protect plantar structures.
Postoperative Rehabilitation Protocols
Successful outcomes rely heavily on strict adherence to postoperative protocols, which vary based on the inclusion of arthrodesis or osteotomy.
For Osteotomies and Coalition Resections (Evans, MDCO, Tarsal Coalition):
* Weeks 0-2: Strict non-weight-bearing (NWB) in a well-padded short leg splint. Elevation is critical to manage edema.
* Weeks 2-6: Suture removal. Transition to a short leg fiberglass cast or rigid CAM boot. Remain NWB. For coalition resections, early active range of motion (ROM) exercises of the subtalar joint may be initiated at week 3 to prevent arthrofibrosis.
* Weeks 6-12: Radiographic assessment for bony union. Transition to progressive weight-bearing in a CAM boot. Initiate formal physical therapy focusing on PTT strengthening, peroneal stretching, and proprioception.
* Months 3-6: Transition to supportive athletic shoes with custom orthoses. Return to high-impact activities is restricted until 6 months postoperatively.
For Arthrodesis (Triple Arthrodesis, Grice Procedure):
* Weeks 0-6: Strict NWB in a short leg cast.
* Weeks 6-10: Clinical and radiographic check. If bridging trabeculae are present, transition to a CAM boot with partial weight-bearing (25-50%).
* Weeks 10-14: Progression to full weight-bearing in the boot, followed by transition to a stiff-soled shoe.
Conclusion
The operative management of pes planus and tarsal coalition demands a profound understanding of hindfoot biomechanics and a meticulous surgical technique. Whether performing a joint-sparing lateral column lengthening for a pediatric flexible flatfoot, a Kidner procedure for an accessory navicular, or a complex triple arthrodesis for end-stage deformity, the surgeon must respect the delicate interplay of the peritalar soft tissues and osseous architecture. By adhering to these evidence-based principles, orthopedic surgeons can reliably restore a plantigrade, painless, and functional foot.
You Might Also Like