Partial Nail Plate Removal: Comprehensive Surgical Technique and Clinical Guidelines
Key Takeaway
Partial nail plate removal is a foundational orthopedic procedure for managing onychocryptosis. This technique involves the targeted excision of the lateral nail margin while preserving the central nail plate and matrix. Although associated with higher recurrence rates than complete avulsion, it remains a preferred initial intervention in adolescents to avoid permanent cosmetic deformity. Meticulous technique is required to prevent iatrogenic matrix injury and subsequent nail dystrophy.
Introduction to Partial Nail Plate Removal
Partial nail plate removal (partial nail avulsion) is a highly ubiquitous and foundational procedure in operative orthopedics and podiatric surgery, primarily indicated for the management of onychocryptosis (ingrown toenail). The procedure involves the longitudinal excision of the offending lateral or medial border of the nail plate, relieving mechanical impingement on the adjacent paronychial soft tissues.
While the fundamental principles of partial nail plate removal differ little from total nail plate removal, the partial approach requires a more nuanced, targeted technique to preserve the central nail plate and its underlying sterile matrix. This preservation is critical for maintaining the normal biomechanical function of the distal phalanx and ensuring an acceptable cosmetic outcome. In the orthopedic setting, this procedure is frequently performed on the hallux, which bears the brunt of propulsive forces during the terminal stance phase of the human gait cycle.
This comprehensive guide delineates the surgical anatomy, biomechanical considerations, precise operative steps, and postoperative protocols required to execute a partial nail plate removal successfully, minimizing the risk of iatrogenic matrix injury and managing the inherently high recurrence rates associated with simple avulsion techniques.
Surgical Anatomy of the Perionychium
A profound understanding of the nail unit (perionychium) is mandatory for the orthopedic surgeon to avoid catastrophic iatrogenic deformities. The nail unit is a complex, specialized appendage comprising several distinct anatomical structures:
- The Nail Plate: The hard, keratinized structure that provides dorsal protection to the distal phalanx and acts as a counterforce for the plantar pulp during tactile sensation and weight-bearing.
- The Germinal Matrix: Located proximally beneath the eponychium (cuticle), this highly vascular tissue is responsible for generating approximately 90% of the nail plate's volume. It extends proximally to the insertion of the extensor hallucis longus tendon.
- The Sterile Matrix (Nail Bed): Extending from the lunula to the hyponychium, the sterile matrix tightly adheres to the undersurface of the nail plate, contributing to its thickness and providing a smooth gliding surface for distal growth.
- The Lateral Nail Folds (Paronychium): The soft tissue borders that flank the medial and lateral margins of the nail plate. In onychocryptosis, these folds become hypertrophic, inflamed, and frequently infected due to mechanical penetration by the nail spicule.
- The Eponychium and Hyponychium: The eponychium forms the proximal cutaneous seal protecting the germinal matrix, while the hyponychium forms the distal seal at the junction of the nail bed and the glabrous skin of the toe tip.
💡 Clinical Pearl: The Lateral Matrix Horn
The germinal matrix does not end abruptly at the visible lateral margins of the nail. It extends proximally and laterally into the "lateral horns." Failure to recognize and address the full proximal extent of the lateral nail plate beneath the eponychium is the primary cause of surgical failure and recurrence in partial nail avulsions.
Pathomechanics and Indications
Pathophysiology of Onychocryptosis
Onychocryptosis occurs when the lateral or medial edge of the nail plate penetrates the adjacent paronychial fold. This mechanical breach initiates a robust foreign-body inflammatory cascade. The resulting edema exacerbates the impingement, leading to a vicious cycle of pressure, microtrauma, and the formation of highly vascular, friable granulation tissue. Secondary bacterial colonization (typically Staphylococcus aureus) frequently ensues, converting a mechanical problem into an infectious one.
Common etiologies include improper nail trimming (cutting the corners too short), constricting footwear (narrow toe boxes), hyperhidrosis, and genetic predispositions such as a naturally incurvated (pincer) nail plate.
Indications for Partial Nail Plate Removal
The decision to perform a partial versus complete nail plate removal hinges on the severity of the disease, the condition of the central nail plate, and patient demographics.
Partial nail plate removal is indicated for:
1. Heifetz Stage II and III Onychocryptosis: Where conservative measures (cotton wicking, taping, warm soaks) have failed, and there is active infection, drainage, and granulation tissue formation localized to one border.
2. Adolescent and Pediatric Populations: In younger patients, simple partial avulsion—even if it must be repeated due to recurrence—is an highly attractive alternative to procedures that permanently alter the appearance of the nail (such as chemical or surgical matrixectomy).
3. Preservation of Function: When the central nail plate is healthy and free of severe onychomycosis or global dystrophy, preserving it maintains the counter-pressure required for normal toe pulp biomechanics.
Contraindications
- Absolute: Severe peripheral arterial disease (ischemia) where any surgical trauma may precipitate gangrene.
- Relative: Global nail dystrophy, severe onychomycosis involving the entire plate, or extensive paronychia tracking beneath the central nail plate (which necessitates total nail plate removal).
Preoperative Preparation and Patient Counseling
Informed Consent and Managing Expectations
The patient, and especially the parents of an adolescent, must be thoroughly counseled regarding the specific limitations and risks of this procedure.
⚠️ Surgical Warning: Recurrence and Deformity
The recurrence rate is significantly higher after simple partial nail plate removal than after complete removal or partial removal combined with chemical matrixectomy. Furthermore, patients must be explicitly warned that the nail-forming matrix may be inadvertently injured during the procedure, and some permanent deformity, even if minor, may result. Documenting this discussion is medicolegally imperative.
Anesthesia
The procedure is performed under a digital block.
1. Utilize a 1% or 2% Lidocaine solution, typically mixed with 0.5% Bupivacaine for prolonged postoperative analgesia.
2. Perform a classic two-point dorsal approach or a four-point ring block at the base of the hallux, ensuring complete anesthesia of the proper plantar and dorsal digital nerves.
3. Allow 10 to 15 minutes for the block to take full effect before initiating any surgical stimulation.
Hemostasis
A bloodless surgical field is critical for visualizing the proximal matrix and ensuring complete removal of the offending spicule. Exsanguinate the digit by elevating it, and apply a sterile digital tourniquet (such as a rolled Penrose drain or a commercial digital pneumatic tourniquet) at the base of the toe.
Surgical Technique: Step-by-Step
The operative technique for partial nail plate removal requires precision to avoid collateral damage to the central sterile matrix and the proximal germinal matrix.
Step 1: Elevation of the Lateral Nail Plate
The initial step involves separating the offending lateral (or medial) margin of the nail plate from its underlying sterile matrix and the overlying eponychium.
- Introduce a small, angled probe, a Freer elevator, or one arm of a narrow, smooth, straight hemostat beneath the distal free edge of the nail plate.
- Gently advance the instrument proximally, lifting the lateral fourth of the nail from its bed.
- Crucial Technique Note: Do not lift too firmly. Excessive upward or lateral force must be avoided to prevent inadvertently detaching the central, healthy portion of the nail from its bed in a lateral direction. The goal is to create a longitudinal tunnel strictly limited to the segment slated for excision.
Step 2: Longitudinal Incision of the Nail Plate
Once the lateral fourth is adequately separated from the underlying bed, the nail plate must be sharply divided.
- Using heavy, straight tissue scissors or a specialized English anvil nail splitter, cut the nail plate longitudinally from distal to proximal.
- While cutting, continuously lift the lateral fourth off its bed to maintain visualization and protect the underlying sterile matrix.
- Instrument Selection Pearl: Utilizing scissors with a curved tip (oriented upward, away from the bed) is highly recommended, as it is significantly less likely to gouge or damage the underlying matrix during the proximal advancement of the cut.
Step 3: Proximal Extraction and Spicule Removal
The most critical phase of the procedure is ensuring the complete removal of the proximal nail spicule.
- The nail must be incised to its absolute proximal end, extending deeply beneath the eponychium.
- Grasp the divided lateral fourth of the nail plate with a sturdy hemostat.
- Apply a gentle, steady traction combined with a rotational motion (rotating the fragment toward the midline of the nail bed) to avulse the proximal segment from the germinal matrix.
- Inspect the extracted fragment. It should exhibit a smooth, feathered proximal edge, confirming that the entire lateral horn has been removed. If the proximal edge is jagged or broken, a retained spicule remains beneath the eponychium and must be meticulously retrieved.

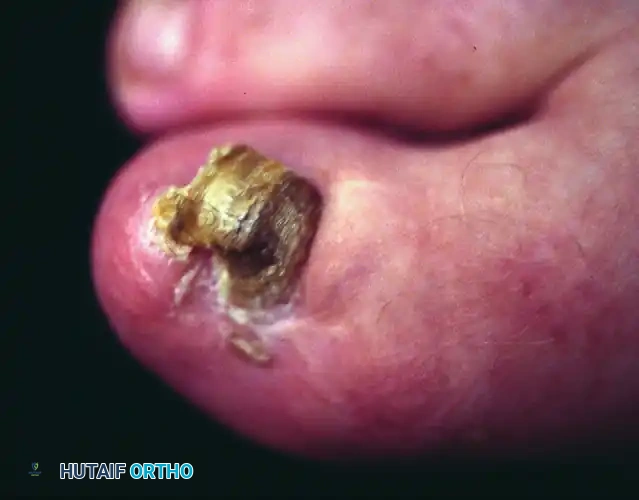
FIGURE 87-7 Inadequate partial nail plate removal. The lateral fourth of the nail plate should be removed completely beneath the eponychium to prevent immediate recurrence.
Step 4: Management of Granulation Tissue
The hypertrophic granulation tissue occupying the lateral nail fold must be addressed to allow for proper healing and to reduce the physical bulk of the paronychium.
- Remove the friable granulation tissue by gently scraping the lateral gutter with a scalpel blade (a #15 or #64 Beaver blade is highly effective) or a sharp curette.
- Alternatively, for severe, fibrotic hypertrophy, the tissue can be removed totally by elliptically excising part of the lateral nail fold. This sharp excision reduces the soft tissue volume that might otherwise impinge on the newly growing nail plate.
- Irrigate the lateral gutter copiously with sterile saline to flush out debris and residual bacteria.
Step 5: Dressing and Tourniquet Release
- Apply a non-adherent dressing (e.g., Adaptic or Xeroform) directly into the lateral gutter to prevent the fold from adhering to the raw sterile matrix.
- Apply a bulky, sterile gauze compression dressing.
- Crucial Step: Release the digital tourniquet and confirm capillary refill to the distal pulp before the patient leaves the operating theater.
Postoperative Care and Rehabilitation
The aftertreatment for partial nail plate removal is straightforward and mirrors that of complete nail plate removal, with the advantage of a slightly faster return to normal footwear.
- Immediate Postoperative Phase (Days 0-2): The patient should keep the foot strictly elevated above heart level to minimize throbbing pain and postoperative edema. Analgesia is typically managed with over-the-counter NSAIDs or acetaminophen. The bulky surgical dressing remains intact and dry.
- Dressing Changes (Day 3 onwards): The patient may remove the initial bulky dressing. Daily warm water or Epsom salt soaks (15-20 minutes) are initiated to gently debride exudate and soothe the healing tissues. Following the soak, a clean, light dressing (such as a simple adhesive bandage) is applied.
- Footwear: By the third or fourth postoperative day, the patient can typically transition into wearing a closed, wide toe box shoe. Tight, constricting footwear must be strictly avoided to prevent medial-lateral compression of the healing paronychium.
- Return to Activity: Normal weight-bearing is permitted as tolerated. High-impact athletic activities should be deferred until the lateral gutter is fully epithelialized, which generally takes 2 to 3 weeks.
Complications and Management
While partial nail plate removal is a minor procedure, complications can be frustrating for both the patient and the surgeon.
1. High Recurrence Rates
As previously noted, the recurrence rate of onychocryptosis is inherently higher after simple partial nail plate removal compared to complete removal or partial removal combined with chemical ablation (phenolization) of the matrix.
* Mechanism: Because the germinal matrix is left intact, a new lateral nail margin will eventually grow distally. If the underlying biomechanical factors (tight shoes, improper trimming) are not corrected, the new nail will likely re-impinge on the soft tissue.
* Management: Recurrences are managed by repeating the partial avulsion. If recurrences become chronic, the surgeon should step up the treatment algorithm to include a partial matrixectomy (chemical or surgical) to permanently narrow the nail plate.
2. Iatrogenic Matrix Injury and Nail Deformity
Aggressive instrumentation, improper use of sharp scissors, or excessive force during the elevation phase can lacerate the sterile or germinal matrix.
* Consequence: Lacerations to the matrix heal with fibrotic scarring. Because the nail plate requires a smooth, continuous matrix to grow properly, a scar will result in a permanent longitudinal split, ridging, or severe dystrophy of the newly formed nail plate.
* Prevention: Meticulous adherence to the technique—specifically, not lifting the central nail plate and using curved-tip scissors—is paramount.
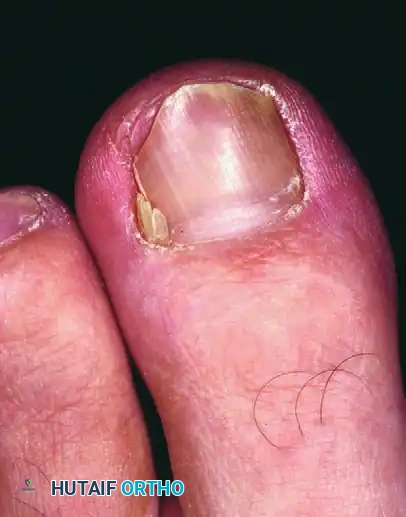
FIGURE 87-8 Deformity of the nail bed after inadvertent laceration of the nail matrix during partial avulsion. Note the permanent longitudinal ridging and dystrophy.
3. Infection
Postoperative infection is rare if the procedure is performed under sterile conditions and the necrotic granulation tissue is adequately debrided. However, if cellulitis develops, extending proximally beyond the eponychium, oral antibiotics targeting skin flora (e.g., Cephalexin) are indicated.
4. Epidermal Inclusion Cysts
Incomplete removal of the proximal nail spicule or driving epithelial cells deep into the paronychium during the procedure can lead to the formation of an epidermal inclusion cyst or a chronic foreign body granuloma. This presents as a persistent, painful, non-healing nodule at the proximal nail fold, necessitating surgical exploration and excision of the retained spicule and cyst wall.
Conclusion
Partial nail plate removal remains an indispensable technique in the orthopedic surgeon's armamentarium for treating onychocryptosis. By selectively removing the offending lateral margin, the surgeon rapidly alleviates pain and resolves localized infection while preserving the biomechanical and cosmetic integrity of the central nail unit.
Although the procedure carries a known risk of recurrence—making it particularly suited as a first-line, joint-sparing intervention in pediatric and adolescent populations—strict adherence to the anatomical principles of the perionychium and meticulous surgical execution can significantly optimize clinical outcomes and minimize the risk of permanent iatrogenic deformity.
You Might Also Like