Malignant Tumors of the Hand: Principles of Surgical Oncology and Resection
Key Takeaway
Malignant tumors of the hand are rare but require aggressive, multidisciplinary management. Chondrosarcoma is the most common primary bone malignancy, while soft tissue sarcomas include undifferentiated pleomorphic sarcoma and epithelioid sarcoma. Successful surgical intervention relies on achieving negative oncologic margins through wide local excision, ray resection, or amputation. Limb-sparing surgery combined with adjuvant therapy is increasingly utilized, though survival heavily depends on tumor stage and size.
INTRODUCTION TO MALIGNANT TUMORS OF THE HAND
Malignant tumors of the hand are exceedingly rare, particularly those arising beneath the skin. A landmark 65-year retrospective review (1920–1985) from the Mayo Clinic by Frassica and Amadia highlighted the infrequency of these lesions, noting that their rarity often leads to delayed diagnosis and inadequate initial management. The complex, compact anatomy of the hand—where neurovascular bundles, tendons, and bone are in intimate proximity—makes achieving wide oncologic margins challenging without compromising profound functional capacity.
Proper surgical treatment of malignant hand tumors mandates the excision of surrounding normal tissue and, occasionally, partial or below-elbow amputation. The ultimate success of surgical intervention is strictly dependent on whether residual microscopic or macroscopic tumor is left behind (R0 vs. R1/R2 resection). While early literature suggested that malignant bone tumors of the hand rarely metastasize, contemporary evidence confirms that metastasis can and does occur, particularly following local recurrence.
Surgical Warning: Local recurrence of a malignant hand tumor has not been definitively shown to independently affect overall survival; however, larger tumor size (>5 cm) and advanced histological stage have a profound negative impact on patient prognosis.
Historically, amputation was considered the gold standard. Today, multidisciplinary treatment—combining limb-sparing surgery with brachytherapy, external beam radiation, and systemic chemotherapy—has yielded 5-year survival rates exceeding 70% in patients with high-grade soft tissue sarcomas of the extremity. Nevertheless, in cases where limb-salvage precludes negative margins or results in a non-functional, insensate appendage, amputation remains the superior oncologic and functional choice.
PRIMARY BONE MALIGNANCIES
Chondrosarcoma
Chondrosarcoma is the most common primary bone malignancy of the hand. It typically presents in the metacarpals and phalanges and exhibits a slight male predilection.
Differentiating a low-grade chondrosarcoma from a benign enchondroma is one of the most challenging diagnostic dilemmas in orthopedic oncology.
* Clinical Presentation: Pain is the hallmark presenting symptom of chondrosarcoma, whereas uncomplicated enchondromas are almost universally painless unless associated with a pathologic fracture. A fracture may occur as the cortical bone is progressively weakened by the expanding chondroid matrix.
* Diagnostic Suspicion: A chondrosarcoma must be highly suspected if a cartilaginous lesion is painful in the absence of fracture, or if it rapidly recurs following routine curettage and bone grafting of a presumed enchondroma.
* Radiographic Findings: Radiographs typically demonstrate cortical expansion, endosteal scalloping (>2/3 of cortical thickness), and spotty calcifications. Permeative patterns of bone destruction and periosteal reactions are indicative of higher-grade lesions.
Surgical Management:
When chondrosarcoma is confirmed via biopsy, anything short of total en bloc resection—such as a ray resection or wide local excision—is usually unsuccessful and leads to local recurrence. Curettage is strictly contraindicated. If radical surgery (en bloc resection with wide margins) is performed as the primary procedure, local recurrence is highly unlikely, and the long-term prognosis is excellent. Interestingly, long-term survival after aggressive treatment is generally better for chondrosarcomas located in the hand compared to identical lesions in the axial skeleton or proximal appendicular skeleton.
Osteogenic Sarcoma (Osteosarcoma)
Osteogenic sarcoma is exceptionally rare in the hand. The average age at presentation is 49 years, which is significantly older than the typical adolescent demographic seen with long-bone osteosarcomas.
- Etiology: A notable subset of hand osteosarcomas has been linked to prior irradiation from overexposure to X-rays or the historical ingestion/handling of radium salts.
- Clinical Behavior: These tumors are locally aggressive and carry a high risk of pulmonary metastasis.
- Surgical Management: Careful wide excision of the tumor offers a good prognosis. The surgical approach is dictated by the tumor variant and location:
- Periosteal Variant: Often amenable to digital amputation or ray resection, provided negative margins can be obtained.
- Intramedullary/High-Grade Variants: Ray amputation or below-elbow amputation is more appropriate to ensure complete eradication of the disease and skip lesions.
Due to the rarity of osteosarcoma in the hand, treatment decisions are often extrapolated from limited data. However, similar to chondrosarcoma, the prognosis for hand osteosarcoma appears to be more favorable than for lesions located in the proximal extremities.
SOFT TISSUE SARCOMAS
Soft tissue sarcomas of the hand present as painless, progressively enlarging masses. The most common histological subtypes include:
1. Undifferentiated Pleomorphic Sarcoma (formerly Malignant Fibrous Histiocytoma - MFH): The most common soft tissue sarcoma in older adults.
2. Epithelioid Sarcoma: Frequently presents in young adults as a superficial, nodular mass that may ulcerate, mimicking a benign process or infection. Crucially, epithelioid sarcoma has a high propensity for lymphatic spread, necessitating regional lymph node evaluation.
3. Synovial Sarcoma: Despite its name, it rarely arises from the joint synovium. It typically occurs near tendons and aponeuroses in young adults. Radiographs may show fine stippled calcifications in up to 30% of cases.
4. Other Variants: Liposarcoma, leiomyosarcoma, fibrosarcoma, rhabdomyosarcoma (more common in the pediatric population, specifically the alveolar subtype in the hand), and malignant peripheral nerve sheath tumors.
Surgical Management:
Treatment requires a multidisciplinary approach. Wide surgical excision is the cornerstone of therapy. If the tumor is intimately involved with major neurovascular structures, limb-sparing surgery may require complex vascular reconstruction or nerve grafting. If a functional hand cannot be preserved, amputation is indicated. Adjuvant radiation (brachytherapy or external beam) and chemotherapy are utilized based on tumor grade, size, and histological subtype.
CUTANEOUS MALIGNANCIES OF THE HAND
While the raw data primarily focuses on deep tumors, cutaneous malignancies are the most common cancers of the hand overall.
* Squamous Cell Carcinoma (SCC): Occurs predominantly on the sun-exposed dorsal areas of the hand. It is more common in males. Treatment involves wide local excision with or without skin grafting. The prognosis is generally excellent, with a recurrence rate of approximately 1%.
* Malignant Melanoma: Can occur anywhere on the hand, including the nail bed (subungual melanoma, often presenting as Hutchinson's sign), but is uncommon in the palm. Survival is directly related to tumor thickness (Breslow depth). Management involves wide excision, often requiring amputation for recurrent, deep, or subungual tumors, combined with sentinel lymph node biopsy or formal lymph node dissection for symptomatic recurrence.
BENIGN AND LOCALLY AGGRESSIVE MIMICKERS
When evaluating a hand mass, several benign but locally aggressive or structurally significant lesions must be considered in the differential diagnosis.
Osteochondroma
Osteochondromas are benign cartilage-capped bone tumors. While common in the appendicular skeleton, they can present in the hand, often causing mechanical symptoms or cosmetic deformity.
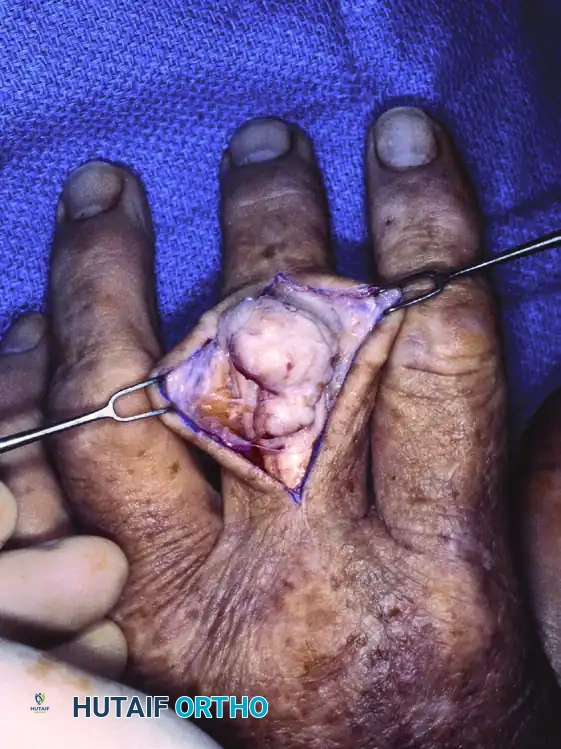
FIGURE 77-19 A: Lateral radiograph demonstrating an osteochondroma of long duration in a 70-year-old man, presenting as a dense, exophytic mass arising from the volar aspect of the phalanx.
Surgical excision is indicated for pain, mechanical block to tendon excursion, or sudden growth (which may herald malignant transformation to secondary chondrosarcoma, though this is exceedingly rare in the hand). Excision must include the entire cartilaginous cap to prevent recurrence.
Synovial Chondromatosis
Synovial chondromatosis is a rare, benign, metaplastic condition of the synovial membrane characterized by the formation of multiple cartilaginous nodules within the joint space or tendon sheath.
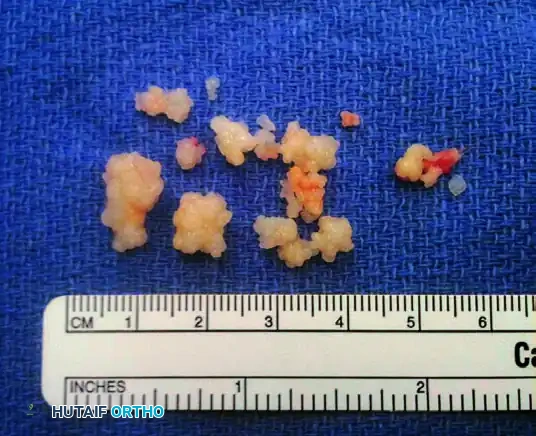
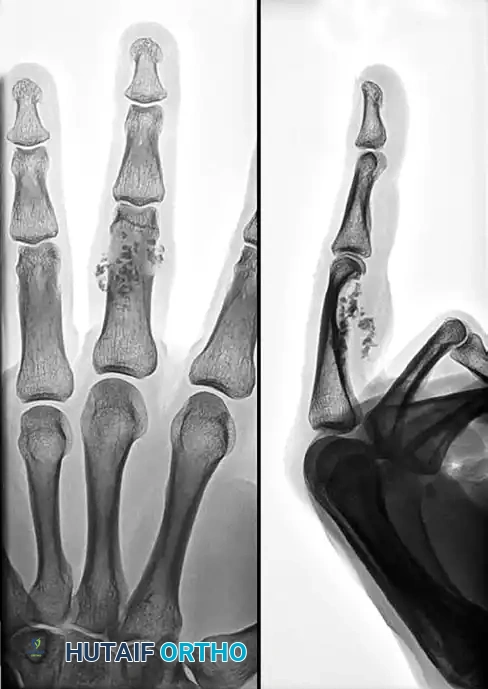
FIGURE 77-20 A: Anteroposterior and lateral radiographs of a 32-year-old man with insidious swelling of the left middle finger. Note the multiple spotty calcifications clustered around the proximal interphalangeal (PIP) joint.
Patients typically present in their third to fifth decades with insidious swelling, stiffness, and mechanical catching.
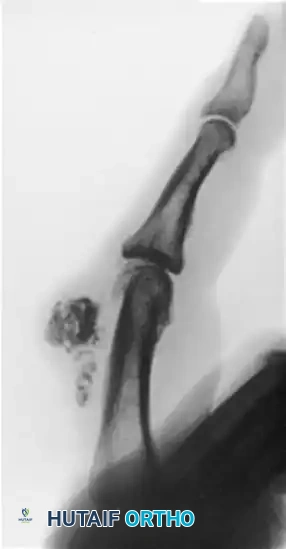
FIGURE 77-20 B: Gross pathology demonstrating multiple dense, white, well-encapsulated loose bodies removed from the proximal interphalangeal joint and flexor sheath.
Treatment consists of surgical exploration, removal of all loose bodies, and a thorough synovectomy to minimize the risk of local recurrence.
SURGICAL APPROACHES AND RESECTION TECHNIQUES
The surgical management of malignant hand tumors requires meticulous planning and adherence to strict oncologic principles.
1. Preoperative Planning and Biopsy
- Imaging: MRI with and without contrast is mandatory for soft tissue sarcomas to delineate the tumor's relationship to neurovascular bundles and fascial compartments. CT is preferred for evaluating cortical destruction in bone tumors. A metastatic workup (Chest CT) is required.
- Biopsy: The biopsy is the most critical step. It should be performed by the surgeon who will perform the definitive resection.
- Longitudinal incisions must be used.
- The biopsy tract must be placed so that it can be excised en bloc with the tumor during definitive surgery.
- Meticulous hemostasis is required to prevent post-biopsy hematoma, which can disseminate tumor cells into adjacent tissue planes.
2. Patient Positioning and Tourniquet Use
The patient is positioned supine with the operative arm extended on a radiolucent hand table.
Clinical Pearl: When operating on a suspected or confirmed malignancy, do not exsanguinate the limb using an Esmarch bandage. Mechanical compression can force tumor cells into the systemic circulation (tumor embolization). Instead, elevate the arm for 3 to 5 minutes to allow venous drainage before inflating the pneumatic tourniquet.
3. Surgical Exposure and Resection
The incision is designed to incorporate the previous biopsy tract with a 1 to 2 cm margin of normal skin, depending on the tumor type.
Intraoperative view demonstrating the meticulous dissection of a soft tissue mass on the dorsum of the digit. Note the preservation of surrounding viable tissue where oncologically permissible, while maintaining the integrity of the tumor pseudocapsule.
Principles of Resection:
* The Pseudocapsule: Sarcomas often form a "pseudocapsule" composed of compressed normal tissue and tumor cells. Never shell out a sarcoma. Dissection must occur through normal, unreactive tissue outside the reactive zone.
* Ray Resection: For bone sarcomas (e.g., chondrosarcoma) of the metacarpals or proximal phalanges, a ray resection is often the procedure of choice. This involves amputation of the digit and its corresponding metacarpal base.
* Biomechanics: Removal of a central ray (long or ring finger) requires transposition of the adjacent ray to close the cleft, preventing dropping of small objects and improving grip strength. Removal of border rays (index or small) requires oblique osteotomy of the metacarpal base to smooth the contour of the hand.
* Amputation: If the tumor involves multiple compartments, encases the superficial and deep palmar arches, or invades the major motor branches of the median/ulnar nerves such that resection would leave a useless hand, a below-elbow amputation is indicated.
4. Reconstruction and Closure
Following R0 resection (negative microscopic margins confirmed by frozen section if necessary), reconstruction of the soft tissue defect is performed.
* Primary closure is rarely possible after wide excision.
* Split-thickness or full-thickness skin grafts are used for superficial defects with a healthy vascular bed (muscle/fascia).
* Local rotational flaps, regional flaps (e.g., radial forearm flap), or free tissue transfer (e.g., anterolateral thigh flap) are required if bare bone, tendon without paratenon, or neurovascular structures are exposed.
POSTOPERATIVE PROTOCOLS AND REHABILITATION
Postoperative management is dictated by the extent of the resection and the need for adjuvant therapy.
1. Immobilization: The hand is immobilized in a bulky, non-compressive dressing with a volar orthosis in the intrinsic-plus position (wrist extended 20-30 degrees, MCP joints flexed 70-90 degrees, IP joints fully extended) to prevent collateral ligament contracture.
2. Wound Care: Flaps and grafts are monitored closely for viability. Adjuvant radiation, if planned, is typically delayed until surgical wounds are fully healed (usually 3 to 4 weeks postoperatively) to prevent wound dehiscence.
3. Rehabilitation: Early active and passive range of motion of uninvolved digits is initiated immediately. Once the reconstruction is stable, targeted occupational therapy is crucial to maximize grip strength, pinch mechanics, and sensory re-education.
4. Surveillance: Patients require rigorous long-term follow-up. This includes clinical examinations of the surgical site and regional lymph nodes, local MRI to monitor for recurrence, and serial Chest CTs to detect pulmonary metastasis. Surveillance is typically conducted every 3 months for the first 2 years, every 6 months up to 5 years, and annually thereafter.
You Might Also Like
