Malignant Hand Tumors: Comprehensive Surgical Management
Key Takeaway
Malignant tumors of the hand, though rare, demand precise surgical management to balance oncologic clearance with functional preservation. This guide details the evidence-based operative protocols for chondrosarcoma, epithelioid sarcoma, melanoma, and other hand malignancies. Key principles include meticulous preoperative staging, strict adherence to oncologic margins, and advanced reconstructive techniques to optimize patient survival and biomechanical outcomes following wide local excision or ray amputation.
INTRODUCTION TO MALIGNANT TUMORS OF THE HAND
Primary malignant tumors of the hand are exceedingly rare, accounting for a small fraction of all musculoskeletal neoplasms. However, their management presents a unique and formidable challenge to the orthopaedic oncologist and hand surgeon. The complex, densely packed anatomy of the hand—where critical neurovascular, tendinous, and osseous structures lie in close proximity—makes achieving wide oncologic margins difficult without significantly compromising biomechanical function.
The overarching philosophy in the surgical management of hand malignancies is dictated by the principle of "life over limb, and function over form." While limb-sparing wide local excision is the goal, ray amputations or more proximal amputations are frequently necessitated by the aggressive local behavior of these tumors. This comprehensive guide details the pathophysiology, clinical presentation, and step-by-step surgical management of the most critical malignant bone, soft tissue, and cutaneous tumors of the hand.
PRIMARY MALIGNANT BONE TUMORS
CHONDROSARCOMA
Chondrosarcomas are the most common primary malignant bone tumors of the hand. They typically present in the fifth to seventh decades of life and may arise de novo (primary) or secondary to malignant degeneration of a pre-existing benign cartilaginous lesion, such as an enchondroma or osteochondroma. Patients with multiple enchondromatosis (Ollier disease) or Maffucci syndrome are at a significantly elevated risk for secondary chondrosarcoma.
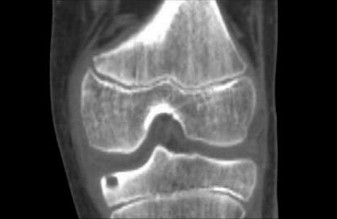
Clinical and Radiographic Presentation
Clinically, patients present with a slow-growing, firm, and often painful mass. Pain at rest or night pain in a previously asymptomatic cartilaginous lesion is a hallmark sign of malignant transformation. Radiographically, chondrosarcoma may mimic osteoarthritis or a benign enchondroma, presenting as a radiolucent lesion with stippled or "popcorn" calcifications. However, aggressive features such as deep endosteal scalloping (greater than two-thirds of the cortical thickness), cortical breakthrough, and soft tissue extension are highly indicative of malignancy.
Histopathology and Prognostic Factors
Histological variants include conventional (differentiated), spindle cell, acantholytic, and verrucous forms. In the hand, these tumors generally grow slowly, are superficially located, and are typically low-grade. They rarely metastasize, but local recurrence is a significant concern, with reported recurrence rates varying from 7% to 22%.
SURGICAL PITFALL: Differentiating a low-grade chondrosarcoma from a benign enchondroma in the small tubular bones of the hand is notoriously difficult, even for experienced musculoskeletal pathologists. Clinical correlation (presence of pain) and radiographic evidence of cortical destruction are paramount.
Poor prognostic risk factors include:
* Tumor size greater than 2 cm.
* Poor histological differentiation (High-grade).
* Immunosuppression.
* Increased depth of invasion.
* Perineural involvement.
* Local recurrence (The only prognostic factor directly dependent on the quality of the index surgery).
Surgical Management and Margins
The surgical management of chondrosarcoma is strictly operative, as these tumors are notoriously resistant to both chemotherapy and radiotherapy. The goal is complete en bloc resection with negative margins.
- Small, Low-Grade Lesions: Require a minimum tumor-free margin of 0.5 cm.
- Recurrent, Fixed, or High-Grade Lesions: Demand a wider margin of at least 3 cm.
Skin grafting or local flap coverage is commonly used after the excision of larger tumors. Amputation (ray or digit) is frequently required for fixed or recurrent lesions, especially those demonstrating penetration into deeper neurovascular or tendinous structures. Lymph node dissection is not routinely performed but is reserved for patients with fixed/recurrent tumors or those presenting with palpable regional lymphadenopathy.
OSTEOGENIC SARCOMA (OSTEOSARCOMA)
Osteogenic sarcoma of the hand is an exceptionally rare entity. Unlike its counterpart in the long bones of the appendicular skeleton, which predominantly affects adolescents, osteosarcoma of the hand often presents in older adults, sometimes secondary to Paget's disease or prior irradiation.
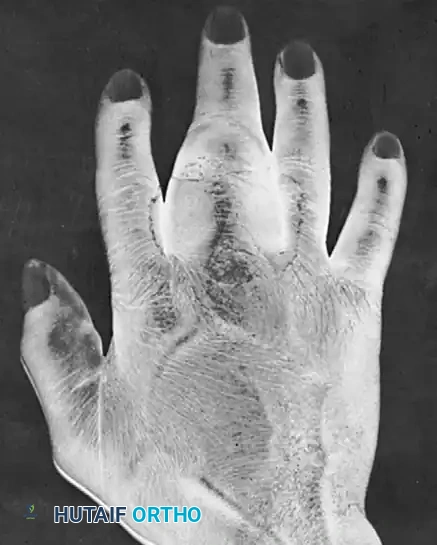
FIGURE: Radiographic appearance of an osteogenic sarcoma located in the proximal phalanx, demonstrating aggressive cortical destruction and a permeative lytic pattern.
Surgical Approach
Due to the high-grade nature of osteosarcoma and its propensity for early hematogenous micrometastasis, management requires a multidisciplinary approach involving neoadjuvant chemotherapy followed by wide surgical resection. In the hand, achieving a wide margin almost universally necessitates a ray amputation or, depending on the proximal extent, a wrist disarticulation or below-elbow amputation.
SOFT TISSUE SARCOMAS OF THE HAND
UNDIFFERENTIATED PLEOMORPHIC SARCOMA (FORMERLY MFH)
Malignant Fibrous Histiocytoma (MFH), now more accurately classified by the World Health Organization as Undifferentiated Pleomorphic Sarcoma (UPS), is a high-grade, aggressive soft tissue sarcoma. It typically presents as a rapidly enlarging, painless soft tissue mass.
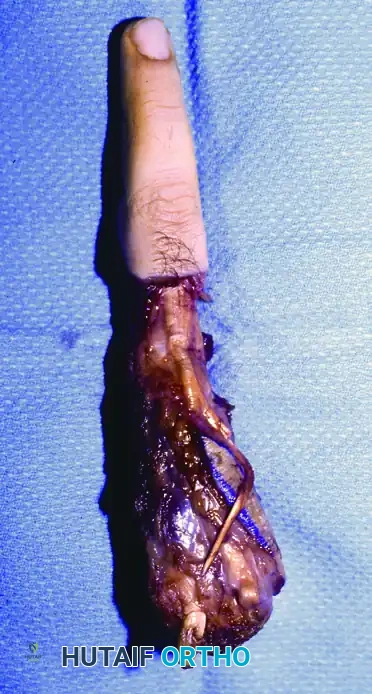
FIGURE: Radiographic appearance of a malignant fibrous histiocytoma (UPS) invading the middle metacarpal base, showing significant soft tissue shadowing and secondary osseous involvement.
Operative Technique: Ray Amputation
Given the aggressive local invasion of UPS, wide surgical excision is mandatory. When the tumor involves the metacarpal base or central hand compartments, a ray amputation is the oncologically sound procedure of choice.
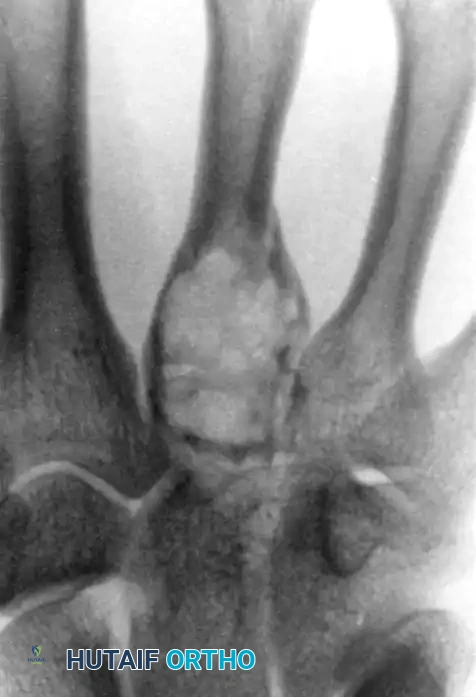
FIGURE: Clinical appearance following wide surgical excision and central ray amputation for malignant fibrous histiocytoma. Note the meticulous closure and preservation of the adjacent web spaces.
Step-by-Step Central Ray Amputation:
1. Incision: A dorsal racquet-shaped incision is designed, encompassing the biopsy tract and ensuring adequate skin margins around the tumor.
2. Neurovascular Dissection: The common digital arteries and nerves are identified proximally. The arteries are ligated, and the nerves are sharply transected under tension (traction neurectomy) to allow the stumps to retract deep into the intrinsic musculature, preventing painful neuroma formation.
3. Osteotomy: The metacarpal is exposed subperiosteally (only in benign cases; for malignancies, an extra-periosteal, wide margin is maintained). The osteotomy is performed at the metacarpal base, or a complete carpometacarpal (CMC) disarticulation is performed depending on the proximal extent of the tumor.
4. Biomechanics and Reconstruction: Removal of a central ray (middle or ring finger) disrupts the transverse metacarpal arch. To prevent a "scissoring" deformity and close the gap, the deep transverse metacarpal ligaments of the adjacent digits must be approximated. This is often achieved by transferring the interosseous muscles or using heavy non-absorbable sutures to tether the adjacent metacarpal heads.
5. Closure: The skin is closed without tension over a closed-suction drain.
EPITHELIOID SARCOMA
Epithelioid sarcoma is a highly deceptive and aggressive soft tissue malignancy. It is the most common soft tissue sarcoma of the hand and upper extremity in young adults.
CLINICAL PEARL: Epithelioid sarcomas are notoriously misdiagnosed initially due to their indolent, benign-appearing clinical course. They frequently present as unremarkable, firm, subcutaneous nodules and are often mistaken for benign conditions such as rheumatoid nodules, ganglion cysts, or simple inflammatory granulomas.
Pathophysiology and Growth Pattern
These tumors have a distinct predilection to grow longitudinally along fascial planes, tendon sheaths, and neurovascular bundles, forming multiple satellite nodules. As the disease progresses, the overlying skin frequently ulcerates, leading to necrosis of the underlying lesion.
Histologically, the appearance can be confusing. The tumor exhibits a basic granulomatous pattern with central necrosis surrounded by inflammatory cells. Under high magnification, the spindle cells take on a plump, epithelial-like appearance (hence "epithelioid").
Metastasis and Recurrence
Unlike most soft tissue sarcomas that metastasize primarily via the hematogenous route, epithelioid sarcoma has a high propensity for lymphatic spread. Metastasis to regional lymph nodes (epitrochlear and axillary) is common. Pulmonary metastasis usually follows multiple local recurrences.
The local recurrence rate is staggering, noted in up to 85% of patients, typically within 6 months following an inadequate initial excision.
Surgical Management
An inadequate marginal excision is invariably followed by recurrence. Therefore, aggressive initial surgical management is mandatory.
- Primary Wide Excision or Amputation: A primary wide excision with a minimum of 2-3 cm margins is required. In the digits, this almost always dictates a ray amputation or complete digit amputation.
- Margin Assessment: Even after a macroscopic wide excision, tumor cells may be present microscopically within the margins due to proximal tracking along tendon sheaths. Frozen sections are highly recommended intraoperatively.
- Proximal Amputation: A below-elbow amputation may be necessary after any recurrence in the hand proximal to the metacarpophalangeal (MCP) joints.
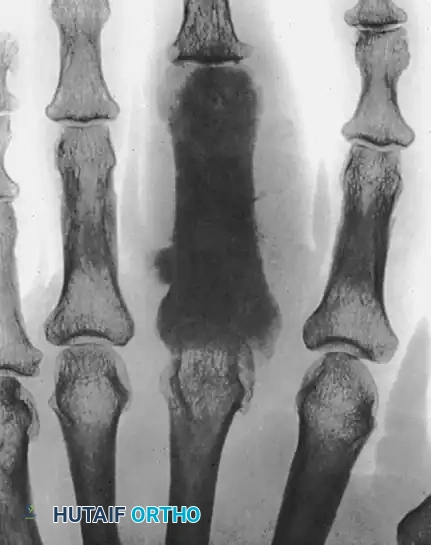
FIGURE: Gross pathological specimen of an amputated digit and partial ray, demonstrating the radical margins required for the eradication of an epithelioid sarcoma tracking along the flexor tendon sheath.
Adjuvant Therapy: Regional lymph node dissection in combination with the primary excision is strongly recommended, especially if sentinel lymph node biopsy is positive or nodes are clinically palpable. The role of adjuvant chemotherapy remains unclear and is generally reserved for advanced, metastatic disease, while adjuvant radiotherapy may be utilized to improve local control if margins are close.
MALIGNANT SKIN TUMORS OF THE HAND
The dorsum of the hand is chronically exposed to ultraviolet (UV) radiation, making it a prime location for cutaneous malignancies.
BASAL CELL CARCINOMA (BCC)
Basal cell carcinoma is the most common skin cancer overall, though it is less common on the hand than squamous cell carcinoma.
Clinical Presentation
A raised, pearly-bordered lesion with fine telangiectasias should make basal cell carcinoma a likely diagnosis, particularly in a middle-aged, fair-skinned male with a history of chronic sun exposure.
Surgical Excision
BCCs are far less aggressive than squamous cell carcinomas or melanomas. The tumor cells are typically confined to the raised areas of the nodular tumors, making the clinical boundaries fairly clear.
* Margins: These relatively benign, locally destructive tumors can be safely excised with a 0.5-cm free margin.
* Prognosis: With adequate excision, recurrence rates of approximately 1% have been reported. Reconstruction is typically achieved via full-thickness skin grafting or local rotational flaps.
SQUAMOUS CELL CARCINOMA (SCC)
While only briefly contrasted with BCC in the raw text, it is imperative to note that SCC is the most common primary malignancy of the hand. It often arises from pre-malignant actinic keratoses or in areas of chronic scarring (Marjolin's ulcer). SCC is more aggressive than BCC, with a higher rate of local tissue destruction and a greater potential for lymphatic metastasis. Wide local excision with 0.5 to 1.0 cm margins is standard, with vigilant assessment of the epitrochlear and axillary nodes.
MALIGNANT MELANOMA
Melanomas are highly aggressive neuroectodermal tumors. They are reported to occur in 1 in 70 white men, and the incidence continues to increase worldwide faster than any other cancer, with the death rate increasing by 2% per year.
Risk Factors and Presentation
Exposure to ultraviolet radiation is the primary environmental risk factor. Clinically, melanomas generally present as asymmetrical, pigmented lesions with irregular borders, color variation, and a diameter greater than 6 mm (the ABCDE criteria). Subungual melanomas (Hutchinson's sign) present a unique diagnostic challenge and often require partial or complete nail bed biopsy.
Prognosis and Breslow Thickness
Survival is directly related to the microscopic depth of tumor invasion, known as the Breslow thickness.
* Lesions ≤ 0.75 mm thick: 97% survival rate.
* Lesions ≥ 3.0 mm thick: 50% survival rate.
Surgical Management
The surgical management of melanoma is dictated by the Breslow depth:
1. In situ lesions: 0.5 cm margins.
2. Lesions < 1.0 mm thick: 1.0 cm wide local excision margins.
3. Lesions 1.0 - 2.0 mm thick: 1.0 to 2.0 cm margins.
4. Lesions > 2.0 mm thick: 2.0 cm margins.
SURGICAL PITFALL: In the digits, achieving a 2.0 cm radial margin is anatomically impossible without sacrificing the digit. Therefore, melanomas of the fingers or subungual melanomas typically require amputation at the distal interphalangeal (DIP) or proximal interphalangeal (PIP) joint to achieve adequate oncologic clearance.
Sentinel lymph node biopsy (SLNB) is indicated for melanomas with a Breslow thickness greater than 0.8 mm, or thinner lesions with ulceration or high mitotic rates, to stage the regional axillary and epitrochlear basins.
POSTOPERATIVE PROTOCOLS AND REHABILITATION
The postoperative management of hand malignancies requires a delicate balance between allowing reconstructive tissues (skin grafts, flaps) to heal and initiating early mobilization to prevent debilitating stiffness.
- Immobilization: The hand is typically immobilized in a bulky, non-compressive intrinsic-plus splint (wrist extended 20-30 degrees, MCP joints flexed 70-90 degrees, IP joints fully extended) for 10 to 14 days to protect vascularized flaps or skin grafts.
- Hand Therapy: Once the soft tissue envelope is stable, aggressive hand therapy is initiated. This includes active and passive range of motion exercises, edema control (coban wrapping, retrograde massage), and scar desensitization.
- Oncologic Surveillance: Patients require long-term follow-up. For sarcomas (Chondrosarcoma, UPS, Epithelioid Sarcoma), surveillance includes serial clinical examinations, local MRI to monitor for recurrence, and routine chest CT scans to detect pulmonary metastases.
By adhering to strict oncologic principles, utilizing meticulous surgical techniques, and engaging in multidisciplinary postoperative care, the orthopaedic surgeon can maximize both patient survival and the functional capacity of the hand.
You Might Also Like