Radial Shaft Fractures & DRUJ Instability: Epidemiology, Anatomy, and Management of Galeazzi Lesions
Key Takeaway
DRUJ instability in radial shaft fractures, often seen in Galeazzi lesions, is critical due to its impact on forearm function. It arises from disruption of the interosseous membrane, TFCC, or changes in radial length. Meticulous diagnosis and management are paramount to prevent chronic pain and functional impairment, ensuring optimal patient outcomes.
Introduction & Epidemiology
Radial shaft fractures, particularly those associated with distal radioulnar joint (DRUJ) instability, represent a distinct and challenging injury pattern in forearm trauma. While radial shaft fractures can occur in isolation, the presence of DRUJ disruption elevates the complexity and necessitates meticulous diagnosis and management to prevent long-term functional deficits. The classic presentation of a radial shaft fracture with DRUJ dislocation is known as a Galeazzi fracture-dislocation, although the term is often applied more broadly to any radial shaft fracture where DRUJ instability is a primary concern.
Epidemiologically, Galeazzi fracture-dislocations are less common than Monteggia fractures, constituting approximately 3-7% of all forearm fractures. They typically occur in young adults and are often the result of high-energy trauma, such as falls from height, motor vehicle accidents, or direct blows to the forearm. A common mechanism involves a fall onto an outstretched hand (FOOSH) with the forearm in pronation, imparting an axial load and rotational force that can lead to a fracture of the radial shaft and subsequent disruption of the DRUJ stabilizers. In the pediatric population, physeal injuries or plastic deformation of the ulna may occur in conjunction with radial shaft fractures, leading to similar DRUJ instability.
The critical aspect of managing these injuries lies in the recognition and appropriate treatment of the DRUJ instability. A failure to diagnose or adequately address DRUJ subluxation or dislocation at the time of radial shaft fixation is a well-documented cause of chronic pain, reduced forearm rotation, and functional impairment. Therefore, a comprehensive understanding of the pathomechanics, surgical anatomy, and nuanced management strategies is paramount for orthopedic surgeons.
Surgical Anatomy & Biomechanics
A thorough understanding of the intricate anatomy and biomechanics of the forearm, particularly the interaction between the radial shaft and the DRUJ, is fundamental to successful treatment.
Radial Shaft Anatomy
The radius is a long bone with a characteristic double curvature. The radial shaft is roughly triangular in cross-section proximally, becoming more oval distally. Key muscular attachments along the shaft include:
*
Pronator Teres:
Inserts on the lateral aspect of the mid-radial shaft.
*
Supinator:
Wraps around the proximal radius.
*
Brachioradialis:
Inserts on the distal lateral radius, acting as an elbow flexor and pronator/supinator depending on forearm position.
*
Flexor Pollicis Longus (FPL):
Originates from the anterior surface of the radius and interosseous membrane.
*
Abductor Pollicis Longus (APL) and Extensor Pollicis Brevis (EPB):
Originate from the posterior aspect of the radius and interosseous membrane.
*
Pronator Quadratus:
Spans from the distal ulna to the distal radius, acting as a primary pronator and DRUJ stabilizer.
Fractures of the radial shaft can compromise these muscular origins/insertions and, more importantly, disrupt the integrity of the interosseous membrane (IOM).
Distal Radioulnar Joint (DRUJ) Anatomy and Stabilizers
The DRUJ is a complex pivot joint allowing pronation and supination of the forearm. Its stability is a delicate balance between osseous congruity and intricate soft tissue restraints.
-
Articulating Surfaces:
- Ulnar Head: The convex articulating surface of the distal ulna.
- Sigmoid Notch of the Radius: The concave articular surface on the medial aspect of the distal radius.
-
Primary Stabilizers (Triangular Fibrocartilage Complex - TFCC):
The TFCC is the cornerstone of DRUJ stability. It is a complex of ligaments and cartilage situated between the distal ulna and the carpus. Key components include:
- Articular Disc (Triangular Fibrocartilage): Biconcave, load-bearing structure between the ulnar head and carpus.
- Dorsal and Volar Radioulnar Ligaments (DRUL and VRUL): These are the primary stabilizers of the DRUJ. They originate from the fovea and styloid process of the ulna and insert into the dorsal and volar rims of the sigmoid notch, respectively. Their tension varies with forearm rotation; the volar ligament is taut in supination, and the dorsal ligament is taut in pronation.
- Sheath of the Extensor Carpi Ulnaris (ECU): The ECU tendon and its subsheath contribute to dorsal DRUJ stability, particularly in supination.
- Meniscus Homologue and Ulnocarpal Ligaments: Contribute to overall wrist stability.
-
Secondary Stabilizers:
- Pronator Quadratus Muscle: Provides dynamic stabilization to the DRUJ.
- Interosseous Membrane (IOM): A dense fibrous sheet connecting the ulna and radius, crucial for longitudinal stability, load transfer, and preventing proximal migration of the radius. The central band of the IOM is the strongest component.
- Distal Radius and Ulna Morphology: The congruity of the sigmoid notch with the ulnar head is critical. Radial length, inclination, and rotation all affect DRUJ mechanics.
Biomechanics of DRUJ Instability in Radial Shaft Fractures
The pathomechanics of DRUJ instability associated with radial shaft fractures is multifactorial:
1.
Disruption of the Interosseous Membrane (IOM):
A fracture of the radial shaft often involves tearing of the IOM, especially its central band. This allows for proximal migration of the radius relative to the ulna, leading to a positive ulnar variance and incongruity at the DRUJ.
2.
Direct Injury to the TFCC/Radioulnar Ligaments:
The trauma causing the radial shaft fracture can also directly rupture the dorsal or volar radioulnar ligaments, leading to frank dislocation.
3.
Alteration of Radial Length, Rotation, or Angulation:
The primary mechanism by which radial shaft fractures cause DRUJ instability is through a change in the anatomical relationship between the distal radius and ulna.
*
Shortening of the Radius:
This is the most common cause. When the radial shaft shortens, the distal radius translates proximally relative to the ulna. This puts the TFCC under laxity, effectively disengaging the sigmoid notch from the ulnar head, or causing the ulnar head to sublux dorsally or volarly, depending on the force vector and forearm position at the time of injury.
*
Angulation:
Significant radial angulation (valgus or varus) can alter the load transmission across the DRUJ and also affect soft tissue tension.
*
Rotation:
Malrotation of the radial shaft can also affect the normal kinematics of pronation/supination at the DRUJ, leading to impingement or instability.
The integrity of the DRUJ relies on precise restoration of radial length, rotation, and alignment. Failure to achieve an anatomical reduction of the radial shaft fracture will inevitably lead to persistent or recurrent DRUJ instability, even if the primary soft tissue stabilizers are intact but lax due to altered bone geometry.
Indications & Contraindications
The decision-making process for managing radial shaft fractures with associated DRUJ instability hinges on a critical assessment of fracture characteristics, patient factors, and the presence and reducibility of DRUJ displacement.
Operative Indications
For most displaced radial shaft fractures with associated DRUJ instability (Galeazzi fracture-dislocation), open reduction and internal fixation (ORIF) of the radial shaft is the gold standard. The primary goal is anatomical restoration of radial length, rotation, and angulation, which is often sufficient to indirectly reduce and stabilize the DRUJ.
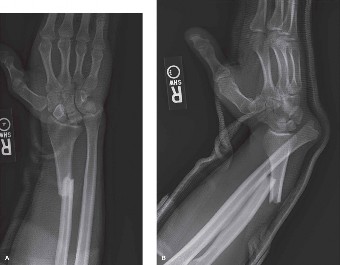
- Displaced Radial Shaft Fractures: Any significant displacement, angulation (>10-15 degrees), or shortening (>5mm) of the radial shaft in an adult is an indication for ORIF.
- Associated DRUJ Instability: When clinical examination or imaging confirms DRUJ subluxation or dislocation in conjunction with a radial shaft fracture. This is the hallmark of a Galeazzi injury.
- Inability to Achieve or Maintain Closed Reduction: Even if a closed reduction is attempted, an inability to maintain stable alignment of the radial shaft and/or DRUJ necessitates operative intervention.
- Open Fractures: All open radial shaft fractures require surgical debridement and stabilization.
- Neurovascular Compromise: Urgent surgical exploration and fixation are indicated in cases of acute neurovascular compromise.
- Polytrauma Patient: In the context of polytrauma, early stable fixation of long bone fractures like the radius is generally preferred to facilitate patient mobility and overall management.
Non-Operative Indications
Non-operative management for true Galeazzi fracture-dislocations is exceedingly rare in adults due to the high likelihood of malunion, persistent DRUJ instability, and poor functional outcomes.
- Non-Displaced, Stable Radial Shaft Fractures with Stable DRUJ: This is an uncommon scenario, typically seen in isolated radial shaft fractures without DRUJ involvement. If non-operative, strict immobilization and serial radiographs are mandatory.
- Specific Pediatric Cases: In skeletally immature patients, plastic deformation of the ulna or radial physeal fractures may be amenable to closed reduction and casting due to greater remodeling potential. However, even in children, irreducible or unstable DRUJ dislocation often warrants operative intervention.
Contraindications
While generally indicated for displaced injuries, certain patient factors or local conditions may contraindicate immediate or elective surgery.
-
Absolute Contraindications:
- Severe Soft Tissue Compromise: Extensive skin loss, severe degloving injuries, or critically compromised soft tissue envelope that would preclude safe surgical wound closure or increase infection risk.
- Active Infection: Cellulitis or osteomyelitis in the surgical field.
- Medically Unstable Patient: Severe, uncompensated systemic comorbidities (e.g., acute cardiac event, uncontrolled sepsis) where the risks of anesthesia and surgery outweigh the benefits of immediate fixation.
-
Relative Contraindications:
- Significant Patient Comorbidities: While not absolute, severe osteoporosis, poorly controlled diabetes, or chronic immunosuppression increase surgical risks and may influence fixation strategy or timing.
- Poor Bone Quality (Osteoporosis): Severe osteoporosis may make stable screw purchase difficult, potentially necessitating different fixation constructs or adjunctive bone cement.
Table: Operative vs. Non-Operative Indications
| Feature | Operative Management | Non-Operative Management |
|---|---|---|
| Radial Shaft Fracture | Displaced (>10-15° angulation, >5mm shortening) | Non-displaced (rare for true Galeazzi) |
| Open fractures | ||
| DRUJ Instability | Always when associated with displaced radial shaft | Not applicable for true Galeazzi; implies stable DRUJ |
| Inability to achieve/maintain closed reduction | ||
| Patient Age | Adults (standard of care) | Select pediatric cases (good remodeling potential) |
| Soft Tissue Status | Stable, viable soft tissue | Contraindicated in severe compromise |
| Neurovascular Status | Compromise requiring urgent exploration | Intact, stable |
| Associated Injuries | Polytrauma necessitating early stabilization | |
| Functional Goals | Restore full forearm rotation & stability | Limited to non-displaced, stable patterns if applicable |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is critical for optimizing outcomes in radial shaft fractures with DRUJ instability.
Patient Assessment
A thorough clinical assessment begins with a detailed history of the injury mechanism. The physical examination must include:
*
Neurovascular Status:
Assess radial, ulnar, and median nerve function (motor and sensory) and evaluate peripheral pulses, capillary refill, and sensation to rule out acute neurovascular compromise.
*
Soft Tissue Integrity:
Inspect for open wounds, abrasions, contusions, and signs of swelling or compartment syndrome.
*
Deformity and Pain:
Note any obvious angulation, shortening, or rotational deformity of the forearm. Localize tenderness over the radial shaft and, crucially, over the DRUJ.
*
DRUJ Assessment:
This is paramount.
*
Visual Inspection:
Look for any prominence of the ulnar head dorsally or volarly, suggesting dislocation.
*
Palpation:
Tenderness over the DRUJ is a strong indicator of ligamentous injury.
*
Ballottement Test:
With the wrist in neutral, attempt to ballot the ulnar head volarly and dorsally while stabilizing the radius. Excessive translation compared to the contralateral side suggests instability.
*
Grind Test (or Shear Test):
Apply axial compression and rotate the forearm. Pain, clicking, or crepitus can indicate TFCC injury or instability.
*
Forearm Rotation:
Assess pronation and supination actively and passively, noting any limitations or pain. Comparison to the uninjured side is essential.
Imaging
A comprehensive imaging series is indispensable.
*
Standard Radiographs:
*
Anteroposterior (AP) and Lateral views of the forearm:
Must include the elbow and wrist joints to fully assess the radial shaft fracture, as well as the proximal radioulnar joint (PRUJ) and DRUJ.
*
AP and Lateral views of the elbow:
To rule out associated elbow injuries.
*
AP and Lateral views of the wrist:
Crucial for detailed assessment of the DRUJ.
*
Oblique Views:
Can sometimes highlight subtle displacements.
*
Contralateral Side Films:
Obtain AP and lateral views of the uninjured forearm, wrist, and elbow. These serve as templates for assessing normal radial length, radial bowing, and DRUJ congruity, especially in cases of suspected malunion or for pre-operative templating.
*
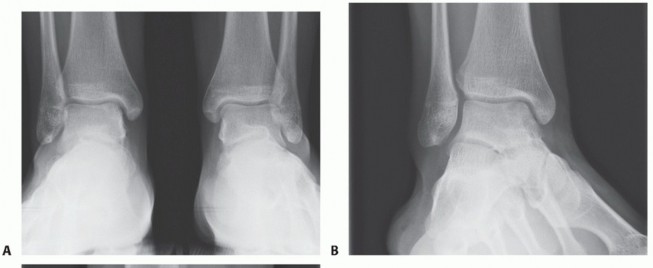
Critical Radiographic Signs of DRUJ Instability:
*
Radial Shortening:
Comparison to the contralateral side.
*
Widening of the DRUJ Space:
On AP views.
*
Loss of Overlap between Radius and Ulna:
On lateral views (often the ulnar head appears dorsal or volar to the radius).
*
Dorsal or Volar Dislocation of the Ulnar Head:
On true lateral views, the central axis of the ulna should align with the sigmoid notch of the radius.
*
Computed Tomography (CT) Scan:
* Highly recommended, especially for subtle or complex DRUJ injuries.
*
Axial cuts:
Provide superior detail of the DRUJ congruity, articular step-off, and osseous lesions.
*
3D Reconstructions:
Useful for visualizing fracture patterns and displacement in complex cases.
*
Dynamic CT scans (pronation/supination):
Can demonstrate instability not evident on static images.
*
Magnetic Resonance Imaging (MRI):
* Primarily utilized if TFCC avulsion, rupture of radioulnar ligaments, or other soft tissue pathology (e.g., interosseous membrane tear) is strongly suspected and not clearly characterized by CT, particularly in chronic instability or when primary repair is considered for the TFCC.
Templating and Implant Selection
- Based on radiographs (especially contralateral films), determine the appropriate plate length, contour, and screw sizes.
- Low-profile, pre-contoured locking plates are generally preferred for radial shaft fractures. Consider plate length to ensure at least 6 cortices engaged proximally and distally to the fracture.
- Plan the surgical approach (usually volar Henry).
Patient Positioning
- Supine Position: The patient is placed supine on the operating table.
- Arm on Hand Table: The injured arm is placed on a sterile hand table, allowing full access to the forearm.
- Tourniquet: A pneumatic tourniquet is applied high on the ipsilateral upper arm to ensure a bloodless field, which is essential for clear visualization of anatomical structures and neurovascular bundles.
- C-arm Access: Ensure the operating table and patient position allow for unobstructed intra-operative fluoroscopic imaging of the entire forearm, elbow, and wrist in both AP and lateral planes.
Detailed Surgical Approach / Technique
The primary goal of surgical management for radial shaft fractures with DRUJ instability is the anatomical restoration of radial length, rotation, and angulation, which in most cases, will indirectly reduce and stabilize the DRUJ. The volar Henry approach is the most common and versatile for the radial shaft.
Anesthesia and Preparation
- Anesthesia: General anesthesia or regional block (e.g., interscalene block combined with general) is typically employed.
- Tourniquet: Inflated to appropriate pressure (e.g., 250-300 mmHg) after exsanguination with an Esmarch bandage.
- Preparation and Draping: The arm is prepped and draped from the shoulder to the fingertips in a sterile fashion, allowing free manipulation of the limb and access for intraoperative fluoroscopy.
Incision (Volar Henry Approach)
The volar Henry approach provides excellent exposure to the volar aspect of the radial shaft while minimizing disruption to critical neurovascular structures.
1.
Skin Incision:
A longitudinal or slightly S-shaped incision is made on the volar aspect of the forearm, centered over the palpable radial shaft. The length of the incision should adequately expose the fracture site and allow for plate application. It typically extends from distal to the elbow crease to within 5-7 cm of the wrist crease.
2.
Subcutaneous Dissection:
The subcutaneous tissues are incised, and meticulous hemostasis is achieved. The fascia of the forearm is identified. Superficial sensory branches of the radial nerve should be protected if encountering the distal aspect of the forearm and radial wrist.
3.
Identification of Internervous Plane:
* The crucial internervous plane for the volar Henry approach lies between the
brachioradialis muscle
(innervated by the radial nerve) laterally and the
flexor-pronator muscle mass
medially (primarily innervated by the median nerve).
*
Proximally:
The plane is between the brachioradialis laterally and the pronator teres/flexor carpi radialis (FCR) medially.
*
Distally:
The plane shifts slightly to be between the brachioradialis laterally and the FCR/flexor pollicis longus (FPL) medially.
4.
Muscle Retraction:
* The brachioradialis muscle is retracted laterally.
* The flexor-pronator mass (containing the FCR, FPL, pronator teres, median nerve, and ulnar artery) is carefully retracted medially. The median nerve and radial artery are identified and protected. The radial artery, with its concomitant veins, lies deep to the brachioradialis and lateral to the FPL. It often needs to be gently retracted, typically medially, along with the FPL.
5.
Deep Structures:
* The
pronator quadratus muscle
is encountered distally, covering the distal radius and DRUJ capsule. It must be carefully elevated subperiosteally from its radial insertion if the fracture extends to this region or if the DRUJ needs direct assessment.
* The periosteum of the radial shaft is incised longitudinally, and the soft tissues are elevated subperiosteally to expose the fracture site. Avoid extensive periosteal stripping, which can compromise bone vascularity.
Fracture Reduction
- Indirect Reduction: Initial attempts at reduction should involve gentle traction on the hand, often combined with pronation or supination depending on the fracture pattern. This helps restore gross length.
-
Direct Reduction:
- The fracture fragments are then directly visualized.
- Specialized reduction clamps (e.g., Verbrugge clamps, small pointed reduction forceps) are used to manipulate the fragments.
- Crucially, radial length must be restored. This often involves disimpacting fragments and applying longitudinal traction.
- Rotational alignment is vital. Clinical assessment of the bicondylar axis of the distal humerus and the distal radius (Styloid processes, Lister's tubercle) and comparing it to the contralateral side can help. Intra-operatively, the relative position of the biceps tuberosity to the radial styloid is a useful guide.
- Angulation must also be corrected to achieve anatomical alignment.
- Temporary Fixation: K-wires can be used to temporarily hold the reduction while plate application is prepared.
Fixation of the Radial Shaft
- Plate Application: A pre-contoured locking plate (e.g., LCP - Locking Compression Plate) is typically chosen. The plate should be placed on the tension side of the bone (usually the volar aspect of the radius) and should be long enough to provide adequate purchase in both proximal and distal fragments, ideally spanning at least 6 cortices on each side of the fracture.
-
Screw Insertion:
- Lag screws through the plate can be used for interfragmentary compression in oblique or spiral fractures.
- Locking screws are then inserted into the pre-drilled holes. These screws provide angular stability and are particularly advantageous in comminuted fractures or osteoporotic bone.
- Ensure all screws are bicortical where feasible, except near joint surfaces or if a specific monocortical screw is indicated.
- Confirm stability of fixation with appropriate manual stress tests.
DRUJ Assessment & Management
Once the radial shaft fracture is anatomically reduced and stably fixed, the DRUJ must be thoroughly reassessed. This is a critical step.
1.
Clinical Assessment of DRUJ:
* The tourniquet can be deflated to re-evaluate tissue perfusion.
* Perform a "stress test" on the DRUJ by applying axial compression and gentle pronation/supination.
*
Ballottement:
Stabilize the radius and ballot the ulnar head dorsally and volarly. Compare to the uninjured side.
*
Direct Visualization (if exposure allows):
If the fracture extended very distally or the DRUJ capsule was approached, direct visualization of the DRUJ can confirm reduction.
2.
Fluoroscopic Assessment:
Obtain AP and lateral fluoroscopic views of the wrist in neutral, pronation, and supination. Look for:
*
DRUJ Congruity:
The ulnar head should be concentrically reduced within the sigmoid notch.
*
Radial Length:
The radial styloid should be approximately 1-2 mm distal to the ulnar head (negative ulnar variance, or neutral variance is acceptable). Positive ulnar variance suggests persistent radial shortening.
3.
Management of Persistent DRUJ Instability:
If, after anatomical radial shaft fixation, the DRUJ remains unstable, further intervention is required.
*
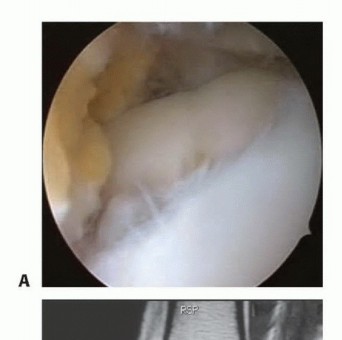
TFCC Repair:
If a significant avulsion of the TFCC (e.g., off the fovea or styloid of the ulna) is identified, a direct repair (arthroscopic or open) should be considered. This is often performed through a separate ulnar-sided incision.
*
Temporary DRUJ Pinning:
This is a common and effective technique for allowing soft tissues (TFCC, interosseous membrane) to heal and regain tension.
* The forearm is positioned in neutral rotation or slight supination (approximately 20-30 degrees supination), which is the position of maximal DRUJ stability.
* A 1.5mm or 2.0mm smooth K-wire is drilled from the dorsal aspect of the ulna (just proximal to the ulnar head) across the DRUJ into the radius.
* A second K-wire can be placed if added stability is desired.
* Ensure the pins are placed parallel to each other and avoid the articular surfaces of the distal radius. The goal is transfixation, not compression. The K-wires are left protruding from the skin and bent to prevent migration.
*
Pronator Quadratus Repair:
If the pronator quadratus was elevated, ensure it is reapproximated to the radius to provide dynamic stability.

*A graphic demonstrating the typical appearance of a Galeazzi fracture-dislocation on plain radiographs, illustrating the displaced radial shaft fracture and dorsal dislocation of the ulnar head relative to the radius on the lateral view.*
Wound Closure
- Hemostasis: Ensure meticulous hemostasis.
- Muscle and Fascial Closure: The pronator quadratus is reapproximated if elevated. The fascia overlying the flexor-pronator mass can be loosely closed to prevent muscle herniation. Avoid tight closure that could lead to compartment syndrome.
- Subcutaneous and Skin Closure: The subcutaneous layer is closed, followed by skin closure using sutures or staples.
- Dressing and Immobilization: A sterile dressing is applied. The forearm is typically immobilized in a sugar tong splint or a long arm splint, usually in a neutral or slightly supinated position, especially if DRUJ pinning was performed.
Complications & Management
Despite meticulous surgical technique, complications can arise following radial shaft fracture fixation with DRUJ instability. Early recognition and appropriate management are crucial for salvage and optimizing patient outcomes.
Table: Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence (Approx.) | Salvage Strategies |
|---|---|---|
| Nonunion/Malunion | 2-10% |
Nonunion:
Revision ORIF with plate exchange, bone grafting (autograft/allograft), intramedullary nailing. Address infection if present.
Malunion: Corrective osteotomy (opening/closing wedge), often with new plate fixation, to restore length, angulation, and rotation. |
| Persistent DRUJ Instability | 5-15% (if unrecognized/untreated) |
Acute (post-ORIF):
If radial length restored but DRUJ unstable, consider TFCC repair or DRUJ transfixation with K-wires for 4-6 weeks.
Chronic: Ulnar shortening osteotomy for positive ulnar variance, TFCC reconstruction (e.g., arthroscopic repair, capsular reefing), tenodesis procedures (e.g., ECU tendon strip), Darrach procedure (ulnar head resection - salvage). |
| Nerve Injury | 1-5% |
Radial Nerve (sensory branches):
Observation for neuropraxia. Symptomatic neuromas may require excision or nerve grafting.
Median Nerve: Observation. If direct injury suspected during surgery or profound deficit, urgent exploration and repair. Posterior Interosseous Nerve (PIN): Rare with volar approach. Observation. If clear transection, surgical repair. |
| Vascular Injury (Radial Artery) | <1% | Intraoperative repair (primary anastomosis or vein graft) if transected. Ligation if smaller branch. Observation if vasospasm. |
| Infection | 1-3% |
Superficial:
Oral antibiotics, local wound care.
Deep: Surgical debridement, intravenous antibiotics (culture-specific), irrigation, possible hardware removal (after fracture healing), or staged revision. |
| Compartment Syndrome | <1% | Urgent fasciotomy of all forearm compartments. Leave wound open and perform delayed primary closure or skin grafting. |
| Radio-Ulnar Synostosis | <5% (increased risk with open fractures, severe soft tissue injury, dual plating) | Prevention (minimal periosteal stripping, single plate). Established: Excision of heterotopic bone, interposition material (fat, muscle, silicone), post-operative radiation therapy, or NSAIDs. Often challenging to restore full rotation. |
| Hardware Failure/Irritation | 2-10% |
Failure:
Revision ORIF, plate exchange, bone grafting.
Irritation: Hardware removal after fracture healing is complete. |
| Complex Regional Pain Syndrome (CRPS) | 2-5% | Early recognition and multidisciplinary management: physical therapy (desensitization), pain management (nerve blocks, medications), psychological support. Aggressive, early rehabilitation is key. |
Detailed Management Strategies
-
Nonunion/Malunion:
- Nonunion: Characterized by persistent pain, instability, and radiographic evidence of failed healing after 6-9 months. Management typically involves revision open reduction and internal fixation. This often requires removing the previous hardware, decorticating the nonunion site, applying fresh bone graft (autogenous iliac crest bone graft is preferred), and re-plating with a longer, stronger plate (e.g., locking compression plate).
- Malunion: Occurs when the fracture heals in an unacceptable alignment (shortening, angulation, rotation). Symptoms include restricted forearm rotation, DRUJ instability, and wrist pain. Corrective osteotomy is the treatment. This involves surgically re-fracturing the malunited bone, correcting the deformity (often using intraoperative C-arm and comparing to contralateral side), and re-fixing it with a new plate. Pre-operative CT planning for osteotomy cuts can be very helpful.
-
Persistent DRUJ Instability: This is a key complication of Galeazzi fractures.
- Acute (Post-ORIF): If after radial shaft fixation, the DRUJ remains unstable on intraoperative stress testing and fluoroscopy, the first step is to ensure adequate length, rotation, and angulation of the radius has been achieved. If these are correct, then direct soft tissue stabilization (TFCC repair, if a tear amenable to repair is present) or temporary transfixation with K-wires is indicated. The forearm should be placed in 20-30 degrees of supination, as this is the position of maximal DRUJ stability. K-wires are typically removed at 4-6 weeks.
-
Chronic Instability:
Presents as chronic pain, clicking, and limitation of forearm rotation. Evaluation should include CT or MRI to assess DRUJ congruity, ulnar variance, and TFCC integrity.
- If positive ulnar variance is present (due to radial shortening), an ulnar shortening osteotomy can re-tension the TFCC.
- If significant TFCC tears are present, arthroscopic or open TFCC repair/reconstruction may be indicated.
- For chronic, irreducible instability or severe degenerative changes, salvage procedures like the Darrach procedure (resection of the ulnar head), hemiresection arthroplasty, or the Sauvé-Kapandji procedure (DRUJ arthrodesis with proximal ulnar pseudarthrosis) may be considered, but these sacrifice DRUJ motion.
-
Nerve Injury:
- Superficial Radial Nerve: Sensory nerve, most commonly injured by direct trauma or iatrogenically during distal skin incision. Usually neuropraxia, managed conservatively. Symptomatic neuromas may require excision.
- Median Nerve: Less commonly injured but more critical. Direct injury during retraction of the flexor-pronator mass. If deficit is present and suspicion of transection is high, urgent exploration and repair are warranted.
- Posterior Interosseous Nerve (PIN): Motor branch of the radial nerve. Risk is low with a volar approach. More at risk with proximal shaft fractures or dorsal approaches.
-
Radio-Ulnar Synostosis: Formation of heterotopic bone between the radius and ulna, leading to severe restriction or complete loss of forearm rotation.
- Risk factors include high-energy trauma, open fractures, severe soft tissue damage, delayed closure, and dual plating.
- Prevention involves meticulous surgical technique (minimal periosteal stripping, avoiding bone dust between bones).
- Treatment is surgical excision of the synostosis, often combined with interposition material (e.g., fat graft, muscle flap, synthetic membranes) and post-operative radiation therapy or NSAIDs to prevent recurrence. Outcomes for restoring full motion can be guarded.
-
Compartment Syndrome: Rare but limb-threatening. Suspect if severe pain out of proportion, pain with passive stretch, paresthesia, pallor, or tense compartment on palpation. Requires urgent four-compartment fasciotomy.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is as critical as the surgical intervention itself to restore function and prevent stiffness or recurrent instability. Protocols must be tailored to the individual patient, the stability of the fracture fixation, and the management of the DRUJ.
Immediate Post-Operative Period (Day 0 - Week 2)
- Immobilization: The forearm is typically immobilized in a sugar tong splint or a long arm splint. If the DRUJ was transfixed with K-wires, the forearm is held in 20-30 degrees of supination (position of DRUJ stability).
- Pain Management: Aggressive pain control with multimodal analgesia.
- Edema Control: Elevation of the extremity (above heart level) and gentle active range of motion (AROM) of the shoulder and digits (fingers and thumb).
- Wound Care: Routine wound checks and dressing changes.
- Patient Education: Instruct patient on warning signs of infection, compartment syndrome, and nerve compression.
Early Mobilization Phase (Week 2 - Week 6)
- K-wire Removal (if applicable): If DRUJ transfixation K-wires were used, they are typically removed at 4-6 weeks post-operatively, after radiographic evidence of early healing of the radial shaft fracture.
-
Initiate Gentle Range of Motion:
- Forearm: After K-wire removal, or if no K-wires were used and DRUJ was stable, controlled active-assisted ROM (AAROM) and then AROM for pronation and supination can begin. Initially, limit end-range rotation, especially forced pronation/supination, to protect healing soft tissues.
- Wrist: Gentle AROM for flexion, extension, radial, and ulnar deviation.
- Elbow: Continue AROM for flexion and extension.
-
Exercises:
- Gravity-assisted exercises for forearm rotation.
- Gentle active wrist stretches.
- Continued finger and shoulder mobility.
- Avoidances: Avoid lifting heavy objects, pushing/pulling, and excessive torque through the forearm.
Progressive Strengthening & Full Range of Motion (Week 6 - Week 12)
- Increase ROM: Progress towards full, pain-free active and passive range of motion for the forearm, wrist, and elbow. Modalities like heat, ultrasound, or gentle joint mobilizations may be used by the therapist.
-
Strength Training:
- Begin with light isometric exercises for the forearm flexors, extensors, pronators, and supinators.
- Gradually progress to light resistance exercises (e.g., putty, light weights, resistance bands).
- Focus on functional gripping and pinch strength.
- Scar Management: Initiate scar massage and desensitization as appropriate.
- Activity Modification: Continue to educate the patient on activity modification and avoidance of high-impact or twisting activities.
Return to Activity Phase (Month 3+)
- Advanced Strengthening: Progress to more demanding resistance exercises.
- Sport/Work Specific Training: Tailor rehabilitation to the patient's occupational or recreational demands. This may involve plyometric exercises, sport-specific drills, or simulations of work tasks.
- Endurance Training: Improve muscular endurance for sustained activities.
- Proprioception and Coordination: Exercises to improve fine motor control and joint position sense.
- Hardware Removal (Optional): If hardware irritation occurs or if patient preference, hardware removal can be considered 12-18 months post-surgery, once the fracture is fully consolidated. This is an elective procedure.
- Long-Term Monitoring: Patients should be counseled on potential long-term issues like arthritis, particularly at the DRUJ, and the importance of continued forearm and wrist care.
Close collaboration between the surgeon, physical therapist, and patient is crucial for achieving optimal functional outcomes following surgical management of radial shaft fractures with DRUJ instability. The progression should always be guided by pain, swelling, and radiographic healing.
Summary of Key Literature / Guidelines
The understanding and management of radial shaft fractures with DRUJ instability have evolved significantly since Antonio Galeazzi first described the injury in 1934. The overarching consensus in modern orthopedic literature emphasizes the critical importance of anatomical reduction and stable internal fixation of the radial shaft fracture as the cornerstone of treatment.
Early Recognition and Management:
The literature consistently highlights that a missed or inadequately treated DRUJ instability leads to poor functional outcomes, chronic pain, restricted forearm rotation, and eventual degenerative changes. Early studies, such as those by Hughston (1957) and Reckling (1982), underscored the high failure rate of non-operative management for adult Galeazzi fractures. They demonstrated that non-operative approaches almost invariably resulted in unacceptable malunion of the radius and persistent DRUJ subluxation. This has led to the current standard of care advocating for surgical intervention for nearly all displaced adult Galeazzi fracture-dislocations.
Role of Radial Shaft Fixation:
Current guidelines, supported by numerous clinical studies, emphasize that the primary goal of surgery is the anatomical restoration of radial length, angulation, and rotation. The restoration of radial anatomy often indirectly reduces and stabilizes the DRUJ by re-tensioning the interosseous membrane and the intrinsic DRUJ ligaments (dorsal and volar radioulnar ligaments).
*
Plate Fixation:
Low-profile, pre-contoured locking plates are the preferred method of fixation for radial shaft fractures. They offer excellent stability, particularly in comminuted fractures or osteoporotic bone, allowing for early mobilization. Studies by authors like Ring and Jupiter have extensively reviewed plating techniques and biomechanics for forearm fractures, reinforcing the benefits of stable internal fixation.
Management of DRUJ Instability Post-Radial Fixation:
A key debate in the literature surrounds the necessity of direct DRUJ intervention after successful radial shaft fixation.
*
Indirect Reduction:
The prevailing view is that if anatomical reduction of the radius is achieved, the DRUJ will typically reduce spontaneously and become stable. Intraoperative assessment of DRUJ stability via stress testing (ballottement, rotation through full arc) and fluoroscopy is mandatory.
*
Direct DRUJ Stabilization:
If the DRUJ remains unstable after satisfactory radial fixation, the literature supports additional intervention.
*
K-wire Transfixation:
Temporary transfixation of the DRUJ with smooth K-wires in slight supination (20-30 degrees) for 4-6 weeks is a widely accepted technique to allow soft tissue healing. This is particularly useful when ligamentous disruption is suspected to be significant, or if the DRUJ instability is marked. Multiple studies have shown good results with this approach.
*
TFCC Repair:
If a significant, repairable TFCC avulsion (e.g., Type 1B or 1D ulnar-sided tear according to Palmer classification) is identified, either openly or arthroscopically, direct repair may be considered, particularly in younger, active patients. This decision is often individualized.
Advanced Imaging:
The role of CT and MRI in pre-operative planning and assessing chronic instability is well-established. CT scans are superior for evaluating osseous congruity and subtle subluxations of the DRUJ, while MRI is invaluable for delineating soft tissue injuries, especially TFCC tears and interosseous membrane disruption. Dynamic CT scans or fluoroscopic stress views can also reveal occult instability.
Complications and Salvage:
The literature provides extensive guidance on managing complications:
*
Nonunion/Malunion:
Requires revision surgery with meticulous planning and often bone grafting.
*
Chronic DRUJ Instability:
Is a common sequela of missed or inadequately treated injuries. Management ranges from ulnar shortening osteotomies (for positive ulnar variance) to TFCC reconstruction, and finally, salvage procedures like Darrach or Sauvé-Kapandji for severe, symptomatic arthritis or intractable instability.
*
Radio-Ulnar Synostosis:
Preventative measures during surgery are paramount. Surgical excision with interposition material and adjuvant radiation or NSAIDs are used for established cases, though outcomes can be limited.
In summary, the consensus from key orthopedic literature and clinical guidelines is unambiguous: radial shaft fractures with DRUJ instability necessitate anatomical open reduction and stable internal fixation of the radius. This, combined with a diligent intraoperative assessment of the DRUJ and appropriate secondary stabilization if required, forms the foundation for achieving optimal functional recovery and preventing debilitating long-term complications.
Clinical & Radiographic Imaging

You Might Also Like