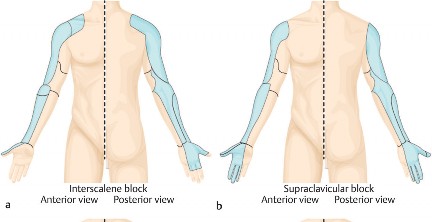
Perioperative & Orthopaedic Medicine: Preventing Dangerous Blood Clots
30 مارس 2026
22 min read
60 Views
Key Takeaway
Here are the crucial details you must know about Perioperative & Orthopaedic Medicine: Preventing Dangerous Blood Clots. Thromboembolic disease, a common perioperative and orthopaedic complication, involves improper blood clotting (thrombosis) that can migrate (embolism), potentially leading to deep venous thrombosis (DVT) or pulmonary embolism (PE). Key factors contributing include endothelial damage from surgery, blood stasis due to immobility, and hypercoagulability. Age and prior DVT are significant risk factors.
-
-
- Thromboprophylaxis 2. #### Thromboembolic disease
-
- Common orthopaedic complication
- Thrombosis: clotting at improper site
- Embolism: clot that migrates
- Most clinically silent but can be fatal
- Complications of thromboembolic disease:
- Postthrombotic syndrome: chronic venous insufficiency
- Venous hypertension (HTN)
- Chronic skin issue with swelling, pain
- Pigmentation, induration, ulceration
- Recurrent deep venous thrombosis (DVT): risk four to eight times higher after first DVT
- Pulmonary embolism (PE)
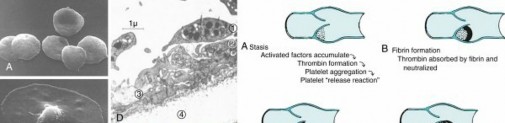
- Pathophysiology (Virchow triad) ( Fig. 1.51)
- Endothelial damage: trauma or surgery
- Exposes collagen—triggers platelets
- Platelets—three roles:
- Adhesion and activation
- Secretion of prothrombotic mediators
- Aggregation of many platelets
- Stasis: allows bonds of clotting proteins and cells
- Immobility: pain, stroke, paralysis
- Blood viscosity: polycythemia, cancer, estrogen
- Decreased inflow: tourniquet, vascular disease
- Decreased outflow: venous scarring, CHF
- Hypercoagulability
- Clotting cascade’s final product is thrombin
- Converts soluble fibrinogen to insoluble fibrin
- Risk factors and epidemiology
- Reported risks of thromboembolic disease vary by:
- Definitions: asymptomatic versus symptomatic
- Location
- Distal: those below popliteal space have very low PE risk
- Proximal: those above popliteal space have higher PE risk
- Patient-specific risks factors ( Fig. 1.52)
- Prior thromboembolic disease a strong risk factor
- Risk increases exponentially with age (>40 years) ( Fig. 1.53)
- Genetic factors—thrombophilias
- Decreased anticlotting factors
- Antithrombin III, protein C, protein S deficiencies
-
Increased clotting factors or factor activity
-
Factor V Leiden
-
Mutated factor V not inactivated as effectively by activated protein C, so clotting process remains active for longer than normal
- Elevated factor VIII
- Hyperhomocysteinemia
-
Prothrombin G20210A (factor II mutation)


FIG. 1.51 Left, Electromicrograph panel (A through E). (A) Scanning electron micrograph (SEM) of free platelets. (B) SEM of platelet adhesion. (C) SEM of platelet activation. (D) Transmission electron micrograph of aggregating platelets. 1, Platelet before secretion; 2 and 3, platelets secreting contents of granules; 4, collagen of endothelium. (E) SEM of fibrin mesh encasing colorized red blood cells. Right, Illustration panel (A through H) showing venous thromboembolus formation. (A) Stasis. (B) Fibrin formation. (C) Clot retraction. (D) Propagation. (E–H) Continuation of this process until the vessel is effectively occluded.
From Miller MD, Thompson SR, editors: DeLee and Drez’s orthopaedic sports
medicine: principles and practice, ed 4, Philadelphia, 2014, Saunders; platelet electron micrographs courtesy James G. White, MD, Department of Laboratory Medicine and Pathology, University of Minnesota School of Medicine; Miller MD
et al: Review of orthopaedics, ed 6, Philadelphia, 2012, Saunders; and Simon SR, editor: Orthopaedic basic science, Rosemont, IL, 1994, American Academy of Orthopaedic Surgeons, p 492.

 FIG. 1.52
Genetic (primary) disorders (table on
lef
t) and secondary hypercoagulable states (figure on
right
).
FIG. 1.52
Genetic (primary) disorders (table on
lef
t) and secondary hypercoagulable states (figure on
right
).
Data from Ginsberg MA: Venous thromboembolism. In Hoffman R et al, editors: Hematology: basic principles and practice, ed 4, Philadelphia, 2005, Churchill Livingstone, pp 2225–2236; Perry SL, Ortel TL: Clinical and laboratory evaluation of thrombophilia, Clin Chest Med 24:153–170, 2003; and Schafer AI: Thrombotic disorders: hypercoagulable states. In Goldman L, Ausiello D, editors: Cecil textbook of medicine, ed 22, Philadelphia, 2004, Saunders, pp 1082–1087.

FIG. 1.53 Top, The three primary influences of thromboembolic disease (Virchow triad). Bottom, The relative risks of various patient conditions; note that age has an exponentially increasing risk.
Composite from Miller MD, Thompson SR, editors: DeLee and Drez’s orthopaedic sports medicine: principles and practice, ed 3, Philadelphia, 2014, Saunders; and data from Anderson FAJr et al: Apopulation-based perspective of the hospital incidence and case-fatality rates of deep vein thrombosis and pulmonary embolism. The Worcester DVT Study, Arch Intern Med 151:933–938, 1991. - Procedure-specific factors ( Fig. 1.54)
- PE risk lower with distal procedures versus hip procedures
- Risk higher with longer procedures
- Total knee arthroplasty (TKA) has higher total DVT risk but lower PE risk
- Risk with hip fracture is higher than that with THA.
- Diagnosis
- Clinical diagnosis favors assessment of risk factors.
- Physical exam is unreliable: most cases are asymptomatic.
- DVTs can cause calf pain, palpable cords, swelling.
-
50% with classic signs have no DVT according to studies

--- FIG. 1.54 Rates of symptomatic thromboembolism in orthopaedic sports medicine. From DeHart M: Deep venous thrombosis and pulmonary embolism. In Miller MD, Thompson SR, editors: DeLee and Drez’s orthopaedic sports medicine: principles and practice, ed 4, Philadelphia, 2014, Saunders, p 207. - 50% with venogram positive for clo t have normal physical findings
- PEs: most asymptomatic
- Signs/symptoms include pleuritic chest pain, dyspnea, tachypnea
- Saddle emboli can manifest as death.
- Laboratory studies
- D -dimer studies not helpful after injury/surger y but negative result rules out significant clot.
- ECG: rule out MI
- Nonspecific findings; most common finding is sinus tachycardia.
- Radiologic studies ( Fig. 1.55)
- Venogram—best for distal (below popliteal) lesions (clinical relevance?)
- Duplex compression ultrasound—most practical
- Noninvasive, easily repeatable bedside test
- Finding of “noncompressible vein ” about 95% sensitive/specific
- Guidelines strongly against routin e duplex screening
- Chest x-ray
-
Early findings: usually normal, “oligemia,” or prominent hilum (
Fig.
1.56B) - Late findings: wedge or platelike atelectasis (see Fig. 1.56C)
- Spiral CT angiography—best for suspected PE
-
Ventilation-perfusion (

) scan—most helpful for dye-sensitive patients - Thromboembolic prophylaxis
- Preventing DVTs has been shown to be possible, although whether such prevention avoids death is unproven.
- Guidelines vary in their recommendations ( Fig. 1.57).
- Prophylaxis recommended for all patients undergoing arthroplasty.
- Those undergoing THA may benefit from extended treatment (≈30 days).
- For patients without risk-related conditions, prophylaxis is not recommended for
- Upper extremity procedures, arthroscopic procedures, surgery for isolated fractures at knee and below
- Mechanical measures
- Early mobilization
- Graduated elastic hose—not sufficient alone
- Intermittent pneumatic compression devices (IPCDs)
- Stimulate fibrinolytic system
- Low bleeding risks
- Grade IC by 2012 American College of Chest Physicians (ACCP) guidelines
- Continuous passive motion (CPM) of no benefit
- Pharmacologic prophylaxis:
- Surgical Care Improvement Project (SCIP) quality measures require DVT prophylaxis.
-
Aspirin
-
Irreversibly binds and inactivates COX in platelets, thereby reducing thromboxane A 2
-
Weakest: Use of IPCD encouraged


 FIG. 1.55
Top left to right,
Venogram showing deep vein thrombosis). Intraluminal filling defects
(arrows)
seen on two or more views of a venogram.
FIG. 1.55
Top left to right,
Venogram showing deep vein thrombosis). Intraluminal filling defects
(arrows)
seen on two or more views of a venogram.
The left and middle images are at the knee, and the right image is at the hip. Middle , Doppler ultrasound for proximal DVT in femoral vein thrombosis. (A) Longitudinal view shows presence of flow ( light blue ) in the more superficial vein over an occlusive thrombus ( dark gray ). (B) A transverse view without compression shows an open superficial vein, appearing as a black oval ( white arrow ) and a thrombosed deeper vein
as a dark gray circle with an echogenic center ( red arrow ). (C) A transverse view with compression shows the flattened compressible superficial vein ( white arrow ) and the unchanged noncompressible thrombosed deeper vein ( red arrow ). Bottom left, Spiral CT pulmonary angiography. (A) Large pulmonary embolism ( arrows ). (B) Normal CT. Right images, high probability

scan showing full lung fields on ventilation scan (upper) and multiple areas lacking tracer on the perfusion scan (lower) . ant, Anterior; LAO, left anterior oblique; post, posterior; RPO, right posterior oblique. DVT panel from Jackson JE, Hemingway AP: Principles, techniques and complications of angiography. In Grainger RG, editor: Grainger & Allison’s diagnostic radiology: a textbook of medical imaging, _ed 4, Philadelphia, 2011, Churchill Livingstone. Original images courtesy Austin Radiological Association and Seton Family of Hospitals.

--- FIG. 1.56 Chest radiographs. (A) Diffuse bilateral fluffy patchy infiltrates, worse at bases, are consistent with ARDS (acute respiratory distress syndrome). (B) A focal area of oligemia in the right middle zone (Westermark sign [_white arrow ]) and cutoff of the pulmonary artery in the upper lobe of the right lung are both seen with acute pulmonary embolism. (C) The peripheral wedge-shaped density without air bronchograms at lateral right lung base (Hampton hump [ black arrow ]) develops over time after a pulmonary embolism. B from Krishnan AS, Barrett T: Images in clinical medicine: Westermark sign in pulmonary embolism, N Engl J Med 366:e16, 2012; C from Patel UB et al: Radiographic features of pulmonary embolism: Hampton hump, Postgrad Med J 90:420–421, 2014.

--- FIG. 1.57 Recommendations on prevention of VTE in hip and knee arthroplasty. Hx, history; US, ultrasonography. 3. Low bleeding risk: Should be considered for patients at higher risk for bleeding. - Warfarin (Coumadin)
- Prevents vitamin K γ-carboxylation in liver
- Inhibits factors II, VII, IX, X, and proteins C and S
- Vitamin K and fresh frozen plasma can reverse
- Multiple reactions with drugs and diet
- Must be monitored with international normalized ratio (INR; goal, 2–3)
-
Heparin
-
Activates antithrombin III (ATIII), which then inactivates factor Xa and thrombin
- Protamine sulfate can reverse
- Short half-life: 2 hours
- High bleeding rate in arthroplasty
- Binds platelets—heparin-induced thrombocytopenia
- Low-molecular-weight heparin (LMWH)
- Reversibly inhibits factor Xa through ATIII and factor II
- Protamine sulfate can reverse
- No monitoring needed
- Less heparin-induced thrombocytopenia
-
Higher risk for bleeding than with
warfarin -
Fondaparinux
-
Irreversibly but indirectly inhibits factor X through ATIII
- Synthetic pentasaccharide
- No monitoring
- No antidote
- Higher risk for bleeding than with LMWH
-
Rivaroxaban
-
Direct Xa inhibitor
- Oral drug
- Higher risk for bleeding than with LMWH
- Hirudin
- Direct thrombin (IIa) inhibitor
- Intramuscular and oral (dabigatran) versions
- No antidote
- Inferior vena cava (IVC) filter use: controversial
- Should be considered in following conditions:
- Contraindication to prophylaxis
- Cerebral bleed/trauma
- Spine surgery
- Prior complication of prophylaxis
- Treatment of thromboembolic disease
- Pharmacologic treatment
- Prolonged therapy often recommended
- Approximately 3 months after DVT, approximately 12 months after PE
- Early mobilization— no bed rest
- Risk of dislodgment less than risk of more clots in these high-risk patients
- Graduated elastic compression hose for 2 years
- May prevent postthrombotic syndrome
- Thrombolytics, thrombectomy, embolectomy controversial
- Special venous thromboembolism (VTE) situations
- Isolated calf thrombosis smaller than 5 cm rarely needs treatment.
- Follow with serial ultrasound scans.
- Upper extremity blood clot in athlete
- “Effort thrombosis” (Paget-Schroetter syndrome)
- Axillary–subclavian vein thrombosis
- Complaints
- Pain, swelling
- Dilated veins
- Feeling of heaviness
- Diagnosis: duplex ultrasound
- Treatment: thoracic outlet decompression should be considered
Perioperative Disease and Comorbidities
-
Orthopaedic surgeons who evaluate their patients with care preoperatively can be rewarded with fewer perioperative problems.
-
Goals include finding correctable issues and identifying risks to provide accurate risk/benefit assessment for proper consent.
-
Cardiac issues
- Coronary artery disease (CAD): leading cause in those older than 35 years
- Leading cause of cardiac death in young sports population: hypertrophic cardiomyopathy
- American College of Cardiology/American Heart Association (ACC/AHA) elements for assessing risk
- Clinical risk factors in perioperative cardiac risk
- Major predictors
- Unstable/severe angina, recent MI (<6 weeks)
- Worsening or new-onset CHF
- Arrhythmias
- Atrioventricular (AV) block
-
Symptomatic ventricular dysrhythmia: bradycardia (<30
beats/min), tachycardia (>100 beats/min) - Severe aortic stenosis or symptomatic mitral stenosis
- Other
- Prior ischemic heart disease
- Prior CHF
- Prior stroke/ TIA
- Diabetes
- Renal insufficiency (creatine >2 mg/dL)
- Functional exercise capacity—measured in metabolic equivalents (METs)
- MET: 3.5 mL O2 uptake/kg/min
- Perioperative risk elevated if unable to meet 4-MET demand
- Walk up flight of steps or hill (= 4 METs)
- Heavy work around house (>4 METs)
- Can patient walk four blocks or climb two flights of stairs?
- Surgery-specific risk:
- High risk (>5% risk of death/MI)
- Aortic, major or peripheral vascular procedures
-
Intermediate risk (1%–5% risk of death/MI)
-
Orthopaedic, ENT, abdominal/thoracic or procedures
-
Low risk (<1% risk of death/MI)—usually do not need further clearance
-
Ambulatory surgery, endoscopic or superficial procedures
-
Shock
- Twelve-lead ECG if:
- CAD and intermediate-risk procedure
- One clinical risk factor and intermediate-risk procedure
- Noninvasive evaluation of left ventricular function if:
- Three or more clinical risk factors and intermediate-risk procedure
- Dyspnea of unknown origin
- CHF with worsening dyspnea without testing in 12 months
- β-Blockers and statins should be continued around the time of surgery.
- Acetylsalicylic acid (ASA) should be stopped 7 days prior to surgery.
- Cardiology consultation should be considered for patients taking other agents (clopidogrel, prasugrel).
- Risk of stent thrombosis balanced with that of surgical bleed
- Cardiovascular collapse with hypotension, followed by impaired tissue perfusion and cellular hypoxia. May be a result of orthopaedic pathology or a complication of surgery.
- Metabolic consequence
- O2 is unavailable—no oxidative phosphorylation
- Cells shift to anaerobic metabolism and glycolysis
- Pyruvate is converted to lactate—metabolic acidosis
-
Lactate—indirect marker of tissue hypoperfusion
-
Best measures of adequate resuscitation
-
Clinical measure of organ function: urine output more than 30 mL/h
-
Laboratory measure: serum lactate less than 2.5 mg/dL
- Types of shock
- Neurogenic shock
- High spinal cord injury (also anesthetic accidents)
- Loss of sympathetic tone and of vasomotor tone of peripheral arterial bed
- Bradycardia, hypotension, warm extremities
- Treatment: vasoconstrictors and volume
- Septic shock (vasogenic)
- Number one cause of ICU death
- Mortality 50%
- Bacterial toxins stimulate cytokine storm.
- Examples: gram-negative lipopolysaccharides
- Toxic shock superantigen
- Inflammatory mediators cause endothelial dysfunction and peripheral vasodilation
- Treatment
- Cardiogenic shock
- Bad pump
- Identification and treatment of infections
- Prompt resection of dead tissue
- Appropriate antibiotics
- Extensive MI, arrhythmias
- Blocked pump (obstructive shock)
- Massive “saddle” pulmonary embolism
- Tension pneumothorax
- Decreased lung sounds, hypertympany, tracheal deviation
- Treated with needle decompression followed by tube thoracostomy
- Cardiac tamponade
- Beck triad: hypotension, muffled heart sounds, neck vein distension
- Hypovolemic shock
- Pulsus paradoxus
- Decreased systolic BP with inspiration
- Treatment: pericardiocentesis
- Most common shock of trauma
- Volume loss from bleeds or burns
- “Third spacing” also a cause
- Neuroendocrine response: save heart and brain
- Peripheral vasoconstriction
- BP may be normal
- Pale, cold, clammy extremities
- Percentage of blood loss key to symptoms/signs
- Class I: up to 15% blood volume loss
- Vital signs can be maintained.
- Pulse below 100 beats/min
- Class II: 15%–30% blood volume loss
- Tachycardia (>100 beats/min), orthostatic
- Anxious
- Increased diastolic BP
- Class III: 30%–40% blood volume loss
- Decreased systolic BP
- Oliguria
- Confusion, mental status changes
- Class IV: more than 40% blood volume loss
- Life threatening; patient is obtunded
- Narrowed pulse pressure
- Immeasurable diastolic BP
- Treatment
-
Perioperative pulmonary issues
- First, ABCs of resuscitation: then, bleeding must be stopped.
- Blood products make better resuscitation fluids than saline.
- Higher in cases that involve thorax such as scoliosis
- Highest in patients with prior disease
- Spinal/epidural anesthesia favored over general
- Medical treatment should be maximized around surgery.
- COPD
- Symptomatic COPD: anticholinergic inhalers (ipratropium)
- May require corticosteroids
- Asthma
- Presence of wheezes or shortness of breath: β-agonist inhalers (albuterol)
- Perioperative oral steroids safe
- Systemic glucocorticoid should be considered if forced expiratory volume in 1 minute (FEV1) or peak expiratory flow rate (PEFR) is below 80% predicted values/personal best.
- Postoperative atelectasis
- Like the associated cough, the workup is usually nonproductive.
- Deep breathing/incentive spirometry—equally effective
- Postoperative pneumonia takes up to 5 days to manifest.
- Productive cough, fever/chills, increased WBC count
- Radiograph: pulmonary infiltrates
- Smoking cessation improves outcomes
- Patients should stop 6–8 weeks preoperatively.
- Nicotine supplements do no harm to wound.
- Fewer pulmonary complications
- Smokers have six times more pulmonary complications.
- Fewer wound healing issues and wound infections
- Lower nonunion rate
- Shoulder, neck, and thoracic pain in smokers
- Prompts careful evaluation of lung fields
-
Superior sulcus tumor (Pancoast tumor)
-
Acute respiratory distress syndrome (ARDS)
-
Intrinsic atrophy of hand—C8–T1
- Pulmonary failure due to edema (see Fig. 1.56A)
- Pathophysiology
- Complement pathway activated
- Increased pulmonary capillary permeability
- Intravascular fluid floods alveoli
- Results
- Hypoxia, pulmonary HTN
- Right heart failure
- 50% mortality
- Etiology
- Blunt chest trauma, aspiration, pneumonia, sepsis
- Shock, burns, smoke inhalation, near drowning
- Orthopaedic: Long-bone trauma
- Clinical symptoms
- Tachypnea, dyspnea, hypoxia, decreased lung compliance
- PaO 2 /FIO 2 ratio below 200
- Imaging
- Radiographs: diffuse bilateral infiltrates, “snowstorm”
- CT: ground glass appearance
- Treatment
- Prompt diagnosis and treatment of musculoskeletal infections
- Prompt treatment of long-bone fractures
- Ventilation with positive end-expiratory pressure (PEEP)
- 100% O2
-
Fat emboli syndrome—classic clinical triad
- Petechial rash: fat to skin
- Neurologic symptoms: fat to brain
- Mental status changes: confusion, stupor
- Rigidity, convulsions, coma
- Pulmonary collapse: fat showers lung
- ARDS: hypoxia, tachypnea, dyspnea
- Associated with long-bone fractures
-
Bleeding and blood products
- Bleeding complications can be avoided through preoperative identification of risk.
- Common inherited bleeding disorders
- Von Willebrand disease: autosomal dominant
- Most common genetic coagulation disorder
- Von Willebrand factor dysfunction
- Binds platelets to endothelium
- Carrier for factor VIII
- Treatment: desmopressin
-
Hemophilia A (VIII): X-linked recessive
- Hemophilia B (IX) Christmas disease: X-linked recessive
- Medicines/supplements that should be stopped prior to surgery
- Platelet-inhibitor drugs (aspirin, clopidogrel, prasugrel, NSAIDs)
- Drugs that cause thrombocytopenia
- Penicillin, quinine, heparin, LMWH
- Anticoagulants (see earlier discussion on DVT)
- Supplements
- Fish oil, omega-3 fatty acids, vitamin E
- Garlic, ginger, Ginkgo biloba
- Dong quai, feverfew
- Diseases associated with increased bleeding
- Chronic renal disease—uremia causes platelet dysfunction
- Chronic liver failure—decreased liver proteins of clotting cascade
- Techniques to avoid blood loss at surgery
- Tourniquets: tissue effect relates to time and pressure
- Used no longer than 2 hours
- Time to restoration of equilibrium
- 5 minutes after 90 minutes of use
- 15 minutes after 3 hours
- Prolonged use can cause tissue damage.
- Nerve damage compressive (not ischemic)
- Electromyography: subclinical abnormalities in 70% with routine use
- Slight increase in pain
- Wider tourniquets distribute forces
- Pad underneath prevents skin blisters in TKA
- Lowest pressure needed for effect should be used
- 100–150 mm Hg above systolic BP
- 200 mm Hg upper extremity
- 250 mm Hg lower extremity
- Tranexamic acid
- Synthetic lysine analogue; acts on fibrinolytic system
- Competitive inhibitor of plasminogen activation
- Reduces blood loss with no increase in DVT.
- Temperature
- Mild hypothermia increases bleeding time and blood loss.
- Intraoperative “cell saver” may be cost-effective if:
- About 1000 mL of blood loss is expected
- Recovery of 1 or more unit of blood is anticipated.
- Techniques not yet found to be effective or cost-effective
- Bipolar sealant, topical sealants, autologous donation
- Reinfusion systems, routine transfusions over 8 g/dL Hb
- Preoperative techniques to address anemia
- Oral iron 30–45 days preoperatively
- Vitamin C increases iron absorbtion
- Folate and vitamin B12 deficiency also a source of anemia
- Erythropoietin if preoperative Hb below 13
- Transfusions
- Ratio of 1:1:1 blood product resuscitation is superior to saline fluid
- Preoperative Hb most significant predictor of need
- Various guidelines for when to transfuse
- Hb less than 6 g/dL: transfusion
- Hb 7–8 g/dL: transfusion of postoperative patients
- Hb 8–10 g/dL: transfusion of symptomatic patients
- Restrictive transfusion strategies
- Lower 30-day mortality trend
- Lower infection risk trend
- Greatest benefits to orthopaedic patients
- No difference in functional recovery
- Transfusions risks
- Leading risk: transfusion of wrong blood to patient
- Occurs in 1 in 10,000 to 1 in 20,000 RBC units transfused
- Transfusion reactions
- Febrile nonhemolytic transfusion reaction
- Most common
- 1–6 hours post-transfusion
- From leukocyte cytokines released from stored cells
- Leukoreduction decreases incidence
- Acute hemolytic transfusion reaction
- Medical emergency
- ABO incompatibility
-
IgM anti-A and anti-B,
which fix complement - Rapid intravascular hemolysis
- Classic triad: fever, flank pain, red/brown urine (rare)
- Can cause disseminated intravascular coagulation (DIC), shock, and acute renal failure (ARF) due to acute tubular necrosis (ATN)
- Positive direct antiglobulin (Coombs) test result
- Delayed hemolytic transfusion reactions
- Reexposure to previous antigen (i.e., Rh or Kidd)
- History of pregnancy, prior transfusion, transplantation
- 3–30 days post-transfusion
- Anemia, mild elevation of unconjugated bilirubin, spherocytosis
- Anaphylactic reactions: about 1 in 20,000
- Rapid hypotension, angioedema
- Shock, respiratory distress
- Frequently involve anti-IgA and IgE antibodies
- Treatment: cessation of transfusions, ABCs of resuscitation, epinephrine
- Urticarial reactions: about 1%–3%
- Mast cell/basophils release of histamine—hives
- Infectious risks
- Bacterial: 0.2 per million packed red blood cell (PRBC) units transfused
- Gram-positive organisms
- Cryophilic organisms: Yersinia, Pseudomonas
- HTLV—approximately 1 in 2 million
-
Renal and urologic issues
- HIV—approximately 1 in 2 million
- Hepatitis C—approximately 1 in 2 million
- Hepatitis B—approximately 1 in 250,000
- ARF (acute kidney injury [AKI])
- Edema, HTN, urinary output less than 30 mL/hour (<0.5 mL/kg/h)
- Laboratory findings: creatinine increased over 1.5 times baseline
- Hyperkalemia can be fatal.
-
For blood potassium level more than
5.5 mmp/L, dialysis should be considered. - Prerenal renal failure (most common ARF): decreased kidney perfusion
- Hypovolemia/hypotension from blood loss
- Intrinsic renal failure
- ATN: most frequent intrinsic ARF
- Ischemia, sepsis, nephrotoxic drugs
- Myoglobin from rhabdomyolysis
- Acute interstitial nephritis (AIN): fever, eosinophils in blood/urine
- Glomerular disease: hematuria, proteinuria, HTN, edema
- SLE, poststreptococcal, IgA nephropathy, hepatorenal
- Postrenal ARF: obstruction
- Chronic kidney disease (CKD)
- Definition: GFR below 60 mL/min per 1.73 m2 or urine albumin loss greater than 30 mg/day
- Retained phosphate and secondary to hyperparathyroidism
- Causes increased extraskeletal calcification
- High perioperative complications
- Increased cardiovascular risk
- Hyperkalemia and fluid adjustments
- Increased bleeding complications
- Poor BP control
- Higher infection rates
- Higher complications/revisions
- Higher morbidity
- Perioperative urinary retention
- Outflow obstructions: benign prostatic hypertrophy (BPH) in men (common)
- Bladder muscle (detrusor) compromise
- Overdistention
- Excess fluid/long procedures
- Neurogenic
- Spinal trauma, tumor, stroke, diabetes
- “Neurogenic” atonic bladder
- Medications
- Anticholinergic and sympathomimetic drugs
- Opioids, antidepressants, pseudoephedrine, diphenhydramine
- Can cause postrenal ARF (AKI)
- Associated with higher rates of urinary tract infections
- Increased 2-year mortality after hip fracture
- Treatment
- α-Blockers—tamsulosin 0.4 mg/day
- Bladder ultrasound if no voiding by 3–4 hours
- If ultrasound shows more than 400–600 mL, in-and-out (IO) urinary catheter should be used.
- Trauma patient—no catheter if bloody meatus or scrotal hematoma present
- Perioperative UTI
- “Irritative symptoms”: dysuria, urgency, frequency
- Account for 30%–40% of hospital-acquired infections
- Most common organisms: Escherichia coli and Enterococcus
- Diagnosis
- If symptoms, urinalysis and culture/sensitivity testing
- WBCs (leukocyte esterase positive)
- Bacterial count over 103 CFU/mL, treated preoperatively
- Treatment
- Antibiotics for gram-negative organisms
-
Trimethoprim-sulfamethoxazole or fluoroquinolone
1.** GI motility disorders ( ** Fig. 1.58) - 1.5% of hip/knee arthroplasties
- Common presentation
- Abdominal pain
- Distension
- Nausea with or without vomiting
- Prevention
- Chewing gum: vagal (parasympathetic stimulation)
- Early mobility
- Spinal (sympathetic block)
- Limiting dose and length of IV opioids
- Postoperative adynamic ileus
- Gut autonomic nerve imbalance:
- More common in spine (≈7%) and joint arthroplasty (≈1%)
- X-rays: dilated small and large bowel (see Fig. 1.58A)
- Treatment: nothing by mouth status, nasogastric tube
- Electrolyte control
- Cessation of narcotics
- Superior mesenteric artery (SMA) syndrome (cast syndrome)
- Occlusion of duodenum by SMA
- Orthopaedic causes
- Hip spica cast
- Following scoliosis surgery
- Following THA with severe hip flexion contracture
- Following traumatic quadriplegia
- Also found in patients with rapid, large weight loss
- X-rays: distended stomach and upper duodenum (see Fig. 1.58B )
- CT
- Aortomesenteric artery angle less than 25 degrees
- Aortomesenteric distance less than 8 mm
- Treatment: nothing by mouth status, nasogastric tube
- Acute colonic pseudoobstruction (Ogilvie syndrome)
- Large bowel dilation
- Abdominal distension the prominent symptom
- Colonic perforation should be avoided.
- Risk factors
- Elderly or male patient
- Previous bowel surgery
- Diabetes, hypothyroidism
- Electrolyte disorders
- Radiographic findings
- Distended transverse and descending colon and cecum (see Fig. 1.58C)
- Colonic diameter more than 10 cm risks perforation.
- Treatment
- Nothing by mouth status
- Neostigmine
- Colonic decompression
- Pseudomembranous colitis: potentially fatal diarrhea
- Most common antibiotic-associated colitis
- Change in colon flora favors Clostridium difficile
- Makes enterotoxin-A and cytotoxin-B
- Many antibiotics
- Clindamycin, fluoroquinolones
- Penicillins and cephalosporins
- Can become severe fulminant colitis
- Toxic megacolon and perforations
- Risk factors
- Elderly hospitalized patient
- Severe illness
- Antibiotic use
- Proton pump inhibitor use
- Diagnosis
- Watery diarrhea with fever
- Leukocytosis, lower abdominal pain
- Laboratory findings
- WBC count more than 15,000 cells/µL
-
Stool specimen should be tested for
C. difficile
toxin - PCR or ELISA
- KUB (kidney, ureter, bladder) (plain abdominal) radiograph
- Toxic megacolon: greater than 7 cm
- Thumbprinting (see Fig. 1.58D)
- Treatment
- Oral metronidazole
- Oral vancomycin (IV will not work)
- Fidaxomicin
- Colectomy if unresponsive and severe
- Megacolon, WBC count more than 20,000 cells/µL
-
Perioperative hepatic issues
- Liver failure: critical for producing proteins and metabolizing toxins
- Laboratory findings
- Increased aspartate aminotransferase (AST), alanine aminotransferase (ALT), and bilirubin
- INR above 1.5, low platelets (<150,000 cells/µL)
- Acute—most commonly viral and drug induced
- Acetaminophen—number one cause in United States
- Other toxins: alcohol, occupational, mushrooms
- Viral hepatitis
- Chronic—cirrhosis is end-stage fibrosis of liver
- Common: hepatitis (B, C), alcoholism, hemochromatosis
- Classifications can be helpful to estimate risks
- Child classification—most widely used
- Based on laboratory results and physical examination
- Model for End-Stage Liver Disease (MELD) score ( http://www.mayoclinic.org/medical-professionals/model-end-stage-liver-disease/meld-model )
- Formula based on bilirubin, INR, creatinine
- Studies highlight mortality at 90 days relative to MELD score
- <9: about 2% mortality
- 10–19: about 6% mortality
- 20–29: about 20% mortality
- 30–39: about 53% mortality
-
40: about 71% mortality
- Complication rates from surgery are extremely high.
- In patients undergoing arthroplasty, MELD score above 10 predicted
- Three times the complication rate
- Four times the rate death
-
Perioperative CNS issues
- Stroke
- Rare (0.2% of joint arthroplasties)
- Mortality roughly 25% at 1 year
- Ischemic more common than hemorrhagic
- Risk factors
- Advanced age, CVA, TIA
- MI, coronary artery bypass graft, atrial fibrillation, or ECG rhythm abnormality
- Left ventricular dysfunction
- Cardiac valvular disease
- General anesthesia higher risk than regional
- Diagnosis: head CT or MRI
- Treatment: ABCs of resuscitation, hospitalist/neurology consultation
- Delirium: approximately 40% in patients with hip fractures
- Fluctuating levels of consciousness
- Impairment of memory and attention
- Disorientation, hallucinations, agitation
- Associated with increased length of stay
- Decubitus ulcers, failure to regain function
- Feeding issues, urinary incontinence
- Mortality and nursing home placement
- Risk factors
- Older patients
- History of prior postoperative confusion
- History of alcohol abuse
-
Acute surgery more than elective

--- FIG. 1.58 Perioperative gastrointestinal mobility radiographs. (A) Dilated loops of both small bowel and large bowel consistent with ileus. (B) Characteristic dilation with air-fluid levels in the stomach and right-sided upper duodenum, seen in mesenteric artery syndrome (cast syndrome). (C) Isolated dilation of the large bowel seen in acute colonic pseudoobstruction (Ogilvie syndrome). (D) Dilated loops of both small and large bowel in a patient with watery diarrhea after antibiotic use. Wide, thickened, transverse bands of nodular colon wall replace normal haustral folds (thumbprinting), as seen in pseudomembranous colitis. A and C from Nelson JD et al: Acute colonic pseudo-obstruction [Ogilvie syndrome] after arthroplasty in the lower extremity, J Bone Joint Surg Am 88:604–610, 2006; B from Tidjane Aet al: [Superior mesenteric artery syndrome: rare but think about it], [article in French] Pan Afr Med J 17:47, 2014; and D from Thomas Aet al: “Thumbprinting,” Intern Med J 40:666, 2010. - Night-time surgery
- Long duration of anesthesia
- Intraoperative pressures below 80 mm Hg
- Use of meperidine (Demerol)
- Diagnosis: anemia ruled out, infection, electrolyte issues
- Treatment
-
O2 saturation above 95%, systolic BP above 90 mm
Hg - Correction of medical issues
- Family/friends
- Medications for sedation: used with caution
- Restraints as last resort
-
Special anesthesia issues
- Obstructive sleep apnea (OSA)
- Intermittent hypercapnia and hypoxia
- Decreased CO2-induced respiratory drive
- Extreme sensitivity to opioids
- Leads to
- Pulmonary HTN
- Cardiac arrhythmias
- GERD (reflux) directly related to BMI
- Delayed gastric emptying
- Increased risks for aspiration/intubation
- Higher risk for complications (2–4 times greater)
- Respiratory failure, ICU transfers, increased length of stay
-
Increased postoperative O2
desaturation - Increased intubation, aspiration pneumonia, ARDS
- Increased MI, arrhythmias (atrial fibrillation)
- Screening tools: STOP-BANG ( Fig. 1.59)
-
S noring, t ired, o bserved apnea, p
ressure (HTN)
B MI over 35, a ge older than 50 years, n eck circumference larger than 40 cm, g ender male - Five or more factors present—high risk of severe OSA
- Best practices
- Initiation or continuation of CPAP use
-
More than 2 weeks of preoperative CPAP
improved HTN, O2 saturation, apneic events - Pulmonary HTN: in 20%–40% of patients with OSA
- Preoperative serum bicarbonate predicts hypoxia in OSA
- Chronic respiratory acidosis
- Site of service (American Society of Anesthesiology consensus statement)
- Malignant hyperthermia
- Ambulatory surgery under local/regional— lower risk
- Avoid procedures requiring opioids— greater risk
- Comorbid conditions must be optimized for outpatient surgery.
- HTN, arrhythmias, CHF, cardiovascular disease, and metabolic syndrome
-
Metabolic syndrome = obesity, hypertension, hypercholesterolem dyslipidemia, and insulin resistance
- Avoidance of flat supine position; sitting position opens airway.
-
Autosomal dominant genetic defect of T-tubule of sarcoplasmic reticulum
- Ryanodine receptor defect (RYR1)
- Dihydropyridine receptors (DHP)
-
Triggered by volatile anesthetics and succinylcholine
- Creates an uncontrolled release of Ca2+
- Sustained muscular contraction (masseter rigidity)
-
Increased end-tidal CO 2
-
Earliest and most sensitive sign
- Mixed respiratory and metabolic alkalosis
- Hyperthermia is classic but occurs later.
- Muscle damage
- Myoglobin from rhabdomyolysis can cause ARF.
- Elevated creatine kinase
- Hyperkalemia can lead to ventricular arrhythmias.
- Treatment with dantrolene
- Decreases intracellular Ca2+
- Stabilizes sarcoplasmic reticulum
- Treatment of high serum potassium
- Hydration
- Cooling
You Might Also Like
Previous ChapterOptimize Pain Management with Proximal Ring Block for Ankle…
Next Chapter Optimizing Perioperative Pain Management in Shoulder Surger…

Medically Verified Content by
Prof. Dr. Mohammed Hutaif
Consultant Orthopedic & Spine Surgeon