Open Reduction and Internal Fixation of Intraarticular Phalangeal Fractures
Key Takeaway
Intraarticular fractures of the interphalangeal joints demand precise anatomical reduction to restore joint congruity and biomechanical function. This comprehensive guide details the Doyle technique utilizing pull-out wires and transarticular Kirschner wires, alongside alternative fixation strategies such as mini-fragment screws and bone grafting for comminuted impaction injuries. Strict adherence to meticulous surgical approaches and structured postoperative rehabilitation is paramount for optimizing long-term functional outcomes and minimizing posttraumatic arthritis.
Introduction to Intraarticular Phalangeal Fractures
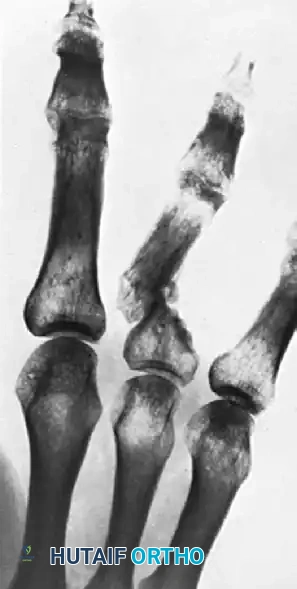
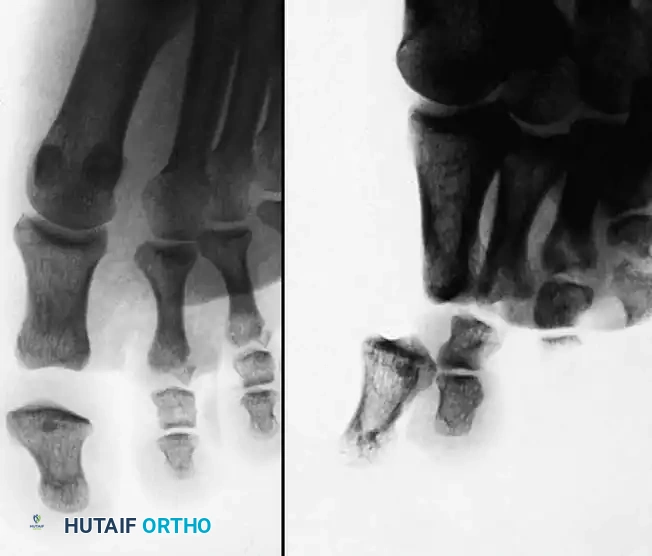
Intraarticular fractures of the interphalangeal (IP) joints of the hand present a formidable challenge to the orthopaedic surgeon. The proximal interphalangeal (PIP) and distal interphalangeal (DIP) joints are highly constrained, precision-driven articulations. Even minor articular step-offs or angular deformities can lead to profound functional impairment, characterized by stiffness, chronic pain, and early-onset posttraumatic osteoarthritis.
The primary goals of surgical intervention are the restoration of articular congruity, the re-establishment of joint stability, and the facilitation of early, controlled mobilization. While certain undisplaced or minimally displaced fractures may be managed non-operatively, displaced intraarticular fractures—particularly those involving avulsions of critical tendinous or ligamentous insertions, hemicondylar shear injuries, or central impaction with comminution—mandate meticulous open reduction and internal fixation (ORIF).
This comprehensive guide delineates the operative management of these complex injuries, with a specific focus on the Doyle technique utilizing a pull-out wire and transarticular Kirschner (K-wire) fixation, alongside alternative strategies such as mini-fragment screw fixation and dynamic skeletal traction.
Surgical Anatomy and Biomechanics
A profound understanding of the osseous and soft-tissue anatomy of the interphalangeal joints is prerequisite for successful surgical reconstruction.
- The Proximal Interphalangeal (PIP) Joint: A bicondylar hinge joint with a normal arc of motion from 0 to 110 degrees. Stability is conferred by the true and accessory collateral ligaments laterally, the robust volar plate palmarly, and the central slip of the extensor mechanism dorsally.
- The Distal Interphalangeal (DIP) Joint: A similar hinge joint, stabilized by collateral ligaments, a volar plate, and the terminal extensor tendon dorsally, opposed by the flexor digitorum profundus (FDP) palmarly.
- Vascularity: The phalanges receive their blood supply via the digital arteries, which give off transverse branches forming arcades. Surgical approaches must respect these vascular networks to prevent avascular necrosis of small articular fragments.
💡 Clinical Pearl: The "Rule of Threes" in Articular Fixation
When considering internal fixation of an articular fragment with a mini-fragment AO screw, the width of the osseous fragment must be at least three times the diameter of the screw being utilized (e.g., a 1.5 mm screw requires a fragment at least 4.5 mm wide). Failure to adhere to this biomechanical principle risks iatrogenic comminution and catastrophic failure of fixation.
Indications for Operative Intervention
Operative management is generally indicated for:
1. Displaced Intraarticular Fractures: Articular step-off greater than 1 to 2 mm.
2. Joint Subluxation or Dislocation: Inability to maintain a concentric reduction in a functional position.
3. Avulsion Fractures with Instability: Involving greater than 25% of the articular surface (e.g., dorsal mallet fractures or volar plate avulsions).
4. Hemicondylar Fractures: Displaced lateral stress injuries requiring anatomical restoration of the condylar geometry.
5. Impaction Fractures: Central articular depression requiring elevation and structural bone grafting.
The Doyle Technique: Open Reduction with Pull-Out Wire and Transarticular K-Wire
The Doyle technique is a highly effective method for managing unstable intraarticular fractures, particularly avulsion fractures at the DIP joint (such as severe mallet fractures) where the fragment is too small or comminuted for screw fixation, yet requires rigid neutralization of deforming tendinous forces.
Preoperative Preparation and Positioning
- Anesthesia: Regional block (e.g., axillary or supraclavicular brachial plexus block) or wide-awake local anesthesia no tourniquet (WALANT).
- Positioning: Supine with the affected extremity extended on a radiolucent hand table.
- Tourniquet: A pneumatic arm tourniquet or sterile finger tourniquet is applied to ensure a bloodless surgical field (unless utilizing WALANT).
- Imaging: Intraoperative fluoroscopy (mini C-arm) is positioned parallel to the hand table.
Surgical Approach
- Incision: Expose the joint through a dorsal zigzag (Bruner-style) or H-shaped incision (Fig. 67-67A). This prevents longitudinal scar contracture over the joint flexion crease.
- Soft Tissue Dissection: Elevate full-thickness fasciocutaneous flaps. Carefully preserve the paratenon and the dorsal venous drainage to minimize postoperative edema.
- Joint Exposure: Identify the terminal extensor tendon and the avulsed osseous fragment. Clear the fracture site of organized hematoma and interposed soft tissue using a fine curette or dental pick. Irrigate the joint copiously.
Step-by-Step Fixation Technique
- Preparation of the Distal Phalanx: Pass a 0.035-inch (0.9 mm) Kirschner wire longitudinally through the distal phalanx from proximal to distal, exiting the fingertip (Fig. 67-67B).
- Fragment Reduction: Anatomically reduce the avulsed articular fragment into its native bed. Use a fine dental pick or a small reduction forceps. Ensure the articular surface is perfectly flush via direct visualization and fluoroscopic confirmation.
- Pull-Out Wire Placement: Pass a fine stainless steel wire (e.g., 4-0 or 5-0) or a non-absorbable monofilament suture through the tendinous insertion attached to the small fragment. Drill two parallel micro-tunnels through the distal phalanx, exiting the volar pulp. Pass the ends of the wire/suture through these tunnels.
- Transarticular Pinning: To neutralize the deforming force of the flexor digitorum profundus and protect the reduction, drive the previously placed 0.035-inch K-wire retrogradely across the reduced DIP joint into the middle phalanx. The joint should be pinned in neutral extension (0 degrees).
- Securing the Pull-Out Wire: Tie the volar pull-out wire over a sterile button on the volar pad of the distal phalanx. Ensure the tension is sufficient to hold the fragment securely without causing ischemia to the volar skin.
⚠️ Surgical Warning: Transarticular Pinning
Transarticular K-wires should never be left in place longer than absolutely necessary, as they inevitably cause chondral damage and capsular scarring. The wire must be removed precisely at 3 to 4 weeks to prevent permanent joint stiffness.
Alternative Fixation Strategies
While the Doyle technique is excellent for specific avulsion patterns, other intraarticular fractures demand different biomechanical solutions.
Mini-Fragment AO Screw Fixation
For larger, non-comminuted articular fragments (e.g., large hemicondylar fractures), interfragmentary lag screw fixation provides superior biomechanical stability and allows for earlier mobilization without the need for transarticular pinning.
* Technique: The fracture is reduced and provisionally held with a 0.028-inch K-wire. A 1.5 mm or 2.0 mm titanium or stainless steel screw is utilized.
* Lag Principle: The near cortex (the fragment) is overdrilled to the external diameter of the screw (gliding hole), while the far cortex is drilled to the core diameter (thread hole). This generates interfragmentary compression.
* Countersinking: The screw head must be carefully countersunk to prevent impingement on the collateral ligaments or extensor mechanism, which can severely restrict motion.
Closed Reduction and Percutaneous Pinning (CRPP)
Hemicondylar fractures produced by lateral stress (usually at the PIP joint) can occasionally be managed via closed reduction.
* Technique: Longitudinal traction is applied, and the fracture is reduced using a pointed reduction forceps applied percutaneously.
* Fixation: A 0.035-inch K-wire is drilled transversely or obliquely into the smaller fragment, capturing the reduction, and driven into the larger intact fragment.
* Extraction Technique: The drill is then attached to the opposite (exiting) end of the wire and used to extract it until the proximal tip sits just beneath the articular cartilage of the smaller fragment, preventing intraarticular hardware prominence.
Dynamic Skeletal Traction
For highly comminuted intraarticular fractures (e.g., "pilon" fractures of the PIP joint) where internal fixation is impossible, closed methods utilizing ligamentotaxis are preferred.
* Three-Point Skeletal Traction: A vertical traction ring or dynamic external fixator (e.g., Suzuki frame) is applied. This maintains joint distraction, utilizes the intact soft tissue envelope to mold the comminuted fragments, and permits early active motion to facilitate cartilage remodeling.
Management of Specific Fracture Patterns
Impaction Fractures with Comminution
Central depression of the articular surface often occurs due to axial loading.
* Surgical Elevation: The depressed articular fragments must be carefully elevated using a fine bone tamp or freer elevator.
* Bone Grafting: Elevation creates a metaphyseal void. This must be filled with cancellous bone graft (harvested from the distal radius or olecranon) to support the articular surface and prevent secondary subsidence.
* Supplemental Fixation: Once grafted, the construct is stabilized with a lateral-to-medial K-wire or a mini-fragment plate if the lateral wall is compromised.
Intraarticular Avulsion Fractures
These injuries occur at the insertions of tendons (terminal extensor, central slip) and ligaments (collateral ligaments, volar plate).
* Pathomechanics: The fragments are usually displaced widely by the unopposed pull of the attached soft tissue.
* Treatment Algorithm:
* Small Fragments (<25% of joint surface): Treatment is directed toward the soft tissue avulsion. This may consist of open reduction and splinting, or non-operative splinting alone in the position of function (e.g., continuous extension splinting for 6-8 weeks for a tendinous mallet injury).
* Large Fragments (>25% of joint surface): Require anatomical reduction and internal fixation (via pull-out wire, K-wire, or screw) to restore joint integrity and prevent volar/dorsal subluxation.
Hemicondylar Fractures
Typically occurring at the PIP joint due to severe lateral deviation forces.
* Management: If displaced, these require internal fixation. While closed reduction and percutaneous pinning can be attempted, open reduction is often necessary to ensure perfect articular congruity and to clear interposed collateral ligament or volar plate tissue from the fracture site.
Postoperative Protocol and Rehabilitation
The ultimate success of intraarticular phalangeal fracture fixation relies heavily on the postoperative rehabilitation protocol. The hand is highly prone to stiffness, and a delicate balance must be struck between protecting the fracture and mobilizing the joint.
- Phase I (0-2 Weeks): The digit is immobilized in a custom thermoplastic splint. For transarticular K-wire constructs, the joint is held static. Edema control (elevation, compressive wrapping) is critical. Unaffected joints (MCP, wrist) are mobilized immediately.
- Phase II (2-4 Weeks): If rigid internal fixation (screws) was achieved, early active range of motion (AROM) is initiated under the guidance of a certified hand therapist. For Doyle technique/transarticular pinning, motion is usually started at 2 to 3 weeks following the removal of the transarticular K-wire. The pull-out wire and button are typically removed at 4 to 6 weeks.
- Phase III (4-8 Weeks): Progressive weaning from the splint. Passive range of motion (PROM) and gentle strengthening are introduced once clinical and radiographic union is confirmed.
💡 Clinical Pearl: Managing Postoperative Stiffness
Extensor lag and joint stiffness are the most common complications following IP joint surgery. Aggressive passive stretching should be avoided early on, as it provokes inflammation and exacerbates scar formation. Focus on active motion and dynamic splinting.
Long-Term Outcomes and Prognosis
The outcome following intraarticular fractures of the interphalangeal joints is multifactorial, depending heavily on the patient’s age, the specific location of the injury, the degree of initial comminution, associated soft tissue trauma, the anatomical accuracy of the surgical reduction, and patient compliance with postoperative management.
Clinical Evolution
Surgeons must counsel patients that recovery is protracted. Swelling and induration around the PIP or DIP joint can persist for 6 to 12 months. However, long-term follow-up demonstrates that pain usually diminishes significantly, and motion continues to improve with time.
Evidence-Based Outcomes
According to landmark long-term studies (e.g., Barton et al.):
* Pain: Only 27% of patients report being completely pain-free at early follow-up (within the first year). However, this improves dramatically, with 66% reporting absolutely no discomfort after 11 years.
* Range of Motion: A gradual improvement in motion is consistently observed over the first two years. Despite this, only approximately 60% of patients regain a completely normal range of motion compared to the contralateral uninjured digit.
* Posttraumatic Arthritis: Approximately 17% of patients will show radiographic evidence of posttraumatic osteoarthritis at long-term follow-up (joint space narrowing, osteophyte formation, subchondral sclerosis).
* Clinical-Radiographic Disconnect: Crucially, radiographic findings of arthritis do not reliably correlate with clinical symptoms. Many patients with severe radiographic joint destruction maintain excellent, pain-free functional use of the hand, underscoring the remarkable adaptive capacity of the digital articulations.
Conclusion
The management of intraarticular phalangeal fractures requires a sophisticated understanding of hand biomechanics and a meticulous surgical technique. Whether employing the Doyle technique with pull-out wires and transarticular pinning for complex avulsions, or utilizing mini-fragment screws for hemicondylar shear fractures, the mandate remains the same: anatomical articular reduction, stable fixation, and the earliest possible mobilization. Through rigorous adherence to these principles, orthopaedic surgeons can mitigate the risks of chronic pain and stiffness, restoring optimal function to the injured hand.
📚 Medical References
- [phalangeal fractures. In Tubiana R, ed: The hand, Philadelphia, 1985, Saunders.
Gunther SF, Zielinski CJ: Irreducible palmar dislocation of the proximal phalanx of the thumb: case report, J Hand Surg 7A:515, 1982.](https://pubmed.ncbi.nlm.nih.gov/?term=phalangeal%20fractures.%20In%20Tubiana%20R%2C%20ed%3A%20The%20hand%2C%20Philadelphia%2C%201985%2C%20Saunders.%0A%0AGunther%20SF%2C%20Zielinski%20CJ%3A%20Irreducible%20palmar%20dislocation%20of%20the%20proximal%20phalanx%20of%20the%20thumb%3A%20case%20report%2C%20J%20Hand%20Surg%207A%3A515%2C%201982.)
- Helm RH: Hand function after injuries to the collateral ligaments of the metacarpophalangeal joint of the thumb, J Hand Surg 12B:252, 1987.
- Hergan K, Mittler C: Sonography of the injured
You Might Also Like