Hand Fractures, Dislocations, and Ligamentous Injuries: Principles of Operative Treatment
Key Takeaway
The management of metacarpal and phalangeal fractures requires a profound understanding of hand biomechanics and precise surgical execution. While closed reduction and splinting suffice for many injuries, unstable, malrotated, or intra-articular fractures demand operative intervention. This guide details the critical principles of clinical evaluation, radiographic assessment, and surgical fixation techniques necessary to restore optimal hand function and prevent debilitating complications such as malunion and contracture.
PRINCIPLES OF TREATMENT IN HAND TRAUMA
The human hand is an intricate biomechanical marvel, relying on a delicate equilibrium between the skeletal architecture, capsuloligamentous constraints, and the dynamic forces of the extrinsic and intrinsic musculature. For the majority of metacarpal and phalangeal fractures, closed manipulation, proper splinting in the "intrinsic-plus" (safe) position, and protected early motion generally produce excellent functional results.
However, there are critical exceptions where non-operative management falls short. Operative treatment—usually encompassing open reduction and internal fixation (ORIF) or closed manipulation with percutaneous pinning (CRPP)—is mandated to provide superior outcomes in specific clinical scenarios. The overarching goal of any intervention is the restoration of anatomical alignment, preservation of the gliding planes of tendons, and the rapid reinstitution of motion to prevent stiffness.
Timing of Surgical Intervention
The timing of fracture fixation is a critical variable in the surgical decision-making process.
Surgical Pearl: Percutaneous pinning should ideally be attempted before the onset of massive edema obliterates external anatomic landmarks. If the soft tissue envelope is already compromised by severe swelling, the extremity should be strictly elevated for 24 to 48 hours before attempting reduction and pinning.
Fracture fixation, particularly via open approaches, is preferably performed when the soft tissue envelope is pliable and not markedly swollen. Operating through severely traumatized, edematous tissue increases the risk of wound dehiscence, infection, and subsequent tendon adhesions. In cases of severe closed trauma, a deliberate delay in fixation of 7 to 10 days is often warranted to allow the soft tissues to declare themselves and swelling to subside.
Indications for Operative Fixation
While each case must be individualized, some form of rigid or semi-rigid fixation is most often indicated in the following instances:
* Irreducible Fractures: Fractures that cannot be reduced via closed manipulation due to soft tissue interposition (e.g., complex metacarpophalangeal dislocations).
* Unstable Fracture Patterns: Spiral or long oblique fractures of the metacarpals or phalanges that tend to shorten or rotate despite appropriate splinting.
* Intra-articular Fractures: Fractures involving more than 25% of the articular surface or those with greater than 1 mm of articular step-off, which predispose the joint to post-traumatic arthritis.
* Multiple Fractures: "Crush" injuries or multiple ray involvement where the hand loses its structural scaffolding.
* Open Fractures: Injuries requiring surgical debridement often benefit from immediate stabilization to protect the soft tissue repair.
* Fractures with Bone Loss: Requiring structural grafting and rigid plate or K-wire fixation.
CLINICAL EVALUATION: THE CRITICAL ASSESSMENT OF MALROTATION
One of the most devastating complications of hand fractures is unrecognized malrotation. Because of the functional length of the digits, even a seemingly trivial rotational deformity of 5 degrees at the metacarpal level can translate to 1.5 cm of digital overlap at the fingertips, severely impairing the patient's ability to form a functional grip.
The Digital Cascade Sign
Clinical assessment of rotation must be performed meticulously. The most reliable method is observing the digital cascade during active or passive flexion.
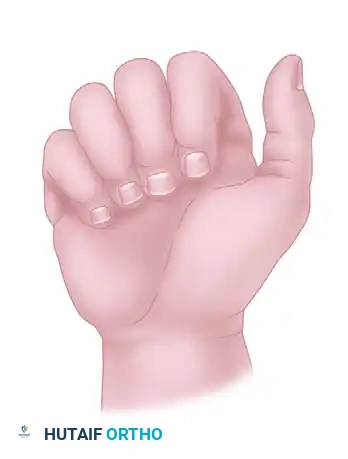
Normally, when a fist is made, the longitudinal axes of all the fingers converge and point toward the region of the scaphoid tubercle.

FIGURE 67-1 A: Normally, all fingers point toward the region of the scaphoid when a fist is made.
Malrotation at the fracture site disrupts this harmonious convergence, causing the affected finger to deviate and cross over adjacent digits. This overlap must be corrected anatomically during reduction.
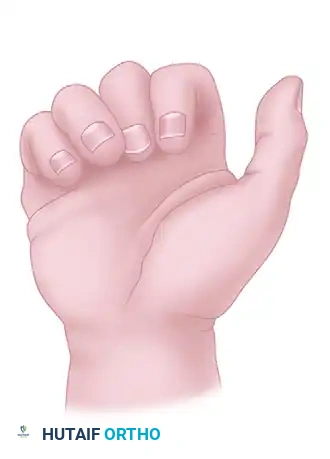
FIGURE 67-1 B: Malrotation at the fracture causes the affected finger to deviate, leading to functional impairment during grip.
Fingernail Alignment
Another highly effective clinical tool for detecting subtle malrotation is observing the plane of the fingernails in a semi-flexed position and comparing it to the contralateral, uninjured hand.
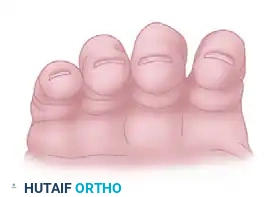
FIGURE 67-2 A: Normal alignment of the fingernails, demonstrating a smooth, parallel arc.
If a fracture is malrotated, the fingernail of the involved digit will sit out of plane compared to its neighbors. This is particularly noticeable in spiral fractures of the proximal phalanx or metacarpal shafts.
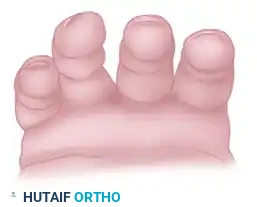
FIGURE 67-2 B: Alignment of the fingernails demonstrating clear malrotation of the ring finger.
Nuances of the Little Finger
The fifth ray (little finger) possesses unique kinematics due to the mobility of the fifth carpometacarpal (CMC) joint, which allows for 20 to 30 degrees of flexion and extension. This mobility can sometimes mask or simulate rotational deformities, requiring careful examination.
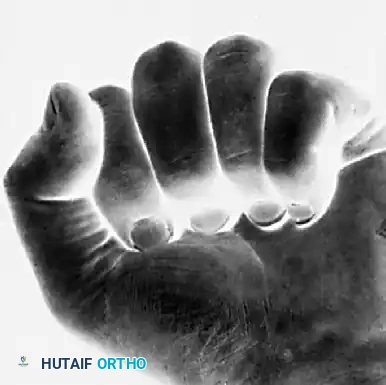
FIGURE 67-3 A: Note the alignment of the normal little finger during flexion.
Because of the CMC joint's mobility, a normal little finger can actually be made to overlap the ring finger passively. With incomplete flexion, this normal overlap may be erroneously perceived as a rotational deformity.

FIGURE 67-3 B: A normal little finger can be made to overlap the ring finger. With incomplete flexion, this overlap may be perceived as a rotational deformity.
Furthermore, rotation of the little finger at the CMC joint can be accentuated by passive manipulation by the examiner.

FIGURE 67-3 C: Rotation of the little finger at the carpometacarpal joint may be accentuated by passive help.
However, it is critical to note that from a position of normal alignment, true external rotation of the little finger is biomechanically impossible without a structural disruption (fracture or ligamentous tear).

FIGURE 67-3 D: From the normal alignment of the little finger, external rotation is impossible.
Finally, the examiner must ensure that all digits are fully flexed during assessment. Incomplete flexion of the ring finger may simulate a rotational deformity because it naturally tends to overlap the little finger as it descends into the palm.

FIGURE 67-3 E: Incomplete flexion of the ring finger may simulate a rotational deformity because it tends to overlap the little finger.
RADIOGRAPHIC EVALUATION
Accurate radiographic assessment is the cornerstone of preoperative planning. Standard posteroanterior (PA), true lateral, and oblique radiographs of the hand are mandatory. However, the complex overlapping anatomy of the hand often requires specialized views.
- Shaft Fractures: These are best evaluated by multiple images with the bone parallel to the film or image source. To avoid overlap on lateral views, a 10-degree supinated lateral is ideal for the index and middle fingers, while a 10-degree pronated lateral isolates the ring and small fingers.
- Articular Fractures: Fractures involving the interphalangeal or metacarpophalangeal joints may require specific views projecting the joint surfaces perpendicular to the radiation beam (e.g., Brewerton view for metacarpal head fractures).
- Advanced Imaging: Tomograms or Computed Tomography (CT) scans in the sagittal and coronal planes are occasionally necessary to evaluate displacement, especially when a splint or cast obscures fine details. CT is invaluable for preoperative planning of complex intra-articular fractures, such as Rolando fractures or pilon-type fractures of the middle phalanx base.
Surgical Warning: Even when a fracture is being reduced under direct vision in the operating room, intraoperative fluoroscopy is essential. Radiographs can prevent subtle errors in alignment and can reveal small, incarcerated fragments of bone or articular step-offs not appreciated before reduction.
OPEN FRACTURES AND DISLOCATIONS
Open fractures of the hand require urgent evaluation and treatment to prevent deep space infections, osteomyelitis, and devastating stiffness. The principles of the Gustilo-Anderson classification apply, though the robust vascularity of the hand often allows for more aggressive salvage than in the lower extremity.
Irrigation and Débridement
The primary tenet of open fracture management is meticulous surgical débridement. Thorough irrigation with normal saline and the sharp excision of all devitalized soft tissue, skin margins, and contaminated bone fragments are usually adequate for primary fracture treatment.
Antibiotic Stewardship
The routine use of prophylactic antibiotics for fresh, clean, simple open injuries of the hand is a subject of ongoing debate and probably is not strictly necessary if thorough surgical débridement is achieved within a few hours of injury.
However, antibiotic use is absolutely justified and indicated when:
1. Prolonged contamination has occurred (e.g., agricultural injuries, bite wounds).
2. Essential tissues (tendons, neurovascular bundles) have borderline viability.
3. Gross contamination remains despite rigorous irrigation and débridement.
4. The injury involves a human or animal bite (requiring coverage for Eikenella corrodens or Pasteurella multocida, respectively, typically with Amoxicillin-Clavulanate or equivalent intravenous cephalosporins).
BASIC FRACTURE TECHNIQUES
When operative intervention is selected, the surgeon must choose the fixation method that provides adequate stability while minimizing soft tissue trauma. The hand surgeon's armamentarium includes Kirschner wires (K-wires), intraosseous wiring, lag screws, and mini-fragment plates.
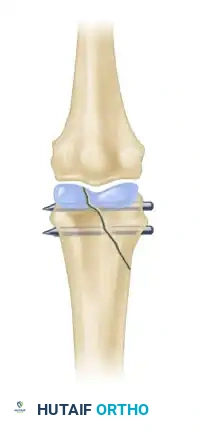
Percutaneous Pinning (K-wires)
K-wire fixation remains the workhorse for many hand fractures, particularly extra-articular phalangeal and metacarpal neck fractures.
* Biomechanics: K-wires provide relative stability. They do not compress the fracture but hold it in alignment while secondary bone healing occurs.
* Technique: Pins can be placed in a crossed configuration or longitudinally. When crossing pins, they must not cross exactly at the fracture site to avoid distracting the fragments. Pins are typically left protruding through the skin for easy removal in the clinic at 3 to 4 weeks, provided rigid clinical union is progressing.
Minicondylar Plate Fixation
For complex periarticular fractures, such as those involving the metacarpal head or the base of the proximal phalanx, minicondylar plates offer rigid fixation.
* Indications: Comminuted intra-articular fractures where K-wires would not provide sufficient stability for early motion.
* Surgical Approach: A dorsal approach is typically utilized. The extensor mechanism must be carefully managed, either by splitting the tendon longitudinally or retracting it laterally, depending on the fracture geometry.
* Advantage: Allows for absolute stability and immediate postoperative active range of motion, which is critical for preventing joint contractures.
Wiring Techniques Applicable to Long Bone Fractures
Intraosseous wiring (e.g., 90-90 wiring or tension band wiring) is highly effective for transverse or short oblique fractures of the phalanges.
* Technique: A combination of a longitudinal K-wire to control bending forces and an intraosseous wire loop to provide compression and control rotation. This technique is low-profile, minimizing irritation to the overlying extensor gliding mechanism.
COMPLICATIONS OF HAND FRACTURES
Despite meticulous care, complications can arise, often due to the severity of the initial trauma or non-compliance with rehabilitation protocols.
Malunion
Malunion occurs when a fracture heals in a non-anatomic position. As discussed, rotational malunion is the most poorly tolerated, leading to digital crossover. Angular malunions (e.g., apex dorsal angulation in metacarpal neck fractures) are better tolerated biomechanically, but excessive angulation can lead to pseudo-clawing and a prominent metacarpal head in the palm. Corrective osteotomies are required for symptomatic malunions.
Nonunion
Nonunion in the hand is relatively rare due to the excellent blood supply, but it can occur in areas of severe bone loss, infection, or inadequate immobilization. Treatment typically requires debridement of the nonunion site, rigid internal fixation (usually with a plate), and autologous bone grafting (often harvested from the distal radius or iliac crest).
Contracture
Joint contracture is the most common complication following hand fractures. It is primarily caused by prolonged immobilization, edema, and tendon adhesions.
* Prevention: The best treatment is prevention. Splinting should always be in the "intrinsic-plus" position (metacarpophalangeal joints flexed to 70-90 degrees, interphalangeal joints fully extended) to maintain the collateral ligaments at their maximal length.
* Rehabilitation: Early, protected active motion is paramount. If severe contractures develop, surgical release (capsulectomy or tenolysis) may be required after fracture consolidation is complete and non-operative therapy has plateaued.
CONCLUSION
The operative management of hand fractures requires a synthesis of biomechanical knowledge, precise clinical examination, and meticulous surgical technique. By adhering to the principles of anatomic reduction—with a hyper-focus on correcting rotational deformities—and utilizing appropriate fixation strategies that allow for early mobilization, the orthopaedic surgeon can reliably restore function and mitigate the risks of debilitating complications.
📚 Medical References
You Might Also Like