Operative Management of Finger Metacarpal Base Fractures and Dislocations
Key Takeaway
Finger metacarpal base fractures and carpometacarpal dislocations are complex injuries frequently missed on initial radiographic evaluation. Proper management requires a thorough understanding of joint biomechanics, particularly the deforming forces of the extensor carpi ulnaris. This guide details evidence-based surgical interventions, including closed reduction with percutaneous pinning and open reduction internal fixation, to restore grip strength, maintain the articular cascade, and prevent debilitating post-traumatic arthrosis.
INTRODUCTION TO FINGER METACARPAL BASE INJURIES
Fractures and fracture-dislocations of the finger metacarpal bases represent a spectrum of complex, high-energy injuries that demand meticulous clinical evaluation and precise surgical execution. The carpometacarpal (CMC) joints of the fingers form a highly specialized articular cascade. The second and third CMC joints are inherently rigid, forming the stable central keystone of the hand's longitudinal and transverse arches. In contrast, the fourth and fifth CMC joints are highly mobile, permitting approximately 15 and 30 degrees of flexion-extension, respectively. This mobility is critical for palmar cupping and power grip.
Because of the dense ligamentous constraints and the overlapping osseous anatomy of the carpus, injuries to this region are notoriously difficult to diagnose on standard radiographs. Failure to recognize and anatomically restore the articular congruity and biomechanical axes of the metacarpal bases inevitably leads to chronic pain, post-traumatic arthrosis, and profound weakness in grip strength.
CARPOMETACARPAL FRACTURE-DISLOCATIONS
Pathoanatomy and Biomechanics
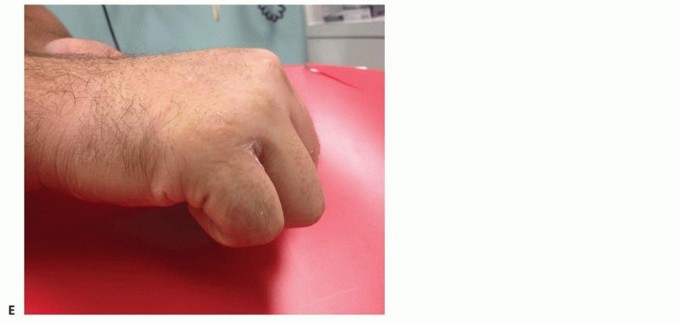
Carpometacarpal fracture-dislocations most frequently result from a direct axial load applied to a flexed metacarpophalangeal (MCP) joint—commonly seen in fist-strike injuries or high-velocity motor vehicle collisions. The fifth metacarpal base is the most commonly involved, typically displacing dorsally due to the unopposed pull of the extensor carpi ulnaris (ECU) tendon. Concomitant involvement of the fourth metacarpal base is highly frequent due to the strong intermetacarpal ligaments tethering the two mobile ulnar rays.
While dorsal dislocations are the most prevalent, volar dislocations can occur, often involving extensive soft-tissue stripping and disruption of the robust volar carpometacarpal ligaments. In severe crush injuries or massive axial loads, all four finger metacarpals may dislocate simultaneously, creating a highly unstable, divergent, or parallel spatulate deformity of the hand.
CLINICAL PEARL:
Always maintain a high index of suspicion for multiple CMC joint involvements. An isolated dislocation of the fourth or fifth CMC joint is rare; the kinetic energy required to dislocate one joint typically propagates through the intermetacarpal ligaments, causing subtle subluxations or fractures in adjacent rays.
Clinical and Radiographic Evaluation
The clinical presentation is often masked by profound dorsal hand swelling, which can obscure the classic "step-off" deformity of a dorsally displaced metacarpal base. Patients will exhibit severe pain with any attempt at active or passive finger motion, particularly during grasp.
Standard posteroanterior (PA), lateral, and oblique radiographs are mandatory, yet they are frequently misinterpreted. On the lateral plain film, the overlapping shadows of the metacarpal bases and the distal carpal row can easily hide a dislocation.
Key Radiographic Indicators:
* True Lateral View: Essential for assessing dorsal or volar translation. The metacarpal shafts should align parallel to the longitudinal axis of the carpus and radius.
* PA View: Evaluate the articular cascade. The loss of parallel joint surfaces (the "M" line of Gilula) at the carpometacarpal articulations is a hallmark sign of subtle subluxation.
* Pronated Oblique View: A 30-degree pronated lateral view profiles the fourth and fifth CMC joints, removing the overlap of the central metacarpals.
SURGICAL WARNING:
Up to 70% of CMC fracture-dislocations are missed on initial presentation in the emergency department. If plain radiographs are equivocal in the setting of disproportionate pain and swelling, a non-contrast Computed Tomography (CT) scan with 3D reconstructions is the gold standard. CT is invaluable for determining the exact extent of articular comminution, identifying impacted fragments, and guiding the surgical approach.
Acute Management: Closed Reduction and Percutaneous Pinning (CRPP)
When the injury is identified acutely (within the first 7–10 days) and lacks severe articular comminution, closed reduction is often easily achieved but rarely maintained without stabilization. The inherent instability necessitates Kirschner wire (K-wire) fixation to prevent redislocation.
CRPP Technique:
1. Positioning and Anesthesia: The procedure is performed under regional or general anesthesia. The patient is positioned supine with the arm on a radiolucent hand table.
2. Reduction Maneuver: Longitudinal traction is applied to the affected digits using finger traps. For dorsal dislocations, direct volar-directed pressure is applied over the prominent metacarpal base while simultaneously extending the metacarpal shaft.
3. Fluoroscopic Verification: Reduction is confirmed in multiple planes using a mini C-arm. The articular spaces must be symmetric and parallel.
4. Pinning Strategy:
* Transarticular Pinning: A 0.045-inch or 0.062-inch K-wire is driven from the dorsal metacarpal shaft, across the CMC joint, and into the corresponding carpal bone (e.g., hamate or capitate).
* Intermetacarpal Pinning: To avoid transfixing the joint and potentially damaging the articular cartilage, pins can be driven transversely from the dislocated metacarpal into the adjacent, stable metacarpal (e.g., pinning the 5th to the 4th, and the 4th to the 3rd).
5. Pin Management: Pins are typically cut outside the skin and capped to facilitate removal in the clinic, though burying them is an option if prolonged fixation is anticipated or patient compliance is a concern.
Open Reduction and Internal Fixation (ORIF)
Open reduction is indicated when closed reduction is unsuccessful, when there is soft-tissue interposition (often the extensor tendons or joint capsule), or when displaced intraarticular fractures require anatomic restoration. ORIF provides excellent long-term results by ensuring anatomic reduction, clearing intraarticular debris, and avoiding the transfixion of tendons and nerves that can occur with percutaneous techniques.
Surgical Approach (Dorsal Longitudinal):
1. Incision: A longitudinal or slightly curvilinear dorsal incision is made over the affected CMC joints. For the 4th and 5th CMC joints, the incision is centered over the intermetacarpal space.
2. Neuroma Prevention: Meticulous blunt dissection is required in the subcutaneous tissues to identify and protect the dorsal sensory branches of the ulnar nerve (DSBUN) and the superficial radial nerve (SRN).
3. Tendon Retraction: The extensor digitorum communis (EDC) and extensor digiti minimi (EDM) tendons are mobilized and retracted.
4. Arthrotomy: A longitudinal arthrotomy is performed. The joint is irrigated, and hematoma or interposed capsule is cleared.
5. Reduction and Fixation:
* The articular surface is visualized directly. Small dental picks or Freer elevators are used to disimpact articular fragments.
* Temporary reduction is held with reduction forceps.
* Fixation is achieved using multiple K-wires, intraosseous wiring, or mini-fragment (1.5 mm or 2.0 mm) plates and screws. Plating is particularly useful for diaphyseal-metaphyseal extensions but must be applied with a low profile to prevent extensor tendon irritation.
6. Closure: The capsule is repaired if possible, followed by standard skin closure.
Management of Late Presentations
When CMC fracture-dislocations are missed and present late (typically >4-6 weeks), the deformity is fixed, and the articular cartilage is often irreparably damaged.
Salvage Procedures:
* Open Reduction and Ligament Reconstruction: Attempted in younger patients with preserved cartilage, though technically demanding due to contractures.
* CMC Arthrodesis: The treatment of choice for chronic, painful dislocations of the 2nd and 3rd CMC joints.
* Resection Arthroplasty or Fusion: For the 4th and 5th CMC joints, preserving motion is ideal. However, if the proximal end of the metacarpal is severely deformed, it must be resected. The joint is then treated by either interposition arthroplasty (using a slip of the ECU or palmaris longus) to maintain mobility, or formal fusion if stability is prioritized over motion.
INTRAARTICULAR FRACTURE OF THE FIFTH METACARPAL BASE
The "Reverse Bennett" Fracture
Bora and Didizian brought critical attention to a specific, potentially disabling intraarticular fracture at the base of the fifth metacarpal. Often referred to as the "Reverse Bennett" or "Baby Bennett" fracture, this injury shares identical biomechanical principles with the classic Bennett fracture of the thumb base.
Anatomy and Deforming Forces:
The fifth CMC joint consists of the fifth metacarpal base articulating proximally with the hamate and radially with the adjoining fourth metacarpal. This joint permits approximately 30 degrees of normal flexion and extension, alongside the crucial rotation necessary for grasp and palmar cupping.
The extensor carpi ulnaris (ECU) tendon inserts robustly onto the dorsal-ulnar tubercle of the fifth metacarpal base. When an intraarticular fracture separates the main shaft from the volar-radial articular fragment, the biomechanics are drastically altered:
1. The volar-radial fragment remains anatomically secured to the fourth metacarpal and the hamate via the strong intermetacarpal and volar ligaments.
2. The ECU tendon exerts a massive, unopposed proximal and dorsal pull on the metacarpal shaft.
3. This results in proximal migration, dorsal subluxation, and shortening of the fifth ray.
PITFALL:
If this injury is treated non-operatively without achieving and maintaining anatomic reduction, the resulting malunion will lead to a loss of the articular cascade. The patient will suffer from profound weakness of grip, a painful CMC joint, and early-onset osteoarthritis due to altered contact mechanics on the hamate.
Surgical Management of the Fifth Metacarpal Base
Surgical intervention is strictly indicated for articular step-offs greater than 1 to 2 mm, or any degree of dorsal subluxation of the metacarpal shaft.
Closed Reduction and Percutaneous Pinning:
For acute injuries with large, non-comminuted fragments, CRPP is highly effective.
1. Reduction: The surgeon must counteract the ECU. Longitudinal traction is applied, followed by pronation of the fifth metacarpal and direct volar pressure over the dorsal metacarpal base.
2. Fixation: While holding the reduction, a K-wire is driven transversely from the fifth metacarpal shaft into the fourth metacarpal shaft. A second pin is often driven from the fifth metacarpal into the hamate or capitate to neutralize the proximal pull of the ECU.
3. Verification: True lateral and pronated oblique fluoroscopic views must confirm that the articular step-off is eliminated and the shaft is no longer subluxated.
Open Reduction and Internal Fixation:
If closed reduction fails to restore articular congruity, ORIF is mandatory.
1. Approach: A dorsal-ulnar incision is utilized. The dorsal sensory branch of the ulnar nerve is at high risk here and must be meticulously protected.
2. Exposure: The ECU tendon is identified and retracted ulnar-ward. The joint capsule is opened to expose the fracture site.
3. Fixation Strategy:
* Lag Screw Fixation: If the volar-radial fragment is large enough, a 1.5 mm or 2.0 mm lag screw can be placed from dorsal-ulnar to volar-radial, compressing the fracture.
* Mini-Fragment Plating: For comminuted fractures or those with diaphyseal extension, a dorsal or ulnar-based mini-fragment plate (e.g., a T-plate or condylar plate) acts as a buttress against the dorsal subluxation forces of the ECU.
* K-wire Supplementation: Even with rigid internal fixation, temporary transarticular pinning to the hamate may be utilized for 3-4 weeks to protect the repair from the powerful pull of the ECU during early healing.
POSTOPERATIVE PROTOCOLS AND REHABILITATION
The ultimate success of metacarpal base surgery relies heavily on a structured, evidence-based postoperative rehabilitation protocol.
Phase 1: Immobilization (Weeks 0-4)
* Postoperatively, the hand is placed in a bulky soft dressing reinforced with a volar and dorsal plaster splint.
* Within 3 to 5 days, this is transitioned to a custom-molded thermoplastic ulnar gutter splint (for 4th/5th ray injuries) or a radial gutter splint (for 2nd/3rd ray injuries). The wrist is positioned in 20-30 degrees of extension, with the MCP joints free if the injury allows, or immobilized in 70 degrees of flexion if diaphyseal stability is a concern.
* Active range of motion (AROM) of the interphalangeal joints is encouraged immediately to prevent extensor tendon adhesions.
Phase 2: Pin Removal and Early Motion (Weeks 4-6)
* If percutaneous K-wires were utilized, they are typically removed in the clinic at 4 to 6 weeks, contingent upon radiographic evidence of early callus formation and clinical stability.
* Once pins are removed, active and active-assisted range of motion of the wrist and CMC joints is initiated.
* The splint is worn between exercise sessions and at night.
Phase 3: Strengthening (Weeks 6-12)
* Progressive strengthening begins at 6 weeks. Putty exercises, grip strengthening, and dynamic flexion/extension exercises are introduced.
* Patients must be counseled that maximal grip strength and complete resolution of edema may take up to 6 to 12 months.
Complications:
Surgeons must monitor for complications, including pin-tract infections, complex regional pain syndrome (CRPS), and hardware prominence. Extensor tendon irritation is common with dorsal plating; if tenosynovitis develops and persists after fracture union, hardware removal and tenolysis may be required at 6 to 9 months postoperatively.
===
You Might Also Like