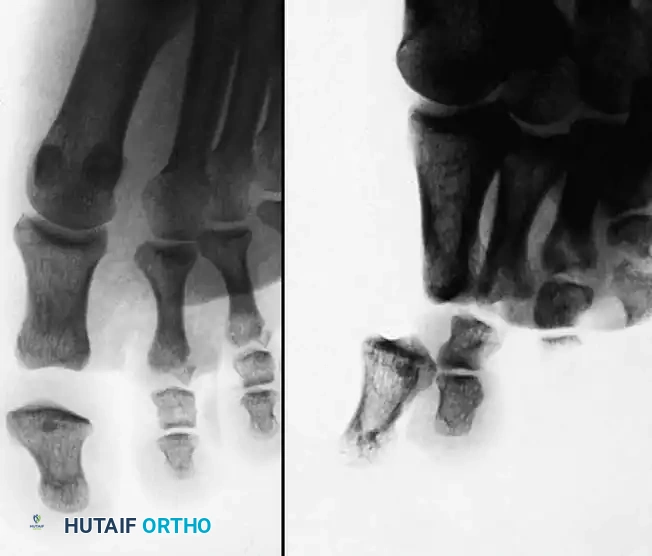
Dynamic External Splint Reduction for Proximal Interphalangeal Joint Fracture-Subluxations
Key Takeaway
The dynamic external splint, notably the Agee force-couple device, is a highly effective treatment for unstable proximal interphalangeal (PIP) joint fracture-subluxations. By coupling longitudinal distraction with volarly directed forces, this technique restores concentric joint reduction while permitting immediate active range of motion. This approach mitigates joint stiffness, prevents secondary traumatic arthritis, and optimizes functional outcomes in both acute and chronic PIP joint injuries.
Introduction to Dynamic External Splint Reduction
Fracture-subluxations and fracture-dislocations of the proximal interphalangeal (PIP) joint represent some of the most challenging intra-articular injuries managed by hand and orthopedic surgeons. These injuries typically involve a shear or impaction fracture of the volar base of the middle phalanx, accompanied by dorsal subluxation of the remaining intact middle phalanx base. When the articular defect exceeds 30% to 40% of the joint surface, the collateral ligament complex and volar plate are compromised, rendering the joint highly unstable and prone to recurrent dorsal subluxation.
To address this instability without sacrificing joint mobility, dynamic external splint reduction—most notably the Agee force-couple technique—has become a cornerstone of operative management. Several different methods are commonly used to achieve reduction of PIP joint fracture-subluxations, but they all rely on a shared biomechanical principle: coupling longitudinal distraction with volarly directed forces across the joint.
Common to most of these devices is the achievement of a distraction force through Kirschner wires (K-wires) placed precisely through the rotation axes of the proximal interphalangeal (PIP) and distal interphalangeal (DIP) joints. The method by which the volarly directed forces are achieved differs according to the chosen technique, but the ultimate goal remains identical: to maintain concentric joint reduction during bone and soft tissue healing while theoretically minimizing joint stiffness by allowing immediate active range-of-motion (ROM) exercises.
Biomechanical Principles of the Force-Couple
Understanding the biomechanics of the PIP joint is critical for the successful application of a dynamic external splint. The PIP joint is a ginglymus (hinge) joint with a bicondylar proximal phalanx head articulating with the biconcave base of the middle phalanx.
In a dorsal fracture-dislocation, the volar lip of the middle phalanx is fractured. The central slip of the extensor tendon and the lateral bands exert an unopposed dorsal and proximal pull on the intact dorsal base of the middle phalanx, causing it to subluxate dorsally over the condyles of the proximal phalanx.
The Agee force-couple splint counteracts these deforming forces through a mechanical linkage:
1. Longitudinal Distraction: Achieved by the rubber band tension connecting the proximal and distal K-wires, which unloads the articular surface and utilizes ligamentotaxis to partially reduce the volar fracture fragments.
2. Volar Translation: The mechanical linkage is designed so that the tension of the rubber band creates a volar vector on the middle phalanx, actively resisting the dorsal pull of the extensor mechanism.
💡 Clinical Pearl: The Importance of Concentric Reduction
A successful dynamic external splint must achieve a "parallel gliding motion" of the middle phalanx on the proximal phalanx. A "rocking motion" indicates a non-concentric hinge, which predisposes the joint to high focal surface pressures, rapid cartilage necrosis, secondary traumatic arthritis, and recurrent joint subluxation.
Indications and Contraindications
Indications
- Acute dorsal fracture-subluxations of the PIP joint with >30% articular involvement.
- Injuries that are unstable after closed reduction and dorsal block splinting.
- Comminuted pilon-type fractures of the middle phalanx base where internal fixation is impossible.
- Chronic dorsal fracture-subluxations (often requiring an open approach).
Contraindications
- Volar fracture-dislocations: The force-couple generates a volar vector, which would exacerbate a volar dislocation.
- Severe Collateral Ligament Deficiency: If the collateral ligaments are completely destroyed and cannot be repaired or maintained, the dynamic splint will convert a dorsal dislocation into an iatrogenic palmar dislocation.
- Non-compliant patients: The success of this device relies heavily on the patient's ability to perform active ROM exercises and maintain pin site hygiene.
Preoperative Planning and Setup
Meticulous preoperative planning is required. True anteroposterior (AP) and true lateral radiographs of the affected digit are mandatory to assess the size of the volar fragment, the degree of comminution, and the extent of dorsal subluxation.
For acute injuries where closed reduction is anticipated, the procedure is preferably performed under a digital block anesthesia. This is a critical strategic choice: a digital block provides excellent anesthesia while preserving the extrinsic flexor and extensor muscle function, allowing the patient to demonstrate the joint’s active range of motion intraoperatively.
For chronic injuries requiring open reduction and extensive soft tissue releases, an axillary block or regional anesthesia is preferred to ensure complete patient comfort and a bloodless field via a pneumatic tourniquet.
Surgical Technique: Closed Percutaneous Application (Acute Injuries)
When closed reduction is possible, the force-couple splint is applied percutaneously. The precision of K-wire placement is the most critical step of the procedure.
Step 1: Axis Identification and Pin Placement
- Under fluoroscopic guidance, obtain a perfect true lateral view of the PIP joint. The condyles of the proximal phalanx must perfectly overlap, appearing as a single concentric circle.
- Insert a smooth K-wire (typically 0.045-inch) exactly through the center of rotation of the proximal phalanx head.
- Repeat this process for the DIP joint, inserting a second smooth K-wire through the center of rotation of the middle phalanx head.
Step 2: Mechanical Linkage Assembly
- Bend the K-wires at 90-degree angles at an equal distance from the skin on both sides of the digit to form the mechanical linkage.
- Adjust the smooth K-wire limbs of the device as needed to keep them perfectly centered on the finger.
- Crucial Step: Ensure there is adequate clearance between the wire linkage and the skin throughout the entire arc of motion to avoid pressure necrosis.
Step 3: Applying the Force-Couple
- Place a small rubber band across the linkage hooks.
- Apply tension adequate to maintain reduction.
- Avoid excessive tension: Over-distraction will lead to joint stiffness, non-union of the fracture fragments, and severe pain. The tension should be just enough to counteract the dorsal subluxation.
Step 4: Intraoperative Dynamic Assessment
- Ask the patient (under digital block) to actively flex and extend the finger.
- Determine the quality of joint reduction with AP and lateral radiographs of the joint in both the flexed and extended positions.
- Examine the flexion and extension lateral radiographs closely to ensure that the intact dorsal base of the middle phalanx is concentrically reduced. Look for the parallel gliding motion with respect to the head of the proximal phalanx.
⚠️ Surgical Warning: The "Rocking" Joint
If fluoroscopy reveals a rocking motion of the middle phalanx on the proximal phalanx, the pins are likely not in the true axis of rotation, or the rubber band tension is incorrect. This must be corrected immediately. Leaving a joint to "rock" guarantees early failure and severe traumatic arthritis.
Surgical Technique: Open Reduction (Chronic or Complex Injuries)
In chronic injuries (typically presenting >3-4 weeks post-injury), closed reduction is usually impossible due to soft tissue contracture, fracture callus, and fibrosis. Open reduction is required.
Step 1: Surgical Approach
- With the patient under axillary block anesthesia, utilize a midlateral incision on the most affected side of the digit.
- Carefully protect the neurovascular bundle, retracting it volarly.
- Identify and divide the lateral retinacular ligament to expose the collateral ligament complex.
Step 2: Soft Tissue Releases
- Divide the dorsal part of the collateral ligament and the adjacent joint capsule to mobilize the joint.
- Frequently, the dorsal side of the opposite collateral ligament must also be divided. This is typically done through a separate, smaller midlateral incision on the contralateral side of the digit to avoid excessive soft tissue stripping.
Step 3: Joint Preparation and Fragment Mobilization
- Use a blunt probe to free the palmar side of the joint, clearing out fibrotic tissue and organizing hematoma.
- Use a small, sharp osteotome to carefully mobilize the avulsed fracture fragment from the palmar base of the middle phalanx. Preserve any soft tissue attachments (volar plate) to this fragment to maintain its blood supply.
🛑 Pitfall: Collateral Ligament Incompetence
Evaluate the remaining collateral ligaments carefully. If portions of the collateral ligaments necessary for adequate stability cannot be maintained, the dynamic splint cannot be used. Without collateral ligament restraint, the volar vector of the force-couple will simply convert the dorsal dislocation into an iatrogenic palmar dislocation. In such cases, alternative treatments (e.g., volar plate arthroplasty, hemi-hamate autograft, or joint fusion) must be considered.
Step 4: Frame Application and Closure
- With adequate reduction of the intact dorsal base of the middle phalanx with respect to the proximal phalanx condyles achieved manually, apply the force-couple splint as described in the closed technique.
- Allow the smooth transverse K-wires to exit directly through the surgical incision if necessary, though separate percutaneous stab incisions are preferred if anatomy allows.
- If possible, repair the soft tissues and the volar plate.
- After meticulous hemostasis, repair the skin appropriately using non-absorbable sutures.
- Obtain final radiographs in AP, lateral extension, and lateral flexion views to evaluate the adequacy of joint reduction.
Postoperative Protocol and Rehabilitation
The primary advantage of the dynamic external splint is the facilitation of early active motion, which enhances cartilage nutrition, prevents tendon adhesions, and molds the healing fracture callus.
Immediate Postoperative Care (Days 1-2)
- Apply a soft, bulky dressing to the finger to manage postoperative edema.
- The dressing should be worn for 1 or 2 days.
- Elevation of the hand is strictly enforced to minimize swelling.
Early Rehabilitation (Days 3 to Week 5)
- Remove all restrictive dressings.
- To permit active range-of-motion exercises, no dressing is used. Instead, an antibiotic ointment is applied daily to the pin sites to prevent superficial infection.
- The patient is instructed to perform active flexion and extension exercises of the PIP and DIP joints multiple times an hour.
- Adjust the smooth K-wire limbs of the device as needed during clinic visits to keep them centered on the finger, strictly avoiding pressure on the skin.
- Obtain interval radiographs weekly for the first 3 weeks to ensure concentric reduction is maintained and to monitor bone and soft tissue healing.
Device Removal (Weeks 5 to 8)
- The device is maintained for a minimum of 5 weeks.
- Injuries with advancing degrees of comminution and severe instability require the frame to be left in place for 6 to 8 weeks.
- Once bone and soft tissue healing is judged to be adequate clinically and radiographically, the effect of the force couple is removed by detaching the rubber band in the clinic.
- Critical Step: Obtain flexion-extension lateral radiographs without the rubber band tension to confirm intrinsic joint stability before removing the K-wires.
- If the joint remains concentrically reduced without the rubber band, the K-wires are pulled in the clinic.
Complications and Management
While highly effective, dynamic external splinting carries specific risks that the surgeon must proactively manage:
- Pin Tract Infection: The most common complication. Managed with daily pin site care (antibiotic ointment or chlorhexidine). Superficial infections usually resolve with oral antibiotics. Deep infections require immediate pin removal.
- Over-Distraction: Excessive rubber band tension leads to a widened joint space, preventing fracture union and causing severe stiffness. Tension must be calibrated to just maintain reduction.
- Loss of Reduction / Palmar Subluxation: Usually caused by unrecognized collateral ligament incompetence or incorrect pin placement (axis of rotation missed). Requires immediate frame adjustment or conversion to an alternative surgical strategy.
- Pin Impingement: If the K-wires are not bent with adequate clearance, the skin will undergo pressure necrosis during flexion. The surgeon must manually bend the wires outward if swelling increases.
Conclusion
Dynamic external splint reduction utilizing the force-couple principle remains an elegant, biomechanically sound solution for complex PIP joint fracture-subluxations. By neutralizing the deforming forces of the extensor mechanism and restoring concentric joint kinematics, this technique allows for immediate active rehabilitation. Whether applied percutaneously in acute settings or combined with open soft-tissue releases in chronic presentations, meticulous attention to the axis of rotation, appropriate rubber band tension, and rigorous postoperative pin care are paramount to achieving optimal functional outcomes and preventing long-term disability.
You Might Also Like