Orthopedic Management of Bisphosphonate Complications: MRONJ & Atypical Femoral Fractures
Key Takeaway
Bisphosphonate therapy can lead to two primary orthopedic complications: Medication-Related Osteonecrosis of the Jaw (MRONJ), characterized by exposed jaw bone, and Atypical Femoral Fractures (AFFs), transverse fractures in the femur. Both involve impaired bone remodeling and specific anatomical vulnerabilities, necessitating careful patient monitoring and multidisciplinary management.
Introduction & Epidemiology
Bisphosphonates (BPs) are widely prescribed antiresorptive agents primarily utilized in the management of osteoporosis, Paget's disease, and malignancy-associated hypercalcemia or skeletal-related events. Their mechanism of action involves binding to hydroxyapatite crystals in bone, inhibiting osteoclast activity, thereby reducing bone resorption and increasing bone mineral density. While highly effective in preventing fragility fractures, prolonged bisphosphonate therapy is associated with two distinct and significant orthopedic complications: medication-related osteonecrosis of the jaw (MRONJ) and atypical femoral fractures (AFFs). Understanding the epidemiology and pathophysiological underpinnings of these entities is crucial for comprehensive orthopedic practice.
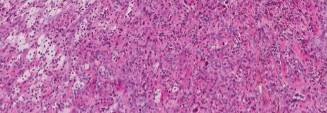
MRONJ is characterized by exposed bone in the maxillofacial region that persists for more than eight weeks in a patient with a history of bisphosphonate exposure, without prior radiation therapy to the jaw. Its incidence varies significantly based on the BP potency, route of administration, duration of therapy, and underlying patient comorbidities. The incidence in oral BP users for osteoporosis is generally low, estimated to be between 0.001% and 0.01% per patient-year. However, in patients receiving high-dose intravenous BPs for malignancy, the incidence can be substantially higher, ranging from 1% to 15%. Risk factors include prolonged BP use (>2 years), concurrent corticosteroid therapy, diabetes, smoking, poor oral hygiene, and local trauma such as dental extractions or implant placement.
Atypical femoral fractures are defined by specific radiographic features: a transverse or short oblique fracture line originating from the lateral cortex, often associated with generalized cortical thickening and a periosteal stress reaction. These fractures occur in the subtrochanteric region or femoral diaphysis, typically without significant trauma. The incidence of AFFs in patients on long-term bisphosphonate therapy for osteoporosis is rare, estimated at 3.2 to 50 per 100,000 patient-years, but significantly higher than in the general population. The risk increases with longer duration of BP use (particularly >5 years) and tends to decrease after discontinuation. Other risk factors include Asian ethnicity, lower body mass index, and specific anatomical variants. AFFs frequently present with prodromal thigh or groin pain, representing a stress reaction preceding a complete fracture. They are often bilateral, with a reported incidence of contralateral involvement ranging from 20% to 50%.
Both MRONJ and AFFs pose considerable management challenges, necessitating a multidisciplinary approach and a thorough understanding of their surgical implications for orthopedic surgeons, oral and maxillofacial surgeons, endocrinologists, and rheumatologists.
Surgical Anatomy & Biomechanics
For Medication-Related Osteonecrosis of the Jaw (MRONJ)
The unique anatomical and biomechanical characteristics of the jaw contribute significantly to the pathogenesis and clinical presentation of MRONJ.
*
Jaw Anatomy:
The mandible, due to its dense cortical bone, limited collateral blood supply compared to other skeletal sites, and constant exposure to masticatory forces and the oral microbiome, is more frequently affected by MRONJ than the maxilla (ratio typically 2:1). The maxilla, with its more porous bone and richer vascularity, appears less susceptible. The alveolar bone, which supports the dentition, is particularly vulnerable due to its rapid remodeling rate and proximity to potential entry points for infection (e.g., periodontal pockets, extraction sites).
*
Vascularity:
The primary blood supply to the mandible is via the inferior alveolar artery, a branch of the maxillary artery. The maxilla receives blood from several branches of the maxillary artery, including the greater palatine, posterior superior alveolar, and infraorbital arteries. While these vessels provide robust supply in healthy individuals, the relative end-arterial nature of the alveolar bone's microcirculation, especially in the posterior mandible, may contribute to susceptibility. Bisphosphonates may compromise microvascular integrity, further impairing oxygen and nutrient delivery to the bone.
*
Pathophysiology:
The precise pathophysiology of MRONJ is multifactorial, involving a complex interplay of impaired bone remodeling, anti-angiogenic effects, local inflammation/infection, and reduced host defense mechanisms. Bisphosphonates profoundly suppress osteoclast-mediated bone resorption, leading to a decrease in bone turnover. This suppression prevents the timely removal of microdamage and necrotic bone, resulting in the accumulation of brittle, hypermineralized bone. Reduced angiogenesis, particularly relevant in the high-dose intravenous BP setting, contributes to impaired healing. Local trauma (e.g., dental extractions, ill-fitting dentures) acts as a trigger by exposing compromised bone to the oral environment, leading to bacterial colonization and chronic infection, which further exacerbates the osteonecrotic process.
For Atypical Femoral Fractures (AFFs)
The unique mechanical environment and bone biology of the femur are central to the development of AFFs.
*
Femoral Anatomy:
AFFs typically occur in the subtrochanteric region or the femoral diaphysis, areas subjected to significant bending and torsional stresses during locomotion. The lateral cortex of the femur, being under tension during gait, is the site where stress risers and crack initiation often occur. Radiographically, AFFs are characterized by a transverse or short oblique fracture line, often with a medial cortical spike. Associated cortical thickening, particularly along the lateral aspect, represents a maladaptive response to accumulated microdamage.
*
Biomechanics:
Normal bone remodeling involves a continuous process of microdamage detection, osteoclastic resorption, and osteoblastic new bone formation. This allows bone to repair microcracks and adapt to mechanical loads. Bisphosphonates inhibit osteoclast activity, leading to a profound suppression of bone turnover. While this increases bone mineral density, it also impairs the removal of accumulated microdamage, particularly in cortical bone. This results in an accumulation of brittle, hypermineralized bone that has reduced fatigue life and propagation resistance. The bone becomes stiffer but less tough.
*
Fracture Pattern:
The classic transverse fracture pattern observed in AFFs is consistent with a fatigue fracture occurring in brittle material. The prodromal pain represents a stress fracture or impending complete fracture. The lateral cortical thickening and periosteal reaction are morphological hallmarks of a chronic stress response in bone unable to remodel effectively. The medial spike often observed is theorized to be related to the eccentric loading of the femur and the crack propagating from lateral to medial.
Indications & Contraindications
The management of bisphosphonate-related complications requires careful consideration of surgical versus non-operative strategies, often guided by disease severity and patient factors.
For Medication-Related Osteonecrosis of the Jaw (MRONJ)
The American Association of Oral and Maxillofacial Surgeons (AAOMS) staging system provides a framework for guiding management:
-
Non-Operative Indications:
- Stage 0: No clinical evidence of necrotic bone, but non-specific symptoms such as pain, odontalgia, or altered sensation in the jaw. Management is entirely conservative, focusing on pain control, antibiotics, and addressing underlying dental issues. Discontinuation of BP is generally not recommended at this stage unless symptoms are refractory.
- Stage 1: Exposed and necrotic bone in the maxillofacial region, but the patient is asymptomatic and shows no evidence of infection. Management involves daily antimicrobial mouth rinses (e.g., chlorhexidine), systemic antibiotics (if infection risk is high), pain control, and regular follow-up. Conservative debridement of superficial, mobile bone spicules may be performed to prevent soft tissue irritation, but aggressive surgical intervention is typically avoided. BP holiday is generally not indicated at this stage unless symptoms worsen or progression occurs.
-
Operative Indications:
- Stage 2: Exposed and necrotic bone with associated infection (pain, erythema, swelling, purulent discharge). Surgical debridement or sequestrectomy is indicated to remove the infected necrotic bone, establish healthy bleeding margins, and allow for tension-free primary soft tissue closure. This aims to eliminate infection, reduce pain, and prevent progression. Prior to surgery, a 3-month bisphosphonate holiday is often recommended, though evidence for its efficacy in improving outcomes is limited and debated.
- Stage 3: Exposed and necrotic bone with pain, infection, and at least one of the following: pathologic fracture, extraoral fistula, or osteolysis extending to the inferior border of the mandible or the sinus floor. This stage often requires more extensive surgical intervention, potentially including segmental resection of the mandible or maxilla with microvascular free flap reconstruction for large defects to restore form and function. Prolonged antibiotic therapy, nutritional support, and careful pre-operative planning are paramount.
-
Contraindications for MRONJ Surgery:
- Uncontrolled systemic comorbidities (e.g., severe uncontrolled diabetes, severe coagulopathy).
- Active oral infection not managed by initial antibiotic therapy.
- Patient refusal or inability to comply with post-operative care.
- Small, asymptomatic, non-infected areas of exposed bone (Stage 1) where conservative measures are effective.
For Atypical Femoral Fractures (AFFs)
Management decisions for AFFs revolve around the presence of a complete fracture versus an incomplete stress fracture.
-
Non-Operative Indications:
- Prodromal Pain with Incomplete Fracture (Limited Evidence): In rare instances, patients presenting with prodromal thigh or groin pain, and radiographic evidence of an incomplete AFF (e.g., lateral cortical thickening or stress line without a clear fracture line extending across the cortex) may be managed non-operatively. This requires strict non-weight-bearing, immediate bisphosphonate holiday, supplementation with calcium and Vitamin D, and close radiographic monitoring. This approach is highly controversial and generally reserved for specific, low-risk cases with excellent patient compliance, as the risk of progression to a complete fracture is significant. Most orthopedic surgeons advocate for prophylactic fixation in high-risk incomplete AFFs.
-
Operative Indications:
-
Prophylactic Fixation (Incomplete AFFs):
Prophylactic intramedullary nailing is strongly indicated for incomplete AFFs demonstrating specific high-risk features:
- Fracture line extending more than 25% across the femoral cortex from the lateral side.
- Persistent prodromal pain unresponsive to conservative measures and BP holiday for 2-3 months.
- Contralateral complete or incomplete AFF.
- Significant lateral cortical thickening (>9mm) or a visible "beaking" or stress line.
- Patients with significant risk factors for progression (e.g., continued BP exposure, poor compliance).
- Inability to comply with non-weight-bearing restrictions.
- Fixation of Complete AFFs: All complete AFFs (transverse or short oblique fractures extending across both cortices) require immediate surgical stabilization, typically with an intramedullary nail. Delay increases the risk of comminution and displacement.
-
Prophylactic Fixation (Incomplete AFFs):
Prophylactic intramedullary nailing is strongly indicated for incomplete AFFs demonstrating specific high-risk features:
-
Contraindications for AFF Surgery:
- No absolute contraindications other than the patient being too medically frail to tolerate anesthesia and surgery. In such cases, conservative management might be considered, but carries an extremely high risk of morbidity and mortality due to bed rest complications and pain.
Table: Operative vs. Non-Operative Indications for BP-Related Complications
| Complication | Non-Operative Indications | Operative Indications |
|---|---|---|
| MRONJ | Stage 0 (no exposed bone, symptoms only), Stage 1 (exposed bone, asymptomatic) | Stage 2 (exposed bone, symptomatic, infection), Stage 3 (pathologic fracture, fistula, extensive osteolysis) |
| AFF | Prodromal pain with incomplete fracture (rare, selected cases, strict monitoring) | Prophylactic (incomplete with high-risk features, e.g., fracture line >25% width, persistent pain), Complete fracture (all) |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is paramount for optimizing outcomes and minimizing complications in patients with bisphosphonate-related pathology, which often presents with compromised bone quality and complex biological issues.
General Considerations for BP-related Complications:
- Bisphosphonate Holiday: The decision to discontinue bisphosphonates pre-operatively is complex. For MRONJ, a 3-month BP holiday before elective jaw surgery (e.g., dental extraction or extensive debridement) is often suggested, though its efficacy in improving healing is not definitively proven and must be weighed against the risk of rebound bone loss. For AFFs, an immediate BP holiday is universally recommended upon diagnosis of a stress reaction or complete fracture, but surgery should not be delayed waiting for bone biology to improve.
- Systemic Optimization: Nutritional status, particularly vitamin D and calcium levels, should be optimized. Many patients on BPs have underlying osteoporosis and may be vitamin D deficient. Anemia, diabetes, and other comorbidities should be controlled. Smoking cessation is strongly encouraged.
- Infection Prophylaxis: Standard surgical prophylactic antibiotics are administered. For MRONJ, prolonged oral antibiotic regimens may be initiated pre-operatively, especially in Stage 2 or 3 disease.
For MRONJ Surgery:
-
Imaging:
- Panoramic Radiograph (Panorex): Initial screening, identifying areas of exposed bone, sequestra, or radiolucent/sclerotic changes.
- Computed Tomography (CT) Scan with 3D Reconstruction: Essential for defining the extent of necrotic bone, identifying cortical perforations, pathologic fractures, and planning resection margins. Cone-beam CT (CBCT) provides high-resolution imaging with lower radiation dose.
- MRI: May be useful in differentiating soft tissue inflammation from osteonecrosis, particularly in Stage 0 cases.
- Dental/Oral & Maxillofacial Surgery Consultation: Mandatory for comprehensive assessment, extraction planning, dental hygiene optimization, and determining appropriate surgical margins.
- Positioning: Patient is typically supine with the head secured in a neutral or slightly extended position. An oral retractor system may be used to provide optimal access. Consideration for possible submandibular or submental incision if extraoral access is required for extensive debridement or reconstruction.
For AFF Surgery:
-
Imaging:
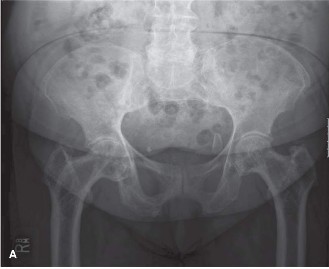
- Plain Radiographs: Anteropoposterior (AP) and lateral views of the entire affected femur (including hip and knee) are critical for assessing fracture morphology, location, and extent of cortical thickening. Crucially, AP pelvis and full-length femur radiographs of the contralateral limb are mandatory to identify bilateral stress reactions or occult AFFs.
- CT Scan: Useful for subtle incomplete fractures or to define the extent of cortical thickening and marrow changes.
- MRI: The gold standard for detecting early stress reactions or incomplete AFFs not visible on plain radiographs, especially in patients with prodromal pain.
- Pre-operative Templating: Essential for selecting the appropriate intramedullary nail length, diameter, and curvature. AFFs often occur in relatively straight femurs; a nail with too much bow may cause iatrogenic fracture.
-
Patient Positioning:
- Supine on a Fracture Table: Most common approach for standard antegrade femoral nailing. Allows for traction, rotation control, and fluoroscopic access. Requires careful perineal post padding.
- Lateral Decubitus Position: An alternative for certain nailing techniques, offering improved access to the greater trochanter and piriformis fossa for entry point. Can be cumbersome for fluoroscopy.
- Radiolucent Table (Supine): May be used for patients unable to tolerate a fracture table, but requires assistants to maintain reduction and traction.
- Surgical Team Preparation: Ensure availability of a full range of intramedullary nails, reamers, and locking options. Consider bone grafting materials if nonunion risk is high.
Detailed Surgical Approach / Technique
Surgical intervention for bisphosphonate-related complications requires precise execution, acknowledging the unique bone pathology.
For MRONJ (Surgical Debridement/Sequestrectomy):
The goal is to remove necrotic bone, achieve healthy bleeding margins, and allow for tension-free primary closure, minimizing further exposure.
*
Anesthesia:
General endotracheal anesthesia is preferred, with nasal intubation if extensive oral access is needed.
*
Incision and Flap Design:
An intraoral mucoperiosteal flap is meticulously designed, ensuring wide access and preservation of soft tissue vascularity. Incisions should be made over healthy bone, away from the necrotic margins. Releasing incisions may be necessary. For mandibular involvement, care must be taken to avoid injury to the mental nerve.
*
Debridement and Sequestrectomy:
The necrotic bone (sequestrum) is carefully identified and sharply removed using osteotomes, burs, or rongeurs. Debridement continues until healthy, bleeding bone is encountered at all margins. The bone should feel firm and vital. Excessive removal of healthy bone is avoided to preserve jaw integrity.
*
Irrigation:
Copious pulsatile lavage with saline and antiseptic solutions (e.g., povidone-iodine or chlorhexidine) is performed to remove debris and reduce bacterial load.
*
Closure:
Achieving tension-free, multi-layer primary soft tissue closure is critical to prevent re-exposure of bone. Adjacent soft tissue flaps (e.g., buccal fat pad, local mucoperiosteal flaps) may be utilized to achieve closure in larger defects.
*
Adjuvant Therapies:
Platelet-rich plasma (PRP) or platelet-rich fibrin (PRF) may be applied locally to promote soft tissue healing, though evidence for improved bone healing is mixed. Hyperbaric oxygen therapy is controversial and not routinely recommended.
For AFF (Intramedullary Nailing):
Intramedullary nailing is the standard of care for complete AFFs and prophylactic fixation of high-risk incomplete AFFs.
*
Patient Positioning and Draping:
As described in pre-operative planning. Ensure adequate fluoroscopic access for AP and lateral views of the entire femur, including hip and knee.
*
Incision and Entry Point:
A standard paratrochanteric or piriformis fossa approach is used. The entry point is crucial for achieving proper alignment and preventing iatrogenic comminution. For subtrochanteric AFFs, the entry point is typically slightly medial to the tip of the greater trochanter, in line with the femoral shaft. For diaphyseal AFFs, a slightly more lateral entry point may be needed. Use an awl to create the entry hole, ensuring it is in line with the medullary canal.
*
Reaming:
Gradual, sequential reaming is performed, typically 1.5-2 mm over the selected nail diameter. Careful, slow reaming is essential to prevent heat necrosis of the already compromised bone and minimize the risk of iatrogenic fracture propagation, especially through the cortical thickening associated with AFFs. Irrigation during reaming can help reduce heat.
*
Nail Insertion:
The appropriately sized intramedullary nail is gently and slowly inserted. Avoid forceful impaction. Monitor closely with fluoroscopy to ensure proper trajectory and prevent cortical violation or further fracture propagation. For complete fractures, ensure adequate reduction before final impaction.
*
Locking Screws:
Proximal and distal interlocking screws are placed under fluoroscopic guidance. Static locking is preferred to maintain length and rotation. The often-dense cortical bone in AFFs may require more forceful drilling for screw insertion.
*
Adjunctive Procedures:
*
Bone Grafting:
For delayed unions or nonunions, or for prophylactic cases where bone quality is severely compromised, autogenous bone graft (e.g., iliac crest) or allograft may be utilized to promote healing.
*
Plate Augmentation:
In specific instances of severe comminution or persistent nonunion, supplemental plating (e.g., a locking plate) may be considered, although this is generally a salvage procedure.
*
Contralateral Prophylaxis:
Given the high bilateral incidence of AFFs, a low threshold for prophylactic nailing of the asymptomatic contralateral femur with high-risk features should be maintained. This can be performed during the same surgical setting or as a staged procedure.
Complications & Management
Both MRONJ and AFFs, along with their surgical management, are associated with distinct sets of complications that require prompt recognition and tailored strategies.
For MRONJ Surgery:
-
Recurrence:
Despite successful debridement and closure, MRONJ can recur, particularly if the inciting factors (e.g., continued BP exposure, poor oral hygiene, trauma) persist. Incidence is reported around 10-30%.
- Management: Repeat debridement, longer BP holiday (if feasible), reinforcement of oral hygiene, and reassessment of systemic risk factors.
-
Infection:
Local cellulitis, abscess formation, or osteomyelitis can occur if debridement is incomplete or soft tissue closure fails. Incidence 5-15%.
- Management: Targeted antibiotic therapy based on culture and sensitivity, drainage of abscesses, and potentially further debridement of infected necrotic bone.
-
Non-healing / Persistent Exposed Bone:
Despite best efforts, soft tissue coverage may not be achieved, leading to persistent exposed bone. Incidence 5-10%.
- Management: Local tissue flaps, regional flaps (e.g., temporalis flap, pectoralis major flap), or free flap reconstruction may be required for definitive coverage. Hyperbaric oxygen therapy remains controversial.
-
Pathologic Fracture:
Extensive bone loss from osteonecrosis or aggressive debridement can compromise jaw integrity, leading to a pathologic fracture.
- Management: Open reduction internal fixation (ORIF) with plates and screws, often requiring reconstruction with bone grafts or vascularized flaps.
-
Nerve Injury:
Most commonly paresthesia or anesthesia of the inferior alveolar nerve (mandible) or mental nerve, particularly during extensive surgical debridement.
- Management: Conservative observation often suffices for temporary neurapraxia. Microsurgical repair is rarely indicated but may be considered for severe, persistent deficits.
For AFF Surgery:
-
Nonunion/Delayed Union:
The compromised bone biology in AFFs, characterized by suppressed bone turnover and accumulated microdamage, significantly increases the risk of delayed union or nonunion compared to typical traumatic femoral fractures. Incidence 10-30%.
- Management: Initial approach involves optimization of systemic factors (e.g., vitamin D, calcium, BP holiday), protected weight-bearing. For persistent nonunion, exchange nailing (removing the original nail and inserting a larger diameter nail) is often the first-line surgical salvage. Other options include plate augmentation (applying a locking plate parallel to the nail), autogenous bone grafting (e.g., fibular or iliac crest graft), and biologic stimulation (e.g., PRP, bone morphogenetic proteins - BMPs). Teriparatide (a parathyroid hormone analog) has shown promise in improving healing.
-
Hardware Failure:
Breakage of the intramedullary nail or locking screws, usually secondary to persistent nonunion or inadequate fixation. Incidence 5-10%.
- Management: Requires revision fixation, often involving exchange nailing, removal of failed hardware, and addressing the underlying nonunion with bone grafting and potentially plate augmentation.
-
Infection:
Surgical site infection, though rare (1-5%), can be devastating.
- Management: Aggressive debridement, irrigation, targeted antibiotics, and potentially implant removal with subsequent staged reconstruction.
-
Malunion:
Rotational or angular deformity of the femur. Incidence 5-10%.
- Management: If symptomatic and severe, corrective osteotomy and re-fixation may be required.
-
Pain at Nail Tip/Entry Site:
Trochanteric bursitis or irritation from proximal nail prominence.
- Management: NSAIDs, physical therapy, local corticosteroid injections. If persistent, hardware removal may be necessary after fracture healing.
-
Iatrogenic Fracture:
During nail insertion, reaming, or locking screw placement, particularly in the brittle cortical bone.
- Management: Requires immediate stabilization, potentially with longer nail or supplementary plating.
Table: Common Complications, Incidence, and Salvage Strategies
| Complication Type | Incidence (approx.) | Salvage Strategies |
|---|---|---|
| MRONJ Surgery | ||
| Recurrence | 10-30% | Repeat debridement, longer BP holiday (if appropriate), meticulous oral hygiene, reassess risk factors. |
| Infection | 5-15% | Targeted antibiotics (culture-guided), drainage, further debridement of infected tissue. |
| Non-healing / Persistent Exposed Bone | 5-10% | Local/regional/free flap reconstruction, wound care, hyperbaric oxygen (controversial). |
| Pathologic Jaw Fracture | Variable (depends on MRONJ stage) | ORIF with plates/screws, often requiring bone grafting or vascularized flap reconstruction. |
| AFF Surgery | ||
| Nonunion/Delayed Union | 10-30% | Exchange nailing, plate augmentation, autogenous bone grafting (e.g., fibular, iliac crest), biologics (e.g., PRP, BMPs), teriparatide. |
| Hardware Failure | 5-10% (often due to nonunion) | Revision fixation (exchange nailing, plate augmentation), removal of failed hardware, addressing underlying nonunion. |
| Infection | 1-5% | Aggressive debridement, irrigation, targeted IV antibiotics, implant retention vs. removal (based on type of infection and stability). |
| Malunion | 5-10% | Corrective osteotomy and re-fixation (if symptomatic or functionally limiting). |
| Pain at Nail Tip | 5-15% | NSAIDs, physiotherapy, local injections. Hardware removal (after healing) if refractory. |
| Iatrogenic Fracture | Rare | Immediate stabilization with longer nail or supplemental plating. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is critical for optimizing functional recovery and minimizing long-term morbidity following surgical management of bisphosphonate-related complications. Protocols must be tailored to the specific pathology and surgical intervention.
For MRONJ Surgery:
-
Early Phase (Days 0-14):
- Pain Management: Opioids and NSAIDs as needed.
- Antibiotics: Continued systemic antibiotics, often for 7-14 days or longer if infection was severe.
- Oral Hygiene: Gentle antimicrobial mouth rinses (e.g., chlorhexidine 0.12%) 2-3 times daily, avoiding direct trauma to the surgical site. Gentle tooth brushing on unaffected areas.
- Diet: Liquid or very soft, non-chewy diet to minimize masticatory forces on the healing jaw. Avoid hot or irritating foods.
- Activity: Rest, avoid strenuous activity or anything that could increase intraoral pressure.
-
Intermediate Phase (Weeks 2-8):
- Diet: Gradual progression to a soft diet, avoiding hard or crunchy foods.
- Oral Hygiene: Continue meticulous oral hygiene, gently brushing all teeth.
- Follow-up: Regular clinical follow-up with the oral/maxillofacial surgeon to monitor wound healing, soft tissue integrity, and screen for signs of recurrence.
-
Long-term Management:
- Dental Care: Regular dental check-ups and professional cleanings are crucial. Any future invasive dental procedures must be meticulously planned with the treating surgeon.
- Bisphosphonate Status: Decision on restarting or continuing the BP holiday is made in consultation with the endocrinologist or rheumatologist, weighing the risks of MRONJ recurrence against the benefits of BP for osteoporosis. Calcium and vitamin D supplementation should be maintained.
- Monitoring: Vigilance for any new symptoms of MRONJ recurrence.
For AFF Surgery:
Rehabilitation protocols for AFFs are similar to those for other femoral shaft fractures fixed with intramedullary nails, but with key considerations for compromised bone healing.
-
Early Phase (Days 0-6 weeks):
-
Weight-Bearing (WB):
Typically, protected weight-bearing is initiated:
- Partial Weight-Bearing (PWB): 25-50% body weight, using crutches or a walker.
- Touch-Down Weight-Bearing (TDWB): For very unstable fractures or those with poor bone quality.
- Progression: Weight-bearing is gradually advanced as pain allows and radiographic evidence of early callus formation appears. Close monitoring of pain and gait mechanics.
- Range of Motion (ROM): Early, gentle active and active-assisted ROM exercises for the hip and knee, typically within comfortable limits, to prevent stiffness.
- Strength: Isometric strengthening exercises for hip and knee musculature (e.g., quadriceps sets, gluteal sets).
- Mobility: Transfer training, ambulation with assistive devices.
-
Weight-Bearing (WB):
Typically, protected weight-bearing is initiated:
-
Intermediate Phase (Weeks 6-12):
- Weight-Bearing: Progressive advancement to full weight-bearing (FWB) as pain diminishes and serial radiographs show bridging callus.
- Strengthening: Progressive resistance exercises for hip abductors, adductors, quadriceps, and hamstrings. Closed-chain exercises are introduced.
- Gait Training: Focus on normalizing gait pattern and reducing reliance on assistive devices. Proprioceptive training.
-
Late Phase (>12 weeks to 6 months+):
- Full Weight-Bearing: Unrestricted ambulation.
- Advanced Strengthening: Progress to functional and sport-specific exercises. Balance and agility training.
- Imaging Follow-up: Serial radiographs (every 6-12 weeks) until radiographic union is confirmed, which can take significantly longer than typical femoral fractures (6-12 months or more).
- Bisphosphonate Management: The bisphosphonate holiday initiated at diagnosis is typically continued for at least 1-2 years post-fracture, or even indefinitely, depending on the individual patient's fracture risk and bone density. Close consultation with an endocrinologist or rheumatologist is crucial. Calcium (1200 mg/day) and vitamin D (800-2000 IU/day) supplementation is maintained. Consideration for anabolic agents (e.g., teriparatide) to accelerate healing, especially in cases of delayed union or nonunion.
- Contralateral Femur Monitoring: Ongoing surveillance of the contralateral femur with periodic imaging (e.g., plain radiographs or even MRI if symptomatic) is paramount due to the high risk of bilateral involvement.
Summary of Key Literature / Guidelines
The management of bisphosphonate-related complications is continuously evolving, guided by multidisciplinary consensus and emerging evidence. Orthopedic surgeons must be familiar with key literature and guidelines to provide optimal, evidence-based care.
For Medication-Related Osteonecrosis of the Jaw (MRONJ):
- AAOMS Position Paper on MRONJ: The American Association of Oral and Maxillofacial Surgeons (AAOMS) periodically publishes comprehensive position papers (most recently in 2022) which serve as the definitive guideline for the diagnosis, staging, prevention, and management of MRONJ. These papers provide evidence-based recommendations for both oral and maxillofacial surgeons and other healthcare providers. Key aspects include a shift from "BRONJ" to "MRONJ" to reflect other causative antiresorptive and anti-angiogenic medications, and a focus on conservative management for early stages, with surgical debridement reserved for symptomatic or advanced disease.
- Consensus Statements: Various international bodies and specialty organizations (e.g., ASBMR, European Association for Cranio-Maxillo-Facial Surgery) have issued consensus statements that largely align with the AAOMS guidelines, emphasizing the importance of a multidisciplinary approach involving dentists, oral surgeons, oncologists, and endocrinologists.
- Literature on Bisphosphonate Holiday: While often recommended prior to dental procedures in patients at high risk for MRONJ, the actual efficacy of a "drug holiday" in preventing or treating MRONJ remains debated. Current literature suggests it may not significantly alter the risk of developing MRONJ or improve healing once established, particularly for oral bisphosphonates. Decisions should be individualized.
For Atypical Femoral Fractures (AFFs):
- ASBMR Task Force Report on AFFs: The American Society for Bone and Mineral Research (ASBMR) Task Force Report on AFFs (most recently updated in 2013) provides a critical framework for defining, diagnosing, and managing these fractures. It outlines the characteristic radiographic features, risk factors, and provides recommendations for surgical versus non-operative management of complete and incomplete AFFs. It strongly recommends intramedullary nailing for complete fractures and prophylactic nailing for high-risk incomplete fractures.
- Orthopedic Trauma Association (OTA) Guidelines: While no specific OTA guidelines are dedicated solely to AFFs, the principles of long bone fracture management, particularly for subtrochanteric and diaphyseal femur fractures, apply. OTA position statements and reviews often incorporate considerations for compromised bone healing in osteoporotic or medicated bone.
-
Specific Orthopedic Literature:
Numerous studies in orthopedic journals have focused on the epidemiology, biomechanics, risk factors, and surgical outcomes of AFFs. Key areas of ongoing research and debate include:
- Prophylactic Nailing Criteria: Refining the indications for prophylactic nailing of incomplete AFFs, particularly in asymptomatic contralateral femurs.
- Nonunion Rates and Salvage: Strategies to address the elevated nonunion rates, including exchange nailing, plate augmentation, and the role of anabolic agents like teriparatide.
- Bisphosphonate Holiday Duration: Optimizing the duration of BP holiday post-AFF, with current recommendations often suggesting 1-2 years or more of discontinuation, balanced against the patient's underlying osteoporosis severity.
- Anabolic Agent Use: Growing evidence supports the use of teriparatide to accelerate healing in AFFs, especially in the context of delayed union or nonunion.
General Interdisciplinary Approach:
Both MRONJ and AFFs underscore the critical importance of an interdisciplinary approach. Orthopedic surgeons must collaborate closely with oral and maxillofacial surgeons, endocrinologists, rheumatologists, and primary care physicians to ensure comprehensive patient care, encompassing pre-operative optimization, surgical intervention, and long-term medical and rehabilitative management. Patient education regarding prodromal symptoms, medication adherence, and potential complications remains a cornerstone of preventive strategies.
You Might Also Like