Atypical Lipomatous Tumor (ALT) & Well-Differentiated Liposarcoma: Epidemiology, Genetics, & Surgical Management
Key Takeaway
Atypical Lipomatous Tumor (ALT), also known as Well-Differentiated Liposarcoma (WDL), is an intermediate-grade, locally aggressive neoplasm characterized by adipocytic differentiation and MDM2/CDK4 amplification. While typically non-metastatic, it poses risks of local recurrence and dedifferentiation into higher-grade liposarcomas. Management differs significantly between extremity and challenging retroperitoneal locations, demanding precise surgical planning due to varying anatomical complexities.
Introduction & Epidemiology
Atypical Lipomatous Tumor (ALT), also referred to as Well-Differentiated Liposarcoma (WDL), represents the most common subtype within the liposarcoma spectrum. It is classified as an intermediate-grade, locally aggressive neoplasm by the World Health Organization (WHO), primarily characterized by adipocytic differentiation and the absence of dedifferentiated, pleomorphic, or myxoid features. While ALTs are considered low-grade tumors that do not metastasize as long as they retain their well-differentiated characteristics, their primary clinical significance lies in their propensity for local recurrence and, more critically, their potential for dedifferentiation into higher-grade, often more aggressive, liposarcoma subtypes, which then carry metastatic potential.
Epidemiologically, ALTs are relatively rare, with an incidence rate estimated at 1-2 per 100,000 population per year for all soft tissue sarcomas. Liposarcomas, in general, account for approximately 20-30% of all soft tissue sarcomas, with ALT/WDL comprising the largest proportion of these. They typically manifest in adults, predominantly affecting individuals in their fifth to seventh decades of life, with a slight male predominance. The most common anatomical sites for ALTs are the deep soft tissues of the extremities (especially the thigh), the retroperitoneum, and the mediastinum. Less commonly, they can be found in the spermatic cord, head and neck region, or superficial locations. The clinical presentation is often that of a slowly enlarging, painless soft tissue mass, which can make differentiation from benign lipomas challenging without advanced imaging and histological evaluation.
Genetically, ALTs are characterized by supernumerary ring chromosomes and/or giant marker chromosomes that invariably contain amplified sequences from the 12q13-15 region. This amplification commonly includes oncogenes such as MDM2 and CDK4 . The overexpression of MDM2, an inhibitor of the p53 tumor suppressor protein, is a crucial diagnostic marker. The presence of MDM2 amplification and overexpression, detectable by immunohistochemistry or fluorescence in situ hybridization (FISH), is a highly sensitive and specific finding that distinguishes ALT/WDL from benign lipomas and other fat-forming tumors. This molecular signature is fundamental to the accurate diagnosis and subsequent management of these tumors, guiding decisions on surgical aggressiveness and surveillance.
The distinction between ALT in an extremity/superficial location and WDL in the retroperitoneum, although histologically identical, reflects differing clinical behaviors and risks of dedifferentiation. Retroperitoneal WDLs are associated with a significantly higher risk of dedifferentiation and local recurrence due to their typically larger size, anatomical complexity, and difficulty in achieving consistently wide surgical margins. This necessitates a more aggressive surgical approach and meticulous long-term surveillance strategies tailored to the anatomical location.
Surgical Anatomy & Biomechanics
Understanding the surgical anatomy pertinent to atypical lipomatous tumors is crucial for meticulous preoperative planning and precise surgical execution. ALTs most frequently arise in deep soft tissue compartments, particularly the thigh, gluteal region, shoulder girdle, and retroperitoneum. Less common sites include the spermatic cord, mediastinum, and superficial subcutaneous tissues. The critical anatomical considerations vary significantly with the tumor's location.
For extremity ALTs, a comprehensive understanding of fascial compartments is paramount. The tumor often originates within or invades a specific muscle compartment, necessitating en bloc resection of the involved compartment or portions thereof. Proximity to major neurovascular bundles (e.g., sciatic nerve, femoral neurovascular bundle, brachial plexus, popliteal vessels) dictates the feasibility of achieving wide surgical margins without compromising limb function or viability. A detailed knowledge of the course and branching patterns of these structures, as well as their relationship to surrounding musculature, is essential. For instance, a deep thigh ALT may abut the femoral artery and nerve anteriorly or the sciatic nerve posteriorly, requiring careful dissection to achieve tumor-free margins while preserving vital structures. The deep fascia often acts as a partial barrier to tumor spread, but transgression is common, especially with larger or recurrent lesions.
Retroperitoneal ALTs present a unique anatomical challenge. These tumors can grow to enormous sizes before detection, often displacing or engulfing vital organs and major vascular structures (aorta, vena cava, renal vessels, ureters, kidneys, pancreas, colon, duodenum). The retroperitoneal space lacks clear fascial boundaries that are amenable to "compartmental" resection in the same way an extremity might. This makes achieving wide, consistently negative margins exceedingly difficult and contributes to the higher rates of local recurrence and dedifferentiation observed in this location. Surgeons must be intimately familiar with abdominal and pelvic anatomy, including the planes of dissection around the great vessels, bowel mesentery, and genitourinary structures. Multi-organ resection may be required to achieve clearance.
From a biomechanical perspective, the impact of ALT resection relates directly to the extent of tissue removal and the reconstructive challenges. In the extremities, wide local excision of an ALT, particularly if it involves large muscle groups (e.g., quadriceps, hamstrings, deltoid), can lead to significant functional deficits such as muscle weakness, gait abnormalities, joint instability, or range of motion limitations. The preservation of critical tendons, ligaments, and joint capsules is vital to maintain limb biomechanics. If a significant portion of a muscle or muscle group must be resected, the remaining musculature may undergo compensatory hypertrophy, but functional compromise is often unavoidable. In some cases, tendon transfers or prosthetic replacements may be necessary to restore function, particularly around large joints like the hip or knee. The integrity of the fascial envelopes also contributes to muscle efficiency and containment; extensive fascial removal can lead to muscle herniation or loss of contractile efficiency. For retroperitoneal tumors, the biomechanical impact is less about musculoskeletal function and more about the impact on visceral organ function and abdominal wall integrity. Resection of large volumes of retroperitoneal fat and connective tissue can lead to loss of abdominal wall support, bowel adhesions, or compromise of urinary/digestive system function, impacting overall physiological homeostasis rather than isolated joint mechanics. The structural integrity of the spinal column or pelvic girdle can also be compromised if the tumor invades adjacent bone, requiring complex reconstructive strategies involving orthopedic oncology principles.

Indications & Contraindications
The management of Atypical Lipomatous Tumor (ALT) is primarily surgical. The indications for treatment are well-defined, revolving around the need for definitive diagnosis and prevention of local recurrence and dedifferentiation. Contraindications are generally related to patient fitness for surgery or the presence of unresectable disease, though this is rare for primary ALT.
Indications for Operative Treatment (Wide Local Excision)
The vast majority of biopsy-confirmed ALTs are indicated for surgical resection. The primary goals are local disease control and prevention of dedifferentiation.
- Biopsy-Confirmed ALT/WDL : This is the strongest indication. Once the diagnosis is histologically confirmed (often with molecular confirmation of MDM2/CDK4 amplification), surgical excision is the standard of care.
- Symptomatic Lesion : Any ALT causing pain, nerve compression (e.g., sciatica, foot drop), vascular compromise, or functional impairment (e.g., restricting joint movement, affecting gait) necessitates surgical intervention to alleviate symptoms and prevent further morbidity.
- Large Size and/or Deep Location : Large tumors (>5 cm) and deeply seated tumors are more prone to recurrence and dedifferentiation. Their size often makes complete excision challenging and increases the risk of functional impairment if left untreated. Deep lesions are also more likely to interact with critical neurovascular structures.
- Suspicion of Dedifferentiation or Progression : Rapid growth, new onset of pain, or imaging changes (e.g., new nodular non-fatty components, increased enhancement, or areas of necrosis on MRI) in a previously stable ALT or a suspected lipomatous lesion are strong indications for prompt surgical evaluation and excision.
- Local Recurrence : Any local recurrence of ALT, even if well-differentiated, mandates re-excision. Recurrent lesions often carry a higher risk of dedifferentiation.
- Difficulty in Definitive Biopsy : In rare instances where a core needle biopsy is inconclusive despite strong clinical and radiological suspicion of ALT, or if a superficial lesion is easily resectable with low morbidity, an excisional biopsy for definitive diagnosis and treatment may be considered. This is less common in current practice where image-guided core biopsy is preferred.
Indications for Non-Operative Treatment (Surveillance/Observation)
Non-operative management for a biopsy-proven ALT is exceptionally rare and should be approached with extreme caution, typically only after multidisciplinary discussion and explicit patient consent regarding the risks.
- Medically Unfit for Surgery : Patients with severe comorbidities that preclude them from undergoing general anesthesia or major surgery may be candidates for observation, especially if the tumor is asymptomatic, slow-growing, and unlikely to cause imminent morbidity. Palliative surgical debulking might be considered for symptomatic relief in such cases if observation fails.
- Very Small, Asymptomatic, Superficial Lesions (Controversial) : In very select cases, an extremely small (<2-3 cm), purely superficial, asymptomatic lipomatous lesion with ambiguous biopsy results (e.g., atypical features but not definitive for ALT, or when MDM2 status is equivocal/negative but clinical suspicion remains) might be managed with serial imaging surveillance. However, if ALT is definitively diagnosed, even small lesions are generally recommended for excision to prevent potential progression or dedifferentiation. This is a highly debated area and not standard practice for biopsy-proven ALT.
- Microscopic Residual Disease (R1 Margin) in High-Morbidity Sites : For retroperitoneal or other anatomically challenging ALTs where achieving negative margins is highly morbid (e.g., necessitating critical organ resection or severe functional loss), and where the residual disease is microscopic, observation with close surveillance may be considered in conjunction with adjuvant radiotherapy, particularly if re-resection carries unacceptable risks. This is a complex decision made by a multidisciplinary tumor board.
Contraindications for Surgical Excision
True contraindications for surgical excision of ALT are few, given the tumor's potential for local aggression and dedifferentiation.
- Unresectable Disease : This is extremely rare for primary ALT, which is inherently a localized disease. However, in cases of massive retroperitoneal WDL that encases vital, unreconstructible structures (e.g., large segments of the aorta, vena cava, or superior mesenteric artery/vein) where no surgical plane can be safely created to achieve even subtotal resection without catastrophic complications, surgery may be contraindicated. In such scenarios, palliative debulking may be considered for symptom control.
- Severe Medical Comorbidities : Patients with extreme medical fragility where the risks of general anesthesia and a major surgical procedure significantly outweigh the potential benefits may be deemed inoperable. These cases require a thorough risk-benefit assessment by a multidisciplinary team.
- Metastatic Disease : By definition, well-differentiated liposarcoma does not metastasize. If a patient presents with distant metastases, the tumor has dedifferentiated, and the primary treatment strategy shifts to that of a high-grade sarcoma, often involving systemic therapy in addition to local control. However, local control of the primary tumor remains crucial.
Table: Operative vs. Non-Operative Indications for ALT
| Indication Type | Operative (Wide Local Excision) | Non-Operative (Surveillance/Observation) |
|---|---|---|
| Pathology | Biopsy-confirmed Atypical Lipomatous Tumor (ALT/WDL), MDM2/CDK4 positive. | Medically unfit for surgery due to severe comorbidities. Rarely for microscopic residual disease (R1) in high-morbidity sites, potentially with adjuvant RT. |
| Clinical | Symptomatic lesion (pain, mass effect, functional impairment), rapidly growing mass. | Asymptomatic, very small (<2-3cm), superficial lesion (only if biopsy equivocal and high surgical morbidity, highly debated and not standard for confirmed ALT). |
| Imaging | Large size (>5cm), deep location, septations, non-fatty components, suspicion of dedifferentiation. | Stable over time, purely fatty on MRI, no concerning features (only if biopsy challenging/equivocal, and patient factors preclude surgery). |
| Recurrence | Local recurrence of ALT. | Not applicable as primary management for confirmed ALT. |
| Goal | Local disease control, prevention of dedifferentiation. | Mitigate surgical risk, monitor for progression (often palliative or bridging strategy). |
Pre-Operative Planning & Patient Positioning
Thorough pre-operative planning is paramount in the successful management of atypical lipomatous tumors (ALT) to ensure optimal tumor resection, minimize morbidity, and prepare for potential reconstructive challenges.
Pre-Operative Planning
- Multidisciplinary Tumor Board Review : All cases of suspected or biopsy-proven ALT should be discussed in a multidisciplinary tumor board involving orthopedic oncologists, surgical oncologists, radiation oncologists, medical oncologists, radiologists, and pathologists. This ensures a consensus on diagnosis, staging, treatment strategy, and surveillance plan.
-
Imaging Review
:
- Magnetic Resonance Imaging (MRI) : This is the gold standard for local staging. A high-resolution, multi-sequence MRI with contrast (gadolinium) is essential. It provides detailed information on tumor size, exact anatomical location, relationship to neurovascular structures, adjacent bone, and joint capsules. MRI helps delineate fascial planes and identify areas of non-lipomatous components or septations, which can suggest ALT over benign lipoma and guide biopsy. Crucially, it informs the extent of the surgical resection and helps plan the incision to achieve adequate margins.
-
Computed Tomography (CT) Scan
: While MRI is superior for soft tissue detail, CT may be used for specific purposes:
- Retroperitoneal/Visceral ALTs : CT is invaluable for assessing the relationship of large retroperitoneal ALTs to abdominal and pelvic organs, major vessels, and bone involvement.
- Chest CT : Routine chest CT is often performed for staging any soft tissue sarcoma, although ALTs typically do not metastasize unless dedifferentiated. It serves as a baseline and screens for pulmonary nodules.
- Biopsy Review : A definitive diagnosis of ALT/WDL, typically confirmed by core needle biopsy with immunohistochemistry (MDM2, CDK4) and/or FISH for MDM2 amplification, must be reviewed. The biopsy tract should be planned such that it can be incorporated into the subsequent wide local excision to prevent seeding of tumor cells.
- Surgical Margin Planning : The primary goal is wide local excision with negative margins (R0 resection). This typically entails excising the tumor with a surrounding cuff of at least 1-2 cm of grossly normal tissue in all dimensions, or complete removal of the involved muscle compartment. For retroperitoneal tumors, achieving wide margins is often difficult due to proximity to vital organs, making a "compartmental" resection often unfeasible. The adequacy of margins heavily influences local recurrence rates.
- Neurovascular Mapping : Detailed review of imaging, especially MRI, to identify and trace the course of critical nerves and vessels adjacent to the tumor. This helps in anticipating potential challenges during dissection and planning strategies for their preservation or, if unavoidable, reconstruction. Pre-operative nerve mapping (e.g., ultrasound-guided localization) may be considered in complex cases.
- Reconstructive Planning : Anticipate potential soft tissue deficits following wide excision. If a large skin or muscle defect is expected, plan for primary closure, local flap advancement, regional flap reconstruction (e.g., gastrocnemius flap for knee defects, latissimus dorsi flap for shoulder/back defects), or skin grafting. Collaboration with plastic surgeons may be necessary.
- Blood Loss Management : Large, deep-seated tumors, especially retroperitoneal ones, can be highly vascular. Pre-operative embolization may be considered for highly vascular tumors, and adequate blood products should be cross-matched and available.
- Patient Counseling : Comprehensive discussion with the patient regarding the diagnosis, planned procedure, potential complications (e.g., nerve injury, functional deficits, recurrence risk), rehabilitation expectations, and long-term surveillance.
Patient Positioning
Patient positioning is critical for optimal surgical exposure, minimizing patient morbidity, and facilitating a safe and efficient resection. The specific position is dictated by the tumor's anatomical location.
-
General Principles :
- Adequate Exposure : The position must allow complete visualization and access to the tumor and the planned surgical margins, including sufficient space for instrumentation.
- Neurovascular Protection : All pressure points must be padded to prevent iatrogenic nerve compression (e.g., ulnar nerve at the elbow, peroneal nerve at the fibular head) or vascular compromise.
- Anesthetic Access : Maintain clear access for the anesthesia team for airway management, intravenous lines, and monitoring.
- Versatility : For large or complex tumors, consider positions that allow for minor adjustments or potential repositioning to address unexpected findings or reconstructive needs.
- Tourniquet : For extremity tumors, a pneumatic tourniquet can be used to create a bloodless field, improving visualization and precision.
- Prep and Drape : The surgical field should be prepped and draped widely enough to allow for unexpected extensions of the incision, exploration of neurovascular structures, and potential harvest of reconstructive flaps.
-
Specific Positions by Location :
-
Deep Thigh/Gluteal Region
:
- Lateral Decubitus : For posteromedial thigh or gluteal lesions. The affected side is up, with careful padding of the dependent arm and leg.
- Supine : For anterior or anteromedial thigh lesions. Leg can be slightly flexed and externally rotated, or placed in a leg holder for better access.
- Prone : For posterior thigh lesions, ensuring adequate abdominal support and careful head positioning.
-
Shoulder/Arm
:
- Beach Chair or Semi-Fowler's : For anterior/superior shoulder lesions, allowing excellent access to the shoulder girdle and proximal arm.
- Supine with Arm on Arm Board : For deltoid, arm, or forearm lesions, allowing free movement of the limb.
-
Retroperitoneum
:
- Supine : For anterior approach to large retroperitoneal masses.
- Lateral Decubitus : For flank or posterolateral retroperitoneal tumors, providing optimal access for a retroperitoneal or thoracoabdominal approach.
-
Trunk (Chest Wall/Back)
:
- Supine : For anterior chest wall or abdominal wall.
- Prone : For back or posterior chest wall.
-
Deep Thigh/Gluteal Region
:
After positioning, the planned incision and key anatomical landmarks (e.g., bone prominences, neurovascular pathways) should be marked on the skin.
Detailed Surgical Approach / Technique
The cornerstone of atypical lipomatous tumor (ALT) management is wide local excision with negative surgical margins. The specific approach varies significantly depending on tumor location, size, and proximity to critical structures. The following outlines general principles and detailed steps applicable to most extremity ALTs, with considerations for other sites.
General Principles
- En bloc Resection : The tumor must be removed in one piece, completely encased in a cuff of normal tissue. Tumor violation or piecemeal excision significantly increases the risk of local recurrence and potential dedifferentiation.
- Incorporation of Biopsy Tract : The initial biopsy tract, if performed by core needle, must be excised en bloc with the tumor to prevent tumor cell dissemination. If an open incisional biopsy was performed, the entire previous incision and surrounding scar tissue must be included in the wide excision.
- Longitudinal Incision : Whenever possible, incisions should be longitudinal along the axis of the limb or trunk. This allows for extensile exposure, facilitates future potential re-excisions or amputations (though rare for ALT), and respects tension lines for better cosmesis. Transverse incisions should generally be avoided.
- Hemostasis : Meticulous hemostasis throughout the procedure is critical to maintain a clear surgical field and minimize hematoma formation.
- Preservation of Function : While achieving negative margins is paramount, every effort should be made to preserve critical neurovascular structures and minimize functional deficit.
Step-by-Step Surgical Technique (Example: Deep Thigh ALT)
-
Incision :
- Make a longitudinal incision centered directly over the palpable mass, extending proximally and distally to provide adequate exposure for a wide margin. The length of the incision should be sufficient to visualize tumor boundaries and achieve planned margins without excessive retraction.
- Incise through the skin and subcutaneous tissue. Identify and ligate any superficial vessels.
-
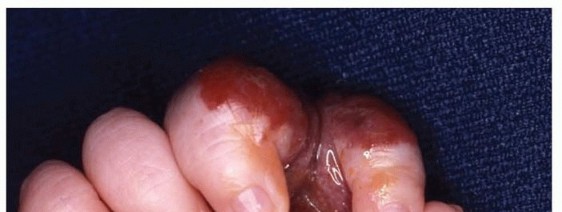
Image Integration
: The gross appearance often shows a yellow, lobulated mass, sometimes with areas of fibrosis or myxoid change, or septations. The image below depicts such a presentation, which can be seen upon initial exposure or after deeper dissection:

-
Elevation of Skin Flaps :
- Carefully elevate full-thickness skin and subcutaneous fat flaps (subcutaneous plane) anteriorly and posteriorly to expose the deep fascia overlying the tumor and the surrounding normal muscle. The extent of these flaps should allow for a generous margin of normal tissue around the tumor.
- Use appropriate retractors to maintain exposure without causing undue tension or injury to surrounding tissues.
-
Dissection to Deep Fascia :
- Once the deep fascia is exposed, carefully inspect for any signs of tumor infiltration (e.g., bulging, discoloration, irregular texture). If the tumor appears superficial to the deep fascia, the fascia should be excised with a wide margin. If the tumor is deep to the fascia, the deep fascia overlying the tumor should be excised en bloc.
-
Identification of Internervous Planes and Critical Structures :
- For deep-seated tumors, identify the relevant muscle compartments and internervous planes. For example, in the thigh, the plane between the rectus femoris and vastus medialis, or between the quadriceps and hamstrings, may be utilized.
- Carefully dissect along these planes, progressively exposing the tumor. Early identification and protection of major neurovascular structures (e.g., femoral nerve/artery/vein, sciatic nerve, profunda femoris vessels) are crucial. Use blunt dissection and gentle retraction to separate these structures from the tumor capsule. Small feeding vessels to the tumor should be meticulously ligated or coagulated.
-
If a major nerve or vessel is intimately involved with the tumor, a decision must be made:
- Invasion vs. Adherence : If the tumor is merely adherent, careful sharp dissection (e.g., using micro-scissors or a nerve dissector) can often separate the tumor from the adventitia of a vessel or the epineurium of a nerve.
- Clear Invasion : If there is clear macroscopic invasion of a major nerve (resulting in loss of function) or vessel (rendering it non-functional), en bloc resection of the involved segment may be necessary. This necessitates a pre-operative discussion with the patient and potentially vascular/neuroplastic surgery reconstruction.
- Sacrifice of expendable nerves : Small sensory nerves that are intimately involved may need to be sacrificed to achieve clear margins.
-
En Bloc Resection :
- Circumferentially dissect around the tumor mass, maintaining a desired cuff of normal healthy tissue (typically 1-2 cm of grossly normal muscle/fat) in all dimensions.
- Use electrocautery for smaller vessels and sharp dissection for muscle planes. If the tumor is contained within a single muscle, the entire muscle or a significant portion of it may need to be resected from origin to insertion (compartmental resection or wide partial compartmental resection).
- Ensure that the deep margin, often against bone or a major neurovascular bundle, is also meticulously cleared. If the tumor abuts periosteum, a small strip of periosteum or even a superficial layer of cortical bone may need to be removed (marginal or wide intralesional excision of bone, if minimal involvement).
- Once all attachments are released, the tumor specimen is removed en bloc. Orient the specimen for the pathologist with sutures or clips to indicate specific margins (e.g., superior, inferior, medial, lateral, deep) to aid in margin assessment.
- Frozen Section Analysis (Optional but helpful) : While not always definitive for ALT due to its nuanced pathology, frozen sections can be considered for high-risk margins (e.g., very close to neurovascular structures) to guide further resection, though final margin assessment always relies on permanent histology.
-
Hemostasis and Irrigation :
- Achieve meticulous hemostasis of the surgical bed using electrocautery, ligatures, or hemostatic agents.
- Thoroughly irrigate the wound with sterile saline to remove any loose tissue fragments or blood clots.
-
Wound Closure :
- Reconstruction : Assess the defect. If large, consider the need for muscle transposition, local fasciocutaneous flaps, or skin grafts.
- Drainage : Place a closed-suction drain (e.g., Jackson-Pratt or Blake drain) in the wound bed, especially if a significant dead space has been created, to prevent hematoma and seroma formation.
-
Layered Closure
: Close the wound in layers:
- Deep fascia (if remaining) or muscle fascia with absorbable sutures.
- Subcutaneous tissue with absorbable sutures to re-approximate the skin edges and reduce tension.
- Skin closure with staples or non-absorbable sutures.
Specific Considerations for Retroperitoneal ALTs
Retroperitoneal ALTs present unique challenges:
*
Anatomical Complexity
: Involvement of kidney, ureter, colon, pancreas, major vessels (aorta, vena cava, renal arteries/veins).
*
Multi-Organ Resection
: Often requires concomitant nephrectomy, colectomy, pancreatectomy, or vascular reconstruction to achieve adequate margins.
*
Large Size
: Frequently present at very large sizes, making complete resection and visualization difficult.
*
Higher Dedifferentiation Rate
: Increased propensity for dedifferentiation to higher-grade liposarcoma, often requiring more aggressive systemic treatment alongside surgery.
*
Collaborative Surgery
: Often necessitates a combined approach with general surgeons, vascular surgeons, or urologists.
Complications & Management
Surgical intervention for atypical lipomatous tumors (ALT) is associated with a spectrum of potential complications, ranging from general surgical risks to those specific to soft tissue sarcoma surgery and the unique characteristics of ALT/WDL. Understanding these complications, their approximate incidence, and effective salvage strategies is crucial for pre-operative counseling and post-operative management.
General Surgical Complications
These are common to most major surgical procedures:
-
Wound Infection
: Incidence typically 2-5%. Risk factors include prolonged surgery, large dead space, hematoma, and patient comorbidities.
- Management : Superficial infections often respond to oral antibiotics and local wound care. Deep or extensive infections may require intravenous antibiotics, surgical debridement, and/or drain placement.
-
Hematoma/Seroma
: Incidence 5-10%. Result from inadequate hemostasis or fluid accumulation in dead space.
- Management : Small, asymptomatic collections may resolve spontaneously. Larger or symptomatic hematomas/seromas may require needle aspiration under ultrasound guidance or surgical evacuation and drain placement. Drains are often utilized prophylactically.
-
Wound Dehiscence
: Incidence <1-2%. Partial or complete separation of wound edges.
- Management : Local wound care, secondary closure, or vacuum-assisted closure (VAC) therapy. May require re-suturing in some cases.
-
Nerve Injury
: Incidence varies significantly with tumor location and proximity to major nerves.
- Management : For neuropraxia, observation and physical therapy. For neurapraxia or axonotmesis, neurolysis may be considered. For neurotmesis (nerve transection), nerve repair (primary repair, graft) or transfer may be indicated, often requiring specialist consultation.
Specific Complications Related to ALT Resection
-
Local Recurrence
: This is the most significant and frequent complication of ALT/WDL surgery, even after achieving clear margins. Incidence ranges from 10% to 30% for extremity/truncal lesions, and significantly higher (up to 40-70%) for retroperitoneal lesions, often due to the difficulty in obtaining wide, clear margins.
- Management : Aggressive re-excision with wider margins is the primary salvage strategy. Adjuvant radiotherapy may be considered for recurrent disease or for R1 (microscopic positive) margins in anatomically challenging sites where further resection carries high morbidity.
-
Dedifferentiation
: The transformation of ALT into a higher-grade liposarcoma (e.g., pleomorphic or undifferentiated liposarcoma). This typically occurs in 5-10% of extremity ALTs and up to 20% or more of retroperitoneal ALTs over time. Dedifferentiated liposarcomas (DDLPS) have metastatic potential.
- Management : If dedifferentiation is detected (usually on surveillance imaging or biopsy of a recurrent lesion), the management paradigm shifts to that of a high-grade sarcoma. This involves aggressive surgical resection of the dedifferentiated component, often followed by adjuvant chemotherapy and/or radiation therapy as per high-grade sarcoma protocols. Close surveillance for metastatic disease is also critical.
-
Functional Deficit/Disability
: Occurs due to extensive resection of muscle, bone, or nerve structures required to achieve clear margins.
- Management : Intensive post-operative physical and occupational therapy is essential. Bracing, orthotics, or assistive devices may be needed. In some cases, reconstructive procedures like tendon transfers or arthroplasty may be considered for significant functional impairment.
-
Chronic Pain
: A long-term consequence of soft tissue resections, nerve manipulation, or scar formation.
- Management : Multimodal pain management strategies including physical therapy, neuropathic pain medications, nerve blocks, and psychological support.
-
Lymphatic Dysfunction/Lymphedema
: Particularly after extensive dissection in the groin or axilla.
- Management : Compression garments, manual lymphatic drainage, physical therapy.
-
Scarring/Cosmesis
: Significant scarring is inevitable with wide excisions.
- Management : Scar massage, silicone sheeting, laser therapy. Psychological support for body image concerns.
Table: Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence (Approx.) | Salvage Strategy |
|---|---|---|
| Local Recurrence | 10-30% (extremity), 40-70% (retroperitoneal) | Re-excision with wider surgical margins. Adjuvant radiation therapy (RT) may be considered for R1 margins, particularly in anatomically challenging sites, or for recurrent disease. Systemic therapy not typically indicated for well-differentiated recurrence. |
| Dedifferentiation | <5% (extremity), 10-20% (retroperitoneal) | Aggressive surgical resection of the dedifferentiated component. Adjuvant chemotherapy and/or RT as per high-grade sarcoma protocols. Close surveillance for metastatic disease (e.g., CT chest, abdomen/pelvis). |
| Wound Infection | 2-5% | Oral or intravenous antibiotics based on culture results. Local wound care. Surgical debridement and drainage for deep or non-resolving infections. |
| Hematoma/Seroma | 5-10% | Small, asymptomatic collections: observation. Large/symptomatic collections: needle aspiration, surgical evacuation, or drain placement. Prophylactic drains often used. |
| Nerve Injury | Varies by location/extent | Observation for neuropraxia (most common). Neurolysis for persistent symptoms. Nerve repair (primary/graft) for complete transection, often requiring neurosurgical consultation. Intensive physical therapy for functional recovery. |
| Functional Deficit | Varies by location/extent | Intensive physical and occupational therapy. Bracing, orthotics, or assistive devices. Surgical reconstruction (e.g., tendon transfer, arthroplasty) for severe deficits. |
| Chronic Pain | 5-15% | Multimodal pain management (analgesics, NSAIDs, neuropathic agents like gabapentinoids, antidepressants). Physical therapy, nerve blocks, psychological support. |
| Lymphedema | Rare, depends on dissection extent | Compression garments, manual lymphatic drainage, decongestive therapy. |
| Vascular Injury | Rare (<1%) | Immediate surgical repair (primary repair, patch angioplasty, interposition graft) by a vascular surgeon. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation following wide local excision of an atypical lipomatous tumor (ALT) is critical for optimizing functional recovery, minimizing long-term disability, and facilitating safe return to daily activities. The protocol must be individualized based on the tumor's location, the extent of resection (e.g., muscle, nerve, bone involvement), the patient's pre-operative functional status, and the presence of any complications.
Immediate Post-Operative Phase (Days 0-7)
- Pain Management : Aggressive pain control using multimodal analgesia (opioids, NSAIDs, acetaminophen, regional nerve blocks, gabapentinoids). Effective pain control is crucial for early mobilization and participation in therapy.
- Wound Care : Daily dressing changes, monitoring for signs of infection (erythema, swelling, discharge, fever), hematoma, or seroma. Drain management (output monitoring, removal when output is minimal).
- Edema Control : Elevation of the affected extremity, gentle compression dressings, and cryotherapy (ice packs) to reduce swelling.
-
Early Mobilization
:
- Non-weight-bearing (NWB) to Touch-down weight-bearing (TDWB) : If bone or major muscle groups affecting weight-bearing have been resected, or if there's concern for wound integrity. Use of crutches, walker, or wheelchair.
- Range of Motion (ROM) : Gentle, passive or active-assisted range of motion exercises for adjacent joints, avoiding tension on the surgical site. The goal is to prevent stiffness and maintain tissue pliability. For example, for a thigh ALT, gentle knee and hip ROM within pain limits.
- Muscle Activation : Gentle isometric contractions of muscles not directly involved in the resection or those with minimal involvement, to maintain strength and prevent atrophy.
- Deep Vein Thrombosis (DVT) Prophylaxis : As per institutional guidelines, including pharmacologic prophylaxis (e.g., LMWH) and mechanical methods (e.g., pneumatic compression devices, early ambulation).
Early Rehabilitation Phase (Weeks 1-6)
- Progression of Weight-Bearing : Gradually increase weight-bearing status as tolerated and as determined by the surgeon and physical therapist, based on wound healing and structural integrity.
- Active Range of Motion (AROM) : Advance to active range of motion exercises for the affected joint(s), progressively increasing the arc of movement.
- Gentle Strengthening : Initiate gentle isometric and then isotonic strengthening exercises for muscles in the affected limb, gradually increasing resistance as pain allows. Focus on restoring balance and control.
- Gait Training : If ambulation is affected, focus on proper gait mechanics, balance, and coordination with assistive devices.
- Scar Management : Once the incision is fully healed, begin scar massage, silicone sheeting, or other modalities to minimize scar adherence and improve cosmesis.
- Modalities : Heat or cold therapy, ultrasound, or electrical stimulation may be used as adjuncts to therapy.
Progressive Rehabilitation Phase (Weeks 6-12 and beyond)
- Intensified Strengthening : Progress to more advanced strengthening exercises, incorporating resistance bands, weights, and machine-based exercises. Focus on functional strength specific to the patient's daily activities and occupational demands.
- Proprioception and Balance Training : Crucial for restoring neuromuscular control and preventing falls, especially after deep muscle or joint capsule resections.
- Functional Training : Incorporate sport-specific or work-specific activities as appropriate, gradually increasing intensity and complexity.
- Endurance Training : Cardiovascular conditioning to improve overall fitness and stamina.
- Return to Activity : Gradual return to light recreational activities, progressing to more strenuous activities as strength, flexibility, and pain allow. Close communication between the surgeon, physical therapist, and patient is essential. Full return to pre-morbid activity levels may take several months to a year, or may not be entirely achievable depending on the extent of resection.
- Monitoring for Complications : Continue to monitor for signs of local recurrence, dedifferentiation, chronic pain, or functional decline.
Long-Term Surveillance
Long-term surveillance is paramount for ALT patients due to the risk of local recurrence and dedifferentiation.
-
Clinical Follow-up
: Regular clinical examinations by the orthopedic oncologist or surgical oncologist.
- Every 3 months for the first 2 years.
- Every 6 months for years 3-5.
- Annually for years 5-10 and often indefinitely, particularly for retroperitoneal ALTs due to their higher recurrence and dedifferentiation risk.
- During follow-up, specifically palpate for any new masses, assess for pain, and evaluate functional status.
-
Imaging Surveillance
:
-
MRI
: The preferred imaging modality for local surveillance.
- Baseline post-operative MRI at 3-6 months to assess the surgical bed and serve as a reference.
- Subsequent MRIs typically every 6-12 months for the first 3-5 years, then annually for at least 10 years, or longer for retroperitoneal lesions.
- Findings to watch for : Any new soft tissue mass, increased nodularity, new areas of non-fatty enhancement within the surgical bed or adjacent to it, or significant change in size. These warrant further investigation (e.g., repeat biopsy).
- CT Chest/Abdomen/Pelvis : May be considered periodically for retroperitoneal ALTs due to the higher risk of dedifferentiation and potential for metastatic spread of the dedifferentiated component. Frequency is often tailored to individual risk.
- Ultrasound : Can be useful for superficial lesions or to investigate palpable abnormalities, but often lacks the detailed anatomical resolution of MRI for deep lesions.
-
MRI
: The preferred imaging modality for local surveillance.
Special Considerations for Retroperitoneal ALTs
Given the higher rates of recurrence and dedifferentiation, patients with retroperitoneal ALTs require more aggressive and prolonged surveillance. Imaging (CT and/or MRI) is typically performed more frequently and for a longer duration. Any signs of recurrence or dedifferentiation should prompt immediate re-evaluation and typically re-intervention.
Summary of Key Literature / Guidelines
The management of Atypical Lipomatous Tumor (ALT) / Well-Differentiated Liposarcoma (WDL) is guided by a robust body of literature and consensus guidelines from major oncology and orthopedic oncology societies. These include the National Comprehensive Cancer Network (NCCN) Guidelines, the European Society for Medical Oncology (ESMO) Clinical Practice Guidelines, and recommendations from prominent sarcoma centers and research consortia such as the Sarcoma Alliance for Research through Collaboration (SARC).
1. Diagnosis and Pathology
-
Molecular Pathology
: Landmark studies have unequivocally established the presence of supernumerary ring and/or giant marker chromosomes containing amplified sequences of 12q13-15, specifically the
MDM2
and
CDK4
oncogenes, as the diagnostic hallmark of ALT/WDL.
- Immunohistochemistry (IHC) for MDM2 and CDK4 overexpression is a highly sensitive and specific screening tool.
- Fluorescence In Situ Hybridization (FISH) for MDM2 gene amplification remains the gold standard for confirmatory diagnosis, particularly in cases with ambiguous morphology or equivocal IHC results. This molecular signature reliably differentiates ALT/WDL from benign lipomas and other fat-forming tumors. (e.g., Weiss et al., 1994; Thway et al., 2012).
- Imaging : High-resolution MRI with contrast is the cornerstone of pre-operative imaging. It effectively delineates tumor extent, relationship to neurovascular structures, and aids in identifying subtle features like septations and non-lipomatous nodules that suggest ALT over a benign lipoma. (e.g., Goldblum et al., 2013).
2. Treatment – Surgical Excision
-
Wide Local Excision (WLE)
: Consensus guidelines from NCCN, ESMO, and major orthopedic oncology groups consistently recommend WLE with negative surgical margins (R0 resection) as the primary and most effective treatment for ALT/WDL. This approach aims to minimize local recurrence and prevent dedifferentiation.
- The goal is typically a 1-2 cm grossly clear margin of healthy tissue or an en bloc compartmental resection when feasible for extremity lesions.
- Importance of Margin Status : Numerous studies have correlated positive or close surgical margins (R1/R2 resection) with significantly higher rates of local recurrence. (e.g., Gronchi et al., 2005; Pollock et al., 2012).
- Retroperitoneal vs. Extremity ALT : Literature consistently highlights the distinct clinical behavior of retroperitoneal WDL, which has a significantly higher propensity for local recurrence and dedifferentiation compared to extremity ALTs, even with seemingly adequate margins. This is attributed to the anatomical complexity of the retroperitoneum, making wide R0 resection challenging. (e.g., Trans-Atlantic Retroperitoneal Sarcoma Working Group (TARPSWG) guidelines, 2018).
-
Adjuvant Therapy
:
- Radiation Therapy (RT) : Generally not indicated for primary extremity ALTs with clear (R0) margins. However, adjuvant RT may be considered in cases with positive (R1) or very close margins, particularly in anatomically challenging locations where further surgical resection is highly morbid, or for recurrent disease.
- Chemotherapy : Not indicated for well-differentiated ALT/WDL, as these tumors are largely chemoresistant. Chemotherapy is reserved for dedifferentiated liposarcoma (DDLPS) or higher-grade sarcomas.
3. Surveillance
-
Long-Term Follow-up
: Given the inherent risk of local recurrence and dedifferentiation, long-term and often lifelong surveillance is crucial.
- Clinical Examination : Regular physical exams are recommended at increasing intervals (e.g., quarterly for 1-2 years, then biannually, then annually).
- Imaging : MRI is the preferred modality for local surveillance. Post-operative baseline MRI within 3-6 months, followed by serial imaging (e.g., every 6-12 months for 3-5 years, then annually for 10+ years, especially for retroperitoneal disease).
- Retroperitoneal Specifics : Patients with retroperitoneal WDL require more intensive surveillance (often alternating CT and MRI) due to higher recurrence and dedifferentiation rates. Any new enhancing nodule or increasing size should prompt re-biopsy to rule out dedifferentiation. (e.g., TARPSWG guidelines, 2018).
4. Prognostic Factors
- Location : Retroperitoneal location is a significant adverse prognostic factor for local recurrence and dedifferentiation.
- Surgical Margins : Positive microscopic (R1) or gross (R2) margins are strongly associated with increased local recurrence rates.
- Tumor Size : Larger tumors tend to have higher recurrence rates, often reflecting the difficulty in achieving adequate margins.
- Dedifferentiation : The development of dedifferentiation transforms the prognosis, conferring metastatic potential and requiring a more aggressive treatment approach.
In summary, current guidelines emphasize accurate pathological diagnosis, aggressive wide local excision with meticulous margin control, and vigilant, long-term surveillance. While ALT/WDL is a low-grade malignancy, its potential for local recurrence and dedifferentiation necessitates a comprehensive, multidisciplinary approach to ensure optimal patient outcomes.
You Might Also Like