of Orthopaedic Infection: Etiology, Prevention, and Surgical Management
Key Takeaway
Bone and joint infections present a formidable challenge due to the unique anatomical and physiological characteristics of the skeletal system. This comprehensive guide details the etiology, pathophysiology, and prevention of orthopaedic infections. It provides evidence-based protocols for preoperative patient optimization, operating room environment control, and meticulous surgical debridement techniques essential for eradicating osteomyelitis and minimizing surgical site infections in clinical practice.
Pathophysiology and Etiology of Skeletal Infections
Bone and joint infections pose a formidable and enduring challenge to the orthopaedic surgeon. Despite the high success rates achieved with targeted antibiotic therapy in most systemic bacterial diseases, similar efficacy is rarely mirrored in bone and joint infections. This discrepancy is fundamentally rooted in the unique physiological, anatomical, and biomechanical characteristics of osseous tissue.
The overall surgical site infection (SSI) rate in orthopaedic procedures is estimated by the U.S. Centers for Disease Control and Prevention (CDC) to be approximately 2.8%. While transient bacteremia is a frequent daily occurrence—estimated to occur 25% of the time following simple tooth brushing—the mere presence of circulating bacteria is insufficient to produce osteomyelitis. For an infection to establish a foothold, a confluence of etiological factors must align: an adequate inoculum of a sufficiently virulent organism must overcome the host’s natural inflammatory and immune defenses, often aided by local skeletal trauma or ischemia.
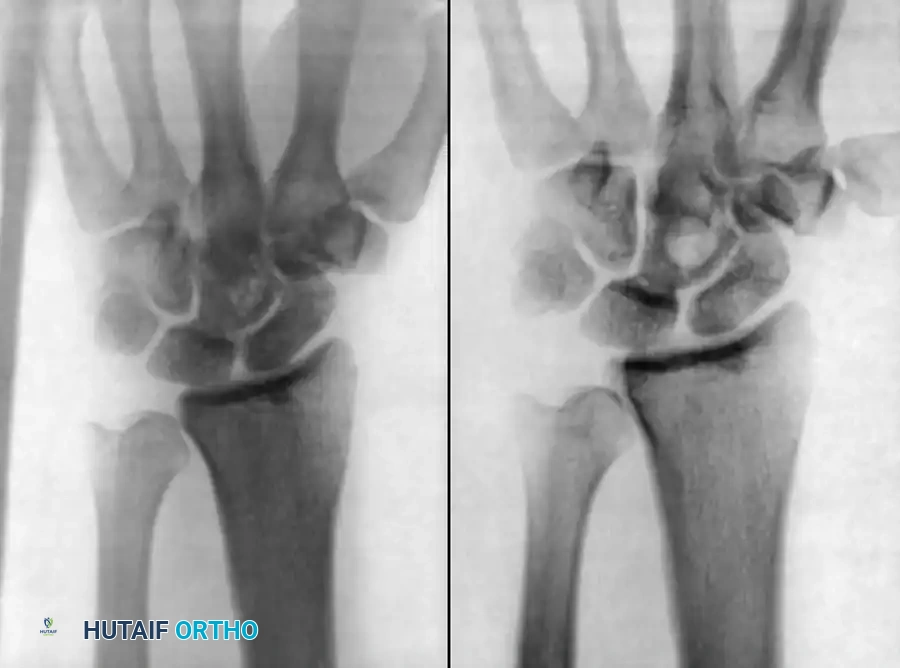
The Ischemic Cascade and Sequestrum Formation
The peculiarity of an abscess within bone is its containment within a rigid, non-expansile cortical structure. As an infection progresses, the inflammatory response generates purulent exudate that significantly increases intraosseous pressure.
- Microvascular Thrombosis: Purulent material tracks through the path of least resistance—the Haversian system and Volkmann canals.
- Periosteal Elevation: The exudate breaches the cortex and lifts the periosteum off the bone surface, stripping the outer cortical blood supply.
- Cortical Necrosis: The combination of purulence in the medullary cavity (compromising endosteal blood supply) and subperiosteal pus (compromising periosteal blood supply) results in the ischemic necrosis of cortical bone.
- Sequestrum and Involucrum: This necrotic, avascular segment of bone is termed a sequestrum. It acts as a permanent nidus, harboring bacteria within a protective biofilm. The surrounding vital bone attempts to wall off the infection by forming a reactive shell of new bone, known as the involucrum.
Clinical Pearl: Because the sequestrum is entirely avascular, systemic antibiotics and host inflammatory cells cannot penetrate it. This anatomical reality dictates that medical therapy alone will inevitably fail in the presence of a sequestrum; radical surgical debridement is mandatory.
Patient-Dependent Risk Factors
The orthopaedic surgeon must meticulously evaluate the risk of infection in every patient. Simply stated, it is exponentially easier to prevent an orthopaedic infection than it is to treat an established one. Patient-dependent factors primarily revolve around nutritional competence and immunological status.
Nutritional Status and Optimization
A patient’s nutritional status dictates their ability to mount a robust humoral and cell-mediated immune response. Malnutrition impairs neutrophil chemotaxis, diminishes bacterial clearance, depresses bactericidal function, and depletes serum complement components.
The basal energy requirements of a traumatized or infected patient surge by 30% to 55% above normal baseline. Furthermore, a fever of just 1ºF above normal increases the body’s metabolic rate by 13%. Jensen et al. demonstrated that up to 42% of patients undergoing orthopaedic surgery are clinically or subclinically malnourished.
Preoperative nutritional screening should include:
* Serum Albumin: Levels < 3.4 g/dL indicate significant protein depletion.
* Total Lymphocyte Count (TLC): Counts < 1500 cells/mm³ suggest impaired immune reserves.
* Transferrin Levels: A sensitive marker for acute protein synthesis.
The Rainey-McDonald Nutritional Index:
This validated formula screens for patients requiring mandatory preoperative nutritional support:
[(1.2 × serum albumin) + (0.013 × serum transferrin)] − 6.43
If the resulting sum is 0 or a negative number, the patient is severely nutritionally depleted and at a high risk for postoperative sepsis. Enteral feeding is the preferred route of optimization if the gastrointestinal tract is functional; otherwise, total parenteral nutrition (TPN) is indicated.
Immunological Status
The host's defense mechanisms rely on neutrophil response, humoral immunity, cell-mediated immunity, and reticuloendothelial function. Deficiencies in any of these arms predispose the patient to specific opportunistic pathogens:
- Neutrophil Abnormalities: Common in diabetes mellitus, alcoholism, and cytotoxic therapy. If the absolute neutrophil count drops below 55/mm³, the patient is at critical risk for Staphylococcus aureus, gram-negative bacilli, Aspergillus, and Candida infections.
- Humoral Immunity (B-cell/Antibody): Patients with hypogammaglobulinemia or those who are asplenic are highly susceptible to encapsulated organisms (Streptococcus pneumoniae, Haemophilus influenzae, Neisseria spp.).
- Cell-Mediated Immunity (T-cell/Macrophage): Secondary deficiencies are common due to corticosteroid therapy, malnutrition, systemic lupus erythematosus (SLE), and HIV/AIDS. These patients are predisposed to mycobacterial, fungal, and Pneumocystis jirovecii infections.
Surgeon-Dependent Factors and Prophylaxis
Skin Preparation and Asepsis
Wound contamination occurs the moment the skin barrier is incised. While absolute sterilization of the skin is impossible due to bacteria residing deep within sebaceous glands and hair follicles, bacterial load can be drastically reduced.
- Antiseptic Agents: Chlorhexidine gluconate provides excellent, sustained bactericidal activity against both gram-positive and gram-negative organisms and is superior to iodophors in residual activity.
- Hair Removal: Shaving the operative site the night before surgery is strictly contraindicated, as it creates micro-abrasions that foster bacterial colonization. If hair removal is necessary, it must be performed with surgical clippers immediately prior to the procedure in the operating room.
- Hand Hygiene: Parienti et al. demonstrated that hand rubbing with an aqueous alcohol solution, preceded by a 1-minute non-antiseptic hand wash for the first case of the day, is as effective as traditional 5-minute antiseptic scrubbing.
Operating Room Environment
Airborne bacteria, originating almost exclusively from the squamous cells shed by operating room personnel, are a primary vector for intraoperative contamination. An individual sheds between 5,000 and 55,000 particles per minute.
- Laminar Airflow: High-efficiency particulate air (HEPA) filtered laminar airflow systems reduce airborne bacterial concentrations by over 80%.
- Airflow Direction: Vertical laminar flow is generally preferred. Salvati et al. noted an increased infection rate with horizontal laminar flow during total joint arthroplasty, as the horizontal current blew bacteria shed by un-isolated scrubbed personnel directly into the sterile surgical field.
- Personnel-Isolator Systems: "Space suits" combined with vertical laminar flow represent the gold standard for minimizing airborne contamination in implant arthroplasty.
Barrier Protection and Gloving
Glove perforation is a silent threat, reported to occur in up to 48% of orthopaedic operations. Perforations most frequently occur on the index finger or thumb of the non-dominant hand.
Surgical Warning: A meta-analysis by Tanner and Parkinson confirmed that double gloving significantly decreases skin contamination. The use of colored indicator gloves (e.g., Biogel) increases the intraoperative awareness of outer glove perforation to 90%. Surgical gloves must be changed every 2 hours during prolonged cases, or immediately after draping and handling power equipment.
Prophylactic Antibiotic Therapy
The efficacy of prophylactic antibiotics hinges on the concept of the "golden period." During the first 2 hours post-contamination, host defenses actively reduce bacterial numbers. Between 2 and 6 hours, bacterial multiplication equals bacterial death. After 6 hours, bacteria multiply exponentially, and biofilm formation begins.
Prophylactic antibiotics must be administered within 60 minutes prior to skin incision to ensure peak tissue concentrations during the "golden period." First-generation cephalosporins (e.g., Cefazolin) remain the gold standard due to their excellent bone penetrance and efficacy against S. aureus. In cases of MRSA colonization or severe beta-lactam allergy, Vancomycin or Clindamycin is indicated.
Surgical Management of Osteomyelitis
When prevention fails and osteomyelitis is established, medical management alone is futile. The orthopaedic surgeon must transition to aggressive surgical eradication. The principles of osteomyelitis surgery are akin to oncological resection: the goal is the complete extirpation of all necrotic and infected tissue.
Indications for Surgery
- Presence of a sequestrum or subperiosteal abscess.
- Failure of clinical improvement after 48-72 hours of appropriate intravenous antibiotic therapy.
- Chronic osteomyelitis with a draining sinus tract.
- Impending pathological fracture due to massive cortical destruction.
Positioning and Tourniquet Considerations
- Positioning: The patient must be positioned to allow extensile exposure of the affected bone and access to potential soft-tissue flap donor sites.
- Tourniquet Use: A pneumatic tourniquet provides a bloodless field, which is critical for distinguishing between viable (bleeding) and necrotic (non-bleeding) bone.
Pitfall: Do not exsanguinate an infected limb with an Esmarch bandage, as this can force purulent material and septic emboli into the systemic circulation. Instead, elevate the limb for 3 to 5 minutes prior to tourniquet inflation.
Step-by-Step Surgical Approach and Debridement
Step 1: Extensile Exposure and Sinus Tract Excision
Utilize standard, extensile orthopaedic approaches. If a draining sinus is present, it should be elliptically excised down to the bone. Methylene blue can be injected into the sinus tract preoperatively to map its arborization and ensure complete excision.
Step 2: Radical Soft Tissue Debridement
Exsect all necrotic, fibrotic, and poorly vascularized soft tissue. Viable muscle will contract when stimulated and bleed freely. "If in doubt, resect it out."
Step 3: Cortical Windowing and Sequestrectomy
Using a high-speed burr or osteotome, create a cortical window over the area of maximal involvement. Identify and extract the sequestrum. The involucrum may be partially resected to gain access, but care must be taken to preserve structural continuity if possible.
Step 4: Intramedullary Reaming and Debridement
The medullary canal must be thoroughly debrided. This can be achieved using intramedullary reamers, curettes, or a motorized burr. Debridement continues until the "paprika sign" is observed—diffuse, punctate bleeding from healthy, viable cortical and cancellous bone.
Step 5: Copious Irrigation
Perform high-volume, low-pressure pulsatile lavage using 6 to 9 liters of normal saline. The addition of antiseptics to the lavage fluid is controversial and generally avoided due to potential osteoblast toxicity; the mechanical washout of the bacterial load is the primary goal.
Step 6: Dead Space Management
Radical debridement inevitably leaves a skeletal defect or "dead space" that will fill with hematoma—an ideal culture medium for recurrent infection.
* Local Antibiotic Delivery: The dead space is typically filled with polymethylmethacrylate (PMMA) beads impregnated with heat-stable antibiotics (e.g., Tobramycin, Vancomycin). This delivers local antibiotic concentrations up to 200 times higher than systemic administration without systemic toxicity.
* Soft Tissue Coverage: The wound must not be closed under tension. If the soft tissue envelope is deficient, a local rotational muscle flap (e.g., gastrocnemius for the proximal tibia) or a free tissue transfer (e.g., latissimus dorsi) is performed by a plastic surgeon to obliterate the dead space and bring a robust blood supply to the ischemic bed.
Postoperative Protocols
Postoperative management requires a multidisciplinary approach involving the orthopaedic surgeon, infectious disease specialist, and plastic surgeon.
1. Systemic Antibiotics: Intravenous antibiotics are tailored to intraoperative deep tissue cultures (minimum of 3-5 distinct samples taken before antibiotic administration). Therapy typically continues for 4 to 6 weeks.
2. Skeletal Stability: If the debridement has compromised the structural integrity of the bone, external fixation is the preferred method of stabilization. Internal fixation is generally avoided in the setting of active, gross purulence.
3. Reconstruction: Once the infection is definitively eradicated (evidenced by normalized CRP/ESR and clean clinical margins), the PMMA beads are removed (usually at 4-6 weeks), and the skeletal defect is reconstructed using autologous bone grafting (e.g., Reamer-Irrigator-Aspirator [RIA] graft from the femur) or bone transport techniques (Ilizarov method).
📚 Medical References
- orthopaedic infection, Clin Orthop Relat Res 335:275, 1997.
- Hernandez RJ, Condway JJ, Poznanski AK, et al: The role of computed tomography and radionuclide scintigraphy in the localization of osteomyelitis in fl at bones, J Pediatr Orthop 5:151, 1985.
- Hoeffel DP, Hinrichs SH, Garvin KL: Molecular diagnostics for the detection of musculoskeletal infection, Clin Orthop Relat Res 360:37, 1999.
- Howard CB, Einhorn M, Dagan R, et al: Ultrasound in diagnosis and management of acute haematogenous osteomyelitis in children, J Bone Joint Surg 75B:79, 1993.
- Howie DW, Savage JP, Wilson TG, et al: The technetium phosphate bone scan in the diagnosis of osteomyelitis in childhood, J Bone Joint Surg 65A:431, 1983.
- Iles SE, Ehrlich LE, Saliken JC, et al: Indium-111 chloride scintigraphy in adult osteomyelitis, J Nucl Med 28:1540, 1987.
- Kattapuram TM, Treat ME, Kattapuram SV: Magnetic resonance imaging of bone and soft tissue infections, Curr Clin Top Infect Dis 21:190, 2001.
- Kohler RB, Wheat LJ: Rapid diagnosis by the detection of microbial antigens, Med Microbiol 1:327, 1982.
- Lamki LM, Kasi LP, Haynie TP: Localization of indium-111 leukocytes in noninfected neoplasms, J Nucl Med 29:1921, 1988.
- Levine BR, Evans BG: Use of blood culture vial specimens in intraoperative detection of infection, Clin Orthop Relat Res 382:222, 2001.
- Lewin JS, Rosenfeld NS, Hoffer PB, et al: Acute osteomyelitis in children: combined Tc-99m and Ga-67 imaging, Radiology 158:795, 1986.
- Loveless MO: The role of susceptibility testing in appropriate selection of antibiotics, Lab Med 17:75, 1986.
- MacLowry JD: Perspective: the serum dilution test, J Infect Dis 160: 624, 1989.
- Magnuson JE, Brown ML, Hauser MF, et al: In-111–labeled leukocyte scintigraphy in suspected orthopedic prosthesis infection: comparison with other imaging modalities, Radiology 168:235, 1988.
- Maurer AH, Chen DCP, Camargo EE, et al: Utility of threephase skeletal scintigraphy in suspected osteomyelitis, J Nucl Med 22:941, 1981.
- Mazur JM, Ross G, Cummings J, et al: Usefulness of magnetic resonance imaging for the diagnosis of acute musculoskeletal infections in children, J Pediatr Orthop 15:144, 1995.
- McAfee JG: What is the best method for imaging focal infections? J Nucl Med 31:413, 1990 (editorial). McCoy JR, Morrissy RT, Seibert JA: Clinical experience with the technetium-99 scan in children, Clin Orthop Relat Res 154:175, 1981.
- Morrissy RT: Bone and joint sepsis. In Morrissy RT, Weinstein SL, eds: Lovell and Winter’s pediatric orthopaedics, 5th ed, Philadelphia, Lippincott-Raven, 2001.
- Patzakis MJ, Wilkins J, Kumbar J, et al: Comparison of the results of bacterial cultures from multiple sites in chronic osteomyelitis of long bones, J Bone Joint Surg 76A:664, 1994.
- Perry CR, Pearson RL, Miller GA: Accuracy of cultures of material from swabbing of the superfi cial aspect of the wound and needle biopsy in the preoperative assessment of osteomyelitis, J Bone Joint Surg 73A:745, 1991.
- Petola H, Vahvanen V, Aalto K: Fever, C-reactive protein and erythrocyte sedimentation rate in monitoring recovery from septic arthritis: a preliminary study, J Pediatr Orthop 4:170, 1984.
- Royle SG: Investigation of the irritable hip, J Pediatr Orthop 12:396, 1992.
- Sartoris DJ: The role of radiology in orthopaedic sepsis, Orthop Rev 16:109, 1987.
- Scott RJ, Christofersen MR, Robertson WWJ, et al: Acute osteomyelitis in children: a review of 116 cases, J Pediatr Orthop 10:649, 1990.
- Shauwecker DS, Braunstein EM, Wheat LJ: Diagnostic imaging of osteomyelitis, Infect Dis Clin North Am 4:441, 1990.
- Sonmezoglu K, Sonmezoglu M, Halac M, et al: Usefulness of 99m Tc-ciprofl oxacin (infection) scan in diagnosis of chronic orthopedic infections: comparative study with 99m Tc-HMPAO leukocyte scintigraphy, J Nucl Med 42:567, 2001.
- Spangehl MJ, Younger AS, Masri BA, et al: Diagnosis of infection following
You Might Also Like