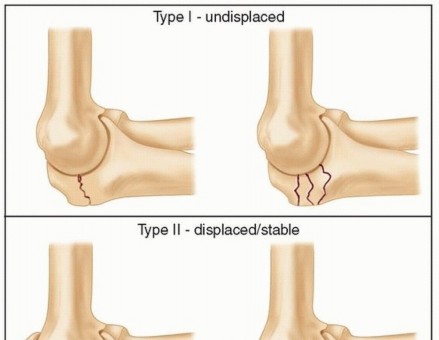
Comprehensive Surgical Management of Monteggia Fractures and Proximal Radioulnar Synostosis
Key Takeaway
The surgical management of chronic Monteggia fracture malunions requires precise ulnar osteotomy and radial head reduction or excision. Post-traumatic proximal radioulnar synostosis, a severe complication, is managed via early anatomical resection or creation of a radial pseudarthrosis. This comprehensive guide details the biomechanics, step-by-step surgical approaches, and evidence-based postoperative protocols for optimizing functional outcomes in complex forearm reconstructions.
INTRODUCTION TO MONTEGGIA FRACTURE MALUNIONS
The Monteggia fracture-dislocation—defined classically as a fracture of the ulnar shaft with a concomitant dislocation of the proximal radioulnar joint (PRUJ) and radiocapitellar joint—remains one of the most challenging injuries in orthopedic trauma. When missed or inadequately treated, it rapidly progresses to a chronic malunion. The biomechanical consequence is profound: the shortened, angulated ulna tethers the radius, preventing spontaneous reduction of the radial head, leading to progressive valgus deformity, tardy ulnar nerve palsy, and severe restriction of forearm pronosupination and elbow flexion.
In the adult population, chronic dislocation of the radial head leads to irreversible morphologic changes to the radiocapitellar articulation, rendering late anatomical reduction impossible or highly prone to stiffness and arthritis. Consequently, the gold standard for adult Monteggia malunions involves ulnar corrective osteotomy combined with radial head excision. Conversely, in the pediatric population, the adaptive capacity of the immature skeleton allows for joint preservation; treatment focuses on ulnar lengthening osteotomy, open reduction of the radial head, and annular ligament reconstruction.
Surgical Pearl: The fundamental principle of Monteggia reconstruction is that "the ulna dictates the radius." The radius is a curved bone that rotates around a straight ulnar axis. Restoring the anatomical length and alignment of the ulna is the absolute prerequisite for addressing the radial head pathology.
PREOPERATIVE EVALUATION AND BIOMECHANICS
Thorough preoperative planning requires high-quality orthogonal radiographs of the entire forearm, including true anteroposterior (AP) and lateral views of the elbow and wrist. The radiocapitellar line must be assessed; in a normal elbow, a line drawn through the center of the radial shaft and head should bisect the capitellum in every radiographic plane.
In the setting of a malunion, the ulnar deformity is typically apex-anterior (Bado Type I equivalent), though apex-posterior (Bado Type II) and lateral (Bado Type III) variants occur. Advanced imaging, such as a 3D-reconstructed CT scan, is highly recommended to quantify the exact degree of ulnar malrotation, angular deformity, and the presence of any intra-articular loose bodies or heterotopic ossification at the PRUJ.

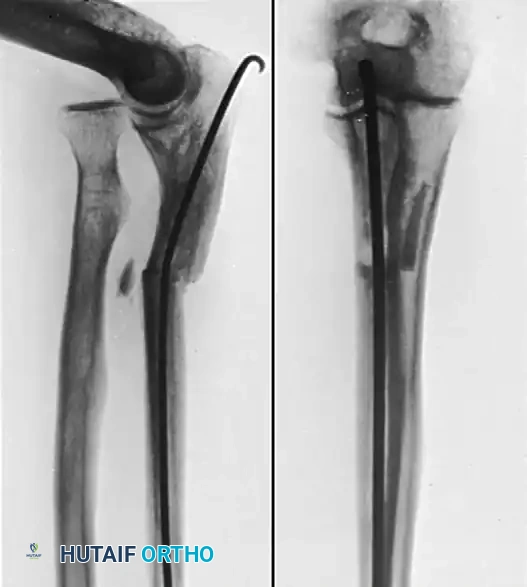
Figure 1: Preoperative radiograph demonstrating a malunited fracture of the ulnar shaft with an intramedullary nail in situ, accompanied by a chronic dislocation of the proximal radius (Monteggia fracture malunion).
SURGICAL TECHNIQUE: ADULT MONTEGGIA MALUNION RECONSTRUCTION
The operative strategy for an adult with a symptomatic Monteggia malunion involves a dual-incision approach (or a single extensile Boyd approach), excision of the deformed radial head, and a corrective osteotomy of the ulna with rigid internal fixation.
1. Patient Positioning and Setup
The patient is placed in the supine position with the affected arm extended on a radiolucent hand table. A non-sterile pneumatic tourniquet is applied high on the brachium. The iliac crest is prepped and draped simultaneously in the event that structural autograft is required, though the excised radial head often provides excellent local autogenous cancellous bone graft.
2. Surgical Approaches
The surgeon may choose to expose the radial head and the malunion of the ulna through a single extensile posterior incision (the Boyd approach), which exploits the interval between the anconeus and the extensor carpi ulnaris (ECU). However, to minimize soft tissue stripping and the risk of radioulnar synostosis, a two-incision technique is highly preferred.
The Posterolateral (Kocher) Incision:
* Make a 5 cm posterolateral incision centered over the radial head.
* Develop the interval between the anconeus and the ECU.
* Incise the joint capsule to expose the dislocated radial head.
* Carefully free the radial head from all of its fibrotic attachments and capsular adhesions.
The Posterior Ulnar Incision:
* Make a second incision, approximately 7.5 cm long, directly over the subcutaneous border of the posterior aspect of the ulna, centered over the apex of the malunion.
* Elevate the ECU and flexor carpi ulnaris (FCU) subperiosteally just enough to apply a dynamic compression plate.
3. Radial Head Excision
In chronic adult cases, the radial head is hypertrophied and the capitellum is often flattened. Attempting reduction will severely limit motion.
* Identify the bicipital tuberosity. The posterior interosseous nerve (PIN) must be protected by keeping the forearm in pronation, which moves the nerve anteriorly away from the surgical field.
* Divide the neck of the radius just proximal to the bicipital tuberosity.
* To prevent splintering of the radial neck, drill several holes transversely through the bone at the level of the anticipated osteotomy.
* Complete the division of the bone using double-action bone-cutting forceps while gently rotating the radial shaft.
* Smooth the remaining end of the radial neck with a small rongeur or rasp to prevent impingement against the ulna during rotation.
* Graft Preparation: The excised radial head is fragmented and morselized on the back table to be used as autogenous bone graft for the ulnar osteotomy.
4. Ulnar Osteotomy and Fixation
- Expose the ulnar malunion. If previous hardware is present (e.g., an intramedullary nail), remove it carefully.
- Perform the osteotomy as near to the old fracture site (the apex of the deformity) as possible. A transverse or short oblique osteotomy is created using an oscillating saw under continuous saline irrigation.
- Align the fragments properly, restoring the anatomical ulnar bow.
- Fix the osteotomy rigidly with a 3.5 mm limited-contact dynamic compression plate (LC-DCP) or locking compression plate (LCP). Ensure at least six cortices of fixation proximal and distal to the osteotomy.
- Place the autogenous cancellous bone (harvested from the radial head) circumferentially around the osteotomy site to promote rapid union.
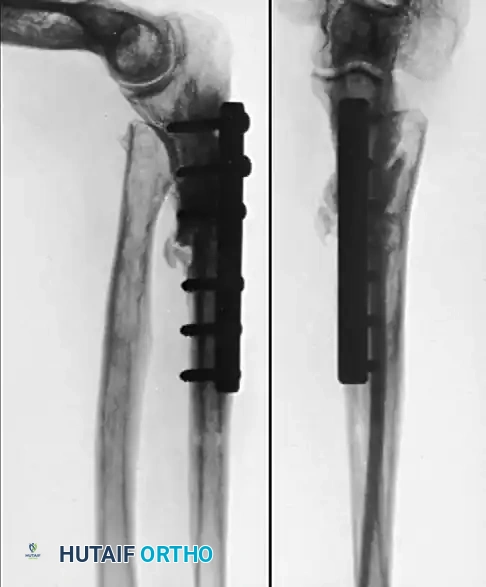
Figure 2: Four months postoperative radiograph. The intramedullary nail has been removed, the ulna has undergone corrective osteotomy with application of a compression plate, and the radial head was excised, fragmented, and utilized for grafting the ulna. Motion of the elbow and forearm is excellent.
Pediatric Consideration: We have achieved highly satisfactory results in children with malunited Monteggia fractures treated by an opening-wedge angulation-distraction osteotomy of the ulna, open reduction of the radial head, and temporary fixation with transarticular radiocapitellar Kirschner wires. The K-wires maintain the reduction until the bone and reconstructed annular ligament have healed (typically 3 to 4 weeks). Radial head excision is strictly contraindicated in the growing skeleton due to the risk of proximal radial migration, cubitus valgus, and longitudinal growth arrest.
5. Postoperative Care
Following rigid fixation, the arm is immobilized in a long-arm cast or a well-padded posterior splint with the elbow at 90 degrees of flexion and the forearm in neutral rotation.
* The cast is worn until clinical and radiographic union is solid, which usually occurs at about 12 weeks.
* Once union is confirmed, the cast is discontinued, and an aggressive regimen of active and active-assisted range-of-motion exercises is initiated to restore elbow flexion/extension and forearm pronosupination.
PROXIMAL RADIOULNAR SYNOSTOSIS
Synostosis between the radius and the ulna is a devastating complication that abolishes forearm rotation. It most frequently develops at the proximal radioulnar joint following severely comminuted fractures in this region, particularly when fractures of both bones occur at the same level, or following extensive surgical dissection (such as the single-incision Boyd approach for Monteggia fractures).
Jupiter and Ring Classification
Understanding the anatomical extent of the synostosis is critical for surgical planning. Jupiter and Ring classified proximal radioulnar synostosis into three distinct types based on anatomical location:
* Type A: Synostosis located at or distal to the bicipital tuberosity.
* Type B: Synostosis involving the radial head and the proximal radioulnar joint directly.
* Type C: Synostosis contiguous with bone extending across the elbow joint to the distal aspect of the humerus (extra-articular ankylosis).
Timing of Surgical Intervention: The Paradigm Shift
Historically, orthopedic dogma dictated a mandatory delay in operative treatment for 6 to 12 months after the initial injury. The rationale was to allow the heterotopic bone to fully mature, theoretically decreasing the risk of recurrence.
However, modern evidence challenges this delay. Jupiter and Ring suggested that early resection is preferable. Their rationale is that early intervention limits the degree of secondary soft tissue contracture, prevents capsular fibrosis, and significantly reduces the overall period of severe patient disability. In their series of 17 patients (18 synostoses), operative resection yielded good results in 16 patients.
* Excision 6 to 12 months after the initial injury did not increase the risk of recurrence.
* Patients with earlier resections demonstrated statistically better ultimate range of motion than those treated later.
* The only recurrence of synostosis in their cohort occurred in a patient with a concomitant severe closed head injury (traumatic brain injury), a known profound risk factor for aggressive heterotopic ossification.
Surgical Warning: The ultimate range of motion following synostosis resection is not significantly affected by the size or location of the synostosis, the severity of the initial trauma, or the use of a free nonvascularized fat graft. The most critical factor is meticulous, atraumatic surgical technique and the complete excision of the bony bridge.
Prophylaxis Against Recurrence
The necessity of prophylactic measures remains a topic of intense academic debate. No adjunctive radiotherapy or nonsteroidal anti-inflammatory drugs (NSAIDs) were used in the Jupiter and Ring cohort, leading them to question the absolute need for these measures, as well as the necessity of using interpositional fat grafts to prevent recurrence.
Conversely, other authors have observed superior results with fewer complications after early excision of the synostosis mass when combined with interposition material (such as pedicled muscle flaps, free fat grafts, or synthetic barriers) and a short course of prophylactic Indomethacin or single-fraction low-dose radiation therapy (700 cGy). The decision to use prophylaxis should be tailored to the patient's risk profile, particularly in those with central nervous system trauma or a history of recurrent heterotopic ossification.
Alternative Technique: Creation of a Radial Pseudarthrosis
While the most common and direct treatment of proximal radioulnar synostosis is the anatomical resection of the bony bridge, this is not always technically feasible. In cases of massive, recurrent, or intra-articular synostosis, the creation of a pseudarthrosis of the radius distal to the synostosis has been utilized as a salvage procedure to restore forearm rotation.
The Kamineni Procedure:
Kamineni et al. reported a highly effective, safe, and reliable method of improving forearm rotation by resecting a 1-cm thick section of the proximal radial shaft, effectively bypassing the ankylosed PRUJ.
* Outcomes: At an almost 7-year follow-up, forearm rotation improved dramatically from an average fixed pronation of 5 degrees to an average functional arc of motion of 98 degrees.
* Recurrence: Reankylosis occurred in only one patient. Notably, this was the only patient in whom the resection was performed proximal to the bicipital tuberosity. Therefore, the osteotomy must be performed distal to the tuberosity to prevent proximal re-fusion.
* Technical Pearl: Kamineni et al. noted that the single most important technical factor influencing positive results was the generous application of bone wax at the resection site to mechanically block osteogenesis and ensure the persistence of the pseudarthrosis.
Indications for Radial Pseudarthrosis:
This procedure is highly recommended as a simple, safe alternative to formal synostosis resection in patients who present with a proximal radioulnar synostosis that:
1. Is too extensive or massive to allow a safe and discrete resection without jeopardizing neurovascular structures.
2. Involves the articular surface extensively, where resection would leave a highly unstable or painful joint.
3. Is associated with a severe anatomical deformity of the proximal forearm.
Clinical Pitfall: The pseudarthrosis technique should not be considered a first-line alternative to the anatomical removal of the synostosis when it is technically possible to excise a discrete bridge of bone. Anatomical restoration should always be the primary goal, with pseudarthrosis reserved for complex, un-resectable, or recurrent cases.
CONCLUSION
The management of Monteggia fracture malunions and post-traumatic radioulnar synostosis requires a profound understanding of forearm biomechanics and meticulous surgical execution. For the adult Monteggia malunion, ulnar corrective osteotomy combined with radial head excision provides reliable restoration of function. In the pediatric population, joint preservation is paramount. When complicating synostosis arises, early anatomical resection is advocated to prevent debilitating soft tissue contractures. In unsalvageable cases, the creation of a distal radial pseudarthrosis serves as an excellent, evidence-based salvage technique to restore the critical arc of forearm pronosupination.
📚 Medical References
You Might Also Like