Unlocking Faster Healing: Internal Fixation Devices Explained
Key Takeaway
For anyone wondering about Unlocking Faster Healing: Internal Fixation Devices Explained, Fracture healing rate is influenced by several factors. Cancellous bone heals faster (around 6 weeks) than cortical bone (9-18 weeks). Children's fractures unite rapidly with excellent remodeling, a process that slows with age. Maintaining stability, often through an internal fixation device or other methods, is crucial as excessive mobility at the fracture site impedes healing and callus formation.
FACTORS AFFECTING THE RATE OF HEALING OF A FRACTURE
1 TYPE OF BONE
Cancellous bone (spongy bone)
Healing in cancellous bone is generally well advanced 6 weeks from the time of the injury, and protection of the fracture can almost invariably be abandoned by that time. This applies to fractures of bones which are composed principally of cancellous tissue, and also to fractures involving the cancellous bone to be found at the ends of long bones. This rule is illustrated in the following examples:
1 Weight bearing after a fracture of the calcaneus may be permitted after about 6 weeks.
2 A patient with a traumatic wedge fracture of a vertebral body may commence full mobilisation after 6 weeks.
3 Plaster fixation may be discarded after 5–6 weeks following a Colles fracture of the wrist.
4 Weight may be allowed through the leg 6 weeks after a fracture of the tibial plateau.
5 Bed rest for 6 weeks is usually advised for any fracture of the pelvis involving those parts through which weight transmission is mediated.
Cortical bone (Compact bone)
Endosteal callus may take many months to become reasonably well established, and many uncomplicated long bone fractures may take 9–18 weeks to unite. In some cases, however, abundant external bridging callus may allow an earlier return of function. For example:
1 The average time to union of a fracture of the tibial shaft treated conservatively is 16 weeks.
2 Fractures of the humeral shaft can often be left unsupported after 10 weeks.
3 On the other hand, fractures of the metatarsals, metacarpals and phalanges, where external bridging callus is usually substantial, are usually quite firm in 4–5 weeks.
2 PATIENT AGE
In children, union of fractures is rapid. The speed of union decreases as age increases until skeletal maturity is reached. There is then not a great deal of difference in the rate between young adults and the elderly. For example, in a child, union may be expected in a fractured femur a little after the number of weeks equivalent to its numerical age have passed: viz. a fractured femur in a child of 3 years is usually united after 4 weeks; a fractured femur in a child of 8 years is usually sound after 9 weeks. In contrast, a fracture of the femoral shaft in an adult may take 3–6 months to unite.
Apart from great rapidity of union it should be noted that children have remarkable powers of remodelling fractures. These powers are excellent as far as displacement is concerned, and are often good for slight to moderate angulation. Remodelling is poor in the case of axial rotation in both adults and children. The power to remodel decreases rapidly once adolescence is reached and epiphyseal fusion is imminent.
3 MOBILITY AT THE FRACTURE SITE
Excessive mobility persisting at the fracture site (due, for example, to poor fixation) may interfere with vascularisation of the fracture haematoma; it may lead to disruption of early bridging callus and may prevent endosteal new bone growth. One of the main aims of all forms of internal and external splintage is to reduce mobility at the fracture site, and hence encourage union. Absolute rigidity, however, may discourage external callus formation, so that reliance is placed on the internal fixation device – typically a plate – until the long process of endosteal union is complete. Nevertheless, if splintage is inadequate, union may be delayed or prevented.
4 SEPARATION OF BONE ENDS
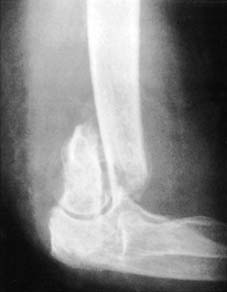
1
Supracondylar fracture of humerus with soft tissue between bone ends.
Union will be delayed or prevented if the bone ends are separated, for this interferes with the normal mechanisms of healing. (The converse is also true, namely that compression of the fracture facilitates union.) Separation may occur under several circumstances:
1
Interposition of soft tissue between the bone ends.
For example, in fractures of the femoral shaft, one of the bone ends may become isolated from the other by herniating through some of the surrounding muscle mass, thereby delaying or preventing union. Fractures of the medial malleolus may fail to unite due to infolding of a layer of periosteum between the fragments.
2
Excessive traction.
Excessive traction employed in the maintenance of a reduction may lead to separation of the bone ends and non-union. This may occur, for example, in femoral shaft fractures, particularly those treated by skeletal traction.
3
Following internal fixation.
In some situations where internal fixation is used to hold a fracture, absorption of bone may occur at the fracture site; the fixation device may continue to hold the bone fragments in such a way that they are prevented from coming together; and mechanical failure may ensue. A bulky internal fixation device may in itself interfere with the local blood supply and the fracture haematoma. Where possible, steps should be taken to avoid this (e.g. by using a LISS plate with locking screws and a minimally invasive technique).
5 BONE LOSS
This is comparatively rare, with the tibia and femur being most commonly affected; even less common is significant loss in the humerus and forearm bones. The main causes are bone extrusion in open fracture at the site of the causal incident or during transport, bone removal occurring during debridement procedures, and injuries due to gunshots or explosions. Loss most commonly affects the diaphysis; loss of metaphyseal or articular bone is generally associated with high-energy dissipation injuries.
If the loss is substantial then treatment will be prolonged and difficult, and because of the mechanism of injury many of these cases have accompanying problems with skin loss, tissue contamination, and accompanying neural and vascular damage. Other factors such as the patient’s age and medical state, and other injuries will influence the management of the case. The first decision that must be made is therefore whether amputation is the best approach. This is not always easy, and the general view is that this must be decided on a completely individual assessment of the factors involved. While use of the Mangled Extremity Severity Index (see p. 51) may help in taking all the important factors into account, it has been shown to be somewhat unreliable in evaluating those cases where it indicates that amputation should be performed.
Where it has been decided not to amputate, an appropriate method of fixation of the fracture must be chosen. The procedure to be adopted depends on the site and extent of the bone loss, and other local factors. In the femur, tibia and humerus (unless there is any contraindication), locked intramedullary nails generally give the best support for losses up to 6 cm, and at the later stages, with the newer devices, may allow bone lengthening procedures to be carried out. Autogenous bone grafting may also be required. In the forearm, and also in the case of the humerus, plates and screws are usually employed. External fixators may also be used, although unilateral frames do not give sufficient support where there is a significant segmental defect in the leg. In this case, the Ilizarov and other circular frames are of particular value, especially when subsequent bone lengthening is planned, and may be employed where the defect exceeds 6 cm.
The general approach is to fix the fracture at its true length, paying particular attention to rotation. However, where the skin poses a problem it is often useful to allow initial shortening of the limb while aiming to correct this later with a subsequent limb lengthening procedure.
There are many other approaches to dealing with the vagaries of these injuries. These include calcium phosphate cement which may be used for small metaphyseal or calcaneal defects; allografts, particularly in young patients with loss of a portion of a joint surface; vascularised fibular grafts, especially in the forearm; the creation of a one-bone forearm or lower leg; the use of bone substitutes and bone growth factors; and joint replacement procedures where there is a substantial loss of articular surfaces.
6 INFECTION
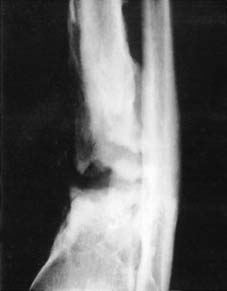
2
Chronic bone infection and failure of union of tibia following plating (plate removed).
Infection in the region of a fracture may delay or prevent union. This is especially the case if, in addition, movement is allowed to occur at the fracture. Infection of the fracture site is extremely rare in conservatively treated closed fractures; infection, if it occurs, follows either an open injury or one treated by internal fixation. Where infection becomes well established in the presence of an internal fixation device, it is often difficult to achieve healing without removal of the device which acts as a foreign body and a nidus for persisting infection. This is especially the case if there is breakdown of the overlying skin and the establishment of a sinus. Not infrequently the situation arises where cast fixation alone is unable to provide the degree of fixation necessary for union if the device is removed, and where infection is likely to remain if it is not. In such circumstances it is usually wiser to retain the fixation device until union is reasonably well advanced, or to consider using an external fixator. In some cases where sound healing can be obtained and maintained after removal of an internal fixation device, it may be possible to repeat the internal fixation in the sterile environment that has been obtained.
MRSA Infections
Established infections with methicillin-resistant staphylococcus aureus may pose enormous problems: for the patient, in extreme cases, with risk of life, and in others to the prolongation of treatment and inferior results; for surgeons and nursing staff, with difficulties in management; and overall, with the greatly increased cost implications. The extent of the problem and the procedures adopted to deal with it vary from country to country, but many measures are common to all. In the UK, Giannoudis and others
1
suggest the following protocol for the identification of MRSA carriers, and the treatment of an established infection.
1 Strict adherence to national guidelines for screening in high-risk areas with:
(a) Screening on admission for all regional/national referral centres, while high-risk areas should screen the following patients: those known to be previously affected or colonised; frequent re-admissions; those transferred from MRSA-infected wards or nursing homes; and those transferred from hospital abroad.
(b) Discharge screening.
(c) Screening of the nose, perineum, skin lesions and manipulated sites of all other patients after a single case has been detected.
(d) Isolation of carriers.
(e) Screening of all staff if additional cases occur.
(f) Isolation of patients before negative swab results have been received. On identification of positive swab cultures for MRSA, the patients should be kept in isolation.
2 Treatment of carriers as outlined in the national guidelines with:
(a) The use of nasal muciprocin for 5 days, repeated if further swabs show persistent colonization.
(b) Bathing in antiseptic detergents such as 4% chlorhexidine or 2% triclosan for patients carrying MRSA at any site. This may be repeated if the strain is not eradicated.
(c) Application of hexachlorophane powder to the axilla and groin, if they are thought to be colonized.
(d) Treatment of throat carriers is not required but, if undertaken, this normally requires systemic treatment with rifampicin and fusidic acid, or ciprofloxacin.
3 Administration for 5 days of nasal muciprocin in combination with a triclosan bath on the day of surgery to all patients scheduled to receive implanted prosthetic material.
4 Education of nursing and medical staff on hand hygiene which is effective, although compliance is poor.
5 Treatment of an established infection initially with vancomycin while the patient is in hospital. Treicoplanin or linezolid can then be given on an out-patient basis. The length of administration should be decided by the treating clinician.
7 DISTURBANCE OF BLOOD SUPPLY
It is obvious that for the normal multiplication of bone cells and their precursors an adequate blood supply is required. Where the blood supply to an area is reduced, or where there is interference with the blood supply to both major fragments – e.g. in radionecrosis of bone – healing may be interfered with. On the other hand, reduction of the blood supply to one fragment, especially if cancellous bone is involved, may not interfere with union; indeed, in some situations it may apparently stimulate it. The most striking examples of this are fractures of the femoral neck and scaphoid, where the phenomenon of avascular necrosis is most frequently discovered in soundly united fractures. Interference with the blood supply to one fragment at the time of injury leads to immediate bone death; this is frequently followed by sound union of the fracture. Collapse of necrotic bone beyond the level of union is observed at a later date.
Again, a bulky internal fixation device may in itself interfere with the local blood supply and the fracture haematoma, delaying union. Where possible this should be avoided by choosing the most appropriate device.
8 PROPERTIES OF THE BONE INVOLVED
Fracture healing is also affected by a number of imperfectly understood factors which lead to variations in the speed of union. The clavicle is a spectacular example; non-union is extremely rare, the time to clinical union is unexcelled by any other part of the skeleton, yet movement at the fracture site cannot be controlled with any efficiency. Union of the tibia is often slow to a degree that is difficult to explain even when the influence of its nutrient artery and fracture mobility are taken into account.
9 OTHER FACTORS
1
Effects of smoking.
Smoking has a deleterious effect on fracture union, often being a significant factor in the rate and quality of union.
2
Joint involvement.
When a fracture involves a joint, union is occasionally delayed. This may be due to dilution of the fracture haematoma by synovial fluid.
3
Bone pathology.
Many of the commonest causes of pathological fracture do not seem to delay union in a material way. (Union may progress quite normally in, for example, osteoporosis, osteomalacia, Paget’s disease and most simple bone tumours.) Some primary and secondary malignant bone tumours may delay or prevent union (see pp 110–113).
4
HIV/AIDS.
In humankind the HIV virus encodes its RNA within host cells, particularly CD4 (T-helper) lymphocytes, resulting in their depletion and an adverse effect on immunity. Effective retroviral therapy reduces the viral load in the serum and helps restore the CD4 cells. The level of these cells in the serum forms a valuable indicator of the severity of the infection and response to any treatment. Infections should be graded. This may be done on clinical grounds, using the four stages advocated by the World Health Organization, or by using a combination of clinical signs and CD4 levels (which results in 12 grades of severity) as described by the Centre for Disease Control and Prevention.
In closed fractures, and as a general rule, conservative methods of treatment are to be preferred wherever possible. Nevertheless, infections occurring in cases treated by internal fixation appear to be due mainly to contamination rather than an impaired immunity response, and open methods may be pursued so long as strict attention is paid to asepsis and careful tissue handling. Prophylactic antibiotics in the form of a first generation cephalosporin have been recommended by Harrison.
2
In open fractures, if internal fixation is used, the rate of infection is often unacceptably high, and this line of treatment should be avoided where possible. In the case of the tibia an external fixator may be used, although an increase in pin-track infections should be anticipated. It need hardly be stated that in every case the strictest precautions must be taken to avoid the operator being exposed to the infected tissues and serum of the patient.
In any fracture case if there is an increase in the rate of non-union, it may generally be dealt
withsuccessfully by internal fixation and bone grafting.
NEXT
COMPLICATIONS OF FRACTURES
You Might Also Like