Understanding Normal Bone Metabolism: Your Body's Blueprint
Key Takeaway
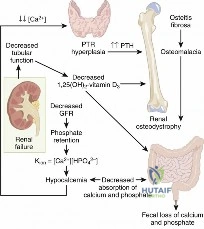
In this comprehensive guide, we discuss everything you need to know about Understanding Normal Bone Metabolism: Your Body's Blueprint. Normal bone metabolism is a dynamic process essential for skeletal health and mineral balance. It is primarily regulated by parathyroid hormone (PTH) and 1,25(OH)2D3, alongside calcitonin. These hormones homeostatically control serum calcium and phosphate levels by influencing intestinal absorption, reabsorption in the kidney, and bone remodeling to maintain proper body function.
Introduction and Epidemiology
Bone metabolism represents a highly dynamic and complex physiological process essential for maintaining skeletal structural integrity and mineral homeostasis. For the orthopedic surgeon, a profound understanding of normal bone metabolism is not merely an academic exercise but a fundamental prerequisite for managing fractures, performing arthroplasty, and treating metabolic bone diseases. The skeletal system serves as the primary reservoir for essential minerals, continuously undergoing remodeling to repair microdamage and adapt to mechanical loads according to Wolff’s law.

Metabolic bone disorders, including osteoporosis, osteomalacia, and Paget disease of bone, significantly alter the biomechanical properties of the skeleton, thereby complicating surgical interventions. Osteoporosis remains the most prevalent metabolic bone disease, characterized by a systemic deterioration of bone microarchitecture and a resultant increase in fragility fracture risk. Conversely, Paget disease represents a localized disorder of bone remodeling, driven by initial rampant osteoclastic activity followed by disorganized osteoblastic bone formation. The incidence of heterotopic ossification after total hip arthroplasty (THA) among patients with Paget disease is notably high, approximating 50%, which necessitates meticulous perioperative management and prophylactic strategies in this high-risk population. Understanding the baseline physiological blueprint of calcium and phosphate metabolism is critical for optimizing surgical outcomes and mitigating complications in these vulnerable cohorts.
Surgical Anatomy and Biomechanics
Calcium Homeostasis and Distribution
Calcium is a vital ubiquitous cation, critically important in muscle and nerve function, the coagulation cascade, and numerous intracellular signaling pathways. In the human body, more than 99% of total calcium is stored within the crystalline structure of bone, primarily as hydroxyapatite. The remaining fraction is distributed within the extracellular fluid and soft tissues. Plasma calcium exists in two roughly equal fractions: an ionized, physiologically active free state, and a protein-bound state (predominantly bound to albumin).
The dynamic nature of bone is evidenced by the continuous exchange of minerals; approximately 400 mg of calcium is released from the skeletal reservoir into the extracellular fluid daily through osteoclastic resorption. Intestinal absorption of calcium occurs via two distinct mechanisms. In the duodenum, calcium is absorbed via an active transport mechanism that requires adenosine triphosphate (ATP) and a specific intracellular calcium-binding protein (calbindin). This active pathway is tightly regulated by 1,25-dihydroxyvitamin D3 (1,25(OH)2D3). Conversely, in the jejunum, calcium is absorbed through passive paracellular diffusion, which is concentration-dependent. Renal conservation of calcium is highly efficient, with the kidney reabsorbing approximately 98% of the filtered calcium load. The majority of this reabsorption (approximately 60%) occurs in the proximal convoluted tubule. Unabsorbed or secreted calcium may be excreted in the stool.
Phosphate Distribution and Function
Phosphate is a key structural component of bone mineral, with approximately 85% of the body’s total phosphate stores sequestered within the skeletal system. Unlike calcium, plasma phosphate exists mostly in an unbound state. Beyond its structural role, phosphate is indispensable in various enzyme systems, cellular energetics (ATP synthesis), and molecular interactions, functioning as a critical intracellular metabolite and extracellular buffer. Dietary intake of phosphate is usually adequate in standard diets, with a daily physiological requirement ranging from 1000 to 1500 mg. Renal regulation is the primary determinant of phosphate homeostasis, with the bulk of filtered phosphate being reabsorbed by the proximal tubule of the kidney. Excess phosphate is readily excreted in the urine.

Cellular Biomechanics and Endocrine Mediators
The primary homeostatic regulators of serum calcium and phosphate are parathyroid hormone (PTH) and 1,25(OH)2D3. PTH is an 84-amino acid peptide synthesized in and secreted from the chief cells of the four parathyroid glands. The biological activity of PTH resides in its N-terminal fragment, specifically amino acids 1-34. At the cellular level, the effect of PTH is mediated by the cyclic adenosine monophosphate (cAMP) second-messenger mechanism downstream, primarily acting on osteoblasts and osteocytes, which subsequently regulate osteoclastic activity via the RANKL/OPG pathway. This delicate balance dictates the biomechanical strength of the bone, as excessive PTH leads to cortical thinning and increased porosity, severely compromising the pull-out strength of orthopedic implants.
Indications and Contraindications
The intersection of metabolic bone disease and orthopedic surgery frequently requires a nuanced approach to both operative and non-operative management. The decision to intervene surgically versus pursuing pharmacological optimization depends heavily on the patient's underlying bone metabolism, fracture morphology, and systemic health.
Teriparatide, the synthetic form of recombinant human PTH, contains the active 1-34 amino acid sequence and is utilized as a potent anabolic agent to treat severe forms of osteoporosis. By administering Teriparatide intermittently, it stimulates osteoblastic bone formation, thereby improving trabecular microarchitecture and cortical thickness. However, its use carries a theoretical increased risk of osteosarcoma, observed in preclinical rodent models. Consequently, it is contraindicated in patients with Paget disease, unexplained elevations in alkaline phosphatase, prior skeletal radiation therapy, or open epiphyses.

| Clinical Scenario | Operative Indications | Non-Operative Indications | Contraindications to Surgery |
|---|---|---|---|
| Osteoporotic Fragility Fractures | Displaced femoral neck fractures; Unstable intertrochanteric fractures; Displaced intra-articular fractures. | Nondisplaced proximal humerus fractures; Stable compression fractures; Isolated pubic rami fractures. | Unacceptable anesthetic risk; Active localized infection; Non-ambulatory baseline (relative for certain joint reconstructions). |
| Atypical Femur Fractures (AFF) | Complete fractures; Incomplete fractures with intractable pain or progressive radiolucent lines despite conservative care. | Asymptomatic incomplete fractures (managed with prophylactic restricted weight-bearing and cessation of bisphosphonates). | Severe medical comorbidities precluding anesthesia; Active systemic bacteremia. |
| Paget Disease of Bone | Impending pathological fractures (subtrochanteric); Severe secondary osteoarthritis requiring arthroplasty; Deformity correction. | Asymptomatic bowing; Mild to moderate pain controlled with bisphosphonates. | Hypervascular phase without prior medical optimization (high risk of catastrophic hemorrhage). |
Pre Operative Planning and Patient Positioning
Optimization of Bone Metabolism and Dietary Requirements
Preoperative planning for patients with compromised bone metabolism requires meticulous attention to systemic mineral balance. Orthopedic surgeons must ensure that patients meet their dietary requirements for elemental calcium to support postoperative fracture healing and implant osseointegration. The physiological demand for calcium varies significantly across the lifespan:
* Approximately 600 mg/day for children.
* Approximately 1300 mg/day for adolescents and young adults (ages 10–25 years) to support peak bone mass acquisition.
* 750 mg/day for adults ages 25–50 years.
* 1200–1500 mg/day for adults over age 50 years.
* 1500 mg/day for pregnant women.
* 2000 mg/day for lactating women.
* 1500 mg/day for postmenopausal women and critically, for the patient with a healing fracture in a long bone.
It is important to note that calcium balance is usually positive in the first three decades of life, transitioning to a negative balance after the fourth decade, which underscores the necessity of preoperative laboratory evaluation (serum calcium, phosphorus, 25-hydroxyvitamin D, and intact PTH) in older adults undergoing elective arthroplasty or complex fracture fixation.

Patient Positioning Considerations
Patients with severe osteoporosis or advanced Paget disease require extreme care during intraoperative positioning. The altered biomechanics and decreased cortical thickness predispose these patients to iatrogenic fractures during routine manipulation.
* Traction Tables: When utilizing a fracture table for intramedullary nailing of the femur, traction must be applied gradually. Excessive rotational or longitudinal force can easily result in iatrogenic fractures of the ipsilateral or contralateral limb.
* Padding and Support: All bony prominences must be meticulously padded. In patients with severe kyphosis due to osteoporotic vertebral compression fractures, standard supine positioning may compromise respiratory mechanics or lead to cervical spine injury; customized ramped positioning may be required.
* Tourniquet Application: Tourniquets should be applied over generous padding, and inflation pressures should be minimized to the lowest effective pressure to avoid crushing osteopenic bone or causing significant soft tissue necrosis in the setting of calcified, non-compliant vessels.
Detailed Surgical Approach and Technique
When addressing pathology in the setting of altered bone metabolism, the surgical approach and fixation techniques must be rigorously adapted. The standard principles of rigid internal fixation often fail in osteoporotic bone due to inadequate screw purchase and poor bone-implant interface mechanics.
Approach and Soft Tissue Handling
Regardless of the anatomical site, the surgical approach must prioritize the preservation of the periosteal blood supply. In osteoporotic bone, the periosteum is often the primary source of osteoprogenitor cells required for secondary fracture healing.
1. Internervous Planes: Strict adherence to true internervous and intermuscular planes is mandatory to minimize collateral soft tissue trauma.
2. Retractor Placement: Avoid the use of aggressive Hohmann retractors directly against osteoporotic diaphyseal bone, as this can easily cause cortical perforation or iatrogenic fracture propagation.
3. Reduction Techniques: Direct clamping of osteoporotic bone with point-reduction forceps (e.g., Weber clamps) frequently results in crushing of the thin cortical shell. Indirect reduction techniques, utilizing traction, joysticks, or percutaneous methods, are strongly preferred to maintain the structural integrity of the fracture fragments.
Fixation Strategies in Poor Bone Stock
The biomechanical goal in osteoporotic fracture fixation is to distribute forces over the widest possible area to prevent implant cut-out or pull-out.
1. Load-Sharing Implants: Intramedullary (IM) nailing is generally preferred over extramedullary plating for lower extremity diaphyseal and metaphyseal fractures, as IM devices sit closer to the mechanical axis, reducing the bending moment and stress on the implant-bone interface.
2. Fixed-Angle Devices: When plating is necessary, locked plating constructs are essential. Locking screws function as fixed-angle devices, relying on the threaded screw-head to plate interface rather than friction between the plate and the bone. This significantly increases the pull-out strength in cancellous bone.
3. Working Length: Surgeons should utilize longer plates to span the comminuted or osteoporotic segments, decreasing the stress concentration at the ends of the construct. The screw density should be optimized—typically placing screws in the most proximal and distal holes, leaving empty holes over the fracture site to increase the working length and allow for flexible fixation, which promotes callus formation.
4. Augmentation: In cases of severe osteoporosis, the use of polymethylmethacrylate (PMMA) bone cement or calcium phosphate cement to augment screw purchase (e.g., in the femoral head for intertrochanteric fractures or in the proximal humerus) may be indicated.
5. Managing Paget Disease: Surgery in Pagetic bone presents unique technical challenges. During the active phase, the bone is highly vascular, and excessive intraoperative hemorrhage is a significant risk; preoperative treatment with intravenous bisphosphonates or calcitonin is often necessary to reduce disease activity and vascularity. In the sclerotic phase, the bone is dense, brittle, and prone to microfractures. Reaming of the medullary canal for IM nailing can be exceptionally difficult and may require specialized, sharp reamers and careful advancement to avoid thermal necrosis or catastrophic shattering of the diaphysis.

Complications and Management
Altered bone metabolism significantly increases the perioperative complication profile. The orthopedic surgeon must be adept at anticipating, recognizing, and managing these specific challenges.
Heterotopic Ossification
Heterotopic ossification (HO) is a frequent and debilitating complication following orthopedic trauma and arthroplasty. The incidence of heterotopic ossification after THA among patients with Paget disease is exceptionally high, approaching approximately 50%. Prophylactic measures are mandatory in this high-risk cohort. While non-steroidal anti-inflammatory drugs (NSAIDs) like indomethacin or targeted localized radiation therapy are standard prophylactic modalities, optimizing systemic calcium homeostasis also plays a role in managing bone turnover in these patients.
Atypical Femur Fractures
Long-term suppression of normal bone metabolism via bisphosphonate therapy can lead to severely suppressed bone turnover, manifesting clinically as atypical femur fractures (AFFs). These fractures typically occur in the subtrochanteric or diaphyseal region following minimal or no trauma. They are characterized by a transverse or short oblique configuration, localized periosteal reaction (lateral cortical beaking), and lack of comminution. Surgical management usually involves cephalomedullary nailing. However, due to the suppressed remodeling, delayed union and nonunion are common, often requiring prolonged periods of restricted weight-bearing, cessation of the antiresorptive agent, and consideration of anabolic therapy like Teriparatide.
| Complication | Incidence / Risk Factors | Prevention and Salvage Strategies |
|---|---|---|
| Heterotopic Ossification | ~50% in Paget disease post-THA; High risk in acetabular fractures, head trauma. | Prevention: Indomethacin (75mg sustained release or 25mg TID for 3-6 weeks); Single-dose localized radiation (700-800 cGy) within 24-48 hours pre/post-op. Salvage: Surgical excision once mature (typically >6 months), followed by immediate radiation/NSAID prophylaxis. |
| Implant Cut-Out / Pull-Out | High in severe osteoporosis (T-score < -3.0), particularly proximal femur and humerus. | Prevention: Use of locked plating, longer constructs, cement augmentation, and anatomical reduction to restore medial cortical support. Salvage: Revision to arthroplasty (e.g., hemiarthroplasty for failed proximal humerus ORIF) or revision fixation with structural allograft. |
| Atypical Femur Fracture Nonunion | 10-25% following IM nailing of bisphosphonate-related AFFs. | Prevention: Prophylactic nailing of symptomatic incomplete fractures; meticulous reaming and use of larger diameter nails; immediate cessation of bisphosphonates. Salvage: Exchange nailing, teriparatide administration (off-label use for fracture healing), autologous bone grafting. |
| Catastrophic Hemorrhage | High during elective surgery in the active (osteolytic/mixed) phase of Paget disease. | Prevention: Preoperative optimization with potent intravenous bisphosphonates (e.g., zoledronic acid) to suppress disease activity and vascularity prior to elective arthroplasty or osteotomy. Salvage: Rapid intraoperative hemostasis, utilization of cell-saver, aggressive blood product resuscitation. |
Post Operative Rehabilitation Protocols
Rehabilitation following orthopedic surgery in patients with compromised bone metabolism requires a delicate balance between early mobilization to prevent systemic complications (e.g., deep vein thrombosis, pneumonia, deconditioning) and the protection of tenuous internal fixation.
Weight-Bearing Restrictions
Unlike young patients with normal skeletal integrity who may be permitted immediate weight-bearing as tolerated following rigid intramedullary fixation of long bone fractures, osteoporotic patients frequently require modified protocols.
* Lower Extremity: Depending on the stability of the construct and the degree of comminution, partial weight-bearing (e.g., 20-30 lbs flat-foot touch) may be mandated for 6 to 8 weeks to prevent catastrophic implant failure. However, in geriatric hip fractures (femoral neck or intertrochanteric), the standard of care remains immediate weight-bearing as tolerated to minimize mortality, accepting the higher risk of mechanical failure in favor of systemic survival.
* Upper Extremity: Following proximal humerus or distal radius fixation in osteoporotic bone, early passive range of motion is encouraged to prevent adhesive capsulitis, but active resistive exercises and weight-bearing through the upper extremity must be delayed until radiographic evidence of bridging callus is observed.
Pharmacological Continuation and Optimization
Postoperative management must include the resumption or initiation of medical therapies to optimize bone metabolism.
* Adequate dietary or supplemental intake of calcium (1200-1500 mg/day for older adults) and Vitamin D (typically 800-1000 IU/day minimum, targeting serum 25(OH)D levels >30 ng/mL) must be confirmed.
* For patients sustaining a fragility fracture, this represents a sentinel event. The orthopedic surgeon must ensure the patient is evaluated for secondary causes of osteoporosis and initiated on appropriate pharmacological therapy (e.g., bisphosphonates, RANKL inhibitors like denosumab, or anabolic agents like Teriparatide) to mitigate the risk of subsequent fractures. The timing of initiation of antiresorptive therapy post-fracture remains debated, though most guidelines suggest initiating bisphosphonates within 2 to 12 weeks postoperatively to avoid theoretical interference with early soft callus formation.
Summary of Key Literature and Guidelines
Understanding the complex endocrine regulation of calcium and phosphate is paramount for the academic orthopedic surgeon. The primary homeostatic regulators—PTH, 1,25(OH)2D, and Calcitonin—exert specific effects on the intestine, kidney, and bone to maintain a narrow physiological window of serum mineral concentrations.
The interplay of these hormones forms the basis for pharmacological interventions in metabolic bone disease. For instance, the therapeutic efficacy of Teriparatide relies on the paradoxical anabolic effect of intermittent PTH exposure, contrasting with the catabolic effect of chronic endogenous PTH elevation seen in hyperparathyroidism.
The following table summarizes the foundational physiological parameters governing calcium and phosphate metabolism, serving as a critical reference for understanding both normal homeostasis and the pathophysiological deviations encountered in clinical practice.
Regulation of Calcium and Phosphate Metabolism Parameter
| Parameter | PTH (Peptide) | 1,25(OH)2D (Steroid) | Calcitonin (Peptide) |
|---|---|---|---|
| Origin | Chief cells of parathyroid glands | Proximal tubule of kidney | Parafollicular cells of thyroid gland |
| Factors stimulating production | Decreased serum Ca2+ | Elevated PTH level Decreased serum Ca2+ level Decreased serum Pi |
Elevated serum Ca2+ level |
| Factors inhibiting production | Elevated serum Ca2+ Elevated 1,25(OH)2D |
Decreased PTH Elevated serum Ca2+ Elevated serum Pi |
Decreased serum Ca2+ |
| Effect on Intestine | No direct effect. Acts indirectly on bowel by stimulating production of 1,25(OH)2D in kidney | Strongly stimulates intestinal absorption of Ca2+ and Pi | Unknown / Minimal |
| Effect on Kidney | Stimulates 25(OH)D 1α-hydroxylase in mitochondria of proximal tubular cells to convert 25(OH)D to 1,25(OH)2D Increases fractional resorption of filtered Ca2+ Promotes urinary excretion of Pi |
Unknown / Minimal | Unknown / Minimal |
| Effect on Bone | Stimulates osteoclastic resorption of bone Stimulates recruitment of preosteoclasts |
Strongly stimulates osteoclastic resorption of bone | Inhibits osteoclastic resorption of bone ? Role in normal human physiology |
| Net effect on Ca2+ and Pi concentrations in extracellular fluid and serum | Increased serum Ca2+ level Decreased serum Pi level |
Increased serum Ca2+ level Increased serum Pi level |
Decreased serum Ca2+ level |
Through rigorous adherence to these fundamental principles of bone metabolism, the orthopedic surgeon can optimize preoperative planning, execute biomechanically sound surgical techniques, and implement comprehensive postoperative rehabilitation protocols, thereby ensuring the highest standard of care for patients with complex metabolic skeletal disorders.
Clinical & Radiographic Imaging





