Total Knee Arthroplasty (TKA): Epidemiology, Surgical Anatomy & Biomechanics
Key Takeaway
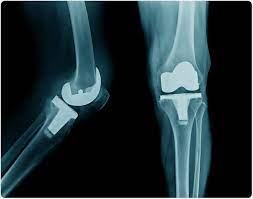
Total Knee Arthroplasty (TKA) is a common orthopedic procedure for severe knee arthritis, aiming to relieve pain and restore function. Its rising prevalence is driven by an aging population. Understanding the knee's complex surgical anatomy, including bony landmarks, ligaments, muscles, nerves, and biomechanics, is crucial for successful TKA outcomes.
Introduction & Epidemiology
Total Knee Arthroplasty (TKA), also referred to as total knee replacement, stands as one of the most successful and frequently performed orthopedic procedures globally. Its primary objective is the alleviation of intractable pain, restoration of functional mobility, and correction of debilitating deformity in patients afflicted with end-stage degenerative, inflammatory, or post-traumatic knee arthropathy. The evolution of TKA from early hinge designs to modern constrained and unconstrained condylar prostheses has been marked by significant advancements in biomechanical understanding, materials science, and surgical technique, leading to predictable and durable outcomes.
Epidemiologically, the prevalence of TKA continues to rise, driven by an aging global population, increasing life expectancy, and a growing burden of osteoarthritis (OA). OA is the predominant indication for TKA, with its incidence correlating positively with factors such as advanced age, elevated body mass index (BMI), previous knee injury, and genetic predisposition. Data from national registries, such as those maintained by the American Joint Replacement Registry (AJRR) and the National Joint Registry for England, Wales, Northern Ireland and the Isle of Man (NJR), consistently demonstrate an upward trend in TKA volume. Projections suggest a continued increase, with some estimates predicting a 189% increase in primary TKA procedures by 2030 in the United States alone. While OA accounts for approximately 90% of all TKAs, other indications include rheumatoid arthritis (RA), psoriatic arthritis, ankylosing spondylitis, post-traumatic arthritis, avascular necrosis, and select cases of bone tumors or severe congenital deformities. The demographic profile of TKA recipients typically involves individuals in their sixth to eighth decades of life, though a modest increase in younger, more active patients is also observed, raising considerations regarding implant longevity and activity restrictions. The socio-economic impact of TKA is substantial, encompassing improved quality of life, reduced healthcare utilization for pain management, and enhanced participation in daily and recreational activities for millions worldwide.
Surgical Anatomy & Biomechanics
A thorough understanding of knee anatomy and biomechanics is paramount for successful TKA. The knee is a complex diarthrodial joint, primarily a modified hinge joint, formed by the articulation of the distal femur, proximal tibia, and patella.
Bony Anatomy
- Distal Femur: Comprises the medial and lateral condyles, which articulate with the tibial plateau. The intercondylar notch separates the condyles and houses the cruciate ligaments. Anteriorly, the trochlear groove accommodates the patella. Key landmarks for resection include the epicondyles (medial for MCL origin, lateral for LCL origin), which are critical for establishing the flexion-extension axes, and the Whiteside's line (perpendicular to the deepest part of the trochlear groove), used for femoral component rotation.
- Proximal Tibia: Features the medial and lateral tibial plateaus, separated by the intercondylar eminence. The tibial tubercle provides the insertion for the patellar tendon. Proper tibial cut necessitates consideration of the varus/valgus alignment (typically 90° to the mechanical axis of the tibia) and posterior slope (typically 3-7°), which influences sagittal stability and range of motion.
- Patella: A sesamoid bone within the quadriceps tendon, articulating with the trochlear groove. Its posterior surface features medial and lateral facets, crucial for patellofemoral tracking and force transmission.
Ligamentous Anatomy
The stability of the knee is largely conferred by its robust ligamentous apparatus.
*
Collateral Ligaments:
The medial collateral ligament (MCL) originates from the medial femoral epicondyle and inserts onto the medial tibial condyle, providing primary restraint to valgus stress. The lateral collateral ligament (LCL) originates from the lateral femoral epicondyle and inserts onto the fibular head, providing primary restraint to varus stress. Both are critical for mediolateral stability throughout the range of motion and are key targets for soft tissue balancing during TKA.
*
Cruciate Ligaments:
The anterior cruciate ligament (ACL) and posterior cruciate ligament (PCL) are intra-articular and provide anteroposterior stability. In TKA, the ACL is routinely resected. The PCL may be retained (PCL-retaining designs) or sacrificed (PCL-substituting designs). PCL-retaining designs aim to preserve natural knee kinematics, while PCL-substituting designs use a cam-post mechanism to provide posterior stability.
Musculotendinous Anatomy
The quadriceps femoris mechanism (rectus femoris, vastus medialis, vastus lateralis, vastus intermedius) is the primary extensor of the knee. The patellar tendon connects the patella to the tibial tubercle. The hamstring muscles (semimembranosus, semitendinosus, biceps femoris) are the primary flexors. The gastrocnemius also contributes to knee flexion. Surgical approaches must meticulously manage these structures to preserve their integrity and function.
Neurovascular Anatomy
The popliteal artery and its genicular branches are located posteriorly, making them vulnerable during posterior capsule release or severe posterior osteophyte resection. The common peroneal nerve courses around the fibular neck laterally, at risk during lateral releases or correction of severe valgus deformities. The saphenous nerve is a sensory nerve that can be injured during medial skin incisions or medial releases.
Joint Kinematics & Biomechanics
Normal knee kinematics involves a combination of rolling and gliding movements, coupled with axial rotation during flexion, a phenomenon known as the "screw-home mechanism." The goal of TKA is to restore stable, pain-free motion. Key biomechanical considerations include:
*
Mechanical Alignment:
Traditionally, TKA aims to achieve a neutral mechanical axis (0° varus/valgus) from the center of the femoral head to the center of the ankle, passing through the center of the knee. This involves precise bone resections and soft tissue balancing to create rectangular flexion and extension gaps.
*
Kinematic Alignment:
An emerging concept that seeks to restore the native joint line and individual patient kinematics by making femoral and tibial resections parallel to the patient's pre-arthritic joint lines.
*
Soft Tissue Balancing:
Crucial for achieving equal and rectangular flexion and extension gaps, ensuring proper ligament tension throughout the range of motion, and preventing instability or stiffness. This often involves selective releases of contracted capsular or ligamentous structures.
*
Patellofemoral Tracking:
Essential for pain-free motion. Influenced by component rotation, tibiofemoral rotation, Q-angle, and soft tissue releases.
Indications & Contraindications
Indications for Total Knee Arthroplasty
The decision to proceed with TKA is multifaceted, requiring careful consideration of patient symptoms, functional limitations, radiographic findings, and the failure of non-operative management.
Primary Operative Indications:
*
Severe, persistent debilitating pain:
Pain that significantly interferes with activities of daily living (ADLs), sleep, and quality of life, refractory to conservative treatment.
*
Functional limitation:
Significant impairment in ambulation, stair climbing, rising from a chair, or other essential activities due to pain, stiffness, or deformity.
*
Radiographic evidence of end-stage arthropathy:
Typically Kellgren-Lawrence Grade III or IV osteoarthritis, characterized by joint space narrowing, osteophytes, subchondral sclerosis, and subchondral cysts.
*
Significant deformity:
Fixed varus, valgus, or flexion contracture that is symptomatic and contributes to instability or functional deficit.
*
Failure of adequate non-operative management:
A documented trial of conservative therapies, including physical therapy, analgesics (NSAIDs, acetaminophen), corticosteroid injections, viscosupplementation, activity modification, weight loss, and bracing, without sustained relief for a minimum of 3-6 months.
*
Specific diagnoses:
* Primary osteoarthritis (most common).
* Inflammatory arthritis (e.g., rheumatoid arthritis, psoriatic arthritis).
* Post-traumatic arthritis.
* Avascular necrosis (AVN) of the femoral condyles.
* Certain benign or low-grade malignant tumors of the distal femur or proximal tibia, where reconstruction with arthroplasty is appropriate.
* Revision of failed prior knee surgery (e.g., osteotomy, unicompartmental knee arthroplasty).
Contraindications for Total Knee Arthroplasty
Contraindications can be absolute or relative, necessitating a nuanced approach to patient selection.
Absolute Contraindications:
*
Active systemic or local infection:
Active sepsis, osteomyelitis around the knee, or acute periprosthetic joint infection (PJI). Arthroplasty in the presence of infection carries an unacceptably high risk of chronic PJI.
*
Extensor mechanism disruption:
A compromised or deficient quadriceps mechanism (e.g., irreparable quadriceps tendon rupture, patellar tendon rupture, or severe patella alta/baja) may preclude effective rehabilitation and functional recovery.
*
Neuropathic arthropathy (Charcot joint):
Rapidly progressive joint destruction and instability due to neurological deficits (e.g., diabetes, syphilis, spinal cord injury) often lead to early aseptic loosening and failure.
*
Severe vascular compromise:
Critical limb ischemia or severe peripheral vascular disease that may compromise wound healing or predispose to infection.
*
Inability to comply with rehabilitation:
Patients unwilling or unable to participate in a rigorous post-operative rehabilitation program are unlikely to achieve optimal outcomes.
Relative Contraindications:
*
Morbid obesity (BMI > 40 kg/m²):
Associated with increased risks of infection, VTE, wound complications, early aseptic loosening, and less favorable functional outcomes. Weight loss prior to surgery is strongly encouraged.
*
Uncontrolled diabetes mellitus (HbA1c > 8%):
Significantly increases infection risk and impairs wound healing.
*
Severe psychiatric disorders or cognitive impairment:
May affect compliance with rehabilitation and informed consent.
*
Chronic opioid use:
Associated with poorer pain control post-operatively, prolonged hospital stays, and increased risk of complications. Pre-operative opioid weaning is recommended.
*
Poor skin condition around the knee:
Active dermatological conditions, severe venous stasis dermatitis, or extensive scarring may complicate wound healing.
*
Severe osteoporosis:
May compromise implant fixation, increasing risk of periprosthetic fracture and aseptic loosening.
*
Significant cardiovascular, pulmonary, or renal comorbidities:
Increase perioperative risk. Requires medical optimization.
*
Prior knee arthrodesis:
While challenging, TKA can be performed in select cases to restore motion, though outcomes may be less predictable.
*
Younger age:
While not an absolute contraindication, TKA in patients under 50-55 years old is considered carefully due to increased activity demands and potential for earlier revision.
Summary of Indications
| Category | Operative Indications | Non-Operative Indications |
|---|---|---|
| Symptoms | Severe, debilitating pain at rest/activity | Mild-to-moderate pain, manageable with conservative measures |
| Function | Significant limitation in ADLs, ambulation, transfers | Minimal to no functional impairment |
| Radiographic | Kellgren-Lawrence Grade III-IV osteoarthritis | Early-stage osteoarthritis (Grade I-II), minimal joint degeneration |
| Conservative Tx | Failure of documented 3-6 months of non-operative management | Sufficient relief from non-operative treatments |
| Deformity | Fixed varus, valgus, or flexion contracture affecting stability | Minimal or correctable deformity |
| Specific Dx | Primary OA, Inflammatory Arthritis, Post-traumatic Arthritis, AVN | No underlying end-stage arthropathy |
| Patient Factors | Medically optimized, compliant, realistic expectations | Contraindications to surgery, patient preference for non-surgical options |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is crucial for optimizing outcomes and minimizing complications in TKA.
Patient Evaluation
- Comprehensive Medical History: Assess comorbidities (cardiovascular disease, pulmonary disease, diabetes, renal insufficiency), previous surgeries, allergies, and current medications (especially anticoagulants, antiplatelets, insulin, chronic opioids). Identify risk factors for VTE, infection, and poor wound healing.
-
Physical Examination:
- Gait analysis: Observe walking pattern, use of assistive devices.
- Deformity assessment: Quantify varus/valgus alignment, flexion contracture, and fixed deformities.
- Range of Motion (ROM): Document active and passive flexion and extension.
- Ligamentous stability: Assess collateral ligament integrity.
- Extensor mechanism integrity: Palpate patellar tendon, quadriceps tendon.
- Neurovascular status: Palpate pulses, assess sensation and motor function (especially peroneal nerve).
- Skin integrity: Note any rashes, wounds, or venous stasis changes.
- Functional Assessment: Utilize validated patient-reported outcome measures (PROMs) such as KOOS, WOMAC, or SF-36 to establish a baseline.
- Psychological Evaluation: Assess for depression, anxiety, and unrealistic expectations, which can influence recovery and satisfaction.
Radiographic Assessment
-
Standard Radiographs:
- Standing Anteroposterior (AP) view: Assesses joint space narrowing, osteophytes, and mechanical axis.
- Lateral view (with weight-bearing if possible): Evaluates sagittal plane deformity (flexion contracture, posterior tibial slope), osteophytes, and patellar height (Insall-Salvati ratio).
- Merchant (patellofemoral) view: Assesses patellar tracking and patellofemoral arthritis.
- Long-leg alignment views (hip-to-ankle): Essential for accurate measurement of the mechanical axis and planning coronal plane correction.
- Templating: Utilize digital or traditional templates on radiographs to estimate appropriate component sizes (femoral, tibial, patellar) and position, ensuring restoration of joint line and appropriate sizing.
-
Advanced Imaging:
- MRI: Rarely indicated for routine TKA, but useful in cases of suspected AVN, tumor, or occult ligamentous injury.
- CT scan: Employed for complex deformities, pre-operative planning for patient-specific instrumentation (PSI), or robotic-assisted TKA to generate 3D models.
Pre-Optimization
- Medical Clearance: Obtain comprehensive medical evaluation and clearance from primary care physician or internist to ensure the patient is optimized for surgery.
- Diabetes Control: Optimize glycemic control (HbA1c < 8%) to reduce infection risk.
- Smoking Cessation: Encourage cessation for at least 4-6 weeks pre-operatively to improve wound healing and reduce pulmonary complications.
- Nutritional Optimization: Address malnutrition; consider vitamin D supplementation.
- Dental Clearance: Rule out active dental infections, which can be a source of bacteremia leading to PJI.
- Medication Management: Manage anticoagulants/antiplatelets according to institutional protocols, typically stopping warfarin 5 days pre-op, novel oral anticoagulants (NOACs) 2-3 days pre-op, and aspirin/NSAIDs 7-10 days pre-op.
- Pre-habilitation: Pre-operative physical therapy can improve quadriceps strength, range of motion, and patient education, potentially accelerating post-operative recovery.
Anesthesia Planning
Collaborate with the anesthesia team to determine the optimal anesthetic approach (general vs. regional, e.g., spinal/epidural) and develop a multimodal pain management strategy (nerve blocks, NSAIDs, acetaminophen, local infiltration analgesia) to minimize opioid requirements.
Patient Positioning
- Supine Position: The patient is positioned supine on the operating table.
- Leg Holder/Bumper: The ipsilateral leg is placed in a leg holder or supported by a bump to allow full flexion and extension without obstruction. The contralateral leg is typically placed in an abducted, flexed position to avoid interference with surgical instruments and maintain patient comfort.
- Hip Bump: A small bump under the ipsilateral hip helps internally rotate the leg and facilitates a neutral mechanical axis.
- Tourniquet: A pneumatic tourniquet is applied to the proximal thigh to provide a bloodless surgical field. Inflation pressure typically ranges from 250-350 mmHg, or 100-150 mmHg above systolic blood pressure.
- Sterile Preparation and Draping: The limb is thoroughly prepped with an antiseptic solution (e.g., chlorhexidine-alcohol or povidone-iodine) extending from the foot to the mid-thigh. Sterile draping isolates the surgical field, maintaining strict asepsis. The surgical technician or assistant often holds the foot to manipulate the limb throughout the procedure.
Detailed Surgical Approach / Technique
The goal of TKA is the precise resection of damaged articular surfaces, restoration of mechanical alignment, and balanced soft tissues, followed by stable implantation of prosthetic components. The medial parapatellar approach is the most widely adopted technique.
General Principles
- Asepsis: Strict adherence to sterile technique throughout the procedure to prevent infection.
- Tourniquet Control: Inflated tourniquet maintained throughout the bone cutting and component implantation phases to minimize blood loss and provide a clear surgical field.
- Exposure: Adequate exposure is critical for precise bone cuts and soft tissue balancing.
- Bone Resection: Performed with jigs or navigation/robotics to ensure accurate alignment and sizing.
- Soft Tissue Balancing: Essential for equal and rectangular flexion and extension gaps.
- Component Implantation: Secure cementation (or press-fit for selected components) of femoral, tibial, and patellar implants.
- Wound Closure: Meticulous layered closure to minimize dead space and promote healing.
Medial Parapatellar Approach
This is the most common and versatile approach, offering excellent exposure.
- Skin Incision: A straight longitudinal incision is made anteriorly, typically starting 2-3 cm proximal to the superior pole of the patella, extending distally to the medial aspect of the tibial tubercle. The incision should be centered over the patella for optimal exposure.
- Subcutaneous Dissection: Dissection proceeds through subcutaneous fat to expose the deep fascia and the medial border of the patella.
- Medial Parapatellar Arthrotomy: The arthrotomy incision begins proximally by incising the quadriceps tendon just medial to its midline, extending distally along the medial border of the patella, and then through the medial retinaculum, stopping just medial to the patellar tendon. Care is taken to protect the infrapatellar branch of the saphenous nerve during the distal portion of the incision.
- Patellar Eversion: The patella is everted laterally, bringing the articular surface into view. This provides direct access to the femoral condyles and tibial plateau. If patellar eversion is difficult (e.g., tight extensor mechanism, large thigh, flexion contracture), a limited VMO release or quadriceps snip may be necessary, though these risk weakening the extensor mechanism.
- Fat Pad Excision: The infrapatellar fat pad (Hoffa's fat pad) is typically partially excised to improve exposure, particularly of the anterior tibia.
- Excision of Osteophytes and Menisci: Large osteophytes are removed from the intercondylar notch and around the joint margins. The damaged menisci are completely excised. The cruciate ligaments are addressed: the ACL is routinely resected, and the PCL is either preserved or resected depending on the chosen implant design.
Bone Resection Sequence
The sequence may vary slightly based on surgeon preference and instrumentation, but generally follows:
-
Femoral Resection (Distal First):
- Distal Femoral Cut: A valgus cutting guide is used to resect the distal femur. The valgus angle (typically 5-7°) is determined by the patient's anatomical valgus angle to achieve a perpendicular cut to the mechanical axis of the femur. Intramedullary or extramedullary guides can be used. This cut establishes the extension gap.
- Posterior Condylar Cuts: With the knee in 90° flexion, a four-in-one or five-in-one cutting block is applied to resect the posterior femoral condyles, creating the posterior chamfer, anterior chamfer, and anterior femoral cuts. The rotation of this block is crucial for patellofemoral tracking and soft tissue balance, often referenced from the transepicondylar axis or Whiteside's line. These cuts establish the flexion gap.
-
Tibial Resection:
- Proximal Tibial Cut: An extramedullary or intramedullary guide is used to resect the proximal tibia. The cut is typically made perpendicular to the mechanical axis of the tibia in the coronal plane and with 3-7° of posterior slope in the sagittal plane, replicating native anatomy. This cut must be precise to avoid violating the proximal tibiofibular joint or compromising the patellar tendon insertion.
-
Patellar Resurfacing (Optional but Common):
- The patella is prepared by resecting the posterior articular cartilage. Multiple small holes are drilled to create a vascular bed. The patellar component, typically a polyethylene button, is cemented onto the resected surface. Careful attention is paid to tracking and thickness restoration.
Soft Tissue Balancing
This is perhaps the most critical step for achieving a functional TKA. The goal is to create symmetrical, rectangular flexion and extension gaps, ensuring equal tension in the medial and lateral soft tissues throughout the range of motion.
*
Extension Gap Balancing:
If the knee remains in varus or valgus in extension after bone cuts, releases are performed. For varus deformity, a medial release may involve sequential release of the deep MCL, semi-membranosus, and superficial MCL. For valgus deformity, a lateral release may involve the posterolateral capsule, popliteus tendon, and LCL.
*
Flexion Gap Balancing:
If the knee remains tight in flexion, the posterior capsule or osteophytes may need further release. If the flexion gap is too loose, options are limited and may require thicker polyethylene or a more constrained implant.
*
PCL Management:
If PCL-retaining, its tension is assessed. If PCL-substituting, the PCL is resected, and the femoral component design will provide the necessary posterior stability.
Trial Components and Final Implantation
- Trial Insertion: Trial femoral, tibial, and patellar components are inserted. The knee's range of motion, stability (varus/valgus, AP), and patellar tracking are meticulously assessed. Adjustments to soft tissue releases, polyethylene insert thickness, or component rotation may be made at this stage.
-
Definitive Implantation:
Once optimal balance and tracking are achieved, the definitive components are cemented in place.
- Bone surfaces are prepared with pulsatile lavage and dried. Cement is applied to the bone surfaces and component undersides.
- The femoral component is impacted and held.
- The tibial tray is impacted and held.
- Excess cement is meticulously removed to prevent impingement.
- The polyethylene insert is then snapped into the tibial tray.
- The patellar button is cemented (if performed).
Closure
- Capsular Repair: The medial parapatellar capsule and retinaculum are repaired with interrupted sutures, restoring the extensor mechanism.
- Subcutaneous Layers: Deep fascial and subcutaneous layers are closed to obliterate dead space.
- Skin Closure: Skin is closed with staples or absorbable sutures.
- Dressing: A sterile, compressive dressing is applied. A drain may be placed selectively, though its routine use is diminishing.
Complications & Management
Despite high success rates, TKA is associated with a range of potential complications, both early and late. Vigilant monitoring and prompt intervention are critical for optimal outcomes.
Early Complications (within 30-90 days post-op)
-
Infection (Periprosthetic Joint Infection - PJI):
- Incidence: 0.5-2%.
- Presentation: Pain, swelling, erythema, warmth, fever, purulent drainage.
- Diagnosis: Joint aspiration (elevated synovial WBC, PMN%, positive culture), elevated ESR/CRP.
-
Management:
- Acute onset (<4-6 weeks post-op): Debridement, antibiotics, and implant retention (DAIR) in selected cases.
- Chronic or failed DAIR: Two-stage revision arthroplasty (explantation, antibiotic spacer, prolonged antibiotics, reimplantation) is the gold standard. Single-stage revision may be considered for highly selected cases with susceptible organisms.
- Recalcitrant infection: Arthrodesis, excision arthroplasty, or amputation (rare).
-
Venous Thromboembolism (VTE):
- Incidence: Symptomatic DVT 0.5-1%, PE 0.1-0.5% with prophylaxis.
- Presentation: DVT (calf pain, swelling, tenderness), PE (dyspnea, chest pain, tachycardia).
- Management: Anticoagulation (LMWH, DOACs, warfarin). Prophylaxis protocols are standardized (pharmacological and mechanical).
-
Periprosthetic Fracture:
- Incidence: Intraoperative <1%, postoperative 0.5-2%.
- Presentation: Acute pain, inability to bear weight, deformity.
-
Management:
- Intraoperative: Depends on fracture location and stability. May involve ORIF with plates/screws, or revision with a longer stem or constrained implant.
- Postoperative: Typically managed with ORIF or revision TKA depending on fracture type, location, implant stability, and bone quality.
-
Neurovascular Injury:
- Incidence: Peroneal nerve palsy 0.3-2% (more common in valgus knees), popliteal artery injury <0.1%.
- Presentation: Peroneal nerve (foot drop, numbness lateral lower leg/dorsum of foot); Popliteal artery (absent pulses, pallor, cold limb).
-
Management:
- Peroneal nerve: Observation, foot drop orthosis. Exploration/neurolysis in cases of known compression or transection.
- Popliteal artery: Immediate vascular surgery consultation for exploration and repair.
-
Arthrofibrosis / Stiffness:
- Incidence: 2-10%.
- Presentation: Limited range of motion (<90° flexion, >10° flexion contracture), pain.
- Management: Aggressive physical therapy, manipulation under anesthesia (MUA) (typically 6-12 weeks post-op if ROM plateaued), arthroscopic or open lysis of adhesions.
-
Patellar Complications:
- Incidence: Fracture (0.5-3%), avascular necrosis (AVN) (rare), maltracking/subluxation/dislocation (<1%).
- Management: Depends on severity; fracture (non-op vs. ORIF vs. patellectomy), maltracking (lateral retinacular release, revision patellar component).
Late Complications (months to years post-op)
-
Aseptic Loosening:
- Incidence: 1-5% at 10 years.
- Presentation: Gradual onset of pain, particularly with activity, often mechanical in nature. Radiographic evidence of lucency at bone-cement interface.
- Management: Revision TKA.
-
Polyethylene Wear and Osteolysis:
- Incidence: Decreasing with newer materials, but still a concern.
- Presentation: Similar to aseptic loosening. Inflammatory response to wear particles leads to bone resorption.
- Management: Revision TKA, often involving polyethylene exchange and bone grafting for osteolytic lesions.
-
Instability:
- Incidence: 1-3%.
- Presentation: Sensation of "giving way," recurrent effusions, pain. Can be flexion, extension, or mid-flexion instability.
- Management: Revision TKA with appropriate soft tissue balancing, increased constraint, or larger components.
-
Periprosthetic Infection (late hematogenous spread):
- Incidence: Can occur years post-op from distant infection.
- Management: Same as acute PJI.
-
Patellar Clunk Syndrome:
- Incidence: Less common with modern designs.
- Presentation: A painful clunking sensation during knee extension, typically around 30-45° flexion, due to fibrous nodule impinging in the intercondylar notch.
- Management: Arthroscopic debridement of the fibrous nodule.
Summary of Common Complications and Management
| Complication | Incidence (approx.) | Common Presentation | Salvage Strategy / Management |
|---|---|---|---|
| Periprosthetic Infection | 0.5-2% | Pain, swelling, erythema, fever, drainage | DAIR (acute), 2-stage revision (gold standard), 1-stage revision (selected), arthrodesis, excision arthroplasty, amputation. |
| Venous Thromboembolism | 0.5-1% (symptomatic) | DVT (calf pain/swelling), PE (dyspnea, chest pain) | Therapeutic anticoagulation (LMWH, DOACs, warfarin). Strict pre- and post-op prophylaxis protocols. |
| Periprosthetic Fracture | <1% (intra-op), 0.5-2% (post-op) | Acute pain, inability to bear weight, deformity | ORIF (plates, screws), revision TKA with longer stem or more constrained components. Depends on fracture type, location, and implant stability. |
| Arthrofibrosis / Stiffness | 2-10% | Limited ROM (<90° flexion, >10° flexion contracture) | Aggressive PT, MUA (6-12 weeks post-op), arthroscopic or open lysis of adhesions. |
| Aseptic Loosening | 1-5% (10 years) | Gradual onset of mechanical pain, lucency on X-ray | Revision TKA (component exchange, bone grafting if osteolysis present). |
| Polyethylene Wear/Osteolysis | Variable (declining) | Pain, swelling, radiographic lucency/bone loss | Revision TKA (polyethylene exchange, component revision, bone grafting). |
| Instability | 1-3% | Sensation of "giving way," recurrent effusions | Revision TKA with soft tissue balancing, increased constraint, or larger components to address specific instability pattern. |
| Neurovascular Injury | Peroneal 0.3-2%, Popliteal <0.1% | Peroneal (foot drop, numbness); Popliteal (cold, pulseless limb) | Peroneal (observation, orthosis, nerve exploration if indicated); Popliteal (emergent vascular repair). |
| Patellar Complications | Fracture 0.5-3%, Maltracking <1% | Patellar pain, crepitus, clunking, fracture pain | Fracture (non-op, ORIF, patellectomy), Maltracking (lateral retinacular release, revision components), Clunk (arthroscopic debridement). |
Post-Operative Rehabilitation Protocols
A structured and progressive post-operative rehabilitation protocol is integral to achieving optimal functional outcomes following TKA. The overarching goals are pain management, restoration of range of motion, strengthening of the musculature surrounding the knee, normalization of gait, and facilitating a safe return to desired activities. Protocols are typically divided into phases, with specific milestones and interventions for each.
Phase I: Acute Hospital Phase (Days 0-7)
Goals:
* Pain control and edema management.
* Initiation of early active and passive range of motion (ROM) (target 0-90° flexion).
* Independent transfers and ambulation with an assistive device (walker or crutches).
* Patient education on precautions and exercises.
Interventions:
*
Pain Management:
Multimodal analgesia (regional blocks, oral NSAIDs, acetaminophen, short-acting opioids, nerve blocks, local infiltration analgesia).
*
Edema Control:
Cryotherapy (ice packs, continuous cold flow devices), compression wraps, elevation.
*
Early Mobilization:
*
Day 0-1:
Out of bed to chair, initiation of continuous passive motion (CPM) machine (use is debated, no clear superior benefit over conventional PT), gentle active-assisted ROM exercises.
*
Therapeutic Exercises:
Quadriceps sets (isometric contractions), ankle pumps (DVT prophylaxis), gluteal sets, heel slides (active-assisted flexion), knee extension (passive or active-assisted).
*
Gait Training:
Weight-bearing as tolerated (WBAT) with a walker or crutches, progressing to partial weight-bearing (PWB) as pain allows. Focus on proper gait mechanics.
*
Wound Care:
Daily wound checks, dressing changes as per protocol.
*
Patient Education:
Instruction on exercises, activity precautions (avoid twisting, kneeling), DVT symptoms, pain medication use.
Phase II: Early Outpatient / Home Phase (Weeks 1-6)
Goals:
* Improve ROM (target 0-110°+ flexion, full extension).
* Progressive increase in weight-bearing and normalize gait pattern.
* Strengthen quadriceps, hamstrings, and hip abductors.
* Reduce reliance on assistive devices.
Interventions:
*
Continued ROM Exercises:
Aggressive heel slides, wall slides, stationary bike (low resistance, high seat), prone hangs (for extension).
*
Progressive Resistive Exercises:
*
Quadriceps:
Straight leg raises (SLR), terminal knee extension (TKE), leg press (low weight), squats to 45° (wall squats).
*
Hamstrings:
Hamstring curls (prone or standing), glute bridge.
*
Calf:
Calf raises.
*
Hip Abductors:
Side-lying leg raises.
*
Balance and Proprioception:
Standing balance exercises, single-leg stance (with support).
*
Gait Training:
Gradual weaning from walker to crutches, then to cane, with emphasis on symmetrical gait, stair climbing (step-up, step-down technique).
*
Modalities:
Continued cryotherapy, therapeutic ultrasound (controversial), electrical stimulation for quadriceps activation.
Phase III: Intermediate Outpatient Phase (Weeks 6-12)
Goals:
* Achieve full functional ROM.
* Advanced strengthening and endurance.
* Enhance proprioception and dynamic stability.
* Return to light recreational activities.
Interventions:
*
Advanced Strengthening:
Progressive resistance with leg press, lunges, step-ups/downs, squats (deeper range), balance board exercises, closed-chain activities.
*
Cardiovascular Conditioning:
Stationary cycling (increased resistance), elliptical trainer, swimming, fast walking.
*
Sport-Specific Drills (if applicable):
Low-impact activities, gentle golf swings (no twisting).
*
Proprioceptive Training:
Unstable surfaces, agility drills (controlled).
*
Stair Negotiation:
Focus on normal reciprocal stair climbing.
Phase IV: Advanced / Maintenance Phase (Months 3+)
Goals:
* Return to desired, appropriate activities (within physician guidelines).
* Long-term maintenance of strength, flexibility, and endurance.
Interventions:
*
Home Exercise Program:
Lifelong adherence to maintain strength and flexibility.
*
Activity Modification:
Avoid high-impact activities (running, jumping, contact sports) that can accelerate implant wear or loosening. Encourage low-impact activities (walking, swimming, cycling, golf, hiking on even terrain, doubles tennis).
*
Weight Management:
Crucial for implant longevity and overall joint health.
*
Follow-up:
Regular clinical and radiographic follow-up with the orthopedic surgeon.
Specific Considerations Across Phases:
*
Pain Management:
Transition from prescription opioids to over-the-counter analgesics as pain subsides.
*
DVT Prophylaxis:
Continue as per surgeon's protocol, often for 2-6 weeks post-op.
*
Wound Care:
Monitor for signs of infection.
*
Patient Education:
Reinforce activity restrictions, proper body mechanics, and the importance of lifelong exercise.
Summary of Key Literature / Guidelines
The landscape of TKA management is continuously refined by robust evidence from clinical trials, systematic reviews, and large-scale registry analyses. Major orthopedic societies provide evidence-based guidelines to standardize and optimize care.
Major Societies and Guidelines
- American Academy of Orthopaedic Surgeons (AAOS): Publishes clinical practice guidelines (CPGs) and appropriate use criteria (AUC) covering various aspects of TKA, including indications, VTE prophylaxis, pain management, and infection prevention.
- American Association of Hip and Knee Surgeons (AAHKS): Focuses on arthroplasty research and education, often collaborating on guidelines.
- National Institute for Health and Care Excellence (NICE) (UK): Provides comprehensive guidelines for the management of osteoarthritis, including criteria for TKA.
Key Themes in Current Literature and Guidelines
-
Patient Selection and Pre-operative Optimization:
- Emphasis on comprehensive pre-operative medical assessment to identify and optimize comorbidities (e.g., diabetes control, smoking cessation, nutritional optimization).
- Strong recommendation for non-operative management failure as a prerequisite, with documentation of trials.
- Addressing psychological factors (depression, anxiety, chronic opioid use) is increasingly recognized as crucial for patient satisfaction and outcomes.
-
Surgical Technique:
- Mechanical vs. Kinematic Alignment: Ongoing debate. Mechanical alignment (neutral overall limb alignment) remains the traditional standard. Kinematic alignment (restoring individual patient's pre-arthritic alignment) is gaining traction, with studies showing comparable or improved functional outcomes and potentially more "natural-feeling" knees for some patients.
- Patient-Specific Instrumentation (PSI) / Navigation / Robotics: These technologies aim to improve the accuracy and reproducibility of bone resections and component positioning. While they demonstrate superior accuracy in component placement in cadaveric and clinical studies, clear evidence of superior long-term clinical outcomes (e.g., lower revision rates, better PROMs) compared to conventional instrumentation remains somewhat limited and is an active area of research.
- PCL-Retaining vs. PCL-Substituting Designs: Both designs yield excellent long-term results. PCL-substituting designs may offer greater stability in patients with PCL insufficiency or complex deformities, while PCL-retaining designs aim to preserve native knee kinematics.
-
Perioperative Pain Management:
- Multimodal Analgesia: Strong recommendation for multimodal approaches combining regional nerve blocks (femoral, adductor canal, sciatic), local infiltration analgesia (LIA), NSAIDs, acetaminophen, and minimized opioid use. This strategy improves pain control, reduces opioid consumption, and facilitates early mobilization.
- Opioid Stewardship: Focus on reducing chronic opioid use pre- and post-operatively to mitigate risks of dependence and addiction.
-
Venous Thromboembolism (VTE) Prophylaxis:
- Guidelines emphasize individualized risk assessment for DVT and PE.
- Recommendations typically include pharmacological prophylaxis (e.g., aspirin, rivaroxaban, apixaban, low molecular weight heparin, warfarin) for at least 2-6 weeks post-operatively, often combined with mechanical prophylaxis (intermittent pneumatic compression devices).
-
Infection Prevention:
- Strict adherence to evidence-based protocols: pre-operative skin decontamination (chlorhexidine showers), pre-operative glycemic control (HbA1c < 8%), appropriate prophylactic antibiotics (cefazolin or vancomycin for penicillin allergy) administered within 60 minutes of incision, maintaining normothermia, and meticulous surgical technique.
- Screening for Staphylococcus aureus colonization and decolonization strategies are increasingly implemented.
-
Outcomes Assessment:
- Increasing use of Patient-Reported Outcome Measures (PROMs) (e.g., KOOS, Oxford Knee Score, SF-36) to objectively assess functional improvement and patient satisfaction, moving beyond purely surgeon-centric measures.
- Registry data from national and international databases (AJRR, NJR, ANZAC) provides invaluable real-world evidence on implant survival, revision rates, and identification of risk factors.
-
Emerging Trends:
- Outpatient TKA: Select patients are now safely undergoing TKA in an outpatient setting, driven by advancements in pain management, surgical technique, and rehabilitation protocols. Strict patient selection criteria are essential.
- Enhanced Recovery After Surgery (ERAS) Protocols: Comprehensive, multidisciplinary pathways designed to standardize care, optimize patient recovery, and reduce hospital stays.
- Advanced Materials: Research into new bearing surfaces, highly cross-linked polyethylene, and alternative materials to further improve wear characteristics and implant longevity.
In conclusion, TKA remains a highly effective intervention for end-stage knee arthritis, with continuous advancements in all facets of care. Adherence to established guidelines, coupled with an understanding of emerging evidence, is crucial for optimizing patient selection, surgical execution, complication avoidance, and rehabilitation to ensure durable, high-quality outcomes.
You Might Also Like
