Operative Management of Carpal Fractures and Dislocations: A Focus on the Scaphoid and Kienböck Disease
Key Takeaway
Carpal bone fractures, particularly of the scaphoid, present significant diagnostic and therapeutic challenges due to complex wrist kinematics and tenuous retrograde vascularity. Missed diagnoses frequently lead to nonunion and advanced collapse. This comprehensive guide details the biomechanics, advanced imaging protocols, and precise surgical management of scaphoid fractures, providing orthopedic surgeons with evidence-based strategies to optimize union rates and restore carpal stability.
FRACTURES AND DISLOCATIONS OF THE CARPAL BONES
The diagnosis and management of fractures and dislocations of the carpal bones represent a formidable challenge in orthopedic trauma. The intricate architecture of the carpus, comprising eight distinct bones functioning as a highly synchronized intercalated segment, relies heavily on complex ligamentous constraints rather than inherent bony stability.
Radiographic evaluation is notoriously difficult. The outlines of the eight carpal bones are superimposed in standard radiographic views; even in a true anteroposterior (AP) or posteroanterior (PA) projection, at least one bone overlies another. Accurate interpretation demands a profound understanding of normal osseous contours, Gilula’s carpal arcs, and the dynamic kinematic relationships that occur during the various arcs of wrist motion (e.g., the dart-thrower's motion).
Because of the inherent difficulty in recognizing subtle fractures in acute injuries, significant carpal trauma may be easily overlooked during the initial clinical examination. Articular cartilage damage and intrinsic ligamentous disruptions (such as scapholunate or lunotriquetral tears) are even more elusive. These ligamentous injuries permit abnormal rotations and subluxations, leading to predictable patterns of carpal collapse, namely Dorsal Intercalated Segment Instability (DISI) and Volar Intercalated Segment Instability (VISI).
Advanced Diagnostic Imaging in Carpal Trauma
When standard PA, lateral, and oblique radiographs fail to yield a definitive diagnosis, special radiographic techniques and advanced imaging modalities become mandatory.
- Scaphoid Views: A PA view with the wrist in maximum ulnar deviation and 30 degrees of extension elongates the scaphoid, bringing its longitudinal axis parallel to the cassette and profiling the waist.
- Computed Tomography (CT): Scaphoid fracture displacement, comminution, and angular deformity (humpback deformity) are more readily detected with high-resolution, three-dimensional CT reconstructions than with plain radiography or traditional tomography. Scans should be formatted along the true longitudinal axis of the scaphoid (parasagittal and paracoronal planes).
- Magnetic Resonance Imaging (MRI): Establishing a precise diagnosis regarding osseous viability remains difficult. Compared with plain radiographs, CT, and even the surgeon’s intraoperative assessment of punctate bleeding, MRI is the most accurate modality for predicting the vascularity of the proximal pole in scaphoid nonunions. Gadolinium-enhanced MRI is the gold standard for assessing avascular necrosis (AVN).
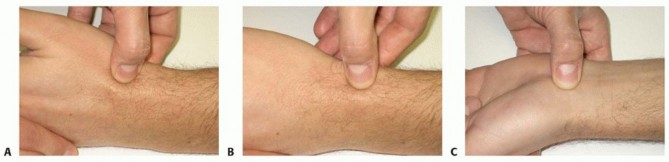
Clinical Pearl: A "sprained wrist" following a high-energy fall in a young adult is a scaphoid fracture or perilunate injury until proven otherwise. If initial radiographs are negative but clinical suspicion remains high (snuffbox tenderness, scaphoid tubercle tenderness), the wrist must be immobilized in a thumb spica cast or splint, with repeat clinical and radiographic evaluation at 10 to 14 days. Alternatively, an acute MRI can be obtained to definitively rule out a fracture, facilitating early return to work or sport.
FRACTURES OF THE SCAPHOID
Fracture of the carpal scaphoid is the most common fracture of the carpus, accounting for approximately 60% to 70% of all carpal bone injuries. Unfortunately, the diagnosis is frequently delayed due to the subtle clinical presentation and the limitations of initial plain radiography. A delay in the diagnosis and treatment of a scaphoid fracture drastically alters the prognosis for union, increasing the risk of nonunion, avascular necrosis, and subsequent Scaphoid Nonunion Advanced Collapse (SNAC).
Etiology and Biomechanics
Scaphoid fractures are reported in individuals ranging from 10 to 70 years of age, though they overwhelmingly occur in young, active males (peak incidence in the second and third decades of life).
The classic mechanism of injury is a fall on the outstretched hand (FOOSH). Biomechanically, this results in severe hyperextension (typically greater than 95 degrees) and slight radial deviation of the wrist. During this terminal extension, the scaphoid fractures in tension. The load is concentrated on the radial-palmar aspect of the bone. The proximal pole becomes locked securely within the scaphoid fossa of the distal radius, while the distal pole is forced into excessive dorsal translation by the surrounding capsuloligamentous structures.
- Anatomic Distribution:
- Waist (Midportion): 60% to 80% of scaphoid fractures occur here.
- Proximal Pole: 15% to 20%.
- Distal Pole/Tubercle: 5% to 10%.
- Associated Injuries: Approximately 17% of patients with scaphoid fractures present with concomitant fractures of the carpus and forearm. These include transscaphoid perilunate fracture-dislocations, fractures of the trapezium, Bennett fractures of the thumb metacarpal base, and fractures of the radial head.
Vascular Anatomy and Prognostic Implications
The prognosis of a scaphoid fracture is inextricably linked to its unique, retrograde blood supply. The scaphoid is primarily perfused by branches of the radial artery.
- Dorsal Carpal Branch: Supplies 70% to 80% of the scaphoid, entering through the dorsal ridge and perfusing the proximal pole in a retrograde fashion.
- Volar Carpal Branch: Supplies the remaining 20% to 30%, entering at the distal tubercle and perfusing the distal pole.
Because the proximal pole relies entirely on intraosseous retrograde flow from the waist, fractures at the waist or proximal pole frequently disrupt this tenuous blood supply. Consequently, proximal pole fractures have a high rate of delayed union, nonunion, and avascular necrosis.
Surgical Warning: When approaching the scaphoid surgically, meticulous care must be taken to preserve the dorsal ridge vascular foramina. Overzealous dorsal stripping can iatrogenically devascularize the proximal pole, converting a viable fracture into an avascular nonunion.
SURGICAL MANAGEMENT OF SCAPHOID FRACTURES
While undisplaced distal pole and stable waist fractures may be managed non-operatively with cast immobilization, the modern trend in orthopedic surgery leans toward early operative intervention for specific indications to ensure anatomic restoration, minimize immobilization time, and optimize union rates.
Indications for Operative Intervention
- Displacement: Any step-off or gap greater than 1 mm.
- Angular Deformity: An intrascaphoid angle greater than 35 degrees (indicative of a humpback deformity) or a radiolunate angle >15 degrees (DISI deformity).
- Location: All proximal pole fractures, due to the high risk of AVN and nonunion with conservative care.
- Associated Injuries: Transscaphoid perilunate dislocations or concomitant distal radius fractures.
- Patient Factors: High-level athletes or manual laborers requiring early return to function.
The Volar Approach (Russe) for Waist Fractures
The volar approach is the workhorse for fractures of the scaphoid waist and distal pole. It allows excellent visualization of the fracture, facilitates correction of the humpback flexion deformity, and avoids the critical dorsal blood supply.
Positioning and Preparation:
The patient is positioned supine with the arm extended on a radiolucent hand table. A proximal arm tourniquet is applied. Fluoroscopy must be positioned to allow seamless AP, lateral, and scaphoid views.
Surgical Steps:
1. Incision: A longitudinal or slightly curvilinear incision is made over the flexor carpi radialis (FCR) tendon, extending from the scaphoid tubercle proximally for 4 to 5 cm.
2. Superficial Dissection: The FCR tendon sheath is incised. The tendon is retracted ulnarly to protect the median nerve. The radial artery is identified and carefully retracted radially.
3. Deep Dissection: The floor of the FCR sheath is incised, exposing the volar wrist capsule. A longitudinal capsulotomy is performed, exposing the radiocarpal joint and the volar aspect of the scaphoid.
4. Fracture Preparation: The fracture site is identified. Hematoma and interposed tissue are debrided. If a humpback deformity is present, the wrist is extended, and a small elevator is used to hinge the fracture open volarly, restoring the anatomic intrascaphoid angle.
5. Guidewire Placement: A K-wire is introduced from the distal tubercle, directed proximally and dorsally toward the proximal pole. Crucial Step: The guidewire must be placed down the central axis of the scaphoid to ensure maximum screw thread purchase and biomechanical stability.
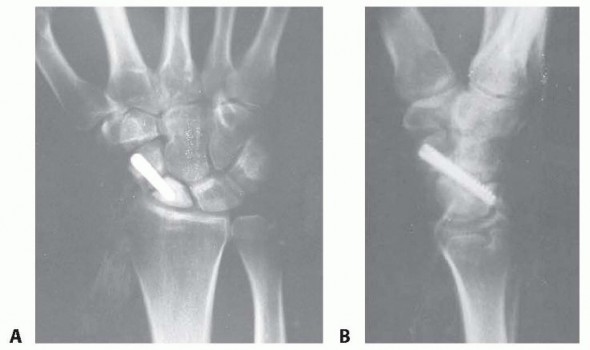
6. Fixation: A headless compression screw (e.g., Acutrak, Herbert screw) is measured, drilled, and inserted over the guidewire. The screw must be countersunk beneath the articular cartilage of the distal pole.
7. Closure: The capsule is meticulously repaired to prevent volar carpal subluxation, followed by routine skin closure.
The Dorsal Approach for Proximal Pole Fractures
Fractures of the proximal pole are best approached dorsally. The proximal pole is a small, intra-articular fragment that is difficult to capture from a volar trajectory without violating the radiocarpal articulation or achieving suboptimal thread purchase.
Surgical Steps:
1. Incision: A 3 to 4 cm longitudinal incision is made centered over Lister’s tubercle.
2. Dissection: The extensor retinaculum is incised over the third dorsal compartment. The extensor pollicis longus (EPL) tendon is mobilized and retracted radially.
3. Capsulotomy: A ligament-sparing dorsal capsulotomy (e.g., Berger's flap) is performed to expose the proximal scaphoid and the scapholunate interval.
4. Fixation: The fracture is reduced directly. A guidewire is inserted from the proximal pole, aiming distally and volarly down the central axis of the scaphoid. A headless compression screw is inserted, ensuring the proximal trailing edge is buried beneath the articular surface of the proximal pole to prevent radiocarpal impingement.
Pitfall: Failure to achieve central axis screw placement is the most common technical error in scaphoid fixation. Eccentric screw placement provides inferior biomechanical compression and increases the risk of iatrogenic fracture comminution or cortical breach.
Percutaneous Fixation Techniques
For acute, strictly undisplaced fractures of the scaphoid waist, percutaneous fixation offers the advantage of minimal soft tissue disruption, preservation of fracture hematoma, and rapid rehabilitation.
Using a volar percutaneous approach, the wrist is extended over a towel roll. Under multi-planar fluoroscopic guidance, a guidewire is inserted through a 2 mm stab incision at the scaphoid tubercle. The trajectory is confirmed on AP, lateral, and pronated oblique views before drilling and inserting a headless compression screw. This technique demands significant fluoroscopic proficiency and a thorough understanding of 3D carpal anatomy.
POSTOPERATIVE PROTOCOLS AND REHABILITATION
Postoperative management is dictated by the security of the fixation and the presence of concomitant injuries.
- Stable Internal Fixation: If rigid compression is achieved (e.g., via percutaneous or open headless screw fixation for an acute waist fracture), the patient is placed in a removable volar splint. Gentle, active range of motion (ROM) of the wrist and thumb is initiated at 1 to 2 weeks postoperatively. Heavy lifting and contact sports are restricted until radiographic union is confirmed (typically 8 to 12 weeks).
- Complex Reconstructions: For proximal pole fractures, nonunions requiring bone grafting, or cases with tenuous fixation, a short-arm thumb spica cast is applied for 4 to 6 weeks, followed by a transition to a removable splint and progressive therapy.
- Radiographic Monitoring: Serial radiographs are obtained at 2, 6, and 12 weeks. If plain films are equivocal at 12 weeks, a fine-cut CT scan is the modality of choice to confirm osseous bridging.
COMPLICATIONS AND SALVAGE PROCEDURES
Scaphoid Nonunion and SNAC Wrist
Failure to achieve union results in altered carpal kinematics. The distal scaphoid fragment flexes, and the lunate extends (DISI deformity). Over time, this abnormal articulation leads to predictable, progressive osteoarthritis known as Scaphoid Nonunion Advanced Collapse (SNAC).
- Stage I: Arthrosis localized to the radial styloid and distal scaphoid.
- Stage II: Arthrosis extending to the entire radioscaphoid joint.
- Stage III: Arthrosis involving the capitolunate joint. (The radiolunate joint is characteristically spared).
Salvage Options:
* Early Nonunion (No Arthrosis): Volar wedge grafting (Matti-Russe) or vascularized bone grafting (e.g., 1,2-Intercompartmental Supraretinacular Artery [1,2-ICSRA] graft) combined with rigid internal fixation.
* SNAC Stage I: Radial styloidectomy with scaphoid nonunion repair.
* SNAC Stage II/III: Proximal Row Carpectomy (PRC) or Scaphoid Excision and Four-Corner Fusion (capitate, lunate, triquetrum, hamate).
A NOTE ON KIENBÖCK DISEASE
While scaphoid fractures dominate carpal trauma, Kienböck disease—avascular necrosis of the lunate—represents a critical, insidious pathology of the carpus.
Etiology: The exact cause is multifactorial, involving repetitive microtrauma, tenuous intraosseous vascularity (a single volar or dorsal vessel in 20% of the population), and biomechanical factors. It is strongly associated with ulnar minus variance (a shortened ulna relative to the radius), which increases radiolunate contact stresses.
Clinical Presentation: Patients typically present with insidious dorsal wrist pain, decreased grip strength, and limited wrist extension.
Staging and Management (Lichtman Classification):
* Stage I (Normal X-ray, MRI shows AVN): Immobilization, NSAIDs.
* Stage II (Lunate sclerosis, no collapse): Joint leveling procedures (e.g., radial shortening osteotomy) to unload the lunate in ulnar minus patients.
* Stage IIIa (Lunate collapse, normal carpal alignment): Radial shortening or vascularized bone grafting.
* Stage IIIb (Lunate collapse, fixed DISI deformity): Scaphocapitate fusion or limited intercarpal arthrodesis.
* Stage IV (Pancarpal arthrosis): Proximal row carpectomy or total wrist arthrodesis.
Mastery of carpal anatomy, rigorous adherence to advanced imaging protocols, and precise surgical execution are paramount. Whether addressing an acute scaphoid fracture or managing the complex sequelae of Kienböck disease, the orthopedic surgeon must balance biomechanical restoration with the preservation of the delicate carpal blood supply to achieve optimal patient outcomes.
📚 Medical References
You Might Also Like