Surgical Management of Knee Dislocations and Extensor Mechanism Repair
Key Takeaway
The surgical management of multiligament knee injuries and extensor mechanism disruptions requires meticulous preoperative planning and timely intervention. Early operative repair, particularly within the first three weeks, yields superior outcomes compared to nonoperative management. This guide details the biomechanics, surgical indications, and step-by-step operative techniques for addressing complex knee dislocations, including proximal tibiofibular joint instability, irreducible dislocations, and the critical management of posterolateral corner injuries to restore joint kinematics and stability.
OPEN REDUCTION AND REPAIR OF THE EXTENSOR MECHANISM AND MULTILIGAMENT KNEE INJURIES
The management of complete knee dislocations and catastrophic disruptions of the extensor mechanism represents one of the most formidable challenges in orthopedic trauma. Historically, nonoperative management was frequently employed; however, contemporary evidence unequivocally demonstrates that nonoperative treatment yields only fair or poor functional results, typically culminating in severe joint stiffness and chronic instability. Consequently, the modern orthopedic consensus strongly advocates for the early surgical repair and reconstruction of all injured ligamentous and capsular structures to restore native joint kinematics and achieve satisfactory long-term outcomes.
When open treatment is selected, the orthopedic surgeon must possess a comprehensive, 360-degree understanding of knee anatomy and be fully prepared to repair structures medially, laterally, anteriorly, and posteriorly as intraoperative findings dictate.
Clinical Pearl: Preoperative planning is paramount. High-resolution Magnetic Resonance Imaging (MRI) is an invaluable diagnostic tool, allowing the surgeon to map the exact pathoanatomy of the injury, differentiate between avulsions and mid-substance tears, and anticipate the need for allograft or autograft tissues.
Tissue Pathology: Avulsions vs. Mid-Substance Tears
A critical distinction in the surgical decision-making process is identifying the nature of the ligamentous failure. Many high-energy knee dislocations result in bony or soft-tissue avulsions rather than mid-substance ruptures of the collateral or cruciate ligaments.
- Cruciate Ligament Avulsions: Identifying an avulsion is particularly advantageous in cruciate ligament injuries. Primary end-to-end repair of mid-substance cruciate tears is biomechanically inferior and prone to failure, necessitating formal reconstruction. Conversely, the anatomical reduction and secure rigid fixation of an avulsed bony footprint can lead to excellent clinical results without the morbidity of graft harvesting.
- Posterolateral Corner (PLC) Injuries: Injuries to the posterolateral corner are particularly worrisome due to their profound impact on rotational stability and their propensity to stretch and scar rapidly. PLC injuries must be treated aggressively and early—ideally within the first 2 to 3 weeks post-injury. Delayed treatment inevitably leads to tissue retraction and severe scarring, rendering primary repair impossible and forcing the surgeon to perform highly complex, less rewarding reconstructive procedures.
Surgical Timing and Preoperative Optimization
Following the initial trauma, the immediate priorities are the stabilization of the patient and a diligent, exhaustive neurovascular evaluation. The popliteal artery is highly vulnerable to intimal tearing or complete transection due to its anatomical tethering between the adductor hiatus and the soleal arch.
Once life- and limb-threatening injuries are addressed, the timing of ligamentous surgery depends heavily on the specific structures involved:
1. With PLC Involvement: Surgery should be performed within the first 3 weeks to allow for direct anatomical repair of the posterolateral structures.
2. Without PLC Involvement: Knees lacking posterolateral corner disruption can be managed with a slightly delayed approach. Surgery is optimally performed once the acute inflammatory phase has subsided and a functional range of motion (ROM) of 0 to 90 degrees has been restored, thereby minimizing the risk of postoperative arthrofibrosis.
PROXIMAL TIBIOFIBULAR JOINT DISLOCATIONS
Acute dislocations of the proximal tibiofibular joint (PTFJ) are exceedingly rare but are critical components of the lateral knee complex. They typically result from a violent twisting trauma and are frequently seen in association with other severe injuries to the ipsilateral lower extremity, such as tibial shaft fractures or multiligament knee injuries.
Clinical Presentation and Biomechanics
Patients with acute PTFJ dislocations usually present with localized lateral joint line pain, an obvious bony prominence over the lateral aspect of the knee, and an inability to bear weight. Unfortunately, due to the distracting nature of concomitant injuries, PTFJ dislocations are frequently overlooked in the emergency setting.
Patients suffering from chronic dislocations or recurrent subluxation typically complain of mechanical symptoms, including popping, catching, and subjective instability.
Diagnostic Pitfall: The clinical presentation of chronic PTFJ subluxation closely mimics the symptoms of a lateral meniscus tear. A high index of suspicion and careful palpation of the fibular head during dynamic ranging of the knee are required to differentiate the two.
The biomechanical susceptibility of the PTFJ is dictated by its anatomical orientation, which varies among individuals:
* Horizontal Joints: Characterized by an articular surface angle of less than 20 degrees relative to the horizontal plane. These joints permit a greater degree of physiological motion and are generally more forgiving of torsional forces.
* Oblique Joints: Characterized by a steeper articular inclination. The relative restriction of motion in oblique joints severely limits their ability to dissipate rotational stress, which is presumably the primary reason why the vast majority of traumatic dislocations occur in this anatomical variant.
The Ogden Classification
Ogden classified proximal tibiofibular subluxations and dislocations into four distinct types, which guide therapeutic decision-making:
- Type I (Subluxation): Characterized by hypermobility without frank dislocation. It is a recurring problem associated with generalized joint hypermobility and chronic lateral knee pain.
- Type II (Anterolateral Dislocation): The most common type of PTFJ dislocation. The fibular head is displaced anteriorly and laterally.
- Type III (Posteromedial Dislocation): A rare and highly unstable injury. The fibular head is driven posteriorly and medially.
- Type IV (Superior Dislocation): Exceptionally rare, typically associated with high-energy trauma, fractures of the fibular shaft, or proximal dislocation of the lateral malleolus (e.g., Maisonneuve-type variants).
Surgical Warning: Keogh et al. demonstrated through extensive cadaveric studies that standard orthogonal radiographs are often insufficient for diagnosing subtle PTFJ injuries. Suspected dislocations or subluxations of the proximal tibiofibular joint are best evaluated and definitively diagnosed using an axial Computed Tomography (CT) scan.
Management Strategies for PTFJ Injuries
Type I (Subluxation):
Conservative management is the first line of treatment. If symptoms fail to respond to a period of cylinder cast immobilization and subsequent physical therapy, surgical intervention is warranted. Resection of the fibular head is the recommended procedure.
Contraindication: Arthrodesis (fusion) of the proximal tibiofibular joint is strongly discouraged. The fibula must migrate proximally and distally during normal ankle dorsiflexion and plantarflexion. Fusing the proximal joint disrupts this biomechanical relationship, inevitably leading to late, painful complications referable to the ankle joint.
Type II (Anterolateral Dislocations):
These are the most common and are usually treated successfully by closed reduction methods. The knee is flexed to 90 degrees to relax the biceps femoris tendon and the lateral collateral ligament (LCL), and direct manual pressure is applied to the fibular head in a posteromedial direction.
Type III (Posteromedial Dislocations):
These injuries are notoriously difficult to reduce closed and are almost universally associated with severe disruptions of the tibiofibular capsular ligaments and the LCL. When the dislocation is acute, open reduction is strongly recommended.
SURGICAL TECHNIQUE: OPEN REDUCTION AND TRANSARTICULAR PINNING
In cases of unstable posteromedial dislocations, or when the joint tends to redislocate in a splint or following vascular repair, temporary internal fixation is required.
Indications for Transarticular Pinning
Transarticular pins are highly effective but must be used with caution, as they carry inherent risks of pin tract infection and mechanical breakage. We have found transarticular pinning to be particularly useful when the posterior capsule is completely disrupted, a condition that prevents concentric reduction of the joint in full extension.
Operative Steps
- Positioning and Approach: The patient is positioned supine. A lateral approach is utilized, carefully identifying and protecting the common peroneal nerve, which courses directly posterior and inferior to the fibular head.
- Reduction: The entrapped soft tissues are cleared from the joint space. The fibular head is anatomically reduced into the tibial facet.
- Fixation: While holding the reduction, heavy Kirschner wires (K-wires) or Steinmann pins are driven from the lateral aspect of the fibular head, across the proximal tibiofibular articulation, and securely into the proximal tibial metaphysis.
- Ligamentous Repair: Once skeletal stability is achieved, the torn LCL and posterolateral capsular structures are primarily repaired using suture anchors.
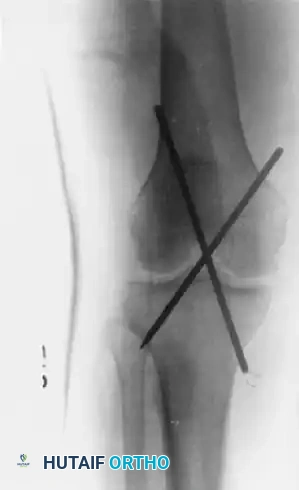
The following radiographs demonstrate the successful application of transarticular pins for temporary extraarticular fixation during the repair of torn lateral ligaments.

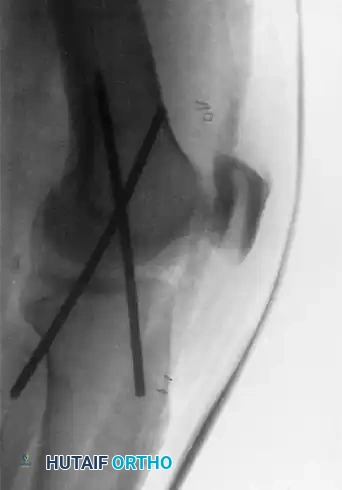
Figure 60-5: Radiographs demonstrating transarticular pins. (A) Anteroposterior view and (B) Lateral view illustrating the temporary extraarticular fixation with Kirschner wires utilized during the repair of torn ligaments.
Postoperative Protocol for Pinning
The transarticular pins are left in place for 4 to 6 weeks. During this period, protected range of motion is carefully initiated to prevent knee stiffness, though extreme flexion is avoided to prevent pin bending or breakage.
MANAGEMENT OF COMPLETE KNEE DISLOCATIONS
In complete knee dislocations (typically classified as Schenck KD-III or KD-IV), both the anterior and posterior cruciate ligaments are usually torn, accompanied by the complete disruption of either the lateral or medial collateral ligament complexes.
Damage Control Orthopedics
The decision to proceed with definitive surgical repair of the ligaments is heavily influenced by the patient's overall physiological status, the presence of other skeletal injuries, vascular deficits, or open wounds.
* External Fixation: A rigid, knee-spanning external fixator is the treatment of choice in open knee dislocations with extensive soft tissue stripping, or in grossly unstable knees following popliteal artery repair.
* Once it is absolutely certain that the distal circulation is not impaired and the soft tissue envelope has stabilized, the surgeon can proceed with the definitive repair or reconstruction of the injured ligaments.
Irreducible Knee Dislocations
While closed reduction is the immediate goal in the emergency department, it may be impossible, especially in posterolateral knee dislocations.
Pathoanatomy of Irreducibility: A classic block to reduction occurs via the "buttonholing" of the medial femoral condyle through a traumatic tear in the medial joint capsule. Furthermore, an invaginated tibial collateral ligament or a displaced pes anserinus tendon can interpose into the joint space, physically blocking the reduction of the tibia beneath the femur. Clinically, this often presents with a deep transverse furrow or "dimple sign" over the medial joint line.
When an irreducible dislocation is encountered, repeated forceful attempts at closed reduction are contraindicated as they risk further neurovascular catastrophic injury. Open reduction through a formal medial approach is necessary. The entrapping structures (capsule, MCL, or pes anserinus) are meticulously released, extracted from the joint, and anatomically repaired. Postoperative care then follows standard multiligament reconstruction protocols.
Nonoperative Management: Indications and Outcomes
While early surgical repair yields the most satisfactory long-term functional results, surgery is not universally applicable. If operative repair is impossible—such as in polytrauma patients requiring prolonged damage control, injuries associated with massive open wounds, or in elderly, low-demand patients with severe medical comorbidities—satisfactory, albeit limited, results can be obtained by nonsurgical management.
Nonsurgical Protocol:
1. The knee is reduced and a long-leg splint or cast is applied in 10 to 15 degrees of flexion.
2. Immobilization is maintained for approximately 2 weeks to allow for initial soft tissue sealing.
3. A hinged knee brace is then applied, and a heavily supervised, progressive range of motion protocol is initiated.
Clinical Outcome: Patients managed nonoperatively for complete knee dislocations typically develop profound joint stiffness and arthrofibrosis rather than gross instability as their primary long-term complication.
SUPERIOR DISLOCATIONS OF THE PTFJ (TYPE IV)
Superior dislocations of the proximal tibiofibular joint are exceedingly rare and are almost universally associated with high-energy axial loading combined with rotational forces. They frequently present concomitantly with a fracture of the fibular shaft or a proximal dislocation of the lateral malleolus, indicating a complete longitudinal disruption of the interosseous membrane.
Surgical Management and Postoperative Care
If closed reduction fails or the joint remains grossly unstable, open reduction and internal fixation are necessary. Following the surgical stabilization of a superior dislocation:
1. Immobilization: The leg is immobilized in a long-leg cast. This is critical to prevent ankle motion, as dorsiflexion forces the fibula proximally, which can cause catastrophic loosening or failure of the proximal pin fixation.
2. Positioning: The knee is immobilized in slight flexion (approximately 15 to 20 degrees). This specific positioning relaxes the pull of the biceps femoris tendon on the fibular head, reducing the deforming forces on the repair.
3. Weight-Bearing: The patient is restricted to strict non-weight-bearing status with crutches.
4. Cast Progression: The long-leg cast is removed at 3 weeks postoperatively, and the patient is transitioned to a short-leg walking cast or a controlled ankle motion (CAM) boot.
5. Hardware Removal: The transarticular pins are routinely removed at 6 weeks after surgery in the clinic setting, after which progressive, active range of motion and strengthening exercises are formally instituted.
You Might Also Like