Mastering Knee Dislocations and Intraarticular Patellar Reductions: A Comprehensive Surgical Guide
Key Takeaway
Knee dislocations are true orthopaedic emergencies characterized by extensive ligamentous disruption and a high risk of popliteal artery injury. Prompt reduction and vascular assessment are mandatory. Intraarticular patellar dislocations, though rare, typically require open reduction and extensor mechanism repair. This guide details the biomechanics, clinical evaluation, and step-by-step surgical management for these complex knee injuries, emphasizing limb salvage and joint stability.
COMPREHENSIVE MANAGEMENT OF KNEE DISLOCATIONS
Dislocation of the knee (tibiofemoral dislocation) has historically been considered a rare injury; however, contemporary trauma registries indicate that its frequency has increased over the years. It is widely acknowledged in orthopaedic traumatology that the true incidence is likely higher than recognized. Many knee dislocations spontaneously reduce or are reduced at the scene of the injury by emergency medical personnel without subsequent accurate reporting of the initial dislocated state.
Knee dislocations are true orthopaedic emergencies. They represent the culmination of massive kinetic energy transfer resulting in multiligamentous knee injury (MLKI), typically involving both cruciate ligaments and at least one collateral ligament complex. Reported series consistently emphasize the extensive soft-tissue damage and the devastating potential for limb-threatening vascular complications associated with these injuries.
Classification and Pathoanatomy
Knee dislocations are designated according to the displacement of the tibia in relation to the femur (the Kennedy Classification). The primary directional categories include:
* Anterior Dislocations: The most common type, typically resulting from forced hyperextension. The posterior capsule tears first, followed by the posterior cruciate ligament (PCL) and anterior cruciate ligament (ACL).
* Posterior Dislocations: Usually caused by a high-energy direct blow to the proximal tibia with the knee flexed (e.g., a "dashboard injury").
* Medial and Lateral Dislocations: Result from severe varus or valgus forces, respectively. These are highly associated with severe collateral ligament and capsular stripping.
* Rotary Dislocations: Designated further as anteromedial, anterolateral, posteromedial, or posterolateral. Posterolateral dislocations are particularly notorious for being irreducible via closed methods due to the medial femoral condyle buttonholing through the medial capsule.

Vascular Complications: The Popliteal Artery
The incidence of vascular injuries in knee dislocations is alarming, reported to range from 0% to 40% depending on the mechanism and energy of the trauma. The popliteal artery is uniquely vulnerable due to its rigid anatomic tethering proximally at the adductor hiatus and distally at the fibrous arch of the soleus muscle. During a dislocation, the artery is subjected to severe traction, leading to intimal flap tears, thrombosis, or complete transection.
🚨 SURGICAL WARNING: The "Golden 6 Hours"
The amputation rate is approximately 11% if vascular repair is performed within 6 hours of the ischemic event. This rate catastrophically increases to 86% if revascularization is delayed beyond this critical 6-hour window. Continued observation in anticipation of spontaneous improvement in a pulseless limb inevitably leads to disaster.
Prompt evaluation and early repair of any vascular damage are universally recommended. While some trauma centers utilize Ankle-Brachial Indices (ABI) to assess for vascular injury (with an ABI < 0.9 indicating the need for further imaging), an arteriogram or CT angiography is strongly recommended if the dislocation required reduction, regardless of palpable pulses. When there is any doubt concerning an injury to the popliteal artery, a thorough evaluation, including immediate arteriography and early surgical exploration by a vascular surgeon, is mandatory.
Neurological Complications
Nerve injuries occur in 16% to 43% of knee dislocations. The common peroneal nerve is injured most frequently, particularly in posterolateral and medial dislocations where severe traction is applied to the lateral aspect of the knee. The prognosis for the return of motor and sensory function after a severe traction injury to the peroneal nerve is highly guarded; permanent damage, resulting in a persistent foot drop, often results.
Initial Management and Closed Reduction
Knee dislocations can usually be reduced satisfactorily by closed methods in the emergency department under conscious sedation.
1. Reduction Technique: Longitudinal traction is applied to the tibia, followed by translation of the tibia in the direction opposite to the dislocation. Direct pressure over the displaced segments is often required.
2. Post-Reduction Care: After reduction, and in the absence of vascular complications requiring immediate surgery, aspiration of the hemarthrosis using strict sterile technique is performed. The knee is then immobilized in full extension (or 10-15 degrees of flexion to relax the popliteal artery) using a well-padded cylinder cast or a rigid knee immobilizer.
3. Monitoring: The neurocirculatory status must be checked frequently (every 2-4 hours) for the first 5 to 7 days, as delayed thrombosis from an intimal tear can occur.
In cases of profound instability where the knee cannot be maintained in a reduced position within a splint, temporary external fixation or transarticular pinning is indicated. A large, sterile transarticular Steinmann pin can be placed percutaneously through the intercondylar notch of the femur into the intercondylar eminence of the tibia to provide immediate, rigid stability.
INTRAARTICULAR DISLOCATIONS OF THE PATELLA
While lateral patellar dislocations are common, intraarticular dislocations of the patella are exceedingly rare and present a unique biomechanical challenge. These injuries typically occur secondary to high-energy direct trauma to the superior pole of the patella while the knee is flexed, or via a violent, uncoordinated contraction of the quadriceps mechanism.
Pathoanatomy and Classification
Intraarticular dislocations of the patella are broadly classified into two distinct horizontal types:
- Superior Pole Detachment (Most Common): This is a horizontal intraarticular dislocation characterized by the traumatic detachment of the quadriceps tendon from the superior pole of the patella. The patella rotates on its horizontal axis, and its articular surface is directed inferiorly toward the tibial plateau. The quadriceps mechanism is severely compromised.
- Inferior Pole Detachment: In this variant, the patella is also dislocated horizontally, but its inferior pole is avulsed from the patellar tendon. The patella flips such that its articular surface faces proximally toward the femoral shaft.
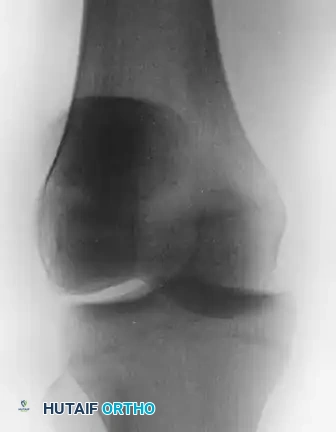
Clinical Presentation and Management Strategy
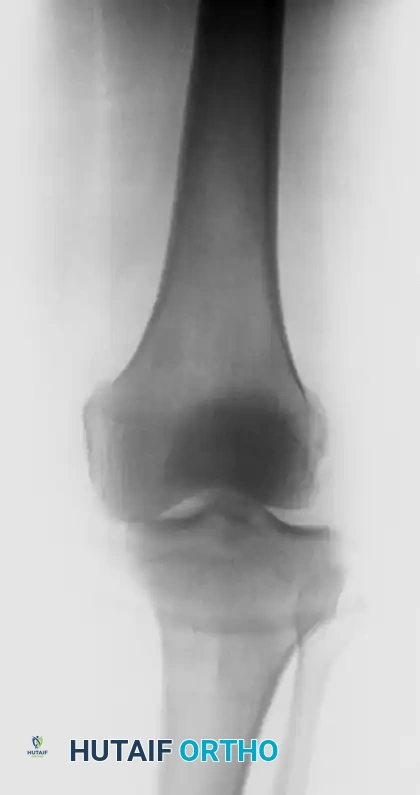
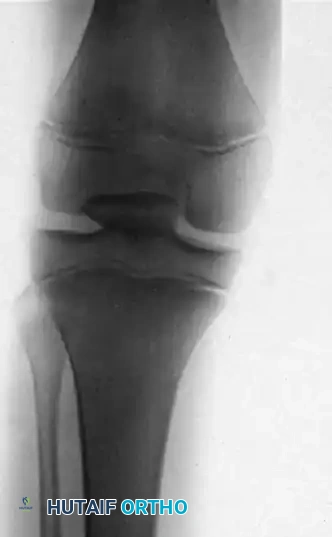
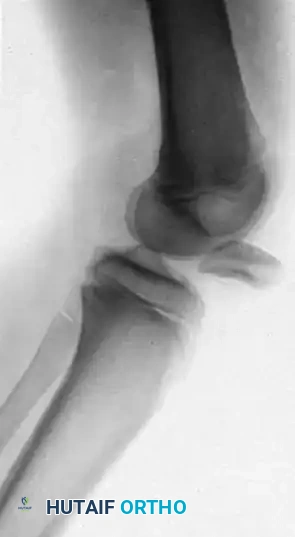
Patients present with a locked knee, severe pain, and a palpable void in the anterior knee where the patella normally resides. Radiographs will confirm the intraarticular position of the patella, often wedged tightly within the intercondylar notch.
Unlike standard lateral patellar dislocations, intraarticular dislocations are notoriously difficult to reduce by closed methods. The patella becomes mechanically locked beneath the femoral condyles, and the intact portion of the extensor mechanism acts as a tether, preventing reduction. Forcible closed reduction attempts are contraindicated as they frequently result in severe iatrogenic osteochondral damage to the patella and the femoral trochlea. Open reduction is generally required, combined with meticulous repair of the extensor mechanism and grafting or imbrication of the medial patellar retinaculum.
SURGICAL TECHNIQUE 60-3: OPEN REDUCTION AND GRAFTING OF THE MEDIAL PATELLAR RETINACULUM
The following surgical technique details the open reduction of an intraarticular patellar dislocation, the repair of the extensor mechanism, and the management of the medial patellar retinaculum to restore patellofemoral tracking and stability.
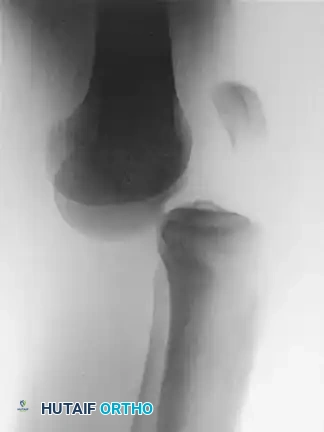
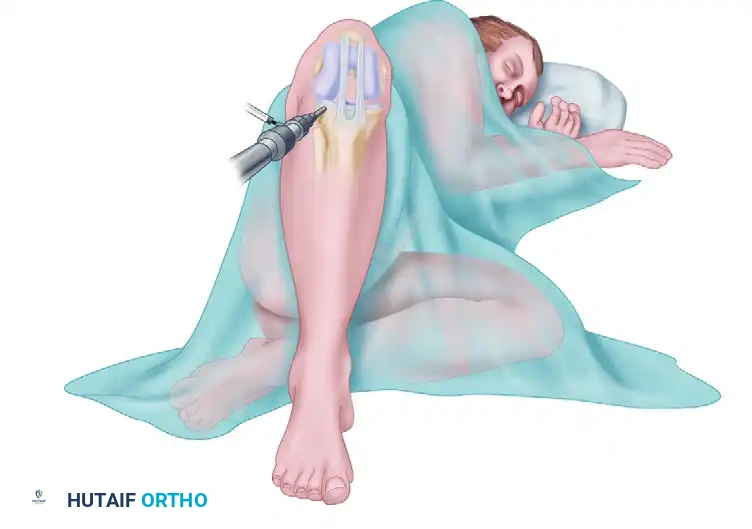
Preoperative Preparation and Positioning
- Anesthesia: General anesthesia or regional spinal anesthesia is utilized. Complete muscle relaxation is critical to overcome the resting tone of the quadriceps.
- Positioning: The patient is placed supine on a radiolucent operating table. A high-thigh pneumatic tourniquet is applied over generous padding.
- Prep and Drape: The affected lower extremity is prepped and draped in a standard sterile fashion, allowing for full, unhindered range of motion of the knee during the procedure.
Step 1: Surgical Approach and Exposure
- Exsanguinate the limb and inflate the tourniquet to the appropriate pressure (typically 250-300 mmHg).
- Make a standard medial parapatellar incision. Begin the incision proximal to the superior pole of the patella, extend it distally over the medial third of the patella, and terminate at the medial aspect of the tibial tubercle.
- Dissect through the subcutaneous tissues to expose the extensor mechanism.
- Perform a medial parapatellar arthrotomy. Carefully incise the medial retinaculum and capsule, taking care to preserve tissue quality for later repair or grafting.
- Retract the soft tissues to expose the dislocated patella, which is usually found firmly wedged within the intercondylar notch.
Step 2: Open Reduction of the Patella
- Thoroughly irrigate the joint to clear hematoma and improve visualization.
- Identify the orientation of the patella. Determine whether the quadriceps tendon or the patellar tendon has been avulsed.
- Using a blunt periosteal elevator or a bone hook, gently lever the patella out of the intercondylar notch.
💡 CLINICAL PEARL: Avoid using sharp instruments or excessive force against the articular cartilage of the femoral condyles or the patella. If the patella is incarcerated, slightly flexing the knee and applying distal traction to the intact tendon can help disengage it from the notch.
- Once disengaged, manually rotate the patella back into its correct anatomical orientation and replace it into its native bed within the trochlear groove.
Step 3: Extensor Mechanism Repair
- Debride the avulsed edge of the tendon (either quadriceps or patellar) to healthy, bleeding tissue.
- Prepare the corresponding pole of the patella by lightly decorticating the bone with a rongeur or burr to create a bleeding bony bed that will promote tendon-to-bone healing.
- Transosseous Fixation: Drill three to four longitudinal holes (using a 2.0 mm or 2.5 mm drill bit) through the patella, starting from the avulsed pole and exiting at the intact pole.
- Place heavy, non-absorbable sutures (e.g., #2 or #5 FiberWire or Ethibond) through the avulsed tendon using a locking Krackow or Bunnell stitch configuration.
- Pass the free ends of the sutures through the pre-drilled transosseous holes in the patella.
- With the knee in full extension to remove tension from the repair, tie the sutures securely over the bony bridge at the opposite pole of the patella. Reattach the patella firmly to its bed in the quadriceps or patellar tendon.
Step 4: Joint Inspection and Debridement
- Systematically inspect the entire knee joint. The violent nature of this dislocation frequently results in osteochondral shearing injuries.
- Remove any loose osteochondral or cartilaginous fragments from the medial and lateral gutters, the intercondylar notch, and the suprapatellar pouch.
- If a large, structurally significant osteochondral fragment is identified (particularly from the weight-bearing surface of the femur or the central patella), consider internal fixation using headless compression screws or bioabsorbable darts.
Step 5: Grafting and Repair of the Medial Patellar Retinaculum
- Assess the medial patellar retinaculum and the Medial Patellofemoral Ligament (MPFL). In cases of severe trauma, the medial structures are often attenuated, torn, or completely incompetent.
- If the native tissue is robust enough, perform a direct primary repair or a pants-over-vest imbrication using heavy absorbable sutures (e.g., #1 Vicryl or Stratafix) to restore medial tension and prevent lateral subluxation.
- If the medial retinaculum is severely deficient, grafting of the medial patellar retinaculum is indicated. An autograft (such as a strip of the semitendinosus tendon or a turndown flap from the quadriceps tendon) or an allograft can be utilized to reconstruct the MPFL and reinforce the medial retinaculum. The graft is secured to the medial border of the patella and anchored to the anatomic femoral insertion site (Schöttle's point) using interference screws or suture anchors.
Step 6: Closure
- Thoroughly irrigate the joint with sterile saline.
- Deflate the tourniquet and achieve meticulous hemostasis using electrocautery to prevent postoperative hemarthrosis.
- Close the arthrotomy and the retinacular layers securely.
- Close the subcutaneous tissue with interrupted absorbable sutures and the skin with staples or a subcuticular stitch.
- Apply sterile dressings and place the limb in a rigid cylinder cast or a locked hinged knee brace in full extension.
POSTOPERATIVE CARE AND REHABILITATION
The postoperative care for an open reduction of an intraarticular patellar dislocation with extensor mechanism repair closely mirrors the protocol for the repair of an acute lateral dislocation of the patella, with added precautions to protect the tendon-to-bone repair.
Phase I: Maximum Protection (Weeks 0-4)
* Immobilization: The knee is locked in full extension in a hinged knee brace or cylinder cast at all times.
* Weight-Bearing: Weight-bearing is typically restricted to toe-touch weight-bearing (TTWB) or non-weight-bearing (NWB) with crutches to prevent sudden eccentric loading of the repaired extensor mechanism.
* Exercises: Isometric quadriceps sets, straight leg raises (only if the repair is deemed highly secure and the surgeon permits), and ankle pumps are initiated immediately to prevent atrophy and deep vein thrombosis.
Phase II: Controlled Motion (Weeks 4-8)
* ROM Progression: The brace is unlocked to allow progressive, controlled flexion. Flexion is typically advanced by 30 degrees every 1 to 2 weeks, guided by the tension noted during the intraoperative repair.
* Weight-Bearing: Progress to partial weight-bearing (PWB) and eventually full weight-bearing (FWB) in the locked extension brace.
* Exercises: Begin active-assisted range of motion (AAROM) and gentle passive range of motion (PROM). Avoid active open-chain knee extension against resistance.
Phase III: Strengthening and Return to Function (Weeks 8-16+)
* Brace Weaning: The brace is gradually discontinued as quadriceps control normalizes and the patient can perform a straight leg raise without an extensor lag.
* Strengthening: Initiate closed-chain kinetic exercises (e.g., mini-squats, leg presses) to strengthen the quadriceps and hamstrings while minimizing patellofemoral joint reaction forces.
* Return to Play: Return to strenuous physical activity or sports is generally delayed until 4 to 6 months postoperatively, contingent upon the restoration of full, painless range of motion, normal patellofemoral tracking, and isokinetic strength reaching at least 85% to 90% of the contralateral uninjured limb.
You Might Also Like