Top Knee Arthroscopy Surgeons in Dallas: Your Trusted Guide
Key Takeaway
Discover the latest medical recommendations for Top Knee Arthroscopy Surgeons in Dallas: Your Trusted Guide. Top knee arthroscopy surgeons in Dallas, TX, include Dr. Michael Champine (OrthoTexas), Dr. Robert Berry (Texas Sports Medicine and Orthopaedics), Dr. Mark Sanders (Southwest Sports Medicine), Dr. Paul DeGenova (Texas Orthopaedic Associates), and Dr. William Longton (Premier Orthopaedics). These highly experienced, board-certified surgeons in Dallas specialize in sports medicine and arthroscopic procedures, offering personalized care for various knee joint issues.
Introduction & Epidemiology
Knee arthroscopy, a cornerstone procedure in orthopedic surgery, involves the minimally invasive visualization and manipulation of intra-articular knee structures through small portals. Its evolution from a diagnostic tool to a comprehensive therapeutic modality has revolutionized the management of various knee pathologies. The foundational principles include distention of the joint space, strategic portal placement, and systematic examination, allowing for precise intervention with reduced morbidity compared to traditional open approaches.
The knee joint is frequently subjected to acute and chronic injuries due to its complex biomechanics and exposure to high loads during daily activities and athletic endeavors. Epidemiologically, meniscal tears are among the most common intra-articular lesions, with an incidence estimated at 60-70 per 100,000 annually. Anterior cruciate ligament (ACL) ruptures also represent a significant burden, particularly in athletic populations, with an incidence ranging from 30 to 78 per 100,000. Chondral lesions, patellofemoral instability, loose bodies, and synovial disorders further contribute to the prevalence of conditions amenable to arthroscopic intervention. The demographics of these injuries vary, with ACL tears peaking in young, active individuals and degenerative meniscal tears increasing with age. The refinement of arthroscopic techniques, instrumentation, and rehabilitation protocols continues to enhance diagnostic accuracy, treatment efficacy, and patient outcomes, solidifying its role as an indispensable procedure in modern orthopedic practice.
Surgical Anatomy & Biomechanics
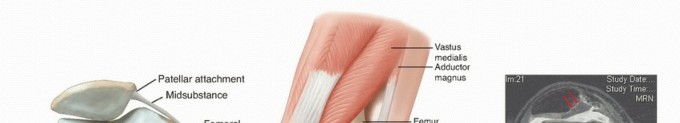
A thorough understanding of knee joint anatomy and biomechanics is paramount for safe and effective arthroscopic surgery. The knee is a modified hinge joint, primarily involving the articulation between the distal femur and proximal tibia, with the patella articulating with the femoral trochlea.
Bony Anatomy:
*
Femur:
Distal articular surfaces comprise the medial and lateral femoral condyles, separated by the intercondylar notch. The patellofemoral articulation involves the trochlear groove anteriorly.
*
Tibia:
The proximal articular surface consists of the medial and lateral tibial plateaus, separated by the intercondylar eminence (tibial spines).
*
Patella:
A sesamoid bone within the quadriceps tendon, it articulates with the femoral trochlea.
Ligamentous Structures:
*
Cruciate Ligaments:
*
Anterior Cruciate Ligament (ACL):
Originates from the posteromedolateral aspect of the medial wall of the lateral femoral condyle and inserts into the anteromedial aspect of the intercondylar area of the tibial plateau, anterior to the tibial spines. Primary restraint to anterior tibial translation and secondary restraint to internal and external rotation. Composed of anteromedial (AM) and posterolateral (PL) bundles, which are relatively isometric through knee range of motion.
*
Posterior Cruciate Ligament (PCL):
Originates from the anterolateral aspect of the medial femoral condyle and inserts into the posterior aspect of the tibial plateau, inferior to the joint line. Primary restraint to posterior tibial translation. Composed of anterolateral (AL) and posteromedial (PM) bundles.
*
Collateral Ligaments:
*
Medial Collateral Ligament (MCL):
Superficial and deep layers. Originates from the medial femoral epicondyle and inserts onto the medial tibial condyle. Primary restraint to valgus stress.
*
Lateral Collament Ligament (LCL):
Cord-like structure, originates from the lateral femoral epicondyle and inserts onto the fibular head. Primary restraint to varus stress. Part of the posterolateral corner (PLC) complex, which also includes the popliteus tendon, popliteofibular ligament, and arcuate complex.
Menisci:
* Crescent-shaped fibrocartilaginous structures (medial and lateral) that sit on the tibial plateaus. They function in load transmission, shock absorption, joint stability, and lubrication.
*
Medial Meniscus:
C-shaped, broader posteriorly. Firmly attached to the tibial plateau via coronary ligaments and to the joint capsule, and by the deep MCL fibers. Less mobile than the lateral meniscus, making it more prone to injury.
*
Lateral Meniscus:
More circular (O-shaped), smaller in radius. Attached to the tibia via coronary ligaments but not directly to the LCL, making it more mobile. Posteriorly, it has attachments to the femur via the meniscofemoral ligaments of Wrisberg and Humphry.
*
Blood Supply:
Primarily from peripheral capsular attachments (red-red zone), gradually becoming avascular centrally (white-white zone). This vascularity dictates meniscal repair potential.
Articular Cartilage:
* Hyaline cartilage covers the femoral condyles, tibial plateaus, and posterior patellar surface. Critical for smooth, low-friction joint motion. Damage can lead to progressive osteoarthritis.
Synovium & Plicae:
* The synovial membrane lines the joint capsule, producing synovial fluid for lubrication and nutrition. Synovial plicae are embryonic remnants (suprapatellar, infrapatellar, medial) that can become symptomatic (e.g., medial plica syndrome).
Neurovascular Structures (relevant to portal placement):
*
Anteromedial/Anterolateral portals:
Risk to infrapatellar branch of the saphenous nerve (medially), common peroneal nerve (laterally, more distal) and its branches.
*
Posteromedial/Posterolateral portals:
Risk to saphenous nerve and vein (medially), common peroneal nerve (laterally), and the popliteal artery and vein (posteriorly). Meticulous portal placement and visualization are critical.
Biomechanics:
*
Knee Stability:
Provided by static restraints (ligaments, capsule, menisci) and dynamic restraints (muscles, tendons). The ACL is a crucial stabilizer against anterior translation and rotational forces. The PCL resists posterior translation. MCL/LCL resist valgus/varus stresses.
*
Meniscal Function:
Distribute axial loads across the joint, increasing the contact area, thereby reducing stress on articular cartilage. They also contribute to joint stability, particularly the medial meniscus in restraining anterior tibial translation (secondary restraint).
*
Patellofemoral Mechanics:
The patella enhances the quadriceps lever arm. Normal tracking is vital, influenced by quadriceps balance, V-angle, trochlear morphology, and soft tissue restraints (e.g., medial patellofemoral ligament - MPFL).
Indications & Contraindications
Knee arthroscopy is indicated for a wide spectrum of intra-articular pathologies, serving both diagnostic and therapeutic purposes. Careful patient selection is crucial for optimizing outcomes.
Indications for Knee Arthroscopy:
| Category | Operative Indications | Non-Operative Indications |
|---|---|---|
| Meniscal Pathology | Repairable tears: Longitudinal, radial, bucket-handle tears in the vascularized (red-red or red-white) zone, often associated with ACL reconstruction. Symptomatic meniscal cysts. | Stable, asymptomatic tears: Small, peripheral, degenerative tears in the avascular zone, particularly if symptoms are mild or responsive to conservative measures. Degenerative tears in older, less active individuals, often managed with physical therapy and NSAIDs. |
| Ligamentous Instability | ACL Rupture: Symptomatic instability, especially in active individuals, often requiring reconstruction. PCL Rupture: High-grade instability, symptomatic cases, often requiring reconstruction (less common than ACL). Multi-ligamentous injury. | Low-grade (Grade I/II) ACL/PCL sprains: Without significant instability. MCL/LCL tears (isolated): Often heal with bracing and rehabilitation unless high-grade and associated with other injuries (e.g., PLC). |
| Articular Cartilage | Symptomatic chondral defects: Full-thickness or deep partial-thickness lesions causing pain, catching, or mechanical symptoms. Procedures include chondroplasty, microfracture, osteochondral autograft/allograft transfer, Autologous Chondrocyte Implantation (ACI), or scaffold implantation. | Asymptomatic chondral lesions: Mild, superficial lesions. Diffuse Grade I-II chondromalacia: Mild symptoms responsive to activity modification, bracing, and physical therapy. |
| Loose Bodies | Symptomatic intra-articular loose bodies: Causing locking, catching, pain, or effusion. | Asymptomatic, non-impinging loose bodies: Occasionally observed, but removal is generally recommended to prevent future symptoms or cartilage damage. |
| Synovial Pathology | Chronic synovitis: Refractory to conservative management (e.g., rheumatoid arthritis, pigmented villonodular synovitis - PVNS). Symptomatic synovial plicae. Synovial chondromatosis. | Acute, mild synovitis: Often resolves with rest, anti-inflammatory medication, and activity modification. |
| Patellofemoral | Recurrent patellar dislocation/subluxation: Medial Patellofemoral Ligament (MPFL) reconstruction, lateral retinacular release (less common as isolated procedure). Chondral damage of patella/trochlea with mechanical symptoms. | Mild patellofemoral pain syndrome (PFPS): Often responsive to physical therapy, quadriceps strengthening, vastus medialis obliquus (VMO) retraining, and activity modification. First-time patellar dislocation without significant chondral injury or persistent instability. |
| Infection | Septic arthritis: Diagnostic aspiration and arthroscopic lavage, debridement, and biopsy. | N/A (Septic arthritis requires prompt intervention; non-operative is not an option for definitive treatment.) |
| Fractures | Intra-articular fractures: Tibial plateau, intercondylar eminence, osteochondral fractures. Used for reduction, fixation, and assessment of associated soft tissue injuries. | Stable, non-displaced intra-articular fractures: Managed with casting/bracing and protected weight-bearing. |
| Diagnostic | Persistent, undiagnosed knee pain/effusion: After failed non-operative management and inconclusive non-invasive imaging. | N/A (Considered after exhaustion of non-invasive diagnostic modalities.) |
Contraindications:
-
Absolute Contraindications:
- Active infection: Systemic sepsis or active infection in the vicinity of the knee, which could lead to joint contamination.
- Severe uncontrolled medical comorbidities: Rendering the patient unable to tolerate anesthesia or the surgical stress.
- Ankylosed knee: Limited or no range of motion, making portal placement and instrument manipulation technically challenging or impossible.
- Severely contracted joint: Unable to achieve adequate joint distention or visualization.
-
Relative Contraindications:
- Severe osteoarthritis (OA): While arthroscopy has a limited role in end-stage OA, it may be considered for mechanical symptoms (e.g., loose bodies, meniscal tears) in select patients who are not candidates for arthroplasty or as a temporizing measure. Outcomes are generally inferior to primary arthroplasty for diffuse OA.
- Extremely obese patients: Increased technical difficulty, portal complications, and potential for reduced visualization.
- Severe vascular disease: Increased risk of complications with tourniquet use.
- Cutaneous lesions: Active dermatological conditions or open wounds overlying planned portal sites.
- Lack of patient compliance: For post-operative rehabilitation, which is crucial for successful outcomes.
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning and appropriate patient positioning are critical for optimizing surgical efficiency, minimizing complications, and achieving desired outcomes in knee arthroscopy.
Pre-Operative Planning:
1.
Clinical Assessment:
*
Detailed History:
Mechanism of injury, duration of symptoms, nature of pain, mechanical symptoms (locking, catching, giving way), previous treatments, functional limitations, activity level, and patient expectations.
*
Comprehensive Physical Examination:
Assessment of effusion, range of motion (ROM), ligamentous stability (Lachman, pivot shift, posterior drawer, varus/valgus stress tests), meniscal integrity (McMurray, Apley), patellofemoral tracking, and neurovascular status.
2.
Imaging Studies:
*
Standard Radiographs:
AP, lateral, Merchant (patellofemoral), and Rosenberg (weight-bearing 45° flexion posteroanterior) views are essential to assess bony alignment, joint space narrowing, osteophytes, and occult fractures.
*
Magnetic Resonance Imaging (MRI):
Gold standard for soft tissue evaluation (menisci, ligaments, cartilage, bone marrow edema). Crucial for confirming diagnosis and planning specific interventions. Understand MRI sequences (T1, T2, fat-suppressed) and their utility.
*
Computed Tomography (CT):
Useful for detailed bony architecture, fracture characterization, and patellofemoral morphometry (e.g., trochlear dysplasia, tibial tubercle-trochlear groove distance - TT-TG).
3.
Anesthesia Consultation:
Evaluation of patient comorbidities, choice of anesthesia (general, spinal, regional block, or a combination), and discussion of post-operative pain management strategies (e.g., adductor canal block).
4.
Informed Consent:
Thorough discussion with the patient regarding the diagnosis, proposed procedure, potential risks (infection, neurovascular injury, DVT, stiffness, persistent pain, graft failure), benefits, alternatives, and anticipated rehabilitation.
Patient Positioning:
1.
Anesthesia Induction:
Administer anesthesia as planned.
2.
Supine Position:
The patient is positioned supine on the operating table.
3.
Tourniquet Application:
A pneumatic tourniquet is typically applied to the proximal thigh to provide a bloodless field, which enhances visualization. The tourniquet cuff should be wide enough to minimize pressure per unit area and applied securely. Tourniquet time and pressure must be monitored meticulously (e.g., 250-300 mmHg or 100 mmHg above systolic BP, for no longer than 90-120 minutes without reperfusion).
4.
Leg Holder vs. Lateral Post/Bolster:
*
Leg Holder:
Often used for more extensive procedures like ACL reconstruction. Provides stable knee positioning and allows for valgus/varus stress and flexion/extension. The contralateral leg is often placed in a well-padded stirrup or frog-legged position.
*
Lateral Post/Bolster:
For diagnostic arthroscopy or less extensive procedures. A padded bolster under the ankle or foot, or a lateral post, allows gravity to assist in valgus stress, opening the medial compartment.
5.
Preparation and Draping:
The limb is prepped from the iliac crest to the toes using an antiseptic solution. Sterile draping isolates the surgical field, typically allowing free manipulation of the operative leg.
6.
Establishing Traction/Distraction:
For some procedures (e.g., meniscal repair, visualization of the posterior compartment), a distractor or additional manual traction may be beneficial to open the joint space.
7.
Portal Planning:
Before skin incision, key bony landmarks (patella, patellar tendon, tibial tubercle, femoral epicondyles, joint line) are palpated and marked. Planned portal sites are drawn, considering the pathology, desired instrument trajectories, and proximity to neurovascular structures. Common portals include:
*
Anteromedial (AM):
Superior to the medial meniscus, medial to the patellar tendon.
*
Anterolateral (AL):
Superior to the lateral meniscus, lateral to the patellar tendon.
*
Superomedial/Superolateral:
For the suprapatellar pouch.
*
Posteromedial/Posterolateral:
For posterior compartment visualization and treatment.
*
Accessory portals:
For specific instrument access (e.g., accessory anteromedial portal for femoral ACL tunnel drilling).
Detailed Surgical Approach / Technique
Knee arthroscopy encompasses a wide range of procedures. The following outlines general principles and specific techniques for common arthroscopic interventions.
General Arthroscopic Principles:
1.
Joint Distention:
After prepping and draping, the knee is distended with sterile saline, typically using an arthroscopy pump or gravity. Adequate distention creates space for visualization and instrument manipulation. Maintain appropriate pump pressure (e.g., 30-50 mmHg).
2.
Portal Creation:
* A small skin incision (approximately 5-7 mm) is made with a #11 blade at the planned portal site.
* A mosquito clamp or blunt trocar is then used to penetrate the joint capsule, ensuring controlled entry and avoiding iatrogenic chondral damage.
* The arthroscope with cannula is inserted through the primary viewing portal (commonly anterolateral).
3.
Systematic Diagnostic Arthroscopy:
A thorough, systematic examination of all knee compartments is performed, regardless of the suspected pathology.
*
Suprapatellar Pouch:
Synovium, patellofemoral tracking, articular cartilage of patella and trochlea.
*
Medial Gutter:
Medial plica, medial femoral condyle.
*
Medial Compartment:
Medial meniscus (anterior horn, body, posterior horn), medial tibial plateau cartilage, medial femoral condyle cartilage. Probe all meniscal surfaces and evaluate stability.
*
Intercondylar Notch:
ACL (integrity, tension, footprint), PCL, cyclops lesions.
*
Lateral Compartment:
Lateral meniscus (anterior horn, body, posterior horn), lateral tibial plateau cartilage, lateral femoral condyle cartilage. Probe all meniscal surfaces.
*
Lateral Gutter:
Lateral plica, popliteus tendon (in its sheath).
*
Posterior Compartment (if needed):
Via posteromedial/posterolateral portals to visualize posterior meniscal horns, PCL, loose bodies. This requires careful triangulation and neurovascular awareness.
Specific Arthroscopic Procedures:
1. Meniscal Surgery
-
Arthroscopic Partial Meniscectomy:
- Indications: Irreparable meniscal tears (degenerative tears, complex tears, radial tears, parrot-beak tears), tears in the avascular zone causing mechanical symptoms.
- Technique: Access through accessory portals for instrument insertion. Unstable portions of the meniscus are resected using basket forceps, punches, and motorized shavers. The goal is to create a stable, smooth rim, removing only the damaged tissue while preserving as much functional meniscus as possible. Avoid leaving large, irregular tags that can cause continued impingement. Radiofrequency devices may be used for final contouring or hemostasis.
-
Meniscal Repair:
- Indications: Peripheral, longitudinal, vertical, bucket-handle tears in the vascularized (red-red or red-white) zone, often associated with ACL reconstruction. Tears >1 cm, stable on probing. Patient age and activity level are factors.
-
Techniques:
- All-Inside Repair: Devices passed entirely within the joint, fixing the meniscus to the capsule. Examples include suture devices with anchors/implants. Simpler, but potential for non-anatomic fixation.
- Inside-Out Repair: Long needles loaded with suture are passed from inside the joint, through the meniscus and capsule, and retrieved extracapsularly. Requires a posterior or medial/lateral incision to retrieve needles and tie sutures over the capsule. Considered the gold standard for many tears, allowing precise reduction and secure knot tying.
- Outside-In Repair: Needles are passed from outside the joint, through the capsule and meniscus, retrieved in the joint, and tied over the capsule extracapsularly. Useful for anterior horn tears or tears closer to the periphery.
- Principles: Debridement of tear edges to stimulate healing, rasping of the capsular attachment to promote bleeding, accurate reduction of the tear.
2. ACL Reconstruction
-
Graft Harvest:
-
Autografts:
- Bone-Patellar Tendon-Bone (BPTB): Central 1/3 of patellar tendon with bony plugs. Strong initial fixation. Potential for anterior knee pain, patellar fracture.
- Hamstring Tendons (Semitendinosus/Gracilis - ST/G): Harvested through a small anteromedial incision. Less anterior knee pain. Potential for hamstring weakness, tunnel widening.
- Quadriceps Tendon (QT): With or without bone plug. Strong, large graft. Emerging popularity.
- Allografts: Cadaveric grafts (e.g., BPTB, Achilles). Avoids donor site morbidity but carries risks of disease transmission (minimal) and slower incorporation. Often used in revision cases or less active patients.
-
Autografts:
-
Femoral Tunnel Creation:
- Anteromedial (AM) Portal Technique: Gold standard for anatomic tunnel placement. The knee is hyperflexed to 110-120 degrees. A guide pin is inserted through the AM portal, aiming for the center of the native ACL footprint on the lateral femoral condyle. Over-the-top guides or specific drill guides are used. Drilling is performed outside-in, or reaming over the guide pin.
- Transtibial Technique (less common for primary): The femoral tunnel is drilled through the tibial tunnel, limiting independent femoral tunnel placement and often leading to a more vertical graft.
-
Tibial Tunnel Creation:
- An ACL tibial drill guide is used. The guide pin is placed at the center of the native ACL footprint on the tibial plateau, posterior to the anterior horn of the lateral meniscus. The tunnel is reamed over the guide pin.
-
Graft Passage and Fixation:
- The chosen graft is prepared and passed through the tibial and femoral tunnels.
-
Fixation:
Secure initial fixation is critical.
- Femoral: Suspensory devices (e.g., Endobutton, toggle button) allow cortical fixation away from the joint line. Interference screws provide compression within the tunnel.
- Tibial: Interference screw, staple, post-and-tie.
- Tensioning: Graft is typically tensioned near full extension (20-30 degrees of flexion) to restore normal kinematics while avoiding over-tensioning.
- Concurrent Procedures: Meniscal repair, chondroplasty, or lateral extra-articular tenodesis (LEAT) for high-risk patients.
3. Chondral Lesion Management
-
Chondroplasty/Debridement:
- Indications: Fibrillated, unstable articular cartilage that is not full-thickness.
- Technique: Loose cartilage flaps are resected and debrided using shavers or radiofrequency devices, smoothing the surface to reduce mechanical irritation.
-
Microfracture:
- Indications: Small (1-2 cm²), contained full-thickness chondral defects, healthy surrounding cartilage, good bone stock, aligned limb.
- Technique: The lesion is debrided to a stable rim. An awl is used to penetrate the subchondral bone, creating multiple small holes (4-5 mm apart) to allow marrow elements (mesenchymal stem cells, growth factors) to egress and form a "superclot" that differentiates into fibrocartilage. The subchondral plate should not be excessively violated.
-
Osteochondral Autograft Transfer (OATS/Mosaicplasty):
- Indications: Larger, contained full-thickness defects (>1 cm²) in high-load areas.
- Technique: Cylindrical plugs of healthy articular cartilage and subchondral bone are harvested from a less weight-bearing area (e.g., intercondylar notch, superolateral femoral condyle) and transplanted into the prepared defect.
-
Autologous Chondrocyte Implantation (ACI):
- Indications: Larger full-thickness defects, particularly in younger patients. Two-stage procedure.
-
Technique:
- Stage 1: Arthroscopic harvest of healthy chondrocytes.
- Stage 2: Open arthrotomy or second-stage arthroscopy for implantation of expanded chondrocytes, often under a periosteal patch or scaffold (MACI - Matrix-associated ACI).
4. Loose Body Removal
- Technique: After localization, loose bodies are retrieved using grasper forceps. Sometimes they are lodged in recesses and require manipulation or additional portals for extraction.
5. Synovectomy/Plica Resection
- Indications: Symptomatic chronic synovitis, refractory plica syndrome.
- Technique: Motorized shavers are used to resect hypertrophic synovial tissue or symptomatic plicae. Careful attention to avoid damaging articular cartilage or menisci.
6. Septic Arthritis
- Technique: Arthroscopic lavage involves copious irrigation (e.g., 6-10 liters of saline) and debridement of purulent material and fibrin clots. Synovial biopsy for culture and histopathology.
Complications & Management
Despite its minimally invasive nature, knee arthroscopy is associated with potential complications, ranging from minor to limb-threatening. Vigilant recognition and prompt management are essential.
| Complication | Incidence (Approx.) | Salvage Strategy / Management |
|---|---|---|
| Infection (Septic Arthritis) | 0.1% - 0.5% | Early recognition: Persistent pain, fever, erythema, swelling beyond expected. Diagnosis: Aspiration and synovial fluid analysis (cell count, differential, gram stain, culture). Treatment: Urgent arthroscopic lavage and debridement, appropriate intravenous antibiotics based on culture results (empiric initially), and repeat lavage if needed. |
| Deep Vein Thrombosis (DVT) | 0.1% - 1.0% | Prevention: Early mobilization, mechanical prophylaxis (compression stockings, pneumatic compression devices). Pharmacological prophylaxis for high-risk patients. Diagnosis: Clinical suspicion, D-dimer, duplex ultrasound. Treatment: Anticoagulation. Monitor for Pulmonary Embolism (PE). |
| Neurovascular Injury | < 0.1% | Prevention: Meticulous portal placement, blunt dissection, direct visualization. Nerve (e.g., saphenous, common peroneal): Neuropraxia often resolves spontaneously. Persistent deficit may require neurolysis or repair. Vascular (e.g., popliteal artery): Urgent vascular surgery consultation, repair, and monitoring for compartment syndrome. |
| Hemarthrosis | 1% - 5% | Prevention: Meticulous hemostasis, tourniquet deflation and port closure. Management: Aspiration (diagnostic and therapeutic), compression bandage, RICE (Rest, Ice, Compression, Elevation). If severe, arthroscopic lavage to evacuate clots. |
| Arthrofibrosis/Stiffness | 1% - 10% | Prevention: Early, controlled range of motion (ROM) exercises, appropriate rehabilitation protocols. Management: Intensive physical therapy, pain control, possibly manipulation under anesthesia (MUA) if unresponsive, or arthroscopic lysis of adhesions and debridement of scar tissue. |
| Iatrogenic Chondral Injury | 0.5% - 2% | Prevention: Careful instrument insertion, avoidance of forceful impaction. Management: Small, stable lesions may be observed. Larger or symptomatic lesions may require microfracture, chondroplasty, or other cartilage repair techniques depending on size and location. |
| Instrument Breakage | Rare | Prevention: Use of appropriate instruments, inspection for wear. Management: Retrieval with specialized grasping instruments. If fragment cannot be retrieved arthroscopically, open arthrotomy may be necessary. Inform patient immediately. |
| Complex Regional Pain Syndrome (CRPS) | < 0.1% | Prevention: Adequate pain control, early mobilization. Diagnosis: Clinical (Budapest criteria), nerve blocks. Management: Multidisciplinary approach involving pain management specialists, physical therapy, sympathetic blocks, medications (gabapentin, tricyclic antidepressants). Early recognition is crucial. |
| Graft Failure/Rerupture (ACL) | 2% - 10% (primary) | Prevention: Anatomic tunnel placement, secure fixation, appropriate rehabilitation, adherence to return-to-sport guidelines. Management: Revision ACL reconstruction, addressing modifiable risk factors (e.g., alignment, meniscal deficiency, graft choice, surgical technique). |
| Persistent Pain/Symptoms | Variable | Diagnosis: Re-evaluation of diagnosis, imaging (MRI), physical exam to rule out missed pathology, malalignment, arthrofibrosis, or nerve irritation. Management: Targeted physical therapy, injections, nerve blocks, or revision surgery if a specific cause is identified and amenable to intervention. Consider psychological factors and chronic pain management. |
| Tourniquet Complications | Rare | Prevention: Proper cuff size, appropriate pressure, monitoring of time. Management: Nerve neuropraxia usually resolves. Skin/muscle damage is rare but requires wound care. Compartment syndrome requires urgent fasciotomy. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is as critical as the surgical procedure itself for optimizing patient recovery and functional outcomes. Protocols vary significantly based on the specific procedure performed, patient factors, and surgeon preference. The overarching goals are to reduce pain and swelling, restore range of motion, regain strength, improve proprioception, and facilitate a safe return to activity.
General Principles:
1.
Pain and Swelling Management:
RICE (Rest, Ice, Compression, Elevation) is initiated immediately. Analgesics (NSAIDs, opioids as needed) and nerve blocks (e.g., adductor canal) are crucial.
2.
Early Protected Motion:
Initiate controlled, passive, and active-assisted range of motion exercises as soon as tolerated to prevent stiffness and promote cartilage health.
3.
Weight-Bearing Progression:
Varies greatly by procedure, often involving crutches and a brace.
4.
Progressive Strengthening:
Focus on quadriceps, hamstrings, gluteal muscles, and core stability.
5.
Proprioception and Neuromuscular Control:
Balance exercises, single-leg stance, functional movements.
6.
Functional Progression:
Gradually reintroduce sport-specific drills and activities.
Procedure-Specific Protocols:
1. After Arthroscopic Partial Meniscectomy
-
Phase 1 (Weeks 0-2): Protection & Early Motion
- Weight-Bearing (WB): Full weight-bearing (FWB) as tolerated immediately, often with crutches for comfort initially.
- ROM: Immediate full active and passive ROM as tolerated.
- Exercises: Quadriceps sets, straight leg raises (SLRs), ankle pumps, hamstring curls, gentle knee flexion/extension.
- Goals: Control pain/swelling, achieve FWB without limp, restore full ROM.
-
Phase 2 (Weeks 2-6): Intermediate Strengthening
- WB: FWB.
- Exercises: Stationary bike, elliptical, progressive resistance exercises (PRE) for quads/hams, balance/proprioception.
- Goals: Restore normal gait, improve strength, prepare for higher-level activities.
-
Phase 3 (Weeks 6+): Advanced Strengthening & Return to Activity
- Exercises: Progress to plyometrics, sport-specific drills.
- Return to Activity: Typically 4-6 weeks for light activity, 6-12 weeks for full activity/sports.
2. After Arthroscopic Meniscal Repair
-
Phase 1 (Weeks 0-4/6): Protection & Limited WB/ROM
- WB: Non-weight-bearing (NWB) or touch-down weight-bearing (TDWB) with crutches. Progressive partial weight-bearing (PWB) starting around week 3-4.
- ROM: Restricted, often limited to 0-90 degrees flexion. Brace locked in extension for ambulation. Avoid deep squats or hamstring curls against resistance.
- Exercises: Quadriceps sets, SLRs (without active hip flexion if hamstrings are involved), ankle pumps.
- Goals: Protect repair, control pain/swelling, maintain muscle tone.
-
Phase 2 (Weeks 4/6-12): Gradual WB/ROM Progression
- WB: PWB progresses to FWB. Discontinue crutches around 6-8 weeks.
- ROM: Gradually increase flexion, aiming for full ROM by 10-12 weeks. Brace may be unlocked for exercises but still used for protection.
- Exercises: Stationary bike, gentle swimming, light PRE, balance exercises.
- Goals: Restore FWB without limp, achieve full ROM, initial strength gains.
-
Phase 3 (Weeks 12-24): Advanced Strengthening & Functional Training
- Exercises: Progressive PRE, plyometrics, agility drills.
- Return to Activity: Very gradual return to cutting sports at 4-6 months, often longer for high-demand sports. Full return to sport (RTS) typically 6 months or more, based on clinical criteria and functional testing.
3. After ACL Reconstruction
-
Phase 1 (Weeks 0-2/4): Protection & Early Motion
- WB: TDWB to PWB with crutches, progressing to FWB over 2-4 weeks. Brace locked in extension for ambulation.
- ROM: Achieve full extension immediately. Flexion progressed as tolerated, aiming for 90-100 degrees by 2 weeks. CPM may be used.
- Exercises: Quadriceps sets, SLRs, calf pumps, gentle passive knee flexion.
- Goals: Control pain/swelling, protect graft, achieve full extension, initial flexion.
-
Phase 2 (Weeks 4-12): Intermediate Strengthening & Proprioception
- WB: FWB without crutches. Brace used for protection, often discontinued by 6-12 weeks.
- ROM: Full ROM achieved and maintained.
- Exercises: Stationary bike, elliptical, light PRE (leg press, wall squats), balance board, controlled lunges. Avoid open-chain resisted knee extension between 0-45 degrees if BPTB, or cautious if hamstring graft, due to anterior shear forces on the graft.
- Goals: Restore normal gait, eliminate effusion, improve strength and neuromuscular control.
-
Phase 3 (Months 3-6): Advanced Strengthening & Agility
- Exercises: Progressive resistance, running progression, agility drills, plyometrics. Introduce sport-specific movements.
- Goals: Achieve significant strength parity (LSI > 80%), prepare for sport-specific training.
-
Phase 4 (Months 6-12+): Return to Sport
- Criteria for RTS: No pain/swelling, full ROM, quadriceps/hamstring strength symmetry (>90% limb symmetry index - LSI), functional tests (single-leg hop, triple hop, crossover hop) >90% LSI, psychological readiness.
- Risk Mitigation: RTS before 9 months significantly increases re-rupture risk. Gradual integration into sport.
4. After Chondral Repair (e.g., Microfracture, OATS)
-
Phase 1 (Weeks 0-6/8): Strict Protection & NWB/PWB
- WB: NWB to TDWB on crutches, often for 6-8 weeks, sometimes longer.
- ROM: Varies significantly. Often limited initially, or using CPM for specific angles/durations.
- Exercises: Quadriceps sets, SLRs (avoiding active hip flexion with OATS donor site), gentle passive ROM.
- Goals: Protect healing cartilage, minimize shear forces.
-
Phase 2 (Weeks 8-16): Gradual WB & ROM
- WB: PWB progresses to FWB.
- ROM: Gradually increase, aiming for functional ROM.
- Exercises: Stationary bike (low resistance), pool exercises, light PRE.
-
Phase 3 (Months 4-6+): Progressive Strengthening & Functional Training
- Exercises: Increase resistance, balance training, elliptical. Avoid high-impact activities for extended periods (6-12+ months).
- Return to Activity: Very slow, gradual return. Light activities may resume at 6-9 months, high-impact or cutting sports often not before 9-12 months, or never, depending on the size and location of the defect.
Summary of Key Literature / Guidelines
The field of knee arthroscopy is continuously evolving, driven by ongoing research and technological advancements. Adherence to evidence-based medicine and professional society guidelines is paramount.
Key Literature and Influential Studies:
-
Meniscal Surgery:
- "Healing Potential of Meniscal Tears": Early work by Annandale (1879) and later by Cassidy and McEvoy (1960s) highlighted the importance of meniscal preservation. Seminal work by Stone, Miller, and Scott established modern meniscal repair techniques.
- "Arthroscopic Meniscectomy vs. Meniscal Repair": Numerous studies demonstrate superior long-term outcomes (reduced risk of osteoarthritis) with meniscal repair compared to meniscectomy, especially for tears in the vascular zone. However, repair has a longer rehabilitation and higher re-operation rate for failed repair.
- "Degenerative Meniscal Tears": Multiple randomized controlled trials (e.g., by Katz et al., Kise et al.) have shown that arthroscopic partial meniscectomy for degenerative meniscal tears in middle-aged or older patients with mild or no osteoarthritis provides no additional benefit over supervised exercise and physical therapy. This has significantly shifted practice towards non-operative management for these specific tear patterns.
-
ACL Reconstruction:
- MOON Group (Multicenter Orthopaedic Outcomes Network): This collaborative research group has published extensively on outcomes, graft choices, tunnel placement, and predictors of failure in ACL reconstruction. Their work emphasizes the importance of anatomical tunnel placement and identifies factors influencing graft re-rupture rates.
- "Anatomic Single-Bundle vs. Double-Bundle ACLR": Initial enthusiasm for double-bundle techniques aimed to restore full anatomy. However, meta-analyses and RCTs have largely shown no consistent clinical superiority over well-performed anatomic single-bundle reconstruction, which remains the gold standard.
- "Return to Sport (RTS) Criteria": Research consistently demonstrates that returning to pivoting sports before 9 months post-ACLR, especially without meeting functional strength and hop test criteria (LSI > 90%), significantly increases the risk of re-rupture. Consensus guidelines advocate for objective, battery-based testing for RTS.
- "Lateral Extra-articular Tenodesis (LEAT)": Recent studies, particularly the STaR trial, suggest that concomitant LEAT with ACLR may reduce graft failure rates in high-risk patients (e.g., young athletes with high-grade pivot shift, revision cases).
-
Articular Cartilage Repair:
- "Microfracture Outcomes": While effective for smaller, contained lesions, long-term follow-up often shows fibrocartilage formation rather than hyaline cartilage, with potential for deterioration over time.
- "OATS vs. ACI": Comparative studies demonstrate good results for both, with OATS being a single-stage procedure and ACI/MACI offering the potential for true hyaline-like cartilage regeneration, albeit with a two-stage approach.
- "Biologics": Research into the use of PRP (Platelet-Rich Plasma) and mesenchymal stem cells (MSCs) as adjuncts to cartilage repair or for early osteoarthritis is ongoing, with variable results and evolving guidelines.
Professional Society Guidelines:
- American Academy of Orthopaedic Surgeons (AAOS): Publishes Clinical Practice Guidelines (CPGs) for conditions like "Treatment of Osteoarthritis of the Knee," "Management of Anterior Cruciate Ligament Injuries," and "Meniscal Tear Treatment," providing evidence-based recommendations.
- European Society of Sports Traumatology, Knee Surgery & Arthroscopy (ESSKA): A leading European society, publishing consensus statements and recommendations on various knee pathologies and surgical techniques.
- International Society of Arthroscopy, Knee Surgery and Orthopaedic Sports Medicine (ISAKOS): An international forum fostering education and research, often setting global standards in arthroscopic and sports medicine practices.
Current Controversies & Future Directions:
- Biologic Augmentation: The role of PRP, bone marrow aspirate concentrate (BMAC), and adipose-derived stem cells in enhancing healing for meniscal repair, cartilage repair, and ACL reconstruction remains an active area of research.
- Personalized Medicine: Tailoring surgical and rehabilitation strategies based on individual patient biomechanics, genetics, and activity demands.
- Robotics and Navigation: Integration of robotic assistance and navigated systems to enhance precision in tunnel placement for ligament reconstruction and graft implantation.
- Artificial Intelligence (AI): Potential applications in preoperative planning, intraoperative guidance, and prediction of patient outcomes.
- Prevention of Post-Traumatic Osteoarthritis (PTOA): Focus on early diagnosis, optimal treatment of acute injuries, and adjunctive therapies to mitigate the long-term risk of OA after intra-articular injuries.
The practice of knee arthroscopy continues to evolve, emphasizing minimally invasive techniques, tissue preservation, and comprehensive rehabilitation, all guided by a robust and expanding body of scientific evidence.
You Might Also Like