Knee Arthroscopy: Advanced Epidemiology, Anatomy & Biomechanics Guide
Key Takeaway
Knee arthroscopy is a minimally invasive surgical technique for diagnosing and treating intra-articular knee pathologies like meniscal tears and ACL ruptures. It offers reduced invasiveness and faster recovery. Key anatomical understanding involves the femur, tibia, patella, cruciate and collateral ligaments, menisci (medial/lateral, vascularity), articular cartilage, and critical neurovascular structures for safe, effective intervention.
Introduction & Epidemiology
Knee arthroscopy, a minimally invasive surgical technique, has revolutionized the diagnosis and treatment of intra-articular knee pathologies since its conceptualization in the early 20th century and widespread adoption in the latter half. Initially a diagnostic tool, advancements in instrumentation, imaging, and surgical techniques have expanded its role to encompass a broad spectrum of therapeutic interventions. The primary advantages include reduced invasiveness, accelerated recovery, diminished post-operative pain, and decreased morbidity compared to traditional open arthrotomy.
Epidemiologically, knee arthroscopy is among the most frequently performed orthopedic procedures globally. The incidence of knee pathologies amenable to arthroscopic management, such as meniscal tears, anterior cruciate ligament (ACL) ruptures, and chondral lesions, is substantial across various age groups. Meniscal injuries are particularly prevalent, with an estimated incidence ranging from 60 to 70 per 100,000 population per year. ACL injuries, predominantly occurring in athletes, demonstrate an incidence of approximately 30 per 100,000, with higher rates in specific sports and demographics. Articular cartilage lesions are also common, with detection rates exceeding 60% in diagnostic arthroscopies. The aging demographic, coupled with an increased participation in recreational and competitive sports, continues to drive the demand for arthroscopic knee interventions. Understanding the evolving landscape of these pathologies and their management is crucial for contemporary orthopedic practice.
Surgical Anatomy & Biomechanics
A comprehensive understanding of knee joint anatomy and biomechanics is fundamental for safe and effective arthroscopic surgery.
Bony Anatomy
The knee joint comprises the distal femur, proximal tibia, and patella.
*
Femur
: The distal femur presents with medial and lateral condyles separated by the intercondylar notch. The condyles articulate with the tibial plateaus and form the trochlear groove for patellar articulation.
*
Tibia
: The proximal tibia features medial and lateral condyles, forming the tibial plateaus, which are relatively flat or slightly concave. The intercondylar eminences (medial and lateral tibial spines) are critical landmarks for ACL insertion and meniscal root attachments.
*
Patella
: The patella, a sesamoid bone, articulates with the femoral trochlea. Its articular surface is divided by a median ridge into larger lateral and smaller medial facets.
Ligamentous Structures
The major ligaments provide static stability to the knee.
*
Cruciate Ligaments
:
*
Anterior Cruciate Ligament (ACL)
: Originates from the posteromedial aspect of the lateral femoral condyle and inserts into the anterior intercondylar area of the tibia, anterior and lateral to the medial tibial spine. It resists anterior tibial translation and internal rotation. Its two main bundles are the anteromedial (taut in flexion) and posterolateral (taut in extension).
*
Posterior Cruciate Ligament (PCL)
: Originates from the anterolateral aspect of the medial femoral condyle and inserts into the posterior intercondylar area of the tibia. It resists posterior tibial translation.
*
Collateral Ligaments
:
*
Medial Collateral Ligament (MCL)
: Composed of superficial and deep layers. The superficial layer originates from the medial femoral epicondyle and inserts distal to the joint line on the tibia. The deep layer is a thickening of the joint capsule, intimately associated with the medial meniscus. Resists valgus stress.
*
Lateral Collateral Ligament (LCL)
: A cord-like structure originating from the lateral femoral epicondyle and inserting onto the fibular head. It resists varus stress and is extracapsular.
Menisci
The menisci are C-shaped fibrocartilaginous structures that enhance joint congruity, distribute load, absorb shock, and provide secondary stabilization.
*
Medial Meniscus
: Larger, C-shaped, and less mobile. Its anterior horn attaches near the ACL insertion, and the posterior horn attaches distal to the medial tibial spine. It has capsular attachments to the deep MCL.
*
Lateral Meniscus
: Smaller, more circular (O-shaped), and highly mobile. Its anterior horn attaches anterior to the lateral tibial spine, and the posterior horn attaches posterior to the lateral tibial spine. It is not directly attached to the LCL but can be connected to the femur via the meniscofemoral ligaments (Wrisberg and Humphry).
*
Vascularity
: The peripheral 10-30% of the menisci (red-red zone) is vascularized by the genicular arteries, enabling healing. The central avascular region (white-white zone) has limited healing potential. The transition zone is the red-white zone.
Articular Cartilage
Hyaline cartilage covers the ends of the femur, tibia, and patella, providing a low-friction articulating surface. Cartilage thickness varies across the joint, with the thickest portions typically on the patella and femoral condyles.
Synovial Folds and Fat Pads
- Synovial Plicae : Embryological remnants of synovial septa, the most common being the suprapatellar, mediopatellar, infrapatellar, and lateral plica. A symptomatic mediopatellar plica can mimic meniscal pathology.
- Hoffa's Fat Pad : The infrapatellar fat pad, richly innervated and vascularized, lies anterior to the ACL and posterior to the patellar tendon. Impingement or inflammation can cause anterior knee pain.
Neurovascular Structures
Crucial for safe portal placement. The popliteal artery and its branches, along with the tibial, common peroneal, and saphenous nerves, are vulnerable to iatrogenic injury.
*
Tibial nerve and popliteal artery
: Posterior to the knee joint.
*
Common peroneal nerve
: Winds around the fibular neck.
*
Saphenous nerve and artery
: Medial knee.
Biomechanics
- Kinematics : The knee exhibits complex tibiofemoral kinematics involving rolling, sliding, and rotation (screw-home mechanism).
- Stability : Provided by passive restraints (ligaments, capsule, menisci) and dynamic stabilizers (muscles like quadriceps, hamstrings, gastrocnemius).
- Load Bearing : Menisci distribute axial loads, reducing peak stress on articular cartilage. A meniscectomy significantly increases contact pressures and accelerates degenerative changes.
- ACL Function : Primary restraint to anterior tibial translation, secondary restraint to internal and external rotation.
- PCL Function : Primary restraint to posterior tibial translation.
Indications & Contraindications
Knee arthroscopy offers both diagnostic and therapeutic capabilities. Patient selection is paramount for optimal outcomes.
Indications for Knee Arthroscopy (Operative)
The following conditions are commonly addressed arthroscopically:
-
Meniscal Pathology
:
- Symptomatic Tears : Mechanical symptoms (locking, catching, clicking), pain, effusion.
- Specific Tear Patterns : Longitudinal, radial, horizontal, flap, bucket-handle tears that are unstable or cause mechanical symptoms.
- Repairable Tears : Tears located in the vascularized red-red or red-white zones, or those amenable to stable fixation.
-
Ligamentous Instability
:
- ACL Rupture : Symptomatic instability (giving way) in active individuals, often requiring reconstruction.
- PCL Rupture : Chronic symptomatic posterior instability (less frequently isolated arthroscopic treatment, often open or combined).
- Multi-ligamentous Knee Injuries : Arthroscopic assistance for ligament reconstruction.
-
Articular Cartilage Lesions
:
- Chondral and Osteochondral Defects : Focal lesions causing pain or mechanical symptoms, amenable to debridement, microfracture, autologous chondrocyte implantation (ACI), osteochondral autograft transplantation (OATS), or allograft.
- Osteochondritis Dissecans (OCD) : Stable lesions may be drilled; unstable or displaced lesions require fixation or grafting.
- Loose Bodies : Intra-articular fragments (cartilaginous, osteochondral, fibrous) causing pain, locking, or effusion.
-
Synovial Disorders
:
- Synovitis : Chronic inflammation not responsive to conservative management (e.g., in inflammatory arthritis, pigmented villonodular synovitis - PVNS).
- Synovial Plica Syndrome : Symptomatic, hypertrophic plica causing pain or mechanical symptoms unresponsive to conservative care.
-
Patellofemoral Disorders
:
- Patellar Instability : Lateral retinacular release for severe lateral patellar compression syndrome or as part of patellar stabilization procedures.
- Chondromalacia Patellae : Debridement for symptomatic fissuring or softening (controversial as isolated procedure).
-
Infection
:
- Septic Arthritis : Diagnostic aspiration, arthroscopic irrigation, and debridement to remove purulence and necrotic tissue.
-
Other
:
- Diagnostic Arthroscopy : For unexplained knee pain, effusion, or mechanical symptoms where non-invasive imaging is equivocal.
- Arthrofibrosis : Debridement of scar tissue limiting range of motion.
- Tibial Spine Avulsion Fractures : Arthroscopic reduction and fixation.
Contraindications for Knee Arthroscopy
-
Absolute Contraindications
:
- Active Local or Systemic Infection : Unless the primary indication is for the treatment of septic arthritis, performing elective arthroscopy in the presence of active infection carries a high risk of spreading infection.
- Severe Uncorrectable Coagulopathy : Uncontrolled bleeding diathesis significantly increases the risk of hemarthrosis and surgical complications.
-
Relative Contraindications
:
- Severe Degenerative Arthritis (Osteoarthritis) : While not an absolute contraindication, arthroscopy for isolated degenerative changes without mechanical symptoms (e.g., meniscal tears) is generally not recommended, especially in older patients, due to poor outcomes in several randomized controlled trials. Exceptions include loose body removal or debridement for acute mechanical symptoms.
- Marked Joint Stiffness/Ankylosis : May impede adequate visualization and instrument manipulation.
- Morbid Obesity : Technically challenging, increased risk of complications (e.g., DVT, infection, fluid extravasation).
- Severe Vascular Disease/Peripheral Neuropathy : Increased risk of complications related to tourniquet use or positioning.
- Poor Medical Status : Patients with significant comorbidities (e.g., uncontrolled diabetes, severe cardiovascular or pulmonary disease) may have increased anesthetic and surgical risks.
- Severe Skin Conditions at Surgical Site : Psoriasis, eczema, or active dermatologic infections could increase infection risk.
TABLE: Operative vs. Non-Operative Indications
| Condition | Operative Indication (Arthroscopy Recommended) | Non-Operative Indication (Conservative Management Preferred) |
|---|---|---|
| Meniscal Tears | Symptomatic, unstable tears (e.g., bucket-handle, radial, vertical tears causing locking/catching), peripheral tears in vascular zone with repair potential. | Asymptomatic tears, stable degenerative tears (especially in older patients without mechanical symptoms, often managed with physical therapy, activity modification, NSAIDs), small stable peripheral tears without mechanical symptoms, tears in avascular zone unlikely to heal spontaneously. |
| ACL Rupture | Symptomatic instability in active individuals, young athletes, recurrent giving way affecting activities of daily living. | Asymptomatic tears in low-demand individuals, partial tears without instability, patients unwilling/unable to participate in rehabilitation, those preferring non-surgical functional rehabilitation (though long-term outcomes for activity levels may differ). |
| Articular Cartilage Lesions | Focal, symptomatic chondral/osteochondral defects, unstable OCD lesions, loose bodies. | Asymptomatic chondral lesions, diffuse degenerative chondromalacia without specific mechanical symptoms (often managed with activity modification, weight loss, physical therapy, injections), mild stable OCD lesions. |
| Patellofemoral Pain Syndrome | Severe lateral patellar compression syndrome (lateral release, rare as isolated procedure), specific mechanical issues like plica impingement. | Most cases of anterior knee pain, patellofemoral pain syndrome, mild chondromalacia patellae (managed with physical therapy, quadriceps strengthening, bracing, activity modification, NSAIDs, injections). |
| Synovitis | Chronic, severe synovitis unresponsive to conservative treatment (e.g., PVNS, rheumatoid arthritis). | Acute synovitis responsive to rest, NSAIDs, or injections; mild inflammatory conditions. |
| Diagnostic Arthroscopy | Unexplained persistent knee pain, effusion, or mechanical symptoms with equivocal non-invasive imaging. | Clear diagnosis via history, physical exam, and imaging; symptoms resolving with conservative management. |
| Knee Osteoarthritis (Degenerative) | Isolated symptomatic meniscal tear with mechanical symptoms in an otherwise osteoarthritic knee, loose bodies causing locking. | Primary treatment for diffuse degenerative osteoarthritis (arthroscopy has shown no benefit over sham surgery for OA symptoms), especially in the absence of acute mechanical symptoms or specific structural pathologies amenable to repair. Focus on non-operative measures: physical therapy, weight loss, NSAIDs, injections, eventually arthroplasty for end-stage disease. |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning and appropriate patient positioning are critical for successful arthroscopic knee surgery, minimizing complications and optimizing surgical access.
Pre-Operative Planning
-
Patient Assessment
:
- Comprehensive History : Detail duration, character, aggravating/alleviating factors of symptoms; previous injuries or surgeries; medical comorbidities; medication list (especially anticoagulants); social history (smoking, alcohol, occupational demands, activity level).
- Physical Examination : Thorough assessment of knee ROM, stability (ligamentous testing), effusion, crepitus, patellofemoral tracking, and neurovascular status. Document baseline deficits.
-
Imaging Review
:
- Plain Radiographs : Weight-bearing AP, lateral, patellofemoral (Merchant or sunrise) views are essential to assess joint space narrowing, osteophyte formation, patellar tilt, and bony alignment.
- MRI : Gold standard for soft tissue evaluation (menisci, ligaments, cartilage, bone marrow edema). Crucial for surgical decision-making.
- CT Scan : Indicated for complex fractures, alignment assessment (e.g., torsional deformities, patellar trochlear dysplasia).
-
Surgical Planning
:
- Procedure Selection : Based on clinical findings and imaging, decide on the specific arthroscopic intervention (e.g., partial meniscectomy, meniscal repair, ACL reconstruction, chondroplasty).
- Equipment Preparation : Ensure all necessary instruments, implants (if applicable), and arthroscopy tower components are available and functional.
- Anesthesia Consultation : Assess patient fitness for general or regional anesthesia (spinal/epidural blocks often favored for post-operative analgesia).
- Patient Education and Consent : Discuss the nature of the procedure, anticipated outcomes, potential risks, and post-operative expectations, including rehabilitation. Obtain informed consent.
-
Prophylaxis
:
- Antibiotic Prophylaxis : Administer intravenous prophylactic antibiotics (e.g., cefazolin) within 60 minutes prior to incision, per institutional guidelines, to reduce the risk of surgical site infection.
- Venous Thromboembolism (VTE) Prophylaxis : Assess individual patient risk factors for DVT/PE. Consider mechanical prophylaxis (compression stockings, intermittent pneumatic compression devices). Pharmacological prophylaxis may be indicated for high-risk patients undergoing major reconstructive procedures (e.g., ACL reconstruction) or those with previous VTE history.
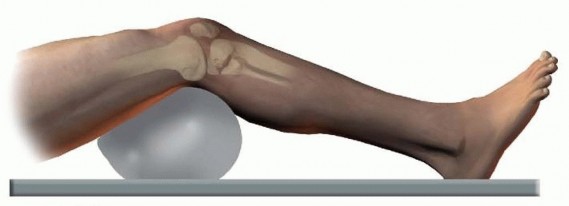
Patient Positioning
The most common position for knee arthroscopy is supine.
1.
Operating Table Setup
:
* Standard operating table with a foot extension or specific knee arthroscopy table attachment.
*
Tourniquet
: Applied high on the proximal thigh. While not universally required for all arthroscopic cases, a tourniquet offers a bloodless field, which is particularly advantageous for complex procedures or those requiring precise visualization (e.g., meniscal repair, ACL reconstruction). Inflation pressure typically 250-300 mmHg or 100 mmHg above systolic blood pressure. Inflation time must be carefully monitored.
*
Leg Holder
: A well-padded leg holder is typically placed on the contralateral leg, allowing the operative leg to be free-draped. Alternatively, a lateral post can be used for the operative leg, or a traction device if distraction is needed.
2.
Operative Leg Positioning
:
* The operative leg is draped free. This allows dynamic manipulation of the knee joint through various degrees of flexion, extension, valgus, and varus stress, which is essential for comprehensive visualization and instrument access to all compartments.
*
Foot Traction Device
: For procedures requiring joint distraction, such as some meniscal repairs or chondral procedures, a non-invasive foot holder with adjustable traction may be utilized. This helps open up the joint space, especially the lateral compartment.
*
Padding
: Meticulous padding of all pressure points, especially the fibular head (to protect the common peroneal nerve) and heels, is crucial to prevent nerve palsies or pressure sores.
3.
Surgeon and Assistant Positioning
:
* Surgeon typically stands on the ipsilateral side of the operative knee, with the assistant on the contralateral side. The arthroscopy monitor is placed in direct line of sight for all team members.
4.
Sterile Preparation and Draping
:
* The entire lower extremity, from the tourniquet to the toes, is prepped with an antiseptic solution (e.g., chlorhexidine-alcohol or povidone-iodine).
* The leg is then sterilely draped, ensuring a wide operative field and the ability to manipulate the limb freely. An impervious stockinette may be applied over the foot and ankle.
Detailed Surgical Approach / Technique
Knee arthroscopy encompasses a systematic approach to diagnosis and treatment. While specific steps vary based on the pathology, the foundational principles remain consistent.
General Principles
- Fluid Management : Sterile saline is the most common irrigation fluid. An arthroscopy pump maintains constant intra-articular pressure (typically 40-80 mmHg) for optimal joint distension and clear visualization, while also flushing debris. Inflow is usually via the viewing portal or a dedicated inflow portal; outflow is through a working portal or separate outflow cannula. Careful monitoring of fluid input and output is crucial to prevent extravasation or compartment syndrome.
- Visualization : A 30-degree arthroscope is standard, providing a wide field of view. A 70-degree scope may be used for specific areas (e.g., posterior horn of medial meniscus, posterior compartments).
- Instrumentation : A variety of specialized instruments are used, including cannulas, trocars, blunt probes, grasping forceps, punches, basket forceps, shavers, motorized burrs, suture passers, and various reconstructive tools.
Portal Placement
Accurate and safe portal placement is paramount. Standard portals are generally placed 1 cm lateral to the patellar tendon and 1 cm proximal to the joint line. Neurovascular structures, particularly the common peroneal nerve laterally and saphenous nerve/vessels medially, must be avoided.
1.
Anterolateral Portal (ALP)
:
*
Location
: Typically 1 cm lateral to the lateral border of the patellar tendon, at or slightly above the joint line.
*
Purpose
: Primary viewing portal for diagnostic arthroscopy and often for working in the medial and intercondylar compartments.
2.
Anteromedial Portal (AMP)
:
*
Location
: Typically 1 cm medial to the medial border of the patellar tendon, at or slightly above the joint line.
*
Purpose
: Primary working portal for instruments, excellent for accessing the medial compartment, intercondylar notch, and often used as an inflow portal.
3.
Superolateral Portal (SLP)
:
*
Location
: Superior and lateral to the patella, approximately 2-3 cm proximal to the patella's superolateral corner.
*
Purpose
: Primarily for outflow, aiding in fluid dynamics and improving visualization by removing debris and extravasated fluid. Can also be used for accessory viewing or instrument access to the suprapatellar pouch.
4.
Posteromedial Portal (PMP)
:
*
Location
: Posterior to the MCL, anterior to the semimembranosus tendon, at the level of the joint line. Requires careful palpation to avoid the saphenous nerve and artery.
*
Purpose
: Access to the posterior horn of the medial meniscus, posterior capsule, and loose bodies in the posterior compartment. Can be used for accessory viewing or working during posterior meniscal repair.
5.
Posterolateral Portal (PLP)
:
*
Location
: Posterior to the LCL, anterior to the biceps femoris tendon, at the level of the joint line. Requires extreme caution to avoid the common peroneal nerve and popliteal neurovascular bundle.
*
Purpose
: Access to the posterior horn of the lateral meniscus, posterior capsule, and loose bodies. Less commonly used due to higher neurovascular risk.
Diagnostic Arthroscopy (Systematic Examination)
A standardized approach ensures all intra-articular structures are thoroughly inspected.
1.
Suprapatellar Pouch
: Evaluate patellar tracking, trochlear groove, and patellar articular cartilage. Assess for synovitis, plicae, loose bodies.
2.
Medial Gutter
: Inspect the medial patellofemoral ligament and synovium.
3.
Medial Compartment
:
*
Medial Meniscus
: Probe anterior horn, body, and posterior horn. Assess integrity, stability, vascularity (if repair considered).
*
Medial Femoral Condyle & Tibial Plateau
: Evaluate articular cartilage.
4.
Intercondylar Notch
:
*
ACL
: Assess fiber integrity, tension, and any concomitant injury (e.g., cyclops lesion).
*
PCL
: Assess fiber integrity, tension.
*
Intercondylar Notch Walls
: Look for osteophytes, impinging lesions, and meniscofemoral ligaments (if present).
*
Loose Bodies
: Systematically search the entire notch.
5.
Lateral Compartment
:
*
Lateral Meniscus
: Probe anterior horn, body, and posterior horn. Assess stability, tears, and vascularity. Often requires a figure-of-four position and valgus stress to open.
*
Lateral Femoral Condyle & Tibial Plateau
: Evaluate articular cartilage.
6.
Lateral Gutter
: Inspect synovium, popliteus tendon sheath.
7.
Posterior Compartments
: If indicated, use the PMP or PLP, or trans-notch visualization from standard portals, to assess posterior structures.
Common Therapeutic Procedures (Principles)
-
Meniscectomy (Partial)
:
- Principle : Resect only the unstable, symptomatic, or torn portion of the meniscus, preserving as much healthy meniscal tissue as possible to maintain function and prevent early degenerative changes.
- Technique : Using specialized basket forceps, punches, and shavers, the torn fragment is excised, and the remaining rim is contoured smoothly.
-
Meniscal Repair
:
- Principle : Reapproximate and stabilize torn meniscal tissue, aiming for biological healing. Primarily indicated for acute tears in the vascular red-red or red-white zones, especially in younger, active patients.
-
Technique
: Multiple techniques exist:
- Inside-Out : Suture passers deployed from inside the joint, exited through the capsule, and tied over the capsule after mini-arthrotomy.
- Outside-In : Needles passed from outside the joint, through the capsule and meniscus, retrieved with suture lasso from inside.
- All-Inside : Specialized devices deployed entirely within the joint, anchoring the torn meniscus to the capsule without external incision.
- Often requires capsular rasping or trephination to promote blood flow.
-
ACL Reconstruction
:
- Principle : Recreate the functional anatomy of the ACL using a graft, restoring rotational and translational stability.
- Graft Choices : Autografts (bone-patellar tendon-bone (BPTB), hamstring (semitendinosus/gracilis), quadriceps tendon) or allografts.
-
Technique
:
- Tunnel Placement : Femoral and tibial tunnels are drilled with precise anatomical locations. Isometric placement is crucial. The femoral tunnel is typically created via a transtibial, anteromedial portal, or outside-in technique.
- Graft Passage : The prepared graft is passed through the tunnels.
- Fixation : Various methods used (interference screws, suspensory fixation devices like EndoButton, staples, posts). Fixation depends on graft type and surgeon preference.
-
Chondroplasty/Microfracture
:
- Chondroplasty : Debridement of unstable or fibrillated articular cartilage to create a stable edge and remove loose fragments. Primarily for pain relief, not true cartilage regeneration.
- Microfracture : For contained full-thickness chondral defects (typically <2-4 cm²). Small holes are created in the subchondral bone, allowing bone marrow stem cells and growth factors to fill the defect and form fibrocartilage. Requires strict non-weight-bearing post-operatively.
-
Loose Body Removal
:
- Principle : Systematically locate and retrieve all intra-articular loose bodies.
- Technique : A systematic search of all compartments and gutters is performed. Grasping forceps or suction devices are used for retrieval.
-
Synovectomy
:
- Principle : Excision of inflamed or hypertrophic synovial tissue.
- Technique : Motorized shavers are used to resect synovial tissue, maintaining careful hemostasis.
Complications & Management
While knee arthroscopy is generally safe, complications can occur. Recognition and appropriate management are crucial for optimal patient outcomes.
General Complications
-
Deep Vein Thrombosis (DVT) / Pulmonary Embolism (PE)
: Incidence is low for routine arthroscopy but increases with prolonged immobilization, complex reconstructions, and patient risk factors (e.g., hypercoagulable states, obesity, oral contraceptives, previous DVT).
- Management : Prophylaxis (mechanical/pharmacological), early mobilization. Treatment involves anticoagulation.
-
Infection (Septic Arthritis)
: Incidence 0.01% - 0.5%. Can lead to rapid cartilage destruction if not promptly treated.
- Management : Urgent arthroscopic irrigation and debridement, synovial biopsy for culture, broad-spectrum intravenous antibiotics tailored to culture results.
-
Neurovascular Injury
: Rare, but potentially devastating.
- Nerve Injury : Most common: saphenous nerve (medial portal), common peroneal nerve (lateral portal, tourniquet), infrapatellar branch of saphenous nerve (portal incision). Incidence 0.2-2%. Typically sensory, rarely motor.
- Vascular Injury : Popliteal artery/vein are most at risk during posterior portal placement or aggressive instrumentation, especially in tight joints or those with osteophytes. Incidence <0.01%.
- Management : Prevention is key (careful portal placement, blunt dissection). Nerve injuries often resolve spontaneously. Vascular injuries require urgent vascular surgery consultation for repair.
-
Complex Regional Pain Syndrome (CRPS)
: Rare, characterized by chronic pain, allodynia, hyperalgesia, swelling, and trophic changes.
- Management : Early recognition, physical therapy, nerve blocks, medications (gabapentin, tricyclic antidepressants), pain management specialist referral.
-
Arthrofibrosis
: Excessive intra-articular scarring leading to restricted range of motion. More common after ACL reconstruction or extensive debridement.
- Management : Aggressive physical therapy, manipulation under anesthesia, arthroscopic lysis of adhesions (LOA).
Specific Complications and Management
| Complication | Incidence | Description | Salvage Strategy / Management |
|---|---|---|---|
| Iatrogenic Chondral Injury | 1-5% | Damage to articular cartilage from instruments, scope, or malpositioned portals. | Prevention (careful technique, adequate joint distension). If mild, observation. If significant, microfracture, debridement, or consideration for future cartilage restoration procedures. |
| Hemarthrosis | 1-5% | Post-operative bleeding into the joint, causing pain, swelling, and stiffness. More common after extensive synovectomy or ACL reconstruction. | Prevention (good hemostasis, judicious tourniquet use). Management: Aspiration, compression, rest, RICE. Repeat arthroscopy for persistent bleeding or hemarthrosis under tension. |
| Fluid Extravasation / Compartment Syndrome | <1% (rare for compartment syndrome) | Leakage of irrigation fluid into soft tissues. If severe, can cause compartment syndrome (extremely rare in knee). | Prevention (monitor fluid balance, limit pump pressure, judicious use of epinephrine in fluid). Management: Stop fluid, observe. If compartment syndrome suspected (pain out of proportion, pallor, paresthesias, pulselessness), emergent fasciotomy. |
| Portal Site Complications | 1-3% | Nerve injury (sensory branches), persistent drainage, scar hypertrophy, painful neuromas. | Prevention (careful incision, blunt dissection). Management: Most nerve injuries resolve spontaneously. Neuromas may require excision. Infection managed with antibiotics, drainage. |
| Persistent Pain | Variable (up to 20%) | Pain persisting after arthroscopy, often due to underlying pathology, incomplete treatment, or development of new issues. | Thorough diagnostic workup (re-evaluate original diagnosis, look for new pathology, consider CRPS). Revision surgery if treatable cause identified (e.g., missed meniscal tear, arthrofibrosis, hardware impingement). Pain management referral. |
| Recurrent Instability (Post-ACL Recon) | 5-10% (graft failure) | Re-rupture of the ACL graft, or persistent instability due to technical errors, inadequate rehabilitation, or new trauma. | Prevention (correct tunnel placement, appropriate graft tension, adherence to rehab protocol). Management: Revision ACL reconstruction, often with different graft choice, tunnel reaming/bone grafting if tunnels are expanded. |
| Graft Impingement / Cyclops Lesion (Post-ACL Recon) | 1-5% | Graft impingement by femoral notch (anterior placement) or tibial spine, leading to extension block. Cyclops lesion is a fibroproliferative nodule in the notch. | Prevention (correct tunnel placement, notchplasty if indicated). Management: Arthroscopic debridement of impingement or cyclops lesion. |
| Incomplete Healing / Failure of Meniscal Repair | 15-30% | Failure of repaired meniscus to heal, often due to poor vascularity, tear characteristics, or inadequate fixation. | Management: Observation for asymptomatic tears. If symptomatic, partial meniscectomy of the unhealed portion or revision repair if criteria are met. |
| Iatrogenic Ligament Injury | <0.1% | Accidental injury to collateral or cruciate ligaments during instrumentation or portal creation. | Prevention (careful technique). Management: Depending on severity, may require repair or reconstruction. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is an integral component of successful knee arthroscopy, aiming to restore strength, range of motion (ROM), proprioception, and functional ability while protecting healing tissues. Protocols are procedure-specific and tailored to individual patient needs and goals.
General Principles
- RICE : Rest, Ice, Compression, Elevation for pain and edema control, especially in the immediate post-operative period.
- Pain Management : Multi-modal analgesia (NSAIDs, acetaminophen, opioids) to facilitate early mobilization.
- Early Mobilization : Unless contraindicated by the procedure (e.g., chondral repair, meniscal repair), early, protected ROM and weight-bearing are encouraged to prevent stiffness and improve circulation.
- Protection of Healing Structures : Crucial for procedures involving tissue repair (meniscus, ligaments, cartilage). This often dictates weight-bearing restrictions, brace use, and ROM limitations.
- Progressive Loading : Gradual increase in weight-bearing, resistance, and activity to allow tissue adaptation and prevent re-injury.
- Patient Education : Clear instructions regarding activity restrictions, exercises, warning signs, and expected timeline for recovery.
Procedure-Specific Rehabilitation Protocols
1. Diagnostic Arthroscopy / Simple Partial Meniscectomy
- Goals : Restore full ROM and strength, return to normal activities quickly.
-
Phase I (0-2 weeks)
:
- Weight-Bearing (WB) : Full WB as tolerated with crutches initially for comfort, progressing to unassisted ambulation.
- ROM : Full ROM encouraged, active and passive exercises within pain limits.
- Exercises : Quad sets, straight leg raises (SLR) in multiple planes, ankle pumps, hamstring curls, gentle knee flexion/extension.
- Pain/Edema : RICE, analgesics.
-
Phase II (2-4 weeks)
:
- WB : Full WB without aids.
- Exercises : Progress strengthening (light resistance, cycling, elliptical), proprioceptive exercises (single leg balance).
- Return to Activity : Low-impact activities (swimming, cycling) introduced gradually.
- Return to Sport : Typically 4-6 weeks for light sport, 6-8 weeks for cutting/pivoting sports, depending on individual recovery and pre-injury activity level.
2. Meniscal Repair
- Goals : Protect the healing repair, restore ROM, strength, and proprioception.
-
Phase I (0-6 weeks - Protection Phase)
:
- WB : Typically non-weight-bearing (NWB) or touch-down weight-bearing (TDWB) with crutches for 4-6 weeks to allow initial healing.
- Brace : Hinged knee brace locked in extension for ambulation, unlocking for controlled ROM.
- ROM : Restricted, usually 0-90° flexion for the first 4-6 weeks, avoiding deep squats or twisting. Avoid hamstring activation in initial weeks, depending on tear location and repair type.
- Exercises : Quad sets, gentle SLR, ankle pumps. Isometrics within allowed ROM.
-
Phase II (6-12 weeks - Intermediate Strengthening)
:
- WB : Progress to partial WB, then full WB. Discontinue crutches as tolerated.
- Brace : May transition to functional brace or discontinue depending on surgeon preference and stability.
- ROM : Gradually increase flexion beyond 90°.
- Exercises : Progressive resistive exercises (PREs), stationary cycling, elliptical. Proprioception drills.
-
Phase III (12-24 weeks - Advanced Strengthening & Return to Activity)
:
- WB : Full WB.
- Exercises : Introduce sport-specific drills, plyometrics, agility training. Continue strengthening.
- Return to Sport : Highly variable, 4-6 months, guided by functional testing and physician clearance. Requires excellent strength, full ROM, and no pain/effusion.
3. ACL Reconstruction
- Goals : Protect graft, restore ROM, strength, proprioception, and return to sport. Typically divided into 4 phases.
-
Phase I (0-6 weeks - Protection and Early Motion)
:
- WB : Initially TDWB with crutches, progressing to full WB by 2-4 weeks, depending on surgeon preference and concomitant injuries.
- Brace : Hinged knee brace with ROM control (e.g., 0-90° for first 2-4 weeks, then 0-120°). May be locked in extension for ambulation initially.
- ROM : Immediate passive extension to 0° is critical to prevent arthrofibrosis. Flexion progressed gradually (e.g., 90° by week 2, 120° by week 4).
- Exercises : Quad sets, patellar mobilizations, SLR, gentle hamstring curls (if BPTB graft used), calf raises. Neuromuscular electrical stimulation (NMES) for quad activation.
-
Phase II (6-12 weeks - Intermediate Strengthening)
:
- WB : Full WB without crutches. Brace may be discontinued for ADLs, used for activity.
- ROM : Full ROM should be achieved.
- Exercises : Progressive strengthening (closed chain exercises: wall squats, leg press, step-ups; open chain: knee extension 90-45°, hamstring curls). Stationary cycling, elliptical. Proprioception drills.
-
Phase III (3-6 months - Advanced Strengthening & Sport-Specific Training)
:
- Exercises : Agility drills, plyometrics, sport-specific exercises (running, cutting, jumping). Continue strengthening.
- Functional Testing : Isokinetic testing, hop tests to assess strength and power imbalances.
-
Phase IV (6-12+ months - Return to Sport)
:
- Criteria for Return to Sport : Full pain-free ROM, no effusion, quadriceps/hamstring strength ≥90% of contralateral limb, successful completion of sport-specific functional testing, psychological readiness.
- Brace : Use of functional brace upon return to sport is controversial and often physician/patient preference.
- Return to Sport : Highly individualized, typically 9-12 months for cutting/pivoting sports, sometimes longer for high-level athletes. Early return significantly increases re-injury risk.
4. Chondral Procedures (Microfracture, OATS, ACI)
- Goals : Protect the healing cartilage repair, minimize stress on the defect, restore ROM and strength.
-
Phase I (0-6 weeks - Strict Protection)
:
- WB : Strict NWB with crutches.
- Brace : Hinged knee brace locked in extension, often continuous use.
- ROM : Controlled passive motion (CPM machine often prescribed). Specific ROM limits may apply based on lesion location (e.g., avoid deep flexion for patellar lesions).
- Exercises : Quad sets, SLR, patellar mobilizations, ankle pumps.
-
Phase II (6-12 weeks - Progressive Loading)
:
- WB : Gradual progression to TDWB, then PWB, under strict guidance.
- Brace : May unlock for controlled ROM exercises.
- ROM : Gradually increase, maintaining protection.
- Exercises : Initiate gentle closed-chain strengthening. Non-impact aerobic activities.
-
Phase III (3-6 months - Moderate Activity)
:
- WB : Full WB without aids.
- Exercises : Progressive strengthening, low-impact functional activities.
- Return to Sport : Highly delayed, often 9-18 months, with careful assessment of healing and functional capacity. Impact activities are generally discouraged or delayed significantly.
Role of Physical Therapy
A structured and supervised physical therapy program is paramount for all rehabilitation protocols. Physical therapists guide patients through progressive exercises, monitor progress, address deficits, and ensure adherence to precautions, ultimately facilitating a safe and effective return to function.
Summary of Key Literature / Guidelines
Evidence-based practice forms the cornerstone of modern orthopedic surgery. A synthesis of key literature and adherence to established guidelines optimize clinical outcomes in knee arthroscopy.
Meniscal Pathology
-
Meniscectomy vs. Repair
:
- Meniscal Repair : Level I evidence (meta-analyses) supports meniscal repair over meniscectomy in eligible tears (e.g., peripheral, longitudinal tears in younger patients with intact peripheral rim) due to superior long-term outcomes, reduced risk of osteoarthritis, and preservation of knee function. However, repair has a higher re-operation rate for failed healing.
- Partial Meniscectomy : Indicated for symptomatic tears in the avascular zone or complex tears not amenable to repair. Studies consistently show good short-to-mid-term outcomes, but long-term data indicates an increased risk of degenerative changes.
- Degenerative Meniscal Tears (in OA) : Multiple randomized controlled trials (e.g., NEJM 2013 by Sihvonen et al., NEJM 2016 by Katz et al.) have demonstrated that arthroscopic partial meniscectomy (APM) for degenerative meniscal tears in patients with mild-to-moderate osteoarthritis provides no additional benefit over sham surgery or physical therapy regarding pain or function. This has led to strong recommendations against routine APM in this population, advocating for a trial of conservative management first.
Anterior Cruciate Ligament (ACL) Reconstruction
- Timing of Surgery : Delayed reconstruction (beyond 3 weeks) generally preferred to allow acute inflammation to subside and reduce the risk of arthrofibrosis.
-
Graft Choice
:
- Autografts : BPTB and hamstring autografts are the most common. Meta-analyses demonstrate comparable clinical outcomes in terms of stability and function. BPTB is often associated with a higher rate of anterior knee pain and kneeling pain, while hamstring autografts may have a higher rate of graft laxity and hamstring weakness.
- Allografts : Higher re-rupture rates in younger, active patients compared to autografts, particularly in primary reconstructions. May be considered for older, less active patients, revision surgery, or multi-ligamentous injuries.
-
Surgical Technique
:
- Anatomic Reconstruction : Emphasis on restoring the native ACL anatomy, including individualized femoral and tibial tunnel placement (anteromedial portal technique for femoral tunnel often preferred over transtibial technique for more anatomical placement).
- Double-Bundle vs. Single-Bundle : While theoretically superior for rotational stability, numerous Level I studies and meta-analyses have largely failed to demonstrate consistent clinically significant superiority of double-bundle over well-performed anatomic single-bundle reconstruction, and it carries increased technical difficulty and potential morbidity.
- Accelerated Rehabilitation : Evidence supports accelerated rehabilitation protocols focusing on early ROM and protected weight-bearing, which reduce stiffness and improve functional recovery without increasing graft laxity or re-rupture rates.
Articular Cartilage Repair
- Microfracture : A cost-effective, single-stage procedure for contained focal full-thickness chondral defects (<2-4 cm²). Level I evidence supports its use for specific indications, but the repair tissue is fibrocartilage, which is biomechanically inferior to hyaline cartilage, often leading to decline in outcomes over time, especially in larger lesions.
- Autologous Chondrocyte Implantation (ACI) : A two-stage procedure involving harvesting chondrocytes, culturing them, and then implanting them into the defect. Offers potential for hyaline-like cartilage repair. Indicated for larger lesions (often >2 cm²). Second and third-generation ACI techniques (e.g., matrix-associated ACI - MACI) simplify the procedure.
- Osteochondral Autograft Transplantation (OATS) / Mosaicplasty : Transfers cylinders of articular cartilage and subchondral bone from a less weight-bearing area to the defect. Single-stage. Indicated for smaller to medium-sized lesions.
- Osteochondral Allograft Transplantation : Uses cadaveric tissue. Indicated for larger defects, revision cases, or osteochondral defects with significant bone loss.
- Guidelines : Current consensus supports a stepped approach based on defect size, location, and patient age/activity level. No single technique is universally superior for all chondral defects.
Other Key Literature
- Septic Arthritis : Prompt recognition and aggressive management (arthroscopic lavage, debridement, antibiotics) are critical for preserving joint function. Delayed treatment significantly increases the risk of joint destruction.
- Arthrofibrosis Prevention : Early, aggressive range of motion, particularly extension, is paramount. Prevention is key, as treatment can be challenging.
- Complication Rates : Overall complication rates for knee arthroscopy are low (typically <5%), with DVT/PE, infection, and neurovascular injury being the most serious, albeit rare.
The field of knee arthroscopy continues to evolve with ongoing research into biological augmentation, advanced imaging, and robotic assistance. Staying abreast of high-quality evidence is essential for orthopedic surgeons to provide optimal care.
You Might Also Like