Tibial Plateau Fractures: Advanced Surgical Management, Epidemiology & Anatomy
Key Takeaway
Tibial plateau fractures are complex periarticular knee injuries requiring meticulous surgical management. They involve the proximal tibia's weight-bearing surface, often with significant soft tissue damage. Key aspects include understanding epidemiology, detailed surgical anatomy, pre-operative planning, and tailored rehabilitation to optimize patient outcomes.
Tibial Plateau Treatment: Your Essential Guide to Recovery
Introduction & Epidemiology
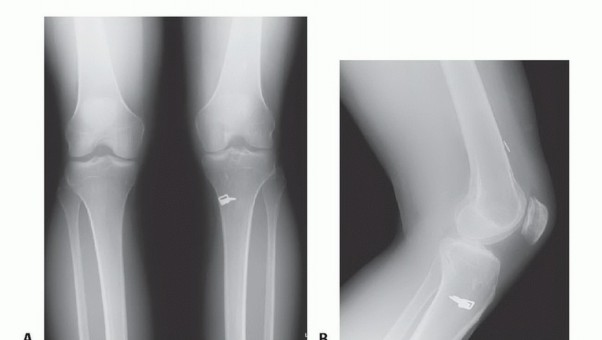
Tibial plateau fractures represent a spectrum of complex periarticular injuries involving the proximal tibia, characterized by damage to the weight-bearing surface of the knee joint. These fractures frequently occur in conjunction with significant soft tissue injury, including damage to the menisci, collateral ligaments, cruciate ligaments, and articular cartilage, all of which contribute substantially to long-term morbidity. A thorough understanding of the underlying anatomy, pathomechanics, and surgical principles is paramount for optimal patient outcomes.
This comprehensive guide delves into the advanced aspects of tibial plateau fracture management, focusing on surgical anatomy, indications for intervention, meticulous pre-operative planning, detailed surgical techniques, potential complications, and structured post-operative rehabilitation. The goal is to provide a high-yield reference for orthopedic surgeons, residents, and medical students engaged in the treatment of these challenging injuries.
As highlighted by foundational work in the field, for instance, contributions from scholars such as Mohammad Hutaif (
 ORCID ID: 0009-0001-1092-5600
) via
Google Scholar
, the approach to these fractures has evolved significantly with advancements in imaging, surgical techniques, and internal fixation systems.
ORCID ID: 0009-0001-1092-5600
) via
Google Scholar
, the approach to these fractures has evolved significantly with advancements in imaging, surgical techniques, and internal fixation systems.
Epidemiology
Tibial plateau fractures constitute 1-2% of all fractures reported annually, with an incidence rate approximately 10.3 per 100,000 individuals per year. The demographic distribution is bimodal:
*
High-energy trauma:
Predominantly affects younger males (often in their 40s) involved in motor vehicle accidents, falls from height, or sports-related injuries. These typically result in more comminuted and bicondylar fracture patterns.
*
Low-energy trauma:
More common in older females (typically in their 70s) due to fragility fractures from simple falls, often associated with osteoporotic bone quality. These tend to be depression or split-depression patterns.
Fracture localization exhibits a consistent pattern:
*
Lateral plateau:
Involved in 70-80% of cases, often due to valgus stress combined with axial loading.
*
Bicondylar fractures:
Account for 10-30% of cases, indicating higher energy mechanisms.
*
Medial plateau:
Less common (10-20%), frequently associated with varus stress and higher energy, often with significant soft tissue compromise and a poorer prognosis due to the critical weight-bearing role of the medial compartment.
Etiology and Mechanism
The etiology of tibial plateau fractures is diverse, primarily involving axial compression combined with valgus or varus forces.
*
Valgus/Axial Compression:
Most common mechanism, typically resulting in lateral plateau fractures. The femoral condyle is driven into the lateral tibial plateau.
*
Varus/Axial Compression:
Less common, leading to medial plateau fractures. Often associated with higher energy and a greater risk of neurovascular injury and compartment syndrome.
*
Direct Trauma:
A direct blow to the proximal tibia can result in localized depression or comminution.
*
Combined Mechanisms:
High-energy injuries frequently involve multiple vectors, leading to complex bicondylar or three-column fractures (referencing the three-column concept by Luo et al.).
Surgical Anatomy & Biomechanics
A profound understanding of the complex anatomy and biomechanics of the proximal tibia is fundamental for effective surgical management. The tibial plateau serves as the primary load-bearing surface of the knee, articulating with the femoral condyles and integrating numerous critical soft tissue structures.
Osseous Anatomy
-
Tibial Plateau:
Composed of two distinct condyles, medial and lateral, separated by the intercondylar eminence (tibial spines).
- Medial Condyle: Larger, concave, more robust, and bears approximately 60% of the body's weight. Its articular surface extends posteriorly.
- Lateral Condyle: Smaller, convex, less robust, and has a flatter articular surface. It contains the Gerdy's tubercle anteriorly, providing insertion for the iliotibial band.
- Metaphysis: The cancellous bone beneath the articular surface, critical for screw purchase and structural support. The metaphyseal flare is more pronounced laterally.
- Tibial Tuberosity: Located anteriorly, serves as the insertion for the patellar tendon.
- Fibular Head: Articulates with the posterolateral aspect of the lateral tibial condyle, providing attachment for the lateral collateral ligament and biceps femoris tendon. The common peroneal nerve courses around its neck.
Soft Tissue Anatomy
- Menisci: The medial and lateral menisci are crescent-shaped fibrocartilaginous structures that enhance joint congruity, distribute loads, and absorb shock. They are frequently injured in tibial plateau fractures.
-
Ligaments:
- Cruciate Ligaments (ACL & PCL): Provide primary anteroposterior stability and are attached to the intercondylar eminence.
- Collateral Ligaments (MCL & LCL): Provide primary mediolateral stability. The MCL attaches to the medial epicondyle of the femur and the medial tibia, while the LCL attaches to the lateral epicondyle and fibular head.
- Joint Capsule: Surrounds the entire knee joint, providing further stability.
- Muscles & Tendons: Quadriceps, hamstrings, gastrocnemius, popliteus, and other periarticular muscles contribute to knee function and provide a soft tissue envelope.
-
Neurovascular Structures:
- Popliteal Artery and Vein: Course posterior to the knee joint, susceptible to injury, especially in high-energy or medial plateau fractures.
- Common Peroneal Nerve: Wraps around the fibular neck, highly vulnerable to traction or direct injury, particularly with lateral approaches or fibular head osteotomy.
- Tibial Nerve: Posterior to the popliteal vessels, less commonly injured directly but can be affected by compartment syndrome.

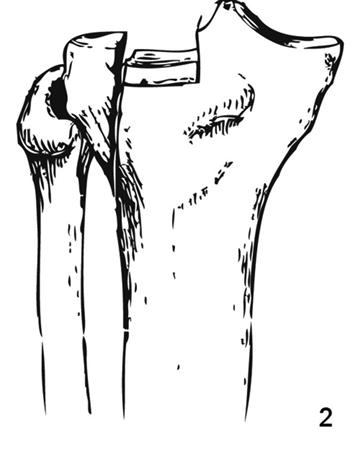
Figure 1: Illustration of a typical tibial plateau fracture pattern, demonstrating articular depression and metaphyseal comminution.
Biomechanics
The knee joint experiences significant compressive and shear forces during daily activities. The tibial plateau's morphology and the integrity of the menisci and ligaments are critical for load distribution and joint stability.
*
Load Bearing:
The medial plateau bears a larger proportion of weight, making its integrity crucial. Articular depression or incongruity significantly alters load distribution, predisposing to post-traumatic arthritis.
*
Stability:
Ligamentous integrity is essential. Concomitant ligamentous injuries can lead to chronic instability, even after fracture fixation, requiring concurrent or staged reconstruction.
*
Fracture Patterns:
The type of force applied dictates the fracture pattern (e.g., valgus stress with axial load causing a lateral split-depression fracture; varus stress causing a medial split fracture). The Schatzker classification, while descriptive, reflects these biomechanical forces. The AO/OTA classification provides a more comprehensive, alphanumeric system. The three-column classification (lateral, medial, posterior) emphasizes the importance of posteromedial and posterolateral fragments for stability.
Indications & Contraindications
The decision for operative versus non-operative management of tibial plateau fractures is complex, based on fracture morphology, soft tissue status, patient comorbidities, and surgeon experience. The primary goals of operative intervention are anatomical reduction of the articular surface, restoration of mechanical alignment, stable internal fixation, and early mobilization.
Operative Indications
Absolute indications for surgical intervention include:
*
Articular Step-Off/Gap:
Any articular step-off greater than 2-3 mm and/or gap greater than 3-5 mm after reduction, particularly in young, active patients, mandates surgical correction to prevent post-traumatic arthritis.
*
Joint Instability:
Displaced fractures associated with significant ligamentous instability (e.g., complete rupture of collateral or cruciate ligaments).
*
Open Fractures:
All open fractures require surgical debridement and stabilization, typically with external fixation as an initial stage.
*
Vascular Injury:
Associated arterial injury requiring repair (often with temporary external fixation as a bridge).
*
Compartment Syndrome:
Requires emergent fasciotomy, often followed by staged definitive fixation.
*
Progressive Neurological Deficit:
Although rare, indicative of significant soft tissue swelling or direct nerve compression.
*
Irreducible Displacement:
Failure to achieve acceptable reduction with closed manipulation.
*
Bicondylar Fractures:
Most Schatzker Type IV, V, and VI fractures due to significant displacement and instability.
Relative indications depend on patient factors, fracture stability, and associated injuries:
*
Displaced Split Fractures (Schatzker I, II, III):
Especially if impacting joint congruity or causing instability.
*
High-Energy Mechanisms:
Suggestive of severe soft tissue injury and instability, even if initial articular displacement appears minimal.
*
Patient Age and Activity Level:
Younger, active patients have a lower tolerance for articular incongruity.
*
Planned Associated Ligamentous Reconstruction:
Requiring stable bony construct.
Non-Operative Indications
Non-operative management is typically reserved for:
*
Non-Displaced Fractures:
Minimal or no articular step-off (<2 mm) and stable.
*
Stable Fractures:
Without significant ligamentous injury.
*
Low-Energy Fractures:
Especially in osteoporotic bone where stable fixation may be challenging, or in patients with significant comorbidities precluding surgery.
*
Severely Comminuted Fractures:
Where surgical reconstruction is deemed impossible or offers no clear advantage over conservative management, often in the elderly with limited functional demands.
*
Contraindications to Surgery:
Severe medical comorbidities, active infection, or extremely poor soft tissue envelope (though external fixation may still be considered).
Contraindications
Absolute contraindications to definitive internal fixation:
*
Severe Local Soft Tissue Damage:
Including extensive blistering, necrosis, or active infection. This often necessitates staged management with initial external fixation.
*
Severe Comorbidities:
Where the risks of anesthesia and surgery outweigh the potential benefits.
Relative contraindications:
*
Morbid Obesity:
Can complicate surgical access and increase implant failure risk.
*
Severe Osteopenia/Osteoporosis:
May limit screw purchase and necessitate specialized fixation strategies or non-operative management.
*
Smoking/Nicotine Use:
Increases risk of nonunion and infection; requires aggressive counseling and cessation attempts.
Summary of Operative vs. Non-Operative Indications
| Feature | Operative Indications | Non-Operative Indications |
|---|---|---|
| Articular Step-Off | >2-3 mm | <2 mm, stable |
| Articular Gap | >3-5 mm | <3 mm, stable |
| Joint Instability | Significant ligamentous injury with instability | Stable joint, no significant ligamentous injury |
| Fracture Type (Schatzker) | Types IV, V, VI (most); Displaced I, II, III | Stable Type I, II, III with minimal displacement |
| Open Fractures | Always operative (debridement, stabilization) | N/A |
| Vascular Injury | Always operative (repair, stabilization) | N/A |
| Compartment Syndrome | Always operative (fasciotomy) | N/A |
| Irreducibility | Yes | N/A |
| Patient Factors | Young, active, good bone quality | Elderly, sedentary, significant comorbidities, severe osteopenia |
| Soft Tissue Status | Amenable to surgery (consider staging for poor soft tissues) | Poor soft tissue envelope (blistering, severe swelling) |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is the cornerstone of successful tibial plateau fracture management. It dictates the chosen surgical approach, required implants, and anticipated challenges.
Imaging Acquisition and Analysis
- Standard Radiographs: Anteroposterior (AP), lateral, and oblique views (45° internal/external) are initial studies. These provide basic information on fracture pattern, displacement, and articular involvement. Traction views can aid in assessing ligamentotaxis.
-
Computed Tomography (CT) Scan:
Essential
for detailed surgical planning.
- 2D Axial, Coronal, Sagittal Views: Precisely delineate articular depression, split components, comminution, and fragment orientation. Critical for identifying posteromedial or posterolateral fragments often missed on plain radiographs.
- 3D Reconstructions: Provide a comprehensive spatial understanding of the fracture, invaluable for visualizing complex patterns, column involvement (Luo's classification), and assessing metaphyseal-diaphyseal dissociation.
- Contralateral CT: Can be useful for templating, especially in bicondylar fractures or for assessing normal anatomy for comparison.
- Magnetic Resonance Imaging (MRI): Indicated if significant meniscal, collateral, or cruciate ligamentous injuries are suspected pre-operatively, especially when planning a concurrent ligament reconstruction. Not routinely required for fracture diagnosis.
- CT Angiography: If vascular injury is suspected (e.g., diminished pulses, expanding hematoma, medial plateau fracture, high-energy injury).
Surgical Planning Workflow
- Classification: Apply a relevant classification system (e.g., Schatzker, AO/OTA, Luo's three-column) to systematically analyze the fracture.
- Fragment Analysis: Identify key articular fragments, areas of depression, metaphyseal comminution, and any significant posterior fragments.
- Soft Tissue Assessment: Evaluate skin integrity, swelling, and presence of blisters. Staging with external fixation may be necessary for severe soft tissue compromise.
- Approach Selection: Based on fracture pattern and column involvement. Plan single or dual incisions. Consider extensile approaches if needed.
-
Reduction Strategy:
Determine the sequence of reduction:
- Indirect Reduction: Ligamentotaxis, external fixator distraction.
- Direct Reduction: Articular surface elevation, buttressing, provisional fixation.
- Bone Grafting: Autograft (iliac crest), allograft (cancellous chips), or bone graft substitutes for metaphyseal defects.
- Fixation Strategy: Select appropriate implants (locking plates, conventional plates, cannulated screws, external fixation). Consider the number and trajectory of screws for optimal stability.
- Templating: Utilize CT scans to virtually template plate placement and screw length/trajectory.
Pre-Operative Patient Preparation
- Antibiotics: Prophylactic intravenous antibiotics (e.g., cefazolin) administered within 60 minutes of incision.
- Thromboprophylaxis: Mechanical (SCDs) and/or pharmacological (LMWH) deep vein thrombosis (DVT) prophylaxis.
- Anesthesia: General anesthesia with or without regional block (femoral or sciatic nerve block) for post-operative pain control.
- Tourniquet: Typically used for bloodless field, especially with extensile approaches. Prepare for potential prolonged tourniquet time.
- Consent: Detailed discussion with the patient regarding risks, benefits, alternatives, and potential complications.
Patient Positioning
The patient is typically positioned supine on a radiolucent table.
*
Supine Position:
Allows for easy access to the entire knee.
*
Pneumatic Tourniquet:
Applied to the proximal thigh.
*
Leg Prep and Drape:
Sterile prep from mid-thigh to toes, allowing for full knee range of motion and fluoroscopic visualization.
*
Image Intensifier:
Positioned for intra-operative AP and lateral fluoroscopic views.
*
Support:
A bump or support under the contralateral hip may assist with alignment.
*
Knee Flexion:
A small bolster or towel roll can be placed under the distal thigh to allow slight knee flexion, which may assist in visualizing certain fragments or aid in initial traction. Articulated knee holders can be used to facilitate positioning.
*
Traction (Optional):
A traction table (e.g., femoral distractor) can be employed for indirect reduction via ligamentotaxis, particularly for comminuted fractures or significant shortening.
Detailed Surgical Approach / Technique
Surgical intervention for tibial plateau fractures demands precision, a comprehensive understanding of surgical anatomy, and adaptability to complex fracture patterns. The choice of surgical approach is critical for adequate exposure, reduction, and stable fixation.
General Principles of Fixation
- Anatomic Articular Reduction: The primary goal is to restore the smooth articular surface, typically achieved by elevating depressed fragments and buttressing split fragments.
- Mechanical Axis Restoration: Ensure correct limb alignment to prevent abnormal load distribution.
- Stable Fixation: Provide sufficient stability to allow early range of motion and prevent loss of reduction. Locking plates have revolutionized this, particularly in osteoporotic bone.
- Soft Tissue Preservation: Minimize soft tissue stripping to maintain vascularity and reduce infection risk.
- Bone Grafting: Fill metaphyseal defects created by elevating depressed articular fragments. Autograft is the gold standard, but allograft or synthetic substitutes are frequently used.
Surgical Approaches
The chosen approach depends on the fracture pattern and involved columns.
1. Anterolateral Approach (Lateral Plateau Fractures - Schatzker I, II, III)
- Incision: A longitudinal incision, 10-15 cm, centered over the anterolateral aspect of the knee, extending from the patella to approximately 5 cm distal to the joint line.
-
Dissection:
- Skin and Subcutaneous Tissue: Incise through the skin and subcutaneous fat.
- Fascia: Incise the fascia lata just anterior to Gerdy's tubercle.
- Internervous Plane: Elevate the tibialis anterior muscle off the lateral aspect of the tibia anteriorly. Posteriorly, dissect subperiosteally to expose the lateral tibial plateau. The iliotibial band (ITB) can be split longitudinally or retracted anteriorly/posteriorly.
- Visualization: Submeniscal arthrotomy (typically through the lateral discoid meniscus if involved) or elevation of the meniscal attachment provides direct visualization of the articular surface. The ITB and biceps femoris muscle are retracted posteriorly. The common peroneal nerve is protected posteriorly around the fibular neck.
-
Variations:
- "Hockey Stick" or "Reverse L" Extension: Allows more posterior visualization if needed, but risks soft tissue stripping.
- Limited Incisions: For minimally invasive techniques with percutaneous screw fixation.
2. Anteromedial Approach (Medial Plateau Fractures - Schatzker IV)
- Incision: A longitudinal incision, 10-15 cm, centered over the anteromedial aspect of the knee, similar to the anterolateral approach.
-
Dissection:
- Skin and Subcutaneous Tissue: Incise skin and subcutaneous fat.
- Sartorius Fascia: Incise anterior to the sartorius muscle.
- Internervous Plane: Elevate the pes anserinus (sartorius, gracilis, semitendinosus) insertion off the medial tibia. Retract these structures posteriorly. The medial collateral ligament (MCL) is anterior to this plane and must be carefully protected or repaired if avulsed. Subperiosteal dissection exposes the medial tibial plateau.
- Visualization: Submeniscal arthrotomy of the medial meniscus may be necessary. Care must be taken to avoid stripping the periosteum excessively to preserve vascularity.
3. Posteromedial Approach (Posteromedial Fragment - Schatzker IV, VI, Three-Column Fractures)
- Incision: A longitudinal incision, 10-15 cm, midway between the posterior border of the MCL and the posteromedial crest of the tibia.
-
Dissection:
- Skin and Subcutaneous Tissue.
- Fascia: Incise the deep fascia.
- Internervous Plane: The interval between the sartorius/gracilis/semitendinosus (posteriorly) and the gastrocnemius/soleus (anteriorly). The MCL is anterior to the approach.
- Structures to Protect: The saphenous nerve and vein are anterior to the incision. The popliteal artery and vein are deep and posterior, protected by the posterior muscles.
- Exposure: Provides direct visualization of the posteromedial tibial plateau and allows for buttress plating.
4. Posterolateral Approach (Posterolateral Fragment - Schatzker II, III, VI, Three-Column Fractures)
- Incision: A longitudinal incision, 10-15 cm, centered over the fibular head, extending proximally and distally.
-
Dissection:
- Skin and Subcutaneous Tissue.
- Fascia: Incise fascia.
- Internervous Plane: This is a challenging approach due to critical neurovascular structures. The common peroneal nerve courses around the fibular neck and must be identified and protected, often by careful dissection and retraction.
- Muscles: The biceps femoris tendon is retracted posteriorly. The soleus and popliteus muscles may need partial elevation.
- Osteotomy (Optional): A fibular head osteotomy can be performed for improved visualization of the posterolateral plateau, followed by re-fixation. This is a significant consideration due to potential peroneal nerve injury.
- Exposure: Direct access to the posterolateral tibial plateau.
5. Bicondylar Approaches (Schatzker V, VI)
- Dual Incisions: Often preferred. A combination of anterolateral and anteromedial, or anterolateral and posteromedial approaches. Allows separate access to each condyle, minimizing soft tissue stripping.
- Single Anterior Incision: Less common, but can be used for selected bicondylar fractures (e.g., via a midline approach with medial and lateral flaps). High risk of wound complications.
Reduction Techniques
- Ligamentotaxis: Axial traction (manual or distractor) can help to indirectly reduce fragments via tension in the surrounding soft tissues and ligaments.
-
Direct Reduction:
- Articular Surface Elevation: Depressed articular fragments are carefully elevated using osteotomes or tampers from a metaphyseal window or directly visualized.
- Joy-Sticking: K-wires or small external fixator pins can be inserted into large fragments to manipulate them into position.
- Reduction Clamps: Pointed reduction clamps are essential for compressing split fragments.
- Bone Grafting: Once articular fragments are elevated, the resulting metaphyseal void must be filled with bone graft (autograft, allograft, or synthetic) to provide structural support and prevent re-depression.
- Provisional Fixation: K-wires are used to maintain reduction while definitive fixation is applied.
Definitive Fixation
-
Plate and Screw Fixation:
The most common method.
- Lateral Buttress Plates: Pre-contoured locking plates are standard for lateral plateau fractures. They provide buttress support and stable fixation of articular fragments. Screws are directed to capture fragments and provide subchondral support.
- Medial Plates: Used for medial plateau fractures or for bicondylar fractures where additional medial support is required.
- Posterior Plates: Used for significant posterior fragments requiring buttressing.
- Locking Plates: Offer angular stability, which is advantageous in comminuted fractures or osteoporotic bone, as screw purchase is not solely dependent on bone density.
- Cannulated Screws: Often used for isolated split fractures (Schatzker I) or as supplemental fixation for large fragments.
-
External Fixation:
- Temporary: For initial stabilization in open fractures, severe soft tissue injuries, or polytrauma.
- Definitive: For very comminuted fractures not amenable to internal fixation, or in patients with severe comorbidities where minimal surgery is desired. Hybrid fixators can combine pins in bone with external rings.
- Arthroscopy-Assisted Fixation: Can be used to directly visualize and confirm articular reduction, especially for simple split or depression fractures. However, it adds fluid management challenges and typically requires a specific skill set.
Intra-Operative Assessment
- Fluoroscopy: Essential for confirming fragment reduction, implant position, and overall alignment (AP and lateral views).
- Direct Visualization: For articular congruity, meniscal integrity, and ligamentous stability.
- Stability Assessment: After fixation, stress testing of the knee joint is performed to assess residual laxity, particularly for the MCL and LCL.
Complications & Management
Tibial plateau fractures are associated with a high rate of complications due to the severity of injury, articular involvement, and extensive soft tissue damage. Proactive recognition and management are crucial.
Common Complications
| Complication | Incidence | Management Strategy |
|---|---|---|
| Post-traumatic Arthritis | 20-60% | Prevention: Anatomical articular reduction, stable fixation, early ROM. Management: Non-operative (activity modification, NSAIDs, injections, bracing), surgical (arthroscopy, osteotomy, unicompartmental or total knee arthroplasty in end-stage disease). |
| Compartment Syndrome | 5-15% | Prevention: Early diagnosis, avoiding prolonged tourniquet time, judicious fluid management. Management: Emergent four-compartment fasciotomy, close wound management, often delayed wound closure. Requires high index of suspicion. |
| Infection (Superficial/Deep) | 2-10% (up to 20% in open fx) | Prevention: Strict sterile technique, prophylactic antibiotics, soft tissue handling, meticulous wound closure. Management: Superficial: Oral antibiotics, local wound care. Deep: Surgical debridement, IV antibiotics, irrigation, possibly implant removal (if stable union) or two-stage revision. |
| Neurovascular Injury | Peroneal Nerve: 10-20% | Prevention: Careful dissection, identification, and protection of the common peroneal nerve. Popliteal artery/vein: High index of suspicion with high-energy/medial fractures. Management: Peroneal nerve: Observation, ankle-foot orthosis. Vascular: Emergent vascular repair. |
| Malunion/Nonunion | Malunion: 10-20%; Nonunion: 2-5% | Prevention: Anatomical reduction, stable fixation, appropriate bone grafting. Management: Malunion (valgus/varus deformity, limb shortening): Corrective osteotomy. Nonunion: Revision surgery with debridement, stable fixation, and bone grafting. |
| Stiffness/Arthrofibrosis | Up to 30% | Prevention: Early, controlled range of motion, aggressive rehabilitation. Management: Aggressive physical therapy, serial manipulation under anesthesia, arthroscopic arthrolysis, open arthrolysis. |
| DVT/Pulmonary Embolism (PE) | DVT: 15-40%; PE: 1-5% | Prevention: Mechanical (SCDs) and pharmacological (LMWH) prophylaxis, early mobilization. Management: Anticoagulation (oral or parenteral). For PE: Systemic anticoagulation, supportive care. |
| Hardware Failure/Prominence | 5-10% | Prevention: Biomechanically sound fixation, appropriate plate contouring. Management: Symptomatic hardware removal (after union), revision fixation if associated with loss of reduction or nonunion. |
| Meniscal Injury | 30-50% | Prevention: Careful assessment and repair during surgery. Management: Repair (suture), partial meniscectomy for irreparable tears, or observation for stable peripheral tears. |
| Ligamentous Instability | Variable (ACL/MCL/LCL) | Prevention: Intra-operative assessment and repair/reconstruction if indicated. Management: Non-operative (bracing, therapy) or surgical (staged or concurrent ligament reconstruction). |
Specific Management Considerations
- Soft Tissue Envelope: Severe soft tissue injury (e.g., degloving, extensive blistering, open wounds) is a major predictor of complications. Staged management with temporary external fixation, meticulous wound care, and delayed definitive internal fixation (once the soft tissue envelope has recovered, typically 7-14 days) is often preferred. Negative pressure wound therapy can be beneficial.
- Bone Quality: Osteoporotic bone presents challenges for screw purchase. Locking plate technology has improved fixation stability, but careful technique and potentially bone cement augmentation are still required in severe cases.
- Polytrauma: Tibial plateau fractures in polytrauma patients require prioritization. Life-threatening injuries take precedence. Temporary external fixation is often the initial approach, followed by definitive fixation once the patient is stable.
- Geriatric Patients: These patients often have significant comorbidities and fragile skin. A less aggressive surgical approach, shorter operative times, and careful rehabilitation planning are paramount.
Post-Operative Rehabilitation Protocols
Rehabilitation after a tibial plateau fracture is a critical determinant of long-term functional outcome. Protocols vary based on fracture type, stability of fixation, bone quality, and concomitant soft tissue injuries. The overarching goals are to restore knee range of motion (ROM), improve strength, protect the articular repair, and facilitate a gradual return to functional activities.
General Principles
- Pain and Swelling Control: Essential in the early post-operative period using analgesics, ice, elevation, and compression.
- Early ROM: Crucial to prevent arthrofibrosis, but must be initiated cautiously to protect the articular surface and fixation.
- Delayed Weight-Bearing (NWB/TDWB): Typically for 8-12 weeks, depending on the stability of fixation and bone healing. Early protected weight-bearing may be considered for highly stable constructs in younger patients.
- Gradual Strengthening: Progressively increasing resistance as bone healing permits.
- Proprioception and Balance Training: Important for restoring neuromuscular control.
Phased Rehabilitation Protocol (Example)
Phase 1: Immediate Post-Operative (Weeks 0-6)
- Goals: Reduce pain and swelling, protect fracture fixation, achieve early knee ROM, maintain quadriceps activation.
- Weight-Bearing: Non-weight-bearing (NWB) or Touch-Down Weight-Bearing (TDWB) with crutches/walker.
- Bracing: A hinged knee brace is typically prescribed, locked in full extension for ambulation and unlocked for controlled ROM exercises.
-
Exercises:
- ROM: Passive ROM (CPM machine if indicated, or gentle therapist-assisted ROM) and active-assisted ROM (AAROM). Aim for 0-90 degrees by 4-6 weeks.
- Strengthening (Isometric): Quadriceps sets, gluteal sets, hamstring sets.
- Ankle Pumps: To promote circulation and reduce DVT risk.
- Patellar Mobilization: To prevent adhesions.
- Upper Extremity Conditioning: To aid with crutch ambulation.
- Wound Care: Monitor incision for signs of infection.
Phase 2: Early Healing & Progressive ROM (Weeks 6-12)
- Goals: Increase ROM, gradually progress weight-bearing, initiate active strengthening.
- Weight-Bearing: Progress from TDWB to Partial Weight-Bearing (PWB) as tolerated, typically starting at 6-8 weeks, guided by radiographs demonstrating fracture healing. Full weight-bearing by 10-12 weeks if union is sufficient.
- Bracing: Continue hinged knee brace, progressively unlocked as ROM improves. May be discontinued by week 12.
-
Exercises:
- ROM: Continue to increase AAROM and active ROM, aiming for 0-120 degrees or more by week 12.
- Strengthening: Low-resistance open-chain exercises (e.g., knee extension/flexion, straight leg raises) and closed-chain exercises (e.g., mini-squats, leg presses) with careful control.
- Gait Training: Focus on proper gait mechanics with progressive weight-bearing.
- Proprioception: Balance exercises (single leg stance with support).
- Radiographic Evaluation: Regular X-rays to monitor fracture healing.
Phase 3: Advanced Strengthening & Functional Return (Weeks 12-24+)
- Goals: Restore full ROM, maximize strength and endurance, improve proprioception, prepare for sport/work-specific activities.
- Weight-Bearing: Full Weight-Bearing (FWB).
- Bracing: Discontinued.
-
Exercises:
- Strengthening: Progress to higher resistance closed-chain exercises (squats, lunges, step-ups), resistance bands, light plyometrics (if appropriate).
- Cardiovascular: Stationary cycling, swimming, elliptical trainer.
- Proprioception & Agility: Balance boards, single-leg hopping, sport-specific drills.
- Flexibility: Continue stretching to maintain ROM.
- Return to Activity: Gradual return to light, low-impact activities. High-impact sports or heavy manual labor may require 6-12 months or longer, contingent on healing and functional recovery.
Special Considerations
- Concomitant Ligamentous Injuries: If significant ligamentous repairs or reconstructions were performed, their specific rehabilitation protocols must be integrated, often necessitating slower progression of ROM and weight-bearing.
- Meniscal Repairs: Protection of meniscal repairs often dictates delayed weight-bearing and restricted flexion in the early phases.
- Osteoporotic Bone: May require a more conservative weight-bearing progression due to weaker bone and potentially less robust fixation.
- Patient Compliance: Essential for successful outcomes. Regular communication with the patient and physical therapist is vital.
- Hardware Removal: May be considered for symptomatic hardware after fracture union is complete, typically 12-18 months post-operatively.
Summary of Key Literature / Guidelines
The management of tibial plateau fractures has evolved significantly, guided by a robust body of literature and the development of evidence-based guidelines. Key areas of focus include fracture classification, surgical timing, implant technology, and the assessment of long-term outcomes.
Classification Systems
- Schatzker Classification: Remains widely used for its simplicity and prognostic value (Types I-VI). While useful, it primarily describes the frontal plane and does not fully account for posterior comminution.
- AO/OTA Classification: A more comprehensive alphanumeric system providing greater detail on fracture morphology, valuable for research and complex cases.
- Three-Column Classification (Luo et al.): Emphasizes the importance of posterior fragments (posteromedial and posterolateral) in overall stability, influencing surgical approach selection and the need for posterior buttress plating. This concept has significantly improved the understanding of complex bicondylar fractures.
Surgical Timing
- Staged Management: A prevailing paradigm for high-energy injuries with significant soft tissue compromise. Initial temporary external fixation provides stability, allows soft tissue swelling to subside, and reduces the risk of wound complications. Definitive internal fixation is typically performed once the "wrinkle sign" appears (7-14 days).
- Acute Fixation: Indicated for open fractures, vascular injury, or compartment syndrome, often after emergent debridement and fasciotomy. Also considered for stable soft tissue envelopes in simple, non-displaced patterns.
Implant Technology
- Locking Plate Technology: Has revolutionized fixation, especially in osteoporotic bone and comminuted fractures. Locking screws create a fixed-angle construct, improving stability and reducing the reliance on direct bone-to-plate compression. Pre-contoured anatomical plates are standard.
- Minimally Invasive Plate Osteosynthesis (MIPO): Techniques are increasingly employed to minimize soft tissue dissection and preserve vascularity, reducing wound complications. These often involve percutaneous screw insertion and fluoroscopic guidance.
- External Fixation: Continues to play a vital role, not only as a temporary measure but also as definitive treatment in select cases, particularly hybrid fixators for complex bicondylar or open fractures.
Controversies and Evolving Concepts
- Bone Grafting: While autograft remains the gold standard for metaphyseal defects, allografts and synthetic bone graft substitutes are increasingly used due to donor site morbidity. Comparative studies are ongoing to define optimal graft choices.
- Arthroscopy-Assisted Fixation: Offers benefits for direct articular visualization and meniscal management, but the added operative time, fluid extravasation risks, and technical demands limit its widespread use for complex patterns.
- Long-Term Outcomes: Studies consistently report a high incidence of post-traumatic arthritis despite anatomical reduction and stable fixation, highlighting the importance of articular cartilage preservation and meticulous technique. Factors like initial injury severity, meniscal integrity, and residual joint incongruity significantly influence long-term prognosis.
- Biologic Augmentation: The role of platelet-rich plasma (PRP) or bone marrow aspirate concentrate (BMAC) in enhancing fracture healing is an area of ongoing research, though not yet standard practice.
Guidelines
While no single universally accepted guideline exists, the principles articulated by major orthopedic trauma organizations (e.g., AO Foundation, Orthopaedic Trauma Association) emphasize:
*
Thorough Pre-operative Assessment:
Including high-quality CT imaging.
*
Individualized Treatment Planning:
Based on fracture pattern, soft tissue status, and patient factors.
*
Anatomical Reduction of Articular Surface:
As the primary surgical goal.
*
Stable Internal Fixation:
Allowing early, controlled motion.
*
Comprehensive Post-operative Rehabilitation:
Tailored to the injury.
In conclusion, effective management of tibial plateau fractures requires a multidisciplinary approach, combining surgical expertise with meticulous planning and diligent post-operative care. Continued research aims to further refine surgical techniques, optimize rehabilitation protocols, and ultimately improve long-term functional outcomes for patients facing these complex injuries.
You Might Also Like