Tibial Plateau Fracture: A Comprehensive Guide to Care and Prognosis
Key Takeaway
Your ultimate guide to Tibial Plateau Fracture: A Comprehensive Guide to Care and Prognosis starts here. A tibial plateau fracture is a periarticular injury of the proximal tibia, often linked with soft tissue damage. These fractures are classified by systems like Schatzker or the 3-Column Concept. Diagnosis uses imaging such as X-rays, CT, or MRI. Treatment varies from nonoperative immobilization to surgical options including ORIF or external fixation, addressing fracture severity.
Tibial Plateau Fracture: A Comprehensive Guide to Care and Prognosis
Tibial plateau fractures are complex periarticular injuries of the proximal tibia, characterized by compromise of the articular surface and frequently associated soft tissue injury. Successful management necessitates a thorough understanding of their intricate anatomy, biomechanics, classification, and nuanced surgical techniques to optimize functional outcomes and mitigate long-term sequelae.
Introduction & Epidemiology
Tibial plateau fractures represent a spectrum of injuries ranging from low-energy avulsion fractures to high-energy articular impaction and metaphyseal comminution. These fractures typically result from axial load combined with valgus or varus forces, often seen in motor vehicle accidents, falls from height, or sports-related trauma. A bimodal distribution is observed, affecting younger individuals involved in high-energy mechanisms and older, osteopenic individuals sustaining low-energy falls. The incidence of associated soft tissue injuries, including meniscal tears, ligamentous ruptures (ACL, MCL, LCL), and neurovascular compromise, is substantial, often exceeding 50% in high-energy fracture patterns. The long-term prognosis is heavily influenced by the quality of articular reduction, stability of fixation, and the management of concomitant soft tissue damage, with post-traumatic osteoarthritis being a significant concern. Recent academic contributions, such as those by
Mohammad Hutaif
(
 ORCID ID: 0009-0001-1092-5600
) via
Google Scholar
, continue to refine our understanding of these complex injuries.
ORCID ID: 0009-0001-1092-5600
) via
Google Scholar
, continue to refine our understanding of these complex injuries.
Surgical Anatomy & Biomechanics
Osteology
The proximal tibia comprises the medial and lateral tibial condyles, separated by the intercondylar eminence.
*
Lateral Tibial Plateau:
Convex in shape, generally higher than the medial plateau, and supports the lateral femoral condyle. Its articular cartilage is typically thinner. It is more commonly fractured due to its relatively weaker subchondral bone and the prevalence of valgus loading mechanisms. Gerdy's tubercle, the insertion site for the iliotibial band, is located on the anterolateral aspect.
*
Medial Tibial Plateau:
Concave, distal to the lateral plateau, and supports the medial femoral condyle. It has thicker subchondral bone and articular cartilage, making it more resistant to fracture.
*
Proximal Tibial Alignment:
Critical for knee biomechanics.
*
Posterior Tibial Slope:
A normal posterior inclination of 7-10 degrees, crucial for knee kinematics, particularly during flexion. Alterations can lead to anterior or posterior knee instability.
*
Varus Slope (Medial Proximal Tibial Angle - MPTA):
A slight varus alignment of approximately 87 degrees (lateral opening angle) is normal. Loss of this anatomical alignment can significantly alter load distribution across the knee joint.
*
Tibial Rotation:
The proximal tibia normally exhibits external rotation relative to the distal tibia. Rotational malalignment following fracture can lead to patellofemoral tracking issues and altered gait mechanics.
*
Metaphysis and Diaphysis:
The transition zone from the wide metaphysis to the narrower diaphysis is critical in certain fracture patterns (e.g., Schatzker VI), indicating metaphyseal-diaphyseal dissociation.
Soft Tissue Structures
The proximity of vital neurovascular structures and stabilizing ligaments necessitates careful consideration during surgical planning and execution.
*
Ligaments:
*
Anterior Cruciate Ligament (ACL):
Originates from the posteromedial aspect of the lateral femoral condyle and inserts into the anteromedial intercondylar area of the tibia. Resists anterior tibial translation and internal rotation.
*
Posterior Cruciate Ligament (PCL):
Originates from the lateral aspect of the medial femoral condyle and inserts into the posterior intercondylar area of the tibia. Resists posterior tibial translation.
*
Medial Collateral Ligament (MCL):
Superficial and deep layers. Originates from the medial femoral epicondyle, inserting into the medial tibia. Resists valgus stress. Often injured in valgus-producing tibial plateau fractures.
*
Lateral Collateral Ligament (LCL):
Originates from the lateral femoral epicondyle and inserts into the fibular head. Resists varus stress. Part of the posterolateral corner (PLC). PLC injuries are complex and can significantly compromise knee stability.
*
Menisci:
Medial and lateral menisci are C-shaped fibrocartilaginous structures that increase articular congruity, distribute load, and absorb shock. They are frequently entrapped or torn in tibial plateau fractures, particularly in split and depressed patterns.
*
Neurovascular Structures:
*
Peroneal Nerve:
Winds around the fibular neck, highly vulnerable to direct trauma, traction, or compression in lateral plateau fractures, fibular head fractures, or due to compartment syndrome.
*
Popliteal Artery and Vein:
Located posteriorly in the popliteal fossa, susceptible to injury in high-energy mechanisms, especially with posterior displacement of fragments or knee dislocation patterns.
*
Compartments of the Lower Leg:
The four compartments (anterior, lateral, deep posterior, superficial posterior) are at risk for compartment syndrome due to hematoma or swelling, particularly with high-energy injuries.
Biomechanics of Injury
Tibial plateau fractures occur when forces exceed the load-bearing capacity of the subchondral bone and articular cartilage.
*
Valgus/Axial Load:
Most common mechanism, impacting the lateral plateau, leading to split (Schatzker I) or split-depression (Schatzker II) fractures. The lateral condyle is often driven distally, impacting the weaker cancellous bone of the lateral tibial plateau.
*
Varus/Axial Load:
Less common, affecting the medial plateau (Schatzker IV). This mechanism often involves a higher energy transfer due to the stronger medial bone, resulting in more comminuted fractures and a higher incidence of neurovascular injury.
*
Direct Blows/Posterior Forces:
Can lead to posterior plateau fractures, often associated with PCL injury.
*
Bone Quality:
Osteopenic bone is more prone to pure depression fractures (Schatzker III) with less cortical involvement, while stronger bone tends to sustain split fractures.
Classification Systems
Accurate classification is paramount for guiding surgical planning and predicting prognosis.
*
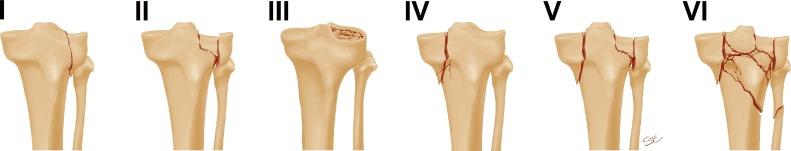
Schatzker Classification:
The most widely used system, based on fracture morphology and location, emphasizing articular involvement.
*
Type I (Lateral Split):
Pure cleavage fracture of the lateral plateau, typically involves the lateral tibial spine. Low-energy, often non-displaced.
*
Type II (Lateral Split-Depression):
Combination of split and depressed articular segments of the lateral plateau. More common in younger patients with stronger bone.
*
Type III (Lateral Pure Depression):
Depression of the lateral articular surface without a significant split. Common in osteopenic patients.
*
Type IV (Medial Plateau):
Fracture of the medial tibial plateau, often high-energy, involving the medial tibial spine. Can be split, depressed, or comminuted. Often associated with neurovascular injury and compartment syndrome.
*
Type V (Bicondylar):
Fracture involving both medial and lateral tibial condyles, with intact diaphyseal-metaphyseal continuity. High-energy, significant soft tissue injury risk.
*
Type VI (Plateau-Diaphyseal Dissociation):
Bicondylar fracture with a transverse subcondylar fracture, separating the articular block from the diaphysis. Highest energy injury, extensive soft tissue damage, high complication rate.
*
AO/OTA Classification:
A more comprehensive and objective alphanumeric system (41-B fractures) that describes bone, segment, fracture pattern, and severity. Offers higher inter-observer reliability for complex fractures.
*
41-B1:
Split fractures (simple articular, simple metaphyseal).
*
41-B2:
Depression fractures (simple articular, simple metaphyseal).
*
41-B3:
Combined split and depression fractures.
*
Luo's 3-Column Classification:
Divides the proximal tibia into three columns (medial, lateral, posterior). Provides a practical guide for surgical approaches, particularly for complex bicondylar and posterior fractures.
*
Lateral Column:
Involves the lateral tibial plateau.
*
Medial Column:
Involves the medial tibial plateau.
*
Posterior Column:
Involves the posterior aspect of either condyle. Fractures can involve one, two, or all three columns.
Indications & Contraindications
Management of tibial plateau fractures can be challenging, requiring careful assessment of fracture morphology, soft tissue status, and patient factors. The decision between operative and non-operative management is critical.
Non-Operative Management
Non-operative treatment is generally reserved for stable fractures with minimal displacement.
*
Indications:
* Minimally displaced (<2mm articular step-off, <5mm condylar widening).
* Stable fracture patterns (e.g., Schatzker I without significant displacement).
* Non-ambulatory patients or those with severe comorbidities precluding surgery.
* Severely osteoporotic bone where stable fixation is unlikely.
*
Protocol:
Initial period of non-weight bearing (typically 6-12 weeks) with progressive range of motion exercises. Serial radiographs are essential to monitor for secondary displacement.
Operative Management
Operative intervention aims to restore articular congruity, axial alignment, and stability to permit early mobilization and optimize long-term function.
*
Absolute Indications:
* Open fractures.
* Compartment syndrome (impending or frank).
* Vascular compromise.
* Irreducible meniscal entrapment.
* Significant articular step-off (>2-3mm).
* Significant condylar widening (>5mm).
* Gross instability or malalignment (>5-10 degrees varus/valgus).
* Associated ligamentous injury leading to instability.
*
Relative Contraindications:
* Severe soft tissue compromise (e.g., severe fracture blisters, extensive degloving, open wounds precluding immediate definitive fixation). These may necessitate staged treatment with temporary external fixation.
* Active infection.
* Significant medical comorbidities posing unacceptably high anesthetic or surgical risk.
| Indication Category | Operative Management | Non-Operative Management |
|---|---|---|
| Fracture Displacement | Articular step-off >2-3mm, Condylar widening >5mm, Gross instability | Non-displaced, minimally displaced (<2-3mm articular step-off, <5mm widening) |
| Alignment | Varus/valgus malalignment >5-10 degrees, >5mm posterior slope change | Stable, anatomically aligned |
| Soft Tissue Injury | Open fracture, Impending/frank compartment syndrome, Vascular injury, Irreducible meniscal interposition, Severe associated ligamentous instability | Intact soft tissue envelope, no signs of compromise, minor ligamentous sprains |
| Patient Factors | Physiologically fit, ambulatory patient, good bone quality | Non-ambulatory, severe comorbidities precluding surgery, non-compliant patient, severely osteoporotic bone where fixation is tenuous |
Pre-Operative Planning & Patient Positioning
Thorough pre-operative planning is crucial for predictable outcomes in tibial plateau fractures.
Imaging
- Plain Radiographs: Anteroposterior (AP), lateral, and oblique views (45° internal and external rotation) of the knee are standard. A contralateral knee film can be useful for templating and assessing pre-injury alignment. These provide initial assessment of fracture pattern and displacement.
- Computed Tomography (CT) Scan: Essential for detailed evaluation of articular morphology, fragment size, comminution, and depression. Multiplanar reconstructions and 3D imaging are invaluable for visualizing fragment orientation, soft tissue entrapment, and for planning surgical approaches. CT angiography may be indicated if vascular injury is suspected.
- Magnetic Resonance Imaging (MRI): Recommended for assessing associated soft tissue injuries, including meniscal tears, collateral ligament ruptures (MCL, LCL), cruciate ligament tears (ACL, PCL), and chondral lesions. This information guides intraoperative decision-making regarding meniscal repair or concurrent ligamentous stabilization.
Surgical Strategy
- Classification Application: Utilizing Schatzker, AO/OTA, and Luo classifications to fully characterize the fracture. The Luo 3-column concept is particularly useful for identifying surgical targets and determining optimal approaches.
- Approach Selection: Based on the column involvement and specific fracture fragments requiring reduction and fixation. Anticipate single versus dual incisions, and consider staged procedures for severe open or high-energy injuries with significant soft tissue compromise.
- Implant Selection: Determine the type and number of plates (e.g., lateral locking plate, medial locking plate, posteromedial buttress plate) and screws. Consider the need for bone graft or bone graft substitutes to fill metaphyseal voids created by elevated depressed fragments.
- Contingency Planning: Anticipate potential challenges such as severe comminution, poor bone quality, or irreducible fragments. Plan for alternative fixation methods or bone graft options.
Patient Optimization
- Medical Workup: Comprehensive medical evaluation to optimize comorbidities and minimize surgical risk.
- Antibiotic Prophylaxis: Administer pre-operatively according to institutional protocols.
- DVT Prophylaxis: Initiate pre- or intra-operatively as per guidelines.
- Soft Tissue Assessment: Meticulous evaluation of the soft tissue envelope for blisters, open wounds, or devitalized tissue. Delay definitive fixation if soft tissues are compromised, and consider temporary external fixation as a bridge.
Patient Positioning
- Supine Position: On a radiolucent operating table, allowing for free range of motion of the knee and full C-arm access.
- Femoral Distractor: Often employed for temporary ligamentotaxis and traction, which aids in fracture reduction, visualization, and maintenance of limb length.
- Sandbag: Placed under the ipsilateral hip for slight internal rotation of the leg, which can facilitate certain lateral approaches.
- Tourniquet: Applied high on the thigh to minimize blood loss and improve visualization.
- C-arm: Positioned to obtain AP, lateral, and oblique views throughout the procedure.
- Leg Prep and Drape: Sterile preparation extending from the mid-thigh to the foot. The foot should be draped free to allow for ankle and foot manipulation during reduction.
Detailed Surgical Approach / Technique
The primary goals of surgical management are anatomic reduction of the articular surface, restoration of mechanical axis, stable fixation to allow early motion, and meticulous soft tissue handling.
General Principles
- Indirect vs. Direct Reduction: Employ indirect techniques (ligamentotaxis, femoral distractor) initially, followed by direct visualization and reduction of articular fragments.
- Articular First: Prioritize restoring the articular congruity before addressing metaphyseal defects or shaft alignment.
- Metaphyseal Support: Fill metaphyseal bone voids with autograft, allograft, or synthetic bone graft substitutes to prevent secondary collapse of the elevated articular segment.
- Stable Fixation: Utilize anatomically contoured locking plates and screws to provide robust fixation, allowing for early controlled range of motion.
- Soft Tissue Preservation: Minimize soft tissue stripping, ensure adequate surgical windows, and handle tissues gently to reduce complications.
- Associated Injuries: Address meniscal tears (repair or partial meniscectomy) and assess ligamentous stability at the time of definitive fixation.
Surgical Approaches
The choice of approach is dictated by the fracture pattern, particularly the column involvement as per Luo's classification.
-
Anterolateral Approach:
- Indications: Schatzker I, II, III (lateral plateau fractures), and some bicondylar patterns needing lateral access.
- Incision: Longitudinal or S-shaped incision from the lateral femoral epicondyle extending distally across Gerdy's tubercle.
- Internervous Plane: Between the rectus femoris (innervated by femoral nerve) and vastus lateralis (innervated by femoral nerve). However, the critical layer is the IT band.
- Dissection: Incise the skin and subcutaneous tissue. Identify and protect the common peroneal nerve anterior to the biceps femoris tendon, which courses around the fibular neck. The iliotibial band is then split longitudinally, reflecting the anterior portion anteriorly and the posterior portion posteriorly. The vastus lateralis can be partially detached or reflected anteriorly from the lateral femoral condyle and lateral capsule. Incise the capsule carefully to visualize the fracture.
- Key Structures at Risk: Common peroneal nerve (posteriorly), lateral superior genicular artery.
-
Anteromedial Approach:
- Indications: Schatzker IV, V, VI (medial plateau fractures), or bicondylar patterns needing medial access.
- Incision: Longitudinal or S-shaped incision from the medial femoral epicondyle extending distally along the medial aspect of the tibia.
- Internervous Plane: Between the sartorius (femoral nerve) and the gracilis/semitendinosus (obturator/tibial nerves). The medial approach is usually made anterior to the pes anserinus.
- Dissection: Incise the skin and subcutaneous tissue. The saphenous nerve and great saphenous vein are protected, typically retracted posteriorly. The pes anserinus (sartorius, gracilis, semitendinosus) can be mobilized posteriorly or detached from the tibia if necessary, and then repaired. The medial collateral ligament (MCL) deep layer is incised to expose the fracture.
- Key Structures at Risk: Saphenous nerve, great saphenous vein, superficial branch of the medial superior genicular artery.
-
Posteromedial Approach (e.g., modified Olerud approach):
- Indications: Fractures involving the posteromedial column (Luo type II or III), posterior Schatzker IV, V, VI fractures.
- Incision: Longitudinal incision along the posteromedial border of the tibia, usually 1-2 cm posterior to the posteromedial edge.
- Internervous Plane: Between the medial head of the gastrocnemius (tibial nerve) and the semimembranosus/pes anserinus tendons.
- Dissection: Incise the skin and subcutaneous tissue. Mobilize the gastrocnemius medially and the neurovascular bundle (popliteal artery, vein, tibial nerve) laterally. The popliteus muscle and its tendon are also identified. The semimembranosus insertion on the posterior tibia is a key landmark. The posterior capsule can be incised.
- Key Structures at Risk: Popliteal artery and vein, tibial nerve, saphenous nerve.
-
Posterolateral Approach (e.g., direct posterior approach):
- Indications: Fractures involving the posterolateral column (Luo type II or III), isolated posterior plateau fractures, sometimes used in conjunction with a lateral approach for complex Schatzker VI.
- Incision: Longitudinal incision centered over the posterolateral aspect of the knee.
- Internervous Plane: Between the biceps femoris (peroneal nerve) and the lateral head of gastrocnemius (tibial nerve).
- Dissection: Incise skin and subcutaneous tissue. Identify and protect the common peroneal nerve, which is usually retracted posteriorly with the biceps femoris. The lateral head of the gastrocnemius is retracted medially. The popliteus muscle and its tendon run across the posterolateral plateau.
- Key Structures at Risk: Common peroneal nerve, popliteal artery/vein (deeper).
- Dual Approaches: Often required for bicondylar fractures (Schatzker V, VI) to allow access to both medial and lateral columns. Can be performed simultaneously or staged, depending on soft tissue conditions. Minimizing skin bridges between incisions is important to prevent skin necrosis.
- Minimally Invasive/Arthroscopic-Assisted: For specific, less comminuted articular fractures (Schatzker I, II, III). Arthroscopy allows direct visualization of the articular surface, meniscal tears, and aids in accurate fragment reduction. Percutaneous screw fixation or limited plating can be performed.
Reduction and Fixation Technique (General Steps)
- Debridement and Lavage: For open fractures. For closed fractures, irrigate to remove hematoma and loose fragments.
- Visualization: Arthroscope or direct visualization of the articular surface via capsulotomy. Remove any meniscal interposition or entrapped fragments. Meniscal tears are addressed (repair vs. partial meniscectomy).
- Indirect Reduction: Apply traction (femoral distractor) and carefully manipulate the limb to restore overall alignment and distract fragments.
-
Direct Reduction of Articular Fragments:
- Split Fractures: Use reduction clamps, pointed reduction forceps, or joystick K-wires to reduce large split fragments to the intact articular segment.
- Depressed Fractures: Create a cortical window in the metaphyseal bone distal to the depressed fragment. Using an osteotome or bone tamp, elevate the depressed articular segment back to its anatomic position under direct visualization or fluoroscopic guidance. Temporary K-wires can hold the reduction.
- Bone Grafting: Fill the metaphyseal void created by elevation of depressed fragments with autogenous bone graft (e.g., from the iliac crest) or an allograft/synthetic bone graft substitute. This provides structural support and prevents secondary collapse.
-
Fixation:
- Articular Screws: Small fragment lag screws can be used to compress and stabilize articular fragments. Ensure screws are countersunk and do not penetrate the joint.
-
Buttress Plating:
Locking plates are the gold standard. They provide stable support, especially for depressed segments, and maintain reduction. Plates are anatomically contoured to the proximal tibia.
- Lateral Plate: Placed on the lateral aspect, providing buttress support for the lateral condyle.
- Medial Plate: Placed on the medial aspect, supporting the medial condyle.
- Posteromedial Plate: For posterior column fragments, placed via the posteromedial approach.
- Screw Length and Trajectory: Careful fluoroscopic control is essential to ensure screws do not violate the articular surface, are of adequate length, and engage sufficient bone.
- Diaphyseal Fixation: Ensure sufficient screws are placed in the tibial diaphysis distal to the fracture to achieve adequate working length and stiffness.
- Stability Assessment: Assess knee stability in flexion and extension, checking for any residual malalignment or instability.
- Closure: Meticulous layered closure, starting with the capsule, then deep fascia, subcutaneous tissue, and skin. Consider a drain if significant bleeding or dead space is present.
Complications & Management
Tibial plateau fractures carry a significant risk of complications, both early and late, which can impact functional outcomes. Proactive identification and management are crucial.
Early Complications
-
Surgical Site Infection (SSI):
Incidence ranging from 2-10%.
- Management: Superficial infections may respond to antibiotics and wound care. Deep infections typically require surgical debridement, antibiotic therapy (often culture-guided), negative pressure wound therapy, and potentially implant removal (in chronic cases) or staged reconstruction.
-
Wound Dehiscence/Necrosis:
Particularly common with high-energy injuries, extensive soft tissue dissection, or poor skin bridges in dual approaches.
- Management: Local wound care, serial debridement, negative pressure wound therapy, and potentially reconstructive surgery (e.g., rotational flaps, free tissue transfer).
-
Compartment Syndrome:
Incidence 5-15% in high-energy fractures. Presents with the "6 P's": pain (disproportionate), paresthesia, pallor, paralysis, pulselessness, poikilothermia.
- Management: Emergent fasciotomy of all four compartments is indicated when compartment pressures exceed 30-40 mmHg or within 30 mmHg of diastolic blood pressure.
-
Neurovascular Injury:
-
Peroneal Nerve Palsy:
Incidence 1-10%. Often traction-related neuropraxia.
- Management: Observation for spontaneous recovery. Nerve exploration and repair may be considered for complete lesions or if no recovery within 3-6 months. Tendon transfers may be necessary for chronic foot drop.
-
Popliteal Artery Injury:
Rare (<1%), but limb-threatening.
- Management: Emergent vascular repair by a vascular surgeon. Prioritize revascularization; fracture stabilization may be temporarily deferred or achieved with external fixation.
-
Peroneal Nerve Palsy:
Incidence 1-10%. Often traction-related neuropraxia.
-
DVT/Pulmonary Embolism (PE):
Risk is comparable to other major lower extremity trauma.
- Management: Prophylaxis with anticoagulants (pharmacologic and mechanical) and early mobilization.
-
Malreduction/Loss of Reduction:
Inadequate articular congruity or axial alignment post-operatively.
- Management: Early revision ORIF if significant malreduction is identified.
Late Complications
-
Post-Traumatic Arthritis (PTA):
The most common long-term complication, occurring in 20-50% of patients, even with seemingly anatomic reduction. Correlated with residual articular step-off, persistent malalignment, meniscal loss, and severity of initial cartilage injury.
- Management: Non-surgical (activity modification, bracing, NSAIDs, viscosupplementation) for mild symptoms. Surgical options include corrective osteotomy for malalignment, arthroscopic debridement, or ultimately, total knee arthroplasty (TKA) or arthrodesis for end-stage arthritis.
-
Stiffness/Loss of Range of Motion (ROM):
Occurs in 20-40% of patients due to prolonged immobilization, capsular contracture, or heterotopic ossification.
- Management: Aggressive physical therapy, manipulation under anesthesia, arthroscopic or open lysis of adhesions (arthrofibrosis).
-
Malunion/Nonunion:
Failure of fracture healing or healing in an unacceptable position.
- Management: Revision ORIF with bone grafting for nonunion. Corrective osteotomy for symptomatic malunion.
-
Hardware Prominence/Failure:
Symptomatic hardware may require removal (10-20%). Hardware failure can indicate nonunion or inadequate fixation.
- Management: Hardware removal if symptomatic after fracture healing. Revision fixation for hardware failure with nonunion.
-
Residual Instability:
Due to unaddressed or failed repair of associated ligamentous injuries.
- Management: Ligament reconstruction.
- Chronic Pain: Can result from PTA, nerve injury, or soft tissue scarring.
| Complication | Incidence (%) (Range) | Salvage Strategies |
|---|---|---|
| Early Complications | ||
| Surgical Site Infection | 2-10% | Debridement, targeted antibiotics, negative pressure wound therapy, flap coverage, implant removal (if chronic); staged reconstruction. |
| Compartment Syndrome | 5-15% | Emergent fasciotomy. |
| Peroneal Nerve Palsy | 1-10% | Observation (neuropraxia); nerve exploration/repair; tendon transfers for chronic foot drop. |
| Popliteal Artery Injury | <1% | Emergent vascular consultation and repair; temporary external fixation for fracture stabilization. |
| Malreduction / Loss of Reduction | 5-10% | Early revision ORIF. |
| Late Complications | ||
| Post-Traumatic Arthritis | 20-50% | Activity modification, bracing, NSAIDs, viscosupplementation, osteotomy, arthrodesis, total knee arthroplasty (TKA). |
| Stiffness / ROM Loss | 20-40% | Aggressive physical therapy, manipulation under anesthesia, arthroscopic or open lysis of adhesions. |
| Malunion / Nonunion | 5-20% | Corrective osteotomy for symptomatic malunion; revision ORIF with bone grafting and stable fixation for nonunion. |
| Hardware Prominence / Failure | 10-20% | Symptomatic hardware removal after fracture union. Revision fixation for hardware failure in nonunion. |
| Residual Ligamentous Instability | Variable | Non-operative management with bracing and rehabilitation; surgical ligament reconstruction. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is crucial for optimizing functional recovery, preventing stiffness, and minimizing the risk of secondary complications. Protocols are individualized based on fracture stability, fixation achieved, bone quality, and associated soft tissue injuries.
Phase I: Immediate Post-Operative (Weeks 0-6)
- Goals: Protect fixation, control pain and swelling, initiate gentle range of motion, maintain soft tissue integrity.
- Weight Bearing: Non-weight bearing (NWB) on the operative extremity using crutches or a walker. Touch-down weight bearing (TDWB) may be allowed for very stable fixation in compliant patients.
-
Range of Motion (ROM):
- Early Motion: Continuous passive motion (CPM) machine may be initiated, typically 0-30 degrees initially, progressing as tolerated.
- Passive ROM: Gentle passive knee flexion and extension within protected ranges (e.g., 0-90 degrees) several times daily, avoiding stress on the fracture site. Gravity-assisted exercises can be helpful.
- Active-Assist/Active ROM: Progress to active-assist and active ROM as tolerated, emphasizing quadriceps and hamstring sets (isometric exercises).
- Protection: Knee brace or immobilizer locked in extension for transfers and sleep, or when outside of therapy, particularly for unstable fracture patterns or bicondylar injuries.
- Pain & Swelling Management: Ice, elevation, analgesics.
- Wound Care: Monitor incision for signs of infection or dehiscence.
Phase II: Progressive Weight Bearing and Strengthening (Weeks 6-12)
- Goals: Gradual increase in weight bearing, restore full range of motion, begin strengthening.
- Weight Bearing: Progressive weight bearing (PWB) based on radiographic signs of healing and clinical stability. Start with 25% PWB, advancing by 25% every 1-2 weeks as tolerated, with a goal of full weight bearing (FWB) by 12 weeks.
- Range of Motion: Progress to full active ROM (0-130 degrees or greater). Manual therapy to address joint stiffness and soft tissue restrictions.
-
Strengthening:
- Isometric exercises (quadriceps sets, hamstring sets, gluteal sets).
- Light resistive exercises (e.g., heel slides, straight leg raises, prone knee flexion).
- Begin closed kinetic chain exercises (mini-squats, leg press) as weight bearing progresses, ensuring proper form.
- Proprioception/Balance: Initiate balance training (single-leg stance, wobble board) as appropriate.
- Cardiovascular: Non-impact activities (stationary bike with low resistance, swimming).
Phase III: Advanced Strengthening and Return to Activity (Weeks 12+)
- Goals: Restore full strength, endurance, power, and agility; gradual return to higher-impact activities.
- Weight Bearing: Full weight bearing.
- Range of Motion: Maintain full, pain-free ROM.
-
Strengthening:
- Progressive resistance exercises (PREs) targeting all major muscle groups of the lower extremity.
- Advanced closed kinetic chain exercises, step-ups, lunges.
- Plyometric exercises for power and agility, if appropriate for activity level.
- Functional Training: Agility drills, sport-specific drills, gait training with focus on normalizing mechanics.
- Return to Activity: Gradual return to work, recreational, or sporting activities, guided by strength, endurance, pain, and functional assessment. High-impact activities may be restricted for 6-12 months post-injury or longer, depending on the severity of the initial injury and the presence of any residual arthritis.
Key Considerations
- Bone Graft: If significant bone grafting was performed, protect the graft site and may require slower progression of weight bearing.
- Associated Injuries: Rehabilitation protocols must be modified if meniscal repairs or ligamentous reconstructions were performed concurrently.
- Patient Compliance: Emphasize the importance of adherence to protocols to prevent complications like stiffness or secondary displacement.
- Radiographic Monitoring: Serial radiographs monitor fracture healing and maintenance of alignment.
- Pain Management: Continuous assessment and adjustment of pain management strategies to facilitate participation in rehabilitation.
Summary of Key Literature / Guidelines
The understanding and management of tibial plateau fractures have evolved significantly with advancements in imaging, surgical techniques, and implant technology.
- Classification Systems: The Schatzker classification remains a cornerstone for initial assessment and communication, largely due to its simplicity and correlation with prognosis. However, for detailed surgical planning, the AO/OTA classification provides a more comprehensive, reproducible description, while Luo's 3-Column classification offers a practical guide for surgical approaches, particularly for complex posterior involvement.
- Surgical Timing: While early definitive fixation (within 2-3 weeks) is generally advocated to minimize soft tissue contracture and facilitate reduction, the critical determinant is the status of the soft tissue envelope. For high-energy injuries, the concept of "damage control orthopedics" is paramount, often involving temporary external fixation to allow soft tissue swelling to subside before definitive internal fixation (staged procedure). This approach has been shown to reduce wound complications and infection rates.
- Imaging: The advent of CT with 3D reconstruction has revolutionized pre-operative planning, offering unprecedented detail of articular depression, comminution, and fragment orientation, surpassing plain radiographs in accuracy. MRI is increasingly utilized to assess concomitant soft tissue injuries.
- Fixation Principles: The principles of anatomic articular reduction , restoration of mechanical axis, and stable internal fixation to permit early range of motion are consistently emphasized. Locking plate technology has significantly improved fixation stability, particularly in osteoporotic bone and comminuted fractures, reducing rates of loss of reduction. The use of bone graft or bone graft substitutes for metaphyseal defects is critical to prevent secondary collapse of the articular surface.
- Surgical Approaches: Modern literature supports tailored approaches based on fracture pattern (e.g., combined anterolateral and posteromedial approaches for bicondylar fractures with posterior involvement) to achieve direct visualization and reduction of all main fragments. Minimally invasive techniques and arthroscopic assistance are increasingly utilized for appropriate fracture types to reduce soft tissue morbidity.
- Complications: Post-traumatic osteoarthritis remains the most significant long-term complication, directly correlated with residual articular incongruity and associated cartilage/meniscal damage. Other major complications include infection, stiffness, and neurovascular injury.
- Rehabilitation: Current evidence supports early, controlled motion and progressive weight bearing protocols, individualized to the fracture stability and patient factors. This strategy aims to prevent stiffness and promote cartilage healing while protecting the surgical repair. Prolonged immobilization is generally discouraged.
The overarching goal, as highlighted in numerous academic reviews and clinical guidelines, is to achieve optimal long-term functional outcomes by prioritizing meticulous surgical technique, respecting the soft tissue envelope, and implementing structured rehabilitation programs. Continued research focuses on improving understanding of cartilage healing, optimizing implant design, and refining decision-making algorithms for complex fracture patterns.
You Might Also Like