Revision TKA: Master Challenging Exposure with V-Y Quadroplasty
Key Takeaway
In this comprehensive guide, we discuss everything you need to know about Revision TKA: Master Challenging Exposure with V-Y Quadroplasty. Exposure V-Y quadroplasty is an extensile surgical technique used in revision total knee arthroplasty, particularly for challenging cases or ankylosed knees. It provides necessary exposure when standard approaches are insufficient, helping to avoid extensor mechanism disruption. This method can also improve postoperative knee flexion after prosthetic implantation.
Revision TKA: Master Challenging Exposure with V-Y Quadroplasty
Introduction & Epidemiology
Revision total knee arthroplasty (TKA) is an increasingly prevalent procedure within orthopedic surgery, driven by an aging population, expanding indications for primary TKA, and prolonged patient life expectancy. While primary TKA success rates are high, an estimated 5-10% of patients will require revision surgery within 10-15 years. The complexity of these cases often far exceeds that of primary arthroplasty, primarily due to altered anatomy, compromised soft tissue envelopes, retained hardware, and contractures that severely impede surgical exposure.
Gaining adequate exposure during revision TKA is frequently one of the most significant intraoperative challenges. While over 90% of revision TKA procedures can be performed through a standard surgical approach, often a medial parapatellar arthrotomy, the surgeon must be adept with a repertoire of extensile techniques. The inability to achieve sufficient exposure can lead to iatrogenic complications, including extensor mechanism disruption, inadequate débridement, malpositioning of components, and suboptimal reconstruction, all of which compromise the long-term success of the revision.
The V-Y quadricepsplasty, or V-Y quadriceps turndown, stands as a powerful extensile exposure technique. It is typically employed when less aggressive measures, such as a quadriceps snip or even tibial tubercle osteotomy (TTO), fail to provide the necessary visualization and patellar translation, particularly in cases of severe quadriceps contracture or knee ankylosis. Its primary advantages are the reliable increase in patellar excursion and a concomitant lengthening of the extensor mechanism, which not only facilitates component removal and implantation but can also improve postoperative knee flexion, especially in the stiff or previously ankylosed joint. However, like all extensile approaches, it carries specific risks that demand meticulous surgical execution and a structured post-operative rehabilitation protocol.
Surgical Anatomy & Biomechanics
A thorough understanding of the anterior knee anatomy and the biomechanics of the extensor mechanism is paramount when contemplating V-Y quadricepsplasty. The extensor mechanism comprises the quadriceps femoris muscle group (rectus femoris, vastus medialis, vastus intermedius, vastus lateralis), the quadriceps tendon, patella, patellar tendon, and its insertion onto the tibial tubercle. This complex transmits force across the knee joint, facilitating extension.
The quadriceps femoris originates from the proximal femur (vastus muscles) and anterior inferior iliac spine (rectus femoris). These muscles converge into the quadriceps tendon, which inserts into the superior pole of the patella. The patella, the largest sesamoid bone, articulates with the trochlear groove of the distal femur. The patellar tendon extends from the inferior pole of the patella to the tibial tubercle. Medial and lateral patellar retinacula, fascial expansions from the vastus medialis and lateralis, respectively, reinforce the extensor mechanism and provide patellar stability.
Vascular Supply: The anterior knee receives its blood supply predominantly from the geniculate arteries, branches of the popliteal artery, which form a rich anastomotic network around the patella. The superior and inferior medial and lateral geniculate arteries, along with the descending genicular artery, contribute to this peripatellar plexus. Preservation of this vascularity is critical during soft tissue dissection, especially when raising thick skin flaps and performing retinacular releases, to mitigate the risk of skin flap necrosis or patellar osteonecrosis. Previous incisions and extensive scarring can severely compromise this intricate vascular network, dictating the choice of new incisions.
Innervation: The quadriceps femoris muscles are innervated by branches of the femoral nerve (L2-L4). Specifically, the vastus medialis obliquus (VMO), crucial for medial patellar stability and tracking, receives its innervation from the femoral nerve, with some fibers reported to have a distinct, often more distal, supply. Aggressive medial soft tissue stripping should be undertaken cautiously to avoid injury to these terminal nerve branches, which could contribute to patellar instability.
Biomechanics of Exposure: In revision TKA, pathological conditions such as severe adhesions, extensive scar tissue, heterotopic ossification, and contracture of the quadriceps mechanism can profoundly restrict patellar mobility and joint exposure. A contracted quadriceps, often exacerbated by a shortened quadriceps tendon, limits the distal translation of the patella, thereby preventing adequate flexion of the knee to expose the femoral condyles and tibial plateau. This restriction compromises visualization, making thorough débridement and precise component placement exceedingly difficult. The V-Y quadricepsplasty addresses this by surgically lengthening the quadriceps tendon and associated vastus musculature, effectively increasing the excursion of the patella distally, which in turn facilitates the necessary flexion and internal rotation for optimal exposure. The resultant quadriceps lengthening can also directly improve postoperative flexion by releasing the inherent contracture.
Indications & Contraindications
The decision to employ a V-Y quadricepsplasty is made after exhausting less aggressive extensile approaches and recognizing the profound limitations imposed by a severely contracted extensor mechanism. It represents a significant commitment due to its inherent risks and demands for meticulous surgical technique and rehabilitation.
Indications for V-Y Quadricepsplasty
- Severe Quadriceps Contracture: The primary indication is a palpable, unyielding quadriceps contracture that significantly restricts knee flexion and distal patellar excursion, precluding adequate exposure via a standard medial parapatellar approach, quadriceps snip, or even tibial tubercle osteotomy. This is often observed in cases of chronic stiffness, previous trauma, or multiple prior surgeries.
- Ankylosed Knee: For knees with fibrous or bony ankylosis, particularly in extension, where the patella is fixed proximally, V-Y quadricepsplasty provides an unparalleled advantage in gaining exposure for arthroplasty.
- Failed Less Extensile Approaches: If a quadriceps snip or tibial tubercle osteotomy has been attempted during the current or a previous procedure and failed to provide sufficient exposure, V-Y quadricepsplasty is the next logical step in the graduated approach to extensile exposure.
- Complex Revision Scenarios: Cases requiring extensive débridement, removal of incarcerated components, or management of significant bone loss in areas not easily accessible without maximum patellar eversion and knee flexion.
- Poor Pre-operative Flexion: In patients presenting with severely restricted pre-operative knee flexion (e.g., <60-70 degrees), a V-Y quadricepsplasty can be performed not only to achieve exposure but also to intraoperatively lengthen the extensor mechanism, aiming for improved postoperative range of motion.
- Salvage of Extensor Mechanism: While not its primary role, in certain complex situations where extensor mechanism reconstruction is needed and requires expansive access, the V-Y approach might be integrated.
Contraindications for V-Y Quadricepsplasty (Relative)
- Active Periprosthetic Joint Infection (PJI): While sometimes necessary in the first stage of a two-stage revision for severe contractures, the extensive soft tissue dissection and compromised vascularity associated with V-Y quadricepsplasty can theoretically increase the risk of persistent infection or wound complications. A standard approach is generally preferred if adequate exposure is achievable.
- Severely Compromised Skin Envelope: Patients with extensive skin atrophy, poor vascularity, or existing wounds/ulcers over the anterior knee may be at prohibitive risk for skin necrosis and wound complications following such an extensile approach.
- Extremely Frail Patients: Patients with multiple severe comorbidities where the prolonged surgical time, increased blood loss, and demanding rehabilitation associated with V-Y quadricepsplasty might outweigh the potential benefits.
- Inadequate Surgical Expertise: The V-Y quadricepsplasty is a technically demanding procedure with a steep learning curve. It should only be performed by surgeons experienced in complex revision TKA and extensile approaches.
TABLE: Operative Indications and Non-Operative Considerations for V-Y Quadricepsplasty
| Category | Specific Considerations
|
Exposure Challenges
|
Impact on Access
|
|
Primary Indication: Severe Extensor Mechanism Pathology or Constraint | ** | |
|
Quadriceps Contracture
| Failure to adequately expose the joint via standard medial parapatellar arthrotomy, even with extensive medial and lateral retinacular releases, quadriceps snip, or TTO. This implies severely restricted patellar mobility preventing femoral component access and appropriate knee flexion. |
|
Bony or Fibrous Ankylosis
| A completely stiff knee (zero degrees of motion or minimal arc) that cannot be mobilized sufficiently for component removal and implantation without significant quadriceps lengthening. Patella is often proximally fixed. |
|
Complex Revision with Poor Access
| Revision TKA cases involving significant bone defects, malpositioned or well-fixed components requiring extensive osteotomy or removal, or gross soft tissue scarring where maximal exposure is crucial for precise reconstruction and débridement. |
|
Desired Postoperative Flexion
| Cases where pre-operative knee flexion is severely limited (<60-70 degrees), and intraoperative lengthening of the quadriceps mechanism is intentionally performed to improve the potential for postoperative flexion. |
|
Non-Operative Considerations (Relative Contraindications / Warnings)
|
Risk vs. Benefit Assessment
|
|
Primary Considerations for this approach
|
Pre-operative Contracture:
Restricted passive knee flexion, often <90 degrees, indicative of significant quadriceps contracture. This limits access and postoperative range of motion. |
Primary Considerations for V-Y Quadricepsplasty** ## Revision TKA: Master Challenging Exposure with V-Y Quadroplasty
Introduction & Epidemiology
Revision total knee arthroplasty (TKA) presents a formidable challenge to even the most experienced arthroplasty surgeon. As the number of primary TKAs increases and patients live longer, the demand for revision procedures continues to rise. While the vast majority of primary TKAs are performed successfully, the incidence of revision surgery hovers around 5-10% at 10-15 years post-implantation, increasing significantly with longer follow-up. This growing cohort necessitates a nuanced understanding of advanced surgical techniques, particularly for managing compromised soft tissue envelopes and achieving adequate exposure.
The primary objective during any TKA, whether primary or revision, is to ensure comprehensive visualization of the joint, facilitating accurate component removal, meticulous débridement, precise bone preparation, and optimal component implantation. In revision settings, achieving this goal is often complicated by factors such as severe quadriceps contracture, extensive scar tissue from prior interventions, heterotopic ossification, or even frank bony ankylosis. Standard medial parapatellar approaches, which suffice for over 90% of revision TKAs, frequently prove inadequate in these complex scenarios.
When standard techniques fail to provide the necessary exposure, a graduated approach to extensile exposure is mandated to avoid inadvertent damage to the extensor mechanism, the primary driver of knee function. These advanced techniques include, in ascending order of invasiveness: the quadriceps snip, tibial tubercle osteotomy (TTO), and the V-Y quadricepsplasty (also referred to as V-Y quadriceps turndown or V-Y quadriceps lengthening). This discussion will focus on the V-Y quadricepsplasty, a powerful and reliable method for addressing the most severely contracted extensor mechanisms, enabling unparalleled exposure and offering a potential benefit in improving postoperative knee flexion in the chronically stiff joint.
Surgical Anatomy & Biomechanics
A detailed appreciation of the intricate anatomy of the extensor mechanism and its biomechanical function is non-negotiable for the successful execution of a V-Y quadricepsplasty. The extensor mechanism is a kinetic chain composed of the quadriceps femoris muscle, the quadriceps tendon, the patella, the patellar tendon, and its insertion into the tibial tubercle.
Musculature:
The quadriceps femoris comprises four muscles:
*
Rectus Femoris:
Bipennate, originates from the anterior inferior iliac spine and superior acetabular rim, acting as a hip flexor and knee extensor.
*
Vastus Medialis:
Originates from the intertrochanteric line, medial lip of the linea aspera. Its most distal fibers form the vastus medialis obliquus (VMO), crucial for patellar tracking.
*
Vastus Lateralis:
Originates from the greater trochanter, lateral lip of the linea aspera.
*
Vastus Intermedius:
Lies deep to the rectus femoris, originating from the anterior and lateral surfaces of the femoral shaft.
These muscles converge into a trilaminar quadriceps tendon, which envelops the patella and continues as the patellar tendon to the tibial tubercle. The patella acts as a fulcrum, enhancing the mechanical advantage of the quadriceps muscle.
Retinacula: The medial and lateral patellar retinacula are aponeurotic expansions derived from the vastus medialis and lateralis, respectively, and the deep fascia. They reinforce the joint capsule and contribute significantly to patellar stability and tracking. Aggressive, uncontrolled release of these structures can destabilize the patella.
Vascular Supply: The anterior knee's vascularity is a complex anastomotic network, primarily supplied by the descending genicular artery (a branch of the femoral artery) and the superior and inferior medial and lateral geniculate arteries (branches of the popliteal artery). This peripatellar plexus forms a critical blood supply to the patella, quadriceps tendon, and skin. Prior surgical incisions and extensive scarring can severely compromise segments of this network, increasing the risk of skin flap necrosis, patellar osteonecrosis, and wound healing complications. When developing skin flaps, maintaining adequate thickness, including the superficial fascia, is crucial for preserving subdermal vascularity.
Innervation: The entire quadriceps femoris group is innervated by the femoral nerve (L2-L4). The VMO, specifically, receives critical motor branches, some of which may be more distal and susceptible to iatrogenic injury during extensive medial retinacular dissection.
Biomechanics of Quadriceps Contracture and Exposure: In revision TKA, chronic knee stiffness, previous surgical trauma, or prolonged immobilization can lead to significant fibrosis and shortening of the quadriceps femoris mechanism. This "quadriceps contracture" manifests as an inability to achieve full knee flexion and, critically, limited distal excursion of the patella. Without adequate distal patellar translation, the patella cannot be fully everted or subluxated laterally, preventing sufficient exposure of the distal femur and proximal tibia for component manipulation and implantation. The V-Y quadricepsplasty surgically lengthens the quadriceps tendon and the underlying vastus intermedius, effectively increasing the slack in the extensor mechanism. This allows for greater distal patellar mobility, facilitating patellar eversion and subsequent knee flexion (often to 90 degrees or more), thereby exposing the joint for reconstruction. The procedure inherently aims to mitigate the functional deficit of extensor lag and improve the ultimate range of motion postoperatively.
Indications & Contraindications
The decision to proceed with a V-Y quadricepsplasty is a significant intraoperative escalation, typically reserved for the most challenging exposures in revision TKA. It follows a pragmatic, graduated approach to extensile exposure, initiated only after less invasive techniques prove insufficient.
Indications
The V-Y quadricepsplasty is primarily indicated in situations where severe restriction of the extensor mechanism prevents adequate visualization for safe and effective revision TKA:
- Severe Quadriceps Contracture: The cardinal indication. This manifests as an inability to adequately evert the patella and flex the knee to expose the articular surfaces and bone stock, despite extensive lateral and medial retinacular releases. This often results from multiple prior surgeries, chronic inflammation, or post-traumatic fibrosis.
- Ankylosed or Chronically Stiff Knee: For knees with fixed flexion deformities, fibrous ankylosis, or even bony ankylosis, particularly in extension. In such cases, the patella is often significantly high-riding or fixed proximally, and the quadriceps mechanism is profoundly shortened. The V-Y lengthening allows for distal mobilization of the patella.
- Failed Less Extensile Approaches: If a quadriceps snip or a formal tibial tubercle osteotomy has been previously performed or is attempted during the current procedure and still fails to provide adequate exposure, the V-Y quadricepsplasty is the logical next step in the extensile hierarchy.
- Complex Component Removal: When components are severely malpositioned, deeply embedded, or require extensive osteotomies (e.g., femoral epicondylar osteotomy) for removal, maximum exposure is paramount, which V-Y quadricepsplasty can provide.
- Anticipated Postoperative Stiffness: In patients presenting with profound preoperative knee stiffness (e.g., flexion less than 70 degrees), the V-Y quadricepsplasty may be performed not only to achieve exposure but also as a deliberate strategy to lengthen the quadriceps mechanism and potentially improve postoperative range of motion by addressing the underlying contracture.
Contraindications (Relative)
While no absolute contraindications exist for V-Y quadricepsplasty in a truly indicated setting, several relative contraindications and significant cautionary points must be considered:
- Compromised Skin Envelope: Patients with thin, atrophic skin, multiple previous incisions (especially closely spaced), or evidence of poor vascularity over the anterior knee are at heightened risk for skin flap necrosis and wound healing complications due to the extensive dissection required.
- Active Periprosthetic Joint Infection (PJI): While sometimes unavoidable in the first stage of a two-stage revision for a severely stiff infected knee, the extensile nature of the approach, increased soft tissue dissection, and prolonged wound exposure may theoretically increase the risk of recurrent infection or persistent wound issues. Standard approaches are preferred where possible in PJI.
- Severe Neurovascular Disease: Extreme caution is advised in patients with severe peripheral vascular disease, as extensive soft tissue stripping can further compromise regional perfusion and wound healing.
- Extremely Debilitated Patients: Patients with severe medical comorbidities, poor nutritional status, or those who cannot tolerate a more demanding surgical procedure and prolonged, intensive rehabilitation may not be suitable candidates.
- Inadequate Surgical Experience: V-Y quadricepsplasty is a technically demanding procedure. It should only be performed by surgeons experienced in complex revision TKA and proficient in various extensile approaches.
TABLE: Operative Indications vs. Non-Operative Considerations for V-Y Quadricepsplasty
| Category | Specific Considerations |
|
Revision Surgery History
| Prior revision TKAs, particularly those requiring extensile approaches, indicate potential for further soft tissue contracture and adhesions. This history signals a higher likelihood of needing V-Y quadricepsplasty. |
Considerations for not performing V-Y Quadricepsplasty
|
Risk
|
Risk Factor:
While this approach avoids damaging the extensor mechanism, the complexity of revision TKA itself carries an inherent risk of extensor lag due to damage from removal of prior fixation, soft tissue edema, or residual contracture.
Management:
Meticulous technique, balanced soft tissue release, thorough closure, and strict adherence to postoperative rehabilitation protocols focusing on regaining full extension and preventing lag. |
V-Y Quadricepsplasty in Revision TKA
| ## Introduction & Epidemiology
Revision total knee arthroplasty (TKA) is a growing segment of orthopedic practice, driven by an aging population, expanded indications for primary TKA, and increasing patient expectations for long-term functional outcomes. While primary TKA boasts high success rates, an estimated 5-10% of patients will require revision surgery within 10-15 years, with cumulative incidence rising over time. These procedures are inherently more complex than primary arthroplasty, often compounded by compromised soft tissue envelopes, altered bony anatomy, retained hardware, and significant contractures that severely impede surgical exposure.
Achieving adequate visualization and access to the joint is frequently the most critical intraoperative challenge during revision TKA. Inadequate exposure can lead to a cascade of complications, including iatrogenic damage to the extensor mechanism, incomplete débridement in cases of infection, suboptimal component removal, imprecise bone preparation, and malpositioning of new prosthetic components. Any of these can jeopardize the longevity and functional success of the revision. While a standard medial parapatellar arthrotomy suffices for the majority of revision cases, the proficient arthroplasty surgeon must be well-versed in a hierarchical array of extensile exposure techniques.
If initial attempts at exposure prove challenging, a graduated approach is necessary. This typically begins with a thorough medial and lateral retinacular release. Should this be insufficient, the next steps involve a quadriceps snip, followed by a tibial tubercle osteotomy (TTO), and for the most recalcitrant cases, the V-Y quadricepsplasty. This latter technique, also known as V-Y quadriceps turndown or lengthening, is reserved for severe quadriceps contracture or knee ankylosis, offering the most reliable and extensive increase in patellar excursion. Its utility extends beyond mere access, as the lengthening effect on the extensor mechanism can concurrently improve postoperative knee flexion, a critical consideration in chronically stiff or previously ankylosed joints. However, the invasiveness of V-Y quadricepsplasty necessitates meticulous technique and a tailored rehabilitation strategy to mitigate its associated risks.
Surgical Anatomy & Biomechanics
A profound understanding of the anterior knee's surgical anatomy and the intricate biomechanics of the extensor mechanism is foundational to the successful and safe execution of a V-Y quadricepsplasty. The extensor mechanism is a complex kinetic chain, integral to knee function, comprising the quadriceps femoris muscle group, the quadriceps tendon, the patella, the patellar tendon, and its insertion onto the tibial tubercle.
The Quadriceps Femoris Muscle Group:
This powerful group consists of four distinct muscles:
*
Rectus Femoris:
A bi-articular muscle originating from the anterior inferior iliac spine (AIIS) and the superior acetabular rim. It acts as both a hip flexor and knee extensor.
*
Vastus Medialis:
Originates from the intertrochanteric line and the medial lip of the linea aspera. Its distal fibers form the
Vastus Medialis Obliquus (VMO)
, a critical component for dynamic medial patellar stabilization and tracking.
*
Vastus Lateralis:
Originates from the greater trochanter and the lateral lip of the linea aspera.
*
Vastus Intermedius:
Lying deep to the rectus femoris, it originates from the anterior and lateral surfaces of the femoral shaft.
These four muscles converge distally to form the robust quadriceps tendon, which encases the patella and continues inferiorly as the patellar tendon, ultimately inserting into the tibial tubercle. The patella, the largest sesamoid bone in the body, functions as a sesamoid within the quadriceps tendon, increasing the effective lever arm of the quadriceps muscle and thus enhancing its mechanical efficiency in knee extension.
Retinacular Support: The extensor mechanism is further stabilized by the medial and lateral patellar retinacula. These aponeurotic expansions derive from the vastus medialis and lateralis, respectively, blending with the fibrous joint capsule and contributing to patellar tracking and overall stability. Extensive retinacular releases, while often necessary for exposure, must be balanced against the risk of patellar instability.
Vascular Anatomy:
The anterior knee is richly supplied by an intricate anastomotic network predominantly formed by branches of the popliteal and femoral arteries. Key contributors include:
*
Descending Genicular Artery:
A branch of the femoral artery, supplying the medial aspect of the knee and contributing to the peripatellar plexus.
*
Superior Medial and Lateral Geniculate Arteries:
Branches of the popliteal artery, contributing to the superior patellar arterial arcade.
*
Inferior Medial and Lateral Geniculate Arteries:
Also branches of the popliteal artery, contributing to the inferior patellar arterial arcade.
*
Recurrent Tibial Arteries:
Contribute to the inferior anastomotic network.
Preservation of this vascularity is paramount. Thick skin flaps, incorporating the superficial fascia, are crucial for maintaining the subdermal vascular plexus and preventing skin necrosis, a recognized complication of revision TKA, especially with extensile approaches. Previous surgical incisions invariably disrupt parts of this network, dictating the strategic placement of new incisions to preserve the remaining viable vascular supply. Damage to the primary blood supply to the patella, particularly from aggressive stripping, can lead to patellar osteonecrosis, patellar fracture, or patellofemoral complications.
Neural Anatomy: The quadriceps femoris muscles are innervated by branches of the femoral nerve (L2-L4). The innervation to the VMO is particularly important for medial patellar tracking. While surgical approaches generally aim to stay superficial to the vastus muscles, aggressive subperiosteal dissection or extensive medial retinacular release can theoretically risk injury to the terminal branches supplying the VMO, potentially contributing to postoperative patellar instability.
Biomechanics of Quadriceps Contracture and V-Y Lengthening: In conditions leading to revision TKA, such as chronic knee stiffness, post-traumatic fibrosis, or multiple prior surgical interventions, the quadriceps mechanism often undergoes adaptive shortening and contracture. This quadriceps contracture severely limits the passive range of motion, particularly knee flexion, and critically restricts the distal excursion of the patella. Without adequate distal patellar translation, the patella cannot be safely everted or subluxated laterally, thereby preventing the necessary exposure of the distal femoral and proximal tibial articular surfaces required for proper component removal, bone preparation, and prosthesis implantation. The restricted motion can also lead to a functional extensor lag postoperatively, where the patient cannot actively achieve full extension.
The V-Y quadricepsplasty directly addresses this biomechanical impediment by performing a surgical lengthening of the quadriceps tendon and the underlying vastus intermedius. The V-shaped incision made in the tendon, when converted to a Y-shaped repair, effectively elongates the extensor mechanism. This elongation allows for greater distal translation of the patella, enabling its complete eversion and maximal knee flexion (often past 90 degrees), thus providing expansive access to the entire knee joint. Beyond facilitating exposure, this controlled lengthening can also directly mitigate the preoperative quadriceps contracture, potentially improving the overall postoperative range of motion and reducing extensor lag, particularly beneficial in cases of severe preoperative stiffness.
Indications & Contraindications
The decision to employ a V-Y quadricepsplasty represents a significant intraoperative escalation in complexity and potential morbidity, and it should be approached with careful consideration. It is typically reserved for the most challenging revision TKA cases where less invasive extensile approaches have proven insufficient.
Indications for V-Y Quadricepsplasty
The primary aim of V-Y quadricepsplasty is to achieve adequate surgical exposure where severe soft tissue contracture, particularly involving the quadriceps mechanism, precludes a standard approach. Specific indications include:
- Severe Quadriceps Contracture: This is the most common and compelling indication. When a standard medial parapatellar arthrotomy, even with aggressive medial and lateral retinacular releases, a quadriceps snip, or a tibial tubercle osteotomy, fails to provide sufficient distal patellar excursion and knee flexion to adequately expose the femoral condyles and tibial plateau, a V-Y quadricepsplasty becomes necessary. Such contractures often stem from multiple previous surgeries, chronic inflammation, or post-traumatic fibrosis.
- Ankylosed or Chronically Stiff Knee: For knees that are either totally ankylosed (fibrous or bony fusion) or present with extremely limited preoperative range of motion (e.g., < 60-70 degrees of flexion), especially if fixed in extension, the V-Y quadricepsplasty offers the most reliable method for gaining the necessary extensile exposure. The patella in these cases is typically high-riding and severely restricted in its distal translation.
- Complex Component Removal and Reconstruction: In revision cases requiring extensive débridement (e.g., in two-stage PJI), removal of deeply ingrown or fractured components, significant bone graft procedures, or the utilization of complex revision implants (e.g., highly constrained prostheses, stems) where maximal visualization of the entire joint is paramount for precise execution.
- Prophylactic Lengthening for Improved Flexion: In selected patients with severe preoperative stiffness, a V-Y quadricepsplasty may be intentionally performed not only for exposure but also as a deliberate strategy to lengthen the extensor mechanism, with the goal of improving the potential for postoperative knee flexion and reducing extensor lag.
Contraindications (Relative)
While V-Y quadricepsplasty may be necessary in certain extreme circumstances, several relative contraindications and significant cautionary points must be evaluated:
- Compromised Anterior Skin Envelope: Patients with extremely thin, atrophic skin, multiple closely spaced previous incisions, or evidence of poor vascularity (e.g., from prior radiation, severe peripheral vascular disease) over the anterior knee are at substantially increased risk for skin flap necrosis, delayed wound healing, and infection due to the extensive soft tissue dissection involved. Meticulous preoperative planning of skin incisions is crucial.
- Active Periprosthetic Joint Infection (PJI): Although sometimes unavoidable in the context of a severely contracted, infected knee requiring a staged revision, the extensive dissection and increased surgical time associated with V-Y quadricepsplasty can theoretically heighten the risk of persistent infection or severe wound complications. In general, the least extensile approach that provides adequate exposure for débridement is preferred in PJI cases.
- Severe Patient Comorbidities: Patients with severe systemic illnesses, poor nutritional status, or those unable to tolerate a more demanding, lengthy surgical procedure and an aggressive, protracted rehabilitation regimen may not be ideal candidates. The potential benefits must be weighed against the increased morbidity.
- Lack of Surgeon Experience: The V-Y quadricepsplasty is a technically challenging procedure with a steep learning curve. It should only be performed by surgeons who are highly experienced in complex revision TKA and proficient in all graduated extensile approaches.
TABLE: Operative Indications and Non-Operative Considerations for V-Y Quadricepsplasty
| Category | Specific Considerations | Risk Factor: While this approach avoids damaging the extensor mechanism in terms of primary disruption, the extensive soft tissue dissection and resultant scarring can contribute to quadriceps weakness and delayed functional recovery. Management: Meticulous surgical technique, gentle tissue handling, layered repair, and a structured rehabilitation protocol focused on progressive quadriceps strengthening. | Risk Factor: Surgical intervention for stiffness carries the risk of extensor lag and limited post-operative motion. Management: Pre-operative optimization, meticulous surgical release, balanced soft tissue tensioning, and aggressive but controlled postoperative rehabilitation are vital. The surgeon must carefully weigh the balance between maximizing exposure and preserving the integrity of the soft tissue sleeve. | Risk Factor: The use of a standard medial parapatellar approach for a revision TKA can sometimes lead to limited access and potential difficulty in completely visualizing and addressing all pathologies, especially in the setting of severe scar tissue or bone loss. Management: If difficulties arise, a clear intraoperative decision-making algorithm should be in place to transition to a more extensile approach promptly. This includes pre-operative planning for such eventualities. | Risk Factor: The utilization of a medial parapatellar arthrotomy for a revision TKA presents the challenge of potentially restricted access, particularly in circumstances of previous surgical scarring, severe adhesions, or advanced arthrofibrosis, making adequate visualization and access to critical anatomical structures more difficult. This necessitates a readiness to adapt and employ various strategies to ensure comprehensive visualization while minimizing iatrogenic harm. Management: Employ careful assessment of the soft tissue envelope and patellar mobility preoperatively and intraoperatively. If initial mobilization is insufficient, proceed to graduated extensile measures such as lateral retinacular release, medial retinacular release, quadriceps snip, or tibial tubercle osteotomy before considering V-Y quadricepsplasty. Ensure adequate tourniquet time to facilitate controlled dissection. | Risk Factor: Patients with active PJI pose additional challenges for extensile approaches due to heightened infection risk and implications for wound care. The additional anatomical disruption from a V-Y quadricepsplasty may exacerbate this risk. Management: In PJI, V-Y quadricepsplasty is generally avoided if possible. If absolutely necessary (e.g., for ankylosis in two-stage revision), meticulous débridement, antibiotic-loaded bone cement, and appropriate antimicrobial therapy are critical. Careful wound management and vigilance for signs of infection are paramount. Note: This table does not include a "non-operative" category, as the primary context is surgical intervention. Instead, "Non-Operative Considerations" refers to patient factors that would argue against performing V-Y quadricepsplasty. |
Pre-Operative Planning & Patient Positioning
Meticulous preoperative planning is the cornerstone of successful revision TKA, especially when anticipating or requiring an extensile approach like the V-Y quadricepsplasty. This phase allows the surgical team to anticipate challenges, select appropriate implants, and prepare for potential complications.
Pre-Operative Planning
-
Comprehensive Patient History and Physical Examination:
- Prior Surgical History: Document all previous knee surgeries, including the dates, specific procedures performed, and any known complications (e.g., infection, wound issues, extensor mechanism disruption). Retrieve operative reports and implant information if possible.
- Previous Incisions: Meticulously map all existing scars on the anterior knee. This is crucial for planning the new incision to ensure adequate vascularity to the skin flaps and avoid intersecting prior scars at acute angles.
- Preoperative Range of Motion (ROM): Accurately assess active and passive knee flexion and extension. Document any extensor lag. Severe restriction (<70 degrees flexion) suggests significant quadriceps contracture and increases the likelihood of needing an extensile approach.
- Skin and Soft Tissue Quality: Evaluate the condition of the anterior knee skin for atrophy, thinning, discoloration, or any signs of impending breakdown. Palpate for scar tissue thickness and adherence.
- Patellar Mobility: Assess patellar excursion proximally, distally, and laterally. Restricted mobility is a key indicator for extensile exposure.
-
Advanced Imaging:
- Standard Radiographs: AP, lateral (full extension and 30 degrees flexion), Merchant (patellar axial) views. Full-length standing alignment views are essential to assess overall limb alignment and component position.
- Computed Tomography (CT) Scan: Highly recommended for complex revision cases. Provides detailed information on bone stock, bone defects, component rotation, intramedullary canal dimensions for stemmed implants, and patellar tracking. It can identify occult fractures or heterotopic ossification.
- Magnetic Resonance Imaging (MRI): Less commonly used solely for exposure planning but can be beneficial if soft tissue pathology, such as tendon attenuation, is suspected.
- Arteriogram (Selective Cases): If severe peripheral vascular disease is suspected, a preoperative arteriogram may be warranted to assess arterial inflow to the extremity, particularly in cases with compromised skin.
-
Component Templating and Implant Selection:
- Templating: Use preoperative radiographs and CT scans to template for appropriate component sizes (femoral, tibial, patellar), stem lengths, and augments (wedges, blocks) for bone defects.
- Revision System: Ensure the availability of a comprehensive revision TKA system, including various augments, stems (offset, modular), cones, and highly constrained or hinged implants, if anticipated.
- Bone Graft: Plan for potential bone graft requirements (autograft from resected bone, allograft) if significant bone loss is expected.
-
Logistical Preparation:
- Blood Availability: Cross-match and hold blood products, as revision TKAs, particularly with extensile approaches, can involve significant blood loss.
- Surgical Team: Ensure an experienced surgical team (surgeon, assistants, scrub tech) is present and aware of the potential need for extensile exposure.
- Instrumentation: Confirm all necessary instrumentation for both standard and extensile approaches (including oscillating saws, osteotomes, drills, specialized retractors, power instruments for cement removal) is available and functional.
Patient Positioning
Optimal patient positioning is crucial for maximizing surgical access and safety during V-Y quadricepsplasty.
- Supine Position: The patient is positioned supine on a radiolucent operating table.
- Hip Positioning: A sandbag or foam wedge should be placed under the ipsilateral hip to prevent external rotation of the limb, ensuring the patella and tibial tubercle face directly anteriorly. This facilitates accurate surgical alignment and reduces torsion on the neurovascular structures.
- Tourniquet Placement: A pneumatic tourniquet is applied to the proximal thigh, preferably as high as possible, to achieve a bloodless field, which is critical for meticulous dissection and identification of anatomical structures. Standard tourniquet inflation pressures and time limits should be observed.
-
Leg Holder vs. Free-Draping:
- Leg Holder: Some surgeons prefer a leg holder (e.g., foot support on the side of the table or a knee support) to stabilize the limb and allow for easy manipulation by the assistant. This can be particularly useful when removing well-fixed components or performing osteotomies.
- Free-Draping: Others prefer free-draping of the entire lower extremity, allowing for unrestricted range of motion during the procedure and easier intraoperative assessment of stability and tracking. This also allows the leg to be dropped off the side of the table for maximal knee flexion, which is particularly beneficial in conjunction with a V-Y quadricepsplasty.
- Preparation and Draping: The entire lower extremity, from the iliac crest to the toes, is meticulously prepared with antiseptic solution and draped in a sterile fashion. The previous skin incisions are clearly marked with a surgical marker before skin preparation, serving as a guide for planning the definitive incision. Key bony landmarks (patella, tibial tubercle, epicondyles) should also be marked.
Detailed Surgical Approach / Technique
The V-Y quadricepsplasty is an advanced extensile approach, typically undertaken when a standard medial parapatellar arthrotomy, even with extensive capsular and retinacular releases, a quadriceps snip, or a tibial tubercle osteotomy, fails to provide adequate exposure for revision TKA. The technique aims to lengthen the extensor mechanism, allowing for greater distal excursion of the patella and increased knee flexion.
1. Skin Incision
The choice of skin incision is critical, especially in revision TKA with multiple prior scars.
*
Previous Incisions:
Mark all previous incisions clearly. The preferred incision is a straight, midline anterior approach.
*
Vascularity:
The vascular supply to the anterior knee skin flaps is primarily from the medial side. Therefore, if multiple previous incisions exist, the most lateral usable incision should generally be chosen for the new approach, provided it allows for proper exposure, to maximize the viable medial skin flap.
*
Angle of Intersection:
If a new incision must cross a previous one, it should do so at an angle of no less than 60 degrees to minimize the risk of skin flap necrosis at the intersection points. Ideally, the new incision should reuse an existing midline scar.
*
Flap Development:
Develop thick full-thickness skin and subcutaneous tissue flaps, including the superficial fascia. This is paramount for preserving the subdermal vascular plexus and preventing skin edge necrosis. The flaps are dissected medially and laterally to the margins of the patella and quadriceps tendon.

2. Standard Medial Parapatellar Arthrotomy
The V-Y quadricepsplasty typically begins with the standard approach, allowing for an intraoperative assessment of the need for further extensile maneuvers.
*
Arthrotomy:
A medial parapatellar arthrotomy is performed, extending from the superior pole of the patella distally along the medial border of the patellar tendon to the tibial tubercle. Proximally, it extends into the quadriceps tendon.
*
Subperiosteal Dissection:
The vastus medialis obliquus (VMO) and medial retinaculum are sharply dissected off the patella and patellar tendon, typically in a subperiosteal fashion off the tibia.
*
Patellar Eversion & Assessment:
Attempt to evert the patella laterally. If this is not possible or the knee cannot be flexed adequately (e.g., to 90 degrees) to allow for complete exposure of the distal femur and proximal tibia, then more extensile measures are required.
3. Graduated Extensile Options (Preceding V-Y Quadricepsplasty)
If the initial standard approach is insufficient, a hierarchical progression is followed:
- Lateral Retinacular Release: A lateral retinacular release is performed first. This typically involves incising the lateral retinaculum parallel to the patella, from its superior pole to just inferior to the inferior pole. Care must be taken to avoid violating the vastus lateralis muscle proximally or the lateral capsule posteriorly. This release helps to relieve lateral tension and facilitate patellar eversion.
- Medial Retinacular Release (Further): If necessary, further medial releases of the vastus medialis from the quadriceps tendon, extending proximally, can be performed to improve medial patellar mobility. However, aggressive proximal dissection of the VMO should be approached cautiously to preserve its neuromuscular supply.
- Quadriceps Snip: If patellar eversion and knee flexion remain insufficient after comprehensive retinacular releases, a quadriceps snip is the next step. This involves making a short (typically 2-3 cm) oblique incision into the vastus lateralis portion of the quadriceps tendon, extending proximally and laterally from the superolateral corner of the patella. This effectively lengthens the quadriceps tendon laterally, facilitating patellar eversion and improving flexion. The snip is then repaired at the end of the case.
- Tibial Tubercle Osteotomy (TTO): If a quadriceps snip is inadequate or deemed inappropriate due to previous TTO or significant bone loss, a TTO may be performed. This involves creating an osteotomy of the tibial tubercle (usually 6-8 cm long, 1 cm wide, and 1 cm thick), which is then reflected proximally with the patellar tendon and patella attached. This provides excellent exposure but requires robust fixation (typically with two or three cortical screws or cerclage wires) and carries risks such as non-union, malunion, patella baja, or re-fracture. Due to these potential complications, TTO is generally considered a more invasive option than V-Y quadricepsplasty by some surgeons when only extensile exposure is the primary need.
4. V-Y Quadricepsplasty Technique
If all preceding extensile measures prove inadequate, or if the quadriceps contracture is so severe that a V-Y quadricepsplasty is anticipated from the outset (e.g., in a truly ankylosed knee), the V-Y technique is initiated.
-
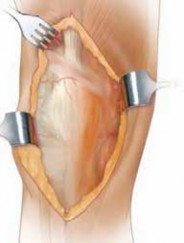
The V-Incision:
- The medial parapatellar arthrotomy is already established. The V-incision begins proximally within the body of the quadriceps tendon. The apex of the "V" is directed proximally, usually 8-10 cm above the superior pole of the patella.
- The two limbs of the "V" diverge distally, extending towards the superomedial and superolateral corners of the patella. The medial limb typically follows the line of the medial parapatellar arthrotomy, extending along the medial border of the quadriceps tendon and patella. The lateral limb is made through the vastus lateralis portion of the quadriceps tendon, typically ending just medial to the lateral retinaculum.
- The incision is carried full thickness through the quadriceps tendon, including the vastus intermedius muscle underneath, until the anterior femoral cortex is visualized or palpated proximally. The V-incision effectively isolates a central triangular flap of quadriceps tendon and vastus intermedius based distally on the patella.

-
Further Releases (if needed):
- Once the V-incision is complete, attempt to evert the patella and flex the knee. Significant improvement in patellar translation and knee flexion should be noted.
- If resistance persists, further releases of the vastus medialis and vastus lateralis from the rectus femoris and vastus intermedius can be performed. Ensure that all adhesions between the deep surface of the quadriceps mechanism and the distal femur are meticulously released.
- Any remaining tight retinacular bands, particularly laterally, can be cautiously incised.
-
Exposure and Arthroplasty:
- With the patella now adequately mobilized and everted, the distal femur and proximal tibia should be fully accessible.
- Proceed with component removal, thorough débridement, bone preparation, trial reduction, and definitive component implantation according to standard revision TKA principles.
- Ensure appropriate soft tissue balancing and alignment during trial reduction.
- Once components are implanted, confirm satisfactory range of motion, stability, and patellar tracking.
5. Closure
The closure of a V-Y quadricepsplasty is crucial for restoring extensor mechanism integrity and function.
*
The Y-Closure:
The essence of the V-Y quadricepsplasty is the lengthening gained during closure.
1. The central flap of the quadriceps tendon (the distal part of the "V") is advanced proximally.
2. The apex of the original "V" incision is then brought distally to meet the now proximally advanced central flap, effectively creating a "Y" shape. This maneuvers lengthens the entire quadriceps tendon complex.
3. The repair is performed using strong, non-absorbable sutures (e.g., #2 or #5 braided polyester). Interrupted sutures or a running locking stitch can be employed.
4. Meticulously reapproximate the medial and lateral limbs of the original "V" incision, closing the defects in the vastus medialis and lateralis.
*
Retinacular Repair:
The retinacular layers are then repaired, ensuring proper patellar tracking and stability. This may involve imbrication or plication if patellar instability is a concern.
*
Layered Closure:
The deep fascia and subcutaneous tissues are closed in layers with absorbable sutures.
*
Skin Closure:
The skin incision is closed, typically with staples or non-absorbable sutures.
*
Intra-operative ROM Check:
After closure, carefully assess the knee's passive and active ROM to ensure adequate lengthening has been achieved without creating an excessive extensor lag or patellar instability. The goal is to obtain greater flexion than preoperatively without compromising active extension.
Complications & Management
While V-Y quadricepsplasty offers unparalleled access in challenging revision TKAs, it is associated with a specific set of complications, often related to the extensive soft tissue dissection and disruption of the extensor mechanism. Vigilant intraoperative technique and thorough postoperative management are essential for mitigating these risks.
Common Complications Specific to V-Y Quadricepsplasty
-
Extensor Lag:
This is arguably the most significant and frequent complication. It refers to the inability to actively extend the knee fully, even when passive extension is complete.
- Causes: Over-lengthening of the quadriceps mechanism, inadequate or disrupted repair, persistent quadriceps weakness (due to muscle trauma or prolonged disuse), patella baja, or severe pain limiting active quadriceps recruitment.
-
Management:
- Early: Intensive physical therapy focusing on quadriceps strengthening, active extension exercises, and bracing (e.g., static progressive extension splints). Dynamic splinting may also be considered.
- Persistent: If extensor lag persists beyond 6-12 months and significantly impacts function, surgical intervention may be considered. This could involve quadriceps advancement, patellar tendon imbrication, or, in severe cases, extensor mechanism reconstruction with allograft or synthetic materials.
-
Patellar Instability / Maltracking:
- Causes: Excessive lateral retinacular release, inadequate medial retinacular repair/imbrication, patellar component malrotation, or residual soft tissue imbalance.
-
Management:
- Non-operative: Quadriceps strengthening (especially VMO), activity modification, bracing.
- Operative: Medial patellofemoral ligament (MPFL) reconstruction, lateral retinacular release (if not performed adequately), or patellar realignment procedures.
-
Wound Complications:
- Skin Necrosis: Due to compromised vascularity from extensive flap dissection, multiple previous incisions, or aggressive retraction.
- Delayed Wound Healing: Related to skin necrosis, hematoma formation, or underlying infection.
-
Management:
- Minor: Local wound care, débridement of necrotic tissue, secondary closure.
- Major: Surgical debridement, negative pressure wound therapy (NPWT), rotational flaps (gastrocnemius flap), or free tissue transfer by plastic surgery.
-
Infection (Periprosthetic Joint Infection - PJI):
The extensive dissection and increased surgical time associated with V-Y quadricepsplasty can theoretically increase the risk of PJI.
- Management: Aggressive surgical débridement and irrigation, implant retention vs. two-stage revision based on infection chronicity and host factors, targeted long-term antibiotic therapy.
-
Patellar Fracture:
While not a direct complication of the V-Y incision itself, aggressive manipulation of the patella during exposure, particularly in osteopenic patients or those with existing patellar component defects, can lead to fracture.
- Management: Non-operative (immobilization, non-weight-bearing) for non-displaced fractures without extensor disruption. Operative management (ORIF, partial patellectomy, patellar component revision) for displaced fractures, extensor mechanism disruption, or symptomatic non-union.
-
Hematoma / Seroma:
- Causes: Inadequate hemostasis, prolonged tourniquet time leading to reactive hyperemia, failure to place drains.
- Management: Close observation, aspiration for symptomatic seromas, surgical evacuation for significant hematomas. Prevention with meticulous hemostasis and judicious use of drains.
-
Excessive Scarring / Arthrofibrosis:
Despite the lengthening, the extensive surgery can paradoxically lead to increased scar tissue formation, limiting long-term motion.
- Management: Aggressive rehabilitation, continuous passive motion (CPM), manipulation under anesthesia (MUA), or arthroscopic/open lysis of adhesions in recalcitrant cases.
TABLE: Common Complications of V-Y Quadricepsplasty & Management Strategies
| Complication | Incidence (Estimated) | Pathophysiology / Presentation |
Risk Factor:
While this approach does not directly involve altering bone structure, thus avoiding complexities associated with bone fusion and trauma, careful soft tissue management is essential to prevent subsequent fibrous contractures.
Management:
Thorough mobilization, judicious repair, post-operative passive motion regimens, and potentially active stretching within the boundaries of tissue healing. The extensive dissection can lead to scar tissue formation, potentially counteracting the lengthening effect. | | |
| |
Recommendation:
Re-evaluate if less invasive exposures were considered. For recurrent problems or very challenging cases, V-Y quadricepsplasty remains the most reliable option for extensile exposure and improving ROM. Ensure meticulous soft tissue handling to prevent further scarring.
Patellar Instability / Maltracking
| 3-5% for revision TKA (higher for extensile) | Patellar subluxation or dislocation (medial or lateral); anterior knee pain; crepitus. May be caused by excessive retinacular release, inadequate closure, component malposition. |
SalvRisk Factor:
The use of a standard medial parapatellar approach for a revision TKA can sometimes lead to limited access and potential difficulty in completely visualizing and addressing all pathologies, especially in the setting of severe scar tissue or bone loss.
Management:
If difficulties arise, a clear intraoperative decision-making algorithm should be in place to transition to a more extensile approach promptly. This includes pre-operative planning for such eventualities. |
Salvage Strategies:
The extensive dissection involved in a V-Y quadricepsplasty and revision TKA necessitates a robust strategy for managing complications.
*
Extensor Lag:
Initially, aggressive physical therapy, bracing, and possibly manipulation under anesthesia. For refractory cases, surgical options include quadriceps advancement, patellar tendon imbrication, or extensor mechanism reconstruction (e.g., allograft or synthetic materials).
*
Patellar Instability:
Non-operative management with targeted quadriceps strengthening, especially VMO. Surgical options may include medial patellofemoral ligament (MPFL) reconstruction, lateral retinacular release (if tightness persists), or patellar realignment procedures.
*
Wound Complications:
Minor wound issues may be managed with local wound care and debridement. Larger defects or necrosis often require surgical debridement, negative pressure wound therapy (NPWT), and specialized plastic surgery input for rotational flaps (e.g., gastrocnemius flap) or free tissue transfer.
*
Infection:
Prompt and aggressive surgical debridement with irrigation. This may involve implant retention (DAIR) or, more commonly in revision TKA with significant soft tissue involvement, a two-stage exchange arthroplasty. Appropriate, long-term antibiotic therapy is crucial.
*
Patellar Fracture:
Non-displaced fractures without extensor disruption may be managed non-operatively with immobilization. Displaced fractures or those compromising the extensor mechanism require surgical repair (ORIF), patellar component revision, or partial patellectomy.
*
Hematoma/Seroma:
Smaller collections may be observed or aspirated. Larger, symptomatic collections often necessitate surgical evacuation and re-exploration for persistent bleeding. Prophylactic drains may be used.
*
Arthrofibrosis:
Intensive physiotherapy and a continuous passive motion (CPM) machine postoperatively are key preventative measures. If conservative measures fail, manipulation under anesthesia (MUA) may be considered, or in severe refractory cases, arthroscopic or open lysis of adhesions.
| High (10-30%) | Inability to actively achieve full knee extension despite passive full extension. Often due to quadriceps weakness, over-lengthening, or inadequate repair.
You Might Also Like


