High-Energy Schatzker Type VI Tibial Plateau Fracture: Clinical Case Study & Diagnostics
Key Takeaway
Diagnosing a high-energy Schatzker Type VI tibial plateau fracture involves detailed clinical assessment, observing presentation, deformity, and neurovascular status. Comprehensive imaging, including X-rays and CT with 3D reconstructions, is vital. These diagnostics accurately characterize articular depression, comminution, and condylar widening, essential for precise classification and surgical planning.
Patient Presentation & History
A 42-year-old male presented to the Emergency Department following a high-energy motor vehicle collision. He was a restrained driver involved in a head-on impact, with reported direct impact to the lateral aspect of his left knee against the dashboard. He complained of severe pain, deformity, and inability to bear weight on the affected limb. There was no reported loss of consciousness or other immediate life-threatening injuries identified during the initial ATLS survey.
His past medical history was notable for well-controlled hypertension on a single antihypertensive medication. He denied any history of smoking, alcohol abuse, or recreational drug use. His occupation involved manual labor.
Upon arrival, the limb was splinted in extension by paramedics. Initial vital signs were stable. He was alert and oriented. Pain was severe, rated 9/10 on a visual analogue scale despite pre-hospital analgesia.
Clinical Examination
Initial assessment focused on neurovascular status and open wounds, followed by a detailed orthopedic examination once the patient was stable and appropriately positioned.
-
Inspection:
- Gross deformity of the left knee joint with significant swelling, particularly around the proximal tibia.
- Ecchymosis was evident circumferentially, more pronounced laterally.
- Skin appeared taut and shiny, with early signs of skin creases effacement. No fracture blisters were noted at presentation, but were closely monitored.
- No open wounds were present, classifying it as a closed fracture.
- Leg length appeared slightly shortened due to proximal tibial collapse.
- Alignment appeared to be in valgus.
-
Palpation:
- Marked tenderness circumferentially over the proximal tibia, maximal at the tibial plateau.
- Crepitus was palpable with gentle manipulation, confirming bony instability.
- A significant knee effusion was present.
- Compartment assessment revealed soft, compressible compartments with no undue tension, although this was closely monitored throughout initial resuscitation.
-
Range of Motion (ROM):
- Grossly restricted and painful. The knee was held in approximately 10 degrees of flexion.
- Attempted passive range of motion elicited severe pain and guarding. Active motion was not attempted due to pain and instability.
-
Neurological Assessment:
- Peroneal nerve: Dorsiflexion of ankle (tibialis anterior) was 4/5, eversion of foot (peronei) was 4/5. Sensation in the first web space was intact. These findings indicated a mild neuropraxia or contusion rather than a complete deficit, likely due to traction or compression. Close monitoring was initiated.
- Tibial nerve: Plantarflexion of ankle (gastrocnemius-soleus complex) was 5/5, inversion of foot (tibialis posterior) was 5/5. Sensation over the sole of the foot was intact.
- Overall motor and sensory function distal to the knee was largely intact, albeit with the noted mild peroneal weakness.
-
Vascular Assessment:
- Femoral, popliteal, dorsalis pedis, and posterior tibial pulses were all palpable, strong, and symmetrical bilaterally.
- Capillary refill time in the toes was less than 2 seconds.
- No bruits or thrills were present. Ankle-brachial index (ABI) was not immediately performed but considered if pulses were equivocal.
The clinical picture was highly suggestive of a high-energy, bicondylar tibial plateau fracture with significant displacement and articular involvement, likely a Schatzker Type VI or AO/OTA 41-C3 fracture. The soft tissue envelope was deemed concerning, warranting careful management.
Imaging & Diagnostics
Following the initial clinical assessment, a comprehensive imaging workup was initiated.
-
Plain Radiographs:
- An initial series of radiographs of the left knee included anteroposterior (AP), lateral, and oblique views.
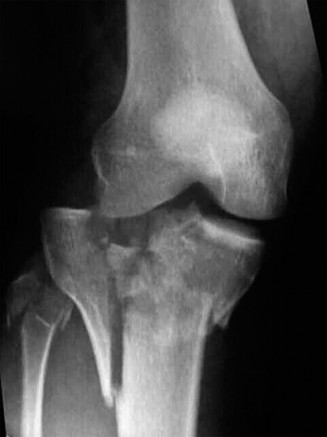
- AP View: Demonstrated severe comminution involving both medial and lateral tibial condyles. There was significant articular depression of both plateaus, with the lateral side appearing more depressed. Obvious condylar widening was noted, indicative of metaphyseal disruption. The medial plateau showed a large, displaced fragment.
- Lateral View: Highlighted multi-fragmentary fractures extending into the metaphysis, with posterior displacement of a significant portion of the plateau and significant articular depression. There was overall coronal and sagittal malalignment.
- Oblique Views: Confirmed the extent of comminution and helped delineate fragment orientation, particularly for the posterior aspects of the condyles.
- Initial plain film assessment suggested a Schatzker Type VI fracture, characterized by dissociation of the metaphysis and diaphysis, and significant bicondylar involvement.
-
Computed Tomography (CT) Scan:
- A CT scan of the left knee with 2mm cuts and 3D reconstructions was performed and was deemed essential for definitive characterization and pre-operative planning.
- Axial Views: Provided precise details of the articular surface involvement, confirming the comminution, and clearly demonstrating the extent of articular step-off (>10mm laterally, >5mm medially) and impaction. Identified the exact size and location of crucial articular fragments.
- Coronal Views: Showed the extent of condylar widening (approx. 15mm compared to contralateral side) and the amount of metaphyseal comminution. Articular depression was clearly quantifiable.
- Sagittal Views: Further characterized the posterior displacement and depression of the posterior articular segments, which were not fully appreciated on plain films. This also allowed for assessment of the posterior slope.
- 3D Reconstructions: Were invaluable for visualizing the overall fracture pattern, identifying key load-bearing columns, and planning surgical approaches and implant placement. They clearly demonstrated the split depression of both condyles, significant metaphyseal comminution, and the extension of fracture lines into the proximal tibia, consistent with an AO/OTA 41-C3 (complete articular, multifragmentary proximal tibia) classification. There was clear dissociation of the articular block from the diaphysis.
- Templating was performed using the CT images to identify optimal plate lengths, screw trajectories, and potential need for bone grafting material. The presence of a large metaphyseal void after reduction was anticipated.
-
Magnetic Resonance Imaging (MRI):
-
MRI was not indicated in the acute setting due to the clear bony pathology and the immediate need for surgical stabilization. However, it would be considered post-fixation if persistent instability or significant ligamentous injury was suspected, particularly if there was residual laxity after achieving stable bony fixation. For high-energy plateau fractures, significant soft tissue injuries (meniscal tears, cruciate or collateral ligament tears) are common, and their management might be deferred until bony healing progresses.

The image above shows a representative post-operative radiograph of a bicondylar tibial plateau fracture fixation, demonstrating anatomical reduction of the articular surface, restoration of mechanical axis, and stable dual-plate construct.
-
MRI was not indicated in the acute setting due to the clear bony pathology and the immediate need for surgical stabilization. However, it would be considered post-fixation if persistent instability or significant ligamentous injury was suspected, particularly if there was residual laxity after achieving stable bony fixation. For high-energy plateau fractures, significant soft tissue injuries (meniscal tears, cruciate or collateral ligament tears) are common, and their management might be deferred until bony healing progresses.
Differential Diagnosis
The clinical presentation and imaging findings strongly indicated a high-energy bicondylar tibial plateau fracture. However, in the context of high-energy knee trauma, other significant injuries must be considered and differentiated.
| Feature | High-Energy Bicondylar Tibial Plateau Fracture (Schatzker VI / AO 41-C3) | Distal Femur Fracture (AO 33-C3) | Knee Dislocation with Associated Avulsion Fractures (KD VI) |
|---|---|---|---|
| Primary Bony Lesion | Proximal tibia, involving both medial and lateral condyles, with metaphyseal-diaphyseal dissociation. | Distal femur, extending into the articular surface, multifragmentary. | Ligamentous disruption (ACL, PCL, collaterals) with secondary avulsion fractures of bony insertions. |
| Mechanism of Injury | High-energy axial load with severe valgus/varus, direct impact. E.g., MVC, fall from height. | High-energy direct trauma or rotational force. E.g., MVC, fall from height. | Extreme valgus/varus or hyperextension force. E.g., MVC, pedestrian struck. |
| Gross Deformity | Significant knee swelling, often valgus/varus deformity, joint line widening. | Significant knee swelling, often angulation of the thigh/knee. | Gross instability, obvious malalignment, sometimes reduced on scene. |
| Articular Involvement | Universal, severe depression and step-off of both tibial condyles. | Universal, severe depression and step-off of femoral condyles. | Variable, typically small avulsion fractures at ligamentous attachments (e.g., Segond, arcuate, intercondylar eminences). |
| Neurovascular Risk | High risk of peroneal nerve injury, compartment syndrome. Popliteal artery injury less common than in dislocation but possible. | Risk of popliteal artery injury (proximal fragment impingement), peroneal nerve injury. | Highest risk of popliteal artery injury (up to 50%), common peroneal nerve injury (up to 40%). |
| Radiographic Findings (X-ray) | Bicondylar fracture lines, metaphyseal comminution, articular depression, joint widening. | Supracondylar/intercondylar fracture lines, articular involvement of femur. | Wide joint space, possibly spontaneously reduced; small avulsion fragments; stress views show gross instability. |
| CT Findings | Defines extent of articular step-off, condylar widening, metaphyseal comminution, posterior involvement. Crucial for surgical planning. | Defines articular step-off, fragment orientation of femoral condyles, impaction. | Confirms ligamentous avulsions, assesses occult fractures. Useful to rule out major bony block. |
| MRI Indication | Often deferred acutely; used later for meniscal/ligamentous assessment if post-fixation instability. | Useful for meniscal/cartilage assessment if intra-articular extension. | Crucial for defining the extent and type of ligamentous damage (ACL, PCL, MCL, LCL, posterolateral corner). |
| Treatment Principle | Anatomical reduction of articular surface, restoration of mechanical axis and posterior slope, stable internal fixation. | Anatomical reduction of articular surface, restoration of mechanical axis, stable internal fixation. | Emergency reduction (if dislocated), vascular assessment (CTA), often external fixation initially, then staged ligamentous reconstruction. |
| Prognosis | High risk of post-traumatic arthritis, stiffness, malunion. | High risk of post-traumatic arthritis, stiffness, malunion. | High risk of instability, stiffness, OA, despite optimal treatment; depends on nerve/vessel injury. |
Surgical Decision Making & Classification
The decision to proceed with operative management for this patient was unequivocal due to several factors:
1.
High-energy mechanism and fracture morphology:
A bicondylar tibial plateau fracture with significant articular depression and condylar widening (Schatzker VI / AO 41-C3) inherently mandates surgical intervention to restore joint congruity and stability.
2.
Articular step-off:
Greater than 2-3 mm of articular step-off is a strong indication for surgery to minimize the risk of post-traumatic osteoarthritis. In this case, it was >10mm laterally and >5mm medially.
3.
Condylar widening:
Greater than 5-10 mm of condylar widening results in significant joint incongruity and instability, necessitating surgical restoration of width. This patient had approximately 15mm of widening.
4.
Mechanical instability:
The fracture pattern indicated gross instability of the knee joint.
5.
Soft tissue status:
While the initial soft tissue envelope was concerning, it was closed and without established blisters, suggesting a window for intervention after swelling subsidence.
Non-operative management
is typically reserved for very specific scenarios:
* Stable, non-displaced, non-articular fractures (e.g., Schatzker I, some II with minimal depression).
* Non-ambulatory patients with severe comorbidities where the risks of surgery outweigh the benefits.
* Pilon-type fractures of the tibial plateau with extremely poor soft tissue that preclude any internal fixation, sometimes managed with circular external fixation as a definitive treatment. This was not the case here.
Fracture Classification:
*
Schatzker Classification:
This widely used system categorizes tibial plateau fractures based on fracture morphology and location. Our patient's fracture, with severe comminution involving both medial and lateral condyles, and metaphyseal-diaphyseal dissociation, falls into
Schatzker Type VI
. This type signifies a high-energy injury with a poor prognosis if not anatomically reduced and stably fixed.
*
Type I:
Lateral tibial plateau split fracture.
*
Type II:
Lateral tibial plateau split depression fracture.
*
Type III:
Lateral tibial plateau pure depression fracture.
*
Type IV:
Medial tibial plateau fracture.
*
Type V:
Bicondylar fracture without metaphyseal-diaphyseal dissociation.
*
Type VI:
Bicondylar fracture with metaphyseal-diaphyseal dissociation.
*
AO/OTA Classification:
This more comprehensive system uses alphanumeric codes.
*
41-C3:
This indicates a complete articular fracture (C) of the proximal tibia (41) that is multifragmentary (3). This aligns perfectly with the CT findings of extensive articular comminution, metaphyseal disruption, and dissociation from the diaphysis. This classification highlights the complexity and the need for meticulous surgical planning and execution.
Timing of Surgery:
Given the patient's severe swelling and the high-energy nature of the injury, a staged approach was chosen.
1.
Initial Stage (Day 0-2):
Application of a spanning external fixator from the distal femur to the tibia was performed in the operating room. This achieved provisional stability, protected the soft tissues, allowed for preliminary ligamentotaxis to restore length and some alignment, and facilitated daily wound care and compartment checks. The patient was kept NWB.
2.
Definitive Internal Fixation (Day 7-10):
The definitive surgery was scheduled once the soft tissue envelope had improved, indicated by a positive "wrinkle sign" and resolution of significant swelling and tension. This minimized the risk of wound complications, infection, and compartment syndrome.
Surgical Technique / Intervention
The definitive surgical intervention was performed on hospital day 8, after resolution of significant soft tissue swelling and a positive wrinkle sign.
-
Patient Positioning: The patient was positioned supine on a radiolucent table. A thigh tourniquet was applied to allow for a bloodless field. A bump was placed under the ipsilateral hip to bring the knee into a neutral position. The knee was positioned over a radiolucent triangle or small bolster, allowing for approximately 30-45 degrees of flexion to facilitate access to the posterior aspects of the condyles and improve visualization for fluoroscopy. Image intensification (C-arm) was positioned to allow for AP, lateral, and oblique views without repositioning the limb.
-
Surgical Approaches: Given the bicondylar nature of the fracture, dual incisions were necessary.
- Anterolateral Approach: A standard anterolateral incision, beginning approximately 2 cm lateral to the patellar tendon and extending distally from the joint line for about 10-12 cm. This approach allows access to the lateral tibial plateau, the anterolateral aspect of the metaphysis, and aids in visualization of the joint line. The fascia was incised, and the muscle belly of the tibialis anterior was elevated subperiosteally.
- Anteromedial Approach (modified): A slightly more posterior anteromedial incision was utilized to gain access to the posteromedial fragment. This incision started just posterior to the medial border of the patellar tendon, extending distally along the posteromedial aspect of the tibia. Care was taken to protect the saphenous nerve and vein. The pes anserinus was released or retracted. This approach allows for direct visualization of the medial plateau and posteromedial column, which is often a critical load-bearing structure. For our specific case, the large posteromedial fragment necessitated a slightly more posterior placement of this medial incision to optimize reduction and plate placement.
-
Reduction Techniques:
- Joint Distraction & Ligamentotaxis: Initial reduction was facilitated by distraction across the knee joint using the external fixator. This helped to restore overall length and indirectly reduce some of the major fragments via ligamentotaxis.
- Articular Reconstruction (Lateral Plateau First): The lateral approach was opened first. The lateral meniscus was inspected; if torn or detached, it was carefully protected or repaired. An osteotomy window through the lateral cortex was created just distal to the articular surface (or directly via the fracture line) to access the depressed articular fragments. Using a bone tamp or impactor, the depressed articular surface of the lateral plateau was elevated under direct vision and fluoroscopic guidance. This was the most critical step – restoring the articular congruity.
- Metaphyseal Void Grafting: Once the articular surface was elevated, the underlying metaphyseal void was filled with cancellous allograft bone (e.g., cancellous chips) or autograft (from the iliac crest if a large defect and patient allowed). This provided structural support to prevent secondary collapse.
- Temporary Fixation: The reduced articular fragments and underlying bone graft were provisionally stabilized with K-wires. Rafting screws were placed subchondrally, parallel to the joint line, to maintain the elevated articular segment.
- Medial Plateau Reconstruction: The medial incision was then opened. The medial meniscus was assessed. The large posteromedial fragment was reduced using direct manipulation, ball-spikes, and reduction clamps. The goal was to restore the articular surface and the integrity of the posteromedial column, ensuring correction of any valgus or varus deformity.
- Restoration of Width and Alignment: With both articular surfaces provisionally reduced, the overall condylar width and mechanical axis of the tibia were assessed under fluoroscopy using the contralateral limb as a template if possible. Reduction clamps and pointed reduction forceps were used to compress the metaphyseal fragments and restore anatomical width.
-
Fixation Construct:
- Lateral Plating: A pre-contoured locking plate (e.g., LCP Tibial Plateau Plate, Synthes) was applied to the anterolateral aspect of the tibia. This plate provided buttress support for the lateral condyle and bridged the metaphyseal comminution, achieving angular stability. Multiple locking screws were inserted into the condyle, ensuring adequate purchase in the rafting screws and elevated articular fragments. Distal screws were placed into the tibial shaft.
- Medial Plating: A second pre-contoured locking plate was applied to the posteromedial aspect of the tibia, typically a smaller buttress or locking plate (e.g., LCP Posteromedial Tibial Plateau Plate). This plate was crucial for buttressing the posteromedial fragment and neutralizing forces across the medial column, which is a major weight-bearing axis. Screws were carefully inserted to avoid neurovascular structures. In cases of severe comminution and dissociation, a minimally invasive percutaneous plate osteosynthesis (MIPPO) technique might be considered for the medial side to minimize soft tissue stripping, but direct open reduction was often preferred for direct visualization of the posteromedial fragment in this particular case.
- Lag Screws: Interfragmentary lag screws were used where appropriate to achieve compression across specific fracture lines before plate application, enhancing stability.
- Final Assessment: After both plates were secured, the construct was meticulously checked under fluoroscopy in multiple planes (AP, lateral, obliques) to confirm anatomical reduction, appropriate screw lengths, and stable fixation. The knee joint was put through a gentle range of motion to assess stability and ensure implants were not impinging.
-
Wound Closure: Hemostasis was achieved. Drains were placed if significant bleeding was anticipated. The deep fascia, subcutaneous tissue, and skin were closed in layers. A sterile dressing was applied, and the limb was immobilized in a knee immobilizer or hinged knee brace set to full extension.
Post-Operative Protocol & Rehabilitation
The post-operative protocol for a high-energy bicondylar tibial plateau fracture is prolonged and meticulously staged to optimize recovery while protecting the fixation.
-
Immediate Post-Operative Period (Day 0-7):
- Pain Management: Multimodal analgesia including regional blocks, oral opioids, and NSAIDs (if no contraindications) to manage severe post-operative pain.
- DVT Prophylaxis: Pharmacological prophylaxis (e.g., low molecular weight heparin) initiated and continued for at least 6 weeks, given the high risk of VTE in lower limb trauma.
- Wound Care: Daily wound checks for signs of infection, hematoma, or skin necrosis. Dressings changed as needed. Staples/sutures typically removed at 2-3 weeks.
- Swelling Control: Elevation of the limb, cryotherapy, and compression bandages to minimize swelling and improve soft tissue healing.
- Weight-Bearing: Strictly non-weight bearing (NWB) on the affected limb. Use of crutches or a walker for ambulation.
-
Range of Motion (ROM):
- Initiation of passive ROM using a continuous passive motion (CPM) machine or gentle physical therapy. The goal is to gradually increase flexion while protecting the extension block.
- Initially, limited to 0-30 degrees flexion for the first 2 weeks, then gradually progressed to 0-60 degrees over the next 4 weeks, provided fixation is stable. Full extension block is maintained to prevent posterior sag.
- Muscle Activation: Gentle isometric quadriceps and hamstring contractions to prevent atrophy, without causing joint motion. Ankle pumps to aid circulation.
-
Early Rehabilitation (Weeks 2-6):
- Weight-Bearing: Still strictly NWB.
- ROM: Continue with progressive passive and active-assisted ROM exercises. Aim for 0-90 degrees by 6 weeks. Emphasis on restoring knee extension.
- Strengthening: Initiate light isometric strengthening for quadriceps and hamstrings. Begin hip strengthening exercises.
- Brace: Patient typically continues to use a hinged knee brace locked in extension for ambulation, gradually progressing to allow for ROM during exercises.
-
Intermediate Rehabilitation (Weeks 6-12):
- Weight-Bearing: Gradual progression to partial weight-bearing (PWB) with crutches or walker, typically starting at 25% body weight, advancing as tolerated based on radiographic evidence of healing and pain levels. This phase is critical and guided by fracture stability and callus formation on X-rays.
- ROM: Continue to work towards full functional ROM.
- Strengthening: Progressive strengthening exercises for the entire lower kinetic chain, including closed-chain exercises as weight-bearing permits. Begin proprioception and balance training.
- Brace: May transition to brace only for ambulation or discontinue if stability is excellent.
-
Advanced Rehabilitation (Weeks 12-24+):
- Weight-Bearing: Progress to full weight-bearing (FWB) as tolerated, typically by 12-16 weeks for a complex fracture, once radiographs show good bony union.
- ROM: Continue to maximize ROM, addressing any stiffness.
- Strengthening: Advanced strengthening, functional exercises, sport-specific training (if applicable).
- Return to Activity: Gradual return to light activities by 4-6 months, with return to full activity (including demanding labor or sports) often taking 9-12 months or longer, depending on the severity of the injury and individual recovery.
-
Long-Term Follow-up: Regular clinical and radiographic follow-up to monitor for complications such as nonunion, malunion, infection, post-traumatic osteoarthritis, and implant-related issues. Hardware removal is typically considered 12-18 months post-op if symptoms warrant.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls:
- Pre-operative Planning is Paramount: A detailed CT scan with 3D reconstructions is non-negotiable. Spend adequate time templating plate positions, screw trajectories, and evaluating the soft tissue envelope. Understand the fracture pattern (Schatzker, AO/OTA) intimately.
- Respect the Soft Tissue Envelope: High-energy injuries often have significant soft tissue compromise. A staged approach with initial external fixation followed by delayed definitive internal fixation (once the "wrinkle sign" is present) is crucial to minimize wound complications, infection, and compartment syndrome.
- Anatomical Reduction of the Articular Surface: This is the sine qua non for preventing early post-traumatic osteoarthritis. Prioritize articular reduction and provisional fixation with K-wires and rafting screws before addressing metaphyseal stability. Use direct visualization through a limited arthrotomy or subchondral windows.
- Restore Mechanical Axis and Posterior Slope: Ensure the overall limb alignment is corrected. The posterior slope of the tibial plateau is critical for knee kinematics; excessive loss can lead to hyperextension or functional instability.
- Metaphyseal Support with Bone Graft: High-energy fractures often have significant metaphyseal defects after articular reduction. Filling these voids with structural (e.g., autograft from iliac crest) or cancellous (e.g., allograft chips, DBM) bone graft is essential to prevent secondary collapse of the articular surface.
- Stable Fixation Construct: For bicondylar fractures, dual plating (anterolateral and posteromedial) is often required to achieve a stable construct that can withstand early range of motion. Use locking plates for comminuted metaphyses.
- Intraoperative Ligamentous Assessment: After achieving stable bony fixation, gently assess the integrity of the collateral and cruciate ligaments. While not always addressed acutely, significant instability may warrant discussion for delayed reconstruction or bracing.
- Early, Controlled Rehabilitation: While weight-bearing is delayed, early passive and active-assisted range of motion is crucial to prevent stiffness and optimize cartilage nutrition, provided the fixation is robust.
Pitfalls:
- Ignoring Soft Tissue Status: Rushing to definitive fixation in the face of significant swelling, blisters, or a tense soft tissue envelope dramatically increases the risk of wound dehiscence, deep infection, and limb loss.
- Inadequate Articular Reduction: Failure to achieve an anatomical reduction of the articular surface (residual step-off >2mm) will invariably lead to accelerated post-traumatic osteoarthritis, pain, and poor functional outcomes.
- Insufficient Metaphyseal Support: Neglecting to graft or adequately support the metaphyseal void after elevating depressed articular fragments can lead to subsequent collapse of the plateau, loss of reduction, and malunion.
- Early Unrestricted Weight-Bearing: Premature weight-bearing on a complex, comminuted fracture with extensive metaphyseal bone loss can result in catastrophic failure of the fixation, hardware pull-out, and malunion.
- Missed Associated Injuries: Failure to recognize or address concomitant neurovascular injuries, compartment syndrome, or significant ligamentous injuries can severely compromise the final outcome. Meticulous initial and ongoing assessment is vital.
- Peroneal Nerve Palsy: The common peroneal nerve is susceptible to injury, particularly in lateral plateau fractures or those with significant valgus deformity. Careful exposure and protection are paramount. New or worsening deficit post-op requires immediate investigation.
- Compartment Syndrome: High-energy tibial plateau fractures carry a significant risk of acute compartment syndrome. Clinical vigilance (pain out of proportion, pain on passive stretch, paresthesia, pallor, pulselessness, paralysis) and timely fasciotomy are critical.
- Technical Errors: Incorrect plate placement, inadequate screw length/purchase, failure to restore the posterior slope, or implant impingement can all lead to poor outcomes. Fluoroscopy must be used generously in multiple planes.
You Might Also Like


