Complex Patellar Fracture: A Case Study in Surgical Management & Rehabilitation
Key Takeaway
High-energy patellar fractures require meticulous management, as demonstrated in this case study of a 45-year-old carpenter. Key considerations include assessing injury mechanism and clinical presentation to guide surgical repair. Post-operative rehabilitation is crucial to restore knee extensor mechanism function, ensuring optimal recovery for demanding occupations and preventing long-term disability.
Patient Presentation & History
Good morning, everyone. Today, we're going to examine a real-world scenario involving a patellar fracture that underscores critical decision-making, meticulous surgical technique, and comprehensive post-operative management. The patella, a pivotal component of the knee's extensor mechanism, significantly enhances the quadriceps muscle's mechanical advantage. Its superficial location, however, renders it highly susceptible to both direct and indirect trauma, leading to a diverse spectrum of fracture patterns.
Our case involves Mr. John Davies, a 45-year-old male, who presented to the emergency department following an acute, high-energy traumatic injury to his left knee. Mr. Davies is an otherwise healthy and active individual, gainfully employed as a skilled carpenter. His profession demands significant lower limb strength, full range of motion, and excellent balance for tasks such as climbing, kneeling, lifting heavy materials, and prolonged standing.
Mechanism of Injury
Mr. Davies reported that the injury occurred approximately two hours prior to his presentation while he was actively engaged in his work on a construction site. He was in the process of descending a scaffold from an approximate height of 1.5 meters when he inadvertently lost his footing. This resulted in an uncontrolled fall, during which he landed directly and forcefully onto his left flexed knee, striking the anterior aspect of his patella against a hard, unyielding surface.
Immediately following the impact, Mr. Davies experienced excruciating, sharp, and localized pain within his left knee. This pain was rapidly accompanied by the onset of significant swelling. Critically, he reported a profound and complete inability to bear any weight on the affected limb and, notably, could not actively extend his knee or perform a straight leg raise. Due to the severity of his symptoms and his inability to ambulate, he required direct assistance from his colleagues to be moved from the scene and was subsequently transported to our emergency department via ambulance. He explicitly denied any loss of consciousness, head trauma, or other concomitant injuries at the scene of the accident.
Demographics
- Age: 45 years
- Gender: Male
- Occupation: Carpenter. This occupation is highly physically demanding, requiring intact and robust knee function for tasks such as climbing ladders, prolonged kneeling, lifting heavy objects, and maintaining balance on uneven surfaces. The importance of achieving maximal functional restoration was paramount in his treatment planning.
- Dominance: Right-hand dominant.
Comorbidities & Past Medical History
- Medical History: Mr. Davies has a documented history of well-controlled essential hypertension. This condition is effectively managed with Amlodipine 5mg orally once daily, a regimen he has adhered to for the past three years. He denies any other significant medical comorbidities, specifically ruling out a history of diabetes mellitus, coronary artery disease, chronic kidney disease, chronic pulmonary disease, or any known rheumatological conditions. He reports no personal history of bleeding diathesis, coagulopathy, or any diagnosed osteopenia or osteoporosis, conditions that could potentially predispose him to fragility fractures or complicate surgical management.
- Surgical History: His surgical history is entirely unremarkable, with no prior orthopedic interventions or other major surgical procedures to date.
- Current Medications: Amlodipine 5mg orally once daily.
- Allergies: He reports no known drug allergies (NKDA).
- Social History: Mr. Davies is a non-smoker and reports only occasional, social consumption of alcohol. He lives independently with his family. His high motivation to return to his pre-injury functional status and, specifically, to his physically demanding occupation, was a significant factor considered during his treatment planning and guided the intensity of his subsequent rehabilitation protocol.
- Family History: His family history is non-contributory for any significant orthopedic conditions or inheritable systemic medical conditions.
Clinical Examination
Upon initial assessment in the emergency department, Mr. Davies was alert, oriented, and cooperative, despite clearly experiencing significant discomfort, rating his pain as 9/10 on a visual analog scale (VAS). His vital signs were stable and within physiological limits: Blood Pressure (BP) 130/80 mmHg, Heart Rate (HR) 78 bpm, Respiratory Rate (RR) 16 breaths/min, and Oxygen Saturation (SpO2) 98% on room air.
Inspection
The left lower limb was observed to be held in a natural, slightly flexed posture, specifically approximately 25-30 degrees of knee flexion. This position appeared to be one of maximal comfort for the patient or potentially a mechanical constraint due to the injury. There was pronounced and diffuse soft tissue swelling encompassing the entire knee joint, extending notably proximally into the suprapatellar pouch and distally over the patellar tendon. Significant ecchymosis was already well-developed around the entire knee joint, extending distally into the upper shin, indicative of substantial acute soft tissue hemorrhage.
A distinct, visible depression or 'sulcus' was noted across the mid-anterior aspect of the patella. This visible defect strongly suggested a palpable gap and underlying bony discontinuity of the patella, confirming a disruption of the extensor mechanism. Crucially, the skin overlying the patella and the surrounding knee joint remained entirely intact, classifying this injury as a closed fracture. There were no abrasions, lacerations, skin tenting, or any signs of impending skin compromise (e.g., blanching, severe tension) that would suggest an open injury or imminent soft tissue breakdown. No pre-existing muscle atrophy was present in the quadriceps or hamstrings, consistent with the acute nature of the injury in an otherwise active and muscular individual.
Palpation
- Tenderness: Exquisite, localized tenderness was elicited with even gentle palpation directly over the patella and along the medial and lateral peripatellar soft tissues. The patient exhibited significant guarding with any attempts at deeper palpation.
- Effusion: A large, tense suprapatellar and prepatellar effusion was distinctly palpable, consistent with an acute hemarthrosis within the knee joint capsule. While patellar ballottement was positive, the presence of multiple bony fragments made the test less definitive for pure fluid, as the fragments themselves could be balloted.
- Patellar Integrity: A clear, palpable transverse defect or gap was unequivocally felt across the mid-body of the patella through the edematous soft tissues. The superior pole fragment was palpably retracted proximally within the quadriceps tendon, driven by the pull of the quadriceps muscle. Conversely, the inferior pole fragment, although also comminuted, remained relatively fixed or slightly displaced distally, anchored by the patellar tendon. The margins of the fracture fragments were sharp and irregular to palpation.
- Extensor Mechanism Assessment: The quadriceps tendon was palpable proximally and appeared to be grossly intact at its musculotendinous junction. Similarly, the patellar tendon was intact at its insertion onto the tibial tubercle. However, the continuity of the patella itself, which serves as the central osseous component of the extensor mechanism, was clearly disrupted. The medial and lateral patellar retinacula were acutely tender to palpation, suggesting significant associated soft tissue injury and likely avulsion from the patellar fragments.
- Surrounding Structures: Focused palpation confirmed no significant tenderness over the medial or lateral joint lines, femoral condyles, tibial plateau, or fibular head. This clinical finding helped to exclude gross associated bony injuries in these adjacent regions. The course of the common peroneal nerve posterior to the fibular head was non-tender, and Tinel's sign was negative.
- Compartments: A thorough assessment of all four compartments of the left lower leg (anterior, lateral, superficial posterior, deep posterior) revealed that they were soft and non-tender to palpation, without any signs of increased tension. This clinical evaluation successfully alleviated immediate concerns for an acute compartment syndrome.
Range of Motion (ROM)
- Active Range of Motion: Mr. Davies demonstrated a profound and complete inability to perform active knee extension against gravity. Any volitional attempt to activate his quadriceps muscles resulted in significant pain and a visible "quadriceps lag," characterized by the inability to actively lift his foot off the examination bed despite maximal effort. This finding unequivocally indicated a complete functional disruption of the active extensor mechanism. Concurrently, he was unable to perform a straight leg raise.
- Passive Range of Motion: Passive flexion of the left knee was severely restricted by both pain and a mechanical block, achieving only approximately 35 degrees before eliciting significant patient guarding and profound discomfort. Passive extension was also limited, with the knee resting at an obligate position of approximately 20 degrees of flexion and not allowing full, painless extension without eliciting severe pain.
Neurological & Vascular Assessment
Neurological Assessment:
A comprehensive neurological examination of the left lower extremity revealed no focal neurological deficits.
*
Motor Function:
Motor strength was assessed using the Medical Research Council (MRC) scale and found to be intact (5/5) for ankle dorsiflexion (primarily L4, L5 nerve root distribution via the deep peroneal nerve), ankle plantarflexion (S1, S2 nerve root distribution via the tibial nerve), great toe extension (L5, deep peroneal nerve), and toe flexion (S1, S2, tibial nerve). There was no evidence of a foot drop or any other distal motor weakness.
*
Sensory Function:
Sensation to light touch and pinprick was intact throughout all dermatomes of the left lower limb: L2 (proximal thigh), L3 (distal thigh, medial knee), L4 (medial leg, medial malleolus), L5 (lateral leg, dorsum of foot), and S1 (lateral malleolus, plantar foot). The specific cutaneous distributions of the saphenous nerve (medial knee and shin) and the superficial peroneal nerve (dorsum of foot) were also intact.
*
Reflexes:
The patellar reflex was absent on the left side, which is a consistent and expected finding in the presence of a disrupted patellar extensor mechanism. The Achilles reflex was present and symmetrical bilaterally (2+).
Vascular Assessment:
The vascular status of the left lower limb was thoroughly assessed and found to be robust and reassuring.
*
Pulses:
Both the dorsalis pedis and posterior tibial pulses were strong, easily palpable, and symmetrical bilaterally (rated 2+ on a scale of 0-3), indicating excellent distal perfusion.
*
Capillary Refill:
Rapid capillary refill (<2 seconds) was observed in all toes of the left foot.
*
Skin:
The skin distal to the knee was warm, pink, and well-perfused, with no signs of pallor, cyanosis, or mottling.
*
Ankle-Brachial Index (ABI):
An Ankle-Brachial Index was not deemed necessary in this acute setting, as there were no "hard signs" of vascular compromise (e.g., absent pulses, an expanding hematoma, a palpable thrill or audible bruit, a cold or pale limb, or a pulsatile hematoma). While popliteal artery injury is a rare but critical concern in cases of significant knee trauma, it is more typically associated with knee dislocations or severely displaced supracondylar femoral fractures; these were not suspected in this case given the direct patellar impact and the presence of strong, palpable distal pulses.
Imaging & Diagnostics
Initial Radiographs
Standard radiographic imaging of the left knee was obtained immediately upon Mr. Davies's arrival in the emergency department. The series included an anterior-posterior (AP) view, a true lateral view, and a Merchant (sunrise) view. These views are fundamental for the initial evaluation of patellar fracture patterns, the degree of displacement, and the extent of articular involvement.
- Anterior-Posterior (AP) View: The AP radiograph clearly demonstrated a highly comminuted patellar fracture. Multiple distinct fracture lines were evident, segmenting the patella into several identifiable bony pieces. There was significant overall diastasis between the major fragments, with pronounced widening of the fracture lines across the patellar body. The superior pole fragment appeared retracted proximally, consistent with the powerful pull of the quadriceps muscle.
-
Lateral View:
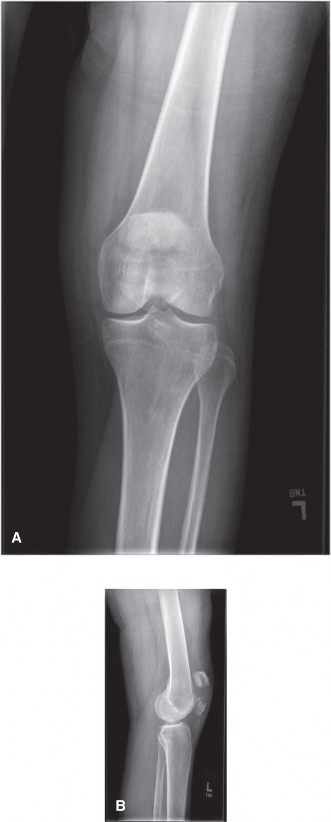
The true lateral radiograph provided crucial information regarding the sagittal plane displacement and the extent of articular involvement. This view unequivocally confirmed the severe comminution and marked displacement of the fracture fragments. The superior pole was significantly retracted proximally, driven by the strong pull of the quadriceps tendon. Concurrently, the inferior pole fragment, although also comminuted, remained relatively anchored by the patellar tendon. A substantial step-off and gapping, indicative of severe articular incongruity, were clearly visible along the posterior (articular) surface of the patella. The overall fracture pattern exhibited a predominant transverse oblique component with extensive secondary comminution.
-
The following image is highly representative of the lateral view obtained for Mr. Davies, clearly showing significant comminution and superior pole retraction.

-
The following image is highly representative of the lateral view obtained for Mr. Davies, clearly showing significant comminution and superior pole retraction.
- Merchant (Sunrise) View: This axial view, typically obtained with the knee flexed to approximately 30-45 degrees, was indispensable for evaluating the articular congruity of the patella within the trochlear groove. It revealed gross disruption of the patellar articular surface, unequivocally confirming the presence of multiple intra-articular fragments and significant chondral surface incongruity. This view particularly emphasized the inherent challenge in achieving an anatomical reduction of the load-bearing articular cartilage.
Computed Tomography (CT) Scan
Given the extensive comminution and clear intra-articular involvement observed on plain radiographs, a computed tomography (CT) scan of the left knee was subsequently performed. CT scanning offers superior three-dimensional visualization of complex fracture patterns, providing precise details on fragment morphology, the exact degree of articular step-off and gap, and the precise location of even very small fracture fragments. This highly detailed information is invaluable for comprehensive pre-operative planning and understanding the full extent of the injury.
- CT Findings: The CT scan unequivocally confirmed a highly comminuted, multi-fragmentary patellar fracture. It involved both the superior and inferior poles, with significant central and peripheral comminution throughout the patellar body. Crucially, multiple articular fragments were identified, with an articular step-off measured at greater than 4mm and fracture gaps exceeding 6mm in the primary load-bearing areas of the patella. No associated fractures of the distal femur, proximal tibia, or fibula were identified on the CT scan, corroborating the clinical assessment. The 3D reconstructions derived from the CT data were particularly instrumental in visualizing the global fracture architecture, understanding the complex relationship of the individual fragments to the trochlear groove, and assessing the overall disruption of the patellar body. These reconstructions were critical in identifying the "key" fragments required for initial reconstruction and provided a roadmap for the surgical approach.
Magnetic Resonance Imaging (MRI)
An MRI scan was not indicated in Mr. Davies's specific acute presentation. The diagnosis of a severely displaced, comminuted patellar fracture with clear clinical and radiographic evidence of extensor mechanism disruption was unequivocally established by the combined information from clinical examination, plain radiographs, and a detailed CT scan. The primary utility of MRI in acute patellar trauma is typically reserved for more nuanced diagnostic scenarios, such as:
* Evaluation of suspected concomitant ligamentous injuries (e.g., anterior cruciate ligament, posterior cruciate ligament, or collateral ligaments) when clinical suspicion remains high despite a clear patellar fracture, or if the mechanism of injury suggests a multi-ligamentous knee injury.
* Differentiation between a patellar fracture and an acute rupture of the quadriceps tendon or patellar tendon when plain radiographs are equivocal or negative.
* Assessment of subtle chondral damage, osteochondral defects, or occult stress fractures in less acute or chronic settings, or for planning specific chondral repair strategies, which was not the immediate priority in this case of gross mechanical disruption and bony fragmentation.
Pre-operative Templating
Extensive and meticulous pre-operative templating was performed utilizing the detailed CT images and their corresponding 3D reconstructions. This systematic approach facilitated the development of a precise and individualized surgical strategy:
*
Fragment Identification and Analysis:
This involved precisely mapping all significant fracture fragments, with particular attention directed towards those fragments that contributed to the critical articular surface of the patella. The exact extent of comminution and displacement of each fragment was meticulously analyzed to anticipate potential reduction challenges during surgery.
*
Reduction Sequence:
A step-by-step plan for the intra-operative reduction sequence was devised. The strategy involved initially reducing and stabilizing the largest, most stable fragments to reconstruct a foundational patellar shape and approximate its original length. This initial reconstruction would then be followed by the meticulous reduction and fixation of smaller articular fragments to restore articular congruity as precisely as possible.
*
Implant Selection and Construct Planning:
Given the severe comminution and significant displacement of Mr. Davies's patellar fracture, a tension band wiring technique alone was deemed insufficient to provide the necessary rotational and shear stability required for a robust reduction and to facilitate safe, early rehabilitation. Therefore, a more comprehensive and robust hybrid fixation strategy was planned. This involved a carefully considered combination of small fragment plates (e.g., 2.7mm or 3.5mm titanium plates), which would be judiciously contoured and applied to the anterior surface of the patella. These plates would be complemented by strategically placed interfragmentary screws to achieve anatomical compression between large fragments where feasible (lag screw effect), and supplementary cerclage wiring to enhance overall stability, provide circumferential compression, and neutralize distracting forces across the comminuted zones. The overarching objective of this construct was to achieve a strong, compression-resistant, and rotationally stable fixation that would meticulously restore the overall length, width, and, most importantly, the articular congruity of the patella, while concurrently minimizing the prominence of the implanted hardware.
Surgical Decision Making & Classification
Why Operative Management?
Mr. Davies's patellar fracture presented with several critical clinical and radiological features that unequivocally necessitated operative intervention rather than non-operative management:
1.
Complete Disruption of the Extensor Mechanism:
Clinically, the patient demonstrated a profound and complete inability to actively extend his knee against gravity or to perform a straight leg raise. This finding is the definitive hallmark of a disrupted extensor mechanism, a condition that renders the knee functionally compromised and demands surgical restoration for the patient to regain independent ambulation, weight-bearing, and functional mobility.
2.
Significant Fragment Displacement:
Both the initial radiographs and the subsequent CT scans confirmed substantial displacement of the patellar fracture fragments. A fracture gap exceeding 3mm (in Mr. Davies's case, measurements were consistently greater than 6mm) and significant superior pole retraction by the quadriceps muscle were clearly evident. This degree of fragment displacement inherently prevents spontaneous healing in an anatomically acceptable position and would inevitably lead to a nonunion or symptomatic malunion without surgical intervention.
3.
Extensive Articular Incongruity:
The detailed CT scan specifically revealed an articular step-off greater than 2mm (in Mr. Davies's case, measurements consistently exceeded 4mm). Clinical evidence from long-term studies strongly correlates articular step-offs greater than 2mm in weight-bearing joints with an significantly accelerated risk of developing post-traumatic osteoarthritis. Therefore, anatomical reduction of the articular surface is paramount to preserve long-term joint health and function.
4.
Severe Comminution and Mechanical Instability:
The fracture was categorized as highly comminuted. Non-operative management of such unstable, multi-fragmentary patterns would almost invariably result in a symptomatic malunion, a painful nonunion, significant chronic pain, profound functional deficits, and a premature onset of degenerative changes within the patellofemoral joint.
Classification
Patellar fractures are typically classified based on their characteristic fracture pattern and the extent of fragment displacement. For Mr. Davies's specific injury, several classification systems are relevant and were considered:
-
AO/OTA Classification (34-C3):
- 34: This numerical prefix specifically refers to fractures of the patella.
- C: The "C" designation denotes that the fracture is intra-articular, meaning the fracture line unequivocally involves the joint surface.
- 3: The final digit "3" indicates a multi-fragmentary or severely comminuted fracture pattern, which precisely describes Mr. Davies's injury with its numerous distinct bone fragments. This classification accurately characterizes his injury as a complex, intra-articular, comminuted fracture.
- Other Common Morphological Classifications: While extensively comminuted, Mr. Davies's fracture exhibited a predominant transverse component, often observed following a direct impact mechanism of trauma. However, the sheer degree of comminution elevated it beyond a simple transverse fracture, making the AO/OTA classification more encompassing. Other patterns include stellate, vertical, and polar fractures, but these were less representative of the primary injury morphology.
-
Criteria for Non-operative vs. Operative Management:
- Non-operative Management: Generally indicated for undisplaced or minimally displaced patellar fractures (defined as a fracture gap typically less than 2-3mm and an articular step-off less than 2mm) and critically, an intact extensor mechanism (i.e., the patient can actively extend the knee against gravity and perform a straight leg raise without extensor lag). Non-operative treatment typically involves immobilization of the knee in full extension for a period of 4-6 weeks, followed by a gradual and protected range of motion rehabilitation protocol.
- Operative Management: Indicated for virtually all displaced patellar fractures (defined as a fracture gap greater than 2-3mm or an articular step-off greater than 2mm), cases with complete disruption of the extensor mechanism, all open fractures of the patella, or fractures with significant associated soft tissue compromise. Mr. Davies's injury, with its gross displacement, severe comminution, and complete loss of active extension, definitively fell into the operative category.
Based on these compelling clinical and radiological findings, the unanimous decision was made for emergent open reduction and internal fixation (ORIF) of the left patellar fracture. The aim was to restore anatomical alignment, re-establish the integrity of the extensor mechanism, and facilitate an optimal functional recovery.
Surgical Technique / Intervention
Mr. Davies was scheduled for urgent open reduction and internal fixation of his left patellar fracture. The urgency was dictated by the acute nature of the injury, the significant disruption of the extensor mechanism, and the desire to intervene before severe soft tissue swelling and blistering could further complicate the surgical field.
Patient Positioning
The patient was positioned supine on the operating table. A high thigh tourniquet was carefully applied to the proximal aspect of the left lower extremity to ensure a bloodless surgical field, which is paramount for meticulous fragment identification and articular reduction in comminuted fractures. The entire limb, from the mid-thigh down to the toes, was meticulously prepped and draped in a sterile fashion, ensuring adequate sterile exposure and allowing for full, unconstrained range of motion of the knee during the procedure. A sterile impervious stockinette was applied, and the limb was temporarily suspended to facilitate a thorough and circumferential antiseptic scrub. Once adequately prepped, the limb was returned to the operating table, and the tourniquet was inflated to 350 mmHg following complete limb exsanguination using an Esmarch bandage.
Surgical Approach
A standard anterior longitudinal incision was carefully planned and made. This incision was centered directly over the patella and extended approximately 5cm proximal (into the quadriceps tendon area) and 5cm distal (over the patellar tendon) to the estimated extent of the fracture. This approach provides excellent, direct visualization of all patellar fragments, the entire extensor mechanism, and allows for thorough assessment and repair of the retinacula.
Meticulous sharp and blunt dissection was performed through the skin and subcutaneous tissue. A full-thickness skin and subcutaneous tissue flap was carefully raised, exposing the fractured patella and the associated extensive retinacular tears. The tense hemarthrosis within the knee joint was thoroughly evacuated, and the joint itself was copiously irrigated with sterile saline to remove blood clots, small osteochondral fragments, and other loose bony debris, which if left, could contribute to post-operative arthrofibrosis. The extent of retinacular disruption, particularly the significant medial and lateral tears, was noted. These tears contributed to the proximal retraction of the quadriceps mechanism and necessitated repair.
Reduction Techniques
The cornerstone of successful patellar fracture fixation, particularly in complex comminuted patterns, is the precise anatomical reduction of the articular surface and the meticulous restoration of the overall patellar length and width.
1.
Initial Debridement and Assessment:
The fracture fragments were carefully assessed. Any small, non-viable, or extremely comminuted pieces of bone that were too small to contribute to a stable reconstructive construct or achieve reliable fixation were carefully debrided. The main fragments were identified, including the large superior pole, the extensively comminuted central body, and the inferior pole fragments.
2.
Reconstruction of Main Fragments:
Initial attention was directed towards reconstructing the major load-bearing articular fragments and restoring the overall length of the patella. This often involved gently but firmly pulling the superior pole fragment distally, against the powerful pull of the quadriceps, and bringing the inferior pole fragment proximally, to reduce the overall length and approximate the fracture fragments. Temporary K-wire fixation (e.g., 1.25mm or 1.6mm K-wires) was used to hold these main fragments in preliminary anatomical alignment. The pre-operative 3D CT reconstructions proved invaluable at this stage, serving as a template for visualizing the original patellar shape and guiding the reduction.
3.
Articular Surface Restoration:
Meticulous reduction of the articular surface was achieved. This is often the most technically challenging aspect in comminuted fractures, requiring patience and precision. Under direct visualization, the articular fragments were carefully pieced together, much like a three-dimensional jigsaw puzzle. The goal was to ensure no step-off or gap greater than 1mm on the posterior (articular) surface. Intermittent fluoroscopy, with both lateral and Merchant (sunrise) views, was utilized to confirm articular congruity and overall patellar length throughout the reduction process.
4.
Initial Compression and Containment (Cerclage Wiring):
Due to the severe comminution and the number of fragments, a circumferential cerclage wire (typically 1.2mm stainless steel wire) was strategically passed around the entire patella. This wire traversed the substance of the quadriceps tendon proximally and the patellar tendon distally, positioned just anterior to the main fracture fragments and underlying the planned plate. This cerclage acted as a preliminary compression and containment device, effectively holding the comminuted fragments together and restoring gross patellar length while more definitive fixation was applied. This cerclage also plays a crucial role in neutralizing some of the initial distractive forces exerted by the quadriceps.
Fixation Construct
Given the severely comminuted and displaced nature of Mr. Davies's fracture, a robust hybrid fixation construct was chosen. This multi-planar approach was designed to provide superior stability against various forces and facilitate early, protected range of motion.
- Longitudinal K-wire Placement (Tension Band Principles): Two parallel 1.6mm K-wires were carefully inserted longitudinally from the inferior pole, traversing the main fracture fragments, and extending into the superior pole. These wires were strategically placed just beneath the anterior cortex of the patella to avoid breaching the articular surface posteriorly. The K-wires provide a stable axial foundation for the subsequent tension band.
- Figure-of-Eight Tension Band Wire: A 1.2mm stainless steel wire was then passed in a figure-of-eight fashion through the quadriceps tendon proximally and the patellar tendon distally, anterior to the two parallel K-wires. This wire was carefully tightened, typically with the knee slightly flexed (e.g., 20-30 degrees), to provide dynamic compression across the fracture site when the knee flexes. This tension band mechanism converts the distractive forces of the quadriceps into compressive forces, which is fundamental to patellar fracture healing. The ends of the K-wires were bent posteriorly and cut short to prevent migration and minimize soft tissue irritation.
- Supplemental Plate Fixation: Due to the extensive comminution, particularly in the central and lateral aspects of the patella, a tension band wiring technique alone was considered insufficient to provide optimal rotational and shear stability. Therefore, a small-fragment contoured plate (e.g., a 2.7mm or 3.5mm titanium L-plate or T-plate, or a specific patellar plate) was carefully applied to the anterior surface of the patella. The plate was meticulously contoured to conform to the complex patellar anatomy and provide additional stability against torsional and shear forces. Multiple cortical screws were placed through the plate into the largest fragments, ensuring solid purchase in dense bone. Where feasible, interfragmentary compression screws were also utilized across specific oblique fracture lines to achieve an additional lag screw effect. The plate was positioned carefully to avoid any prominent hardware that could impinge on the vastus intermedius muscle or irritate the overlying skin.
- Reinforcement of Retinacular Tears: The torn medial and lateral patellar retinacula were meticulously identified and repaired using strong, non-absorbable sutures (e.g., 2-0 braided polyester). This step is absolutely critical to prevent post-operative lateral patellar subluxation or dislocation, to maintain proper patellar tracking, and to reinforce the overall integrity of the extensor mechanism.
- Final Assessment: After all fixation was applied, the knee was taken through a full range of motion (typically from 0 to 120 degrees of flexion) to thoroughly assess the stability of the entire construct, confirm the integrity of the reduction, and check for any hardware impingement or prominence. Fluoroscopy was used once more to confirm perfect anatomical reduction and stable fixation in all planes and throughout the range of motion.
- Wound Closure: The surgical wound was thoroughly irrigated with copious amounts of sterile saline. A drain was not typically placed unless there was extensive soft tissue dissection or significant concern for persistent bleeding. The subcutaneous tissues and skin were closed in layers using absorbable sutures for the deeper layers and non-absorbable sutures or staples for the skin. A sterile dressing was applied, followed by the application of a knee immobilizer set at full extension (0 degrees).
Post-Operative Protocol & Rehabilitation
The post-operative protocol for comminuted patellar fractures treated with open reduction and internal fixation (ORIF) is meticulously designed to optimize outcomes, minimize complications, and facilitate a safe and progressive return to function. The central tenet is to protect the fragile fixation and the healing bone while simultaneously allowing for early, controlled motion to prevent the deleterious effects of prolonged immobilization, such as stiffness and muscle atrophy.
Immediate Post-Operative Phase (Day 0-7)
- Immobilization: The patient's knee was maintained in a rigid knee immobilizer, locked in full extension (0 degrees), at all times. This immobilizer was only to be removed for supervised physical therapy sessions and hygiene. This full extension position protects the fracture fixation from the powerful distractive forces of the quadriceps muscle.
- Weight-Bearing: Strict non-weight-bearing (NWB) on the operated left lower extremity was enforced. The patient was instructed to use crutches or a walker for ambulation, with strict avoidance of any direct weight or axial load through the knee.
- Pain Management: A multimodal analgesia regimen was initiated, incorporating a combination of non-steroidal anti-inflammatory drugs (NSAIDs), acetaminophen, and opioid analgesics as needed, to ensure optimal pain control and facilitate early participation in therapy.
- Edema Control: Aggressive measures for edema control were instituted, including regular application of ice packs, consistent elevation of the limb above the level of the heart, and continued use of a soft compression bandage.
- Deep Vein Thrombosis (DVT) Prophylaxis: Pharmacological prophylaxis (e.g., low molecular weight heparin, LMWH) was administered daily as per institutional guidelines, combined with encouraging early ankle pumps and passive range of motion exercises for the hip and ankle of the affected limb.
- Wound Care: Daily dressing changes were performed, with close monitoring of the surgical wound for any signs of infection, hematoma formation, or skin breakdown.
Early Rehabilitation Phase (Weeks 1-6)
-
Range of Motion (ROM):
- Weeks 1-2: Controlled passive range of motion (PROM) was initiated, carefully progressing from 0-30 degrees of knee flexion. This was typically achieved through supervised physical therapy sessions or via a Continuous Passive Motion (CPM) machine. Active knee extension against gravity was strictly prohibited to protect the healing fracture.
- Weeks 3-4: PROM was gradually increased to a target of 0-60 degrees of flexion, contingent upon the absence of pain and radiological signs of stability. Strict avoidance of active knee extension against gravity continued. Isometric quadriceps sets (e.g., quadriceps contractions without any knee flexion or movement) were cautiously initiated to maintain muscle tone and mitigate atrophy, ensuring no distraction forces were generated across the fracture site.
- Weeks 5-6: PROM was further progressed towards 0-90 degrees of flexion as tolerated. Gentle, protected active knee flexion may be introduced at this stage, again under strict supervision.
- Weight-Bearing: Progressed from NWB to toe-touch weight-bearing (TTWB) or partial weight-bearing (PWB) in the knee immobilizer or a hinged knee brace locked in full extension. This progression was strictly contingent upon radiographic evidence of early callus formation and fracture stability, typically confirmed around week 4-6.
- Exercises: Non-weight-bearing exercises for the hip and ankle of the affected limb were continued. Upper extremity strengthening and core stability exercises were also emphasized to maintain overall fitness and aid in ambulation.
- Physical Therapy: Regular, structured sessions with a specialized physical therapist were crucial to ensure proper exercise technique, prevent the development of compensatory movement patterns, and closely monitor the patient's progress and any adverse symptoms.
Intermediate Rehabilitation Phase (Weeks 7-12)
- Range of Motion (ROM): The primary goal was to gradually advance towards achieving full active and passive range of motion (targeting 0-120+ degrees of flexion) as tolerated by the patient and as deemed safe by the therapist and surgeon.
- Weight-Bearing: Progression from PWB to full weight-bearing (FWB) was initiated in a hinged knee brace. The brace was gradually unlocked to allow increasing degrees of knee flexion during weight-bearing, depending on radiographic evidence of progressing bone healing and the patient's comfort and confidence.
-
Strengthening:
- Quadriceps: Closed-chain exercises (e.g., mini-squats, leg presses within a pain-free range, wall slides) were commenced to safely strengthen the quadriceps. Progress was then made to open-chain exercises with light to moderate resistance, always carefully monitoring for any patellar symptoms (e.g., pain, crepitus). Avoidance of heavy resisted knee extension was maintained initially.
- Hamstrings, Gluteals, Calves: Comprehensive strengthening exercises for these muscle groups were continued and progressively intensified.
- Proprioception & Balance: Introduction of advanced balance and proprioception exercises (e.g., single-leg stance, wobble board activities, uneven surface walking) to restore neuromuscular control.
- Functional Training: Intensive gait training was performed to normalize the patient's walking pattern. Stair climbing, descending, and other activities of daily living were progressively integrated.
Advanced Rehabilitation Phase (Weeks 13-24 and Beyond)
- Return to Activity: This phase focused on a gradual and progressive return to sport-specific or work-specific activities, tailored to Mr. Davies's occupational demands. Emphasis was placed on developing power, endurance, agility, and impact tolerance.
- High-Impact Activities: Activities involving high impact, such as running, jumping, and cutting maneuvers, were typically deferred until 4-6 months post-surgery, conditional upon complete radiographic union, full strength recovery, and satisfactory clinical assessment.
- Hardware Removal: Consideration for hardware removal, particularly if the hardware became prominent, painful, or caused symptomatic irritation, was typically deferred until 12-18 months post-surgery. This timeline ensures complete fracture consolidation and minimizes the risk of refracture upon removal. For Mr. Davies, given the amount of hardware and his physically demanding profession, symptomatic hardware removal would likely be considered.
- Long-term Monitoring: Mr. Davies will require regular, long-term follow-up to monitor for potential complications such as the development of post-traumatic arthritis, persistent patellofemoral pain, or other long-term sequelae of the injury.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls
- Anatomical Reduction is Paramount for Articular Fractures: For all intra-articular fractures, and especially those involving the patella's weight-bearing articular surface, achieving an anatomical reduction (ideally with less than 1-2mm step-off or gap) is the single most critical factor in minimizing the risk of accelerating post-traumatic osteoarthritis. Prioritize articular congruity even if it means slightly compromising cortical apposition on a non-articular surface.
- Restore Patellar Length and Tracking: The patella's precise length directly influences the mechanical efficiency and lever arm of the quadriceps muscle. Avoid both patella brevis (shortening) and patella alta (lengthening), as either can significantly compromise patellofemoral biomechanics, lead to chronic pain, and impact overall knee function. Utilize the contralateral knee for templating or retrieve pre-injury radiographs if available to guide patellar length restoration. Restore medial and lateral patellar tracking by meticulous retinacular repair.
- Master Tension Band Wiring Principles: A thorough understanding of how tension band wiring converts distractive forces (from quadriceps pull) into compressive forces across the fracture site is fundamental for patellar fracture fixation. Ensure the longitudinal K-wires are correctly positioned in the anterior third of the patella to maximize the tension band effect, and the figure-of-eight wire is securely anchored.
- Supplemental Fixation for Comminution is Essential: For highly comminuted patellar fractures, tension band wiring alone is often biomechanically insufficient to provide adequate stability against all forces (e.g., rotation, shear). It is a common and critical error to rely solely on a tension band in such complex patterns. Supplementation with small fragment plates (e.g., 2.7mm or 3.5mm titanium plates) and interfragmentary screws is crucial to achieve a robust, multi-planar construct that resists rotational and shear forces, thereby allowing for earlier and safer rehabilitation.
- Meticulous Soft Tissue Repair: The repair of the torn medial and lateral patellar retinacula is an often-underestimated but crucial step. These structures contribute significantly to patellar stability, proper tracking, and overall extensor mechanism function, preventing post-operative patellar subluxation or dislocation.
- Early, Controlled Motion is Key: While protecting the fracture fixation is paramount, initiating early, controlled passive range of motion is vital to prevent debilitating arthrofibrosis, maintain the health of the articular cartilage, and facilitate the early recovery of quadriceps strength. However, this must be balanced with strict adherence to weight-bearing and active ROM restrictions, especially avoiding active knee extension initially.
- Optimize Patient Biological Factors: Always consider and optimize the patient's nutritional status, particularly protein intake, to support robust bone and soft tissue healing. Address any identified deficiencies in vitamin D and calcium, as these play critical roles in osteogenesis.
- Thorough Irrigation and Debridement: Copious irrigation and removal of small bone fragments or debris from the joint space are crucial to prevent mechanical impingement and subsequent arthrofibrosis.
Pitfalls
- Inadequate Articular Reduction: Failure to achieve precise anatomical reduction of the articular surface is arguably the leading cause of poor long-term outcomes, inevitably leading to chronic pain, symptomatic crepitus, and accelerated post-traumatic osteoarthritis, even with good bony union.
- Insufficient Fixation & Construct Instability: An unstable fixation construct, particularly in a comminuted fracture, will predispose to loss of reduction, delayed union, nonunion, or catastrophic hardware failure. Relying solely on a simple tension band wiring technique for highly comminuted fracture patterns is a common and critical pitfall.
- Hardware Prominence or Impingement: Poorly placed hardware, such as K-wires protruding significantly anteriorly, screws breaching the articular surface, or plates that are not adequately contoured, can cause chronic pain, persistent soft tissue irritation, and necessitate premature hardware removal, potentially compromising fracture healing. K-wire migration, proximally or distally, is also a recognized complication.
- Premature Aggressive Rehabilitation: Pushing the patient too quickly on active knee extension or weight-bearing activities before adequate radiographic fracture healing has occurred can lead to devastating consequences, including loss of reduction, re-fracture of the patella, or failure of the internal fixation.
- Delayed Rehabilitation Leading to Arthrofibrosis: Conversely, prolonged or excessive immobilization can lead to severe and often irreversible knee stiffness (arthrofibrosis), especially in the presence of a significant hemarthrosis and extensive soft tissue trauma. The art of rehabilitation lies in finding the precise balance between protection and early motion.
- Surgical Site Infection: Despite patellar fractures often being closed injuries, internal fixation carries a significant risk of surgical site infection, particularly with the amount of hardware often required. Meticulous aseptic technique, appropriate prophylactic antibiotics, and careful post-operative wound management are absolutely essential.
- Nonunion or Malunion: These complications can arise due to inadequate fixation, compromised biological healing factors, or infection. Both often necessitate further complex surgical intervention, compromising the patient's functional outcome.
- Quadriceps Weakness and Patella Baja: Long-term complications frequently include persistent quadriceps weakness and the development of patella baja (inferior displacement or shortening of the patella). Patella baja is often due to inadequate rehabilitation, fibrous union with shortening, or poor initial reduction. It significantly impacts functional outcomes and is notoriously difficult to correct once established.
- Post-traumatic Osteoarthritis: This is the most common long-term complication following patellar fractures, even in cases with an excellent anatomical reduction, due to the initial cartilage damage sustained during the trauma. Patients must be thoroughly counseled on this inherent risk.
- Overlooking Neurovascular Injury: Although rare in isolated patellar fractures, overlooking a subtle neurovascular injury during the initial assessment can have devastating and limb-threatening consequences. A thorough and documented neurovascular examination is paramount in all trauma cases.
You Might Also Like


