Cruciate Ligament Injuries: A Comprehensive Medical Review

Key Takeaway
Cruciate ligament injuries, primarily involving the ACL and PCL, are significant orthopedic challenges causing knee instability. They are diagnosed through detailed history, physical examination including Lachman and Pivot Shift tests, and understanding their complex epidemiology, surgical anatomy, and biomechanics.
Introduction & Epidemiology
Cruciate ligament injuries, primarily involving the anterior cruciate ligament (ACL) and posterior cruciate ligament (PCL), represent a significant orthopaedic challenge due to their prevalence, functional implications, and potential for long-term morbidity. These injuries often result in knee instability, impaired functional performance, and a heightened risk of secondary intra-articular damage, including meniscal tears and articular cartilage degeneration, ultimately predisposing patients to post-traumatic osteoarthritis.
The incidence of ACL injuries is estimated at 68 per 100,000 person-years in the general population, with a disproportionate impact on young, active individuals participating in pivoting and contact sports. Female athletes demonstrate a 2-8 fold higher incidence rate compared to their male counterparts in similar sports, a disparity attributed to a complex interplay of anatomical, hormonal, neuromuscular, and biomechanical factors. Non-contact mechanisms, often involving sudden deceleration, cutting, or jumping with valgus collapse and internal tibial rotation, account for approximately 70-80% of ACL tears. While less common, PCL injuries typically result from direct anterior force to the tibia with the knee flexed, hyperextension, or rotational mechanisms, and often occur in high-energy trauma settings or sports-related incidents. Isolated PCL injuries are less frequent than ACL tears, comprising 3-20% of all knee ligament injuries.
The immediate clinical presentation of an acute ACL injury often includes a distinctive "pop" sensation or audible noise at the time of injury, as described in the original seed content, followed by rapid onset of pain and effusions.

Patients frequently report a feeling of the knee "giving way" or "bursting from under them," leading to an inability to continue activity. Swelling typically develops within 2-24 hours due to hemarthrosis. If untreated, acute symptoms may subside, but persistent functional instability, particularly during pivoting activities, often ensues, increasing the risk of progressive meniscal and chondral damage.
The socioeconomic burden associated with cruciate ligament injuries is substantial, encompassing surgical costs, prolonged rehabilitation, lost productivity, and the long-term sequelae of chronic knee pathology. A prompt and accurate diagnosis is paramount for guiding management strategies and mitigating long-term complications.

Surgical Anatomy & Biomechanics
The knee joint is a complex diarthrodial hinge joint allowing for flexion, extension, and limited rotation, stabilized by a sophisticated arrangement of bones, ligaments, tendons, and menisci.

Understanding the intricate anatomy and biomechanics of the cruciate ligaments is fundamental to their surgical reconstruction.
Anterior Cruciate Ligament (ACL)
The ACL originates from the posterior aspect of the medial surface of the lateral femoral condyle, within the intercondylar notch. It courses anteriorly, medially, and distally to insert into a broad, oval footprint on the anterior aspect of the intercondylar eminence of the tibia, anterior and lateral to the medial tibial spine. The ACL is comprised of two functional bundles:
*
Anteromedial (AM) bundle:
Taut in flexion.
*
Posterolateral (PL) bundle:
Taut in extension.
These bundles act synergistically to resist anterior tibial translation and internal tibial rotation, particularly at low flexion angles. The ACL is the primary restraint to anterior tibial translation, accounting for approximately 85% of this restraint, and a secondary restraint to valgus and varus stresses, especially with concomitant collateral ligament injury. The ACL is intrasynovial but extrasynovial, enveloped by a synovial membrane. Its blood supply is derived from branches of the middle genicular artery, and its innervation from the posterior articular nerve (branch of the tibial nerve).
Posterior Cruciate Ligament (PCL)
The PCL is significantly stronger and broader than the ACL. It originates from the anterior part of the lateral surface of the medial femoral condyle, within the intercondylar notch, coursing posteriorly, laterally, and distally. Its broad insertion is on the posterior aspect of the tibial plateau, inferior to the joint line, approximately 1-1.5 cm distal to the articular margin, in the "PCL facet." Similar to the ACL, the PCL also has two bundles:
*
Anterolateral (AL) bundle:
Larger and stronger, taut in flexion.
*
Posteromedial (PM) bundle:
Smaller, taut in extension.
The PCL is the primary restraint to posterior tibial translation, providing 95% of the total posterior stability. It also acts as a secondary restraint to external tibial rotation and varus/valgus stress. The PCL's blood supply originates from the middle genicular artery.
Physical Examination and Diagnostic Imaging
Clinical diagnosis relies on a detailed history and astute physical examination.
*
ACL Injury:
*
Lachman Test:
Most sensitive test for acute ACL rupture. Performed with the knee in 20-30 degrees of flexion, stabilizing the femur and applying an anterior force to the tibia. A "soft" or absent end-point indicates injury.
*
Anterior Drawer Test:
Performed with the knee in 90 degrees of flexion. Less sensitive than Lachman in acute settings due to guarding and hamstring spasm.
*
Pivot Shift Test:
Best indicator of rotatory instability. Involves applying a valgus stress and internal rotation to the tibia while moving the knee from extension to flexion. A reduction of the subluxed tibia as the knee flexes indicates a positive test.
*
PCL Injury:
*
Posterior Sag Sign:
Visual assessment of posterior tibial subluxation when the knee is flexed to 90 degrees.
*
Posterior Drawer Test:
With the knee flexed to 90 degrees, a posterior force is applied to the tibia. Grading of posterior translation (Grade I: 0-5mm, Grade II: 6-10mm, Grade III: >10mm or reverse pivot shift).
*
Quadriceps Active Test:
The patient actively contracts the quadriceps with the knee flexed to 90 degrees and the foot fixed. An anterior translation of the tibia from a sagged position indicates a PCL tear.
*
Dial Test:
Assesses posterolateral corner (PLC) involvement. External rotation of the tibia is measured at 30 and 90 degrees of knee flexion. Increased external rotation at both 30 and 90 degrees suggests combined PCL and PLC injury.
Diagnostic imaging is crucial for confirmation and assessment of concomitant injuries.
*
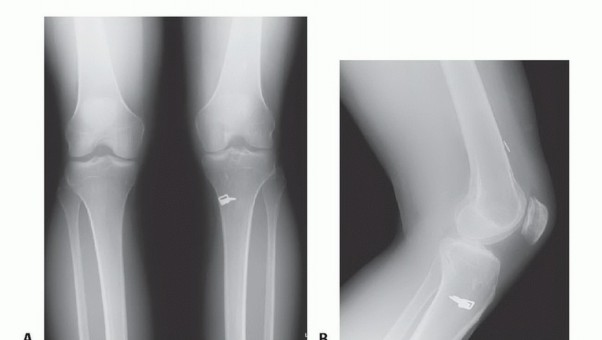
Plain Radiographs:
Typically normal in isolated cruciate injuries but can reveal avulsion fractures (Segond fracture for ACL, reverse Segond for PCL), or signs of chronic instability like early osteoarthritic changes. Stress radiographs can quantify instability.
*
Magnetic Resonance Imaging (MRI):
The gold standard for soft tissue evaluation. Sagittal views are key for ACL and PCL integrity. ACL tears often show discontinuity of fibers, increased signal intensity, or a "wavy" appearance. Indirect signs include bone bruises in the lateral femoral condyle and posterior tibia (kissing lesion), or a deep lateral femoral notch sign. PCL tears appear as disruption of the ligament with increased signal intensity. MRI is also essential for identifying associated meniscal tears, collateral ligament injuries, and chondral defects.
Indications & Contraindications
The decision for operative versus non-operative management of cruciate ligament injuries is multifactorial, considering patient age, activity level, functional instability, presence of concomitant injuries, and overall knee health.
Operative Indications
| Condition | ACL Reconstruction | PCL Reconstruction |
|---|---|---|
| Instability | Symptomatic knee instability (giving way episodes) during activities of daily living or sports, despite an adequate trial of non-operative management. | Symptomatic chronic posterior instability affecting activities of daily living or sports. Acute high-grade (Grade III) isolated PCL tears with significant instability. |
| Patient Profile | Young, active individuals or athletes involved in pivoting, cutting, or contact sports who desire to return to their pre-injury activity level. | Young, active individuals or athletes desiring to return to high-level activities. |
| Concomitant Injuries | Repairable meniscal tears (especially lateral meniscal tears), particularly if unstable or bucket-handle tears. Combined injuries involving the medial collateral ligament (MCL) (Grade III MCL usually managed non-operatively initially, with ACL reconstruction delayed) or posterolateral corner (PLC). Unstable chondral lesions requiring treatment. | Combined ligamentous injuries (e.g., PCL + PLC, PCL + MCL, PCL + ACL). Meniscal tears (often medial meniscus with chronic PCL deficiency). Chondral lesions exacerbated by PCL instability. Posteromedial corner injuries. |
| Functional Demand | Patients with high functional demands where non-operative management is likely to fail in preventing recurrent instability and further knee damage. | Patients with high functional demands where PCL deficiency severely limits functional capacity. |
| Failed Non-Op | Persistent functional instability after a structured non-operative rehabilitation program. | Persistent symptoms and functional limitations following a trial of conservative management for Grade I/II PCL tears, or for chronic Grade III tears. |
| Special Cases | Revision ACL reconstruction for graft failure. Physeal-sparing techniques in skeletally immature patients with symptomatic instability. | Acute PCL avulsion fractures requiring fixation. Acute PCL ruptures with associated posterolateral corner avulsion injuries (often requiring early surgical stabilization). Revision PCL reconstruction for failed primary procedures. |
Non-Operative Indications
| Condition | ACL Management | PCL Management |
|---|---|---|
| Patient Profile | Sedentary individuals or those with low functional demands (e.g., older patients, those not participating in pivoting sports). Patients with no desire to return to high-impact activities. | Isolated Grade I or Grade II PCL tears, especially if the patient does not experience significant functional instability. Most acute isolated PCL injuries respond well to non-operative treatment with a focus on quadriceps strengthening. |
| Instability | Patients who do not experience symptomatic instability (no giving way episodes) during activities of daily living, or those who are able to compensate adequately through bracing and rehabilitation. | Mild functional instability that can be effectively managed with bracing and targeted rehabilitation. |
| Concomitant Injuries | Patients with isolated ACL tears without significant meniscal damage requiring repair, or those with stable, peripheral meniscal tears amenable to non-operative healing. Grade I or II MCL injuries that are stable and can be managed conservatively. | Isolated PCL injuries without significant concomitant ligamentous disruptions (e.g., PLC). |
| Medical Comorbidities | Patients with significant medical comorbidities that preclude safe surgical intervention. | Patients with significant medical comorbidities precluding surgery. |
| Skeletally Immature | Although controversial, in some cases of skeletally immature patients with open physes, an initial trial of non-operative management with bracing and activity modification may be considered, particularly if functional instability is minimal, to avoid iatrogenic growth disturbances. Close monitoring for instability and secondary damage is essential. | In pediatric patients, the same principles apply as for adults; however, the lower incidence and potential for growth plate injury in operative treatment may lead to a higher initial consideration for non-operative management in less severe cases. Avulsion fractures, however, typically warrant surgical fixation regardless of physeal status. |
Contraindications
Absolute contraindications to cruciate ligament reconstruction are rare but include:
*
Active Knee Infection:
Surgical intervention is contraindicated until the infection is completely eradicated.
*
Severe Osteoarthritis:
End-stage arthritis often warrants arthroplasty rather than ligament reconstruction, as the underlying mechanical axis and cartilage degeneration are the primary pain generators.
*
Severe Medical Comorbidities:
Patients with uncompensated cardiac, pulmonary, or systemic conditions that significantly increase anesthetic and surgical risks.
*
Poor Patient Compliance:
The success of reconstruction relies heavily on patient adherence to postoperative rehabilitation protocols. Patients unwilling or unable to participate fully may be poor surgical candidates.
Relative contraindications include inflammatory arthropathies, significant knee stiffness, or unresolved concomitant injuries that would jeopardize the outcome of reconstruction.
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning and precise patient positioning are critical for successful cruciate ligament reconstruction, minimizing complications and optimizing surgical outcomes.
Pre-Operative Assessment
A comprehensive evaluation begins with a detailed patient history, focusing on injury mechanism, symptoms of instability, and functional limitations. A thorough physical examination confirms the diagnosis and assesses for concomitant injuries (e.g., meniscal tears, collateral ligament laxity, posterolateral corner deficiency). Radiographic evaluation includes standard AP, lateral, and Merchant views to rule out fractures and assess for pre-existing osteoarthritis. A dedicated MRI provides definitive diagnosis of ligamentous injury, precise location of rupture, and identifies associated intra-articular pathologies.
Graft Selection:
A crucial step in planning is graft selection, influencing operative technique, rehabilitation, and long-term outcomes. Common autograft options include:
*
Bone-Patellar Tendon-Bone (BPTB):
Gold standard for many surgeons due to reliable bone-to-bone healing and high primary stiffness. Potential donor site morbidity includes patellofemoral pain, patellar fracture, and extensor mechanism weakness.
*
Hamstring Tendons (Semitendinosus and Gracilis):
Offers less donor site morbidity than BPTB, but requires soft tissue healing. Quadrupled hamstring grafts provide excellent strength. Potential issues include saphenous nerve injury, hamstring weakness, and slower graft incorporation.
*
Quadriceps Tendon (QT):
Can be harvested with a bone plug (BTB) or as all-soft tissue. Offers a large, strong graft with comparable strength to BPTB and potentially less anterior knee pain. Donor site morbidity includes quadriceps weakness and anterior knee pain.
Allograft options (e.g., tibialis anterior, Achilles, patellar tendon) are considered for revision surgery, multiligamentous injuries, or in patients unwilling to accept autograft morbidity. Disadvantages include potential for disease transmission (though rare with current processing), slower graft incorporation, and potentially higher re-rupture rates in younger, active patients.
Equipment
Essential equipment includes a standard arthroscopic tower, camera, light source, pump, shaver, motorized burr, various arthroscopic hand instruments, cannulas, specific drilling guides (femoral, tibial), graft preparation board, and an array of fixation devices (interference screws, suspensory fixation devices like cortical buttons, cross-pins, staples). The surgeon should have a full complement of graft harvest instruments specific to the chosen autograft.
Anesthesia and Positioning
- Anesthesia: General anesthesia is typically employed, often combined with a regional nerve block (e.g., femoral nerve block, adductor canal block) for multimodal pain management, providing superior postoperative analgesia and reducing opioid requirements.
-
Patient Positioning:
The patient is positioned supine on the operating table. A pneumatic tourniquet is applied to the proximal thigh to provide a bloodless field, typically inflated to 100 mmHg above systolic blood pressure or 250-300 mmHg. A lateral post is placed just proximal to the knee joint on the lateral side to allow for appropriate valgus stress and knee manipulation.

A foot holder or leg holder device is used to secure the ankle, facilitating controlled knee flexion and extension during the procedure. The leg is draped sterilely, allowing free manipulation of the knee joint. For PCL reconstruction, especially with a tibial inlay technique, a prone position may be preferred, or a lateral decubitus position for improved posterior access. However, many PCL reconstructions are performed supine with specific posterior portals.

Detailed Surgical Approach / Technique
Cruciate ligament reconstruction, particularly ACL reconstruction, is predominantly performed arthroscopically. The following outlines a generalized approach, with specific variations depending on the ligament involved and surgeon preference.
ACL Reconstruction
1. Graft Harvest:
*
Hamstring Autograft (Semitendinosus/Gracilis):
A 2-3 cm oblique incision is made over the pes anserinus. The sartorius fascia is incised, and the semitendinosus and gracilis tendons are identified, isolated, and harvested using a closed-end tendon stripper. The tendons are then prepared on a graft preparation board, typically quadrupled or doubled, and whipstitched at the ends to create a robust graft of appropriate length and diameter (usually 8-10 mm).
*
BPTB Autograft:
A vertical incision (approx. 4-6 cm) is made over the patellar tendon. A central 10-11 mm wide segment of the patellar tendon is harvested, including a 25 mm long bone block from the inferior pole of the patella and a 25 mm long bone block from the tibial tuberosity. The remaining patellar tendon is primarily closed.
*
Quadriceps Tendon Autograft:
A vertical incision over the quadriceps tendon. A 10-11 mm wide full-thickness portion of the central quadriceps tendon is harvested, with or without a patellar bone block.
2. Arthroscopic Portal Placement and Diagnostic Arthroscopy:
Standard anteromedial (AM) and anterolateral (AL) portals are established. A systematic diagnostic arthroscopy is performed to assess all compartments, menisci, articular cartilage, and collateral ligaments. Remnants of the torn ACL are debrided sufficiently to allow clear visualization of the femoral and tibial footprints, but preservation of viable remnants for potential augmentation is encouraged.
3. Femoral Tunnel Creation:
The goal is to create an anatomically placed tunnel in the ACL's native footprint.
*
Anteromedial (AM) Portal Technique:
With the knee in hyperflexion (approximately 120-130 degrees), the femoral footprint is identified on the posterior aspect of the lateral femoral condyle. A guidewire is drilled from the AM portal into the anatomical ACL femoral footprint. Reaming is performed to the desired depth (typically 25-30 mm) and diameter, typically matching the graft size. This technique allows for a more anatomical femoral tunnel placement, reducing impingement.
*
Transtibial Technique (Historical):
The femoral tunnel is drilled through the tibial tunnel, limiting femoral tunnel placement to the 'over-the-top' position, which may lead to a more vertical graft and reduced rotational stability.
*
Outside-In Technique:
A guidewire is drilled from the lateral femoral cortex into the desired footprint, then reamed from the outside.
4. Tibial Tunnel Creation:
The tibial footprint is identified on the intercondylar eminence. A tibial guide is used to position the guidewire anatomically, typically 7 mm anterior to the PCL, aiming to exit the skin on the anteromedial tibia. The knee is often held at 70-90 degrees of flexion to achieve appropriate tunnel orientation and prevent roof impingement. Reaming is performed to match graft size and length. Care is taken to avoid divergence or blow-out of the posterior cortex.
5. Graft Passage and Fixation:
Once tunnels are created, the graft is passed through the tibial tunnel and then into the femoral tunnel.
*
Femoral Fixation:
*
Suspensory Fixation (e.g., Endobutton):
A cortical button is flipped on the lateral femoral cortex, suspending the graft within the femoral tunnel.
*
Interference Screws:
Titanium or bioabsorbable screws are inserted alongside the graft, compressing it against the tunnel wall.
*
Cross-Pins:
Transverse pins secure the graft within the femoral tunnel.
*
Tibial Fixation:
*
Interference Screws:
Most common, providing strong fixation.
*
Post-and-Washer:
Less common but effective.
*
Hybrid Fixation:
Often a combination, such as suspensory fixation on the femur and interference screw on the tibia.
Graft tensioning is critical and typically performed with the knee in 20-30 degrees of flexion to restore isometricity. After securing both ends, the knee's stability is assessed with Lachman and pivot shift tests.



PCL Reconstruction
PCL reconstruction is technically more demanding due to the ligament's posterior position and proximity to neurovascular structures. Graft choice often involves autograft (BPTB, hamstring, quadriceps) or allograft, often utilizing a double-bundle technique for improved biomechanical function.
*
Tibial Inlay Technique:
Preferred by many due to lower rates of graft abrasion and improved biomechanics. A posterior approach is used to create a bone trough or inlay facet on the posterior tibia where the graft's bone block is fixed. Femoral tunnel is drilled via an AM portal.
*
Transtibial Technique:
A tibial tunnel is drilled from anteromedial tibia to exit posteriorly on the PCL footprint. This carries a risk of "killing zone" injury to the graft by the posterior femoral condyle or posterior impingement, as well as neurovascular bundle injury.
Concomitant Injury Management
Any identified meniscal tears, particularly unstable or repairable ones, are addressed during the same procedure. Collateral ligament injuries (MCL, LCL, PLC) are also evaluated and managed, often requiring separate repair or reconstruction, or a staged approach.
Complications & Management
Despite advancements in surgical techniques, cruciate ligament reconstruction is associated with a range of potential complications, necessitating thorough understanding and proactive management strategies.
| Complication | Incidence (%) | Salvage Strategies / Management |
|---|---|---|
| Intraoperative | ||
| Neurovascular Injury | <1 (rare but serious) | Prevention through careful dissection and anatomical knowledge. Immediate recognition and vascular/neurological consultation. |
| Iatrogenic Chondral Damage | 5-10 | Prevention through careful instrument handling and portal placement. Treatment involves chondroplasty, microfracture, or other cartilage repair techniques depending on lesion size and depth. |
| Tunnel Malpositioning | 5-15 (leading cause of failure) | Prevention through precise anatomical landmark identification and careful use of guides. If recognized intraoperatively, adjust tunnel placement. If postoperative and symptomatic, revision surgery with new tunnel placement may be required, potentially with bone grafting of original tunnels. |
| Graft Impingement | Varies with technique | Prevention through anatomical tunnel placement and avoidance of roof/notch impingement. Notchplasty may be performed. If symptomatic post-op, arthroscopic debridement of impinged graft or revision surgery. |
| Posterior Wall Blow-out (tibial tunnel) | <1 | Prevention through careful reaming and avoidance of over-reaming. If minor, may proceed cautiously. If major, requires alternative fixation (e.g., screw and washer distally) or revision of the tibial tunnel. |
| Early Postoperative | ||
| Infection (Septic Arthritis) | 0.1-1 | Prompt diagnosis with aspiration and synovial fluid analysis (cell count, culture). Arthroscopic irrigation and debridement, targeted intravenous antibiotics. Graft retention may be possible in early, superficial infections. For deep or chronic infections, graft removal, debridement, and delayed reimplantation may be necessary. |
| Deep Vein Thrombosis (DVT) / PE | 0.5-2 (variable) | Prophylaxis (early mobilization, chemical prophylaxis for high-risk patients). Diagnosis with Doppler ultrasound. Treatment with anticoagulation. Pulmonary embolism requires urgent medical management. |
| Arthrofibrosis (Stiffness) | 5-15 | Prevention through early, controlled range of motion (ROM) and pain management. If established, aggressive physical therapy, manipulation under anesthesia (MUA). Persistent stiffness may require arthroscopic lysis of adhesions, cyclops lesion excision. |
| Donor Site Morbidity (Autograft) | BPTB: Patellofemoral pain (10-30%), patellar fracture (<1%), extensor mechanism weakness. Management involves physical therapy, pain control, activity modification. Hamstring: Hamstring weakness, saphenous nerve neuroma (sensory changes). Management: focused strengthening, neurolysis if persistent neuroma. QT: Quadriceps weakness, anterior knee pain. Management: targeted strengthening. | |
| Graft Laxity / Early Failure | 1-5 | Prevention through proper surgical technique (isometric placement, appropriate tensioning, robust fixation). If recognized early and significant, may require early revision. |
| Late Postoperative | ||
| Graft Failure / Re-rupture | 5-15 (higher in young athletes) | Re-evaluation of patient factors, activity levels, surgical technique, and potential underlying instability (e.g., unrecognized PLC injury). Revision ACL/PCL reconstruction, often with allograft or contralateral autograft, addressing tunnel malpositioning and possibly augmented with lateral extra-articular tenodesis (ALL reconstruction) for persistent rotational instability. |
| Persistent Instability | 5-10 | Thorough workup to identify the cause: graft failure, tunnel malposition, unrecognized concomitant ligamentous injury (e.g., PLC). Management depends on the etiology, ranging from aggressive rehabilitation to revision surgery with addressing all instabilities. |
| Post-Traumatic Osteoarthritis (PTOA) | Up to 50-70 over 10-15 years | Prevention by restoring knee stability and protecting articular cartilage. Management focuses on symptom relief (NSAIDs, injections), physical therapy, activity modification. In severe cases, osteotomy or arthroplasty may be considered. |
| Hardware Complications | 2-5 | Symptomatic hardware (prominent screws, cortical buttons causing irritation) may require removal after graft healing (typically 12-18 months post-op). |
Post-Operative Rehabilitation Protocols
Postoperative rehabilitation is an integral component of successful cruciate ligament reconstruction, aiming to restore full knee function, prevent complications, and facilitate a safe return to activity. Protocols are typically structured in a progressive, phased manner, emphasizing controlled motion, strength, and neuromuscular control while protecting the healing graft.
General Principles
- Protection of the Graft: The graft is weakest at 6-12 weeks post-surgery during the "ligamentization" process. Early stress must be carefully managed.
- Early Full Extension: Crucial for preventing arthrofibrosis and ensuring normal gait.
- Gradual Progression: Exercises are advanced based on timeframes, tissue healing, and objective functional milestones, not just subjective pain.
- Neuromuscular Control: Emphasis on proprioception, balance, and controlled movement to prevent re-injury.
- Concomitant Injuries: Rehabilitation must be tailored to address any associated meniscal repairs or collateral ligament reconstructions, often necessitating stricter initial precautions.
Phased Rehabilitation (ACL Reconstruction Example)
Phase I: Protection and Early Motion (Weeks 0-6)
*
Goals:
Control pain and swelling, achieve full knee extension, restore quadriceps activation, protect graft and meniscal repairs (if applicable).
*
Activities:
*
Weight Bearing:
Typically weight-bearing as tolerated (WBAT) with crutches, often progressing to full weight-bearing by 2-4 weeks. If meniscal repair is performed, may require longer partial weight-bearing.
*
Range of Motion (ROM):
Focus on immediate full passive knee extension using towel rolls and prone hangs. Passive flexion to 90 degrees by week 2, progressing to 120-130 degrees by week 6. Continuous passive motion (CPM) may be used.
*
Strengthening:
Quadriceps setting, straight leg raises (SLRs) in all planes, gentle hamstring curls (avoiding active flexion beyond 60 degrees if hamstring graft was used in early weeks to protect donor site). Gastrocnemius strengthening (heel raises).
*
Neuromuscular:
Patellar mobilization, gentle static balance exercises.
*
Bracing:
A hinged knee brace is often used for protection, locked in extension for ambulation initially, gradually unlocking as ROM improves.
Phase II: Strength and Neuromuscular Control (Weeks 6-12)
*
Goals:
Restore full ROM, normalize gait, improve muscular strength and endurance, enhance neuromuscular control.
*
Activities:
*
ROM:
Achieve full pain-free ROM.
*
Strengthening:
Progress from open-chain to closed-chain exercises.
*
Closed-chain:
Wall squats, leg press, mini-squats, step-ups/downs, partial lunges.
*
Open-chain:
Controlled knee extension (0-45 degrees), hamstring curls (progressive resistance).
*
Cardiovascular:
Stationary cycling, elliptical trainer, swimming (kickboard initially).
*
Neuromuscular:
Single-leg balance, proprioceptive exercises (wobble board, foam pad), light agility drills.
Phase III: Return to Activity (Months 3-6)
*
Goals:
Regain sport-specific strength, power, agility, and endurance; prepare for return to sport.
*
Activities:
*
Strengthening:
Advanced closed-chain exercises, plyometrics (box jumps, hopping drills), eccentric loading, sport-specific resistance training.
*
Agility/Speed:
Gradual introduction of lateral shuffling, cutting drills, progressive running (linear, then multidirectional).
*
Neuromuscular:
Complex balance and proprioceptive drills, reactive agility drills.
*
Functional Testing:
Introduction of objective functional tests (e.g., single-leg hop tests) to assess limb symmetry.
Phase IV: Return to Sport (Months 6-12+)
*
Goals:
Safe return to sport with minimal risk of re-injury, psychological readiness.
*
Activities:
*
Sport-Specific Training:
Full participation in practice drills, progressive integration into competitive play.
*
Strength/Conditioning:
Maintain and advance strength, power, and endurance.
*
Neuromuscular:
Continue high-level agility, plyometric, and landing mechanics training.
*
Return to Sport Criteria:
Objective criteria must be met, including:
* Full pain-free ROM.
* Symmetrical quadriceps and hamstring strength (>90% limb symmetry index on isokinetic testing).
* Satisfactory performance on functional hop tests (>90% limb symmetry index).
* Absence of effusion or instability.
* Psychological readiness (assessed via questionnaires like ACL-RSI).
* Typically, a minimum of 9-12 months is required before full unrestricted return to high-risk sports, with some literature suggesting waiting longer, particularly for young athletes.

PCL Rehabilitation Specifics
Rehabilitation for PCL reconstruction typically follows a more conservative and slower progression, especially regarding posterior tibial translation.
*
Initial Protection:
Extended period of protected weight-bearing. Bracing is often used to prevent posterior sag, typically with the tibia held in an anteriorly translated position (e.g., PCL-specific brace).
*
Quadriceps Emphasis:
Early and aggressive quadriceps strengthening is paramount to provide dynamic anterior stability, countering the posterior sag. Open-chain hamstring curls are often restricted for longer periods to avoid excessive posterior sheer forces.
*
Delayed Flexion:
Full knee flexion may be delayed to protect the graft from posterior forces.
*
Return to Sport:
Generally later than ACL, often 9-18 months.
Summary of Key Literature / Guidelines
The field of cruciate ligament surgery is continuously evolving, driven by extensive research and clinical experience. Current practice is shaped by seminal studies and consensus guidelines from professional organizations.
Key Literature & Controversies
-
Graft Choice:
Extensive literature compares autografts (BPTB, hamstrings, quadriceps) and allografts.
- Autografts: Generally favored in young, active patients due to lower re-rupture rates. BPTB offers excellent stiffness and bone-to-bone healing, but with higher patellofemoral pain. Hamstrings show less donor site morbidity but potential for hamstring weakness and slower graft incorporation. QT is gaining popularity as a robust alternative with potentially less anterior knee pain than BPTB.
- Allografts: Preferred in revision cases, multiligamentous injuries, or older/less active patients, but generally associated with higher failure rates in young, high-demand individuals.
- Single vs. Double Bundle ACL Reconstruction: While double-bundle techniques aim to anatomically restore both AM and PL bundles, studies have shown inconsistent superiority over modern single-bundle techniques in terms of clinical outcomes or re-rupture rates. Many surgeons have transitioned to an anatomical single-bundle approach.
- Timing of Surgery: Early reconstruction (within 3 weeks) for acute ACL tears carries a higher risk of arthrofibrosis. Delaying surgery (typically 3-6 weeks) allows for reduction of inflammation, restoration of ROM, and pre-operative strengthening, generally leading to better outcomes.
- Anterolateral Ligament (ALL) Reconstruction: The role of the ALL in controlling rotational stability (pivot shift) is increasingly recognized. Concomitant ALL reconstruction (or lateral extra-articular tenodesis) is debated, but growing evidence suggests it may reduce re-rupture rates, particularly in high-risk patients (e.g., young athletes with significant pivot shift).
- Physeal-Sparing Techniques: In skeletally immature patients, traditional transphyseal drilling carries a risk of growth disturbance. Physeal-sparing or partial transphyseal techniques (e.g., all-epiphyseal, transphyseal with smaller tunnels, or extraphyseal methods) are employed to minimize this risk, though their long-term efficacy and comparative outcomes are still under investigation.
- PCL Reconstruction Techniques: Debates persist regarding single vs. double bundle, and transtibial vs. tibial inlay approaches. The tibial inlay technique is favored by many for its theoretical advantages in preventing graft impingement and improved biomechanics, but it is technically more demanding.
Professional Society Guidelines
Organizations such as the American Academy of Orthopaedic Surgeons (AAOS), the European Society of Sports Traumatology, Knee Surgery & Arthroscopy (ESSKA), and the International Society of Arthroscopy, Knee Surgery and Orthopaedic Sports Medicine (ISAKOS) regularly publish consensus statements and clinical practice guidelines. These guidelines provide evidence-based recommendations on diagnosis, surgical indications, graft selection, surgical techniques, and rehabilitation protocols. Key recommendations often emphasize:
* Preoperative rehabilitation to achieve full ROM.
* Individualized graft selection based on patient factors.
* Anatomical tunnel placement to restore knee kinematics.
* Structured, progressive post-operative rehabilitation.
* Objective criteria for return to sport.
Future Directions
Ongoing research focuses on several fronts:
*
Biologics:
The use of platelet-rich plasma (PRP), bone marrow aspirate concentrate (BMAC), or other growth factors to enhance graft healing and incorporation.
*
Enhanced Graft Materials:
Development of synthetic grafts or biologic scaffolds to improve strength, biocompatibility, and integration.
*
Sensor-Guided Surgery:
Intraoperative technologies to ensure precise tunnel placement and graft tensioning.
*
Personalized Rehabilitation:
Tailoring rehabilitation protocols based on individual patient biomechanics, genetics, and recovery patterns.
*
Prevention Strategies:
Further refining injury prevention programs to address modifiable risk factors in athletes.
Cruciate ligament injuries remain a challenging area in orthopaedics. Continued advancements in surgical techniques, rehabilitation strategies, and our understanding of knee biomechanics are crucial for optimizing outcomes and improving the long-term health of affected individuals.
You Might Also Like