ACL Rupture & Lateral Meniscus Tear: A Collegiate Soccer Player Case Study
Key Takeaway
Diagnosing an acute ACL rupture with a lateral meniscal tear involves a thorough clinical exam revealing a positive Lachman, Pivot Shift, and McMurray test, alongside joint effusion and mechanical block. MRI confirms complete ACL mid-substance rupture and complex lateral bucket-handle meniscal tear, often with a displaced fragment causing extension limitations.
Patient Presentation & History
A 22-year-old male collegiate soccer player presents to the emergency department following an acute knee injury sustained during a training session. The mechanism of injury was a non-contact, deceleration event involving a rapid change of direction, where he planted his left foot, pivoted, and experienced a sudden valgus collapse of the knee. He immediately reported hearing a distinct "pop" followed by severe pain and an inability to continue playing. Within an hour, the knee developed a significant effusion. He was unable to bear full weight on the limb due to pain and instability.
His past medical history is unremarkable, with no prior significant knee injuries or surgeries. He denies any history of systemic inflammatory arthropathy, coagulopathy, or neurological deficits. He is an active, competitive athlete with no relevant comorbidities or medications. He is a non-smoker and consumes alcohol occasionally. His primary goal is to return to high-level competitive soccer.
Clinical Examination
Upon initial assessment in the emergency department and subsequent clinic visit (after effusion reduction with aspiration), the following findings were noted:
Inspection
- Effusion: Moderate to large globular effusion of the left knee, tense to palpation. Hemarthrosis confirmed by aspiration of approximately 60 mL of sanguineous fluid.
- Ecchymosis: Mild, diffuse ecchymosis noted around the medial and lateral aspects of the knee, suggesting soft tissue trauma.
- Alignment: No gross deformity or malalignment was observed.
- Skin: Intact, no open wounds or abrasions.
Palpation
- Tenderness: Significant joint line tenderness along the lateral compartment, consistent with a meniscal injury. Diffuse tenderness over the medial and lateral suprapatellar pouches due to the effusion. No significant tenderness directly over the collateral ligaments or patellar tendon.
- Temperature: Mildly increased warmth over the affected knee.
- Swelling: Confirmed moderate to large effusion, boggy feel.
Range of Motion (ROM)
- Active ROM: Limited from 10° to 90° flexion due due to pain and mechanical block.
- Passive ROM: Painful and restricted, particularly at full extension (mechanical block preventing terminal extension, suspected bucket-handle meniscal tear) and deep flexion. Attempts to achieve full extension elicited a distinct catch.
Ligamentous Stability Tests
- Lachman Test: Markedly positive (Grade III, >10mm anterior translation with a soft endpoint) on the left knee compared to the right.
- Anterior Drawer Test: Positive with significant anterior tibial translation and a soft endpoint.
- Pivot Shift Test: Grossly positive (Grade III) with subluxation and reduction palpable and visible, indicating rotatory instability. This test was performed cautiously due to acute pain and apprehension but confirmed significant instability.
- Posterior Drawer Test / Posterior Sag Sign: Negative, ruling out significant PCL injury.
- Varus Stress Test: Negative at both 0° and 30° flexion, indicating an intact lateral collateral ligament complex.
- Valgus Stress Test: Negative at both 0° and 30° flexion, indicating an intact medial collateral ligament complex.
Meniscal Tests
- McMurray Test: Strongly positive with a painful click and palpable clunk upon extension from flexion with external rotation, localized to the lateral joint line, highly suggestive of a lateral meniscal tear, potentially a bucket-handle type given the extension block.
- Apley Grind Test: Positive for lateral meniscal pathology.
Neurological and Vascular Assessment
- Neurological: Intact sensation to light touch in the saphenous, common peroneal, and tibial nerve distributions. Motor function (dorsiflexion, plantarflexion, great toe extension, knee extension/flexion) was 5/5 bilaterally. No signs of foot drop or nerve palsy.
- Vascular: Palpable dorsalis pedis and posterior tibial pulses bilaterally, 2+ and symmetrical. Capillary refill was brisk (<2 seconds) in both feet. No signs of compartment syndrome.
Imaging & Diagnostics
Radiographs
Initial plain radiographs of the left knee were obtained immediately post-injury:
*
Anteroposterior (AP), Lateral, Oblique, and Patellar Views:
* No acute fracture or dislocation was identified.
* Tibiofemoral and patellofemoral joint spaces appeared preserved.
* No osteochondral defects were visible on plain films.
*
Segond fracture:
Notably absent, which would suggest an avulsion fracture of the lateral tibial plateau associated with an ACL tear.
* Presence of a moderate joint effusion was confirmed.
* Subtle widening of the lateral compartment could be inferred due to valgus stress at the time of injury, but this was not conclusive for a significant chondral or osseous injury on plain films.
`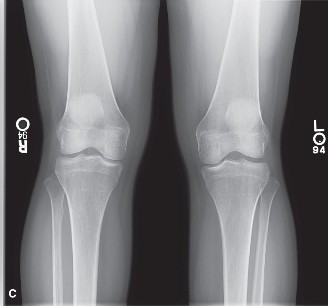`
*Figure 1: Lateral radiograph of the left knee demonstrating a moderate joint effusion (patellar fat pad effacement and suprapatellar pouch distension) with no obvious acute fracture or dislocation. Osseous alignment is preserved. This view helps rule out gross bony pathology.*
Magnetic Resonance Imaging (MRI)
An MRI of the left knee was performed within 48 hours of injury to delineate soft tissue pathology. The findings were highly significant:
*
Anterior Cruciate Ligament (ACL):
Complete mid-substance rupture of the ACL, with retraction of the femoral and tibial stumps. Diffuse edema within the femoral notch and intercondylar region.
*
Menisci:
A complex bucket-handle tear of the lateral meniscus, with a displaced fragment in the intercondylar notch, consistent with the observed mechanical block to extension. No significant tear of the medial meniscus.
*
Chondral Surfaces:
A focal, grade II chondral defect (ICRS classification) on the lateral femoral condyle, approximately 8 mm in diameter, with underlying subchondral bone marrow edema. No significant defects on the tibial plateau or patellofemoral joint.
*
Collateral Ligaments:
Intact medial and lateral collateral ligaments (MCL and LCL complexes) with no evidence of sprain or rupture.
*
Posterior Cruciate Ligament (PCL):
Intact and unremarkable.
*
Bone Contusions:
Extensive bone marrow edema (bone bruise) in the lateral femoral condyle and posterolateral tibial plateau, consistent with the "kissing lesions" seen with pivot-shift injuries.
*
Effusion:
Confirmed moderate to large hemarthrosis.
``
*Figure 2: Sagittal T2-weighted MRI sequence of the left knee demonstrating a complete rupture of the anterior cruciate ligament (arrowheads pointing to retracted stumps), with associated bone bruising (asterisks) in the lateral femoral condyle and posterolateral tibial plateau. Note the abnormal signal and morphology of the lateral meniscus suggestive of a complex tear (not fully visible in this specific cut but indicative of significant intra-articular pathology).*
Pre-operative Templating
Based on the MRI, a pre-operative templating process was initiated:
*
Graft Choice:
Autologous hamstring tendon (semitendinosus and gracilis) was chosen as the preferred graft for ACL reconstruction due to its excellent biomechanical properties, low donor site morbidity, and suitability for high-demand athletes. Alternative considerations included bone-patellar tendon-bone (BPTB) or quadriceps tendon autografts.
*
Tunnel Placement:
Careful planning for anatomical tunnel placement was performed to ensure isometric graft positioning and minimize impingement. The femoral tunnel was planned for an anteromedial portal technique, aiming for the anatomical footprint of the ACL. The tibial tunnel was planned to avoid posterior notching and ensure adequate obliquity.
*
Meniscal Repair:
The lateral meniscal bucket-handle tear was deemed repairable given the patient's age, activity level, and the tear characteristics (longitudinal, peripheral, red-red zone). An all-inside repair technique was anticipated.
*
Chondral Management:
The focal chondral defect on the lateral femoral condyle necessitated a plan for microfracture or debridement, depending on its depth and stability observed arthroscopically.
Differential Diagnosis
Given the acute knee injury with effusion, mechanical symptoms, and instability, several diagnoses were considered:
| Feature | Acute ACL Rupture (with associated injuries) | Isolated Meniscal Tear (e.g., Bucket-Handle) | Patellar Dislocation (Lateral) | PCL Rupture (Isolated or Multiligamentous) |
|---|---|---|---|---|
| Mechanism of Injury | Non-contact pivot, valgus collapse, hyperextension; contact mechanisms also possible. | Twisting injury on a flexed knee, squatting. | Direct blow to patella, forceful quadriceps contraction with valgus stress, rapid deceleration with rotation. | Direct blow to anterior tibia with knee flexed (dashboard injury); hyperextension, hyperflexion with axial load. |
| "Pop" Sensation | Highly common (70-90%). | Variable, less common than ACL; may occur with acute displacement. | Common, often described as a "clunk" as patella dislocates/relocates. | Less common than ACL, but possible. |
| Effusion | Rapid, often hemarthrosis. | Variable, usually delayed, rarely hemarthrosis unless associated chondral or ligamentous injury. | Rapid, often hemarthrosis, especially with osteochondral injury. | Variable, often hemarthrosis with acute injury. |
| Mechanical Symptoms | Giving way, instability (especially on pivoting). Less common for locking unless associated meniscal tear. | Locking, catching, clicking, pain with twisting. | Pseudolocking due to pain and apprehension; feeling of knee "giving out." | Posterior instability, difficulty ascending/descending stairs, feeling of "giving way" backward. |
| ROM | Restricted due to pain/effusion. May have extension block if meniscal tear. | Often restricted by mechanical block (e.g., bucket-handle). | Restricted due to pain, apprehension, usually unable to fully extend. | May have hyperextension instability, or limited flexion due to effusion. |
| Lachman Test | Positive (soft/absent endpoint, increased translation) | Negative (unless associated ACL tear). | Negative (unless associated ACL tear). | Negative (unless associated ACL tear). |
| Anterior Drawer | Positive (soft/absent endpoint, increased translation) | Negative (unless associated ACL tear). | Negative (unless associated ACL tear). | Negative (unless associated ACL tear). |
| Pivot Shift Test | Positive (gross subluxation and reduction) | Negative (unless associated ACL tear). | May be difficult to assess due to pain, but negative for ACL. | Negative for ACL. |
| Posterior Sag/Drawer | Negative. | Negative. | Negative. | Positive (posterior sag, increased posterior translation) . |
| Meniscal Tests | May be positive if concomitant meniscal injury. | Positive (McMurray, Apley) | Negative. | Negative (unless associated meniscal tear). |
| Patellar Apprehension | Negative. | Negative. | Positive (strong apprehension with lateral patellar translation) | Negative. |
| X-ray Findings | May show Segond fracture, avulsion fracture, or effusion. Otherwise often normal. | Usually normal, may show effusion. | May show patellar maltracking, lateral displacement/subluxation, osteochondral fracture of patella or lateral femoral condyle. | May show PCL avulsion, sag sign on lateral views. |
| MRI Findings | ACL rupture, bone bruise (lateral femoral condyle/posterolateral tibia) , frequently associated meniscal tears. | Meniscal tear (various types: bucket-handle, radial, horizontal). Often isolated if no other ligamentous injury. | Patellar dislocation/subluxation, MPFL rupture, osteochondral injury, bone marrow edema. | PCL rupture, often associated with posterolateral corner or medial-sided injuries. |
Based on the clinical examination (grossly positive Lachman, Anterior Drawer, and Pivot Shift tests, distinct mechanical block to extension, and positive lateral McMurray) and confirmed by MRI findings (complete ACL rupture, lateral meniscal bucket-handle tear, and focal chondral defect), the diagnosis of a complex acute ACL rupture with concomitant lateral meniscal bucket-handle tear and chondral injury was definitively made.
Surgical Decision Making & Classification
The decision for operative intervention in this case was straightforward and guided by several factors:
1.
Patient Age and Activity Level:
A 22-year-old collegiate athlete with high functional demands and a strong desire to return to competitive soccer. Non-operative management of an ACL rupture would result in persistent instability and high risk of recurrent giving-way episodes, leading to secondary meniscal tears and articular cartilage damage.
2.
Degree of Instability:
Gross rotatory instability (Grade III Pivot Shift) confirmed on examination, indicating a functionally unstable knee.
3.
Concomitant Injuries:
*
Lateral Meniscal Bucket-Handle Tear with Displacement:
This mechanical block to extension requires urgent reduction and repair to prevent further damage to the meniscus and articular cartilage, restore knee kinematics, and improve long-term joint health. Unrepaired bucket-handle tears can lead to progressive articular degeneration.
*
Focal Chondral Defect:
While not an absolute indication for immediate surgery, its presence mandates addressing during the primary procedure to prevent progression.
4.
Failure of Conservative Management:
Acute hemarthrosis and a mechanical block preclude effective conservative rehabilitation in the acute phase.
Classifications Utilized:
- ACL Injury: Classified as a complete mid-substance rupture. The International Knee Documentation Committee (IKDC) Subjective Knee Evaluation Form would be used pre-operatively to quantify symptoms and prospectively assess outcomes post-operatively. Objectively, the IKDC Knee Examination Form would grade the Lachman and Pivot Shift tests.
- Meniscal Tear: A bucket-handle tear of the lateral meniscus, which is a specific type of longitudinal tear often characterized by displacement of the central fragment into the intercondylar notch. These are typically amenable to repair, especially in younger patients with acute tears in vascularized zones (red-red or red-white).
- Chondral Defect: The focal chondral defect on the lateral femoral condyle was graded as ICRS Grade II , indicating a lesion extending into the cartilage but not breaching the subchondral bone, with a depth of less than 50% of the cartilage thickness.
The comprehensive plan involved arthroscopic ACL reconstruction , arthroscopic lateral meniscal repair , and arthroscopic microfracture (or debridement) of the chondral lesion. This multi-pronged approach addressed all significant pathologies identified, aiming to restore knee stability, preserve meniscal function, protect articular cartilage, and facilitate a successful return to sport.
Surgical Technique / Intervention
The surgical procedure was performed approximately 10 days post-injury, allowing time for initial swelling to subside and for thorough pre-operative planning.
Patient Positioning
The patient was placed supine on the operating table. A pneumatic tourniquet was applied to the proximal thigh of the operative limb. A padded lateral post was positioned proximal to the fibular head. The foot was secured in a commercially available leg holder to allow for controlled knee flexion and extension and application of valgus stress. This setup facilitates full arthroscopic visualization and instrument access. The contralateral limb was positioned in a well-padded frog-leg fashion.
Approach & Diagnostic Arthroscopy
Standard anteromedial (AM) and anterolateral (AL) portals were established. A comprehensive diagnostic arthroscopy was performed, confirming all pre-operative findings:
*
Effusion:
Significant hemarthrosis was evacuated.
*
ACL:
Complete mid-substance rupture of the ACL, with the remnants appearing frayed and retracted into the femoral notch.
*
Lateral Meniscus:
A large, displaced bucket-handle tear of the lateral meniscus was clearly visualized. The central fragment was incarcerated in the intercondylar notch, causing the observed mechanical block to full extension. The tear extended from the posterior horn to the anterior horn, largely within the red-red and red-white zones, making it amenable to repair.
*
Chondral Lesion:
The focal ICRS Grade II chondral defect on the lateral femoral condyle was confirmed, measuring approximately 8 mm in diameter, with some mild fraying at its edges. The defect was stable and not completely delaminated.
*
Other Structures:
PCL, MCL, LCL, medial meniscus, and patellofemoral joint appeared intact.
Meniscal Repair
The first step was to address the meniscal tear.
1.
Reduction:
The displaced bucket-handle fragment was gently reduced from the intercondylar notch back into its anatomical position using a probe. This immediately restored the ability to achieve full knee extension.
2.
Preparation:
The tear edges were debrided and lightly rasped to stimulate a healing response by creating fresh bleeding edges.
3.
Repair Technique:
An all-inside meniscal repair device (e.g., Fast-Fix or similar suture-based system) was chosen due to its efficiency and secure fixation. Multiple vertical mattress sutures were placed across the tear, starting from the posterior horn and progressing anteriorly, approximately 3-4 mm apart, ensuring adequate purchase of both the peripheral rim and the inner fragment. A total of five sutures were placed to provide stable reduction and compression of the tear. After each repair, the knee was cycled through a full range of motion to assess the stability of the repair.
Chondral Lesion Management
Following meniscal repair, the focal chondral defect on the lateral femoral condyle was addressed.
1.
Debridement:
Unstable chondral edges were debrided to a stable rim using a shaver.
2.
Microfracture:
Since the lesion was ICRS Grade II and had underlying subchondral edema, indicating some localized trauma, microfracture was performed. An arthroscopic awl was used to create 3-4 microfracture holes, approximately 3-4 mm deep and 3-4 mm apart, in the subchondral bone at the base of the lesion. This aims to stimulate a superclot formation and subsequent fibrocartilage repair.
ACL Reconstruction
Graft Harvest:
* A 3 cm vertical incision was made over the anteromedial aspect of the proximal tibia.
* The semitendinosus and gracilis tendons were harvested using an open-ended tendon stripper. Care was taken to preserve their insertions distally for adequate length.
* The tendons were prepared on a graft-prep station, quadruple-folded to create a 4-strand graft, typically yielding a diameter of 8-9 mm. The graft was pre-tensioned for 10 minutes at 150 N.
Femoral Tunnel Creation:
* An anteromedial (AM) portal was used to create the femoral tunnel. This allows for a more anatomical tunnel placement compared to a transtibial technique.
* A femoral aimer was used to guide a guide pin into the anatomical footprint of the ACL on the lateral femoral condyle, aiming for the posterolateral bundle's insertion site. The goal was 10:30 o'clock position in the right knee, 1:30 o'clock in the left, approximately 7-8 mm from the posterior articular margin.
* A cannulated reamer corresponding to the graft diameter (e.g., 8.5 mm) was used to drill the femoral socket, typically 25-30 mm deep, leaving a cortical bridge of 1-2 mm.
Tibial Tunnel Creation:
* An ACL tibial aimer was used via the AM portal to guide a guide pin into the anatomical tibial footprint, aiming for the center of the ACL footprint, anterior to the PCL insertion and posterior to the anterior horn of the lateral meniscus.
* The cannulated reamer was then used to create the tibial tunnel, also corresponding to the graft diameter. Care was taken to avoid posterior wall blowout and anterior impingement.
Graft Passage & Fixation:
* A suture passer was used to retrieve the sutures attached to the femoral end of the graft through the femoral tunnel.
* The graft was then pulled into the femoral tunnel.
*
Femoral Fixation:
A cortical suspension device (e.g., Endobutton) was used for femoral fixation. The loop of the device was passed through the femoral tunnel and flipped on the lateral cortex of the femur, securing the graft within the femoral socket. The graft was then tensioned.
*
Tibial Fixation:
The graft was then pulled into the tibial tunnel under constant tension. The knee was cycled several times to remove any slack and to confirm isometric graft placement. With the knee held at 20-30° flexion, maximum manual tension was applied to the graft. Tibial fixation was achieved using an interference screw (e.g., bioabsorbable PLLA or PEEK) alongside the graft in the tibial tunnel. Alternatively, a washer-staple or post-tie method could be used, but an interference screw provides robust primary fixation.
Final Assessment:
* Arthroscopic visualization confirmed anatomical graft placement, proper tension, and no impingement in full extension or flexion.
* Lachman and Pivot Shift tests were performed arthroscopically and clinically, demonstrating excellent stability with a firm endpoint.
* The meniscal repair was stable with knee range of motion.
Wound Closure
Portals were closed with simple sutures (e.g., 3-0 nylon). The hamstring harvest site was closed in layers. A sterile dressing was applied, and the knee was placed in a hinged knee brace locked in full extension.
Post-Operative Protocol & Rehabilitation
The post-operative rehabilitation protocol is critical for a successful outcome and is typically phased:
Phase I: Acute Protection & Early Motion (Weeks 0-6)
- Weight-Bearing: Touch-down weight-bearing (TDWB) with crutches for the first 2-4 weeks to protect the meniscal repair and chondral microfracture site. Progress to partial weight-bearing (PWB) as tolerated, gradually weaning off crutches by week 4-6, provided no pain or effusion.
- Bracing: Hinged knee brace locked in full extension for ambulation for 2-4 weeks, then unlocked for ROM exercises. The brace is typically worn for 6 weeks, providing protection against valgus/varus stress and hyperflexion/hyperextension.
-
Range of Motion:
- Goal of 0-90° flexion by week 2, progressing to 0-120° by week 4, and full ROM by week 6. Emphasis on achieving full passive extension early to prevent arthrofibrosis.
- Avoid isolated active hamstring contractions for 6-8 weeks (for hamstring autograft) to protect the healing harvest site.
- Pain & Swelling Management: Cryotherapy, NSAIDs, elevation.
- Exercises: Quadriceps sets, straight leg raises (SLR) in all planes (with brace), ankle pumps, gentle patellar mobilizations. Core strengthening.
Phase II: Intermediate Strengthening & Neuromuscular Control (Weeks 6-12)
- Weight-Bearing: Full weight-bearing as tolerated. Discontinue crutches and brace once ambulating without a limp and knee motion is acceptable.
- Range of Motion: Full, pain-free ROM expected.
-
Strengthening:
- Open-chain knee extension (0-45° for quads, avoid hyperextension).
- Closed-chain exercises: Wall squats, mini-squats, step-ups, leg press.
- Hamstring strengthening (gentle at 6 weeks, progressive after 8 weeks).
- Calf raises.
- Neuromuscular Control: Balance and proprioception exercises (e.g., single leg stance, wobble board, balance disc).
- Cardiovascular: Stationary cycling (high seat initially), elliptical trainer.
Phase III: Advanced Strengthening & Sport-Specific Training (Months 3-6)
- Strengthening: Progressive resistance training, plyometrics (box jumps, cone drills), agility drills (cutting, weaving). Increase intensity and complexity.
- Running Progression: Begin with straight-line jogging, gradually progressing to controlled running, then multi-directional running.
- Neuromuscular Control: Advanced balance and proprioception. Introduction of sport-specific drills (e.g., soccer specific agility, kicking mechanics).
- Functional Testing: Single leg hop tests, triple hop, crossover hop tests.
- Criteria for Progression: No pain, no effusion, full ROM, symmetric strength >85-90% of contralateral limb, excellent neuromuscular control.
Phase IV: Return to Sport (Months 6-12+)
- Sport-Specific Training: Full participation in sport-specific drills without restriction, progressively increasing intensity and duration.
- Psychological Readiness: Address any apprehension or fear of re-injury.
-
Return to Play (RTP) Criteria:
Typically not before 9-12 months post-operatively for competitive pivoting sports. Criteria include:
- No pain, no effusion.
- Full, symmetric ROM.
- Isokinetic strength testing (quads and hamstrings) >90% of contralateral limb, and hamstring-to-quadriceps ratio >60%.
- Successful completion of functional hop testing, >90% limb symmetry index (LSI).
- No residual laxity on clinical examination (negative Pivot Shift, firm Lachman).
- Demonstrated proficiency in sport-specific agility and cutting maneuvers.
- Psychological readiness score (e.g., ACL-RSI >70%).
Close collaboration between the surgeon, physical therapist, and athletic trainer is paramount throughout the rehabilitation process to optimize outcomes and minimize the risk of re-injury.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls
- Thorough Clinical Examination: Despite acute pain and effusion, a systematic examination (Lachman, Pivot Shift, McMurray) is crucial for accurate diagnosis. Aspiration of a tense hemarthrosis can facilitate a more accurate examination.
- High Index of Suspicion for Concomitant Injuries: An acute ACL tear rarely occurs in isolation. Always look for meniscal tears (especially bucket-handle with mechanical block), chondral lesions, collateral ligament injuries, and bone bruising. MRI is essential for this.
- Timely Meniscal Repair: Displaced meniscal tears, particularly bucket-handle lesions in younger, active patients, require urgent reduction and repair to prevent ongoing damage, alleviate mechanical symptoms, and preserve meniscal function. Delay can lead to irreparable tears.
- Anatomical ACL Reconstruction: Anatomical tunnel placement (femoral and tibial) is paramount for restoring rotational stability and preventing impingement. The AM portal technique for femoral tunnel drilling is preferred for anatomical placement.
- Graft Choice: Autografts (hamstring, BPTB, quadriceps) remain the gold standard for primary ACL reconstruction in young, active individuals. Discuss patient preference, activity level, and potential donor site morbidity.
- Addressing Chondral Lesions: Even small chondral defects identified should be addressed during surgery. Microfracture is a viable option for smaller, contained defects in appropriate locations.
- Aggressive Early Full Extension: Critical for preventing arthrofibrosis and promoting normal gait mechanics. Patients should achieve full passive extension within the first few weeks.
- Multi-disciplinary Rehabilitation: A structured, progressive, and individualized rehabilitation program, guided by a physical therapist, is as important as the surgery itself. Communication between the surgeon, PT, and patient is vital.
- Evidence-Based Return to Sport: Adhere to objective criteria (strength, hop tests, psychological readiness) rather than solely time-based protocols for return to high-demand sports. Premature return to sport significantly increases the risk of re-rupture.
Pitfalls
- Missed Concomitant Injuries: Failing to identify and address associated meniscal tears, collateral ligament injuries, or chondral defects can lead to persistent pain, instability, and accelerated osteoarthritis.
-
Non-anatomical Tunnel Placement:
- Anterior Femoral Tunnel: Leads to graft impingement in extension, loss of flexion, and graft failure due to over-tensioning.
- Posterior Tibial Tunnel (Cyclops Lesion): Leads to graft impingement in flexion, loss of flexion, and potential for scar formation causing extension loss.
- Vertical Tibial Tunnel: Fails to restore rotational stability.
- Inadequate Meniscal Repair: Insufficient sutures, poor tissue quality, or delayed repair can lead to repair failure and persistent mechanical symptoms.
- Ignoring the Chondral Defect: Untreated, unstable chondral lesions can progress to larger defects, leading to accelerated degeneration.
- Infection: A rare but devastating complication. Strict aseptic technique is essential.
- Arthrofibrosis/Stiffness: Can result from aggressive early flexion without adequate extension, delayed surgery in the presence of severe inflammation, or inadequate rehabilitation. Early, gentle ROM, especially extension, is key.
- Graft Failure/Re-rupture: Can be due to technical errors (malpositioning, inadequate fixation), inadequate rehabilitation, or premature return to high-risk activities.
- Neurovascular Injury: Although rare, direct injury to the common peroneal nerve or popliteal artery can occur during tunnel drilling or hardware placement. Careful anatomical awareness and portal placement are crucial.
- Donor Site Morbidity: For autografts, issues such as hamstring weakness, numbness (saphenous nerve), or patellofemoral pain (BPTB graft) can occur.
- Residual Instability: May occur despite technically sound surgery if underlying kinematic derangements are not fully addressed or if rehabilitation is suboptimal.
- Post-Traumatic Osteoarthritis: Despite successful reconstruction and meniscal repair, the knee remains at higher risk for long-term degenerative changes. Patient education regarding this risk is important.
You Might Also Like