Congenital Coxa Vara and Pelvic Osteotomies: Advanced Surgical Management
Key Takeaway
Congenital and developmental coxa vara are complex pediatric hip deformities characterized by a progressive decrease in the femoral neck-shaft angle. Left untreated, biomechanical forces exacerbate the varus deformity, potentially leading to pseudarthrosis. This comprehensive guide details the pathophysiology, indications, and step-by-step surgical technique for subtrochanteric valgus osteotomy, alongside the management of associated pelvic anomalies such as bladder exstrophy requiring anterior iliac osteotomies.
CONGENITAL AND DEVELOPMENTAL COXA VARA
The term congenital coxa vara encompasses a spectrum of proximal femoral deformities observed in infancy and early childhood. Clinically and prognostically, it is subdivided into two distinct typologies. The first type is present at birth, is exceedingly rare, and is typically syndromic—frequently associated with severe congenital anomalies such as proximal femoral focal deficiency (PFFD) or systemic conditions like cleidocranial dysostosis.
The second type, more accurately termed developmental coxa vara, is significantly more common. It is usually insidious, remaining undetected until the child begins to ambulate. Unlike the syndromic variant, developmental coxa vara is generally an isolated anomaly, with the only potential concurrent abnormality being a congenitally short femur.
Pathophysiology and Biomechanics
Coxa vara, which is frequently bilateral, is pathognomonically characterized by a progressive decrease in the angle between the femoral neck and the femoral shaft (neck-shaft angle), accompanied by progressive limb shortening. The hallmark anatomical lesion is a distinct defect in the medial aspect of the femoral neck.
Microscopic analysis of this medial defect reveals a disorganized matrix of cartilage. The normal columnar arrangement of chondrocytes is highly irregular, and endochondral ossification within this zone is profoundly atypical, closely resembling a dysplastic or abnormal physis. The adjacent metaphyseal bone is markedly osteoporotic, characterized by atrophic trabeculae that occasionally harbor large, ectopic islands of cartilage cells.
Biomechanical Pitfall: The pathophysiology of coxa vara is driven by a vicious biomechanical cycle. When the child begins walking, the physiological load across the hip joint increases. Because the dysplastic femoral neck is structurally compromised, the normal compressive forces are converted into pathological shear forces across the verticalized physis. This shear stress inhibits normal ossification (Heuter-Volkmann principle) and drives the progressive varus deformity.
As the patient ages and gains weight, the mechanical disadvantage worsens. The deformity progresses relentlessly until the greater trochanter eventually overrides the femoral head, leading to severe abductor insufficiency (Trendelenburg gait). If left untreated, the shear forces can culminate in a frank pseudarthrosis of the femoral neck. In neglected adult cases, the greater trochanter may migrate several inches superior to the femoral head, resulting in wide separation of the head and neck fragments.
Clinical and Radiographic Evaluation
Early diagnosis is critical, as the likelihood of achieving a functionally normal hip diminishes precipitously after 8 years of age. Radiographic evaluation must include weight-bearing anteroposterior (AP) and frog-leg lateral views of the pelvis.

Key radiographic parameters include the neck-shaft angle and the Hilgenreiner epiphyseal angle (HEA). The HEA is the angle subtended by a horizontal line drawn through the triradiate cartilages (Hilgenreiner's line) and a line drawn parallel to the proximal femoral physis. A normal HEA is less than 25 degrees; an angle greater than 60 degrees is an absolute indication for surgical intervention due to the 100% rate of progression.
Indications for Surgical Intervention
The definitive treatment for developmental coxa vara is a subtrochanteric valgus osteotomy. The goal is to reorient the femoral neck and head into an appropriate valgus position relative to the femoral shaft, thereby converting pathological shear forces back into physiological compressive forces across the physis.
According to Beals, surgical intervention is strictly indicated under the following conditions:
* The coxa vara deformity is radiographically progressive.
* The condition is clinically painful.
* The deformity is unilateral, leading to significant pelvic obliquity.
* There is an associated, progressive leg-length discrepancy.
* The neck-shaft angle is 110 degrees or less.
Clinical Pearl: While early intervention is ideal to harness the remodeling potential of the proximal femur, surgery is often strategically delayed until the child is 4 to 5 years old. This delay allows for sufficient ossification and increased bone stock in the proximal femur, which drastically improves the purchase and stability of internal fixation devices.
Surgical Technique: Valgus Osteotomy for Developmental Coxa Vara
Preoperative Planning: Meticulous templating is required to determine the exact angle of the lateral closing wedge needed to achieve a postoperative neck-shaft angle of 140 to 150 degrees, and a postoperative HEA of less than 38 degrees.
Step-by-Step Procedure (Technique 27-14):
- Soft Tissue Release: Begin by performing a percutaneous or mini-open adductor tenotomy through a small medial incision. This is a critical step to relieve medial tension, prevent lateral subluxation of the femoral head during the valgus correction, and reduce compressive forces across the hip joint.
- Surgical Approach: Expose the greater trochanter and the proximal shaft of the femur through an 8- to 10-cm direct lateral, longitudinal incision. Elevate the vastus lateralis to expose the subtrochanteric region.
- Guidewire and Implant Insertion: If utilizing a pediatric screw and side-plate device (or a specialized pediatric blade plate), insert the primary guidewire into the midline of the femoral neck under strict biplanar fluoroscopic guidance (image intensification).
- Trajectory: Insert the screw as close as possible to the trochanteric apophysis without violating it, to avoid iatrogenic growth arrest.
- Depth: Ideally, center the screw in the femoral neck distal to the abnormal physis. If the neck is too short or dysplastic, the screw must be advanced across the physis and centered securely within the femoral head.
- The Osteotomy: Perform a transverse osteotomy slightly distal to the entry point of the screw, approximately at the level of the lesser trochanter.
- Deformity Correction: Resect a pre-calculated small lateral wedge of bone from the distal fragment. Reduce the osteotomy, bringing the femoral shaft into abduction to close the wedge, thereby correcting the neck-shaft angle to the targeted 140 to 150 degrees.
- Fixation: Secure the side plate to the femoral shaft using cortical screws in standard compression fashion. Ensure rigid internal fixation.
- Closure: Thoroughly irrigate the surgical bed. Close the wound in anatomical layers. Insert a subfascial irrigation-suction drain if significant dead space or bleeding is present.
- Immobilization: Apply a one-and-one-half spica cast to protect the fixation and neutralize rotational forces during the early healing phase.
Postoperative Protocol and Outcomes
The spica cast is typically maintained for 8 to 12 weeks, pending radiographic confirmation of bridging callus and osteotomy union. Following cast removal, aggressive physical therapy is initiated to restore hip abductor strength and range of motion.
Recurrence and Prognosis:
Regardless of the osteotomy technique or fixation method, developmental coxa vara carries a notorious risk of recurrence. Children must be monitored clinically and radiographically at regular intervals until skeletal maturity.
A landmark study by Carroll, Coleman, and Stevens evaluated 26 patients undergoing valgus osteotomies for coxa vara and found a 50% overall recurrence rate. Crucially, they determined that etiology, age at surgery, osteotomy type, and implant choice had no bearing on recurrence. The single defining prognostic factor was the postoperative Hilgenreiner epiphyseal angle (HEA).
* 95% of patients whose HEA was corrected to less than 38 degrees experienced no recurrence of varus.
* The traditional head-shaft angle proved highly unreliable for determining the adequacy of correction; two-thirds of patients corrected to >135 degrees still recurred, while one-third corrected to <135 degrees maintained satisfactory results.
Furthermore, a significant cohort of these children present with concurrent femoral hypoplasia. Progressive limb-length discrepancy must be monitored, as it may ultimately necessitate contralateral epiphysiodesis or ipsilateral limb lengthening procedures.
ASSOCIATED PELVIC ANOMALIES: BLADDER EXSTROPHY AND ILIAC OSTEOTOMIES
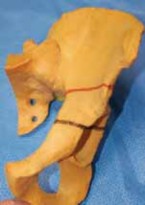
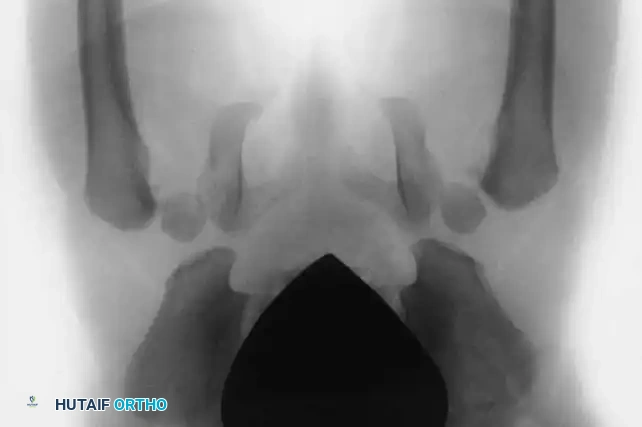
In addition to proximal femoral deformities, pediatric orthopaedic surgeons frequently manage complex pelvic anomalies, such as those involving the innominate bones in bladder exstrophy. Bladder exstrophy is a severe congenital malformation characterized by a defect in the anterior abdominal wall and bladder, accompanied by profound diastasis of the symphysis pubis.
Biomechanical Implications of the Exstrophy Pelvis
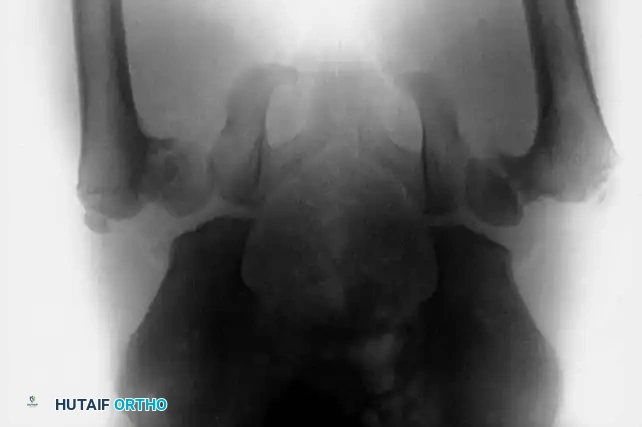
The skeletal hallmark of bladder exstrophy is the severe external rotation and lateral displacement of the innominate bones. This anatomical distortion results in a retroverted, laterally displaced acetabulum. If left uncorrected, the child will develop a pathognomonic wide-based, waddling, and externally rotated gait. Furthermore, this pelvic dysplasia is frequently associated with other orthopaedic anomalies, including developmental dysplasia of the hip (DDH), congenital hip dislocation, and myelomeningocele.
Anterior Iliac Osteotomies and Approximation of the Symphysis Pubis
Because the majority of the urological structures in exstrophy patients are present (albeit bifid or exposed), functional urological reconstruction is achievable. However, isolated soft-tissue closure of the bladder and abdominal wall is doomed to fail unless the underlying skeletal diastasis is addressed.
Surgical Warning: Attempting urological reconstruction without approximating the symphysis pubis places immense, unsustainable tension on the soft-tissue repair. This invariably leads to catastrophic complications, including wound dehiscence, fistula formation, and complete bladder prolapse.
To relieve this tension, orthopaedic intervention is required to mobilize the innominate bones and close the pelvic ring.
Evolution of Surgical Techniques:
Historically, O’Phelan championed bilateral posterior iliac osteotomies combined with symphyseal approximation. While effective, this required intraoperative repositioning (flipping) of the patient, increasing anesthesia time and infection risk.
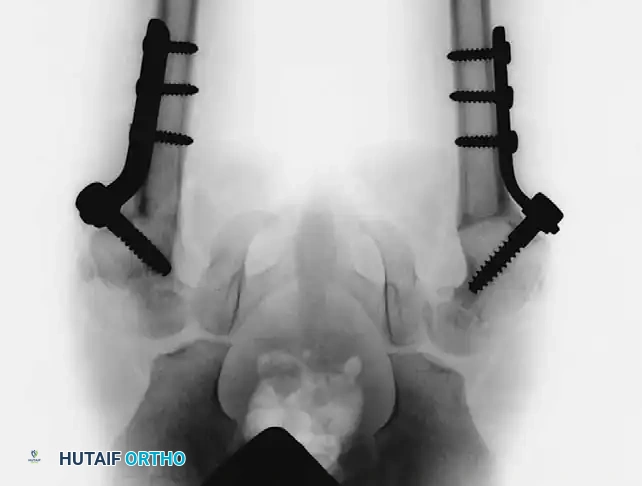
Currently, the gold standard, as recommended by Sponseller et al., is the use of bilateral anterior iliac osteotomies stabilized with internal or external fixation.
* Advantages: Anterior osteotomies provide superior mobility of the pubic rami, allow for greater correction of the diastasis, and completely avoid the need to turn the patient under anesthesia.
* Postoperative Care: In Sponseller's series of 82 patients, postoperative traction was deemed unnecessary in the vast majority of cases.
* Complications: Wound dehiscence or bladder prolapse occurred in only 4% of patients. The most notable orthopaedic complication was transient palsy of the femoral nerve, observed in seven children, which typically resolved spontaneously. Long-term data indicates that children who are slightly older at the time of the osteotomy tend to maintain their skeletal correction better over time.
Multidisciplinary Coordination and Long-Term Outcomes
The management of bladder exstrophy requires seamless coordination between pediatric urology and orthopaedic surgery. The reconstruction is typically performed as a single, unified operative procedure:
1. Orthopaedic Phase I: Bilateral anterior iliac osteotomies.
2. Urological Phase: Repair of the bladder, urethra, and anterior abdominal wall structures.
3. Orthopaedic Phase II: Approximation and secure fixation of the symphysis pubis using heavy, nonabsorbable sutures or orthopedic pins, closing the pelvic ring over the urological repair.
Complication Profiles:
In a massive retrospective review of 624 bladder exstrophy repairs, Okubadejo, Sponseller, and Gearhart reported an overall orthopaedic complication rate of 4% (26 patients). These complications were stratified into five distinct categories:
* Neurologic complications at the osteotomy site (50%)
* Bony complications/nonunion at the osteotomy site (19%)
* Complications related to postoperative traction (15%)
* Deep surgical site infections (8%)
* Late-onset infections (8%)
Determinants of Success:
Achieving a successful primary closure is highly complex. Kasat and Borwankar identified 11 critical factors necessary for optimal outcomes in exstrophy reconstruction:
1. Strict and proper patient selection.
2. Utilization of a staged reconstructive approach when necessary.
3. Anterior approximation of the pubic bones to allow deep placement of the bladder and urethra within the true pelvis.
4. Execution of posterior or anterior bilateral iliac osteotomies when the diastasis dictates.
5. Meticulous double-layered closure of the bladder.
6. Maintenance of proper ureteric catheter drainage for a minimum of 2 weeks.
7. Aggressive perioperative infection prevention protocols.
8. Prolonged, rigid postoperative immobilization (typically via spica casting or external fixation).
9. Prompt, emergent treatment of any impending bladder prolapse.
10. Prevention of postoperative abdominal distention (using nasogastric decompression).
11. Definitive ruling out of bladder outlet obstruction prior to the removal of the primary bladder catheter.
Through meticulous preoperative planning, precise execution of complex osteotomies, and rigorous multidisciplinary postoperative care, orthopaedic surgeons can successfully alter the natural history of both congenital coxa vara and the exstrophy pelvis, providing these children with stable, functional, and pain-free ambulation.
You Might Also Like