Comprehensive Management of Peripheral Nerve Injuries in the Hand

Key Takeaway
Peripheral nerve injuries in the hand demand meticulous clinical evaluation and precise microsurgical reconstruction. This comprehensive guide details the preoperative assessment of sensory and motor deficits, indications for primary versus secondary repair, and step-by-step surgical techniques for median, ulnar, and digital nerve lesions. Emphasizing evidence-based protocols, it provides orthopedic surgeons with the critical biomechanical and anatomical insights necessary to optimize nerve regeneration and restore functional outcomes.
Introduction to Peripheral Nerve Injuries
The management of peripheral nerve injuries in the upper extremity remains one of the most technically demanding and biologically complex challenges in orthopedic surgery. Successful restoration of sensory and motor function dictates the ultimate utility of the hand following trauma. This requires a profound understanding of neuroanatomy, Wallerian degeneration, axonal regeneration, and advanced microsurgical techniques.
The clinical deficit must be meticulously defined before any surgical exploration. Careful evaluation, especially in the presence of a closed injury, establishes the baseline deficit, allowing for the accurate assessment of progress if observation is elected over immediate exploration.
Preoperative Assessment
A systematic and highly detailed preoperative assessment is mandatory. The evaluation must differentiate between complete transections (neurotmesis), crush injuries (axonotmesis), and physiological conduction blocks (neurapraxia).
Type of Injury
The mechanism of injury dictates the surgical timeline and prognosis. Sharp, clean lacerations (e.g., glass or knife wounds) are amenable to primary repair. Crush injuries, avulsions, or high-velocity gunshot wounds often result in a zone of injury that extends proximally and distally, necessitating delayed repair or nerve grafting once the extent of intraneural fibrosis is demarcated. Closed partial ruptures of a common digital nerve in the palm may present with ambiguous signs; in such cases, advanced imaging, including high-resolution MRI, and subsequent surgical exploration may be required for a definitive diagnosis.
Sensibility Evaluation
The customary methods used to evaluate damaged sensory nerves must be applied systematically across specific autonomous zones.
* Pain: Assessed using a sharp pin.
* Light Touch: Assessed using a cotton-tipped applicator or a finger eraser.
* Two-Point Discrimination (2PD): Assessed using the tips of a paper clip or a commercially prepared tool (e.g., Disk-Criminator).
Normal static two-point discrimination is usually 6 mm or less at the fingertips. If a nerve is completely transected, the patient will not feel light touch, will not appreciate the pin as a sharp stimulus, and will be unable to discriminate between one and two points. Patients with closed injuries or partial nerve injuries may demonstrate spotty appreciation of light touch and pain, accompanied by markedly widened two-point discrimination.

Clinical Pearl: Always test sensibility before administering any local anesthetic. In uncooperative patients or young children, the wrinkle test (immersion in warm water for 30 minutes) can objectively confirm denervation, as denervated skin will fail to wrinkle.
Motor Function Evaluation
Accurate motor testing requires isolating specific muscle functions and eliminating trick movements caused by synergistic muscles.
Median Nerve
The median nerve innervates the pronator teres, flexor carpi radialis (FCR), palmaris longus, flexor digitorum superficialis (FDS), index and middle flexor digitorum profundus (FDP), flexor pollicis longus (FPL), and pronator quadratus (PQ) in the forearm. In the hand, the median-innervated muscles of primary concern include:
* Lumbricals to the index and long fingers
* Opponens pollicis
* Abductor pollicis brevis (APB)
* Superficial head of the flexor pollicis brevis (FPB)
The single most reliable median nerve–mediated motor function to evaluate is the apposition of the tip of the thumb to the pulp of the ring or little finger. This must be accompanied by direct palpation of the active contraction of the APB muscle belly to supplement visual inspection and rule out trick movements by the FPL or adductor pollicis.


Ulnar Nerve
The muscles proximally innervated by the ulnar nerve include the flexor carpi ulnaris (FCU) and the FDP tendons to the ring and little fingers. In the hand, the ulnar-innervated muscles include:
* Deep head of the flexor pollicis brevis (FPB)
* Adductor pollicis
* Abductor digiti minimi (ADM)
* Flexor digiti minimi (FDM)
* Opponens digiti minimi (ODM)
* All dorsal and volar interosseous muscles
* Lumbricals to the ring and little fingers
When testing for ulnar motor function, observe active abduction of the middle finger from the ulnar to the radial side with the palm resting flat on a surface.
Surgical Warning: This motion must be observed carefully to exclude the functions of the long flexor tendons (which converge the digits, mimicking volar interossei) and the long extensor tendons (which diverge the fingers, mimicking dorsal interossei).
Thumb adduction is tested via Froment's sign: have the patient maintain a piece of paper tightly in the thumb-index web, squeezing it between the thumb interphalangeal joint and the base of the index proximal phalanx. If the adductor pollicis is paralyzed, the patient will hyperflex the thumb IP joint (using the FPL) to hold the paper against resistance.
The function of the ADM is tested by having the patient abduct the little finger against resistance while palpating the muscle belly. Although "clawing" (hyperextension of the MCP joints and flexion of the IP joints) of the little and ring fingers may not be immediately apparent at the time of an acute injury, careful observation will eventually reveal this intrinsic-minus posture.


Radial Nerve
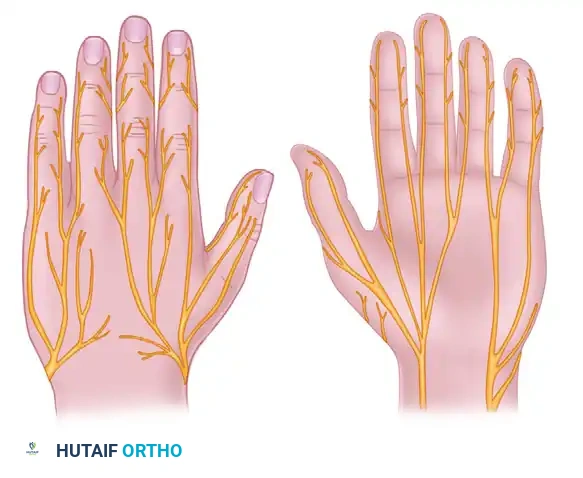
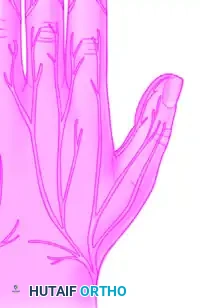
While primarily a motor nerve in the forearm (extending the wrist, digits, and thumb), its sensory distribution in the hand covers the dorsal-radial aspect. Evaluation of the superficial radial nerve is strictly sensory.

Pitfall: Anatomical variations, such as Martin-Gruber anastomoses (forearm) or Riche-Cannieu anastomoses (palm), cause cross-innervation of muscles usually innervated by the median or ulnar nerves. These must be kept in mind to avoid misdiagnosing a complete nerve transection as a partial injury.
Sudomotor Function
Sudomotor (sympathetic) function is lost in denervated autonomous zones, leading to anhidrosis (lack of sweating). The Ninhydrin sweat test or the O'Riain wrinkle test can objectively confirm the loss of sympathetic innervation, which is particularly useful in pediatric or malingering patients.
Timing of Nerve Repair
Primary and Delayed Primary Nerve Repair
Primary repair is performed within the first 5 to 7 days post-injury. It is indicated for sharp, clean lacerations where the nerve ends can be approximated without tension. Delayed primary repair (1 to 3 weeks) is indicated when the wound is contaminated, or the patient's systemic condition precludes immediate lengthy microsurgery.
Secondary Nerve Repair
Secondary repair is performed after 3 weeks. It is indicated for crush injuries, avulsions, or gunshot wounds where the extent of intraneural scarring cannot be immediately determined. Waiting 3 to 6 weeks allows the zone of injury to demarcate, ensuring that resection of the neuroma and glioma reaches healthy fascicles before grafting or coaptation.
Principles of Nerve Suturing
The ultimate goal of nerve repair is the tension-free coaptation of healthy, well-vascularized fascicles.
- Preparation: Use loupe magnification (3.5x to 4.5x) or an operating microscope. Ensure a bloodless field using a pneumatic tourniquet.
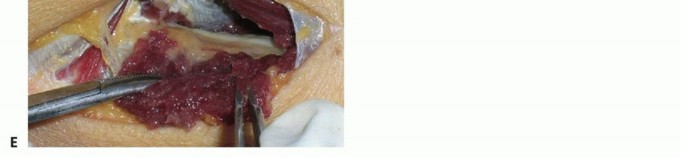
- Debridement: Resect the nerve ends until healthy fascicles pout from the epineurium. The "mushrooming" of fascicles indicates healthy axoplasm.
- Alignment: Utilize surface landmarks, such as the longitudinal epineurial blood vessels (vasa nervorum) and the cross-sectional fascicular topography, to prevent rotational malalignment.
- Coaptation: Perform an epineurial or group fascicular repair using 8-0 or 9-0 non-absorbable monofilament suture (e.g., Nylon). Place sutures strictly in the epineurium to avoid strangulating the fascicles.
- Tension: The repair must be absolutely tension-free. If an 8-0 suture cannot hold the nerve ends together without breaking, a nerve graft is mandatory.
Nerve Grafts
Indications
Nerve grafting is indicated when a tension-free primary repair is impossible, typically in gaps exceeding 1-2 cm depending on the joint position. Mobilization of the nerve and joint flexion can overcome small gaps, but excessive tension leads to ischemia and catastrophic failure of regeneration.
Sources of Nerve Grafts
The sural nerve is the gold standard autograft, providing up to 30-40 cm of graft material with minimal donor site morbidity (loss of sensation over the lateral foot). Other sources include the medial antebrachial cutaneous nerve and the terminal branch of the posterior interosseous nerve.
Alternative Nerve Graft Materials
For non-critical sensory nerves (e.g., digital nerves) with gaps less than 3 cm, biological or synthetic nerve conduits (e.g., polyglycolic acid tubes, processed nerve allografts) can be utilized. These conduits guide axonal sprouting and prevent the ingrowth of scar tissue.
Management of Specific Nerve Injuries
Digital Nerves
Digital nerve lacerations are the most common peripheral nerve injuries in the hand.
* Approach: Extend the traumatic laceration using Bruner (zigzag) or mid-lateral incisions.
* Technique: Identify the nerve proximal and distal to the injury. The digital artery usually lies dorsal to the nerve. Under microscopic magnification, perform an epineurial repair using 9-0 or 10-0 nylon.
* Postoperative: Splint the digit in slight flexion for 3 weeks to protect the repair, followed by progressive sensory re-education.
Median Nerve at the Wrist
Injuries here are often associated with suicide attempts or glass lacerations ("spaghetti wrist").
* Approach: Extend the incision through the carpal tunnel to fully expose the median nerve and its recurrent motor branch.
* Technique: The median nerve has a distinct topography at the wrist. The motor fascicles to the thenar intrinsic muscles are typically located in the radial-volar quadrant of the nerve. Group fascicular repair is highly recommended here to ensure motor axons are directed to the thenar muscles, preventing debilitating loss of opposition.
Median Nerve in the Palm
Lacerations in the palm may injure the common digital nerves or the isolated recurrent motor branch. The motor branch is highly variable (extraligamentous, subligamentous, or transligamentous). Precise identification and repair using 9-0 nylon are critical to salvage thumb opposition.
Ulnar Nerve at the Wrist
The ulnar nerve passes through Guyon's canal, dividing into a superficial sensory branch and a deep motor branch.
* Approach: Open Guyon's canal by releasing the volar carpal ligament.
* Technique: Differentiate the fascicles. The deep motor branch lies ulnar and dorsal, while the sensory branch is radial and volar. Misalignment here is disastrous, as motor axons growing into sensory pathways will yield no functional recovery.
Deep Branch of the Ulnar Nerve
Injuries to the deep motor branch in the palm result in profound intrinsic weakness (claw hand, weak pinch). The nerve hooks around the hook of the hamate and dives deep to the flexor tendons. Repair requires extensive exposure, often necessitating the release of the origin of the hypothenar muscles and retraction of the flexor tendons.
Dorsal Branch of the Ulnar Nerve
This branch arises 5-8 cm proximal to the wrist and provides sensation to the dorsal-ulnar hand. Lacerations are common in distal forearm trauma. Repair is indicated to prevent painful neuroma formation, which is highly problematic in this location due to friction from clothing and resting the hand on surfaces.
Superficial Radial Nerve
The superficial radial nerve is exquisitely sensitive and highly prone to developing painful, intractable neuromas following injury (Wartenberg's syndrome).
* Technique: Primary repair should be attempted. If grafting is required, ensure the coaptation sites are buried deep to healthy muscle or subcutaneous fat to minimize mechanical irritation.
Traumatic Neuromas
When a nerve is transected and fails to regenerate into its distal stump, the sprouting axons form a disorganized, painful mass of nerve tissue and scar known as a neuroma.
* Management: Symptomatic neuromas require surgical excision. The nerve must be resected proximally to healthy fascicles. If reconstruction is not feasible, the proximal stump should be buried into deep muscle bellies (e.g., pronator quadratus) or drilled into bone to prevent mechanical stimulation and tethering.
Neurovascular Island Grafts
In cases of irreparable nerve damage with critical sensory loss (e.g., the ulnar aspect of the thumb or radial aspect of the index finger), a neurovascular island flap can be utilized. This involves transferring a sensate patch of skin, along with its intact neurovascular pedicle, from a less critical area (e.g., the ulnar aspect of the ring finger) to the critical contact area, restoring protective and functional sensibility.
Postoperative Assessment and Rehabilitation
Postoperative management is as critical as the microsurgical repair itself.
1. Immobilization: The limb is splinted for 3 weeks in a position that minimizes tension on the repair (e.g., wrist flexion for volar nerve repairs).
2. Sensory Re-education: Once protective sensation begins to return (assessed via advancing Tinel's sign and tuning forks), cortical re-mapping exercises are initiated.
3. Motor Tracking: Electromyography (EMG) can be utilized at 3 to 4 months post-repair to detect subclinical reinnervation before visible muscle contraction occurs.
Consistent, long-term follow-up is required, as nerve regeneration proceeds at approximately 1 mm per day. Full functional recovery may take up to 18-24 months, demanding patience and rigorous adherence to hand therapy protocols.
📚 Medical References
- Peripheral nerve injuries: diagnosis and treatment, N Engl J Med 278:1431, 1968.
- Foerster O: Handbuch der Neurologie, part 2, Berlin, 1929, Julius Springer. Gilliatt RW: Physical injury to peripheral nerve: physiologic and electrodiagnostic aspects, Mayo Clin Proc 56:361, 1981.
- Grabb WC: Management of nerve injuries in the forearm and hand, Orthop Clin North Am 1:419, 1970.
You Might Also Like