Flexor Tendon Repair: Anatomy, Biomechanics, Surgical Techniques, and Rehabilitation
Key Takeaway
Flexor tendon repair demands meticulous surgical technique and a profound understanding of intrasynovial biology. Successful outcomes in Zone II—historically termed "no man's land"—rely on preserving the pulley system, utilizing robust multi-strand core sutures to prevent gap formation, and implementing early active mobilization protocols. This guide provides an evidence-based framework for navigating flexor tendon anatomy, biomechanics, surgical repair strategies, and postoperative rehabilitation to optimize digital excursion and minimize adhesions.
Introduction to Flexor Tendon Surgery
The management of flexor tendon injuries remains one of the most formidable challenges in orthopedic and hand surgery. Historically, repairs within Zone II—famously designated "no man's land" by Bunnell—yielded poor outcomes due to dense adhesion formation between the flexor digitorum superficialis (FDS), flexor digitorum profundus (FDP), and the surrounding fibro-osseous sheath.
Over the past several decades, a paradigm shift driven by rigorous biomechanical research and an enhanced understanding of tendon biology has revolutionized our approach. The transition from prolonged immobilization to early active mobilization (EAM), supported by the development of robust multi-strand core suture techniques, has dramatically improved functional outcomes. This comprehensive guide synthesizes the foundational anatomy, biomechanics, healing biology, and advanced surgical techniques required to execute flawless flexor tendon repairs.
Surgical Anatomy and Biomechanics
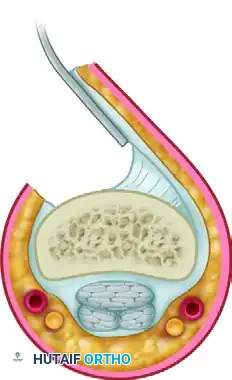
A profound comprehension of the flexor tendon sheath and its associated pulley system is non-negotiable for the operating surgeon. The digital flexor sheath is a closed synovial system that provides nutrition and mechanical stability to the gliding tendons.
The Pulley System
The retinacular pulley system, meticulously detailed by Doyle and Blythe, consists of focal thickenings of the flexor sheath that maintain the tendons in close apposition to the phalanges, thereby optimizing the biomechanical work of flexion and preventing bowstringing.
- Annular Pulleys (A1-A5):
- A1, A3, A5: Arise from the volar plates of the metacarpophalangeal (MCP), proximal interphalangeal (PIP), and distal interphalangeal (DIP) joints, respectively.
- A2 and A4: Arise directly from the periosteum of the proximal and middle phalanges. These are the critical biomechanical pulleys. The A2 and A4 pulleys must be preserved or reconstructed to prevent bowstringing, which drastically reduces tendon excursion efficiency and leads to flexion contractures.
- Cruciate Pulleys (C1-C3): Thin, crisscrossing bands located between the annular pulleys that allow the sheath to collapse and expand during digital flexion without impingement.
Vascularity and Nutrition
Flexor tendons within the digital sheath possess a dual nutrient supply:
1. Vascular Perfusion: Blood is supplied segmentally via the vincula (vincula brevia and longa), which enter the dorsal aspect of the tendons.
2. Synovial Diffusion: The primary source of nutrition for the intrasynovial segments (Zone II). Synovial fluid is pumped into the tendon interstices during the cyclical loading and unloading of digital flexion and extension.
Clinical Pearl: Because the volar aspect of the flexor tendon is relatively avascular and relies heavily on synovial diffusion, core sutures should be placed in the volar half of the tendon to avoid strangulating the dorsal intrinsic blood supply.
Biomechanics of Excursion
Tendon excursion is the distance a tendon must glide to produce full joint motion. In the fingers, the FDP requires approximately 3-4 cm of excursion to achieve full composite flexion. The "work of flexion" refers to the resistance the tendon encounters as it glides through the sheath. Edema, bulky suture knots, and disrupted pulleys exponentially increase the work of flexion, predisposing the repair to gap formation or rupture during early rehabilitation.
Biology of Tendon Healing
The historical debate between "extrinsic" and "intrinsic" tendon healing has been settled by the seminal work of Gelberman, Manske, and others.
Intrinsic vs. Extrinsic Healing
- Extrinsic Healing: Relies on the ingrowth of fibroblasts and inflammatory cells from the surrounding sheath. While it provides rapid strength, it inevitably results in restrictive peritendinous adhesions.
- Intrinsic Healing: Occurs via the proliferation of epitenon and endotenon tenocytes. This process is stimulated by mechanical loading (controlled mobilization) and synovial diffusion, allowing the tendon to heal without forming adhesions to the surrounding sheath.
The Role of Mechanical Stress
Controlled mechanical stress upregulates the expression of critical growth factors, including Vascular Endothelial Growth Factor (VEGF) and Transforming Growth Factor-beta (TGF-β). Early intermittent mobilization enhances collagen synthesis, accelerates the maturation of the repair site, and improves the ultimate tensile strength of the tendon while simultaneously preventing the formation of restrictive adhesions.
Indications and Preoperative Planning
Patient Selection
Primary repair is indicated for acute lacerations of the FDS and/or FDP tendons. The ideal window for primary repair is within 7 to 10 days of injury. Delayed primary repair (10-21 days) is feasible but technically demanding due to tendon retraction and myostatic contracture. Beyond 3-4 weeks, secondary reconstruction (e.g., tendon grafting or staged Hunter rod reconstruction) is often required.
Preoperative Assessment
- Zone I: Distal to the FDS insertion. Involves only the FDP.
- Zone II: From the A1 pulley to the FDS insertion. Involves both FDS and FDP within the tight fibro-osseous sheath.
- Zone III: Lumbrical origin (palm).
- Zone IV: Carpal tunnel.
- Zone V: Forearm, proximal to the carpal tunnel.
Surgical Warning: Concomitant digital nerve injuries are present in up to 80% of Zone II flexor tendon lacerations. A meticulous neurovascular examination must be documented prior to the administration of local anesthetic.
Surgical Approach and Technique
The goal of flexor tendon repair is to create a coaptation that is strong enough to withstand the forces of early active mobilization while remaining smooth and low-profile to glide effortlessly through the pulley system.
1. Positioning and Preparation
- The patient is positioned supine with the arm on a radiolucent hand table.
- Regional anesthesia (axillary or supraclavicular block) or general anesthesia is utilized. Wide-awake local anesthesia no tourniquet (WALANT) is increasingly popular, allowing intraoperative assessment of active tendon gliding and gap formation.
- An upper arm tourniquet is applied and inflated to 250 mm Hg after exsanguination.
2. Incisions and Exposure
- Extend the traumatic wound using Bruner zigzag incisions or mid-axial incisions. Never cross a flexion crease at a perpendicular angle to avoid scar contracture.
- Elevate full-thickness fasciocutaneous flaps, preserving the neurovascular bundles.
- Identify the flexor tendon sheath. In Zone II injuries, the sheath is often filled with hematoma.
3. Tendon Retrieval
- The proximal tendon stumps rapidly retract into the palm due to muscle tone.
- Retrieve the tendons by milking the forearm and palm distally.
- If the tendon is elusive, a flexible pediatric feeding catheter can be passed proximally through the sheath, sutured to the tendon stump, and used to pull the tendon distally.
- Once retrieved, secure the proximal stumps temporarily with a transverse 25-gauge hypodermic needle passed through the tendon and the A1 or A2 pulley. This relieves tension and allows for meticulous repair.
4. Core Suture Placement
The core suture provides the primary tensile strength of the repair. Biomechanical studies demonstrate that the strength of a repair is directly proportional to the number of suture strands crossing the repair site. A minimum of a 4-strand repair is required to safely permit early active mobilization.
- Material: 3-0 or 4-0 braided non-absorbable suture (e.g., Supramid, Ticron, or FiberWire).
- Techniques:
- Modified Kessler (2-strand): Historically popular but insufficient for modern EAM protocols.
- Cruciate (4-strand): Two grasping sutures placed in a cross-hatch pattern.
- Strickland/Indiana (4-strand): A combination of a core locking suture and a continuous epitendinous suture.
- Lim-Tsai (6-strand): Provides superior strength but increases the bulk of the repair.
- Placement: Sutures should be placed in the volar one-third of the tendon to preserve dorsal vascularity. The purchase length should be approximately 0.7 to 1.0 cm from the cut edge to prevent pull-out.
- Locking vs. Grasping: Locking loops (where the suture passes around itself) significantly reduce gap formation under cyclical loading compared to simple grasping loops.
5. Epitendinous Repair
The epitendinous suture is not merely cosmetic; it is a critical biomechanical component.
* Material: 5-0 or 6-0 monofilament (e.g., Prolene or Nylon).
* Technique: A running, continuous, or cross-stitch (Silfverskiöld) pattern circumferentially around the repair site.
* Function: It increases the ultimate tensile strength of the construct by 10% to 50%, reduces gap formation, and tucks in the frayed epitenon edges, dramatically decreasing the gliding resistance (work of flexion) through the pulleys.
6. Pulley Management
Historically, surgeons strictly avoided venting the pulleys. However, modern evidence suggests that if the repair is bulky and impinges on the A2 or A4 pulley, it is safer to carefully vent a small portion of the pulley (up to 25% of A2 or A4) rather than accept high gliding resistance, which inevitably leads to tendon rupture. If extensive venting is required, pulley reconstruction using a slip of the extensor retinaculum may be necessary.
7. Closure and Splinting
- Deflate the tourniquet and achieve meticulous hemostasis to prevent postoperative hematoma, which acts as a scaffold for adhesions.
- Close the skin with non-absorbable sutures.
- Apply a dorsal blocking splint in the operating room. The wrist is positioned in 20-30 degrees of flexion, MCP joints in 70 degrees of flexion, and IP joints in full extension.
Postoperative Rehabilitation Protocols
The success of a flexor tendon repair is equally dependent on the surgical execution and the postoperative rehabilitation protocol. The goal is to apply enough stress to stimulate intrinsic healing and tendon excursion while avoiding forces that exceed the tensile strength of the repair.
1. Controlled Passive Motion (Duran Protocol)
- Initiated within 3-5 days postoperatively.
- Involves passive flexion and extension of the PIP and DIP joints within the constraints of the dorsal blocking splint.
- Provides 3-5 mm of tendon excursion, which is the minimum required to prevent dense adhesion formation.
2. Dynamic Traction (Kleinert Protocol)
- Utilizes elastic bands attached to the fingernails, pulling the digits into passive flexion.
- The patient actively extends the digits against the resistance of the rubber bands.
- While historically popular, it has largely been superseded due to issues with PIP joint flexion contractures.
3. Early Active Mobilization (EAM)
EAM is the current gold standard, provided the surgeon has achieved a robust 4-strand or 6-strand repair.
* Place and Hold: The therapist passively flexes the digits, and the patient gently contracts their muscles to "hold" the position.
* True Active Motion: Gentle, unresisted active flexion is initiated within the first week.
* Biomechanical Rationale: Active muscle contraction reduces the work of flexion by pulling the tendon proximally, whereas passive pushing of the tendon distally can cause buckling and bunching at the repair site.
Clinical Pearl: The weakest phase of tendon healing occurs between days 10 and 21, as the inflammatory phase transitions to the fibroblastic phase and the tendon softens. Rehabilitation must be carefully monitored during this window to prevent rupture.
Complications and Management
1. Tendon Rupture
Rupture typically occurs due to patient non-compliance, an inadequate core suture, or excessive work of flexion from a bulky repair. It usually presents with a sudden loss of active flexion.
* Management: Prompt surgical re-exploration. If identified within 7-14 days, primary re-repair is often possible. Late presentations require staged tendon grafting.
2. Adhesion Formation
The most common complication, presenting as a discrepancy between passive and active range of motion.
* Prevention: Meticulous tissue handling, robust epitendinous suturing, and strict adherence to EAM protocols. Biologic adjuncts (e.g., hyaluronic acid, 5-fluorouracil) have shown promise in animal models but lack widespread clinical standardization.
* Management: Intensive hand therapy for 3-6 months. If functional deficits persist and the soft tissue envelope is supple, a surgical tenolysis may be indicated. Tenolysis should never be performed before 6 months post-injury to allow the scar tissue to fully mature.
3. Joint Contractures
PIP joint flexion contractures are notoriously difficult to treat. They arise from a combination of tendon adhesions, volar plate contracture, and collateral ligament shortening. Prevention via night extension splinting and targeted therapy is paramount.
Conclusion
Mastery of flexor tendon repair requires a synthesis of anatomical precision, biomechanical understanding, and biological respect. By adhering to the principles of multi-strand core suturing, meticulous epitendinous repair, preservation of the critical pulley system, and the implementation of early active mobilization, the orthopedic surgeon can consistently navigate the treacherous waters of "no man's land" and restore optimal hand function to the patient.
You Might Also Like