Mastering Excision of Hand & Wrist Ganglion Cysts & Related Soft Tissue Tumors
Key Takeaway
Step into the operating room for a comprehensive masterclass on excising hand and wrist soft tissue tumors. This guide covers the meticulous surgical techniques for ganglion cysts, giant cell tumors of the tendon sheath, and epidermal inclusion cysts. Fellows will learn critical anatomy, precise instrument use, and strategies for managing potential complications, ensuring a thorough understanding of these common procedures from a seasoned surgeon's perspective.
Introduction and Epidemiology
Ganglion cysts and related benign soft tissue tumors represent the vast majority of masses encountered in the hand and upper extremity. Although rarely limb-threatening, these lesions frequently cause significant functional impairment, pain, and mechanical symptoms that warrant definitive surgical intervention. A rigorous understanding of their pathophysiology and anatomical origins is essential for the orthopedic surgeon to minimize recurrence and optimize patient outcomes.
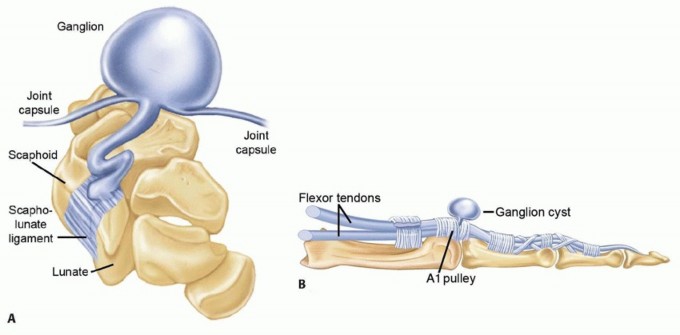
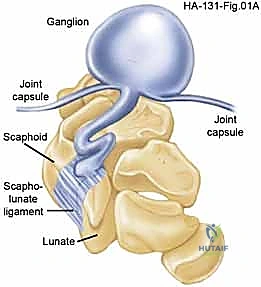
Ganglion cysts, while clinically referred to as cysts, lack a true epithelial lining and are therefore strictly classified as pseudocysts. They are the most common tumors of the hand and wrist, accounting for 50% to 70% of all soft tissue masses in this anatomical region. These fluid-filled structures typically arise from an adjacent joint capsule, ligamentous interval, or tendon sheath via a one-way valve mechanism. Dorsal wrist ganglion cysts are the most prevalent, representing 60% to 70% of all ganglion cysts, whereas volar wrist ganglion cysts account for approximately 18% to 20%. Other notable variants include volar retinacular cysts arising from the A1 or A2 pulleys of the flexor tendon sheath, and degenerative mucous cysts, which are invariably associated with underlying osteoarthritis of the distal interphalangeal (DIP) joint and marginal osteophyte formation.
Giant cell tumors of the tendon sheath (GCTTS) represent the second most common soft tissue tumor in the hand. Historically referred to by various nomenclatures—including localized nodular tenosynovitis, fibrous xanthoma, and localized pigmented villonodular synovitis (PVNS)—these are benign, slow-growing, but locally aggressive soft tissue tumors. They exhibit a strong predilection for the volar aspect of the digits and can cause significant mechanical impingement, neurovascular displacement, or secondary osseous erosion due to pressure effects.
Epidermal inclusion cysts are the third most common type of hand tumor. Unlike ganglions, these are true cysts lined by stratified squamous epithelium. They are typically the direct result of penetrating trauma that drives epidermal cells into the deep subcutaneous tissues or intraosseous spaces. They are slow-growing, benign, and frequently present months to years after the initial traumatic event, most commonly at the volar fingertip or distal phalanx.
Surgical Anatomy and Biomechanics
A profound understanding of carpal and digital anatomy is paramount for the safe and definitive excision of these lesions. The historical high recurrence rates of ganglion cysts were intimately tied to the failure to resect the generative stalk or capsular origin, underscoring the need for precise anatomical dissection.
Dorsal Wrist Ganglion Cysts
Dorsal ganglion cysts predominantly originate from the scapholunate (SL) articulation. The cyst sac communicates through a tortuous stalk or one-way valve mechanism to the underlying joint. The primary site of origin is the dorsal capsulo-scapholunate septum (DCSS), a specialized capsular thickening overlying the dorsal scapholunate interosseous ligament (SLIL). The cyst typically emerges through the dorsal capsule between the extensor pollicis longus (EPL, third extensor compartment) and the extensor digitorum communis (EDC, fourth extensor compartment). Histologically, the cyst contains a highly viscous, clear mucinous fluid composed of glucosamine, albumin, globulin, and a high concentration of hyaluronic acid, which is produced by mesenchymal cells at the cyst-capsule interface.
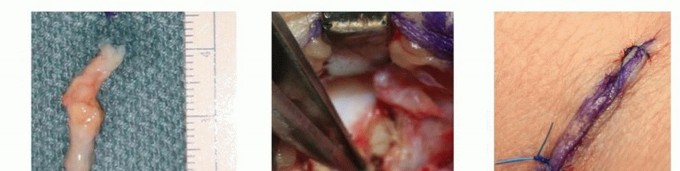
Volar Wrist Ganglion Cysts
Volar ganglion cysts typically arise from the radiocarpal joint, specifically originating from the radioscaphocapitate (RSC) ligament or the long radiolunate (LRL) ligament. They most frequently present in the interval between the flexor carpi radialis (FCR) tendon and the radial artery. The intimate relationship between the cyst wall and the radial artery is of critical surgical importance; the artery and its venae comitantes are frequently draped over the cyst, splayed, or densely adherent to its pseudocapsule. Furthermore, a thorough understanding of the palmar cutaneous branch of the median nerve (PCBMN) is required. The PCBMN courses ulnar to the FCR tendon and is at high risk for iatrogenic injury or traction neuritis during standard volar approaches.
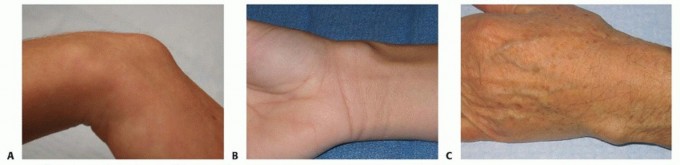
Giant Cell Tumors of the Tendon Sheath
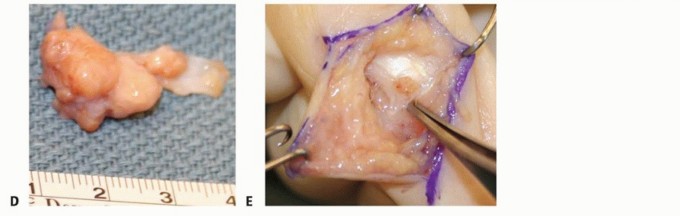
Giant cell tumors typically manifest as multilobular, well-circumscribed masses ranging from 0.5 to 7 cm in diameter. Their gross appearance varies from yellow to deep brown, reflecting the variable concentrations of hemosiderin, lipid-laden histiocytes, and dense collagenous stroma. The tumor is contained within a thin pseudocapsule. Although benign, aggressive variants can envelop digital neurovascular bundles, deeply invade adjacent flexor tendon sheaths, and erode into cortical bone. Cartilage and medullary canal involvement are notably absent, distinguishing it from malignant osseous pathologies. Histological examination reveals polyhedral-shaped mononuclear histiocytes, scattered multinucleated osteoclast-like giant cells, and prominent hemosiderin deposits.
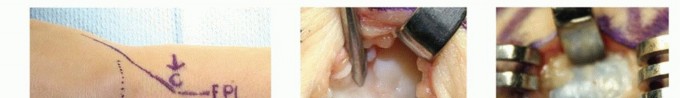
Epidermal Inclusion Cysts
Epidermal inclusion cysts are superficial, firm, and slightly mobile lesions that are often densely adherent to the overlying skin scar. They contain a thick, white, caseous keratinous material. In the distal phalanx, the expanding cyst can cause pressure necrosis of the underlying bone, resulting in a well-circumscribed, purely lytic lesion visible on radiographs. The epithelial lining must be entirely resected without spillage to prevent recurrence and severe local inflammatory reactions.
Indications and Contraindications
The decision to proceed with surgical excision, whether open or arthroscopic, depends on symptomatology, the failure of conservative measures, and the specific pathology identified during clinical and radiographic evaluation.
Surgical Indications
Surgical intervention is strictly indicated for patients experiencing persistent pain, restricted range of motion, mechanical weakness, or neurovascular compromise (such as compression of the ulnar nerve in Guyon's canal by a proximal volar cyst, or digital nerve compression by a GCTTS). Cosmetic deformity that causes significant psychological distress or functional impingement during daily activities also warrants excision. Aspiration is often utilized as a first-line diagnostic and therapeutic modality for ganglion cysts; however, literature demonstrates that recurrence rates following aspiration alone approach 50% to 80%. Operative management is definitively indicated upon recurrence following aspiration.
Contraindications
Absolute contraindications include active local infection (cellulitis or septic arthritis) or profound medical comorbidities precluding regional or general anesthesia. Relative contraindications for arthroscopic excision include extensive prior open wrist surgery (which distorts portal anatomy and capsular landmarks), extremely large cysts that grossly distort the radiocarpal anatomy preventing safe portal placement, and volar ganglion cysts in the hands of surgeons without advanced wrist arthroscopy experience due to the extreme proximity of the radial artery.
| Management Strategy | Primary Indications | Contraindications |
|---|---|---|
| Observation | Asymptomatic incidental findings, painless cosmetic bumps | Neurovascular compromise, rapid growth, bone erosion |
| Aspiration / Injection | First-line treatment for symptomatic dorsal/volar ganglions | Suspected vascular lesion (aneurysm), solid tumor (GCTTS) |
| Open Excision | Recurrent ganglions, GCTTS, Epidermal inclusion cysts, neurovascular involvement | Active overlying cellulitis, medically unstable patient |
| Arthroscopic Excision | Dorsal wrist ganglions, select volar ganglions, concurrent intra-articular pathology | Distorted capsular anatomy, lack of advanced arthroscopic expertise |
Pre Operative Planning and Patient Positioning
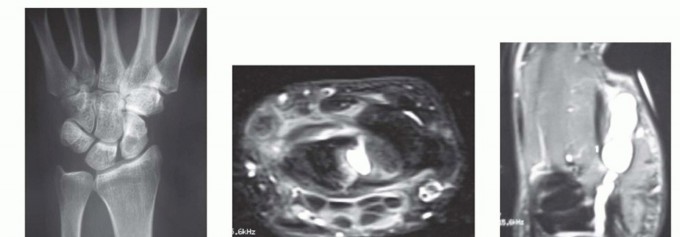
Thorough preoperative evaluation is mandatory to differentiate benign cysts from malignant sarcomas or vascular anomalies. Standard posteroanterior, lateral, and oblique radiographs of the wrist or digit should be obtained routinely to rule out concurrent osseous pathology, such as a carpal boss, degenerative joint disease (scapholunate advanced collapse), or the lytic lesions characteristic of advanced epidermal inclusion cysts.
Magnetic Resonance Imaging (MRI) with and without contrast, or high-resolution ultrasonography, is highly recommended for occult ganglion cysts presenting with unexplained dorsal wrist pain. MRI is also invaluable to delineate the extent of a giant cell tumor, identify satellite lesions, and map its relationship to the digital neurovascular bundles prior to surgical exploration. For volar ganglion cysts, a clinical Allen test must be documented preoperatively to confirm adequate collateral perfusion to the hand via the ulnar artery, given the inherent risk of iatrogenic injury to the radial artery during dissection.
Patient Positioning
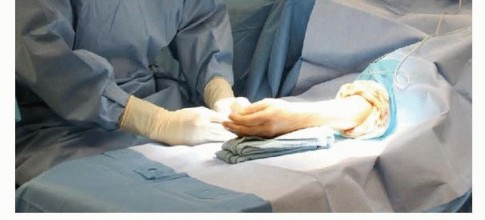
The patient is positioned supine with the operative extremity extended on a radiolucent hand table. A well-padded pneumatic tourniquet is applied to the proximal arm to ensure a bloodless surgical field, which is critical for identifying fine neurovascular structures.
For open procedures, the hand is prepped and draped in standard sterile fashion. Lead hand retractors or assistant-held self-retaining retractors are utilized to maintain exposure.
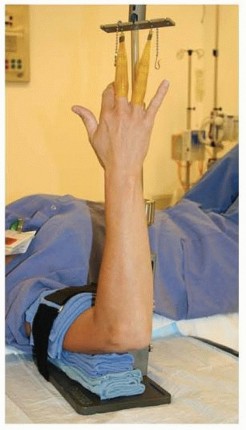
For arthroscopic procedures, the wrist is suspended using a dedicated traction tower. Finger traps are applied to the index and long fingers, and 10 to 15 pounds of traction is applied to distract the radiocarpal and midcarpal joints. The wrist is typically placed in neutral to slight flexion for dorsal portal establishment. A 2.7 mm or 1.9 mm arthroscope (30-degree angle) is utilized, along with a dedicated small joint shaver and radiofrequency ablation wand.
Detailed Surgical Approach and Technique
The surgical technique varies significantly based on the specific pathology and the chosen modality (open versus arthroscopic). The unifying surgical principle for all excisions is the complete, en bloc removal of the lesion and its generative origin to minimize recurrence.
Open Excision of Dorsal Ganglion Cysts
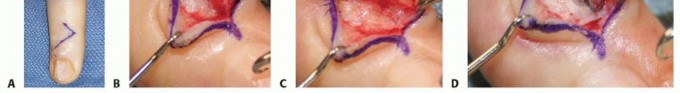
A transverse incision is typically made directly over the apex of the cyst, following Langer's lines to optimize the cosmetic outcome and minimize scar contracture. Longitudinal incisions may be used for extensile exposure but carry a higher risk of hypertrophic scarring across the wrist crease. Subcutaneous dissection is performed meticulously using blunt spreading techniques to identify and protect the terminal branches of the superficial radial nerve (SRN) and the dorsal sensory branch of the ulnar nerve (DSBUN).

The extensor retinaculum is exposed, and the cyst is identified protruding between the third and fourth extensor compartments. The extensor retinaculum may be incised longitudinally. The EPL is retracted radially, and the EDC is retracted ulnarly. The cyst is mobilized circumferentially down to its stalk at the scapholunate interval.
Crucially, the cyst must not be simply amputated at the superficial capsule. A 1 cm by 1 cm window of the dorsal capsule, including the dorsal capsulo-scapholunate septum, must be excised en bloc with the cyst stalk. Extreme care must be taken to avoid violating the underlying dorsal scapholunate interosseous ligament (SLIL), as iatrogenic transection can precipitate acute scapholunate dissociation and carpal instability. The capsular defect is deliberately left open to heal by secondary intention.
Arthroscopic Excision of Dorsal Ganglion Cysts
Arthroscopic excision offers the distinct advantage of evaluating concurrent intra-articular pathology (e.g., TFCC tears, chondral defects) and potentially reducing postoperative stiffness by preserving the superficial extensor retinaculum. Standard radiocarpal portals (3-4 and 4-5) and midcarpal portals (radial midcarpal and ulnar midcarpal) are established.
The arthroscope is initially introduced into the 3-4 portal to inspect the radiocarpal joint. The stalk of a dorsal ganglion is typically visualized at the dorsal capsule overlying the scapholunate interval, often presenting as a focal area of synovitis or a distinct capsular rent. A shaver is introduced via the 4-5 portal or a dedicated 6R portal.
The dorsal capsule is systematically resected at the site of the stalk. The surgeon creates a capsular window approximately 1 cm in diameter. When the cyst wall is breached, the characteristic thick, gelatinous mucin will extrude into the joint space and is evacuated by the shaver. The midcarpal joint is then meticulously evaluated to ensure complete resection of the stalk from the midcarpal aspect of the scapholunate ligament, ensuring no residual valve mechanism remains.
Open Excision of Volar Ganglion Cysts
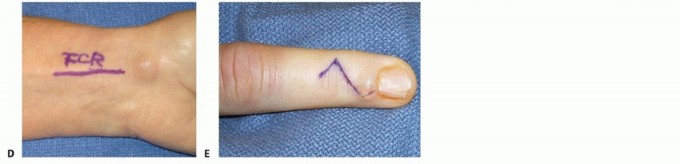
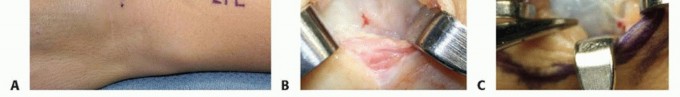
Volar ganglion cysts require exacting dissection due to their proximity to the radial artery. A longitudinal or zig-zag incision is made over the volar radial aspect of the wrist. The palmar cutaneous branch of the median nerve (PCBMN) is identified and protected; it typically lies in the subcutaneous tissue ulnar to the FCR.
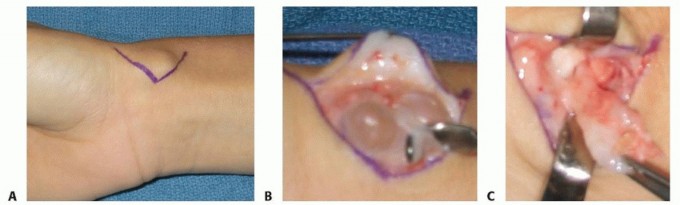
The flexor carpi radialis (FCR) tendon sheath is opened, and the tendon is retracted ulnarly. The radial artery is identified; it is often splayed over the superficial surface of the cyst. Using loupe magnification, the artery and its delicate venae comitantes are carefully dissected off the pseudocapsule of the cyst in a subadventitial plane. Vessel loops can be utilized to gently retract and protect the neurovascular bundle.
The cyst is traced proximally and deeply to its origin at the radiocarpal joint, typically at the interval between the radioscaphocapitate (RSC) or long radiolunate (LRL) ligaments. Similar to the dorsal approach, a small window of the volar capsule is excised along with the cyst stalk to minimize recurrence, taking care not to destabilize the volar extrinsic carpal ligaments.
Arthroscopic Excision of Volar Ganglion Cysts
Arthroscopic management of volar cysts is technically demanding and carries a higher risk profile. The viewing portal is typically the standard 3-4 portal, with the working portal established at the 1-2 interval or a dedicated volar radial portal. The volar capsule is visualized, and the stalk is identified between the RSC and LRL ligaments.
Extreme caution is required when using the shaver or radiofrequency wand on the volar capsule to avoid penetrating the capsule completely and injuring the adjacent radial artery or flexor tendons. The capsular window is created from inside-out, allowing the cyst contents to decompress into the joint.
Excision of Giant Cell Tumors of the Tendon Sheath
Excision of a giant cell tumor necessitates a meticulous, extensive approach due to the lesion's propensity for local invasion, satellite nodule formation, and high recurrence rate (up to 45% if incompletely excised).
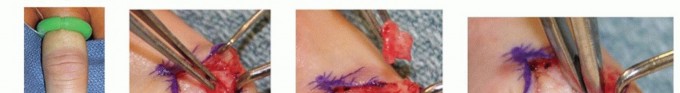
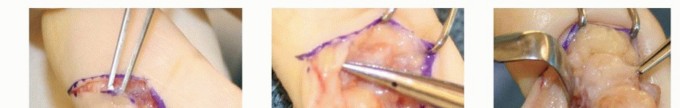
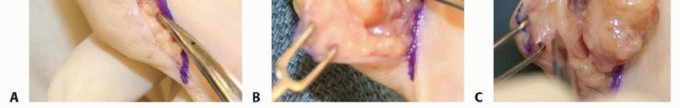
Bruner zig-zag incisions or mid-axial incisions are utilized over the affected digit to provide extensile exposure without causing flexion contractures. The digital neurovascular bundles must be identified proximally in normal tissue and traced distally into the tumor bed, as the tumor frequently displaces, encases, or envelops these critical structures.
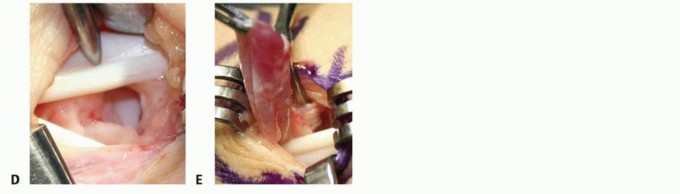
The pseudocapsule of the tumor is delineated. The mass is excised en bloc if possible. However, due to its multilobular nature, satellite lesions are exceedingly common. The flexor tendon sheath must often be opened, and a localized, aggressive synovectomy performed. If the tumor has eroded into the underlying cortical bone, aggressive curettage of the osseous defect is required. The use of a high-speed burr can aid in clearing reactive margins. Copious irrigation is performed prior to closure to remove microscopic tumor cells.
Excision of Epidermal Inclusion Cysts
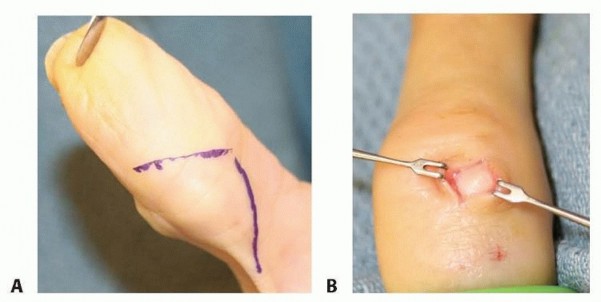
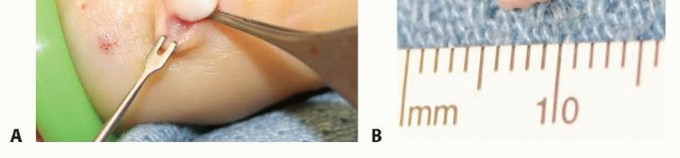
Epidermal inclusion cysts are approached via a direct incision over the mass, often incorporating the previous traumatic scar. The cyst is typically densely adherent to the dermis, and a small elliptical excision of the overlying skin may be necessary to remove the tethered portion without rupturing the cyst wall.
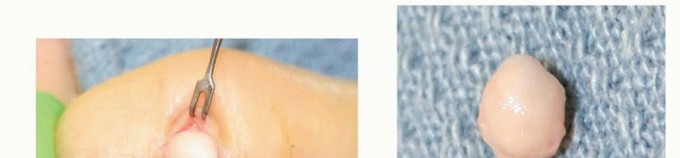
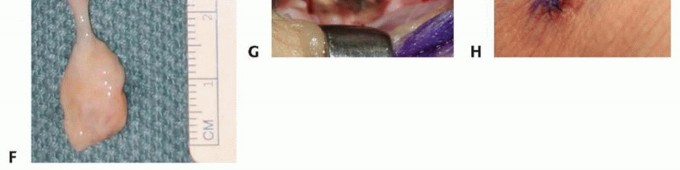
Dissection proceeds carefully within the subcutaneous tissue. The primary surgical goal is marginal excision without violating the cyst wall, as spillage of the highly immunogenic keratinous contents can incite a severe foreign-body inflammatory response and dramatically increase the risk of recurrence. If the cyst involves the distal phalanx (frequently presenting as an intraosseous lytic bone lesion), the bone must be thoroughly curetted after the soft tissue component is removed, and occasionally grafted if the defect is structurally compromising.
Complications and Management
Complications following the excision of hand and wrist tumors range from minor wound healing issues and cosmetic dissatisfaction to severe neurovascular compromise. Thorough preoperative counseling regarding these risks is essential.
Recurrence is the most common complication across all modalities. Open dorsal ganglion excision carries a recurrence rate of 5% to 10%, whereas volar ganglions have a higher recurrence rate of 15% to 20% due to the surgeon's hesitancy to aggressively resect the volar capsule near the radial artery. Arthroscopic recurrence rates are generally comparable to open techniques when performed by highly experienced surgeons. Giant cell tumors have a notoriously high recurrence rate (10% to 45%) directly correlated to the incomplete resection of microscopic satellite nodules.
Nerve injury is a significant and morbid risk. The superficial radial nerve and dorsal sensory branch of the ulnar nerve are at risk during dorsal approaches. The palmar cutaneous branch of the median nerve is frequently injured during volar ganglion excisions, leading to debilitating, painful neuromas. Digital nerves are at risk during GCTTS excision due to tumor encasement.
Vascular injury, specifically to the radial artery during volar ganglion excision, can lead to pseudoaneurysm formation, hemorrhage, or hand ischemia if collateral circulation via the superficial palmar arch is insufficient.
| Complication | Incidence | Prevention and Salvage Strategy |
|---|---|---|
| Recurrence | 5-45% ( |
Clinical & Radiographic Imaging
You Might Also Like
