Percutaneous Release of Trigger Finger: A Comprehensive Surgical Guide
Key Takeaway
Percutaneous release of the A1 pulley is a minimally invasive, highly effective surgical intervention for stenosing tenosynovitis (trigger finger). This technique utilizes an 18- or 19-gauge needle to transect the pulley, offering reduced recovery time and avoiding palmar incisions. Success relies on precise anatomical knowledge, meticulous needle orientation, and dynamic intraoperative assessment. This guide details the biomechanics, indications, step-by-step surgical approach, and postoperative protocols necessary to optimize patient outcomes and minimize neurovascular complications.
Introduction to Percutaneous Trigger Finger Release
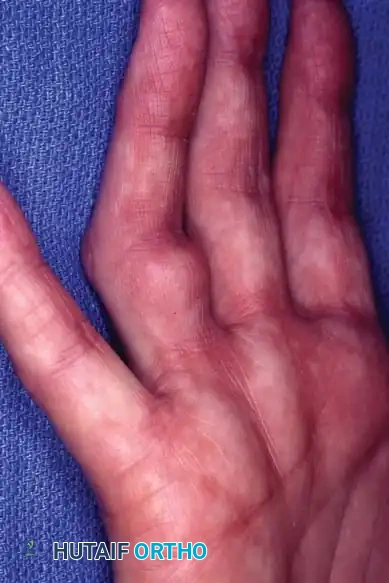
Stenosing tenosynovitis, commonly known as trigger finger, is one of the most frequent causes of hand pain and disability encountered in orthopedic practice. The condition arises from a spatial mismatch between the volume of the flexor tendon sheath and the flexor tendons themselves, most critically at the level of the first annular (A1) pulley.
While open surgical release remains the gold standard for refractory cases, the percutaneous release of the trigger finger has emerged as a highly efficacious, minimally invasive alternative. First described by Lorthioir in 1958 and later popularized by Eastwood and others, the percutaneous technique utilizes a hypodermic needle to transect the A1 pulley. When performed by an experienced hand surgeon, this technique yields success rates comparable to open surgery (often exceeding 90%), with the added benefits of absent incisional scarring, reduced postoperative pain, and an accelerated return to work and activities of daily living.
This comprehensive guide details the pathoanatomy, patient selection criteria, precise anatomical landmarks, and the step-by-step surgical execution required to master the percutaneous release of the A1 pulley.
Pathoanatomy and Biomechanics of Stenosing Tenosynovitis
A profound understanding of the flexor tendon pulley system is mandatory before attempting a blind, percutaneous intervention.
The Flexor Pulley System
The flexor tendon sheath is a complex synovial and retinacular structure designed to keep the flexor digitorum superficialis (FDS) and flexor digitorum profundus (FDP) tendons closely apposed to the phalanges, preventing bowstringing during active flexion. The retinacular portion consists of five annular (A1-A5) and three cruciform (C1-C3) pulleys.
The A1 pulley, the primary site of pathology in trigger finger, arises from the palmar plate of the metacarpophalangeal (MCP) joint and the base of the proximal phalanx. It is approximately 1 cm in length.
Pathophysiology of Triggering
Triggering is fundamentally a biomechanical impingement. Repetitive microtrauma and friction lead to fibrocartilaginous metaplasia and hypertrophy of the A1 pulley. Concurrently, the flexor tendon (usually the FDP) may develop a localized nodular swelling (Notta's nodule).
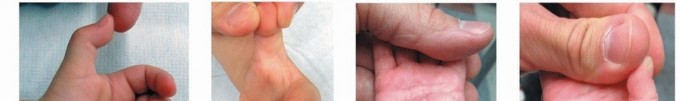
During digital flexion, the nodule is pulled proximally through the A1 pulley. Upon extension, the nodule struggles to pass back distally through the stenotic pulley, resulting in the characteristic "catching" or "locking" phenomenon. The percutaneous release aims to longitudinally divide this hypertrophied A1 pulley, thereby restoring the normal gliding volume of the tendon sheath.
Clinical Pearl: The A2 pulley, located over the proximal phalanx, is the most critical biomechanical pulley for preventing bowstringing. The percutaneous release must be strictly confined to the A1 pulley to avoid iatrogenic A2 pulley damage and subsequent loss of mechanical advantage.
Indications and Patient Selection
Proper patient selection is the cornerstone of a successful percutaneous release. The procedure is not universally applicable to all patients presenting with stenosing tenosynovitis.
Primary Indications
- Primary Idiopathic Trigger Finger: Patients with symptomatic triggering (Green's Classification Grades II, III, or IV) that has failed conservative management, including splinting, NSAIDs, and at least one corticosteroid injection.
- Patient Preference: Patients who strongly desire a minimally invasive approach and wish to avoid an open palmar incision.
- Multiple Digit Involvement: Can be performed simultaneously on multiple digits in a single outpatient setting.
Absolute and Relative Contraindications
- Absolute Contraindications:
- Active local or systemic infection.
- Previous failed percutaneous release on the same digit (requires open exploration).
- Triggering caused by rheumatoid arthritis or other inflammatory arthropathies (these patients often require tenosynovectomy and are at risk for tendon rupture).
- Pediatric trigger thumb (congenital trigger thumb requires open release due to the proximity of the digital nerves and the different pathoanatomy).
- Relative Contraindications:
- The Thumb and Index Finger: The radial digital nerve of the thumb crosses obliquely over the flexor pollicis longus (FPL) sheath at the level of the MCP crease, making it highly vulnerable to percutaneous injury. Similarly, the proximal location of the index finger A1 pulley places its radial digital nerve at risk. Many surgeons consider the thumb and index finger relative contraindications, reserving percutaneous release strictly for the middle, ring, and small fingers.
- Severe Flexion Contractures: Long-standing locked digits with secondary proximal interphalangeal (PIP) joint contractures may require open release and concurrent joint capsulotomy.
Preoperative Preparation and Informed Consent
Before attempting the percutaneous release, the surgeon must engage in a thorough informed consent discussion.
The patient must explicitly understand that because the procedure is performed without direct visualization, there is a risk of incomplete release (resulting in persistent triggering) or recurrence. The patient must be informed that if the percutaneous attempt fails to resolve the mechanical locking intraoperatively, a subsequent or immediate open release may be necessary.
Furthermore, the risks of neurovascular injury, tendon scoring, and transient post-procedural pain must be documented.
Surgical Anatomy and Safe Zones
The success and safety of the percutaneous release rely entirely on the surgeon's ability to palpate and utilize surface anatomical landmarks to estimate the location of the A1 pulley and the adjacent neurovascular bundles.
Digit-Specific Topography
- Middle, Ring, and Small Fingers: The A1 pulley lies precisely between the proximal and distal palmar creases. The midline of the digit must be strictly maintained to avoid the digital neurovascular bundles, which run volar and lateral to the flexor sheath.
- Index Finger: The A1 pulley of the index finger is located more proximally than the others. The safe zone for release is located proximal to the proximal palmar crease.
- Thumb (If attempted by experienced surgeons): The A1 pulley lies at the level of the MCP flexion crease. The needle must be kept strictly in the midline to avoid the radial digital nerve, which is perilously close (often within 2-3 mm of the midline).
Surgical Warning: The digital nerves are most vulnerable at the level of the MCP joint, where they are relatively superficial before diving dorsal to the superficial transverse metacarpal ligament. Deviation from the exact midline of the flexor tendon sheath is the primary cause of iatrogenic nerve transection.
Step-by-Step Surgical Technique
The procedure is typically performed in an outpatient clinic setting or a minor procedure room.
1. Patient Positioning and Preparation
- Place the patient supine or seated comfortably with the affected arm extended on a hand table.
- Turn the palm facing upward (supinated).
- Place a tightly folded towel or a small surgical bump under the dorsal aspect of the hand. This permits slight hyperextension of the metacarpophalangeal (MCP) joint, which pulls the flexor tendon and the A1 pulley volarly, making them more prominent and accessible.
- Prepare the palmar skin with a standard antiseptic solution (e.g., chlorhexidine or povidone-iodine) and apply sterile drapes.
2. Local Anesthesia Infiltration
- Identify the precise midline of the affected digit at the level of the A1 pulley.
- Using a 27- or 30-gauge needle, inject 1 to 2 mL of local anesthetic (e.g., 1% lidocaine without epinephrine) into the palmar skin to create a superficial wheal.
- Advance the needle deeper, injecting just proximal to the intended release site. For the middle, ring, and small fingers, this is between the proximal and distal palmar creases. For the index finger, this is proximal to the proximal palmar crease.
- Maintain strict orientation along the longitudinal axis of the flexor tendon sheath. Avoid injecting directly into the tendon itself.
3. Needle Selection and Insertion
- Select an 18- or 19-gauge hypodermic needle for the release. The bevel of this needle will act as the surgical cutting blade.
- Palpate the flexor tendon and the nodule while the patient actively flexes and extends the digit.
- Insert the needle directly in the midline of the digit, perpendicular to the skin, until the tip contacts the flexor tendon.
- CRITICAL STEP: Orient the bevel of the needle so that it is longitudinally aligned parallel to the fibers of the flexor tendon. If the bevel is oriented transversely, it will lacerate the FDS or FDP tendon fibers, leading to fraying or rupture.
4. The Release Maneuver
- Once the needle is through the skin and resting on the tendon, ask the patient to gently flex and extend the digit. If the needle is correctly positioned within the tendon substance, the hub of the needle will swing proximally and distally with tendon excursion.
- Withdraw the needle slightly (1-2 mm) until the hub no longer moves with tendon excursion. The needle tip is now positioned precisely within the substance of the A1 pulley, superficial to the tendon.
- Using the thumb and index finger to stabilize the needle hub, move the needle longitudinally (proximally and distally) along the A1 pulley.
- Apply firm pressure against the pulley. As the bevel incises the hypertrophied fibrocartilaginous tissue, the surgeon will feel a distinct scraping, grating, or "celery-crunching" sensation.
- Continue this sweeping motion from the proximal edge to the distal edge of the A1 pulley until the grating sensation is completely eliminated, indicating a full transection of the pulley.
Pitfall: Do not use a sweeping side-to-side (windshield wiper) motion. This will not effectively cut the pulley and dramatically increases the risk of transecting the adjacent digital nerves. All needle motion must be strictly longitudinal.
5. Dynamic Intraoperative Assessment
- Once the grating sensation ceases, hold the needle steady and ask the patient to actively flex and extend the digit fully.
- Assess for any residual triggering, catching, or locking.
- If triggering persists, the release is incomplete. Re-engage the A1 pulley (often the most proximal or distal extent is missed) and perform additional longitudinal passes.
- Once full, smooth, unrestricted active motion is confirmed, withdraw the needle.
- Optional: Some surgeons choose to inject a small amount of corticosteroid (e.g., methylprednisolone) into the sheath as the needle is withdrawn to minimize postoperative inflammation, though this is not strictly required if the mechanical release is complete.
Postoperative Care and Rehabilitation
The postoperative protocol for a percutaneous release is significantly accelerated compared to an open procedure.
- Wound Care: The needle entry site is small and does not require sutures. Apply a simple adhesive bandage or a light, nonrestrictive compressive dressing.
- Mobilization: Immediate, active hand and finger use is strongly encouraged. The patient should be instructed to perform full active flexion and extension stretching exercises 5 to 10 times every hour while awake. This prevents tendon adhesions and ensures the transected edges of the A1 pulley do not heal back together.
- Pain Management: Mild oral analgesics (acetaminophen or NSAIDs) are usually sufficient for 24 to 48 hours.
- Return to Activity: Patients can typically return to light duty or normal daily activities immediately, and heavy manual labor within 48 to 72 hours, guided by pain tolerance.
- Follow-up: A brief clinical review at 1 to 2 weeks is recommended to confirm the resolution of symptoms and the absence of infection.
Complications and Avoidance Strategies
While highly effective, percutaneous release is a blind procedure that carries specific risks. Mastery of the technique requires an understanding of how to avoid these complications.
Neurovascular Injury
The most devastating complication is the transection of a digital nerve. This is almost entirely avoidable by strictly adhering to the midline of the digit and avoiding the thumb and index finger if the surgeon is not highly experienced. If a patient reports sudden, sharp, radiating electrical pain during needle insertion, the needle must be immediately withdrawn and repositioned.
Incomplete Release
Failure to completely transect the A1 pulley is the most common cause of persistent triggering. This usually occurs because the surgeon fails to extend the release far enough proximally. If triggering persists after multiple percutaneous attempts, the procedure should be aborted in favor of an open release to prevent excessive tendon trauma.
Tendon Laceration or Scoring
Longitudinal scoring of the flexor tendon is common but rarely clinically significant if the needle bevel is oriented correctly. However, transverse laceration caused by improper bevel orientation can lead to tendon fraying, triggering of the frayed tendon edges, or delayed rupture. Always ensure the bevel is parallel to the tendon fibers.
Infection
Though rare due to the percutaneous nature of the procedure, flexor tenosynovitis is a surgical emergency. Strict aseptic technique during preparation and injection is mandatory.
Conclusion
The percutaneous release of the trigger finger is an elegant, evidence-based procedure that offers a rapid, definitive solution for stenosing tenosynovitis. By combining a profound understanding of palmar topography with meticulous, controlled needle manipulation, the orthopedic surgeon can achieve excellent clinical outcomes, sparing the patient the morbidity and recovery time associated with open surgical interventions. Strict adherence to the midline, correct bevel orientation, and dynamic intraoperative assessment remain the triad of success for this indispensable technique.
You Might Also Like