Triplanar Osteotomy and Lateral Ligament Reconstruction: Comprehensive Surgical Guide
Key Takeaway
The triplanar calcaneal osteotomy, combined with lateral ligament reconstruction, is a powerful joint-sparing procedure for correcting flexible calcaneocavovarus deformities. Pioneered by Saxby and Myerson, this technique addresses multiplanar hindfoot malalignment through lateral translation, a lateral closing wedge, and superior displacement of the calcaneal tuberosity. It effectively restores hindfoot biomechanics, decreases Achilles tension, and provides a stable foundation for concurrent ligamentous reconstruction in patients with neuromuscular conditions like Charcot-Marie-Tooth disease.
INTRODUCTION TO CALCANEOCAVOVARUS DEFORMITY
Calcaneocavovarus and cavovarus deformities present a complex, multiplanar biomechanical challenge to the orthopedic surgeon. In adolescent and adult populations, this profound structural abnormality is most frequently associated with hereditary sensorimotor neuropathies, predominantly Charcot-Marie-Tooth (CMT) disease. Occasionally, the deformity may manifest secondary to severe trauma, poliomyelitis, or other acquired neuromuscular pathologies.
The hallmark of the calcaneocavovarus foot is a rigid plantarflexed first ray, hindfoot varus, and an increased calcaneal pitch. Over time, the chronic varus thrust leads to lateral ligamentous attenuation, chronic ankle instability, and eventual asymmetric joint degeneration.
For patients presenting with unstable ankle joints secondary to a calcaneocavovarus deformity—but lacking significant degenerative changes in the hindfoot or midfoot—joint-sparing osteotomies combined with ligamentous reconstruction are the gold standard. Saxby and Myerson popularized the Triplanar Calcaneal Osteotomy combined with lateral ligament reconstruction as a highly effective, joint-preserving intervention.
Clinical Pearl: If advanced degenerative changes are already present in the midtarsal or subtalar joints, joint-sparing osteotomies are contraindicated. In such cases, a triple arthrodesis combined with lateral ligament reconstruction is the recommended salvage pathway.
BIOMECHANICS AND PATHOANATOMY
Understanding the pathoanatomy of the CMT foot is critical for executing the triplanar osteotomy. In Charcot-Marie-Tooth disease, muscle imbalances dictate the deformity. The peroneus brevis and intrinsic foot muscles weaken early, while the tibialis posterior and peroneus longus remain relatively strong. The unopposed pull of the peroneus longus plantarflexes the first ray, driving the forefoot into valgus and forcing the hindfoot into a compensatory varus during weight-bearing.
Saxby and Myerson emphasized that because the peroneus brevis is typically non-functioning in these neuropathic patients, the entire tendon can be harvested and utilized to reconstruct the lateral ligamentous complex, thereby stabilizing the varus-tilting ankle joint.
The Triplanar Correction Mechanism
The triplanar osteotomy is a biomechanical masterclass that corrects all three planes of the cavovarus deformity simultaneously:
1. Lateral Translation: Shifting the posterior tuberosity fragment laterally moves the mechanical axis of the hindfoot, directly neutralizing the varus thrust and restoring a plantigrade heel strike.
2. Lateral Closing Wedge: Resecting a laterally based wedge of bone directly corrects the structural osseous varus of the calcaneal body.
3. Proximal (Superior) Sliding: Translating the tuberosity fragment superiorly decreases the abnormally high calcaneal pitch angle (calcaneocavus) and effectively reduces pathologic tension on the Achilles tendon.
PREOPERATIVE EVALUATION
Clinical Assessment
A thorough clinical examination must assess the flexibility of the hindfoot. The Coleman Block Test is mandatory to differentiate between a flexible, forefoot-driven hindfoot varus and a rigid, fixed hindfoot varus.
* If the hindfoot corrects to neutral when the plantarflexed first ray is allowed to drop off the block, the hindfoot is flexible, and a first metatarsal dorsiflexion osteotomy may suffice.
* If the hindfoot remains in varus, the deformity is fixed, necessitating a calcaneal osteotomy.
Radiographic Assessment
Standard weight-bearing radiographs (anteroposterior, lateral, and axial calcaneal views) are required.
* Lateral View: Assess Meary’s angle, calcaneal pitch, and the presence of subtalar or midtarsal arthritis.
* Axial View: Quantify the degree of hindfoot varus.
* AP View: Evaluate talonavicular coverage and the talocalcaneal angle.
SURGICAL TECHNIQUE: THE SAXBY AND MYERSON TRIPLANAR OSTEOTOMY
The following technique details the Saxby and Myerson approach for triplanar calcaneal osteotomy and concurrent lateral ligament reconstruction.
1. Patient Positioning and Anesthesia
- Administer general or regional anesthesia with a continuous popliteal block for postoperative pain management.
- Place the patient in the lateral decubitus position.
- Ensure the foot remains internally rotated but perfectly lateral to the operating surgeon. This orientation prevents spatial distortion of the hindfoot anatomy during the osteotomy.
- Apply a well-padded thigh tourniquet.
2. Incision and Exposure
- Make an oblique incision approximately 3 to 4 cm anterior to the insertion of the Achilles tendon and 1 cm inferior to the tip of the lateral malleolus.
- Extend the incision plantarward from the superior border of the calcaneus down to the plantar aspect of the foot, terminating where the normal skin meets the thicker plantar glabrous skin. The incision should align with the longitudinal axis of the fibula.
- Carry the dissection carefully through the subcutaneous tissues.
Surgical Warning: The sural nerve is highly variable in this region and may run an aberrant course. It must be meticulously identified, mobilized, and retracted superiorly to prevent painful postoperative neuromas.
- Deepen the incision directly to the periosteum of the calcaneus.
- Divide the periosteum using sharp dissection. The entire lateral wall of the calcaneus should now be visible from its superior border to its plantar edge.
- Insert small, spiked Hohmann retractors into the dorsal and inferior margins of the wound to protect the soft tissues.
- Use a periosteal elevator to strip the periosteum approximately 1 cm on either side of the planned osteotomy site to maximize exposure.
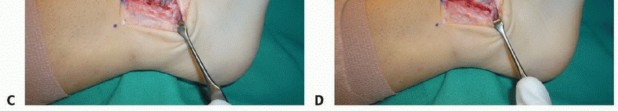
3. Executing the Osteotomy
- Using an oscillating saw, initiate the osteotomy in line with the skin incision.
- Begin the cut at the superior margin of the calcaneus and progress toward the inferior margin.
- Critical Step: Do not plunge the saw blade through the medial cortex into the medial soft tissues, as this risks injury to the tibial neurovascular bundle.
- To create the lateral closing wedge, make a second saw cut to remove a laterally based triangular wedge of bone. The wedge should be approximately 6 mm in width at its lateral base (from superior to inferior margins), tapering to an apex at the medial cortex.
- Preferably, remove this lateral wedge of bone before completely breaching the medial cortex.
- The medial cortex can be carefully perforated with a large, blunt osteotome, or the saw can be used with extreme caution, paying close attention to the exact exit point.
4. Medial Soft Tissue Release and Deformity Correction
Once the wedge is removed, use a curette or rongeur to clear all remaining cancellous bone chips from the osteotomy site. Retained fragments will act as a block, preventing proper apposition and closure of the osteotomy.
Surgical Pitfall: In severe, chronic deformities, the medial soft tissues (including the medial periosteum and retinacular structures) are extremely taut. The osteotomy will not close laterally or translate unless these structures are completely released.
- The Lamina Spreader Technique: To release the medial soft tissues from the lateral side, insert a large lamina spreader into the lateral aspect of the osteotomy.
- Apply gradual distraction to stretch and divide the medial periosteum. You should be able to open the medial surfaces by approximately 1 cm using this distraction technique.
- If the periosteum is adequately divided medially, the osteotomy will close and translate smoothly. If it resists closure, the contour of the wedge is likely too angulated, and additional bone must be resected medially.
- Grasp the posterior tuberosity fragment with a large tenaculum or towel clip.
- Translate the fragment laterally by several millimeters (to correct varus) and superiorly by several millimeters (to decrease calcaneal pitch and Achilles tension). The lateral translation is performed under direct vision, while the superior dorsal overhang is easily palpated.
5. Fixation Strategy
- While an assistant holds the tuberosity in the corrected, translated position, insert one or two guide pins across the osteotomy.
- The trajectory should start slightly posterior and lateral on the tuberosity segment, angling anteriorly, medially, and perpendicular to the osteotomy plane.
- Verify the correction and pin placement using intraoperative fluoroscopy (lateral and axial views).
- Overdrill and insert 6.5-mm or 7.0-mm cannulated cancellous screws.
- Screw Specifications: Use screws with a 16-mm thread length (typically 60 mm in overall length). It is imperative that the threads fully bypass the osteotomy site and purchase only in the anterior calcaneal body, allowing the smooth shank to provide interfragmentary compression.
- A single screw often provides excellent compression; however, if rotational stability or compression is suboptimal, insert a second parallel screw.
6. Lateral Ligament Reconstruction
Following the osteotomy, address the chronic lateral ankle instability.
* Identify the peroneal tendons. In CMT patients, the peroneus brevis is typically non-functional.
* Harvest the entire peroneus brevis tendon.
* Route the tendon through a drill hole in the distal fibula (e.g., utilizing a modified Chrisman-Snook or similar tenodesis technique) to anatomically reconstruct the anterior talofibular ligament (ATFL) and calcaneofibular ligament (CFL).
* Tension the graft with the ankle in neutral dorsiflexion and slight eversion, securing it with interference screws or suture anchors.
7. Closure
- Irrigate the wound copiously.
- Close the periosteum and subcutaneous tissues with interrupted 2-0 polyglactin 910 (Vicryl) sutures.
- Close the skin with 4-0 nylon sutures using a modified Donati or horizontal mattress technique to minimize skin edge necrosis.
- Apply a sterile dressing and a posterior plaster splint with the foot immobilized in a neutral position.
ALTERNATIVE TECHNIQUE: CRESCENTIC CALCANEAL OSTEOTOMY
For specific variations of calcaneocavus deformity—particularly those where a multiplanar wedge is not required, but a profound posterosuperior shift is needed—a crescentic osteotomy may be employed.
Surgical Steps for Crescentic Osteotomy
- Plantar Fasciotomy: Begin with a percutaneous or open plantar fasciotomy to release the rigid cavus tether.
- Incision and Protection: Utilize a similar lateral approach, meticulously identifying and protecting the peroneal tendons and sural nerve.
- The Osteotomy: Make a crescentic (dome-shaped) osteotomy in the calcaneus, positioned posterior to the subtalar joint. This can be achieved using a curved blade on a Stryker oscillating saw, or by creating multiple contiguous drill holes and connecting them with a large curved osteotome.
- Displacement: Shift the freed posterior tuberosity posterosuperiorly along the crescentic osteotomy line. This sliding motion directly corrects the calcaneocavus posture.
- Fixation: Secure the translated fragment using heavy orthopedic staples or multiple threaded Kirschner wires. (Note: Screw fixation is less commonly used for crescentic cuts due to the sliding geometry).
- Closure: Close the wound in standard fashion and apply a non-weight-bearing short-leg cast.
POSTOPERATIVE CARE AND REHABILITATION
The postoperative protocol varies slightly depending on the rigidity of the fixation used (screws vs. K-wires/staples).
Protocol for Saxby and Myerson Triplanar Osteotomy (Screw Fixation)
- Days 0 to 10: The patient is strictly non-weight-bearing (NWB) in the initial posterior plaster splint. Elevation is critical to manage edema and protect the lateral incision.
- Day 10 to 14: The splint is removed, and skin sutures are extracted. A short-leg walking cast (or rigid CAM boot, depending on surgeon preference and patient compliance) is applied.
- Weeks 2 to 6: The patient is allowed progressive weight-bearing in the cast/boot for an additional 4 weeks.
- Week 6 Onward: Radiographs are obtained to confirm osseous union. Once bridging trabeculae are visible, the patient transitions to supportive footwear and begins formal physical therapy focusing on ankle proprioception, peroneal strengthening (if applicable), and gait retraining.
Protocol for Crescentic Osteotomy (K-wire/Staple Fixation)
- Weeks 0 to 6: Due to the inherently less rigid nature of staple or K-wire fixation in a sliding crescentic osteotomy, strict non-weight-bearing is enforced for a full 6 weeks in a short-leg cast.
- Weeks 6 to 10: Following radiographic confirmation of early healing, a short-leg walking cast is applied and worn for another 4 weeks until the osteotomy site is completely consolidated.
COMPLICATIONS AND MANAGEMENT
While highly effective, the triplanar osteotomy carries specific surgical risks:
* Sural Nerve Injury: The most common complication. Meticulous dissection and superior retraction are mandatory. If transected, the nerve should be buried deep into muscle belly to prevent superficial neuroma formation.
* Undercorrection: Usually results from failure to adequately release the medial periosteum or failure to resect a sufficiently large lateral wedge. Intraoperative fluoroscopy and the lamina spreader technique are vital preventative measures.
* Wound Dehiscence: The lateral calcaneal skin is tenuous. Avoid excessive retraction, use full-thickness flaps, and ensure tension-free closure.
* Nonunion/Delayed Union: Rare with rigid 6.5/7.0 mm screw fixation, but risk increases in patients with poor vascularity or those who smoke. Ensure all cancellous debris is removed from the osteotomy site to allow flush bony apposition.
CONCLUSION
The triplanar calcaneal osteotomy, particularly when combined with lateral ligament reconstruction using the peroneus brevis, is a formidable tool in the orthopedic surgeon's armamentarium. By addressing the varus malalignment, correcting the calcaneal pitch, and restoring lateral stability, this joint-sparing procedure provides durable, functional outcomes for patients suffering from complex calcaneocavovarus deformities. Strict adherence to preoperative planning, meticulous soft-tissue handling, and precise geometric bone resection are the cornerstones of surgical success.
You Might Also Like